Biden Mental Health Parity Health Insurance Rule
Biden mental health parity health insurance rule – Biden’s Mental Health Parity health insurance rule aims to finally level the playing field for mental healthcare access. For too long, mental health treatment has been unfairly treated differently than physical health in insurance coverage. This rule seeks to rectify that, mandating that health insurance plans provide equal coverage for mental health and substance use disorder treatment, just like they do for physical health conditions.
It promises to change the lives of millions struggling to access the care they desperately need.
This rule builds upon previous efforts but includes significant improvements and stronger enforcement mechanisms. We’ll explore the key provisions, analyze its impact on access and costs, and examine the challenges of implementation. We’ll also delve into real-world patient experiences, discuss future directions, and address frequently asked questions surrounding this crucial legislation.
The Biden Administration’s Mental Health Parity Rule
The Biden administration has significantly strengthened the Mental Health Parity and Addiction Equity Act (MHPAEA) of 2008, aiming to ensure that health insurance coverage for mental health and substance use disorder (SUD) treatment is comparable to coverage for medical and surgical care. This isn’t just about equal access; it’s about dismantling systemic inequalities that have historically left individuals struggling with mental health and SUD issues facing significant barriers to care.The key provisions of the strengthened rule focus on improving enforcement, clarifying ambiguous aspects of the original legislation, and increasing transparency.
This means insurance companies are held to a higher standard of accountability, making it easier to identify and address disparities in coverage. The administration’s efforts are designed to prevent insurers from creating unnecessary obstacles to accessing essential mental healthcare services.
Specific Requirements for Health Insurance Plans
The strengthened parity rule mandates that health plans must apply the same criteria for determining medical necessity, coverage limitations, and treatment limitations to both medical/surgical benefits and mental health/SUD benefits. This means that if a plan covers a certain number of physical therapy sessions, it must offer a comparable number of sessions for mental health therapy. Similarly, any prior authorization requirements, cost-sharing (copays, deductibles, etc.), and network adequacy standards must be consistent across all covered benefits.
The rule also addresses issues like limitations on the number of days of inpatient care or the duration of outpatient treatment, ensuring that these limitations are not more restrictive for mental health and SUD treatment than for other medical conditions. Failure to comply can result in significant penalties for insurance providers.
Comparison to Previous Parity Rules: Key Differences and Improvements
While the MHPAEA of 2008 established the foundational principle of parity, its implementation was often inconsistent and lacked strong enforcement mechanisms. The Biden administration’s rule strengthens enforcement by requiring insurers to provide more detailed documentation justifying any differences in coverage between mental health/SUD services and medical/surgical services. It also clarifies previously ambiguous terms and definitions, leaving less room for insurers to exploit loopholes.
President Biden’s mental health parity rule is a huge step forward, ensuring equal coverage for mental and physical healthcare. It makes me wonder, though, about the implications for companies like NextGen Healthcare, which, according to this Reuters article, nextgen exploring sale reuters , is exploring a sale. Will a change in ownership impact their commitment to providing compliant systems for the new parity standards?
Ultimately, the success of Biden’s initiative depends on widespread adoption and robust technology supporting it.
For example, the updated rule provides clearer guidance on the application of parity to different types of mental health and SUD services, such as residential treatment, medication management, and crisis care. This improved clarity reduces the potential for insurers to deny or limit coverage based on technicalities. The focus is on ensuring that individuals can access the full continuum of care they need, without facing unnecessary financial or administrative barriers.
Furthermore, increased transparency requirements allow for better monitoring of compliance and easier identification of discriminatory practices. The administration’s actions are geared towards empowering individuals to access the care they deserve, fostering a more equitable and just healthcare system.
Impact on Insurance Coverage

Source: googleusercontent.com
The Biden Administration’s Mental Health Parity and Addiction Equity Act significantly alters the landscape of mental healthcare insurance coverage in the United States. Its aim is to ensure that mental health and substance use disorder benefits are treated no differently than medical/surgical benefits under group health plans. This parity, however, has far-reaching consequences, impacting access, cost, and the types of services offered.
Increased Access to Mental Healthcare Services
The rule’s primary impact is on accessibility. Prior to its full implementation, many individuals faced significant barriers to accessing necessary mental healthcare. High out-of-pocket costs, limited networks of providers, and restrictive benefit designs often prevented individuals from seeking or receiving the care they needed. The Parity Act aims to dismantle these barriers by requiring insurers to offer comparable coverage for mental health and substance use disorder treatment as they do for physical health conditions.
This means improved access to therapy, medication management, inpatient treatment, and other essential services. For example, a person previously denied coverage for intensive outpatient therapy might now find it readily available with comparable cost-sharing as for physical therapy.
Cost Implications for Individuals and Insurance Providers
While improved access is a key goal, the rule’s impact on cost is complex. For individuals, the expectation is a reduction in out-of-pocket expenses for mental healthcare, as cost-sharing should align with that of physical healthcare. However, the increased utilization of mental healthcare services, a likely consequence of improved access, could lead to higher overall premiums for everyone.
For insurance providers, the immediate costs may increase due to the expanded coverage, but this might be offset by long-term benefits like reduced hospitalizations and improved overall health outcomes, leading to potential cost savings in the long run. The actual financial impact remains to be fully seen and will vary depending on factors such as the insurer’s specific plan design and the demographics of their insured population.
Influence on Types of Mental Health Services Offered
The Parity Act influences the types of mental health services offered by encouraging a wider range of treatment options. Insurers are less likely to restrict access to specific therapies or limit the number of sessions, as they would be required to offer comparable benefits to those offered for physical health treatments. This could lead to a greater emphasis on evidence-based practices, a broader selection of therapists and specialists, and potentially an increase in the availability of innovative treatment approaches.
For instance, telehealth services, previously limited in some plans, are now more likely to be covered equally to in-person visits, reflecting a change in service delivery models.
Comparison of Mental Health Service Coverage Before and After the Rule
| Service | Coverage Before Parity (Example) | Coverage After Parity (Example) |
|---|---|---|
| Individual Therapy Sessions | Limited to 10 sessions per year, high copay | Unlimited sessions within reasonable limits, copay comparable to physical therapy |
| Medication Management | Restricted to specific medications, prior authorization required | Broader range of medications covered, reduced prior authorization requirements |
| Inpatient Treatment | Limited number of days covered, high deductible | Increased coverage for inpatient stays, deductible comparable to medical/surgical care |
| Telehealth Services | Often excluded or severely limited | Covered at the same rate as in-person visits |
Challenges in Implementation and Enforcement
The Biden Administration’s Mental Health Parity and Addiction Equity Act (MHPAEA) aims to ensure equal coverage for mental health and substance use disorder treatment as for medical and surgical care. However, achieving true parity faces significant hurdles in implementation and enforcement. The complexities of insurance plans, the diverse nature of mental healthcare, and the challenges in monitoring provider practices all contribute to the difficulty of ensuring compliance.The sheer volume of insurance plans and the intricacies of their benefit designs present a major obstacle.
Each plan needs to be meticulously reviewed to ensure that its provisions for mental healthcare meet the requirements of the MHPAEA. This requires significant resources and expertise, and inconsistencies in interpretation and application of the rule across different plans are inevitable. Furthermore, the rule’s requirements extend beyond simple financial equivalence; it also addresses issues like access to care, network adequacy, and treatment limitations.
Ensuring compliance across these multiple dimensions presents a formidable challenge.
President Biden’s mental health parity rule aims to ensure equal coverage, but access remains a challenge. Improving documentation efficiency is key, and that’s where advancements like those detailed in this article, nuance integrates generative ai scribe epic ehrs , become incredibly relevant. Faster, more accurate record-keeping could free up clinicians’ time, ultimately leading to better patient care and potentially boosting compliance with the parity rule itself.
Methods for Effective Enforcement and Monitoring
Effective enforcement requires a multi-pronged approach combining robust oversight by government agencies, proactive monitoring by insurers, and a system for addressing complaints from individuals experiencing disparities in coverage. The Department of Labor, the Department of Health and Human Services, and the Department of the Treasury share responsibility for enforcing the MHPAEA, utilizing a combination of audits, investigations, and enforcement actions against non-compliant entities.
They can impose significant financial penalties for violations. However, the limited resources available to these agencies often restrict the scale of their oversight efforts. Proactive monitoring by insurers themselves, involving regular internal reviews of their plans’ compliance with the parity rule, is crucial. This self-monitoring, however, needs to be accompanied by external audits and oversight to ensure its effectiveness and prevent manipulation.
Finally, a clear and accessible process for individuals to file complaints about potential violations is vital to hold insurers accountable.
Government Agency Roles in Oversight and Addressing Violations
Government agencies play a critical role in overseeing compliance and addressing violations of the mental health parity rule. The Department of Labor (DOL), the Department of Health and Human Services (HHS), and the Department of the Treasury (Treasury) each have responsibilities in enforcing the MHPAEA. The DOL focuses on employer-sponsored plans, HHS oversees plans offered through the Health Insurance Marketplaces, and Treasury addresses self-funded plans.
These agencies conduct audits, investigate complaints, and take enforcement actions against plans found to be non-compliant. This can include issuing warning letters, imposing fines, and even pursuing legal action. However, the resources available to these agencies are often limited, resulting in challenges in effectively monitoring the vast number of plans subject to the rule. Effective collaboration between these agencies is essential to ensure a consistent and effective enforcement approach.
Furthermore, public education campaigns are needed to raise awareness among both consumers and providers about their rights and responsibilities under the MHPAEA.
Complaint Filing Process Flowchart
The process of filing a complaint regarding non-compliance with the mental health parity rule can be visualized in a flowchart. The flowchart would begin with the individual identifying a potential violation, such as denial of coverage for mental health treatment that is covered for medical treatment. Next, the individual would gather relevant documentation, including insurance policy details, treatment records, and denial of coverage letters.
The complaint would then be filed with the appropriate agency, depending on the type of insurance plan involved (e.g., DOL, HHS, or Treasury). The agency would review the complaint and conduct an investigation. The investigation could involve contacting the insurer, reviewing plan documents, and potentially interviewing the individual and other involved parties. The agency would then issue a determination, which could include a finding of non-compliance, resulting in enforcement action against the insurer, or a finding of compliance.
The individual would be notified of the agency’s decision and their right to appeal. This process can be complex and time-consuming, highlighting the need for streamlined and accessible complaint mechanisms.
Patient Experiences and Outcomes: Biden Mental Health Parity Health Insurance Rule
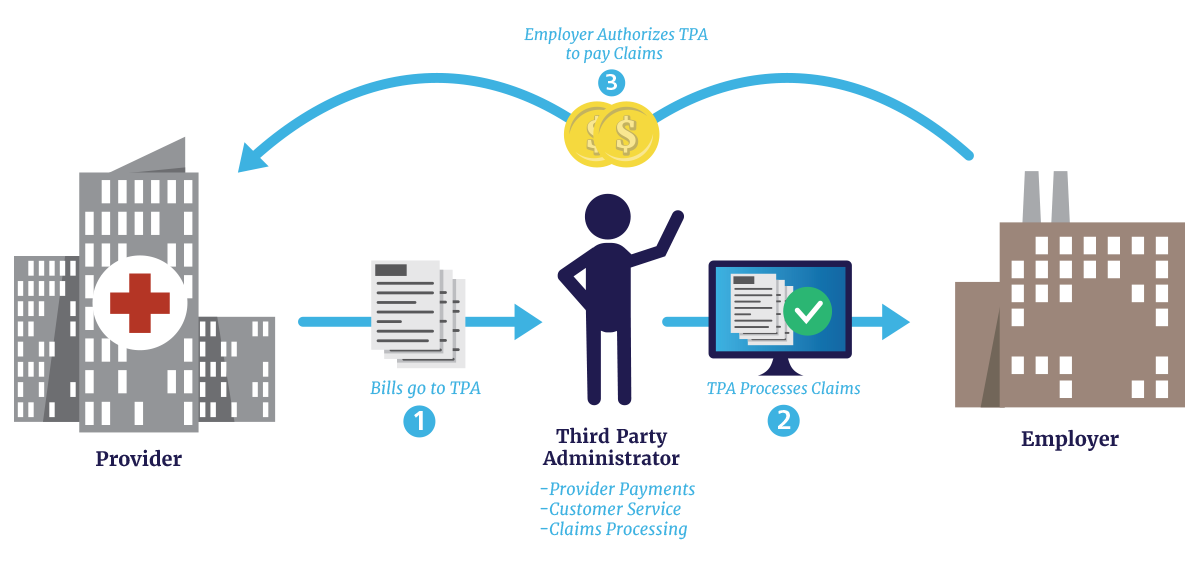
Source: varipro.com
The Biden Administration’s Mental Health Parity and Addiction Equity Act (MHPAEA) aims to ensure that mental healthcare is treated equally to physical healthcare under insurance plans. While the full impact is still unfolding, early anecdotal evidence and emerging data suggest significant improvements in access and, potentially, patient outcomes for some, while others continue to face significant hurdles. The rule’s success hinges on effective implementation and enforcement, as well as widespread awareness among both patients and providers.The improved access to mental healthcare brought about by the MHPAEA has led to observable positive changes in the lives of many individuals.
For instance, increased coverage for therapy sessions has allowed individuals struggling with anxiety and depression to receive consistent treatment, leading to improved symptom management and a greater sense of well-being. Similarly, the expanded coverage of medication management has enabled individuals with severe mental illnesses to maintain stability and avoid hospitalizations. The effects are not always immediate or uniform, varying greatly based on individual circumstances, the type of insurance coverage, and the availability of mental health professionals in a given area.
Improved Access to Care and Treatment
Increased parity has made mental health services more accessible to many individuals previously unable to afford treatment. One example is Sarah, a single mother of two who was previously denied coverage for her depression treatment because her insurance plan deemed it “not medically necessary.” After the MHPAEA was implemented, her insurance company was forced to reconsider her case and approve her treatment plan, which included therapy and medication.
Sarah reported a significant improvement in her mental health and her ability to care for her children. Another case study involves a young adult diagnosed with schizophrenia who, due to the improved access to medication management and therapy, has been able to maintain stable employment and live independently.
Potential Effects on Patient Outcomes
While definitive long-term data on the MHPAEA’s impact on patient outcomes is still being collected and analyzed, preliminary findings suggest a positive trend. Studies are showing a potential decrease in hospital readmissions for mental health crises, which indicates better management of symptoms and preventative care. Further, there’s evidence suggesting an increase in the number of individuals seeking treatment and improved adherence to treatment plans due to reduced financial barriers.
However, the magnitude of these improvements varies considerably across different demographics and geographic locations. It is crucial to continue monitoring and evaluating the long-term effects of the MHPAEA to fully understand its impact on various patient populations.
Resources for Patients Experiencing Difficulties Accessing Mental Healthcare
The following resources can assist patients facing challenges in accessing mental healthcare due to insurance coverage issues:
It is vital to remember that navigating insurance complexities can be challenging. These resources offer support and guidance to ensure individuals receive the mental healthcare they need.
President Biden’s mental health parity rule aims to ensure equal coverage for mental and physical healthcare, a crucial step forward. However, the ongoing legal battle highlighted in this aha hospital groups court brief urging a stay to restore the Affordable Care Act’s preventive services could indirectly impact access to these services. Ultimately, strengthening the ACA is vital to upholding the spirit and effectiveness of Biden’s mental health parity initiative.
- Your insurance company’s member services department: Contact them to clarify your coverage, understand your benefits, and address any denials of care.
- The Substance Abuse and Mental Health Services Administration (SAMHSA): SAMHSA’s National Helpline (1-800-662-HELP (4357)) provides confidential treatment referral and information services.
- The Centers for Medicare & Medicaid Services (CMS): CMS oversees Medicare and Medicaid programs and provides information on mental health coverage under these programs.
- Your state’s insurance commissioner’s office: These offices can help resolve disputes with insurance companies regarding mental healthcare coverage.
- Mental health advocacy organizations: Numerous organizations advocate for improved mental healthcare access and can provide assistance with insurance-related issues.
Future Directions and Potential Improvements
Source: ytimg.com
The Biden Administration’s Mental Health Parity and Addiction Equity Act (MHPAEA) represents a significant step forward, but its full potential remains unrealized. Further strengthening and refinement are crucial to ensure equitable access to mental healthcare and achieve meaningful improvements in patient outcomes. This requires a multifaceted approach encompassing improved enforcement, expanded coverage, and adaptation to evolving healthcare landscapes.
Several areas within the MHPAEA warrant attention for potential improvement. While the law aims for parity, significant disparities persist in access and reimbursement between mental healthcare and physical healthcare. This necessitates a more robust and proactive approach to enforcement, coupled with increased transparency in insurance practices to ensure compliance. Furthermore, the rule’s applicability to emerging modalities of care, particularly telehealth, requires careful consideration and adaptation.
Strengthening Enforcement and Monitoring, Biden mental health parity health insurance rule
Effective enforcement is paramount to the MHPAEA’s success. Current mechanisms for identifying and addressing non-compliance need strengthening. This includes increasing the resources dedicated to investigations and penalties for violations, empowering patients with clearer avenues for redress, and establishing more transparent reporting mechanisms to track compliance rates across insurance providers. A robust, data-driven approach, leveraging technology to monitor claims and identify potential disparities, is essential.
Expanding Coverage and Addressing Gaps in Access
The MHPAEA should be expanded to address specific gaps in coverage. This includes explicitly covering a wider range of mental health services, such as intensive outpatient programs, residential treatment, and peer support services. Furthermore, addressing geographic disparities in access to mental healthcare providers is critical, particularly in underserved rural and urban communities. Incentivizing providers to establish practices in these areas, and leveraging telehealth to overcome geographic barriers, are vital strategies.
Adapting to the Rise of Telehealth
The COVID-19 pandemic dramatically accelerated the adoption of telehealth services for mental healthcare. The MHPAEA needs to explicitly incorporate telehealth parity, ensuring that coverage and reimbursement for telehealth mental healthcare services are equivalent to in-person services. This includes addressing potential challenges related to licensing, reimbursement rates, and access to technology, especially for patients with limited digital literacy or access to reliable internet.
Illustrative Scenario: Sarah’s Journey to Recovery
Sarah, a 32-year-old teacher, experienced a debilitating anxiety disorder following a traumatic event. Prior to the strengthened MHPAEA, her insurance company severely limited coverage for therapy sessions, resulting in limited access to care. Under the improved MHPAEA, however, Sarah’s insurance covered 20 weekly therapy sessions with a licensed therapist, 10 sessions of Cognitive Behavioral Therapy (CBT) focusing on managing anxiety, and access to a telehealth platform for ongoing support.
She also received coverage for medication management from a psychiatrist via telehealth, significantly reducing travel time and cost. The comprehensive care allowed Sarah to manage her anxiety, return to work, and rebuild her life. This improved access to care resulted in a significant improvement in her mental well-being, showcasing the positive impact of a strengthened MHPAEA.
Concluding Remarks
The Biden administration’s Mental Health Parity rule represents a landmark step towards ensuring equitable access to mental healthcare. While challenges remain in implementation and enforcement, the potential positive impact on millions of lives is undeniable. By fostering equal coverage and promoting better access to services, this rule holds the promise of transforming the mental health landscape, leading to improved outcomes and a more inclusive healthcare system.
The journey towards true parity is ongoing, but this rule marks a significant turning point.
FAQ Section
What specific services are covered under the Biden Mental Health Parity rule?
The rule covers a wide range of services, including therapy, medication management, inpatient and outpatient treatment, and substance abuse services. The specific services covered can vary depending on the individual insurance plan, but the parity requirement ensures that the coverage is comparable to physical health benefits.
How can I file a complaint if my insurance company isn’t complying with the rule?
You should first contact your insurance company’s customer service department to address the issue. If that fails to resolve the problem, you can file a complaint with your state’s insurance department or the federal government. Specific instructions on filing a complaint will vary depending on your location and the nature of the issue.
Does this rule cover telehealth services for mental health?
Yes, the rule generally covers telehealth services for mental health, although specific details may vary by plan. The increasing use of telehealth during the pandemic has highlighted the importance of ensuring parity in this area.
How will this rule affect the cost of mental healthcare?
While the rule aims to increase access, the impact on cost is complex. Increased access could lead to higher overall spending, but improved preventative care and reduced hospitalizations could potentially offset some of these costs in the long run. The long-term cost-effectiveness will require further analysis.





