
The Link Between Periodic Fasting and Longevity
The link between periodic fasting and longevity is a fascinating area of research, sparking intense debate and curiosity. Does skipping meals really add years to our lives? The answer, as with most things related to health, isn’t a simple yes or no. This exploration delves into the science behind periodic fasting, examining its impact on cellular processes, metabolic function, and the evidence from both animal and human studies.
We’ll uncover the mechanisms by which fasting might extend lifespan, weigh the potential benefits against the risks, and ultimately consider whether this dietary practice is right for you.
We’ll journey through the complex world of autophagy, cellular repair, and metabolic shifts, exploring how periodic fasting influences these processes. We’ll also examine various fasting methods – intermittent fasting, time-restricted feeding, and more – and discuss their unique effects on the body. Get ready to dive deep into the science and discover how manipulating our eating patterns might just hold the key to a longer, healthier life.
Mechanisms of Action
Periodic fasting, encompassing various regimens like intermittent fasting and time-restricted feeding, exerts its influence on longevity through a complex interplay of cellular and molecular mechanisms. These mechanisms aren’t fully understood, but research points to several key pathways contributing to the observed lifespan extension in animal models and potential benefits in humans.
Autophagy, Apoptosis, and Sirtuin Activation, The link between periodic fasting and longevity
Periodic fasting triggers cellular processes that promote cellular health and repair. Autophagy, a process of cellular self-digestion, is significantly upregulated during fasting. This “self-cleaning” mechanism removes damaged organelles and misfolded proteins, preventing cellular dysfunction and age-related decline. Conversely, apoptosis, or programmed cell death, eliminates damaged or dysfunctional cells, preventing the accumulation of cells that could contribute to disease.
These processes are tightly regulated and crucial for maintaining cellular homeostasis. Furthermore, fasting activates sirtuins, a family of proteins that regulate metabolism, stress resistance, and DNA repair, all contributing to extended lifespan. Studies have shown that sirtuin activation is a key mediator of the longevity benefits associated with caloric restriction and periodic fasting.
Oxidative Stress Reduction
Oxidative stress, caused by an imbalance between the production of reactive oxygen species (ROS) and the body’s antioxidant defenses, is a major contributor to aging and age-related diseases. Periodic fasting has been shown to reduce oxidative stress by modulating the production of ROS and enhancing antioxidant defenses. This reduction in oxidative stress protects cells from damage, contributing to improved cellular function and overall healthspan, which is closely linked to lifespan.
For instance, studies on rodents have shown improved mitochondrial function and reduced levels of oxidative markers following periods of fasting.
Inflammation and Lifespan
Chronic low-grade inflammation is implicated in many age-related diseases. Periodic fasting has demonstrated anti-inflammatory effects, reducing the production of pro-inflammatory cytokines. This reduction in inflammation can contribute to a decreased risk of chronic diseases, ultimately extending lifespan. The mechanisms behind this anti-inflammatory effect are multifaceted and involve modulation of immune cell activity and signaling pathways. For example, research suggests that fasting can alter the gut microbiome, leading to a reduction in systemic inflammation.
Comparison of Fasting Regimens
Different periodic fasting regimens, such as intermittent fasting (e.g., 16/8 method, 5:2 diet) and time-restricted feeding (eating within a specific window each day), may differentially impact these mechanisms. While both generally promote autophagy and reduce inflammation, the specific effects can vary depending on the duration and frequency of fasting. For example, longer fasting periods may induce more pronounced autophagy, while time-restricted feeding might be more suitable for long-term adherence and may offer similar benefits with less stringent restrictions.
More research is needed to fully understand the optimal fasting regimen for maximizing longevity benefits.
Key Cellular and Molecular Pathways Influenced by Periodic Fasting
| Pathway | Mechanism | Contribution to Longevity | Example Fasting Regimen |
|---|---|---|---|
| Autophagy | Cellular self-cleaning, removal of damaged organelles and proteins | Improved cellular function, reduced cellular senescence | 16/8 intermittent fasting |
| Apoptosis | Programmed cell death, elimination of dysfunctional cells | Prevention of accumulation of damaged cells, reduced risk of cancer | 5:2 intermittent fasting |
| Sirtuin Activation | Increased activity of sirtuin proteins, regulating metabolism, stress resistance, and DNA repair | Improved metabolic health, increased stress resistance, enhanced DNA repair | Time-restricted feeding |
| Oxidative Stress Reduction | Decreased ROS production, enhanced antioxidant defenses | Protection against cellular damage, improved mitochondrial function | Alternate-day fasting |
| Inflammation Modulation | Reduced production of pro-inflammatory cytokines | Decreased risk of chronic diseases | Any periodic fasting regimen |
Metabolic Effects and Longevity

Source: says.com
Periodic fasting, encompassing various regimens like intermittent fasting or time-restricted feeding, exerts profound metabolic effects that are increasingly linked to improved healthspan and longevity. These effects aren’t simply about weight loss; they involve intricate changes in how our bodies utilize energy, regulate hormones, and manage cellular processes. Understanding these metabolic shifts is key to appreciating the potential benefits of periodic fasting.
Impact of Periodic Fasting on Insulin Sensitivity and Glucose Metabolism
Periodic fasting significantly improves insulin sensitivity. Insulin, the hormone responsible for regulating blood sugar, becomes less effective in individuals with insulin resistance, a hallmark of metabolic syndrome and type 2 diabetes. During fasting periods, the body shifts from primarily using glucose for energy to utilizing stored fat. This metabolic switch enhances insulin’s ability to transport glucose into cells, leading to improved blood sugar control.
Studies have shown that even short-term intermittent fasting can improve glucose tolerance and reduce fasting insulin levels, mitigating the risks associated with insulin resistance and type 2 diabetes, both significant contributors to reduced lifespan. The reduced reliance on glucose also promotes a healthier metabolic environment.
Relationship Between Periodic Fasting, Weight Management, and Lifespan Extension
The link between periodic fasting, weight management, and longevity is multifaceted. Weight loss, often observed with periodic fasting, contributes to improved metabolic health. However, the benefits extend beyond simple calorie restriction. The hormonal shifts induced by fasting, such as increased levels of growth hormone and adiponectin (a hormone associated with improved insulin sensitivity and fat metabolism), play a significant role in weight regulation and longevity.
Animal studies have consistently demonstrated that caloric restriction mimetics, which mimic the metabolic effects of calorie restriction without requiring severe food restriction, extend lifespan. Periodic fasting acts as a caloric restriction mimetic, triggering these beneficial metabolic adaptations.
Metabolic Changes Triggering Improved Healthspan and Longevity
Periodic fasting triggers a cascade of metabolic changes contributing to improved healthspan and longevity. These include: autophagy (a cellular self-cleaning process), reduced inflammation, improved mitochondrial function (the powerhouses of our cells), and increased production of protective antioxidants. Autophagy removes damaged cellular components, preventing the accumulation of cellular debris that contributes to aging and age-related diseases. Reduced inflammation counteracts chronic low-grade inflammation, a key driver of many age-related illnesses.
Improved mitochondrial function ensures efficient energy production, while increased antioxidant production protects cells from damage caused by oxidative stress.
Effects of Periodic Fasting on Lipid Profiles and Cardiovascular Health
Studies have demonstrated that periodic fasting can favorably alter lipid profiles, reducing levels of triglycerides and LDL cholesterol (“bad” cholesterol) while potentially increasing HDL cholesterol (“good” cholesterol). These improvements in lipid profiles contribute to reduced risk of cardiovascular disease, a major cause of mortality. The mechanisms behind these effects are complex and involve improved insulin sensitivity, reduced inflammation, and changes in lipoprotein metabolism.
Improved cardiovascular health directly translates to increased longevity, as cardiovascular disease significantly impacts lifespan.
Metabolic Benefits of Periodic Fasting and Their Implications for Aging
The following list summarizes the metabolic benefits of periodic fasting and their implications for aging:
- Improved insulin sensitivity: Reduced risk of type 2 diabetes and its associated complications.
- Weight management: Reduced body fat and improved body composition.
- Enhanced autophagy: Removal of damaged cellular components and improved cellular function.
- Reduced inflammation: Mitigation of chronic inflammation, a driver of aging and disease.
- Improved mitochondrial function: Increased energy production and reduced cellular damage.
- Increased antioxidant production: Protection against oxidative stress and cellular damage.
- Favorable lipid profile changes: Reduced risk of cardiovascular disease.
- Potential for lifespan extension: Through a combination of the above mechanisms.
Animal Studies and Longevity
Source: nutritionfacts.org
The connection between periodic fasting and longevity has been extensively investigated in various animal models, providing valuable insights into the underlying mechanisms and potential benefits. These studies, while not directly translatable to humans, offer crucial preclinical evidence supporting the exploration of periodic fasting as a longevity intervention. The results vary depending on the animal species, fasting protocol employed, and other factors such as genetics and environmental conditions.
Rodent Studies and Longevity Outcomes
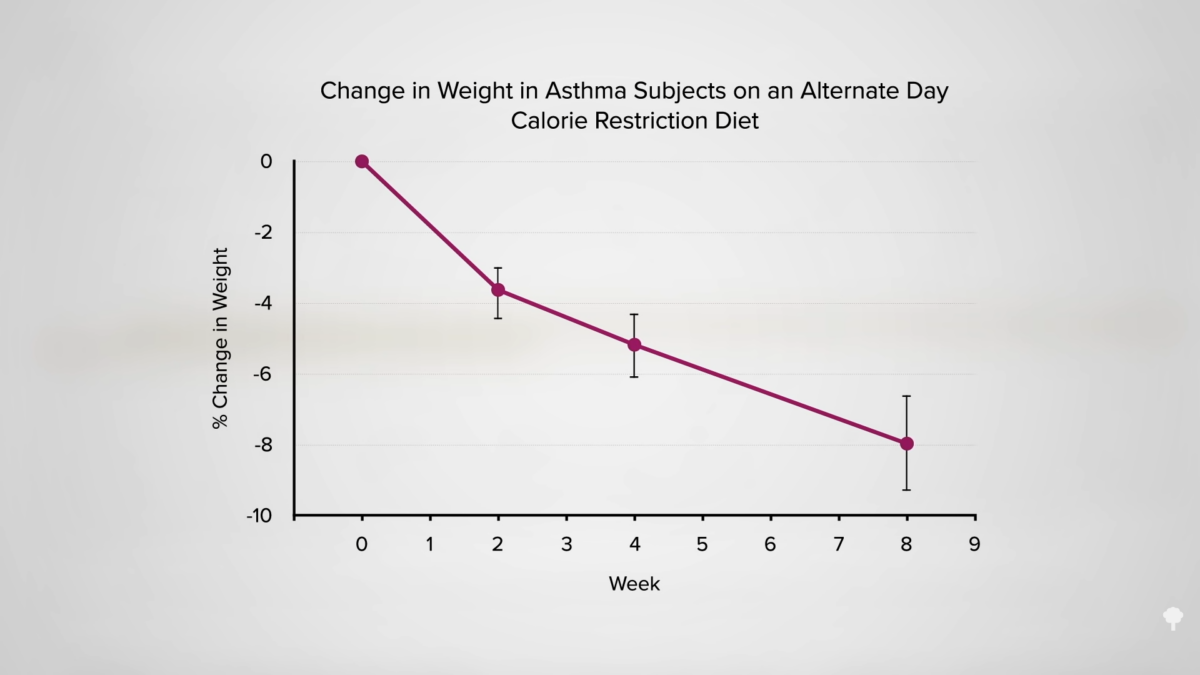
Numerous studies using rodents, primarily mice and rats, have demonstrated a significant increase in lifespan and healthspan (the duration of healthy life) associated with various periodic fasting regimens. These regimens include intermittent fasting (IF), where animals are fed during a restricted time window each day, and alternate-day fasting (ADF), where animals consume food on alternate days. For example, studies have shown that mice subjected to ADF exhibited extended lifespans compared to control groups fed ad libitum (meaning they had unrestricted access to food).
These extended lifespans were often accompanied by improvements in various health markers, including reduced body weight, improved insulin sensitivity, and decreased incidence of age-related diseases such as cancer and cardiovascular disease. Variations in the specific fasting protocols, such as the length of the fasting periods or the composition of the diet during feeding periods, have influenced the observed longevity effects.
Invertebrate Model Organisms and Longevity
Studies on invertebrate model organisms, such as the nematode
- Caenorhabditis elegans* and the fruit fly
- Drosophila melanogaster*, have also provided valuable data supporting the link between periodic fasting and longevity. These organisms are attractive models due to their short lifespans, ease of manipulation, and well-characterized genetics. Studies have shown that dietary restriction, which often overlaps with periodic fasting paradigms, can significantly extend lifespan in these organisms. For instance,
- C. elegans* subjected to intermittent periods of starvation have exhibited increased lifespan and improved stress resistance. Similarly,
- Drosophila* exposed to periodic fasting protocols have shown extended lifespans and improved metabolic health. The specific mechanisms involved may differ between species, but the overall trend suggests a conserved role for dietary restriction in promoting longevity across diverse organisms.
Caloric Restriction and Periodic Fasting: A Comparative Analysis
Caloric restriction (CR), a dietary regimen involving a consistent reduction in caloric intake without malnutrition, is well-established as a robust intervention that extends lifespan in various animal models. While CR and periodic fasting are distinct interventions, they share some overlapping effects. Both CR and periodic fasting can lead to reduced body weight, improved insulin sensitivity, and increased cellular stress resistance.
So I’ve been diving deep into the research on periodic fasting and its potential to extend lifespan – it’s fascinating! A key aspect of longevity, of course, is maintaining cognitive health, and that’s where this article on whether an eye test can detect dementia risk comes in: check out this interesting piece can eye test detect dementia risk in older adults.
Understanding early warning signs for neurodegenerative diseases is crucial, and it ties directly back to the bigger picture of how lifestyle choices, like periodic fasting, might impact our overall health and longevity.
Many studies suggest that the beneficial effects of periodic fasting may, in part, be mediated through the induction of similar metabolic adaptations observed in CR. However, periodic fasting offers a potentially more practical and sustainable approach compared to lifelong CR for many individuals. Direct comparisons between the effectiveness of CR and different periodic fasting regimens in extending lifespan require further investigation, as results can be dependent on factors like species and specific protocol used.
Summary of Key Findings from Animal Studies
| Species | Fasting Protocol | Longevity Effects | Other Observed Effects |
|---|---|---|---|
| Mice | Alternate-Day Fasting | Increased lifespan, up to 20% in some studies | Reduced body weight, improved insulin sensitivity, decreased cancer incidence |
| Rats | Intermittent Fasting (16/8) | Increased lifespan, improved metabolic markers | Improved cardiovascular health, reduced inflammation |
| C. elegans | Intermittent starvation | Significant lifespan extension | Increased stress resistance |
| Drosophila | Dietary restriction mimicking periodic fasting | Extended lifespan, improved metabolic health | Delayed aging-related decline |
Human Studies and Longevity

Source: healthfacts.ng
While animal studies provide valuable insights, the ultimate test of periodic fasting’s impact on longevity lies in human research. However, translating the promising results from animal models to humans presents significant challenges. Longitudinal studies, tracking individuals over many years, are necessary to observe the long-term effects on lifespan, making this area of research both complex and time-consuming.
Data from Human Studies and Associated Health Markers
Several human studies have explored the association between periodic fasting interventions, such as intermittent fasting (IF) and time-restricted feeding (TRF), and various health markers linked to longevity. These markers often include improvements in blood pressure, cholesterol levels, insulin sensitivity, and markers of inflammation. For example, a meta-analysis of several studies on intermittent fasting showed a significant reduction in body weight, body mass index (BMI), and waist circumference, all factors associated with increased longevity.
Another study examining time-restricted feeding demonstrated improvements in insulin sensitivity and reduced markers of oxidative stress, processes linked to aging and age-related diseases. However, the effects on lifespan itself remain largely inconclusive due to the limitations of the studies.
Limitations and Challenges in Conducting Human Studies
Conducting robust human studies on periodic fasting and longevity faces several key limitations. Firstly, the long lifespan of humans makes it difficult to conduct truly longitudinal studies that definitively prove an increase in lifespan. Secondly, adherence to fasting protocols varies significantly among individuals, making it difficult to control for compliance and accurately assess the effects of the intervention.
Thirdly, the diversity in human populations (genetics, lifestyle, dietary habits) makes it challenging to isolate the specific impact of periodic fasting on longevity. Finally, the lack of standardized protocols for periodic fasting makes it difficult to compare results across different studies.
Potential Confounding Factors
Many factors can confound the results of human studies on periodic fasting. Lifestyle factors such as exercise, overall dietary quality, and stress levels significantly influence health and longevity. Genetic predisposition also plays a crucial role in determining an individual’s susceptibility to age-related diseases. Furthermore, the presence of pre-existing health conditions and the use of medications can impact the outcomes, making it difficult to isolate the effects of periodic fasting alone.
For instance, an individual who engages in regular exercise and maintains a healthy diet alongside periodic fasting might experience greater health benefits than someone who does not.
Comparison of Observational Studies and Clinical Trials
Observational studies, which track individuals over time without intervention, can provide valuable insights into the association between periodic fasting and health markers. However, they cannot establish causality. Clinical trials, which involve controlled interventions, can better assess the effects of periodic fasting on specific health outcomes. While observational studies may suggest a correlation between periodic fasting and improved health markers, clinical trials are needed to demonstrate a causal relationship and to determine the optimal fasting protocols for maximizing health benefits.
A key difference lies in the ability to control for confounding factors, a strength of clinical trials over observational studies.
Ethical Considerations in Human Studies
Ethical considerations are paramount in research involving human subjects. Informed consent is essential, ensuring participants fully understand the risks and benefits of participating in the study. The potential for adverse effects, such as nutrient deficiencies or metabolic imbalances, must be carefully monitored and mitigated. The design of studies should minimize risks and maximize benefits, adhering to strict ethical guidelines and regulatory approvals.
Furthermore, researchers have a responsibility to ensure that the findings are accurately reported and interpreted, avoiding any misleading or exaggerated claims.
Potential Risks and Considerations
Periodic fasting, while showing promise in boosting longevity in some studies, isn’t without potential drawbacks. It’s crucial to understand these risks and tailor any fasting regimen to your individual health and circumstances. Ignoring potential problems can lead to negative consequences, undermining any potential benefits.
Potential Side Effects and Risks
The most common side effects of periodic fasting are generally mild and temporary, including headaches, fatigue, dizziness, and irritability, often experienced during the initial adaptation phase. More serious complications are rare but can occur, particularly in vulnerable populations. These might include nutrient deficiencies, electrolyte imbalances, and exacerbation of existing health conditions. For example, individuals with a history of eating disorders may find periodic fasting triggers unhealthy behaviors.
It’s vital to remember that the severity and likelihood of side effects vary considerably depending on the type of fasting, the individual’s health status, and adherence to proper guidelines.
Specific Populations and Considerations
Periodic fasting is not recommended for everyone. Pregnant and breastfeeding women should absolutely avoid it due to the increased nutritional needs of both mother and child. Individuals with certain medical conditions, such as diabetes, heart disease, or eating disorders, should consult their physician before attempting any fasting regimen. The body’s response to fasting is highly individual; those with a history of hypoglycemia, for example, are at a higher risk of experiencing dangerous blood sugar drops.
Children and adolescents are also generally advised against periodic fasting because of their developmental needs.
Factors Influencing Safe and Effective Fasting
Several factors can significantly influence an individual’s ability to safely and effectively practice periodic fasting. These include overall health status, genetic predisposition, medication use (some medications may interact negatively with fasting), level of physical activity, and the chosen fasting protocol itself. For instance, someone who is very active may require a different approach compared to someone with a sedentary lifestyle.
The type of fasting—whether it’s intermittent fasting, alternate-day fasting, or prolonged fasting—also impacts the potential risks and benefits. Proper hydration and mindful nutrient intake during eating windows are also essential for mitigating risks.
Recommendations for Safe and Effective Implementation
Before starting any periodic fasting regimen, it is crucial to consult with a healthcare professional. They can assess your individual health status, identify potential risks, and help you develop a safe and personalized plan. Gradual introduction to fasting, starting with shorter fasting periods and gradually increasing the duration, is generally recommended. Prioritizing whole, unprocessed foods during eating windows is vital to ensure adequate nutrient intake.
Regular monitoring of blood glucose levels (especially for those with diabetes or a history of hypoglycemia) and careful attention to hydration are also essential. Listening to your body and adjusting the plan based on individual needs is key to long-term success and safety.
Potential Risks and Precautions Related to Periodic Fasting
It is important to be aware of the following potential risks and take appropriate precautions:
- Nutrient deficiencies
- Electrolyte imbalances (e.g., low potassium)
- Headaches, dizziness, and fatigue
- Irritability and mood swings
- Exacerbation of existing medical conditions (e.g., diabetes, heart disease)
- Muscle loss (if protein intake is insufficient)
- Menstrual irregularities in women
- Increased risk of gallstones in some individuals
- Potential for triggering or worsening eating disorders
- Interactions with certain medications
Closure: The Link Between Periodic Fasting And Longevity
So, is periodic fasting the fountain of youth? While the research is still ongoing, the evidence strongly suggests a compelling link between periodic fasting and increased lifespan, at least in certain animal models and with certain health markers in humans. The key takeaway isn’t about strict adherence to a rigid fasting schedule, but rather a mindful approach to eating.
By understanding the mechanisms involved and carefully considering your individual health needs, you can explore the potential benefits of periodic fasting while mitigating any potential risks. Remember to always consult your doctor before making significant dietary changes.
Commonly Asked Questions
Is periodic fasting safe for everyone?
No, periodic fasting isn’t suitable for everyone. Pregnant or breastfeeding women, individuals with eating disorders, or those with certain medical conditions should avoid it without consulting a doctor. Even healthy individuals should start slowly and listen to their bodies.
What are the common side effects of periodic fasting?
Common side effects can include hunger, headaches, fatigue, dizziness, and irritability, especially in the initial stages. These usually subside as the body adapts.
How long does it take to see results from periodic fasting?
The timeframe varies depending on the individual and their goals. Some people report noticeable improvements in energy levels and weight within weeks, while others may take longer to see significant changes.
Can I combine periodic fasting with exercise?
Yes, but be mindful of your energy levels and listen to your body. Adjust your exercise intensity and duration as needed, especially when starting out.
