ACA Broker Enforcement Rule Biden, CMS & You
Aca broker enforcement rule biden cms – ACA Broker Enforcement Rule: Biden, CMS & You – sounds dry, right? Wrong! This actually impacts
-you*, whether you’re an ACA broker navigating the shifting sands of regulatory compliance, or a consumer trying to understand the Affordable Care Act. The Biden administration’s approach to enforcing rules governing ACA brokers is dramatically different from its predecessor, creating both opportunities and challenges.
We’ll unpack the changes, the CMS’s role, and what it all means for you.
From stricter penalties for violations to a renewed focus on consumer protection, the landscape has shifted significantly. This post delves into the specifics of these changes, examining the CMS’s regulatory authority, the impact on brokers, and the implications for those seeking health insurance. We’ll also explore real-world case studies to illustrate the consequences of non-compliance and highlight the importance of understanding these new rules.
Biden Administration’s Approach to ACA Broker Enforcement: Aca Broker Enforcement Rule Biden Cms

Source: ytimg.com
The Biden administration inherited a complex landscape regarding the Affordable Care Act (ACA) and the role of brokers in its marketplace. Previous enforcement actions had varied, leading to inconsistencies and concerns about consumer protection. The current administration’s approach aims to strike a balance between fostering a competitive marketplace and ensuring consumers are not misled or harmed by unethical practices.
Stated Policy Goals Regarding ACA Broker Enforcement
The Biden administration’s stated policy goals concerning ACA broker enforcement center on protecting consumers and ensuring the integrity of the ACA marketplace. This involves preventing fraud, deception, and other unfair practices by brokers. The administration seeks to promote transparency and accountability within the broker community, empowering consumers to make informed decisions about their health insurance coverage. This goal is achieved through a combination of proactive outreach, education, and robust enforcement actions against those who violate the rules.
The ultimate aim is to maintain a healthy and competitive marketplace that serves the needs of all Americans.
Changes in Enforcement Strategies Since the Biden Administration Took Office
Since taking office, the Biden administration has implemented several changes in its ACA broker enforcement strategies. These changes reflect a shift towards a more proactive and preventative approach, focusing on education and outreach alongside robust enforcement. The administration has increased resources dedicated to investigating complaints and pursuing violations. There has also been a greater emphasis on collaboration with state insurance departments to share information and coordinate enforcement efforts.
This collaborative approach leverages the expertise of state regulators and streamlines investigations. Furthermore, the administration has focused on clarifying existing regulations and providing more guidance to brokers to help them understand their obligations and avoid unintentional violations.
Comparison of Current and Previous Administration’s Enforcement Approaches
Compared to the previous administration, the Biden administration’s approach to ACA broker enforcement is characterized by a greater emphasis on consumer protection and a more collaborative approach with state regulators. While the previous administration also pursued enforcement actions, the current administration seems to prioritize proactive measures, such as education and outreach, to prevent violations before they occur. This preventative approach aims to reduce the overall number of violations and improve compliance within the broker community.
The previous administration’s approach, while effective in certain instances, may have been perceived as more reactive, focusing primarily on responding to reported violations rather than proactively preventing them.
The Biden administration’s tightening of ACA broker enforcement rules is a hot topic, especially with the CMS’s recent actions. This increased scrutiny comes at a time when Robert F. Kennedy Jr. cleared a key hurdle in his bid to become HHS Secretary, as reported here: rfk jr clears key hurdle on path to hhs secretary. His potential appointment could significantly impact the future direction of ACA enforcement and the CMS’s overall approach to healthcare regulations.
Key Differences in Enforcement Priorities Between Administrations
| Enforcement Aspect | Trump Administration | Biden Administration |
|---|---|---|
| Enforcement Focus | Reactive, responding to reported violations | Proactive, preventing violations through education and outreach |
| Interagency Collaboration | Limited interagency collaboration | Increased collaboration with state insurance departments |
| Emphasis on Consumer Protection | Less emphasis on proactive consumer protection | Strong emphasis on consumer protection and education |
| Resource Allocation | Limited resources allocated to ACA broker enforcement | Increased resources dedicated to investigations and enforcement |
CMS Role in ACA Broker Enforcement
The Centers for Medicare & Medicaid Services (CMS) plays a crucial role in ensuring compliance with the Affordable Care Act (ACA) marketplace regulations. Their oversight of ACA brokers is vital to maintaining the integrity of the health insurance marketplace and protecting consumers. This involves a multifaceted approach encompassing regulatory authority, enforcement actions, and penalties for non-compliance.CMS’s regulatory authority over ACA brokers stems from its responsibility for administering the ACA marketplaces.
This authority is established through various sections of the ACA and related regulations. Essentially, CMS acts as the primary regulatory body overseeing the conduct of brokers who participate in the ACA marketplace. Their power to enforce rules is considerable, extending to investigations, penalties, and even exclusion from the marketplace.
Key Regulations Governing ACA Broker Activities
The primary regulations CMS utilizes to oversee ACA broker activities are focused on ensuring brokers act ethically and in the best interest of their clients. These regulations address key areas such as broker certification, marketing practices, and client interactions. For example, brokers are required to complete specific training and pass an examination before being certified to sell ACA plans.
They are also subject to rules prohibiting deceptive or misleading marketing practices, and are obligated to act as fiduciaries, prioritizing the needs of their clients above their own financial gain. Failure to comply with these regulations can result in serious consequences.
Penalties for Violations of ACA Broker Regulations
CMS can impose a range of penalties for violations of ACA broker regulations, depending on the severity and nature of the offense. These penalties can include warnings, fines, temporary or permanent suspension of certification, and even referral to state or federal law enforcement agencies for further action. The financial penalties can be substantial, and the reputational damage caused by a CMS enforcement action can severely impact a broker’s business.
The Biden administration’s ACA broker enforcement rules are definitely a hot topic, impacting access to healthcare. It’s crucial to remember that pre-existing conditions, like high blood pressure – a major risk factor for stroke – can significantly impact affordability and access. Understanding the risk factors that make stroke more dangerous is vital, especially given the complexities of navigating the ACA marketplace and the new enforcement measures.
This highlights the need for clear, accessible information to help individuals make informed decisions about their health coverage.
The aim is not only to punish offenders but also to deter future violations and protect consumers.
Examples of Past CMS Enforcement Actions Against ACA Brokers
While specific details of enforcement actions are often confidential due to privacy concerns, public records may reveal instances where CMS has taken action against brokers for violations such as misrepresenting plan benefits, engaging in deceptive marketing practices, or failing to maintain proper records. These actions highlight the seriousness with which CMS takes enforcement and serve as a reminder of the importance of compliance for all ACA brokers.
For instance, past cases might involve brokers facing fines for knowingly enrolling individuals in plans that didn’t meet their needs, or brokers being suspended for failing to complete required continuing education. The specific details of such cases are often not publicized in full detail, but the general outcomes demonstrate CMS’s commitment to enforcement.
Impact of the Rule Changes on ACA Brokers
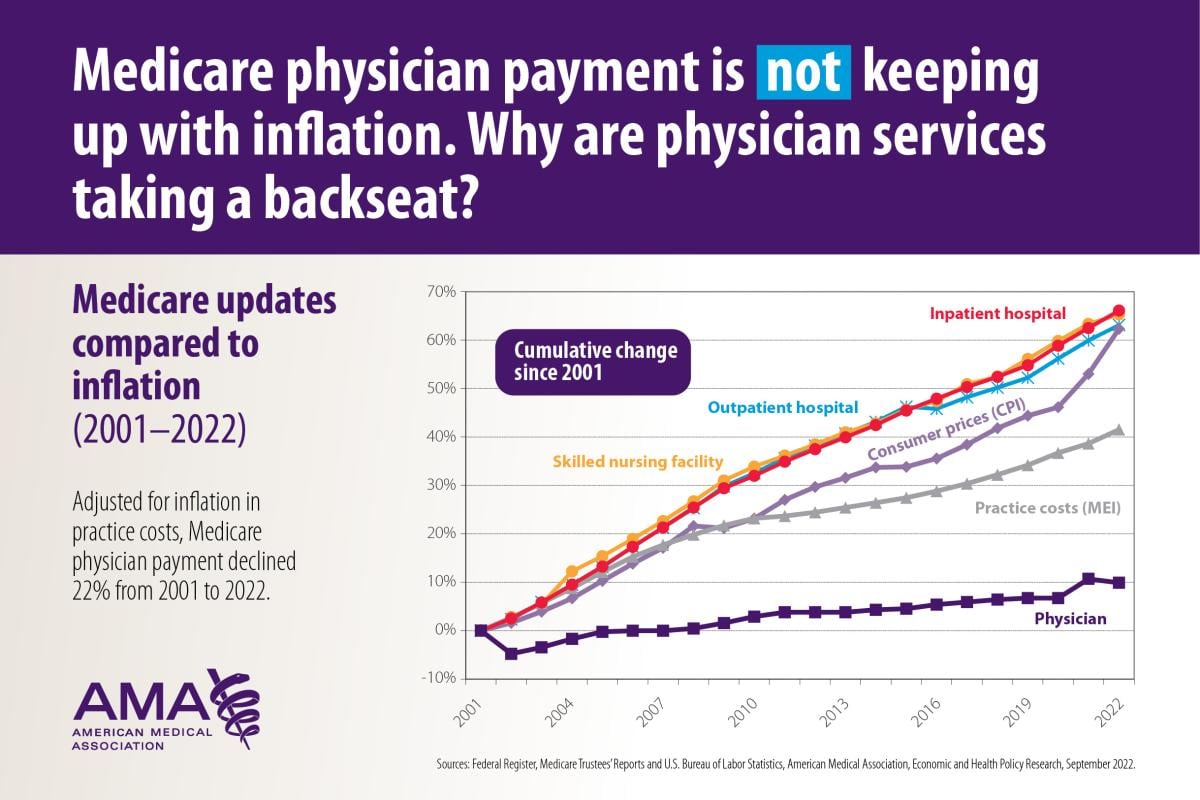
Source: ama-assn.org
The Biden administration’s strengthened enforcement of ACA broker regulations has significantly reshaped the landscape for those navigating the Affordable Care Act marketplace. These changes, while aimed at protecting consumers, have introduced new challenges and complexities for brokers, impacting their operations, legal compliance, and ultimately, their bottom lines. The ripple effects are far-reaching, necessitating adaptation and potentially impacting the accessibility of ACA plans for some consumers.The stricter enforcement measures have forced ACA brokers to re-evaluate their business practices, focusing on enhanced compliance and risk mitigation.
This has resulted in increased administrative burdens, requiring more rigorous documentation, training, and internal controls. The financial implications are substantial, demanding significant investments in compliance infrastructure and potentially impacting profitability. We can analyze these effects across legal, operational, and financial categories.
Legal Implications for ACA Brokers, Aca broker enforcement rule biden cms
The heightened scrutiny necessitates a meticulous approach to compliance. Brokers now face a higher risk of penalties for even minor infractions, such as inaccurate information provided to clients or failure to maintain proper documentation. This increased risk of legal action necessitates significant investment in legal counsel and compliance training to ensure adherence to all regulations. For example, a broker might need to invest in new software to ensure accurate data entry and reporting, or hire additional staff to manage the increased paperwork.
This heightened legal risk translates directly into increased costs for brokers.
Operational Changes in Broker Practices
Many brokers have responded to the stricter enforcement by implementing robust internal control systems. This includes more thorough client onboarding processes, enhanced record-keeping practices, and regular internal audits to ensure compliance. Some brokers have opted to utilize specialized software designed to automate compliance tasks, reducing the risk of human error and streamlining workflows. For instance, a broker might switch to a new CRM system that integrates with the CMS data systems to ensure all client information is accurate and up-to-date.
This operational overhaul, while necessary for compliance, comes at a significant cost.
Financial Impacts on ACA Brokers
The financial consequences of the stricter enforcement are multifaceted. Increased legal fees, compliance software costs, and the need for additional staff all contribute to higher operating expenses. The potential for penalties and legal action adds another layer of financial uncertainty. Some brokers, especially smaller firms, might find it challenging to absorb these increased costs, potentially leading to reduced profit margins or even business closures.
For example, a broker who faces a significant fine for a compliance violation might struggle to recover financially, potentially impacting their ability to serve clients effectively. The overall financial burden necessitates a thorough reassessment of business models and pricing strategies.
Consumer Protection Aspects of the Rule

Source: logos-world.net
The new ACA broker enforcement rules represent a significant step towards bolstering consumer protection in the marketplace for Affordable Care Act health insurance plans. These rules aim to prevent unscrupulous practices by brokers, ensuring consumers receive accurate information and are not misled into purchasing unsuitable or overpriced plans. The enhanced oversight and penalties significantly reduce the risk of consumers falling victim to fraud or deceptive sales tactics.The rules specifically target several consumer vulnerabilities.
Many individuals navigating the complexities of the ACA marketplace lack the time, resources, or expertise to independently verify the information provided by brokers. Others may be particularly susceptible to high-pressure sales tactics or deceptive marketing strategies, especially those with pre-existing conditions or limited health literacy. Finally, the sheer volume of plan options and ever-changing regulations can overwhelm consumers, making them more vulnerable to misinformation.
Vulnerable Consumer Groups and Targeted Protections
The rules aim to protect several vulnerable groups. For instance, those with limited English proficiency are particularly vulnerable to misinformation, as are seniors who may be less tech-savvy and more reliant on in-person broker assistance. The rules address this by requiring brokers to provide clear and accurate information in multiple languages and through accessible formats. Individuals with pre-existing conditions are also specifically protected; the rules prohibit brokers from steering them towards plans that don’t adequately cover their needs.
Furthermore, the rules explicitly address the vulnerability of low-income individuals who may be more susceptible to pressure tactics promising low premiums without fully explaining the implications.
Mechanisms Enhancing Consumer Protection
The enhanced enforcement mechanisms include stricter licensing requirements for brokers, increased monitoring of their activities, and significantly higher penalties for violations. CMS (Centers for Medicare & Medicaid Services) will have more robust oversight capabilities, enabling quicker detection and resolution of consumer complaints. This includes improved data collection and analysis to identify patterns of misconduct and proactively address potential problems.
The rules also mandate increased transparency, requiring brokers to disclose all commissions and incentives they receive, preventing conflicts of interest that could lead to biased recommendations. Consumers now have clearer avenues for filing complaints and accessing redress for any harm suffered due to broker misconduct.
Hypothetical Scenario Illustrating Consumer Protection
Imagine Maria, a 65-year-old retiree with a limited income and a pre-existing heart condition. Before the new rules, a broker might have steered her towards a plan with a low premium but extremely high out-of-pocket costs, failing to fully explain the implications. This broker might have received a substantial commission for selling this plan. Under the new rules, this broker would be subject to stricter scrutiny.
The required transparency regarding commissions would expose the potential conflict of interest. Furthermore, Maria would have clearer access to information about the plan’s cost-sharing, and any misleading statements by the broker could lead to significant penalties for the broker and potential compensation for Maria. The increased oversight and robust complaint mechanisms would ensure a faster and more effective resolution to Maria’s situation.
Challenges and Future Directions in ACA Broker Enforcement
Effectively enforcing ACA broker regulations presents a complex challenge, demanding a multifaceted approach that balances consumer protection with the practical realities of a dynamic marketplace. The sheer volume of brokers, coupled with the intricacies of the ACA itself, creates significant hurdles for regulators. Moreover, the rapid evolution of technology and the increasing sophistication of fraudulent schemes require constant adaptation and innovation in enforcement strategies.
Challenges in ACA Broker Enforcement
Several key challenges hinder effective enforcement of ACA broker regulations. Firstly, resource constraints within regulatory agencies often limit their capacity for comprehensive oversight. This can lead to delays in investigations and a potentially slower response to emerging compliance issues. Secondly, the decentralized nature of the broker market makes it difficult to track and monitor all activities. Many brokers operate independently, making it challenging to detect and address widespread non-compliance.
Finally, the complexity of the ACA itself presents a challenge for both brokers and regulators. The numerous rules and regulations, coupled with frequent updates, can lead to unintentional errors and misunderstandings, even among well-intentioned brokers. For example, accurately determining eligibility for subsidies and navigating the nuances of plan selection requires a high level of expertise, making it easy for mistakes to occur.
Areas for Improvement in the Enforcement Process
Improving the enforcement process requires a multi-pronged approach. Increased funding for regulatory agencies would enable more robust oversight and investigation capabilities. The development of sophisticated data analytics tools could help identify patterns of non-compliance and prioritize investigations. This could include analyzing sales data, consumer complaints, and other relevant information to flag potential problems. Furthermore, enhancing collaboration between regulatory agencies and other stakeholders, such as consumer advocacy groups, would improve information sharing and facilitate more effective enforcement.
A standardized reporting system across different agencies would also streamline data collection and analysis.
Potential Future Changes to ACA Broker Regulations
Future changes to ACA broker regulations could focus on greater clarity and simplification. Streamlining the rules and providing more easily accessible guidance for brokers would reduce ambiguity and minimize unintentional errors. Regulations could also be updated to reflect the evolving landscape of health insurance and technology. For instance, regulations might address the increasing role of online platforms and digital marketing in the sale of ACA plans.
This could include clear guidelines on advertising practices and consumer data protection. Moreover, increased penalties for serious violations could serve as a stronger deterrent against non-compliance. The implementation of stricter licensing requirements could also help improve the overall quality and competence of ACA brokers.
Technology’s Role in Improving ACA Broker Enforcement
Technology plays a crucial role in enhancing the effectiveness of ACA broker enforcement. The development of a centralized database to track broker licenses, compliance history, and consumer complaints would provide regulators with a comprehensive overview of the market. This database could be used to identify high-risk brokers and prioritize investigations. Furthermore, advanced data analytics techniques could help detect patterns of fraud and non-compliance, allowing for proactive intervention.
AI-powered tools could be employed to analyze large datasets, identify anomalies, and flag potential violations. Real-time monitoring of broker activities, through the use of secure data sharing agreements, could enable regulators to respond quickly to emerging compliance issues. This could include the use of web scraping technologies to monitor broker websites for compliance with advertising regulations. Finally, improved online portals for brokers to submit required information could streamline the reporting process and reduce administrative burdens.
Case Studies of ACA Broker Enforcement Actions
The Affordable Care Act (ACA) relies heavily on brokers to guide consumers through the complexities of health insurance marketplace. Consequently, robust enforcement is crucial to ensure brokers act ethically and legally, protecting consumers from fraud and misleading practices. While precise details of enforcement actions aren’t always publicly available due to privacy concerns, several significant cases highlight the consequences of non-compliance.
The following case studies illustrate the range of violations, penalties, and outcomes in ACA broker enforcement.
Case Study 1: Misrepresentation of Plan Benefits
This case involved a broker who consistently misrepresented the benefits and coverage details of several ACA plans to prospective clients. The broker exaggerated the coverage provided by certain plans, omitted crucial information about deductibles and out-of-pocket costs, and falsely claimed that plans offered specific services not actually included in the policy. This led to several consumers enrolling in plans unsuitable for their needs, resulting in unexpected and substantial medical expenses.
The penalties imposed included a significant fine, a suspension of their broker license, and a mandatory retraining program focused on ethical sales practices and accurate plan representation. The outcome was a strong deterrent to similar deceptive practices within the brokerage community.
- Violation: Misrepresentation of plan benefits and omission of material facts.
- Penalties: Substantial fine, license suspension, mandatory retraining.
- Outcome: Deterrent to future deceptive practices, highlighting the importance of accurate information.
Case Study 2: Unauthorized Enrollment and Fee Collection
In this instance, a broker was found to have enrolled consumers in ACA plans without their explicit consent. Furthermore, the broker collected fees from consumers for services they did not provide, such as assistance with completing the enrollment application. This case involved multiple victims, and the investigation revealed a pattern of fraudulent activity. The penalties involved a hefty fine, revocation of their broker license, and referral to law enforcement for potential criminal charges.
The Biden administration’s tightening of ACA broker enforcement rules is a complex issue, impacting healthcare access for many. It’s a reminder that navigating the complexities of healthcare can be challenging, much like managing conditions like Tourette Syndrome in children. For helpful resources on effective strategies, check out this informative guide on strategies to manage Tourette syndrome in children , which offers valuable insights.
Understanding these challenges helps us advocate for better, more accessible healthcare policies, like improved ACA enforcement.
The broker was also ordered to reimburse all affected consumers for the unauthorized fees.
- Violation: Unauthorized enrollment and fraudulent fee collection.
- Penalties: Significant fine, license revocation, referral to law enforcement, consumer reimbursement.
- Outcome: Illustrates the severe consequences of unauthorized actions and emphasizes the need for transparent fee structures.
Case Study 3: Failure to Comply with Certification Requirements
This case involved a broker who failed to maintain the necessary certifications and training required to operate legally as an ACA broker. This broker neglected to renew their certification, rendering their activities unlawful. Although no direct consumer harm was demonstrated in this specific instance, the violation of regulatory requirements still resulted in penalties. The penalties included a fine and a period of probation during which the broker was required to successfully complete all necessary certifications and training before resuming operations.
This case underscores the importance of ongoing compliance with regulatory standards.
- Violation: Failure to maintain required certifications and training.
- Penalties: Fine, probationary period with required certification completion.
- Outcome: Highlights the importance of ongoing compliance with regulatory standards and the consequences of non-compliance.
Last Point
Navigating the complexities of ACA broker enforcement under the Biden administration requires careful attention to detail. The changes implemented by the CMS are far-reaching, impacting brokers’ operations, financial stability, and ultimately, the consumer experience. By understanding the new rules, brokers can adapt their practices to ensure compliance and maintain their business viability. Consumers, meanwhile, gain a stronger understanding of their rights and protections within the ACA marketplace.
Staying informed is key in this ever-evolving landscape.
Top FAQs
What are the most common violations committed by ACA brokers?
Common violations include misrepresenting plan benefits, engaging in deceptive sales practices, and failing to comply with disclosure requirements.
How can consumers report suspected ACA broker misconduct?
Consumers can usually file complaints with the CMS or their state insurance department.
What resources are available to help ACA brokers understand the new rules?
The CMS website provides guidance documents, FAQs, and other resources to assist brokers in complying with the regulations. Professional organizations also often offer training and support.
What types of technology can improve ACA broker enforcement?
Data analytics, AI-driven fraud detection, and improved online reporting systems can enhance enforcement efforts.