3 Trends That Will Define the Future of Healthcare
3 Trends That Will Define the Future of Healthcare: The healthcare landscape is undergoing a radical transformation, driven by technological advancements and evolving patient needs. We’re on the cusp of a future where personalized medicine, AI-powered diagnostics, and telehealth redefine how we prevent, diagnose, and treat illness. This exploration delves into these key trends, examining their potential to revolutionize the industry and the challenges we must overcome to fully realize their promise.
From the genetic blueprint informing individual treatment plans to AI algorithms assisting doctors in diagnosis and drug discovery, the changes are profound. The rise of telehealth is breaking down geographical barriers, offering remote access to care and empowering patients to actively manage their health. This isn’t just about technological innovation; it’s about creating a more equitable, efficient, and ultimately, healthier future for all.
The Rise of Personalized Medicine
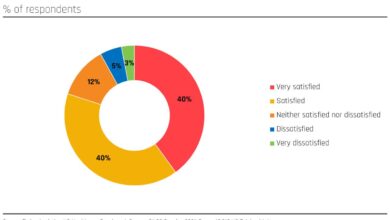
Source: ecosystm.io
Personalized medicine represents a paradigm shift in healthcare, moving away from a “one-size-fits-all” approach to treatments tailored to the unique genetic, environmental, and lifestyle factors of individual patients. This approach promises more effective therapies, reduced side effects, and improved overall health outcomes. It’s fueled by advancements in genomics and the exponential growth of big data, allowing for a deeper understanding of disease at a molecular level.Genomics and big data are revolutionizing how we diagnose and treat diseases.
Genomic sequencing allows us to identify individual genetic variations that influence disease susceptibility and response to treatment. Big data analytics, meanwhile, helps us integrate genomic information with other patient data – such as medical history, lifestyle factors, and environmental exposures – to create comprehensive patient profiles. This holistic view enables the development of highly targeted therapies and preventative strategies.
Examples of Personalized Medicine Applications
Several personalized medicine applications are already making a difference in patient care. Pharmacogenomics, for instance, analyzes how an individual’s genes affect their response to drugs. This allows doctors to prescribe the most effective medication and dosage, minimizing adverse reactions. For example, certain genetic variations can predict whether a patient will experience severe side effects from clopidogrel, a blood thinner.
Knowing this allows clinicians to choose an alternative medication. Another example is cancer treatment, where genomic profiling of tumors is used to guide targeted therapies. Identifying specific mutations within a cancer cell allows oncologists to select drugs that specifically target those mutations, leading to more effective treatment with fewer side effects compared to traditional chemotherapy. These targeted therapies are significantly improving outcomes for certain types of cancer.
Ethical Considerations of Genetic Information
The use of genetic information in healthcare raises important ethical considerations. Privacy and data security are paramount. Genetic information is highly sensitive, and robust safeguards are needed to prevent unauthorized access and misuse. Another key concern is genetic discrimination. There’s a risk that individuals could face discrimination in employment, insurance, or other areas based on their genetic predispositions to certain diseases.
Furthermore, the interpretation and communication of genetic information require careful consideration. Patients need clear and understandable explanations of their genetic test results and the implications for their health. The potential for psychological distress associated with receiving unfavorable genetic information also needs to be addressed. Informed consent is crucial to ensure patients understand the risks and benefits before undergoing genetic testing.
Hypothetical Personalized Medicine Program for Type 2 Diabetes
A personalized medicine program for Type 2 diabetes could integrate genetic testing to identify individuals at high risk, assess their response to different medications, and personalize lifestyle recommendations. The program would begin with a comprehensive assessment, including genetic testing to identify variations associated with diabetes risk and drug response. This would be coupled with detailed lifestyle assessments, including diet, physical activity levels, and stress management techniques.
Based on this information, a personalized treatment plan would be developed, including tailored medication regimens, dietary recommendations, and exercise programs. Regular monitoring and adjustments to the treatment plan would be essential, using continuous glucose monitors and other technologies to track progress and make necessary modifications. Challenges include the high cost of genetic testing and the need for robust data infrastructure to support the analysis and integration of diverse data sources.
Three trends shaping healthcare’s future are AI, personalized medicine, and remote monitoring. A key area benefiting from this shift is senior care, where effective collaboration is crucial; check out this insightful article on reimagining collaboration in senior care a technology driven approach for a deeper dive. Ultimately, these technological advancements will improve care access and outcomes across the board, influencing those three major trends significantly.
The program’s success would depend on strong patient engagement and the availability of qualified healthcare professionals to implement and monitor the personalized plans.
Thinking about the future of healthcare, I see three major trends emerging: AI-driven diagnostics, personalized medicine, and a greater focus on preventative care. The upcoming impact of these trends could be significantly shaped by who leads the charge, which is why the news that rfk jr clears key hurdle on path to hhs secretary is so interesting.
His stance on these issues will undoubtedly influence how these three trends play out, impacting the future of healthcare for all of us.
Cost-Benefit Comparison of Personalized Medicine vs. Traditional Approaches
| Feature | Personalized Medicine | Traditional Medicine |
|---|---|---|
| Cost | Higher upfront costs due to genetic testing and specialized treatments. | Lower upfront costs, but potential for higher long-term costs due to ineffective treatments and complications. |
| Effectiveness | Potentially more effective due to targeted treatments and preventative measures. | Less effective for some individuals due to the “one-size-fits-all” approach. |
| Side Effects | Potentially fewer side effects due to tailored treatments. | Higher risk of side effects due to generalized treatments. |
| Long-term Outcomes | Improved long-term health outcomes and quality of life. | Variable long-term outcomes, depending on individual response to treatment. |
Artificial Intelligence and Machine Learning in Healthcare

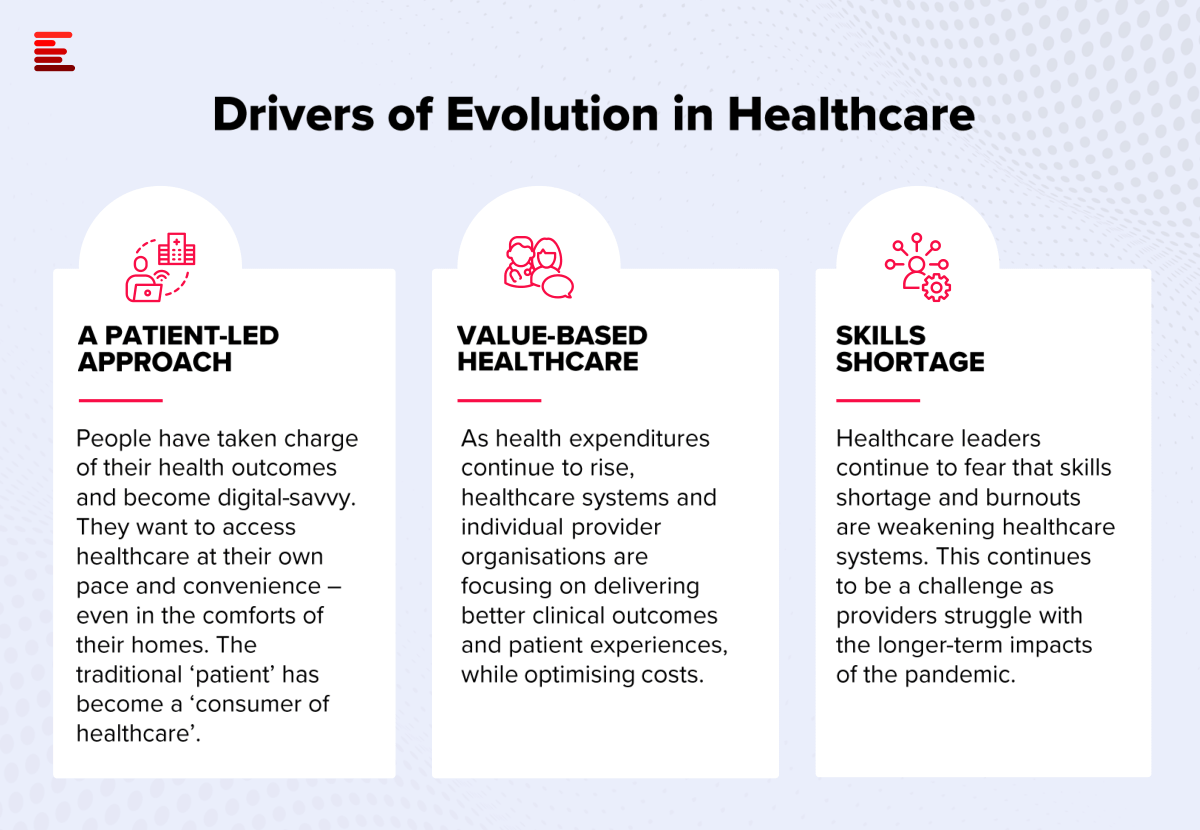
Source: ecosystm.io
The integration of artificial intelligence (AI) and machine learning (ML) is rapidly transforming healthcare, offering the potential to revolutionize diagnosis, treatment, and drug discovery. These technologies are no longer futuristic concepts; they are actively being implemented in various aspects of medical practice, leading to improved patient outcomes and more efficient healthcare systems. The power of AI and ML lies in their ability to analyze vast datasets, identify patterns imperceptible to humans, and make predictions with remarkable accuracy.AI’s potential applications in healthcare are vast and continuously expanding.
Its ability to process and interpret complex medical data allows for advancements across numerous specialties.
AI in Disease Diagnosis and Treatment Planning
AI algorithms are proving increasingly adept at analyzing medical images, such as X-rays, CT scans, and MRIs, to detect diseases like cancer at earlier stages than traditional methods. For example, AI-powered systems can identify subtle anomalies in mammograms that might be missed by a human radiologist, leading to earlier diagnosis and treatment. Beyond image analysis, AI can also integrate patient data, including medical history, genetic information, and lifestyle factors, to assist in developing personalized treatment plans.
This precision medicine approach tailors therapies to individual needs, potentially improving treatment efficacy and reducing adverse effects. AI can also help predict the likelihood of a patient developing certain conditions based on risk factors, enabling proactive interventions and preventative care.
Examples of AI-Powered Medical Devices and Software
Several AI-powered medical devices and software are already available. IBM Watson Oncology, for example, assists oncologists in making treatment decisions by analyzing patient data and suggesting evidence-based treatment options. PathAI uses AI to improve the accuracy of pathology diagnoses, reducing the potential for human error. IDx-DR is an FDA-cleared AI system that autonomously diagnoses diabetic retinopathy, a leading cause of blindness.
These examples demonstrate the practical applications of AI in improving diagnostic accuracy and treatment planning.
Challenges and Limitations of AI in Healthcare
Despite its immense potential, the adoption of AI in healthcare faces significant challenges. Data privacy is paramount, and ensuring the security and confidentiality of patient data is crucial. Algorithmic bias is another concern; if the data used to train AI algorithms is biased, the resulting algorithms may perpetuate and even amplify existing health disparities. The need for robust validation and regulatory oversight is essential to ensure the safety and efficacy of AI-powered medical devices and software.
Furthermore, the integration of AI into existing healthcare workflows requires significant investment in infrastructure and training.
Machine Learning in Predicting Patient Outcomes and Optimizing Resource Allocation
Machine learning algorithms can analyze large datasets of patient information to predict outcomes, such as the likelihood of readmission after surgery or the risk of developing complications. This predictive capability allows healthcare providers to proactively manage patients at high risk, potentially preventing adverse events and improving overall care. Furthermore, ML can optimize resource allocation by predicting patient demand, optimizing staffing levels, and improving the efficiency of hospital operations.
For instance, by predicting patient flow, hospitals can better manage bed capacity and reduce wait times.
AI Applications in Different Medical Specialties
The potential applications of AI span various medical specialties:
- Oncology: Cancer diagnosis, treatment planning, prognosis prediction.
- Cardiology: Heart disease risk prediction, arrhythmia detection, treatment optimization.
- Radiology: Image analysis for disease detection, improved diagnostic accuracy.
- Pathology: Automated cell and tissue analysis, improved diagnostic accuracy.
- Neurology: Disease diagnosis, treatment planning, monitoring of neurological conditions.
- Pharmacology: Drug discovery and development, personalized medicine.
Telehealth and Remote Patient Monitoring: 3 Trends That Will Define The Future Of Healthcare
Telehealth and remote patient monitoring (RPM) are rapidly transforming healthcare delivery, offering convenient and accessible care while potentially improving patient outcomes. This shift is driven by technological advancements, increasing healthcare costs, and a growing demand for patient-centered care. The integration of these technologies is not without its challenges, however, and careful consideration must be given to implementation strategies and infrastructure needs.Telehealth Advantages and Disadvantages Compared to Traditional In-Person CareTelehealth offers several key advantages over traditional in-person care.
It significantly improves access to care, particularly for patients in rural or underserved areas with limited access to specialists. Convenience is another major benefit, eliminating travel time and costs associated with visiting a clinic or hospital. Furthermore, telehealth can improve patient engagement through increased access to their healthcare providers and personalized care plans. However, telehealth is not without its drawbacks.
The digital divide, where access to technology and reliable internet connectivity is unevenly distributed, limits its reach for certain populations. Concerns about data privacy and security are also paramount, requiring robust security measures to protect sensitive patient information. Finally, the lack of physical examination in some telehealth encounters can limit the diagnostic capabilities compared to traditional in-person visits.
Successful Telehealth Implementations, 3 trends that will define the future of healthcare
Telehealth has demonstrated effectiveness across various healthcare needs. Chronic disease management, such as for diabetes or hypertension, benefits greatly from remote monitoring of vital signs and regular virtual consultations with healthcare providers. Mental health services, including therapy and counseling sessions, are increasingly delivered through telehealth platforms, expanding access to mental healthcare professionals. Similarly, telehealth has proven useful in post-surgical care, allowing for remote monitoring of patients’ recovery and early detection of potential complications, thus reducing hospital readmissions.
For example, the Mayo Clinic has successfully implemented telehealth programs for chronic disease management, resulting in improved patient outcomes and reduced healthcare costs. Another example is Teladoc, a leading telehealth provider offering virtual consultations for a wide range of medical conditions.
Remote Patient Monitoring and Improved Patient Outcomes
Remote patient monitoring (RPM) technologies, such as wearable sensors and connected medical devices, play a crucial role in improving patient outcomes and reducing hospital readmissions. By continuously monitoring vital signs like heart rate, blood pressure, and blood glucose levels, RPM allows for early detection of potential health issues. This proactive approach enables timely interventions, preventing complications and reducing the need for emergency room visits or hospitalizations.
For instance, RPM programs for heart failure patients have demonstrated a significant reduction in hospital readmissions and improved quality of life. Data collected through RPM systems also provide valuable insights into patient health trends, enabling healthcare providers to personalize treatment plans and improve overall care coordination.
Telehealth Infrastructure and Technological Requirements
Effective telehealth deployment requires a robust infrastructure and appropriate technology. High-speed internet access is crucial for reliable video conferencing and data transmission. Secure platforms for storing and sharing patient data are essential to maintain privacy and comply with regulations. In addition to the technological infrastructure, training for healthcare providers and patients on the use of telehealth technologies is necessary for successful implementation.
In areas with limited internet access, alternative solutions such as satellite internet or mobile broadband may be required. The cost of implementing and maintaining telehealth infrastructure can be significant, requiring investment in both technology and personnel. For example, rural healthcare providers may need government subsidies or partnerships with technology companies to overcome infrastructure limitations.
A Typical Telehealth Consultation
Imagine a patient sitting at home, using a tablet or laptop computer equipped with a high-definition camera and microphone. They are connecting to their physician via a secure video conferencing platform. The physician, located in a different city or even state, is using a similar setup. During the consultation, the patient and physician can see and hear each other clearly.
The patient may also be using connected medical devices, such as a blood pressure monitor or a glucose meter, to share real-time data with the physician. The physician can review the patient’s medical history and other relevant information displayed on their screen. The consultation concludes with the physician providing a diagnosis, treatment plan, and any necessary follow-up instructions.
The entire interaction is securely recorded and stored for future reference.
The Growing Importance of Preventative Care

Source: cobait.com
Preventative care, focusing on proactive health maintenance rather than reactive treatment, is increasingly recognized as a cornerstone of a sustainable and effective healthcare system. By shifting the emphasis from treating illnesses to preventing them, we can significantly reduce healthcare costs, improve overall population health, and enhance the quality of life for individuals. This approach requires a multi-faceted strategy involving individual responsibility, effective public health initiatives, and equitable access to preventative services.Preventative care significantly reduces healthcare costs by mitigating the need for expensive treatments and hospitalizations associated with chronic diseases.
Early detection and intervention through screenings, vaccinations, and lifestyle modifications can prevent or delay the onset of conditions like heart disease, diabetes, and cancer. This proactive approach leads to fewer emergency room visits, shorter hospital stays, and a decreased burden on the healthcare system as a whole. Moreover, a healthier population translates to increased productivity and reduced absenteeism in the workforce, further contributing to economic benefits.
So, what are the big three trends shaping healthcare’s future? AI-driven diagnostics and personalized medicine are definitely up there, alongside telehealth expansion. But ensuring equitable access is crucial, and that’s where the work of Rene Quashie at the Consumer Technology Association shines, as highlighted in this insightful article on the ais health equity revolution rene Quashie consumer technology association.
Ultimately, these three trends, combined with a focus on equity, will redefine how we receive and experience healthcare.
Successful Preventative Care Programs and Their Impact
Several successful preventative care programs demonstrate the effectiveness of this approach. For example, widespread vaccination campaigns have virtually eradicated diseases like polio and measles, dramatically improving global public health. Similarly, organized screenings for colorectal cancer, through programs like the National Colorectal Cancer Roundtable in the US, have led to earlier detection and improved survival rates. These programs highlight the significant impact that well-designed and implemented preventative care initiatives can have on health outcomes.
The reduction in mortality rates and improved quality of life associated with these programs underscore the value of investing in preventative care.
Barriers to Accessing Preventative Care
Despite the clear benefits, significant barriers exist to accessing preventative care, particularly for underserved populations. Socioeconomic factors play a crucial role, with individuals facing financial constraints, lack of health insurance, and limited access to transportation often unable to afford or reach preventative services. Geographic location is another key barrier, with individuals in rural or underserved areas facing significant challenges in accessing healthcare facilities offering preventative services.
Furthermore, language barriers, cultural beliefs, and a lack of health literacy can also hinder access to and utilization of preventative care. Addressing these systemic inequalities is critical to ensuring equitable access to preventative services for all.
The Role of Public Health Initiatives
Public health initiatives play a vital role in promoting preventative care through various strategies. These initiatives include public awareness campaigns aimed at educating the public about the importance of preventative care, the development and implementation of evidence-based guidelines for preventative services, and the creation of supportive environments that encourage healthy behaviors. Government regulations, such as mandatory vaccinations for children entering school, also contribute to the success of preventative care initiatives.
Moreover, public health agencies conduct surveillance and monitoring to identify and address emerging health threats, further promoting population health. Investment in public health infrastructure and workforce is essential for effective implementation of preventative care programs.
Improving Access to Preventative Care in a Specific Community: A Plan for Urban Neighborhood X
To improve access to preventative care in the underserved urban neighborhood of “X,” a comprehensive plan is needed. This plan will focus on addressing the barriers identified earlier. Resource allocation will prioritize establishing a community health center within easy reach of residents, offering affordable screenings, vaccinations, and health education programs. Outreach efforts will include culturally sensitive educational campaigns using multiple languages and accessible formats.
Transportation assistance will be provided to overcome geographic barriers. Partnerships with local organizations and community leaders will be crucial in building trust and ensuring the program’s success. This multi-pronged approach, addressing both systemic and individual barriers, aims to significantly improve preventative care access and health outcomes for the residents of neighborhood X. Funding will be sought through grants, public health initiatives, and community fundraising.
Last Word
The future of healthcare is undeniably intertwined with personalized medicine, artificial intelligence, and telehealth. While challenges remain – ethical considerations surrounding genetic data, algorithmic bias in AI, and ensuring equitable access to technology – the potential benefits are immense. By embracing these trends responsibly and strategically, we can pave the way for a healthcare system that is more precise, efficient, accessible, and ultimately, more patient-centered.
The journey will be transformative, and the destination promises a healthier world.
Expert Answers
What are the biggest privacy concerns with personalized medicine?
The biggest concern is unauthorized access and misuse of sensitive genetic information. Strict data security protocols and regulations are crucial to protecting patient privacy.
How reliable are AI diagnoses compared to human doctors?
AI is a tool to assist, not replace, doctors. While AI can be highly accurate in specific areas, human expertise is still essential for complex cases and nuanced judgment.
Will telehealth completely replace in-person visits?
No. Telehealth is a valuable supplement, particularly for routine checkups and monitoring. However, in-person care remains essential for many conditions requiring physical examinations and hands-on treatment.
What are the costs associated with implementing telehealth infrastructure?
Costs vary depending on the scale and complexity of the implementation, including technology investment, training, and ongoing maintenance. However, long-term cost savings are often realized through reduced hospital readmissions and improved patient outcomes.