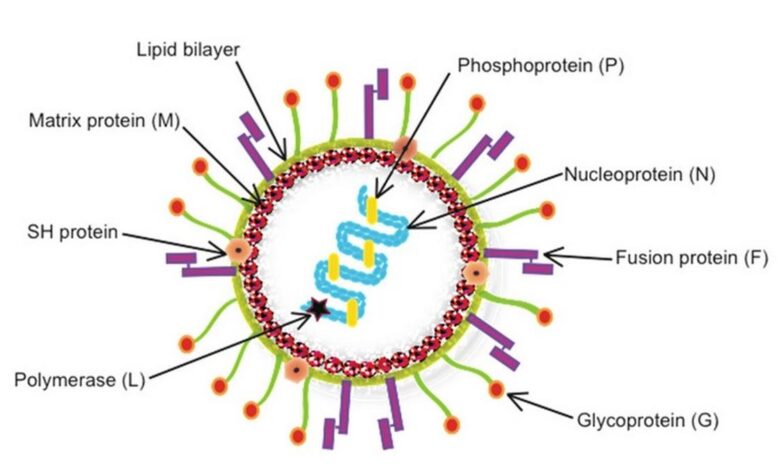
Is HMPV Fatal? Understanding HMPV Health Complications
Is hmpv fatal understanding the health complications of hmpv – Is HMPV fatal? Understanding the health complications of HMPV is crucial, especially given its global prevalence and potential for severe outcomes, particularly in vulnerable populations. This isn’t just another dry medical report; we’re diving deep into the realities of HMPV – from its sneaky transmission methods to the potentially life-threatening complications it can cause. We’ll explore the symptoms, the high-risk groups, and the treatments available, painting a clearer picture of this often-overlooked respiratory virus.
Get ready to learn something new – and maybe even save a life!
We’ll unpack everything from the basic symptoms and how HMPV spreads to the serious complications that can arise, including those that can sadly prove fatal. We’ll also look at who’s most at risk and what steps can be taken to prevent infection and manage the disease effectively. Think of this as your comprehensive, friendly guide to navigating the world of HMPV.
HMPV Infection
Human metapneumovirus (HMPV) is a common respiratory virus causing illness worldwide. Understanding its prevalence, transmission, and comparison to other respiratory viruses is crucial for effective prevention and management strategies. This post delves into the specifics of HMPV infection, focusing on its spread and impact across different age groups.
HMPV Prevalence and Age Group Distribution
HMPV infections are globally prevalent, affecting individuals of all ages, but the impact varies significantly depending on age. Young children (under 5 years old) and older adults (over 65 years old) experience the most severe symptoms and are at higher risk of complications. While precise global prevalence figures are difficult to obtain due to variations in testing and reporting, studies consistently show HMPV as a significant cause of respiratory illness in these vulnerable populations.
In younger children, HMPV can contribute to bronchiolitis and pneumonia, requiring hospitalization in some cases. In older adults, HMPV exacerbates existing respiratory conditions and can lead to increased morbidity and mortality. Adults in the intermediate age range typically experience milder symptoms, often resembling a common cold.
HMPV Transmission Modes
HMPV primarily spreads through respiratory droplets produced during coughing, sneezing, or talking. These droplets can be inhaled directly by others in close proximity, representing the most effective transmission route. Indirect transmission can also occur via contact with contaminated surfaces, such as doorknobs or toys, followed by touching the nose or mouth. The effectiveness of indirect transmission is generally considered lower than direct contact with respiratory droplets.
The virus’s ability to survive on surfaces varies depending on environmental factors, but generally, the risk of indirect transmission diminishes significantly within hours.
Comparison of HMPV Transmission with Other Respiratory Viruses
HMPV transmission shares similarities with other respiratory viruses like influenza and RSV (respiratory syncytial virus). All three spread primarily via respiratory droplets and, to a lesser extent, through contact with contaminated surfaces. However, the precise mechanisms of transmission and the relative effectiveness of each route can vary slightly between these viruses. Influenza, for example, is known for its rapid spread through airborne droplets, while RSV transmission often involves close contact with infected individuals.
HMPV transmission falls somewhere in between, with direct contact through respiratory droplets being the dominant mode of spread. The overall transmissibility of these viruses also varies depending on factors such as viral strain, environmental conditions, and the immune status of the population.
HMPV Infection: Age, Rate, Severity, and Mortality
The following table summarizes the general trends of HMPV infection across different age groups. Note that these are broad generalizations, and actual infection rates and severity can vary significantly based on various factors. Precise mortality rates are difficult to determine definitively due to complexities in attributing deaths solely to HMPV infection.
| Age Group | Infection Rate | Severity of Symptoms | Mortality Rate |
|---|---|---|---|
| 0-5 years | High | Can range from mild to severe; often leads to bronchiolitis and pneumonia | Low, but higher risk of hospitalization |
| 5-65 years | Moderate | Generally mild, resembling a common cold | Very low |
| >65 years | High | Can be severe, particularly in those with underlying respiratory conditions; increases risk of pneumonia and other complications | Higher than in younger adults |
HMPV Symptoms and Disease Progression
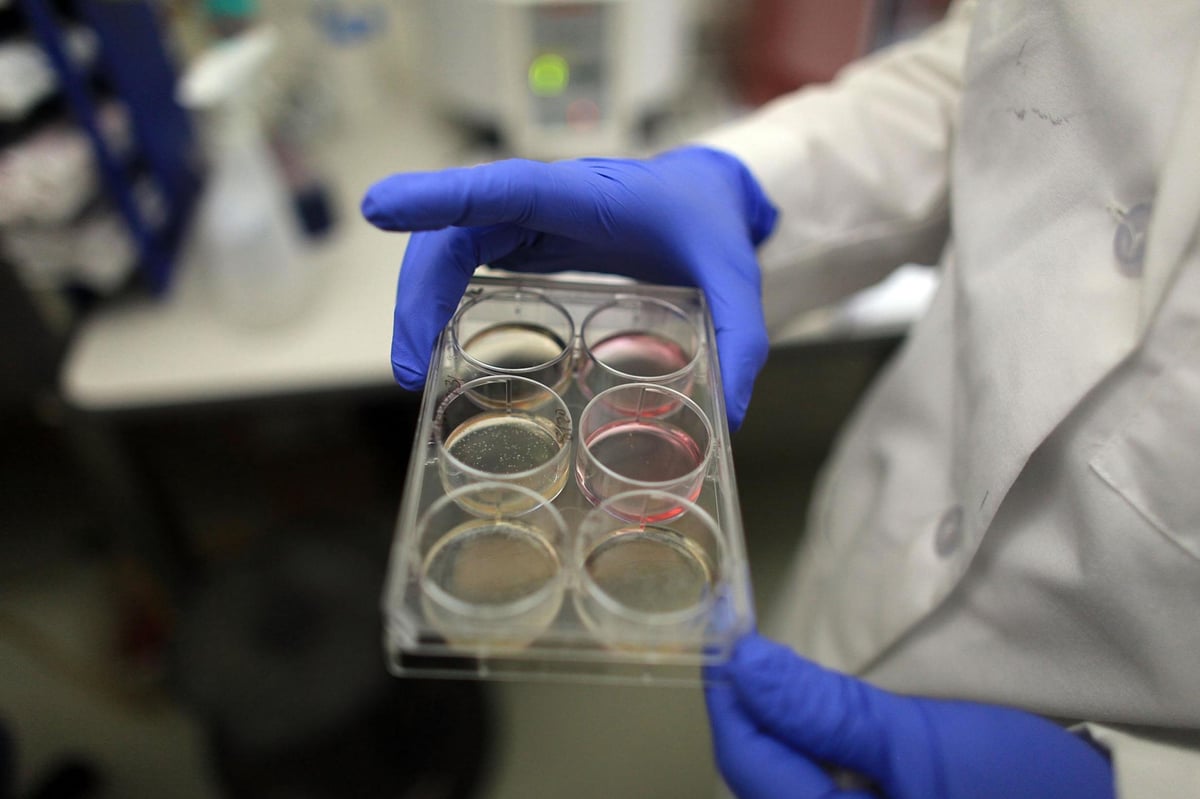
Source: zenfs.com
Human metapneumovirus (HMPV) infection presents differently depending on the age and overall health of the individual. Understanding the typical symptoms and the progression of the illness is crucial for early diagnosis and appropriate management. While most infections are mild, particularly in older children and adults, severe complications can arise, especially in infants and young children, and those with underlying health conditions.HMPV symptoms often mimic those of other respiratory viruses, making accurate diagnosis challenging without laboratory testing.
The incubation period, the time between infection and symptom onset, is typically 3-6 days.
So, is HMPV fatal? Understanding the health complications of HMPV is crucial, as severe cases can lead to pneumonia and respiratory failure. These complications, like those increasing stroke risk, can be devastating. Learning about the risk factors that make stroke more dangerous highlights how pre-existing conditions can worsen outcomes; similarly, underlying health issues can significantly impact the severity of HMPV.
Therefore, early detection and appropriate treatment are key to managing this virus.
Symptoms in Different Age Groups
The symptoms of HMPV infection vary depending on the age group. Infants and young children often experience more severe symptoms than older children and adults. Infants may present with fever, cough, difficulty breathing (wheezing or rapid breathing), and poor feeding. Older children and adults typically experience milder symptoms, such as a runny nose, cough, sore throat, headache, and muscle aches.
So, is HMPV fatal? While usually not life-threatening for healthy adults, understanding the health complications of HMPV is crucial, especially for vulnerable populations. It’s amazing to see advancements in other areas of medicine though, like the incredible news that the FDA has approved clinical trials for pig kidney transplants in humans – check out this article for more info: fda approves clinical trials for pig kidney transplants in humans.
This highlights how medical breakthroughs are happening across various fields, reminding us of the ongoing fight against disease, including better understanding and managing the effects of HMPV.
However, even in older individuals, HMPV can lead to pneumonia or bronchitis in vulnerable populations. In elderly individuals, symptoms may be more subtle, potentially presenting as a worsening of existing chronic respiratory conditions.
Progression of HMPV Infection
The typical progression of HMPV infection begins with mild upper respiratory symptoms, such as a runny nose and cough. These initial symptoms can last for several days before progressing to lower respiratory tract involvement in some cases. This may manifest as bronchitis (inflammation of the bronchi) or pneumonia (infection of the lungs). In severe cases, particularly in young infants, the infection can lead to respiratory distress, requiring hospitalization and supportive care.
The severity of the illness depends on several factors, including the age and immune status of the individual, the viral load, and the presence of underlying medical conditions.
Atypical HMPV Presentations
While the typical presentation involves respiratory symptoms, atypical presentations can occur. For example, some individuals may experience gastrointestinal symptoms such as vomiting and diarrhea alongside the respiratory symptoms. In other cases, the infection might present primarily as bronchiolitis, characterized by inflammation of the small airways in the lungs, leading to significant breathing difficulties. These atypical presentations highlight the importance of considering HMPV in the differential diagnosis of various respiratory and gastrointestinal illnesses, especially in young children.
Timeline of Symptom Development in a Typical HMPV Infection
The following timeline represents a typical progression, but individual experiences may vary:
- Days 1-3: Onset of mild upper respiratory symptoms, such as runny nose, mild cough, and possibly low-grade fever.
- Days 4-7: Symptoms may worsen, with increased cough, potentially developing into a more significant cough with wheezing or difficulty breathing. Fever may become more pronounced.
- Days 7-14: If the infection progresses to lower respiratory tract involvement, symptoms such as shortness of breath, chest pain, and increased respiratory rate may develop. In severe cases, hospitalization may be necessary.
- Days 14 onwards: Gradual resolution of symptoms, although a lingering cough may persist for several weeks.
High-Risk Groups and Severity of Illness
Human metapneumovirus (HMPV) infection can range from mild, cold-like symptoms to severe respiratory illness, particularly in vulnerable populations. Understanding which groups are at higher risk and the factors influencing disease severity is crucial for effective prevention and management strategies. This section will explore these high-risk groups, the contributing factors to severe illness, and the varying clinical outcomes observed.
Several factors increase the risk of severe HMPV complications. These factors often interact, creating a complex picture of risk. Age, underlying health conditions, and immune status play significant roles in determining the severity of the infection.
High-Risk Populations for Severe HMPV
Certain populations are disproportionately affected by severe HMPV. These include infants, young children, the elderly, and individuals with pre-existing respiratory or immune conditions. The severity of illness varies significantly across these groups.
- Infants (under 6 months): Infants are particularly vulnerable due to their immature immune systems and underdeveloped respiratory tracts. They are at increased risk of bronchiolitis, pneumonia, and respiratory failure.
- Young Children (under 5 years): While risk decreases with age, young children still face a higher likelihood of severe HMPV compared to older children and adults. This is partially due to the ongoing development of their immune response to respiratory viruses.
- Older Adults (over 65 years): Older adults have weakened immune systems, making them more susceptible to severe HMPV. Pre-existing conditions like heart disease or chronic lung disease further increase their risk.
- Individuals with Pre-existing Conditions: Those with chronic respiratory diseases (asthma, cystic fibrosis, COPD), weakened immune systems (due to HIV/AIDS, chemotherapy, or organ transplantation), and cardiovascular diseases are at significantly higher risk of severe HMPV complications.
Factors Contributing to Severity of HMPV in High-Risk Individuals
The severity of HMPV infection in high-risk individuals is influenced by several interacting factors. These factors can exacerbate the effects of the virus, leading to more severe clinical outcomes.
- Immune Status: A compromised immune system, whether due to age, underlying disease, or immunosuppressive medications, significantly increases the risk of severe HMPV.
- Pre-existing Respiratory Conditions: Individuals with asthma or other chronic lung diseases are at greater risk of severe lower respiratory tract infections, including HMPV-related pneumonia and bronchiolitis. The underlying inflammation in their airways can be worsened by HMPV infection.
- Underlying Cardiovascular Disease: Severe HMPV can strain the cardiovascular system, leading to complications in individuals with pre-existing heart conditions. The body’s response to infection can place additional stress on the heart.
- Viral Load and Strain: The amount of virus encountered and the specific viral strain can influence disease severity. Some strains may be more virulent than others.
Clinical Outcomes in Different High-Risk Groups
The clinical outcomes of HMPV infection vary depending on the individual’s risk factors. While some may experience only mild symptoms, others may develop life-threatening complications.
For example, infants may present with bronchiolitis requiring hospitalization and respiratory support, while older adults might experience pneumonia necessitating intensive care. Individuals with compromised immune systems may experience prolonged illness and increased susceptibility to secondary bacterial infections. Specific outcomes are influenced by the interplay of factors mentioned previously.
Management of Severe HMPV Cases: A Decision-Making Flowchart
Managing severe HMPV cases requires a systematic approach. The following flowchart illustrates a simplified decision-making process for healthcare professionals.
Imagine a flowchart. It would start with “HMPV suspected/confirmed”. Branches would lead to “Severe Illness (e.g., respiratory distress, hypoxia)” and “Mild Illness”. The “Severe Illness” branch would further branch into “Hospitalization required” and “Outpatient management”. “Hospitalization required” would then branch into “Supportive care (oxygen, fluids)” and “Intensive care (mechanical ventilation)”.
The “Outpatient management” branch would lead to “Close monitoring and supportive care”. The “Mild Illness” branch would simply lead to “Symptomatic treatment and monitoring”.
So, is HMPV fatal? Understanding the health complications of HMPV is crucial, as it can lead to severe respiratory issues, especially in vulnerable populations. The recent news about actress Monali Thakur being hospitalized after struggling to breathe, as reported in this article monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases , highlights the importance of preventative measures.
While not always fatal, HMPV can be incredibly dangerous, emphasizing the need for awareness and proactive health strategies.
HMPV-Related Complications and Fatality
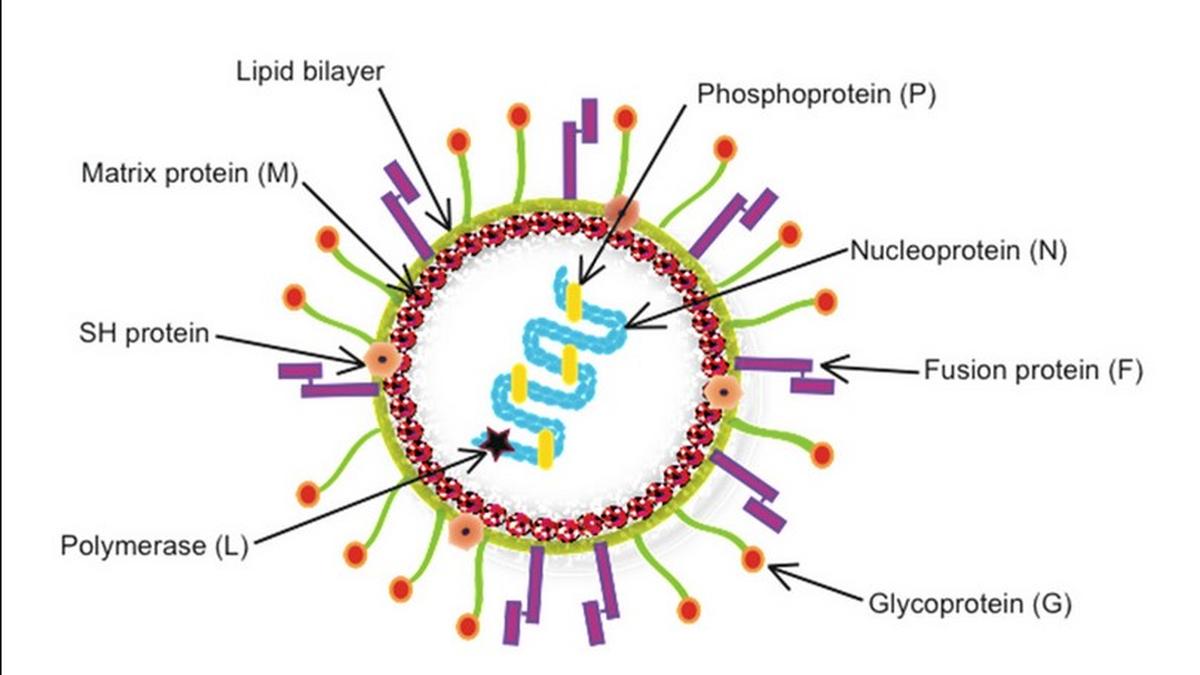
Source: thgim.com
Human metapneumovirus (HMPV) infection, while often mild, can lead to severe respiratory complications, particularly in vulnerable populations. Understanding these potential life-threatening outcomes is crucial for effective prevention and management. This section will explore the serious complications associated with HMPV, the mechanisms behind their development, and examples illustrating the severity of the virus.
HMPV’s ability to cause severe illness stems from its impact on the lower respiratory tract. The virus replicates in the cells lining the airways, triggering inflammation and potentially leading to bronchiolitis (inflammation of the small airways) and pneumonia (infection of the lungs). This inflammation can obstruct airflow, making breathing difficult, especially for infants, young children, and the elderly. The body’s immune response, while crucial for fighting the infection, can also contribute to the severity of the illness through excessive inflammation and tissue damage.
Bronchiolitis and Pneumonia
Bronchiolitis and pneumonia are the most common and potentially life-threatening complications of HMPV infection. Bronchiolitis, characterized by inflammation and swelling of the small airways in the lungs, leads to wheezing, coughing, and difficulty breathing. Pneumonia, an infection of the lung tissue, can cause severe respiratory distress, fever, and potentially respiratory failure. The severity of these conditions varies depending on factors such as the patient’s age, underlying health conditions, and the extent of viral replication.
Respiratory Failure
In severe cases, HMPV infection can lead to respiratory failure, a condition where the lungs are unable to adequately exchange oxygen and carbon dioxide. This can necessitate mechanical ventilation, a life-saving intervention that involves using a machine to assist breathing. Respiratory failure often occurs when the inflammation and swelling in the airways are so severe that they obstruct airflow to a critical degree, leading to dangerously low oxygen levels in the blood.
Other Complications
While less common, HMPV can also contribute to other serious complications, including dehydration, ear infections (otitis media), and in rare instances, encephalitis (brain inflammation). Dehydration can occur due to the difficulty breathing and loss of fluids from fever and increased respiratory rate. Ear infections are common in children and can lead to hearing problems if left untreated. Encephalitis, a rare but serious complication, is usually associated with severe systemic infection and requires prompt medical attention.
Examples of Severe HMPV Outcomes
Numerous studies have documented cases of severe HMPV infections resulting in hospitalization and even death, particularly in high-risk populations. For example, a study published in the journal Pediatrics highlighted a significant number of hospitalizations among infants with HMPV bronchiolitis. Another study in the Journal of Infectious Diseases detailed cases of severe pneumonia in immunocompromised adults, emphasizing the increased risk of severe illness in this population.
These studies underscore the potential for HMPV to cause severe and life-threatening complications.
HMPV Complications: A Summary Table
| Complication | Description | Risk Factors | Treatment Strategies |
|---|---|---|---|
| Bronchiolitis | Inflammation of the small airways, causing wheezing, coughing, and difficulty breathing. | Infancy, prematurity, chronic lung disease, weakened immune system | Supportive care (oxygen therapy, fluids), bronchodilators in some cases. |
| Pneumonia | Infection of the lung tissue, causing severe respiratory distress, fever, and potentially respiratory failure. | Infancy, older age, chronic lung disease, weakened immune system | Antiviral medications (in some cases), oxygen therapy, antibiotics if bacterial co-infection is present. |
| Respiratory Failure | Inability of the lungs to adequately exchange oxygen and carbon dioxide. | Severe bronchiolitis, pneumonia, weakened immune system | Mechanical ventilation, supportive care. |
| Dehydration | Fluid loss due to fever, increased respiratory rate, and difficulty breathing. | Infants, young children, individuals with severe respiratory illness | Intravenous fluids, oral rehydration solutions. |
Diagnosis and Treatment of HMPV Infection
Diagnosing and treating human metapneumovirus (HMPV) infection involves a combination of laboratory tests and supportive care, with antiviral treatments playing a limited role. Early and accurate diagnosis is crucial, especially in high-risk individuals, to initiate appropriate management and reduce the severity of illness. The treatment approach focuses primarily on alleviating symptoms and preventing complications.
Diagnostic Methods for HMPV
Identifying HMPV infection relies primarily on laboratory testing. Several methods are employed, each with its own advantages and limitations. Rapid diagnostic tests offer quick results but may have lower sensitivity compared to more sensitive molecular tests. Accurate diagnosis is critical for guiding treatment decisions and informing public health surveillance efforts.
- Rapid Antigen Detection Tests: These tests use nasal or throat swabs to detect HMPV antigens. Results are typically available within minutes, making them useful for rapid triage in clinical settings. However, they might miss some infections due to lower sensitivity compared to molecular tests.
- Molecular Tests (RT-PCR): Reverse transcription-polymerase chain reaction (RT-PCR) is the gold standard for HMPV detection. This highly sensitive test amplifies HMPV genetic material from respiratory specimens, providing accurate and reliable results. RT-PCR is particularly useful for confirming HMPV infection and differentiating it from other respiratory viruses.
- Viral Culture: While less commonly used due to the time required for results (several days), viral culture can isolate and identify HMPV. This method allows for further characterization of the virus but is less practical for routine diagnosis.
Treatment Options for HMPV Infection
Currently, there’s no specific antiviral therapy specifically approved for HMPV. Treatment focuses primarily on supportive care to manage symptoms and prevent complications. The goal is to alleviate symptoms and support the body’s natural immune response to clear the infection.
- Supportive Care: This forms the cornerstone of HMPV treatment. It includes adequate hydration, rest, and symptomatic relief. Over-the-counter medications such as acetaminophen or ibuprofen can help manage fever and pain. In severe cases, hospitalization may be necessary for oxygen therapy, respiratory support, or intravenous fluids.
- Antiviral Therapies: While no specific antiviral drug targets HMPV, some studies have explored the potential use of ribavirin, an antiviral with broad activity against several respiratory viruses. However, its effectiveness against HMPV remains controversial and it’s generally not recommended unless there are severe complications or in immunocompromised patients. The efficacy and cost-benefit ratio often outweigh the potential benefits in most cases.
Comparison of Antiviral Therapies for HMPV
The limited availability of targeted antiviral treatments makes a direct comparison difficult. While ribavirin has shown some activityin vitro* and in limited clinical studies, its efficacy against HMPV is not consistently demonstrated and it carries potential side effects. Therefore, supportive care remains the primary treatment strategy. Further research is needed to develop effective antiviral therapies specifically targeting HMPV.
Diagnosis and Treatment Process Flowchart
The following illustrates a simplified flowchart for diagnosing and managing HMPV infection:
- Symptoms Appear: Respiratory symptoms such as cough, fever, and shortness of breath develop.
- Clinical Evaluation: A healthcare professional assesses symptoms and medical history.
- Diagnostic Testing: Rapid antigen test or RT-PCR is performed on a respiratory specimen (nasal or throat swab).
- Positive HMPV Result: Confirms HMPV infection.
- Negative HMPV Result: May indicate another respiratory infection, requiring further investigation.
- Treatment Initiation: Supportive care is implemented (rest, hydration, symptomatic relief). In severe cases, hospitalization and oxygen therapy may be required.
- Monitoring: Close monitoring of the patient’s condition for any complications.
Prevention and Public Health Measures: Is Hmpv Fatal Understanding The Health Complications Of Hmpv
Preventing the spread of human metapneumovirus (HMPV) relies on a multi-pronged approach encompassing individual hygiene practices, community-level interventions, and the development of effective vaccines. Understanding these strategies is crucial for minimizing the impact of HMPV infections, particularly among vulnerable populations.Effective prevention strategies center around limiting the transmission of the virus, which primarily occurs through respiratory droplets produced during coughing or sneezing.
These droplets can land on surfaces or be inhaled by others in close proximity. Therefore, measures that reduce contact with these droplets are paramount. Furthermore, good hygiene practices significantly reduce the risk of infection.
Vaccination Strategies for HMPV
While a widely available and universally effective HMPV vaccine is not yet a reality, research is ongoing to develop such a vaccine. The development of an effective HMPV vaccine would represent a significant advancement in public health, potentially leading to a substantial reduction in HMPV-related hospitalizations and deaths, particularly amongst high-risk individuals like infants, young children, and the elderly.
Current research focuses on various vaccine platforms, including live-attenuated and subunit vaccines, aiming to elicit a robust and long-lasting immune response. Clinical trials are evaluating the safety and efficacy of these candidate vaccines. The success of these trials would pave the way for widespread vaccination programs, significantly altering the landscape of HMPV prevention.
Public Health Interventions to Reduce HMPV Burden
Public health initiatives play a critical role in mitigating the burden of HMPV. These interventions often focus on educating the public about effective prevention strategies, improving hygiene practices in communal settings, and implementing surveillance systems to monitor HMPV activity. For instance, public health campaigns emphasizing frequent handwashing, respiratory etiquette (covering coughs and sneezes), and staying home when sick are crucial.
Furthermore, improving ventilation in public spaces and implementing effective cleaning protocols in healthcare facilities and schools can help reduce the spread of the virus. Robust surveillance systems allow public health officials to track HMPV outbreaks, enabling timely implementation of targeted interventions. This proactive approach is vital for managing the impact of HMPV, especially during peak seasons.
Recommendations for Preventing HMPV Spread
Effective prevention requires a layered approach implemented consistently across various settings. The following recommendations are crucial for mitigating HMPV transmission:
- Schools: Regular handwashing, respiratory etiquette education, improved ventilation, and prompt exclusion of sick children from school are vital. Thorough cleaning and disinfection of frequently touched surfaces are also essential.
- Hospitals: Strict adherence to infection control protocols, including hand hygiene, use of personal protective equipment (PPE), and isolation of infected patients, is paramount. Regular environmental cleaning and disinfection are critical to preventing nosocomial transmission.
- Healthcare Settings (beyond hospitals): Similar to hospitals, strict adherence to infection control protocols and hygiene practices are essential in all healthcare settings, including clinics and nursing homes.
- Homes and Community Settings: Frequent handwashing, covering coughs and sneezes, and staying home when sick are crucial. Regular cleaning and disinfection of frequently touched surfaces help reduce the virus’s spread.
Illustrative Case Studies
Understanding the wide spectrum of HMPV infection severity requires examining real-world cases. The following examples illustrate the contrasting experiences of patients with mild and severe HMPV infections, highlighting the importance of early diagnosis and appropriate management.
Mild HMPV Infection in a Young Child, Is hmpv fatal understanding the health complications of hmpv
This case involves a 2-year-old previously healthy child who presented with a mild upper respiratory infection. Symptoms included a runny nose, mild cough, and low-grade fever (37.8°C) for three days. The child remained playful and had a good appetite. A rapid antigen test at a local clinic confirmed HMPV infection. Treatment consisted of supportive care, including increased fluid intake and acetaminophen for fever as needed.
The child’s symptoms resolved completely within a week without complications. This case demonstrates that HMPV infection can present mildly, particularly in young children with no underlying health conditions. The rapid antigen test allowed for early diagnosis and reassurance, enabling parents to provide appropriate supportive care at home.
Severe HMPV Infection in an Elderly Patient with Underlying Conditions
This case details an 80-year-old woman with a history of chronic obstructive pulmonary disease (COPD) and congestive heart failure who developed severe HMPV pneumonia. Initial symptoms included a worsening cough, shortness of breath, and high fever (39.5°C). She rapidly deteriorated, experiencing increased respiratory distress, requiring supplemental oxygen. Chest X-ray revealed extensive bilateral pneumonia. Laboratory tests confirmed HMPV infection.
She was hospitalized and received intravenous antiviral medication (though the efficacy of antivirals in HMPV is still under investigation), supplemental oxygen, and bronchodilators to manage her respiratory symptoms. Despite aggressive treatment, her condition worsened, leading to respiratory failure and the need for mechanical ventilation. She experienced multiple complications including bacterial superinfection, requiring broad-spectrum antibiotics. While she eventually recovered after a prolonged hospital stay, her experience highlights the potential for severe, life-threatening outcomes in elderly patients with pre-existing respiratory or cardiovascular conditions.
This case emphasizes the importance of prompt medical attention and aggressive management in high-risk individuals.
Ending Remarks
So, is HMPV fatal? While thankfully not always, it’s clear that HMPV is a serious respiratory virus that demands our attention. Understanding its transmission, symptoms, and potential complications is key to effective prevention and treatment. By recognizing high-risk groups and implementing preventative measures, we can significantly reduce the burden of HMPV and improve outcomes for those affected. Remember, knowledge is power – and in the case of HMPV, that power can mean the difference between a mild illness and a serious health crisis.
Let’s stay informed and proactive in protecting ourselves and our communities.
Clarifying Questions
What is the best way to protect myself from HMPV?
Practicing good hygiene (frequent handwashing, covering coughs and sneezes), avoiding close contact with sick individuals, and staying up-to-date on vaccinations (if available) are excellent preventative measures.
How long does a typical HMPV infection last?
The duration varies, but most people recover within a week or two. However, severe cases can last much longer.
Is there a specific HMPV vaccine?
Currently, there isn’t a widely available vaccine for HMPV, but research is ongoing.
Can HMPV be treated with antibiotics?
No, antibiotics are ineffective against viruses like HMPV. Treatment focuses on supportive care to manage symptoms.