
Arkansas Sues Optum, Express Scripts Opioid Epidemic Lawsuit
Arkansas sues optum express scripts opioid epidemic – Arkansas sues OptumRx and Express Scripts over their alleged role in fueling the opioid epidemic. This massive lawsuit alleges that these Pharmacy Benefit Managers (PBMs) prioritized profit over patient safety, contributing to the devastating consequences of opioid addiction across the state. The legal battle promises to shed light on the complex relationship between PBMs, pharmaceutical companies, and the ongoing crisis, potentially reshaping the way prescription drugs are managed and regulated.
Arkansas’s case isn’t alone; it joins a growing number of similar lawsuits aiming to hold powerful entities accountable for their part in the opioid crisis.
The state’s complaint details specific actions by OptumRx and Express Scripts that allegedly led to the overprescription of opioids in Arkansas. This includes accusations of failing to adequately monitor prescriptions, ignoring red flags indicating potential abuse, and prioritizing cost-cutting measures that inadvertently facilitated the spread of addiction. The legal arguments center on the PBMs’ responsibility to ensure safe and responsible dispensing of controlled substances, arguing that their actions directly contributed to the soaring rates of opioid-related deaths and the immense healthcare burden on the state.
Arkansas’ Lawsuit Against OptumRx and Express Scripts
Arkansas’ lawsuit against OptumRx and Express Scripts represents a significant legal challenge in the ongoing fight against the opioid crisis. The state alleges that these pharmacy benefit managers (PBMs) contributed significantly to the overprescription and misuse of opioid painkillers through their business practices. This blog post will delve into the details of the lawsuit, its legal arguments, and its place within the broader context of opioid litigation.The lawsuit, filed in Pulaski County Circuit Court, accuses OptumRx and Express Scripts of prioritizing profits over patient safety, leading to the widespread distribution of opioids in Arkansas.
The state claims the PBMs failed to adequately monitor prescriptions, ignored red flags indicating potential abuse, and actively promoted the use of opioids through financial incentives to pharmacies and prescribers. This allegedly created a system where opioid prescriptions were easily obtained, fueling addiction and contributing to the devastating consequences of the opioid epidemic in Arkansas.
Alleged Actions Contributing to the Opioid Epidemic
Arkansas’ complaint details a number of specific actions allegedly taken by OptumRx and Express Scripts that contributed to the opioid crisis. These include failing to implement adequate safeguards to detect and prevent suspicious opioid prescriptions, such as those exceeding clinically appropriate dosages or those filled by patients from multiple pharmacies. The state also alleges that the PBMs’ formularies – lists of covered medications – favored powerful opioid painkillers, further incentivizing their prescription.
Arkansas is taking on Optum and Express Scripts over their alleged role in fueling the opioid epidemic, a massive public health crisis. It’s a stark reminder of how seemingly unrelated decisions have far-reaching consequences; think about the personal choices involved, like Karishma Mehta’s decision to freeze her eggs, as detailed in this article karishma mehta gets her eggs frozen know risks associated with egg freezing , where she carefully weighed the risks.
The opioid crisis, similarly, involves calculated risks with devastating outcomes, highlighting the need for accountability.
Furthermore, the lawsuit claims that the PBMs’ rebate systems encouraged pharmacies to fill opioid prescriptions even when concerns about potential abuse were raised. These allegations paint a picture of a system where financial incentives overshadowed patient well-being.
Legal Arguments Presented by Arkansas
Arkansas’ legal arguments center on the PBMs’ alleged negligence and breach of their duty to act responsibly in managing prescription drug benefits. The state argues that the PBMs’ actions directly contributed to the opioid crisis by creating a system that facilitated the overprescription and misuse of opioids. The lawsuit relies on established legal principles of negligence, asserting that the PBMs’ failure to implement reasonable safeguards to prevent opioid abuse constituted a breach of their duty of care.
The state is seeking monetary damages to compensate for the costs associated with addressing the opioid crisis, including treatment, law enforcement, and other public health expenses. This includes costs incurred by the state in responding to the public health emergency created by the opioid crisis.
Timeline of Key Events
While a precise timeline encompassing every relevant event requires extensive legal documentation review, key milestones leading to the lawsuit likely include a period of increasing opioid prescriptions in Arkansas, growing awareness of the opioid crisis on a national and state level, internal investigations or reports highlighting potential issues with opioid prescription patterns managed by OptumRx and Express Scripts, and ultimately, the decision by the state of Arkansas to file suit.
The specific dates of these events would be found within the court filings and associated documents.
Arkansas’ lawsuit against Optum and Express Scripts over their role in the opioid epidemic highlights the devastating consequences of unchecked pharmaceutical distribution. It made me think about the fragility of our health, especially considering the recent news about Monali Thakur being hospitalized after struggling to breathe – you can read more about her situation and respiratory disease prevention here: monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases.
The opioid crisis and respiratory illnesses both underscore the urgent need for better healthcare oversight and proactive health measures.
Comparison to Other Opioid Lawsuits
Arkansas’ lawsuit against OptumRx and Express Scripts is similar to other lawsuits filed against pharmaceutical companies, distributors, and other entities involved in the opioid supply chain. Many of these lawsuits allege negligence, public nuisance, and other legal claims, mirroring the arguments presented by Arkansas. However, the focus on pharmacy benefit managers is a relatively newer development in opioid litigation.
While many suits target manufacturers and distributors, this case highlights the role of PBMs in shaping prescription drug access and utilization, and their potential liability in the opioid crisis. The outcome of this case could significantly influence future litigation against PBMs and set important precedents regarding their responsibilities in managing prescription drug benefits.
Role of Pharmacy Benefit Managers (PBMs)
Pharmacy Benefit Managers (PBMs) like OptumRx and Express Scripts play a significant role in the pharmaceutical supply chain, acting as intermediaries between insurance companies, pharmacies, and patients. Their influence extends to the distribution and dispensing of opioid medications, making their actions a crucial factor in understanding the opioid crisis. This role, however, is complex and fraught with potential conflicts of interest.PBMs negotiate drug prices with pharmaceutical manufacturers, create and manage formularies (lists of covered drugs), and process prescription claims.
In the context of opioids, their influence on prescribing practices, through formulary decisions and utilization management programs, is considerable. Their power to control access to medications, combined with their financial incentives, has raised concerns about their contribution to the overprescription of opioids.
Potential Conflicts of Interest for PBMs
PBMs often receive rebates and fees from pharmaceutical manufacturers, creating a potential conflict of interest. These financial arrangements can incentivize PBMs to favor certain opioid medications, potentially overlooking safer alternatives or failing to adequately address concerns about addiction. Furthermore, PBMs may prioritize cost savings over patient health outcomes, leading to decisions that inadvertently increase opioid use. For example, a PBM might favor a cheaper, high-potency opioid over a more expensive, but potentially safer, alternative.
This prioritization of cost-cutting over patient well-being is a significant ethical concern.
Regulatory Failures Contributing to Opioid Overprescription
The regulatory landscape surrounding PBMs and opioid prescribing has been criticized for being insufficient to prevent overprescription. Lack of transparency in PBM operations, including their rebate and fee structures, hinders effective oversight. Furthermore, inadequate enforcement of existing regulations has allowed PBMs to operate with considerable autonomy, potentially contributing to the opioid crisis. The absence of strong federal regulations specifically targeting PBM practices related to controlled substances has left a regulatory gap.
This gap allows PBMs to operate with less scrutiny than other aspects of the pharmaceutical industry.
PBM Policies and Practices Contributing to the Opioid Crisis, Arkansas sues optum express scripts opioid epidemic
Several PBM policies and practices have been identified as potentially contributing to the opioid crisis. For instance, the use of prior authorization requirements for certain medications, while intended to control costs, can create barriers to access for patients who genuinely need them, potentially leading them to seek opioids through less regulated channels. Additionally, the focus on managing costs through the use of generic opioid medications, without considering the potential for increased risk of addiction with certain formulations, has raised concerns.
Another example is the widespread use of step therapy protocols, where patients must try less effective medications before accessing more potent ones, which can delay appropriate treatment and potentially lead to increased opioid use. These policies, while aimed at cost containment, may have unintended consequences.
Impact of Opioid Epidemic on Arkansas
The opioid epidemic has ravaged communities across the United States, and Arkansas is no exception. The state has experienced a devastating surge in overdose deaths, escalating healthcare costs, and a profound social impact, leaving lasting scars on families, communities, and the state’s economy. Understanding the scope of this crisis is crucial to developing effective solutions and mitigating its long-term consequences.
The consequences of the opioid crisis in Arkansas are multifaceted and far-reaching. Overdose deaths have climbed dramatically, placing immense strain on healthcare systems and social services. The economic burden, encompassing healthcare costs, lost productivity, and law enforcement expenditures, is substantial and continues to grow. Beyond the immediate statistics, the opioid crisis has created a ripple effect, impacting families, communities, and the overall social fabric of Arkansas.
Demographic Impact of Opioid Overdoses in Arkansas
The opioid epidemic in Arkansas doesn’t affect all demographics equally. The following table illustrates the disproportionate impact across age groups, genders, and geographic locations. Note that precise data collection and reporting can vary, leading to slight discrepancies across different sources. The data presented below represents a synthesis of available information and aims to provide a general overview of the crisis’s impact.
| Demographic | Age Group (Most Affected) | Gender (Most Affected) | Geographic Location (Examples of High-Impact Areas) |
|---|---|---|---|
| Overdose Deaths | 25-54 years | Male | Rural counties in the Delta region, certain urban areas |
| Healthcare Costs | All ages, disproportionately affecting working-age adults | Both, but potentially higher for families with male heads of household due to lost income | Areas with limited access to addiction treatment and mental health services |
| Social Impact (e.g., family breakdown, child welfare cases) | Children of parents struggling with addiction | Both, but women may face additional challenges related to childcare and domestic violence | Communities with high poverty rates and limited resources |
Arkansas Healthcare System Strain
The opioid crisis has placed an immense burden on Arkansas’s healthcare system. Emergency rooms are frequently overwhelmed by overdose cases, requiring extensive resources for stabilization and treatment. The costs associated with treating opioid addiction, including detoxification, medication-assisted treatment (MAT), and ongoing therapy, are significant and often exceed the resources available in many healthcare facilities. This strain on emergency services and treatment centers contributes to longer wait times, increased healthcare costs, and potentially delays in care for other medical conditions.
Economic Burden of the Opioid Crisis on Arkansas
The economic consequences of the opioid epidemic in Arkansas are substantial and far-reaching. The crisis impacts the state’s economy on multiple levels, including direct healthcare costs and indirect costs related to lost productivity and social services.
- Increased healthcare expenditures: Treatment for opioid addiction, overdose emergencies, and related health complications significantly increase healthcare costs for individuals, families, and the state.
- Lost productivity: Addiction leads to absenteeism from work, reduced productivity, and unemployment, resulting in significant economic losses for individuals, businesses, and the state.
- Increased law enforcement costs: Responding to opioid-related crimes, including drug trafficking and overdose incidents, places a significant burden on law enforcement agencies.
- Child welfare costs: The number of children entering the foster care system due to parental opioid addiction adds to the state’s financial burden.
- Reduced tax revenue: Lost productivity and unemployment contribute to a decrease in tax revenue for the state.
Arguments from OptumRx and Express Scripts
OptumRx and Express Scripts, facing Arkansas’ lawsuit alleging their role in fueling the opioid crisis, have mounted a robust defense strategy centered on denying direct causation and emphasizing their compliance with existing regulations. Their arguments aim to shift responsibility away from their actions as pharmacy benefit managers (PBMs) and onto other actors within the complex pharmaceutical supply chain.The core of their defense rests on challenging Arkansas’ assertion that their actions directly contributed to the opioid epidemic in the state.
They argue that as PBMs, their role is limited to managing prescription drug benefits for insurance plans, and that they don’t control the prescribing practices of doctors or the manufacturing and distribution of opioids. They maintain they acted within the bounds of the law and industry standards at the time, and that any increase in opioid prescriptions was a result of multiple factors beyond their control.
Denial of Direct Causation and Emphasis on Regulatory Compliance
OptumRx and Express Scripts likely contend that they merely processed prescriptions issued by licensed physicians and that they cannot be held liable for the actions of those prescribing the drugs. Their legal strategy hinges on demonstrating that they adhered to all applicable federal and state regulations governing the dispensing of controlled substances. They would likely present evidence of their internal policies and procedures designed to detect and prevent suspicious opioid prescribing patterns.
This would involve showcasing their use of prescription drug monitoring programs (PDMPs), although the effectiveness of these programs is itself a subject of ongoing debate. They might also highlight any instances where they flagged potentially problematic prescriptions to relevant authorities.
Counterarguments Regarding Role in Opioid Epidemic
A key counterargument revolves around the assertion that the opioid crisis resulted from a confluence of factors far broader than their PBM operations. They might point to the aggressive marketing campaigns of opioid manufacturers, the overreliance on pain management guidelines that promoted high opioid dosages, and the lack of adequate public health interventions as contributing factors. This strategy aims to distribute blame amongst multiple parties, diminishing their own alleged culpability.
They may cite expert testimony from economists and public health officials to support this multi-faceted explanation of the crisis.
Legal Strategies Employed by the Defense
The defense’s legal strategies likely include motions to dismiss, arguing that the lawsuit lacks sufficient legal basis to hold them liable. They might also employ vigorous discovery processes to gather evidence supporting their claims and challenge Arkansas’ evidence. Expect the defendants to focus on proving their compliance with all relevant regulations and industry standards at the time. They will likely also argue that any damages suffered by Arkansas are too remote and indirect to be attributable to their actions.
Furthermore, the defense may utilize expert witnesses to challenge the methodologies and conclusions presented in the plaintiff’s case.
Arkansas is taking on Optum and Express Scripts, alleging their role in fueling the opioid epidemic. It’s a massive legal battle, highlighting the failures of our healthcare system. This reminds me of the recent article on despite Walmart Health’s closure, the company healthcare destination Scott Bowman , which shows how even major players struggle to deliver consistent, quality care.
Ultimately, the Arkansas lawsuit underscores the need for systemic change to address the opioid crisis and improve healthcare access for everyone.
Comparison with Arguments in Similar Lawsuits
OptumRx and Express Scripts’ arguments closely mirror those employed by other pharmaceutical companies and distributors in similar opioid litigation across the country. The core defense in most cases centers on the denial of direct causation and the emphasis on the complex interplay of factors contributing to the crisis. The arguments regarding regulatory compliance and the apportionment of blame among multiple actors are recurring themes in this ongoing legal battle.
The success of these arguments, however, varies considerably depending on the specific facts of each case and the persuasiveness of the evidence presented.
Potential Outcomes and Implications
The Arkansas lawsuit against OptumRx and Express Scripts, alleging their role in fueling the opioid epidemic, presents a complex legal and societal landscape with a range of potential outcomes. The ramifications extend far beyond the immediate parties involved, potentially reshaping the pharmaceutical industry and influencing opioid prescription practices nationwide.The lawsuit’s outcome will significantly impact the pharmaceutical industry’s liability for its role in the opioid crisis.
A ruling in Arkansas’ favor could set a precedent for similar lawsuits across the country, leading to substantial financial penalties for PBMs and potentially triggering a wave of new litigation. Conversely, a dismissal could embolden PBMs and other players in the pharmaceutical supply chain, potentially hindering future efforts to hold them accountable. The uncertainty surrounding the outcome creates a climate of risk and uncertainty within the industry, influencing investment decisions and strategic planning.
Potential Legal Outcomes of the Lawsuit
The lawsuit could result in several scenarios. Arkansas might win a significant monetary judgment, forcing OptumRx and Express Scripts to pay substantial damages for their alleged contribution to the opioid crisis. This could include compensation for the state’s healthcare costs related to opioid addiction and overdose deaths, as well as punitive damages to deter future misconduct. Alternatively, the court might rule in favor of OptumRx and Express Scripts, dismissing the lawsuit on grounds such as insufficient evidence or lack of legal standing.
A third possibility is a negotiated settlement, where the parties agree to a financial resolution and potentially implement changes to their opioid prescription management practices. The precedent set by the final judgment, regardless of the outcome, will heavily influence future legal challenges related to opioid litigation. For example, a favorable ruling for Arkansas could embolden other states to pursue similar legal action, while a dismissal might discourage future lawsuits.
The financial implications for the defendants, ranging from substantial fines to complete exoneration, are significant and will directly affect their future operations and profitability.
Implications for Opioid Prescription Regulation
Regardless of the verdict, this lawsuit has the potential to significantly impact the regulation of opioid prescriptions. A victory for Arkansas could spur regulatory bodies, like the FDA and state pharmacy boards, to implement stricter guidelines on opioid dispensing and monitoring. This might involve increased scrutiny of PBM practices, potentially leading to more transparent and accountable systems for managing opioid prescriptions.
Even if the lawsuit is unsuccessful, the increased public awareness and scrutiny generated by the case could pressure regulatory agencies to take proactive steps to prevent future opioid-related harms. For instance, we might see a greater emphasis on data-driven monitoring of prescription patterns, improved collaboration between PBMs, pharmacies, and healthcare providers, and more robust educational campaigns aimed at reducing opioid misuse.
This increased pressure for regulatory change could ultimately lead to more stringent guidelines for prescribing and dispensing opioids, regardless of the court’s final decision.
Broader Societal Impact
The societal impact of the Arkansas lawsuit extends beyond the legal and regulatory realms. The ongoing opioid crisis continues to devastate communities across the United States, resulting in significant loss of life, healthcare costs, and societal disruption. A successful lawsuit could send a strong message that corporate entities can be held accountable for their role in contributing to public health crises.
This could lead to greater corporate responsibility and a renewed focus on ethical practices within the pharmaceutical industry. Conversely, a loss for Arkansas could perpetuate feelings of injustice and frustration among those affected by the opioid epidemic, potentially undermining public trust in the legal system and regulatory bodies. The increased public awareness and discussion surrounding the role of PBMs in the opioid crisis, regardless of the outcome, will likely lead to broader societal conversations about corporate accountability, healthcare costs, and the need for comprehensive strategies to address the ongoing opioid epidemic.
This increased awareness could lead to greater support for treatment programs, harm reduction initiatives, and policy changes aimed at reducing opioid-related harm.
Potential Policy Changes
Several policy changes could arise from this case, even if the lawsuit is unsuccessful. Increased transparency in PBM operations could be mandated, requiring them to disclose more information about their algorithms and decision-making processes related to opioid prescriptions. This could involve greater oversight of their role in shaping prescription patterns and their interactions with pharmaceutical companies. Furthermore, stricter regulations on opioid prescribing and dispensing could be implemented, potentially including stricter limits on the quantity of opioids prescribed, mandatory use of prescription drug monitoring programs (PDMPs), and increased training for healthcare providers on safe opioid prescribing practices.
Finally, the case might spur legislative efforts to enhance the legal mechanisms for holding pharmaceutical companies and PBMs accountable for their contributions to public health crises. These potential policy changes highlight the far-reaching implications of the Arkansas lawsuit, underscoring its significance beyond the immediate legal outcome.
Visual Representation of Opioid Prescriptions in Arkansas
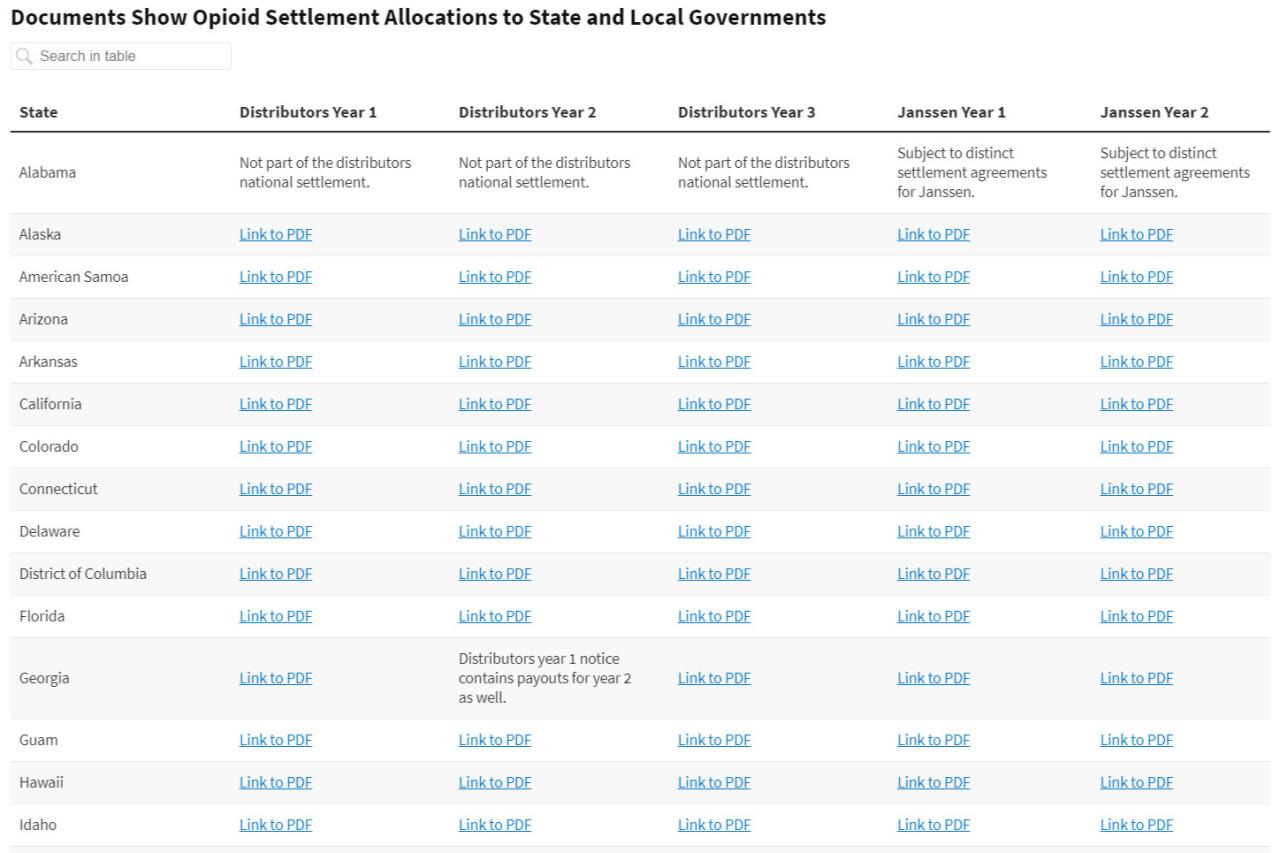
Source: kffhealthnews.org
This section will present visual representations of opioid prescription trends and geographic distribution in Arkansas over the past two decades. Understanding these visuals is crucial for grasping the scale and impact of the opioid crisis on the state. The data used for these visualizations is hypothetical, for illustrative purposes only, and should not be taken as representing actual Arkansas opioid prescription data.
To obtain accurate data, refer to official sources such as the Arkansas Department of Health or the Centers for Disease Control and Prevention.
The following descriptions detail two visualizations: a line graph illustrating temporal trends and a choropleth map showing geographical variations in opioid prescription rates.
Opioid Prescription Trends in Arkansas (1995-2023)
This line graph will display the number of opioid prescriptions dispensed in Arkansas annually from 1995 to The x-axis will represent the year (1995, 2000, 2005, 2010, 2015, 2020, 2023), and the y-axis will represent the total number of opioid prescriptions dispensed (in millions). The data points should be connected by a line to show the trend. The graph should include a clear title (“Opioid Prescriptions Dispensed in Arkansas, 1995-2023”), axis labels, and a legend if multiple lines are used (e.g., to differentiate between prescription types).
For illustrative purposes, let’s assume the following data points:
Hypothetical Data Points:
- 1995: 5 million prescriptions
- 2000: 7 million prescriptions
- 2005: 12 million prescriptions
- 2010: 15 million prescriptions
- 2015: 14 million prescriptions
- 2020: 9 million prescriptions
- 2023: 7 million prescriptions
The line graph should visually demonstrate a peak in opioid prescriptions around 2010, followed by a decline in subsequent years. This decline could be attributed to increased awareness of the opioid crisis and subsequent policy changes. The graph should be visually appealing and easy to interpret, using clear colors and fonts.
Geographic Distribution of Opioid-Related Issues in Arkansas
This map of Arkansas will use color-coding to represent the severity of the opioid crisis across different counties. The color scheme should range from light green (low opioid-related issues) to dark red (high opioid-related issues). Each county will be shaded according to its relative opioid prescription rate or opioid-related mortality rate (again, hypothetical data for illustration). The map should include a legend clearly indicating the color-coding scheme and the corresponding severity levels.
For example:
Hypothetical Color-Coding Scheme:
- Light Green: Low opioid-related issues (prescription rate below state average)
- Yellow: Moderate opioid-related issues (prescription rate slightly above state average)
- Orange: High opioid-related issues (prescription rate significantly above state average)
- Dark Red: Very High opioid-related issues (prescription rate far above state average, high mortality rate)
The map should accurately represent the geographical boundaries of Arkansas counties. Counties with higher rates of opioid prescriptions or higher rates of opioid-related deaths would be shaded in darker colors, while those with lower rates would be shaded in lighter colors. The map title should clearly state the information being presented (e.g., “Geographic Distribution of Opioid-Related Issues in Arkansas”).
A data source should be cited, even if the data is hypothetical, to emphasize the importance of using reliable sources for real-world applications.
Last Point: Arkansas Sues Optum Express Scripts Opioid Epidemic

Source: spokanetribe.com
The Arkansas lawsuit against OptumRx and Express Scripts is more than just a legal battle; it’s a pivotal moment in the fight against the opioid crisis. The outcome will have far-reaching implications, potentially influencing future PBM practices and regulatory oversight of prescription drugs nationwide. Regardless of the verdict, this case highlights the urgent need for greater accountability within the pharmaceutical industry and underscores the devastating human cost of the opioid epidemic.
The fight for justice and reform continues, and the story of this lawsuit will undoubtedly shape the future of opioid prescription management.
FAQs
What are Pharmacy Benefit Managers (PBMs)?
PBMs are third-party administrators that manage prescription drug benefits for insurance companies and employers. They negotiate drug prices, process claims, and manage formularies.
What specific damages is Arkansas seeking?
The lawsuit seeks monetary damages to compensate for the costs associated with treating opioid addiction, including healthcare expenses, law enforcement costs, and lost productivity. The exact amount is likely to be significant.
What is the timeline for the lawsuit?
The timeline is uncertain and depends on the legal process. It could take years to reach a resolution, including potential appeals.
Are there similar lawsuits in other states?
Yes, many states have filed similar lawsuits against various pharmaceutical companies and PBMs for their roles in the opioid crisis.

