Are Antidepressant Withdrawal Symptoms Serious? Expert Tells All
Are antidepressant withdrawal symptoms serious expert tells – Are antidepressant withdrawal symptoms serious? Expert tells all. Stopping antidepressants can be tricky, and understanding the potential for withdrawal is crucial. This isn’t just about feeling a bit off; we’re talking about a range of symptoms, from mild discomfort to serious complications, depending on the individual, the medication, and how it’s stopped. We’ll explore the severity of these symptoms, common experiences, and what you can do to navigate this process safely and effectively.
This post dives deep into the realities of antidepressant withdrawal, offering insights from medical professionals and real-life experiences. We’ll cover everything from recognizing the signs of mild, moderate, and severe withdrawal to understanding the risk factors and available medical management options. We’ll also discuss the importance of tapering off medications gradually and the vital role of communication with your healthcare provider.
Severity of Antidepressant Withdrawal Symptoms
Antidepressant withdrawal is a real and sometimes challenging experience for individuals discontinuing these medications. The severity of symptoms varies greatly from person to person, making it crucial to understand the factors involved and the potential range of outcomes. While some experience minimal discomfort, others face significant challenges that can impact their daily lives.
The intensity of withdrawal symptoms is influenced by several interconnected factors. The type of antidepressant plays a significant role, with shorter-acting medications like paroxetine (Paxil) often associated with more intense and abrupt withdrawal compared to longer-acting medications like fluoxetine (Prozac). The dosage taken, the duration of treatment, and the speed of tapering also contribute significantly. Higher doses, longer treatment durations, and abrupt cessation are all associated with a greater likelihood of more severe symptoms.
Finally, individual factors such as age, overall health, and pre-existing conditions can also influence the withdrawal experience. Some individuals are simply more sensitive to medication changes than others.
Antidepressant Withdrawal Symptom Severity
The symptoms experienced during antidepressant withdrawal can range from mild to severe. It’s important to remember that not everyone will experience all of these symptoms, and the intensity will vary greatly. Understanding the spectrum of possibilities allows for better preparation and management.
| Symptom | Mild Description | Moderate Description | Severe Description |
|---|---|---|---|
| Flu-like symptoms | Mild headache, slight nausea, fatigue | Moderate headache, nausea with vomiting, significant fatigue affecting daily activities | Severe headache, persistent vomiting, debilitating fatigue requiring bed rest |
| Mood changes | Irritability, mild anxiety, slight sadness | Increased irritability, significant anxiety, noticeable sadness and tearfulness | Severe anxiety attacks, intense depression with suicidal ideation, significant emotional lability |
| Sleep disturbances | Difficulty falling asleep, slightly disrupted sleep | Insomnia, vivid dreams, significant difficulty sleeping through the night | Severe insomnia, nightmares, significant daytime sleepiness despite nighttime sleeplessness |
| Sensory disturbances | Mild dizziness, slight tingling sensations | Dizziness impacting balance, noticeable electric shock-like sensations | Severe dizziness causing falls, intense electric shock-like sensations, visual disturbances |
| Gastrointestinal issues | Mild stomach upset | Nausea, diarrhea, or constipation | Severe diarrhea or constipation, significant abdominal pain |
Common Antidepressant Withdrawal Symptoms
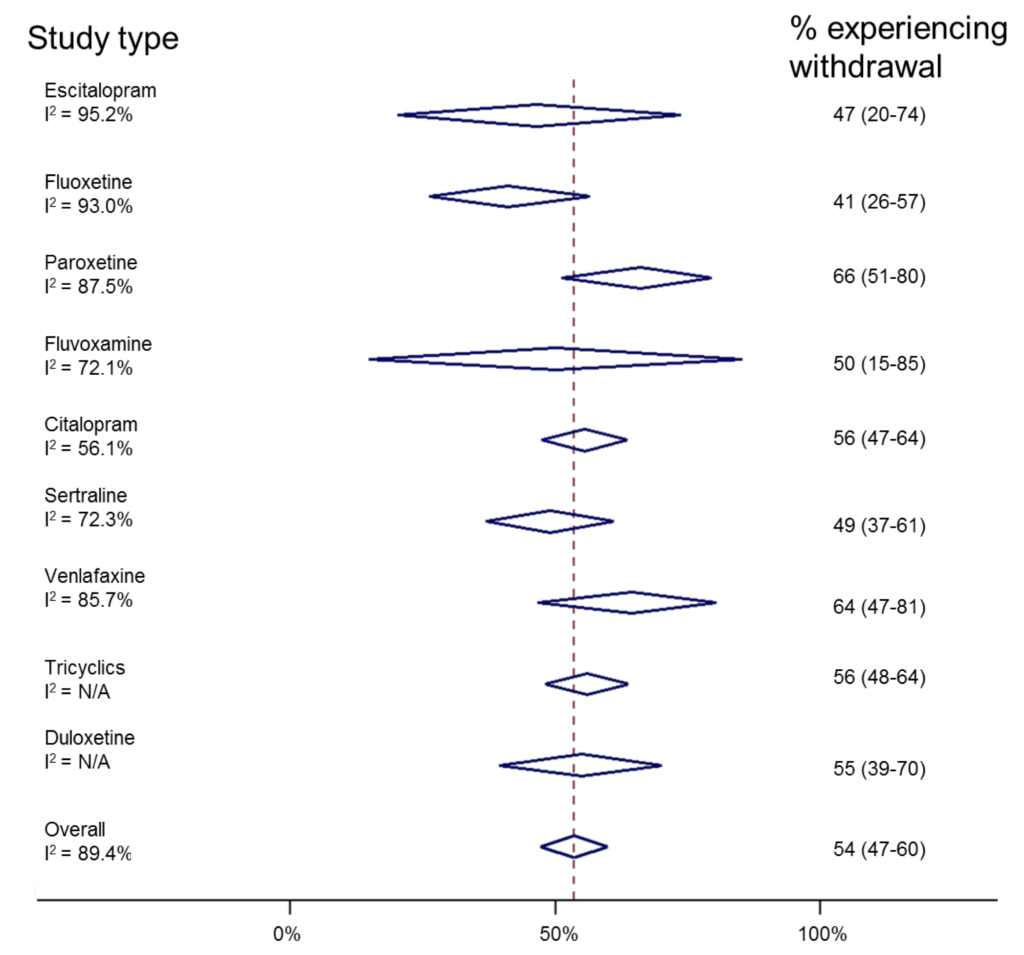
Source: nationalelfservice.net
Discontinuing antidepressants, even gradually, can trigger a range of withdrawal symptoms. The severity and type of symptoms vary depending on several factors, including the specific antidepressant, the dosage, the duration of treatment, and individual patient sensitivity. Understanding these common symptoms is crucial for both patients and healthcare providers to manage the discontinuation process effectively and minimize discomfort.
Withdrawal symptoms are thought to arise from the brain’s attempt to readjust to the absence of the antidepressant. The abrupt cessation of medication disrupts the delicate balance of neurotransmitters, leading to a cascade of physiological changes that manifest as various withdrawal symptoms. These symptoms are not simply a sign of underlying depression returning, but rather a direct consequence of the medication’s withdrawal.
It’s vital to remember that experiencing withdrawal symptoms does not indicate failure of treatment or a need to restart the medication immediately. Rather, a careful and gradual tapering-off strategy is generally recommended.
Withdrawal Symptoms by Antidepressant Class
The most frequently reported withdrawal symptoms differ slightly depending on the class of antidepressant. While overlapping symptoms exist, some are more characteristic of certain classes. Proper identification helps in managing expectations and tailoring a suitable discontinuation plan.
So, are antidepressant withdrawal symptoms serious? An expert tells us they can be, and managing them requires careful planning. It’s fascinating to consider this alongside other medical breakthroughs, like the recent news that the fda approves clinical trials for pig kidney transplants in humans , showcasing how medical science pushes boundaries. Understanding the complexities of both mental and physical health is crucial, and responsible tapering off antidepressants is as important as finding a suitable kidney transplant.
Here’s a breakdown of common withdrawal symptoms categorized by antidepressant class:
- SSRIs (Selective Serotonin Reuptake Inhibitors): These include fluoxetine (Prozac), sertraline (Zoloft), paroxetine (Paxil), citalopram (Celexa), and escitalopram (Lexapro). Common withdrawal symptoms include flu-like symptoms (headache, nausea, fatigue), dizziness, anxiety, irritability, insomnia, vivid dreams, sensory disturbances (electric shock sensations), and emotional lability (rapid shifts in mood).
- SNRIs (Serotonin-Norepinephrine Reuptake Inhibitors): Venlafaxine (Effexor) and duloxetine (Cymbalta) are examples. Withdrawal symptoms are similar to SSRIs but may include more pronounced anxiety, increased blood pressure, and potentially more intense flu-like symptoms.
- TCAs (Tricyclic Antidepressants): Amitriptyline (Elavil) and nortriptyline (Pamelor) are examples. Withdrawal symptoms can be more severe and include anxiety, insomnia, vivid dreams, nightmares, nausea, vomiting, and even cardiovascular effects. These require a very gradual tapering schedule under close medical supervision.
- MAOIs (Monoamine Oxidase Inhibitors): These are less commonly prescribed now. Withdrawal symptoms can be significant and include flu-like symptoms, anxiety, and potentially severe cardiovascular effects. Discontinuation must be managed very carefully under a doctor’s guidance.
Typical Withdrawal Timelines
The duration of withdrawal symptoms varies significantly depending on several factors, most importantly the half-life of the medication and the duration of treatment. Shorter half-life medications (like paroxetine) often lead to more intense but shorter-lived withdrawal symptoms, while longer half-life medications (like fluoxetine) may cause milder but more protracted symptoms. The length of treatment also plays a role; longer treatment durations often correlate with more prolonged withdrawal.
Generally, withdrawal symptoms can start within days of stopping or reducing the dose, peaking within 1-2 weeks, and gradually subsiding over several weeks or months. However, some individuals may experience symptoms for significantly longer periods.
Physiological Mechanisms Underlying Withdrawal Symptoms
The precise mechanisms responsible for antidepressant withdrawal are complex and not fully understood. However, the leading hypothesis centers on the disruption of neurotransmitter systems in the brain. Antidepressants primarily affect serotonin and norepinephrine levels. When these medications are abruptly stopped, the brain’s attempt to re-establish its neurochemical balance can lead to various symptoms. For example, the sudden drop in serotonin levels might contribute to anxiety, insomnia, and mood disturbances.
Similarly, changes in norepinephrine levels might manifest as cardiovascular symptoms. The process is further complicated by the brain’s plasticity and its ability to adapt to the presence and absence of these medications over time. This adaptation, while beneficial during treatment, can lead to withdrawal symptoms when the medication is discontinued.
Risk Factors for Severe Withdrawal: Are Antidepressant Withdrawal Symptoms Serious Expert Tells
Antidepressant withdrawal can range from mild discomfort to severe symptoms, significantly impacting a person’s quality of life. Understanding the factors that increase the risk of severe withdrawal is crucial for both patients and healthcare professionals in developing safe and effective discontinuation strategies. Several individual characteristics and pre-existing conditions can contribute to a more challenging withdrawal experience.The severity of antidepressant withdrawal isn’t solely determined by the type of antidepressant or the length of treatment.
Individual factors play a significant role. For example, a person’s genetic predisposition, their overall health, and even their coping mechanisms can influence how their body reacts to the cessation of medication. Understanding these factors allows for a more personalized approach to tapering and managing withdrawal symptoms.
Individual Characteristics Influencing Withdrawal Severity
Several individual characteristics can heighten the risk of severe antidepressant withdrawal. These include factors such as the patient’s age, the presence of other mental health conditions, and their overall sensitivity to medication changes. Rapid tapering, or stopping the medication abruptly, significantly increases the risk of severe symptoms regardless of other factors. People with a history of substance abuse may also be at increased risk due to potential overlapping withdrawal mechanisms.
Furthermore, individuals with a history of severe or recurrent depressive episodes may experience more intense withdrawal symptoms. Finally, personal factors such as stress levels and overall health can also impact the severity of withdrawal.
Pre-existing Medical Conditions and Withdrawal Severity
Pre-existing medical conditions can significantly interact with antidepressant withdrawal, increasing the likelihood of severe symptoms. For instance, individuals with cardiovascular conditions may experience heightened risk due to the potential impact of withdrawal on heart rate and blood pressure. Similarly, those with pre-existing anxiety disorders or other mood disorders might find their symptoms exacerbated during withdrawal. Underlying neurological conditions can also complicate the withdrawal process, leading to a more severe experience.
It’s vital for healthcare professionals to carefully consider a patient’s complete medical history when planning an antidepressant discontinuation strategy.
So, are antidepressant withdrawal symptoms serious? An expert tells us they can be, and managing them carefully is crucial. It’s fascinating to consider that early detection of other neurological issues is also key, like with dementia – I recently read an interesting article on how an eye test might help, check it out: can eye test detect dementia risk in older adults.
Understanding early warning signs for various health conditions, including mental health and neurological decline, is essential for proactive care. This highlights the importance of both careful medication management and regular health checkups.
Strategies for Minimizing the Risk of Severe Withdrawal
Careful planning and a gradual reduction in dosage are paramount in minimizing the risk of severe withdrawal. This process, often referred to as tapering, should be guided by a healthcare professional and tailored to the individual’s needs and response to the medication. It’s crucial to emphasize the importance of open communication between the patient and their doctor. This includes reporting any symptoms, however mild, to allow for timely adjustments to the tapering schedule.
- Gradual Tapering: Slow and steady reduction of the dosage, guided by a healthcare professional, is the cornerstone of safe withdrawal.
- Close Monitoring: Regular check-ups with the doctor to monitor symptoms and adjust the tapering schedule as needed.
- Addressing Co-occurring Conditions: Managing any pre-existing mental or physical health conditions before and during the tapering process.
- Lifestyle Adjustments: Implementing stress-reduction techniques, such as regular exercise, mindfulness, and sufficient sleep, can help mitigate withdrawal symptoms.
- Support System: Having a strong support network of family, friends, or support groups can provide emotional and practical assistance.
Medical Management of Withdrawal
Antidepressant withdrawal can be a challenging experience, but thankfully, there are several medical approaches to manage the symptoms and make the process smoother. Healthcare professionals utilize a combination of strategies tailored to the individual’s specific needs and the severity of their withdrawal symptoms. The key is a gradual and carefully planned reduction of the antidepressant dosage, combined with supportive therapies when necessary.Successfully navigating antidepressant withdrawal hinges on a collaborative approach between the patient and their healthcare provider.
Open communication about symptoms and any concerns is crucial.
Tapering Off Antidepressants
The cornerstone of managing antidepressant withdrawal is a gradual tapering of the medication. This process involves slowly reducing the dosage over weeks or even months, depending on the individual’s medication, dosage, and the duration of treatment. A rapid reduction can significantly increase the risk of severe withdrawal symptoms. The tapering schedule is personalized and carefully monitored by the healthcare professional.
They may adjust the schedule based on the patient’s response, ensuring a balance between minimizing withdrawal symptoms and achieving a successful discontinuation of the medication. For example, a patient on a high dose of an SSRI might start by reducing their dose by a small percentage every few weeks, gradually decreasing until they reach zero. The pace of tapering is not a one-size-fits-all approach and requires regular monitoring and adjustments.
Pharmacological and Therapeutic Interventions
Various medications and therapies can help alleviate withdrawal symptoms. These interventions are often used in conjunction with the tapering process to provide additional support and reduce discomfort.
| Treatment | Mechanism of Action | Benefits | Potential Side Effects |
|---|---|---|---|
| Low-dose Antidepressant (same class or different) | Provides continued neurotransmitter support, mitigating abrupt changes. | Reduces intensity and duration of withdrawal symptoms. Can be gradually reduced alongside the original medication. | Similar to original antidepressant, but usually milder due to lower dosage. |
| Benzodiazepines (e.g., Lorazepam) | Reduces anxiety and promotes relaxation. | Helps manage anxiety, insomnia, and other distressing symptoms. | Sedation, dizziness, cognitive impairment, dependence with prolonged use. |
| Anticonvulsants (e.g., Gabapentin) | Modulates neurotransmitter activity, potentially reducing nerve pain and anxiety. | May alleviate some neurological symptoms associated with withdrawal. | Drowsiness, dizziness, fatigue, nausea. |
| Cognitive Behavioral Therapy (CBT) | Helps individuals identify and manage negative thought patterns and coping mechanisms. | Improves emotional regulation and stress management, potentially reducing the impact of withdrawal symptoms. | Requires commitment to therapy sessions. May initially unearth difficult emotions. |
Seeking Professional Help

Source: co.uk
Discontinuing antidepressant medication without proper medical supervision can be risky, potentially leading to uncomfortable and sometimes dangerous withdrawal symptoms. It’s crucial to remember that your mental health is paramount, and a collaborative approach with your healthcare provider is the safest and most effective way to manage any transition in your medication regimen. Ignoring professional guidance could unnecessarily prolong discomfort and potentially jeopardize your overall well-being.The importance of consulting a healthcare professional before even considering stopping antidepressant medication cannot be overstated.
Your doctor is best equipped to assess your individual situation, considering factors like the type of antidepressant, dosage, duration of treatment, and your overall health. They can help you develop a tapering schedule that minimizes the risk of withdrawal symptoms, and monitor you for any complications. Attempting to stop abruptly or without guidance can significantly increase the severity and duration of withdrawal, making the process far more challenging.
A carefully planned reduction, under professional supervision, is the key to a smoother transition.
Steps to Take During Severe Withdrawal Symptoms, Are antidepressant withdrawal symptoms serious expert tells
A structured approach is vital when dealing with severe antidepressant withdrawal. The following flowchart Artikels the recommended steps:
Flowchart: Managing Severe Antidepressant Withdrawal Symptoms
Step 1: Identify Severe Symptoms
– Are you experiencing intense symptoms such as significant anxiety, insomnia, nausea, dizziness, or other debilitating effects? If yes, proceed to Step 2.
Step 2: Contact Your Doctor Immediately
-Call your prescribing physician or seek immediate medical attention at your nearest urgent care or emergency room. Do not attempt to manage severe symptoms alone.
Step 3: Follow Medical Advice
-Your doctor will assess your symptoms and may recommend adjustments to your medication regimen, supportive therapies, or other interventions. Strictly adhere to their recommendations.
Step 4: Monitor Symptoms and Report Changes
– Keep a detailed record of your symptoms, including their intensity and duration. Regularly update your doctor on any changes in your condition.
Step 5: Consider Support Systems
-Lean on your support network (family, friends, support groups) for emotional and practical assistance during this challenging time.
Communicating with Healthcare Providers about Withdrawal Concerns
Open and honest communication with your healthcare provider is essential for effective management of antidepressant withdrawal. Be prepared to provide a detailed history of your medication use, including the type of antidepressant, dosage, duration of treatment, and any previous attempts to discontinue the medication. Clearly describe your symptoms, including their onset, severity, and duration. Don’t hesitate to express your concerns and ask questions.
So, are antidepressant withdrawal symptoms serious? An expert tells us they can be, and careful tapering is crucial. Managing complex conditions in children, like the challenges detailed in this helpful article on strategies to manage Tourette syndrome in children , highlights the importance of a gradual approach to medication changes. This mindful strategy mirrors the need for careful antidepressant withdrawal to minimize potential adverse effects.
Keeping a journal of your symptoms can be incredibly helpful in providing your doctor with accurate and detailed information. Remember, your doctor is there to help you navigate this process safely and effectively. Bringing a family member or friend to appointments can also provide additional support and ensure that important information is not overlooked. Finally, be proactive in advocating for your own health and well-being; don’t be afraid to seek a second opinion if you have concerns about your treatment plan.
Patient Experiences and Perspectives
Antidepressant withdrawal can significantly impact daily life, causing distress and disruption for many individuals. Understanding these personal experiences is crucial for providing effective support and managing the challenges involved. The following sections explore the lived realities of those navigating this difficult process.
It’s important to remember that everyone’s experience with antidepressant withdrawal is unique, influenced by factors such as the type and dosage of medication, duration of treatment, individual sensitivity, and pre-existing conditions. There’s no one-size-fits-all experience, and what one person finds manageable, another might find debilitating.
Case Studies Illustrating the Impact of Antidepressant Withdrawal on Daily Life
Let’s consider two hypothetical cases to illustrate the varied challenges faced during antidepressant withdrawal. Sarah, a 35-year-old teacher, experienced intense flu-like symptoms, including nausea, dizziness, and brain zaps, after gradually reducing her antidepressant dose. These symptoms made it impossible for her to concentrate at work, impacting her teaching ability and leading to increased stress and anxiety. Her social life suffered as she lacked the energy and mental clarity to engage with friends and family.
Conversely, Mark, a 40-year-old accountant, experienced primarily emotional symptoms such as intense irritability, insomnia, and feelings of hopelessness. His withdrawal was less physically debilitating but equally disruptive, affecting his ability to maintain his professional responsibilities and leading to conflict with his colleagues and family members.
Potential Psychological and Social Consequences of Severe Withdrawal Symptoms
Severe antidepressant withdrawal can have profound psychological and social consequences. Understanding these potential impacts helps healthcare professionals and support networks to anticipate and address the challenges faced by individuals undergoing withdrawal.
- Increased anxiety and depression: Withdrawal symptoms can exacerbate pre-existing mental health conditions or trigger new ones.
- Impaired cognitive function: Difficulty concentrating, remembering things, and making decisions can significantly impact daily life and work performance.
- Irritability and mood swings: These can strain relationships with family, friends, and colleagues.
- Social isolation: The debilitating nature of withdrawal symptoms can lead to withdrawal from social activities and support networks.
- Relationship difficulties: Changes in mood and behavior can put a strain on personal relationships.
- Occupational impairment: Difficulty concentrating and managing emotions can negatively impact work performance and job security.
- Increased risk of self-harm or suicidal ideation: In severe cases, withdrawal symptoms can increase the risk of self-harm or suicidal thoughts, highlighting the need for close monitoring and support.
The Importance of Patient Support and Resources During Withdrawal
Having access to adequate support and resources is crucial for navigating the challenges of antidepressant withdrawal. A supportive environment can significantly improve outcomes and reduce the negative impact on daily life.
This support can come from various sources, including mental health professionals, support groups, family, and friends. Access to reliable information about withdrawal symptoms and management strategies is also essential. Open communication with healthcare providers is vital for adjusting medication tapering schedules and addressing any emerging concerns. Support groups offer a safe space for individuals to share their experiences, reducing feelings of isolation and providing practical coping strategies.
Finally, exploring complementary therapies like mindfulness or relaxation techniques can help manage some of the psychological distress associated with withdrawal.
Long-Term Effects of Withdrawal
Antidepressant withdrawal can be a challenging experience, and many individuals understandably worry about the potential for long-term consequences. While acute withdrawal symptoms are well-documented, the long-term effects are less clearly defined and often depend on factors like the type of antidepressant, the dosage, the duration of treatment, and individual patient characteristics. It’s crucial to understand that research in this area is ongoing, and more studies are needed to fully elucidate the long-term impact.The potential long-term effects of antidepressant withdrawal can manifest both mentally and physically.
Some individuals report persistent fatigue, sleep disturbances, cognitive difficulties (such as problems with concentration and memory), and emotional lability (meaning significant mood swings). These symptoms can significantly impact quality of life and daily functioning. The severity and duration of these lingering effects vary widely. It’s important to note that some individuals experience a complete resolution of symptoms within a relatively short period, while others may experience persistent challenges for months or even longer.
Comparison of Long-Term Effects of Withdrawal and Continued Use
Understanding the potential long-term effects of antidepressant withdrawal requires comparing them to the potential long-term effects of continued antidepressant use. Continued use of antidepressants can also have potential long-term consequences, such as weight gain, sexual dysfunction, and an increased risk of certain medical conditions. Furthermore, long-term dependence on medication can sometimes hinder the development of natural coping mechanisms for managing mental health challenges.
The optimal course of action—whether to continue medication, gradually reduce dosage, or explore alternative therapies—is a complex decision that should always be made in close consultation with a healthcare professional, considering the individual’s specific circumstances and risk factors. There’s no one-size-fits-all answer. The decision must carefully weigh the potential long-term risks and benefits of both withdrawal and continued medication use.
Resources for Ongoing Support
Navigating prolonged antidepressant withdrawal can be isolating and overwhelming. Fortunately, several resources offer ongoing support and guidance. Support groups, either in-person or online, provide a safe space to connect with others who understand the challenges of withdrawal. These groups can offer invaluable emotional support, practical advice, and a sense of community. Additionally, many mental health professionals specialize in managing antidepressant withdrawal and can provide tailored guidance and support throughout the process.
These professionals can help individuals develop coping strategies, monitor symptoms, and make informed decisions about their treatment. Reputable online resources, such as those provided by national mental health organizations, can offer evidence-based information, support forums, and links to local services. Remember, seeking professional help is crucial, and there are many resources available to assist individuals in navigating this challenging period.
Wrap-Up
Navigating antidepressant withdrawal requires careful planning and a strong support system. Remember, it’s not a one-size-fits-all situation. What works for one person might not work for another. The key takeaway is proactive communication with your doctor, a gradual tapering-off process, and a willingness to seek additional support if needed. Don’t hesitate to reach out for help—your well-being is paramount.
Understanding the potential challenges and resources available empowers you to make informed decisions and manage this transition as smoothly as possible.
Question & Answer Hub
What if I experience withdrawal symptoms after stopping my medication?
Contact your doctor immediately. They can help assess the severity of your symptoms and recommend appropriate management strategies.
How long do antidepressant withdrawal symptoms typically last?
This varies greatly depending on the medication, dosage, and individual factors. Symptoms can range from a few days to several weeks or even months in some cases.
Are there any natural remedies that can help with antidepressant withdrawal?
While some natural remedies might offer mild relief for certain symptoms, they shouldn’t replace medical advice. Always discuss any complementary therapies with your doctor before trying them.
Can I stop taking antidepressants cold turkey?
Generally, no. Stopping antidepressants abruptly significantly increases the risk of experiencing severe withdrawal symptoms. Always consult your doctor for a safe tapering schedule.