AI in Healthcare A Strategic Response to Todays Challenges and Tomorrows
Ai in healthcare a strategic response to todays challenges and tomorrows – AI in Healthcare: A Strategic Response to Today’s Challenges and Tomorrow’s – that’s a pretty big statement, right? But it’s true. We’re on the cusp of a revolution in how we diagnose, treat, and manage healthcare, all thanks to the incredible advancements in artificial intelligence. This isn’t just about futuristic gadgets; it’s about using AI to solve real, pressing problems – from streamlining hospital workflows to developing life-saving drugs faster than ever before.
Think faster diagnoses, personalized treatments, and a healthcare system that’s more efficient and accessible for everyone.
This post dives deep into the exciting world of AI in healthcare, exploring its transformative potential across various aspects of the medical field. We’ll look at how AI is enhancing diagnostics, revolutionizing personalized medicine, accelerating drug discovery, and even reshaping the healthcare workforce. But we’ll also tackle the ethical considerations and challenges that come with this rapidly evolving technology.
It’s a complex landscape, but one brimming with opportunities to improve lives.
AI’s Role in Enhancing Diagnostics
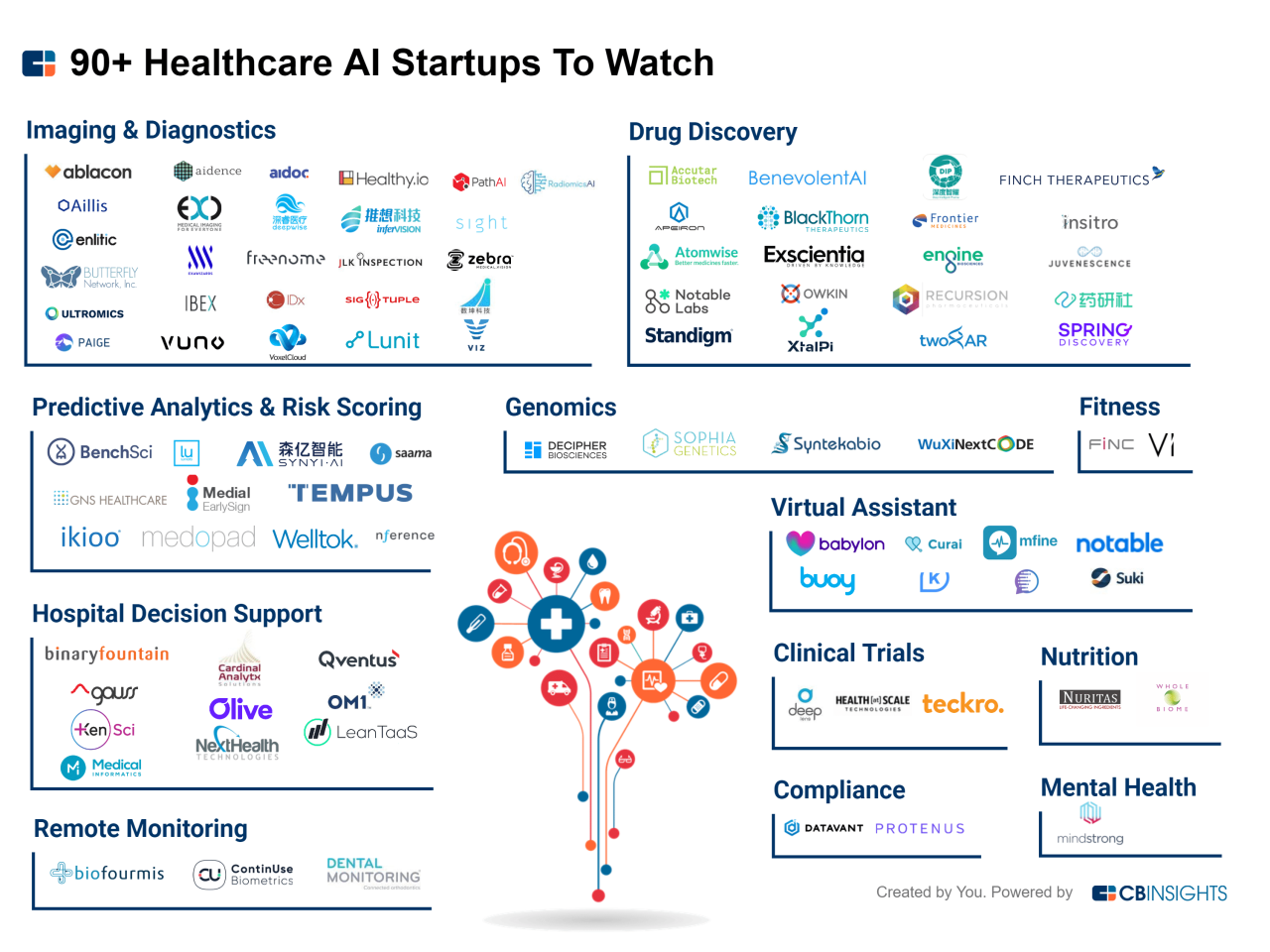
Source: cbinsights.com
The integration of artificial intelligence (AI) into healthcare diagnostics is revolutionizing the way we detect and diagnose diseases. AI-powered tools are significantly impacting both the accuracy and speed of diagnosis, leading to improved patient outcomes and more efficient healthcare systems. This increased efficiency translates to faster treatment initiation, reduced healthcare costs, and ultimately, improved patient survival rates in many cases.AI algorithms are transforming diagnostic procedures across various medical specialties.
The ability to analyze vast amounts of data rapidly and identify subtle patterns invisible to the human eye is a game-changer, especially in areas like radiology and pathology where image interpretation is critical.
AI Algorithms in Medical Image Analysis
AI algorithms are proving invaluable in analyzing medical images, leading to faster and more accurate diagnoses. These algorithms leverage machine learning techniques, particularly deep learning, to identify patterns and features in images that might be missed by human observers. For example, in radiology, AI can detect subtle abnormalities in X-rays, CT scans, and MRIs, aiding in the early detection of cancers, fractures, and other conditions.
In pathology, AI can assist in analyzing microscopic images of tissue samples, helping to identify cancerous cells and other abnormalities.
| Algorithm Name | Application Area | Accuracy Improvement Percentage | Limitations |
|---|---|---|---|
| Convolutional Neural Networks (CNNs) | Radiology (image classification, object detection), Pathology (tissue classification) | Varying, but studies show improvements ranging from 5-20% depending on the specific application and dataset. | Data bias, need for large labeled datasets, potential for overfitting, lack of explainability in some cases. |
| Recurrent Neural Networks (RNNs) | Time-series analysis of medical data (e.g., ECG interpretation) | Improvements vary widely depending on the specific application, but can significantly improve detection of arrhythmias. | Computational complexity, difficulty in handling long sequences, sensitivity to noise in the data. |
| Generative Adversarial Networks (GANs) | Image enhancement, data augmentation | Indirect improvement through improved training data quality; leading to better accuracy in downstream tasks. | Training instability, difficulty in controlling the generated images, potential for generating unrealistic images. |
| Support Vector Machines (SVMs) | Image classification, particularly useful in simpler image analysis tasks. | Improvements are task-specific but generally offer a robust and interpretable alternative to deep learning models. | Performance can be sensitive to the choice of kernel function, computationally expensive for very large datasets. |
Ethical Considerations in AI-Driven Diagnostics
The increasing reliance on AI in diagnostic decision-making raises several crucial ethical considerations. One major concern is algorithmic bias. If the training data used to develop AI algorithms reflects existing biases in healthcare, the algorithms may perpetuate or even amplify these biases, leading to disparities in diagnosis and treatment across different patient populations. For example, an algorithm trained primarily on data from one demographic group might perform poorly on data from another group.
Another important consideration is the transparency and explainability of AI algorithms. It is crucial that clinicians understand how an AI system arrives at its diagnosis, allowing them to assess the reliability and validity of the AI’s recommendations. The responsibility for final diagnostic decisions remains with the healthcare professional, but it is essential that they have confidence in the AI tools they are using.
Finally, issues of data privacy and security must be addressed to ensure the responsible use of patient data in the development and deployment of AI diagnostic tools. Robust safeguards are necessary to protect patient information and maintain confidentiality.
AI-Driven Personalized Medicine: Ai In Healthcare A Strategic Response To Todays Challenges And Tomorrows
The potential of artificial intelligence (AI) to revolutionize healthcare is immense, and nowhere is this more evident than in the field of personalized medicine. By analyzing vast amounts of patient data – including genomics, medical history, lifestyle factors, and even environmental influences – AI algorithms can create highly tailored treatment plans, maximizing effectiveness and minimizing side effects. This shift from a “one-size-fits-all” approach to a truly individualized strategy promises to significantly improve patient outcomes and enhance the overall quality of care.AI’s ability to sift through complex datasets and identify subtle patterns invisible to the human eye allows for the development of predictive models that can anticipate individual responses to different therapies.
This proactive approach enables clinicians to make more informed decisions, optimize treatment strategies, and potentially avoid unnecessary interventions. This precision medicine paradigm is particularly transformative in areas like oncology and cardiology, where individual variations in disease progression and treatment response are significant.
AI Applications in Personalized Oncology and Cardiology
The integration of AI in personalized medicine is already yielding impressive results across various specialties. The following examples highlight the transformative potential of this technology.AI is proving invaluable in cancer treatment. By analyzing a patient’s tumor genetics, medical history, and lifestyle, AI algorithms can predict the likelihood of treatment success with different therapies, helping oncologists select the most effective course of action.
Similarly, AI can monitor treatment response in real-time, adjusting the therapy as needed to optimize outcomes and minimize adverse effects. For example, AI-powered tools are now being used to predict the risk of recurrence after surgery, allowing for more targeted surveillance and early intervention.
- Improved Cancer Treatment Selection: AI algorithms analyze genomic data to predict the effectiveness of various chemotherapy regimens, leading to better treatment outcomes and reduced side effects.
- Real-time Treatment Monitoring: AI systems track patient responses to treatment, allowing for adjustments to the therapy based on individual needs.
- Predictive Modeling for Recurrence: AI models analyze patient data to predict the risk of cancer recurrence, enabling proactive monitoring and early intervention.
In cardiology, AI is being used to personalize risk assessments, predict heart attacks, and optimize treatment strategies for heart failure. For instance, AI can analyze electrocardiograms (ECGs) and other cardiac data to detect subtle abnormalities that might indicate an impending heart attack, allowing for timely intervention. AI also helps personalize treatment plans for heart failure by considering factors such as the patient’s age, lifestyle, and genetics, resulting in more effective and safer management of the condition.
- Early Detection of Heart Attacks: AI algorithms analyze ECG data to identify subtle patterns indicative of an impending heart attack, allowing for timely intervention.
- Personalized Risk Assessment: AI models incorporate various patient data points to provide a more accurate assessment of individual cardiovascular risk.
- Optimized Treatment for Heart Failure: AI helps personalize treatment strategies for heart failure, considering individual patient characteristics to maximize effectiveness and minimize adverse events.
Data Privacy and Security in Personalized Medicine
The widespread adoption of AI in personalized medicine presents significant challenges in data privacy and security. The use of sensitive patient data, including genomic information and medical history, requires robust security measures to prevent unauthorized access and breaches. Moreover, the ethical implications of using this data must be carefully considered, with stringent regulations and safeguards in place to protect patient confidentiality and autonomy.
Robust data anonymization techniques, secure data storage, and strict adherence to data privacy regulations like HIPAA are crucial for maintaining trust and ensuring responsible use of patient data. The potential for bias in AI algorithms trained on imbalanced datasets also needs to be addressed to ensure equitable access to personalized medicine. This requires careful consideration of data representation and algorithm design to mitigate potential disparities in care.
AI for Drug Discovery and Development
The pharmaceutical industry faces immense challenges: lengthy development times, high failure rates, and escalating costs. AI offers a powerful toolkit to address these hurdles, dramatically accelerating the drug discovery and development process. By leveraging its ability to analyze massive datasets and identify patterns invisible to the human eye, AI is revolutionizing how we approach the creation of new therapies.AI accelerates drug discovery primarily through its ability to sift through and interpret vast amounts of data.
This data includes genomic information, clinical trial results, chemical structures, and biological pathways – all crucial pieces of the puzzle in understanding disease mechanisms and identifying potential drug candidates. Traditional methods rely heavily on manual analysis and educated guesses, a process that is both time-consuming and often inefficient. AI algorithms, however, can process this data far more rapidly and comprehensively, uncovering hidden correlations and predicting the efficacy and safety of potential drugs with greater accuracy.
Comparison of Traditional and AI-Assisted Drug Development
The table below illustrates the key differences between traditional drug development methods and those enhanced by AI.
| Traditional Method | AI-Assisted Method |
|---|---|
| Relies heavily on hypothesis-driven research, often involving years of experimentation and trial-and-error. | Utilizes machine learning algorithms to analyze vast datasets, identifying promising drug candidates and predicting their efficacy and safety more efficiently. |
| Target identification and validation are time-consuming and often involve significant costs. | AI can rapidly analyze genomic data and identify potential drug targets with higher precision, significantly reducing time and cost. |
| Lead optimization is a lengthy and iterative process. | AI can simulate and predict the properties of various drug molecules, accelerating the optimization process and reducing the number of experiments needed. |
| Clinical trial design and patient selection can be challenging, leading to delays and increased costs. | AI can analyze patient data to identify ideal candidates for clinical trials, improving trial efficiency and reducing the risk of failure. |
Potential Risks and Limitations of AI in Drug Development
While AI offers significant advantages, it’s crucial to acknowledge its limitations and potential risks. One major concern is the reliance on high-quality data. AI algorithms are only as good as the data they are trained on; biased or incomplete datasets can lead to inaccurate predictions and flawed conclusions. Another challenge is the “black box” nature of some AI algorithms – their decision-making processes can be opaque, making it difficult to understand why a particular prediction was made.
This lack of transparency can hinder the validation and acceptance of AI-driven drug development strategies. Furthermore, the regulatory landscape surrounding AI in drug development is still evolving, presenting challenges for obtaining approvals and ensuring the safety and efficacy of AI-developed drugs. Finally, the high computational costs associated with training and deploying complex AI models can be a barrier for smaller pharmaceutical companies.
Addressing these challenges requires a multi-faceted approach involving robust data quality control, explainable AI techniques, and clear regulatory guidelines.
AI in Healthcare Operations and Management
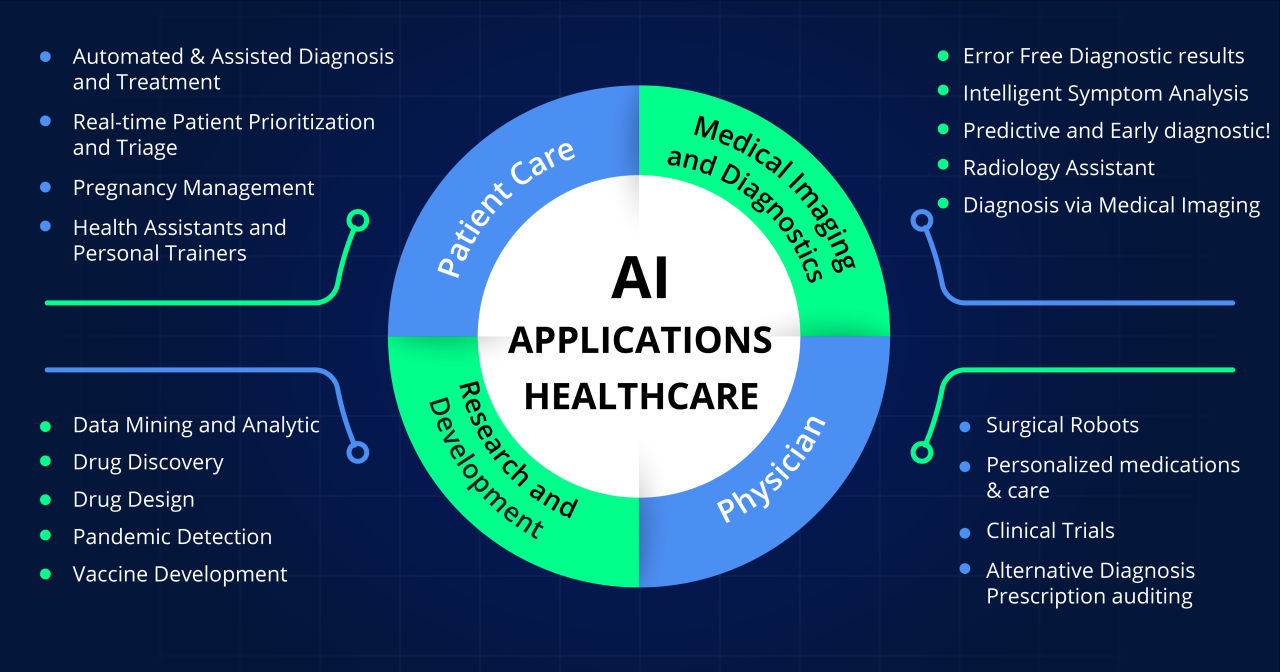
Source: techment.com
The healthcare industry is ripe for disruption, and artificial intelligence (AI) is poised to revolutionize its operational efficiency. From streamlining administrative tasks to optimizing resource allocation, AI offers significant potential for improving patient care while simultaneously reducing costs. This section explores how AI is transforming hospital workflows and management, focusing on specific applications and demonstrating its impact on overall operational efficiency.AI’s application in hospital operations aims to reduce inefficiencies and improve resource utilization, ultimately leading to better patient outcomes and cost savings.
By automating repetitive tasks, predicting resource needs, and providing data-driven insights, AI empowers healthcare professionals to focus on what matters most: patient care. This shift towards intelligent automation frees up valuable time and resources, allowing for more efficient and effective healthcare delivery.
AI-Driven Optimization of Hospital Workflows, Ai in healthcare a strategic response to todays challenges and tomorrows
AI algorithms can analyze vast amounts of data – patient demographics, appointment schedules, staffing levels, equipment utilization – to identify bottlenecks and inefficiencies in hospital workflows. For instance, AI can predict patient arrival times, optimize appointment scheduling to minimize wait times, and even predict potential staffing shortages, allowing for proactive adjustments. This predictive capability allows hospitals to better manage resources and avoid costly overstaffing or understaffing scenarios.
For example, a hospital in Boston implemented an AI-powered system that reduced patient wait times by 20% and improved staff scheduling efficiency by 15%.
Specific Applications of AI in Hospital Administration
The implementation of AI in hospital administration is multifaceted, offering solutions to various operational challenges. A key area is improving patient flow and resource management.
- Patient Scheduling: AI algorithms can analyze patient needs and physician availability to create optimized schedules, minimizing wait times and maximizing appointment slots. This can lead to increased patient satisfaction and improved operational efficiency.
- Bed Management: AI can predict patient discharge times and anticipate bed availability, optimizing bed allocation and reducing the risk of bed shortages. This intelligent approach minimizes patient delays and improves hospital throughput.
- Supply Chain Management: AI can analyze consumption patterns to predict and optimize the ordering of medical supplies, reducing waste and ensuring timely availability of essential resources. This prevents shortages and minimizes disruptions to patient care.
- Staffing Optimization: AI can forecast staffing needs based on patient volume and predicted demand, ensuring optimal staffing levels and reducing the costs associated with overstaffing or understaffing. This also contributes to improved employee satisfaction and reduced burnout.
The Potential of AI to Improve Operational Efficiency and Reduce Healthcare Costs
The integration of AI in healthcare operations promises substantial improvements in efficiency and cost reduction. By automating tasks, optimizing resource allocation, and providing predictive insights, AI can significantly reduce administrative overhead, improve resource utilization, and ultimately, lower healthcare costs.
Effective implementation of AI in hospital operations can lead to a measurable reduction in operational costs, ranging from 10% to 25%, depending on the specific applications and scale of implementation.
For example, a large hospital system in California reported a 15% reduction in administrative costs and a 10% improvement in bed utilization after implementing an AI-powered bed management system. These results demonstrate the significant potential of AI to transform healthcare operations and deliver substantial cost savings while simultaneously enhancing the quality of patient care.
AI and the Future of Healthcare Workforce
The integration of artificial intelligence (AI) into healthcare is rapidly transforming the roles and responsibilities of healthcare professionals. While concerns about job displacement exist, a more accurate perspective highlights AI’s potential to augment human capabilities, leading to improved efficiency, accuracy, and patient care. This shift necessitates a focus on adapting the healthcare workforce to leverage AI’s strengths and address potential challenges.AI’s impact on the healthcare workforce will be multifaceted, influencing everything from clinical practice to administrative tasks.
Instead of replacing human professionals, AI will increasingly act as a powerful tool, allowing healthcare providers to focus on tasks requiring human empathy, critical thinking, and complex decision-making. This collaborative approach, where AI handles repetitive or data-heavy tasks, will ultimately enhance the overall quality and accessibility of healthcare.
AI Augmenting Human Capabilities in Healthcare Delivery
AI algorithms can analyze vast amounts of patient data—medical history, imaging results, genetic information—far faster and more comprehensively than any human. This capability leads to improved diagnostics. For example, AI-powered diagnostic tools can detect subtle patterns in medical images, such as early signs of cancer, that might be missed by the human eye. This allows for earlier interventions and better patient outcomes.
Furthermore, AI can assist in personalized treatment planning by analyzing individual patient data to predict treatment response and identify potential side effects, leading to more effective and safer therapies. In surgery, robotic surgery systems guided by AI can enhance precision and minimize invasiveness, improving recovery times and reducing complications.
AI Reshaping the Healthcare Workforce in the Next Decade: A Scenario
Imagine a 2033 healthcare setting. A general practitioner uses AI-powered diagnostic tools to analyze a patient’s symptoms and medical history, receiving immediate insights and suggested diagnostic tests. The AI system flags a potential risk factor missed in the initial examination. The GP, empowered by this information, conducts a more targeted examination and orders additional tests, ultimately leading to an earlier and more accurate diagnosis.
Meanwhile, administrative tasks such as scheduling appointments, managing medical records, and processing insurance claims are largely automated by AI, freeing up administrative staff to focus on patient interaction and support. Specialized nurses work alongside AI-powered robots in assisting with patient care, particularly in tasks requiring precision or repetitive movements. AI-driven predictive analytics identifies patients at high risk of readmission, allowing proactive interventions to improve their outcomes and reduce healthcare costs.
The overall healthcare system is more efficient, patient-centered, and delivers higher-quality care thanks to the strategic integration of AI. This scenario, while fictional, is built on current technological advancements and projected trends in AI development and healthcare needs. The roles of healthcare professionals will evolve, demanding new skills in interpreting AI-generated insights and working collaboratively with intelligent systems. The focus will shift towards human-AI partnerships, enhancing the skills and expertise of the existing workforce.
Addressing Ethical and Societal Concerns
The integration of artificial intelligence (AI) into healthcare offers transformative potential, but its implementation necessitates careful consideration of ethical and societal implications. Failure to address these concerns proactively could lead to unintended consequences, undermining public trust and hindering the widespread adoption of beneficial AI technologies. This section explores key ethical challenges and proposes strategies for responsible AI development and deployment in healthcare.AI algorithms, while powerful, are not immune to biases present in the data they are trained on.
These biases can perpetuate and even amplify existing health disparities, leading to inaccurate diagnoses, inappropriate treatments, and unequal access to care. For example, an algorithm trained primarily on data from a specific demographic group may perform poorly when applied to patients from other groups, potentially resulting in misdiagnosis or delayed treatment.
Bias in AI Algorithms and Mitigation Strategies
Addressing bias requires a multi-faceted approach starting with data collection. Diverse and representative datasets are crucial for training unbiased algorithms. This means actively seeking data from a wide range of populations, including those often underrepresented in medical research. Furthermore, algorithmic transparency allows for the identification and correction of biases. Techniques like explainable AI (XAI) can help uncover how an algorithm arrives at its conclusions, making it possible to detect and rectify discriminatory patterns.
Regular audits and independent evaluations of AI systems are also vital to ensure ongoing fairness and accuracy. Finally, the involvement of diverse stakeholders, including patients, clinicians, and ethicists, in the design and implementation phases of AI systems can help prevent biases from entering the system in the first place. For instance, a team developing an AI for diagnosing skin cancer should include dermatologists with experience treating diverse skin tones to ensure the algorithm accurately identifies lesions across different skin types.
Transparency and Explainability in AI-Driven Healthcare
Transparency and explainability are paramount for building trust and ensuring accountability in AI-driven healthcare. When an AI system makes a critical decision affecting a patient’s health, clinicians and patients need to understand the reasoning behind that decision. Black-box algorithms, where the decision-making process is opaque, are unacceptable in healthcare settings. Explainable AI (XAI) techniques aim to make the decision-making process of AI systems more transparent, allowing clinicians to scrutinize the algorithm’s logic and identify potential errors or biases.
This transparency is not only essential for clinical decision-making but also for building patient trust and fostering informed consent. For example, if an AI system recommends a specific treatment, clinicians should be able to understand the factors that influenced the recommendation and explain this to the patient, facilitating shared decision-making.
Regulatory and Legal Frameworks for AI in Healthcare
The rapid advancement of AI in healthcare necessitates the development of robust regulatory and legal frameworks to ensure safety, efficacy, and ethical use. These frameworks should address issues such as data privacy, algorithm bias, liability for AI-related errors, and the ethical implications of using AI in sensitive areas like diagnosis and treatment. Existing regulations, such as HIPAA in the United States, provide a foundation, but they need to be updated and expanded to specifically address the unique challenges posed by AI.
International collaboration is also crucial to establish consistent standards and prevent regulatory fragmentation. The development of clear guidelines on data governance, algorithm validation, and clinical oversight will be vital to ensure the responsible and beneficial use of AI in healthcare. These guidelines should balance the need for innovation with the imperative to protect patient safety and rights.
For example, clear guidelines on how to handle AI-related medical errors and establish liability would be crucial for fostering responsible innovation.
Illustrative Case Studies

Source: cryptopolitan.com
AI’s impact on healthcare is best understood through real-world examples demonstrating its ability to improve patient outcomes and revolutionize healthcare delivery. These case studies highlight the transformative potential of AI, showcasing its effectiveness across various medical domains.The following sections detail a specific case study where AI significantly improved patient outcomes and provide a visual representation of AI’s impact on a key healthcare metric.
Finally, a compelling narrative illustrates AI’s transformative power in healthcare.
AI in healthcare offers a powerful response to rising costs and staffing shortages, but ensuring equitable access remains crucial. The recent FTC lawsuit against the Novant Health and Community Health Systems merger, as reported by this article , highlights the complexities of healthcare consolidation. This underscores the need for AI solutions that are not only innovative but also accessible and prevent monopolies that could stifle competition and innovation in the field of AI-driven healthcare.
AI-Enhanced Diabetic Retinopathy Detection
This case study focuses on the application of AI in detecting diabetic retinopathy (DR), a leading cause of blindness in people with diabetes. The problem was the significant shortage of ophthalmologists, particularly in underserved areas, leading to delayed diagnosis and treatment of DR. Many patients with diabetes lacked access to timely eye exams, resulting in preventable vision loss.
AI in healthcare is revolutionizing how we approach diseases, offering faster diagnoses and personalized treatments. The recent news about Monali Thakur being hospitalized after struggling to breathe, as reported in this article monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases , highlights the urgent need for proactive healthcare solutions. Early detection and prevention, areas where AI excels, are key to combating such illnesses and improving overall health outcomes, making it a strategic response to today’s challenges and tomorrow’s needs.
The solution involved developing an AI-powered system trained on a vast dataset of retinal images. This system could automatically analyze retinal scans, identifying signs of DR with accuracy comparable to human ophthalmologists. The results were dramatic. Studies showed a significant reduction in the time taken to diagnose DR, allowing for earlier intervention and improved patient outcomes. In one study, the AI system correctly identified DR in over 95% of cases, significantly reducing the number of patients experiencing vision loss.
The system also improved access to care, as it could be deployed in remote clinics with limited access to specialists.
Visual Representation: Reduction in DR-Related Blindness
Imagine a bar graph. The x-axis represents years (e.g., 2018, 2019, 2020, 2021). The y-axis represents the number of new cases of blindness due to diabetic retinopathy. The bars for 2018 and 2019 show a relatively high number of new cases. Starting in 2020, however, there’s a sharp decline in the height of the bars, reflecting the introduction and widespread adoption of the AI-powered DR detection system.
AI in healthcare is revolutionizing how we approach medical challenges, from diagnostics to personalized treatments. The advancements are incredible, impacting even reproductive health decisions, like those faced by Karishma Mehta, who recently chose to freeze her eggs – you can read more about her experience and the associated risks in this article: karishma mehta gets her eggs frozen know risks associated with egg freezing.
This highlights how AI’s potential extends to informing crucial life choices, ultimately contributing to a healthier future for all.
The graph visually demonstrates a significant reduction in new cases of DR-related blindness following the implementation of the AI system, illustrating its direct positive impact on patient outcomes. The difference in bar height between pre- and post-AI implementation clearly shows the impact.
Transformative Narrative: The Case of Sarah
Sarah, a 62-year-old diabetic living in a rural community, previously faced significant challenges accessing timely eye care. Due to the shortage of ophthalmologists in her area, her annual eye exams were often delayed, increasing her risk of vision loss from undiagnosed diabetic retinopathy. However, with the introduction of the AI-powered system, her local clinic now offers automated retinal scans.
Her latest exam utilized this technology. The AI system quickly analyzed her retinal images, identifying early signs of DR. This early detection allowed for prompt treatment, preventing further vision loss. Sarah’s story represents thousands of patients who have benefited from the accessibility and efficiency of AI in healthcare, showcasing how technology can bridge the gap in access to quality care and dramatically improve patient lives.
This is a testament to the transformative potential of AI to address critical healthcare challenges.
Final Wrap-Up
The integration of AI in healthcare isn’t just a technological advancement; it’s a fundamental shift in how we approach patient care. From improving diagnostic accuracy to personalizing treatment plans and accelerating drug discovery, AI offers a powerful toolkit to address some of healthcare’s most pressing challenges. While ethical considerations and potential biases need careful attention, the transformative potential is undeniable.
The future of healthcare is undeniably intertwined with AI, promising a future where care is more precise, efficient, and accessible to all. Let’s embrace this exciting journey responsibly and thoughtfully, ensuring that AI benefits everyone.
FAQ Section
What are the biggest risks associated with using AI in healthcare?
The biggest risks include algorithmic bias leading to unfair or inaccurate diagnoses/treatments, data privacy breaches, and the potential for job displacement in the healthcare workforce. Ensuring transparency, accountability, and robust regulatory frameworks is crucial to mitigate these risks.
How will AI impact my doctor’s role?
AI will likely augment, not replace, doctors. AI tools can handle tasks like analyzing medical images and identifying patterns, freeing up doctors to focus on patient interaction, complex decision-making, and providing personalized care.
Is my health data safe if it’s used by AI systems?
Data security and privacy are paramount. Strong regulations and robust security measures are essential to protect patient data used in AI systems. Choosing providers with strong data protection policies is crucial.
Will AI make healthcare more expensive?
While initial investment in AI technology can be significant, the long-term goal is to increase efficiency and reduce costs. AI can optimize resource allocation, reduce errors, and improve outcomes, potentially leading to cost savings in the long run.