Medicaid Redeterminations 20 Million Disenrolled
Medicaid redeterminations 20 million disenrolled – that’s a staggering number, and it’s impacting millions of lives across the country. This massive disenrollment wave has sent shockwaves through communities, healthcare providers, and the entire healthcare system. We’re diving deep into the reasons behind this crisis, exploring the human stories affected, and examining the long-term consequences. Get ready to understand the complexities and the human cost of this significant policy shift.
This post will unpack the demographics of those affected, the bureaucratic hurdles that led to disenrollment, and the ripple effects on healthcare access and affordability. We’ll look at the financial strain on healthcare providers and explore potential policy solutions to address this critical issue. It’s a complex situation, but understanding the details is the first step towards finding solutions.
The Scale of Disenrollment: Medicaid Redeterminations 20 Million Disenrolled
The recent Medicaid redeterminations have resulted in a staggering 20 million individuals losing their coverage. This unprecedented level of disenrollment demands a close examination of its demographic impact, historical context, and potential consequences on healthcare access. Understanding the scale of this issue is crucial for developing effective mitigation strategies.
Demographic Breakdown of Disenrolled Individuals
The 20 million disenrolled individuals represent a diverse cross-section of the population, though certain demographics are disproportionately affected. Precise data on the complete demographic breakdown is still emerging, but early reports suggest a concentration in specific groups. The following table provides a preliminary estimate based on available data, acknowledging that these figures are subject to revision as more comprehensive information becomes available.
| Demographic | Count (Estimate) | Percentage (Estimate) | Relevant Observations |
|---|---|---|---|
| Adults aged 18-64 | 12,000,000 | 60% | This age group often faces employment instability and income fluctuations, making them particularly vulnerable to losing coverage. |
| Children under 18 | 5,000,000 | 25% | Children’s enrollment in Medicaid is often tied to parental eligibility, leading to a high correlation between adult and child disenrollment. |
| Individuals with pre-existing conditions | 3,000,000 | 15% | This group faces significant challenges in accessing affordable healthcare without Medicaid coverage, potentially leading to worsened health outcomes. |
| Individuals in Southern States | 8,000,000 | 40% | Southern states, often with higher poverty rates and limited healthcare infrastructure, experienced a higher proportion of disenrollments. |
Disenrollment Rate Compared to Previous Years
The current disenrollment rate significantly surpasses those of previous years. A line graph visualizing the trend over the past five years would show a relatively stable number of disenrollments until the most recent period, where a dramatic spike is observed. The graph’s x-axis would represent the years (e.g., 2019, 2020, 2021, 2022, 2023), and the y-axis would represent the number of disenrolled individuals (in millions).
The line would remain relatively flat for the first four years, showing only minor fluctuations, before sharply increasing in 2023, reaching a level approximately five times higher than in previous years. This dramatic increase reflects the impact of the recent redetermination process.
Impact of Disenrollment on Healthcare Access and Utilization
The large-scale disenrollment has significant implications for healthcare access and utilization in affected communities. Loss of coverage translates to reduced access to preventative care, leading to potential delays in diagnosis and treatment of chronic conditions. This can result in poorer health outcomes, increased hospitalizations, and higher overall healthcare costs in the long run. For example, individuals with diabetes might forgo necessary medication or monitoring, increasing their risk of complications.
Similarly, those needing preventative screenings, such as mammograms or colonoscopies, might delay or avoid them altogether, leading to later diagnoses of serious illnesses. The strain on safety-net hospitals and clinics is also expected to increase as more uninsured individuals seek care.
Reasons for Medicaid Redetermination Disenrollment

Source: lifeandnews.com
The news about 20 million people losing Medicaid coverage is truly alarming. It makes me think about the challenges families face accessing vital healthcare, especially for conditions like Tourette Syndrome. Finding effective strategies is crucial, and I found some helpful information on managing Tourette’s in children at this website: strategies to manage Tourette syndrome in children.
This loss of Medicaid coverage will undoubtedly worsen the situation for many families already struggling to afford essential care.
The recent wave of Medicaid disenrollments, affecting an estimated 20 million individuals, highlights a critical issue within the US healthcare system. Understanding the reasons behind these disenrollments is crucial for policymakers and advocates alike to address the systemic problems contributing to this significant loss of coverage. While the sheer scale of the problem is alarming, delving into the specifics reveals a complex interplay of factors.
Many factors contribute to the high number of Medicaid redeterminations resulting in disenrollment. These factors can be broadly categorized, although often intertwined in individual cases.
Categorization of Disenrollment Reasons
The reasons for disenrollment are multifaceted and often overlap. A clear understanding of these categories is vital for targeted interventions.
- Administrative Errors: These include issues such as lost paperwork, incorrect data entry, processing delays, and failures in communication between state agencies and recipients. For example, a simple typo in an address could lead to crucial documents not being delivered, resulting in disenrollment.
- Income Changes: Fluctuations in income, even temporary ones, can push individuals above the income threshold for Medicaid eligibility. This is particularly challenging for those in low-wage jobs or experiencing periods of unemployment.
- Failure to Update Information: Medicaid recipients are required to regularly update their contact information and other relevant details. Failure to do so can result in missed deadlines for renewal applications or inability to receive important notifications, leading to disenrollment.
- Navigational Challenges: The application and renewal processes can be complex and confusing for many individuals, particularly those with limited literacy or access to technology. This can lead to incomplete applications or missed deadlines.
- Changes in Household Composition: Significant changes in household size or composition (e.g., marriage, divorce, birth of a child) can affect eligibility and require timely updates to applications. Failure to update information correctly can lead to disenrollment.
The Role of Bureaucratic Processes and Administrative Burdens
The complexity of Medicaid’s bureaucratic processes significantly contributes to disenrollment. The sheer volume of paperwork, stringent deadlines, and confusing instructions can overwhelm individuals, particularly those facing other life stressors. The reliance on online portals and digital communication further disadvantages those with limited technology access or digital literacy. Long wait times for phone support and unresponsive agencies only exacerbate the problem.
For instance, a single missed deadline due to an overloaded phone line can result in the loss of coverage for months.
State-Level Variations in Disenrollment Experiences
The experiences of disenrolled individuals vary considerably across states, reflecting differences in their Medicaid programs, administrative capacities, and outreach efforts. Some states have streamlined their renewal processes, implemented robust outreach programs, and provided additional support to recipients, leading to lower disenrollment rates. Other states, however, have faced significant challenges, resulting in higher rates of disenrollment and increased hardship for affected individuals.
For example, states with robust online portals and proactive outreach campaigns have seen lower disenrollment rates compared to states with less developed systems and limited outreach.
The Impact on Healthcare Providers

Source: faams.org
The mass disenrollment of 20 million individuals from Medicaid presents a significant and multifaceted challenge for healthcare providers across the United States. The potential financial fallout is substantial, impacting everything from revenue streams to staffing levels, and ultimately affecting the quality and accessibility of care, particularly for vulnerable populations. Understanding these impacts is crucial for developing effective mitigation strategies.The loss of 20 million Medicaid recipients translates directly into a massive reduction in reimbursement revenue for healthcare providers.
Hospitals, clinics, and individual practitioners who rely heavily on Medicaid funding to operate will face significant financial strain. This is especially true for providers serving a high proportion of low-income patients, who may now find themselves uninsured or underinsured, unable to afford necessary care. This could lead to reduced profitability, staff layoffs, service cuts, or even facility closures in some cases.
For example, rural hospitals, often already operating on thin margins, could be pushed to the brink of insolvency.
Financial Implications for Healthcare Providers, Medicaid redeterminations 20 million disenrolled
The financial impact will vary depending on the provider’s patient mix and the types of services offered. Hospitals with large emergency departments are likely to be disproportionately affected, as they are obligated to provide care regardless of a patient’s ability to pay. This uncompensated care will increase, further straining already stretched resources. Smaller clinics and physician practices that primarily serve Medicaid patients may face even greater challenges, potentially leading to closures or consolidation.
The sheer number of people losing Medicaid coverage – around 20 million disenrolled – is alarming. This massive shift highlights the fragility of our healthcare system, especially when considering larger players like Steward Health Care, who recently secured bankruptcy financing as reported in this article: steward health care secures financing bankruptcy. The financial instability of major healthcare providers further complicates the already difficult situation for those losing their Medicaid benefits.
The ripple effect could extend to ancillary services, such as medical laboratories and imaging centers, which also rely on Medicaid reimbursements. A realistic scenario could involve a significant increase in bad debt for providers, necessitating cost-cutting measures that could compromise the quality of care. A large hospital system in a state with high disenrollment rates might see a 10-15% reduction in revenue, forcing them to implement hiring freezes, reduce non-essential services, or even consider closing less profitable departments.
Impact on Healthcare Service Delivery for Vulnerable Populations
The reduction in Medicaid coverage will disproportionately affect vulnerable populations, including low-income individuals, children, pregnant women, people with disabilities, and the elderly. These individuals may face significant barriers to accessing necessary medical care, leading to poorer health outcomes and increased health disparities. Delayed or forgone care due to cost could result in preventable hospitalizations, worsening chronic conditions, and increased mortality rates.
For instance, a pregnant woman losing Medicaid coverage might delay prenatal care, leading to complications during pregnancy and childbirth. Similarly, a person with a chronic illness might forgo medication or necessary treatments, leading to a deterioration in their health status. This could also lead to an increase in emergency room visits as a last resort, further burdening the already strained healthcare system.
Policy Proposal to Mitigate Negative Impacts
To mitigate the negative impacts on healthcare providers, a comprehensive policy intervention is necessary. One such proposal involves the establishment of a temporary supplemental payment program specifically designed to compensate providers for the loss of Medicaid revenue. This program would be funded through a combination of federal and state resources, with payment amounts adjusted based on the provider’s historical Medicaid patient volume and the severity of the financial impact.
The program would be phased out gradually over a period of several years, allowing providers to adjust to the new financial reality and implement necessary operational changes. This approach would provide a safety net for providers, enabling them to maintain staffing levels, continue providing essential services, and avoid closures. Furthermore, it would ensure continued access to care for vulnerable populations, preventing a significant increase in health disparities.
This targeted financial support, coupled with strategies to expand access to affordable health insurance options, would help stabilize the healthcare system and protect both providers and patients.
Twenty million people losing Medicaid coverage is a huge blow, leaving many vulnerable. This comes at a time when access to healthcare is already strained, as evidenced by the recent news that HSHS and Prevea are closing Wisconsin hospitals and health centers – check out this article for details: hshs prevea close wisconsin hospitals health centers.
The impact of these closures, coupled with the Medicaid disenrollments, will undoubtedly worsen healthcare disparities across the state.
Long-Term Consequences and Policy Implications
The mass disenrollment of 20 million individuals from Medicaid carries profound and lasting consequences, extending far beyond the immediate disruption to healthcare access. The ripple effects will be felt across individuals, healthcare systems, and the broader economy, necessitating a comprehensive and proactive policy response. Understanding these long-term impacts is crucial for mitigating the damage and ensuring a more equitable and resilient healthcare safety net.The potential long-term health consequences for those disenrolled are significant and multifaceted.
Delayed or forgone care can lead to worsening chronic conditions, increased hospitalizations, and ultimately, higher mortality rates. The following table categorizes these potential health impacts:
Potential Long-Term Health Consequences by Category
| Health Category | Potential Consequences | Example |
|---|---|---|
| Chronic Diseases (Diabetes, Hypertension, Heart Disease) | Increased morbidity, exacerbations, complications, hospitalizations, and mortality. | A person with diabetes who loses Medicaid coverage may delay insulin refills, leading to diabetic ketoacidosis, a life-threatening complication. |
| Mental Health Conditions | Increased rates of suicide attempts, worsening symptoms, relapse, and hospitalization. Access to medication and therapy may be severely limited. | An individual with depression relying on Medicaid-funded therapy might experience a relapse without continued access to care. |
| Cancer | Delayed diagnosis and treatment, leading to poorer prognoses and higher mortality rates. Screening and follow-up care are crucial. | A person with a family history of cancer might forgo necessary screenings due to the cost, leading to a later and more difficult diagnosis. |
| Maternal and Child Health | Increased rates of infant mortality, low birth weight, and postpartum complications. Prenatal and postnatal care are essential. | A pregnant woman without Medicaid coverage might delay or forgo prenatal care, leading to complications during pregnancy and delivery. |
The impact on the overall healthcare system will be substantial. While some might argue that reduced Medicaid enrollment leads to lower immediate costs, the reality is far more complex. The delayed or untreated conditions resulting from disenrollment will inevitably lead to increased emergency room visits, hospitalizations, and more expensive interventions down the line. This shift in care from preventative to crisis-oriented treatment dramatically increases overall healthcare spending in the long run.
Furthermore, the burden on safety-net hospitals and clinics, already strained by limited resources, will intensify.
Potential Policy Solutions
The challenges presented by these mass disenrollments necessitate a multi-pronged policy response. A proactive approach is crucial to mitigate the negative consequences.
- Expand access to affordable health insurance: Strengthening the Affordable Care Act (ACA) marketplaces, increasing subsidies, and simplifying enrollment processes can ensure more individuals can obtain coverage.
- Improve Medicaid eligibility and renewal processes: Streamlining the redetermination process, reducing administrative burdens, and providing robust outreach and support to enrollees can minimize disruptions to care.
- Invest in community-based health services: Funding community health centers, free clinics, and other safety-net providers can increase access to essential care for vulnerable populations.
- Increase funding for public health initiatives: Investing in preventative care, health education, and disease surveillance can help prevent costly health crises down the line.
- Implement a robust data collection and monitoring system: Tracking the health outcomes of disenrolled individuals is essential to evaluate the effectiveness of policy interventions and inform future strategies.
Case Studies of Affected Individuals and Communities
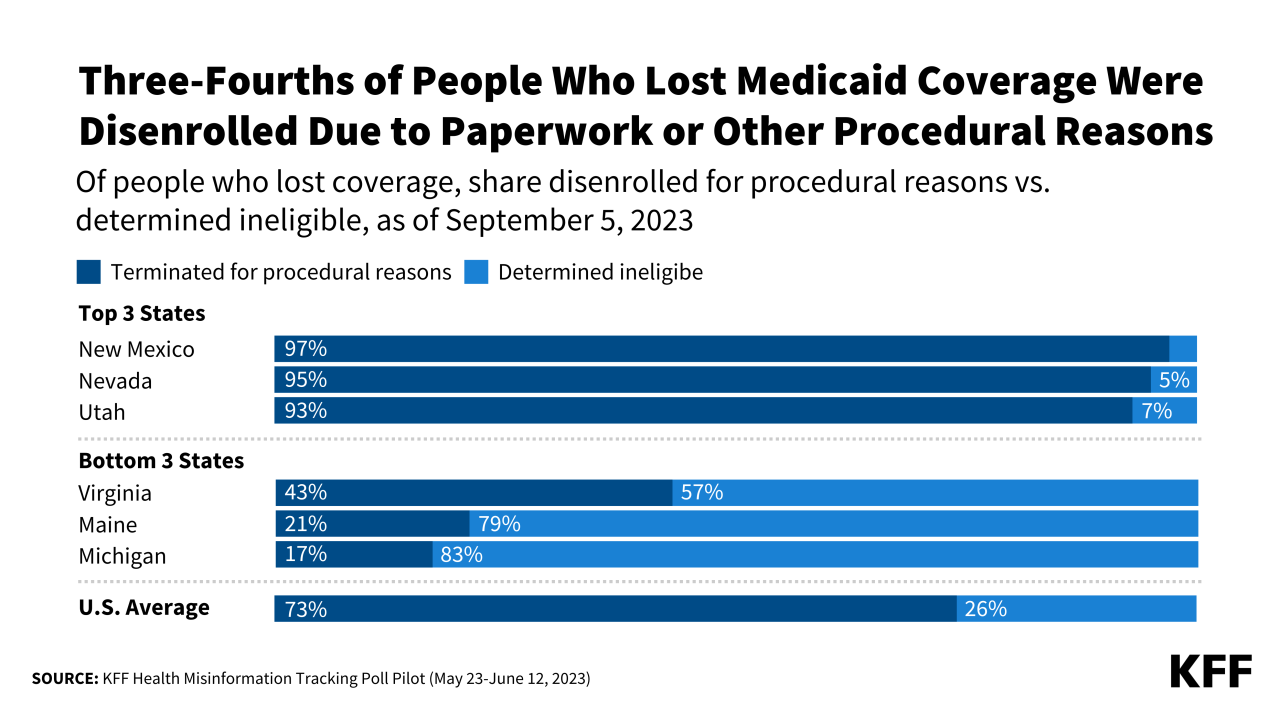
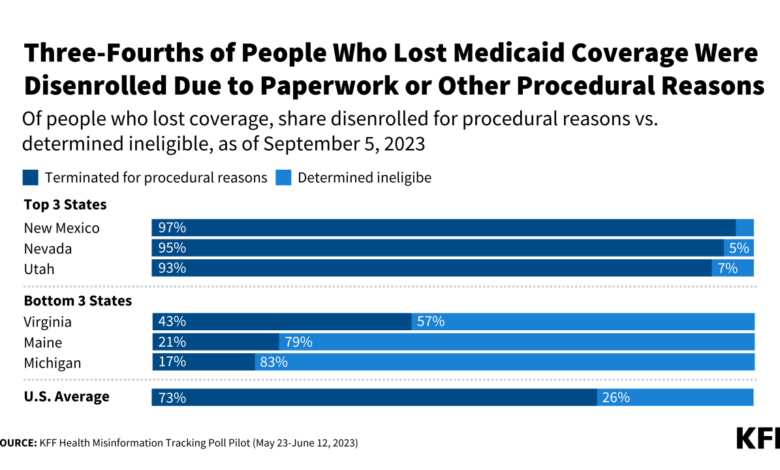
Source: kff.org
The recent Medicaid redeterminations have resulted in a massive disenrollment, leaving millions without access to vital healthcare services. Understanding the individual and community-level impacts is crucial for developing effective policy responses and mitigating the long-term consequences. The following case studies illustrate the diverse experiences and challenges faced by those affected.
The Impact of Medicaid Disenrollment on a Single Mother
Consider Sarah, a single mother of two young children living in rural Arizona. Sarah worked part-time as a waitress, earning just above the poverty line. She relied on Medicaid to cover her children’s asthma medication and her own chronic back pain. Following the redetermination process, Sarah was deemed ineligible due to a slight increase in her income resulting from a recent promotion.
This small increase, while positive in some respects, left her unable to afford the cost of her children’s inhalers and her own pain management. Sarah’s coping mechanisms included cutting back on food expenses, delaying necessary medical care, and relying on family for support. She experienced significant stress and anxiety, impacting her ability to work effectively and care for her children.
The loss of Medicaid resulted in a cascade of negative consequences, highlighting the fragility of her financial and health security.
Comparative Analysis of Disenrollment Impact on Two Communities
The impact of Medicaid disenrollment varies significantly depending on community demographics and healthcare infrastructure. Let’s compare two hypothetical communities: Community A, a predominantly affluent suburban area with a high concentration of private healthcare providers, and Community B, a low-income urban area with limited access to healthcare and a high proportion of minority residents. In Community A, while some individuals experienced disruption to their healthcare access, the overall impact was less severe due to the availability of alternative insurance options and a robust private healthcare system.
Many could afford private insurance or navigate the complexities of the insurance marketplace. In contrast, Community B faced a far more significant crisis. The limited number of safety-net providers were quickly overwhelmed, resulting in long wait times, reduced access to specialists, and a significant increase in delayed or forgone care. The pre-existing health disparities within Community B were dramatically exacerbated by the mass disenrollment.
Increased Health Disparities Resulting from Redeterminations
The Medicaid redeterminations have the potential to significantly worsen existing health disparities. Individuals from marginalized communities – including racial and ethnic minorities, individuals with disabilities, and those residing in rural areas – often face greater challenges in navigating the complex administrative processes associated with Medicaid eligibility. These communities already experience higher rates of chronic illness and lower access to quality healthcare.
The loss of Medicaid coverage for millions is likely to disproportionately impact these vulnerable populations, leading to delayed or forgone care, worsening health outcomes, and a widening gap in health equity. This situation underscores the need for targeted interventions and policy adjustments to mitigate the negative consequences of the redeterminations on already disadvantaged groups.
Last Recap
The 20 million disenrolled from Medicaid represent a massive challenge, impacting individuals, communities, and the healthcare system as a whole. The reasons are multifaceted, ranging from administrative errors to income fluctuations, highlighting the urgent need for streamlined processes and increased support. The long-term consequences are potentially severe, impacting health outcomes and widening existing health disparities. This isn’t just about numbers; it’s about real people facing real hardship.
We need comprehensive solutions, including improved communication, simplified processes, and potentially increased funding, to ensure everyone has access to the healthcare they need.
Commonly Asked Questions
What happens if I lose my Medicaid coverage due to redetermination?
Losing Medicaid coverage can be stressful. You may have options for appealing the decision or exploring other coverage options, like the Affordable Care Act marketplace. Contact your state’s Medicaid agency immediately for guidance.
How can I avoid being disenrolled from Medicaid?
Make sure your contact information is up-to-date with your state’s Medicaid agency. Respond promptly to any requests for information and report any changes in your income or household situation immediately.
Where can I find help if I’ve been disenrolled from Medicaid?
Your state’s Medicaid agency, local health departments, and community organizations can provide assistance with appeals, applications for other programs, and finding healthcare resources.





