Hospice Acquired Private Equity Dementia Patient Care
Hospice acquired private equity public companies dementia patient home care JAMA Network Open – wow, that’s a mouthful, right? But it speaks to a really important and complex issue: the intersection of big business, healthcare, and the often heartbreaking realities of caring for dementia patients at the end of life. This post dives into the world of for-profit hospices, exploring the financial incentives, the potential impacts on care quality, and the ethical considerations involved.
We’ll look at how private equity shapes the landscape, examining both the benefits and drawbacks, and consider the role of publicly traded companies as reported in the JAMA Network Open. It’s a multifaceted topic, and I hope to shed some light on its complexities.
We’ll be examining the practical aspects of dementia care within a hospice setting, including best practices for symptom management and effective communication with families. We’ll also consider the differences between home-based and facility-based care, discussing the crucial role of family caregivers and the resources available to support them. Ultimately, this exploration aims to foster a deeper understanding of the challenges and opportunities in providing compassionate, high-quality hospice care for individuals with dementia.
Hospice Care and Private Equity Involvement
The increasing involvement of private equity firms in the hospice industry is a complex issue with significant implications for patients, families, and the healthcare system as a whole. While private equity investment can bring capital and operational expertise to improve efficiency and expand access, concerns remain regarding the potential prioritization of profits over patient care. Understanding the financial mechanisms and potential consequences is crucial for navigating this evolving landscape.
Financial Implications of Private Equity Investment in Hospice Care
Private equity firms typically invest in hospice providers with the goal of increasing profitability and eventually selling their stake at a significant profit. This often involves strategies aimed at improving operational efficiency, such as consolidating smaller providers, streamlining administrative processes, and negotiating better rates with suppliers. However, these strategies can sometimes lead to cost-cutting measures that may impact the quality of care delivered.
For example, reducing staffing levels or limiting access to certain therapies to enhance profit margins could negatively affect patient well-being. The financial returns for private equity investors are largely dependent on the successful implementation of these strategies and the subsequent increase in the hospice’s market value.
Comparison of For-Profit and Non-Profit Hospice Business Models
For-profit hospices, often backed by private equity, operate with the primary goal of generating profit for their investors. Their business models focus on maximizing revenue and minimizing expenses. In contrast, non-profit hospices prioritize patient care and reinvest their surpluses back into improving services and expanding their reach. While both types of hospices must adhere to regulatory standards, their underlying motivations and financial structures differ significantly.
For-profit hospices may be more inclined to pursue strategies that enhance short-term profitability, potentially at the expense of long-term patient care quality. Non-profit hospices, having a different financial structure and mission, might be better positioned to invest in comprehensive patient support services, even if those services don’t directly translate to increased revenue.
Potential Impact of Private Equity Ownership on the Quality of Hospice Care
The impact of private equity ownership on hospice care quality is a subject of ongoing debate. While some argue that private equity investment can improve efficiency and lead to better outcomes, others express concern that the focus on profitability might compromise the quality of care. Studies have shown mixed results, with some suggesting a correlation between private equity ownership and reduced staffing levels or increased patient turnover.
It’s crucial to note that the quality of care is not solely determined by ownership structure but is also influenced by factors such as staffing ratios, access to resources, and the overall culture of the hospice provider. Further research is needed to fully understand the long-term effects of private equity investment on patient care.
Key Performance Indicators (KPIs) for Hospices Under Different Ownership Structures
| KPI | For-Profit Hospice (Private Equity-backed) | Non-Profit Hospice | Government-Run Hospice |
|---|---|---|---|
| Patient Satisfaction Scores | Potentially lower due to pressure on staffing and resources | Generally higher due to focus on patient well-being | Variable, depends on funding and resources |
| Staffing Ratios (RNs per patient) | Potentially lower due to cost-cutting measures | Generally higher, reflecting commitment to patient care | Variable, subject to government budgetary constraints |
| Length of Stay | Potentially shorter, potentially influenced by efficiency targets | Variable, determined by patient needs | Variable, depends on patient needs and resource availability |
| Readmission Rates | Potentially higher due to potential pressure to discharge patients sooner | Variable, depends on patient health and support systems | Variable, depends on patient health and post-discharge support |
Dementia Patient Care in Hospice Settings
Hospice care for individuals with dementia presents unique challenges that differ significantly from caring for patients with other terminal illnesses. The progressive nature of the disease, coupled with the often unpredictable behavioral changes and communication difficulties, requires a highly specialized and compassionate approach. Successful hospice care in this context hinges on a multifaceted strategy encompassing symptom management, comfort measures, and effective communication with both the patient and their family.
Challenges in Providing Hospice Care for Dementia Patients
Dementia significantly impacts a patient’s ability to communicate their needs and preferences, making accurate assessment of pain and other symptoms a considerable hurdle. Behavioral changes, such as agitation, aggression, or wandering, can be distressing for both the patient and caregivers, demanding careful management and a calming environment. Furthermore, the fluctuating cognitive abilities of dementia patients can make consistent symptom monitoring and treatment adjustment a complex undertaking.
Finally, providing care for dementia patients often requires specialized training and expertise for hospice staff to effectively manage the unique challenges posed by the disease.
Best Practices for Managing Symptoms and Providing Comfort
Effective symptom management is paramount. This involves a multi-pronged approach that includes pharmacological interventions for pain, anxiety, and agitation, as well as non-pharmacological strategies like music therapy, aromatherapy, and reminiscence therapy. Creating a safe and predictable environment is crucial. This can involve familiar objects, routines, and consistent caregivers to reduce confusion and anxiety. Regular monitoring of vital signs and close observation for changes in behavior are essential for timely intervention.
Comfort measures focus on minimizing physical discomfort through proper positioning, skin care, and bowel and bladder management. Finally, ensuring the patient’s dignity and respect is vital throughout the care process.
Care Plan for a Hypothetical Dementia Patient
Let’s consider Mrs. Smith, an 85-year-old woman with advanced Alzheimer’s disease receiving hospice care at home. Her care plan would include: daily assessments of pain and agitation levels using validated scales; regular administration of prescribed medications to manage symptoms; implementation of a structured daily routine to minimize confusion; use of reminiscence therapy using photographs and familiar music to stimulate positive memories; and frequent repositioning to prevent pressure sores.
Her family would be actively involved in care, and trained in basic care techniques and symptom recognition. Regular communication with the hospice team would ensure timely adjustments to the care plan based on Mrs. Smith’s changing needs.
Effective Communication Strategies for Families
Open and honest communication with families is critical. Regular family meetings should be scheduled to provide updates on the patient’s condition, address concerns, and offer emotional support. Active listening and empathy are crucial in acknowledging the family’s grief and anxieties. Providing education on dementia and hospice care can empower families to participate effectively in their loved one’s care.
Clear and concise explanations of medical terms and treatment plans, avoiding jargon, are essential. The hospice team should also be available for emotional support and bereavement counseling, both during and after the patient’s passing. Written materials summarizing key information can serve as valuable resources for families.
Home Care for Dementia Patients

Source: huntsvillehealthcarecenter.com
Providing compassionate care for individuals with dementia, especially in their final stages of life, requires careful consideration of the setting and support systems. The decision between home-based hospice care and facility-based care significantly impacts the patient’s quality of life and the burden on family caregivers. This section explores the nuances of home care for dementia patients, highlighting its benefits and challenges.
Home-Based Hospice Care Versus Facility-Based Care for Dementia Patients
Home-based hospice care offers a familiar and comfortable environment for dementia patients, reducing the stress associated with relocation and unfamiliar surroundings. Patients can maintain a sense of normalcy and routine, surrounded by cherished possessions and loved ones. However, providing comprehensive care at home requires significant commitment from family caregivers, who may face physical and emotional exhaustion. Facility-based care, conversely, offers professional 24/7 support, relieving the strain on family members.
Yet, it can lead to feelings of isolation and disorientation for the patient, potentially exacerbating dementia symptoms. The optimal choice depends on the individual’s needs, the availability of family support, and access to home healthcare services. A careful assessment of the patient’s condition and the family’s capabilities is crucial in determining the best approach.
The Role of Family Caregivers in Providing Home-Based Hospice Care for Dementia Patients
Family caregivers play a pivotal role in ensuring the comfort and well-being of dementia patients receiving home-based hospice care. Their presence provides emotional support, familiarity, and a sense of security. Caregivers often assist with activities of daily living, such as bathing, dressing, and feeding, as well as medication management and monitoring for changes in the patient’s condition. This responsibility, however, can be physically and emotionally demanding, leading to caregiver burnout.
Therefore, it is crucial for caregivers to prioritize their own well-being and seek respite care when needed. Open communication with the hospice team and other support systems is essential to manage the challenges effectively. For example, a caregiver might utilize respite care for a few hours each week to prevent burnout and maintain their ability to provide consistent and quality care.
Resources and Support Systems Available to Families Caring for Dementia Patients at Home
Numerous resources and support systems are available to families caring for dementia patients at home. Hospice agencies provide comprehensive medical and emotional support, including skilled nursing visits, medication management, and bereavement counseling. Support groups offer a platform for caregivers to connect with others facing similar challenges, share experiences, and receive emotional support. Governmental and non-profit organizations offer financial assistance, caregiver training, and respite care services.
For instance, the Alzheimer’s Association provides extensive resources, including education, support groups, and a 24/7 helpline. Accessing these resources is critical in mitigating the burden on family caregivers and ensuring the patient receives the best possible care.
Essential Considerations for Ensuring a Safe and Comfortable Home Environment for a Dementia Patient Receiving Hospice Care
Creating a safe and comfortable home environment for a dementia patient receiving hospice care involves several key considerations. Home modifications, such as removing tripping hazards and installing grab bars, enhance safety and mobility. A simplified and clutter-free environment reduces confusion and agitation. Visual cues, such as large clocks and calendars, can help orient the patient. The use of calming techniques, such as playing familiar music or engaging in reminiscence therapy, can alleviate anxiety and promote relaxation.
Regular monitoring of the patient’s condition and prompt communication with the hospice team are crucial to address any emerging needs or concerns. For example, a simple modification such as brightly colored contrasting tape on the edges of steps can dramatically improve safety. These measures aim to create a supportive and nurturing environment where the patient feels secure and comfortable during their final days.
Public Companies and Hospice Care
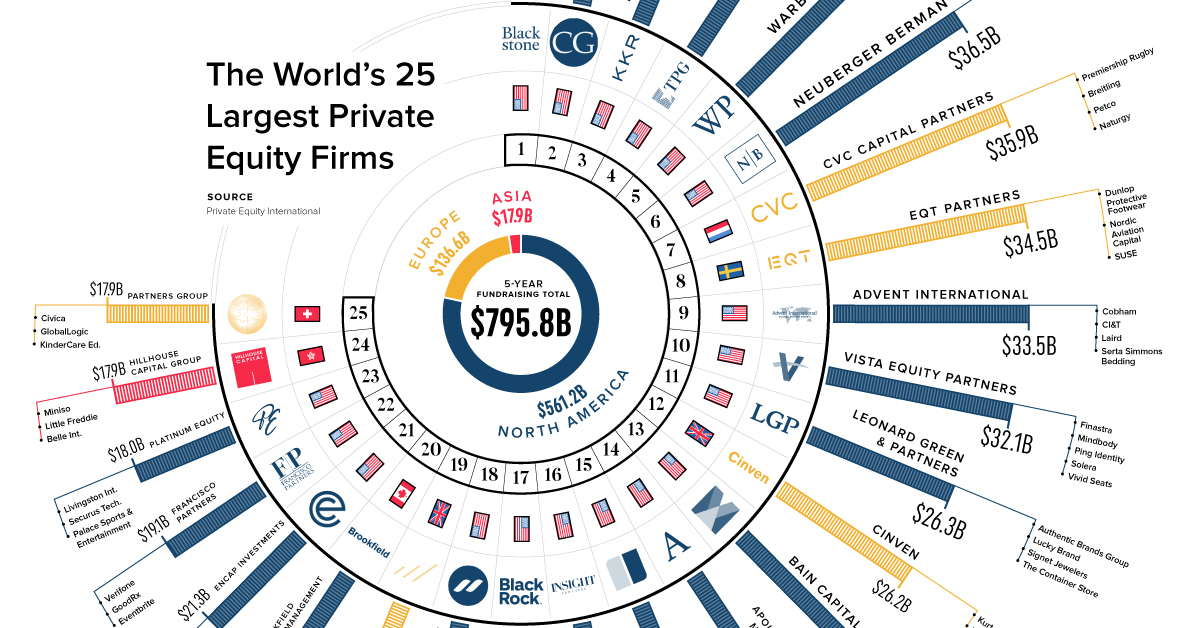
Source: visualcapitalist.com
The increasing involvement of publicly traded companies in the hospice care industry presents a complex landscape with both opportunities and challenges. Understanding the trends, financial performance, and regulatory environment surrounding these companies is crucial for stakeholders, including patients, families, and healthcare policymakers. This examination delves into relevant research from the JAMA Network Open to shed light on this evolving sector.
JAMA Network Open, a peer-reviewed, open-access medical journal, offers valuable insights into various aspects of healthcare delivery, including hospice care. Analyzing articles published within this journal allows for a data-driven assessment of the public company presence in hospice and its implications for the quality and accessibility of end-of-life care.
Trends in Hospice Care Provision by Public Companies
Publicly traded hospice companies often exhibit a focus on efficiency and scalability. This can manifest in strategies like acquiring smaller, independent hospice providers, leading to a consolidation of the market. Another trend is the increasing integration of technology into care delivery, such as telehealth platforms for remote monitoring and virtual consultations. This integration aims to improve efficiency and potentially expand the reach of services, though it also raises questions about the potential impact on the personal touch that is often considered vital in hospice care.
Further, some publicly traded companies are expanding their service offerings beyond traditional hospice care to include palliative care and other supportive services, creating a more comprehensive care model.
Financial Performance Comparison: Public vs. Non-Public Hospice Companies
Direct comparisons of financial performance between public and non-public hospice companies are difficult due to limited publicly available data on the latter. However, publicly traded companies are generally subject to more stringent financial reporting requirements, providing greater transparency into their revenue streams, profitability, and operational costs. This transparency allows for easier analysis of factors such as return on investment, revenue growth, and operating margins.
Anecdotal evidence suggests that public companies may exhibit higher growth rates due to their access to capital markets, allowing for strategic acquisitions and expansion. However, it’s important to note that profitability can vary significantly depending on factors like geographic location, service mix, and reimbursement rates. A comprehensive comparative analysis would require access to a broader dataset than is currently readily available.
Regulatory Landscape for Public Hospice Companies
Publicly traded hospice companies are subject to a complex web of regulations at both the federal and state levels. These regulations encompass aspects such as Medicare and Medicaid reimbursement policies, licensing requirements, and compliance with standards of care. The Centers for Medicare & Medicaid Services (CMS) plays a central role in overseeing hospice reimbursement and quality assurance. Public companies must adhere to strict financial reporting standards mandated by the Securities and Exchange Commission (SEC), which further adds to the regulatory burden.
The rising tide of private equity acquisitions in hospice care, particularly impacting dementia patient home care as highlighted in a recent JAMA Network Open article, is further complicated by severe staffing shortages. This is a huge problem, as healthcare executives say talent acquisition and labor shortages are a major business risk , making it even harder for these already stretched companies to provide adequate care.
The pressure on these publicly traded hospice providers to maintain profitability only intensifies the situation for both patients and caregivers.
Failure to comply with these regulations can result in significant financial penalties and reputational damage. The regulatory landscape is constantly evolving, requiring ongoing adaptation and compliance from public hospice providers.
Ethical Considerations in Hospice Care for Dementia Patients
Providing hospice care for individuals with dementia presents unique and complex ethical challenges. The progressive nature of the disease often obscures the patient’s wishes and capacity for self-determination, forcing caregivers and families to grapple with difficult end-of-life decisions in the absence of clear directives. This necessitates a careful consideration of ethical principles to ensure the patient’s dignity, comfort, and autonomy are respected throughout their care.
End-of-Life Decision-Making for Dementia Patients
Determining the appropriate course of action at the end of life for a dementia patient is fraught with ethical complexities. As the disease progresses, patients often lose the capacity to express their preferences regarding medical treatment, life-sustaining measures, or even basic daily care. This leaves family members and healthcare professionals responsible for making decisions on their behalf, raising concerns about substituted judgment and the potential for conflict between what the patient might have wanted and what is deemed to be in their best interests.
The process requires careful consideration of the patient’s past wishes, values, and beliefs, as well as a thorough assessment of their current condition and prognosis. Advance care planning, including the creation of advance directives like living wills and durable power of attorney for healthcare, plays a crucial role in guiding these difficult decisions.
Informed Consent and Patient Autonomy in Dementia Care
The principle of informed consent, a cornerstone of medical ethics, becomes particularly challenging in the context of dementia. As cognitive decline progresses, patients may lose the capacity to understand their medical condition, treatment options, and the potential risks and benefits involved. Maintaining patient autonomy requires a delicate balance between respecting the patient’s remaining capacity and recognizing the limitations imposed by the disease.
This often involves engaging family members in the decision-making process, ensuring they are fully informed and understand the patient’s wishes to the best of their ability. Furthermore, healthcare professionals have a responsibility to provide clear and concise information to the family, addressing their concerns and supporting them in making informed decisions that align with the patient’s best interests.
Open communication and shared decision-making are paramount.
Potential Conflicts of Interest in Hospice Care Provision
The involvement of private equity firms in hospice care raises concerns about potential conflicts of interest. The profit-driven nature of these companies might incentivize cost-cutting measures that could compromise the quality of care provided to patients. This could manifest in understaffing, inadequate training for personnel, or a focus on maximizing profits rather than prioritizing patient well-being. Transparency regarding ownership structures, financial incentives, and the allocation of resources is crucial to mitigate these risks.
Regulatory oversight and robust ethical guidelines are essential to ensure that financial interests do not supersede the ethical obligations of providing compassionate and high-quality hospice care. For example, a private equity-owned hospice might prioritize shorter patient stays to maximize revenue, potentially neglecting patients’ needs for longer-term care.
Ethical Dilemmas in Dementia Patient Hospice Care and Proposed Solutions
Several ethical dilemmas can arise in the care of dementia patients in hospice. One common example is the decision to withhold or withdraw life-sustaining treatment. When a patient lacks the capacity to consent, family members may disagree on the best course of action, leading to emotional distress and ethical conflicts. Another dilemma involves the use of antipsychotic medications to manage behavioral disturbances associated with dementia.
While these medications can improve patient comfort and reduce caregiver burden, they also carry significant side effects and risks. Balancing the benefits and risks of medication requires careful consideration of the patient’s individual circumstances and preferences, as well as open communication with family members. To address these dilemmas, ethical consultation and multidisciplinary care teams, including ethicists, physicians, nurses, social workers, and family members, can help navigate complex decisions, fostering open dialogue and ensuring that all voices are heard.
Establishing clear communication protocols and providing access to ethical resources can help resolve conflicts and promote ethically sound decision-making.
The recent JAMA Network Open article highlighting the challenges of dementia patient home care within the context of hospice acquired by private equity public companies got me thinking about the larger healthcare landscape. This is especially relevant considering Walgreens’ positive outlook, fueled by their Summit acquisition, as reported here: walgreens raises healthcare segment outlook summit acquisition.
The implications for expanding access to quality home care, especially for vulnerable dementia patients, are significant, given the increasing role of large corporations in this space.
Impact of Public Company Involvement on Dementia Care Access: Hospice Acquired Private Equity Public Companies Dementia Patient Home Care Jama Network Open
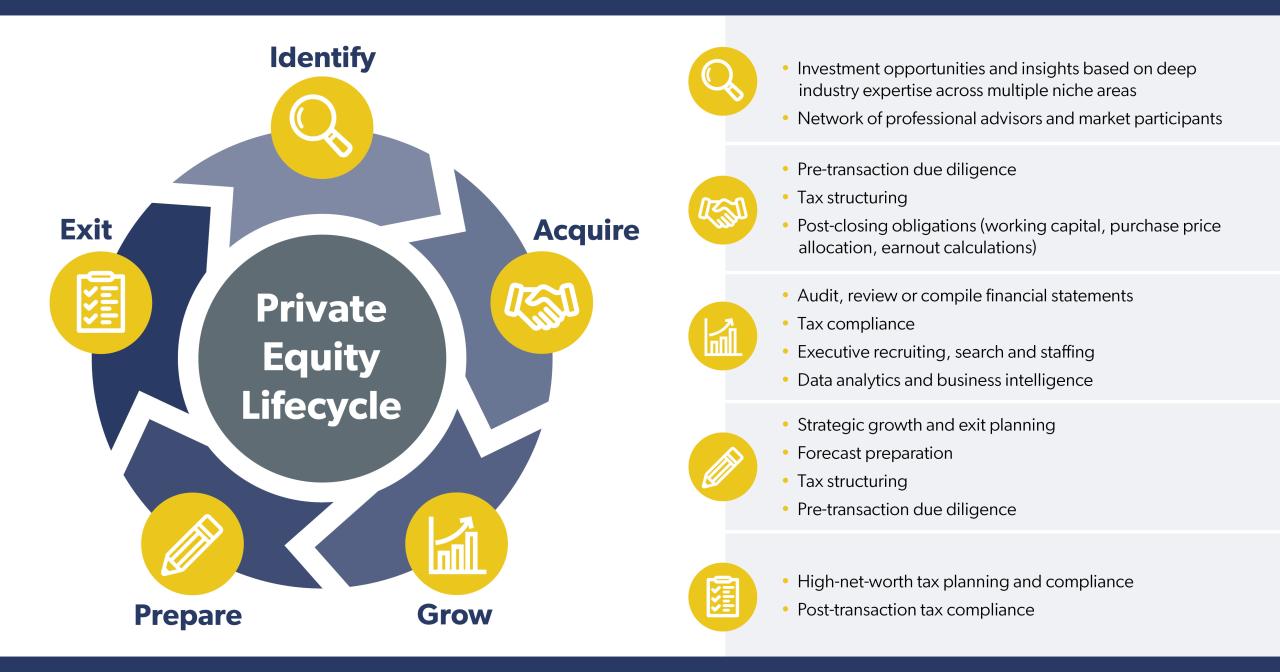
Source: cloudfront.net
The increasing involvement of publicly traded companies in the hospice care industry presents both opportunities and challenges for dementia patients, particularly concerning access to quality care, especially in underserved communities. This section explores the potential effects of this trend, examining accessibility disparities and the correlation between public company involvement and cost.
Accessibility of Hospice Services in Underserved Communities
Public company involvement in hospice care could theoretically improve access to services in underserved areas. Larger companies often have greater resources to expand geographically, potentially reaching communities previously lacking access to specialized dementia care. However, profit motives might lead to a prioritization of more lucrative markets, leaving underserved communities with limited or no improvement. For example, a publicly traded hospice company might focus its expansion efforts on affluent suburban areas with higher reimbursement rates, neglecting rural or economically disadvantaged regions where the need is often greatest.
This disparity necessitates a thorough investigation into the actual impact of public company involvement on accessibility in different geographic locations.
Comparison of Hospice Service Accessibility Across Regions
A comparative analysis of regions with varying concentrations of publicly traded hospice providers reveals significant disparities in access to care. Areas with a high concentration of such providers may experience increased competition, potentially leading to better pricing and a wider range of services. Conversely, regions with limited public company involvement might face restricted access, longer wait times, and higher costs due to limited competition and potentially less efficient, smaller, independent providers.
Data from Medicare claims and surveys on patient satisfaction could provide valuable insights into these regional differences, highlighting the true impact of provider type and density on care accessibility.
The JAMA Network Open article on hospice acquired by private equity and its impact on dementia patient home care really got me thinking. It highlights the complexities of the system, especially considering the recent news about the new york nurse strike deal reached at Mount Sinai and Montefiore ; the nurses’ fight for better patient care underscores the need for systemic reform within healthcare, directly impacting the quality of care available, even in specialized areas like dementia care within the private equity-owned hospice system.
Correlation Between Public Company Involvement and Cost of Hospice Care
The relationship between public company involvement and the cost of hospice care for dementia patients is complex and requires careful examination. While some argue that economies of scale achieved by large public companies could lead to lower costs, others express concern about potential profit maximization leading to higher prices. The actual cost impact will depend on several factors, including the company’s business model, the regulatory environment, and the specific services provided.
Analyzing cost data from various regions with differing levels of public company involvement is crucial to determining whether a clear correlation exists and to understand the nature of this correlation (positive, negative, or nonexistent).
Geographic Distribution of Hospice Care Providers and Ownership Structures, Hospice acquired private equity public companies dementia patient home care jama network open
Imagine a map of the United States. Each dot represents a hospice provider. The color of the dot indicates ownership structure: red for publicly traded companies, blue for non-profit organizations, and green for privately owned businesses. The size of the dot corresponds to the number of patients served. This visual representation would immediately highlight geographic disparities in access.
For instance, densely populated urban areas might be dominated by red dots, indicating a high concentration of public companies, while rural areas might show a preponderance of blue or green dots, reflecting a greater reliance on non-profit or privately owned providers. Such a map would provide a powerful illustration of the distribution of resources and the potential impact on dementia care access across diverse communities.
Closure
Navigating the world of hospice care, especially for dementia patients, is a journey fraught with emotional and logistical complexities. The involvement of private equity and publicly traded companies adds another layer to this intricate landscape, raising questions about profit motives versus patient well-being. While financial considerations are undeniably important, the core of excellent hospice care remains centered on providing comfort, dignity, and support to patients and their families.
This exploration hopefully highlighted the nuances of this crucial area, prompting further discussion and encouraging us all to advocate for the highest standards of care for those in their final stages of life.
Questions Often Asked
What are the potential downsides of private equity investment in hospice care?
Some critics worry that profit motives might lead to cost-cutting measures that compromise the quality of care, potentially impacting staffing levels, resources, and patient outcomes.
How does the regulatory environment affect publicly traded hospice companies?
Publicly traded companies are subject to stricter regulations and reporting requirements compared to privately owned hospices. This can impact their operations and financial decisions.
Are there specific challenges in providing home-based hospice care for dementia patients?
Yes, home-based care requires careful assessment of the home environment and the family’s ability to provide care. Specialized training and support are often needed for family caregivers.
What resources are available to support families caring for dementia patients at home?
Many resources exist, including support groups, respite care services, and government assistance programs. Local hospice organizations and Alzheimer’s associations are excellent starting points.