
Northwell Nuvance Deal State AG Approval
Northwell Nuvance deal approval state attorneys general – it’s a headline that’s been making waves! This massive healthcare merger between Northwell Health and Nuvance Health is facing intense scrutiny from state attorneys general, raising serious questions about antitrust concerns and the potential impact on patients across the region. The deal’s complexity, involving billions of dollars and impacting countless individuals, makes it a fascinating – and potentially consequential – case study in modern healthcare economics and regulation.
The proposed merger promises potential benefits like increased efficiency and resource sharing. However, the significant market share consolidation has understandably sparked worries about higher costs, reduced competition, and diminished access to care for some communities. The state attorneys general are meticulously reviewing the deal, carefully weighing the potential advantages against the risks, and their decisions will significantly shape the future of healthcare in the affected areas.
We’ll explore the key arguments for and against the merger, the regulatory hurdles, and what the future might hold.
Deal Overview
The proposed merger between Northwell Health, New York’s largest health system, and Nuvance Health, a large Connecticut-based health system, represents a significant shift in the landscape of healthcare in the Northeast. This combination aims to create a powerful, integrated healthcare network spanning a wide geographic area, impacting patient access, provider networks, and overall healthcare delivery.The agreement, announced in late 2022, details a complex structure involving the integration of both systems’ hospitals, physician practices, and other healthcare services.
While the exact financial terms haven’t been publicly disclosed in full detail, the deal is expected to significantly increase the combined entity’s market share and influence. The merger is predicated on achieving substantial cost synergies and operational efficiencies, allowing for investment in advanced technologies and improved patient care. The deal’s structure likely includes provisions for governance, management responsibilities, and the distribution of ownership stakes, though these specifics remain largely confidential at this stage.
Deal Timeline
The merger process began with the initial announcement of the agreement between Northwell Health and Nuvance Health in late 2022. This was followed by a period of regulatory review and due diligence, a process that typically involves extensive scrutiny by state and federal authorities to ensure compliance with antitrust laws and other regulations. This period included public comment periods and the addressing of concerns raised by various stakeholders, including state attorneys general.
The deal’s progression has been marked by significant hurdles and negotiations. The current status reflects the successful navigation of these regulatory challenges, leading to the approval by state attorneys general, paving the way for the deal’s finalization. The timeline anticipates a final closing of the deal in the near future, though the exact date remains dependent on the completion of all remaining administrative procedures.
State Attorney General Involvement
The Northwell Health and Nuvance Health merger, while promising increased healthcare access and efficiency, has understandably drawn significant scrutiny from state attorneys general. Their involvement stems from the potential for anti-competitive practices that could negatively impact patients and the healthcare market. These concerns necessitate a thorough review process to ensure the merger doesn’t harm consumers through price increases, reduced service quality, or limited choices.The legal basis for their involvement primarily rests on antitrust laws, specifically those designed to prevent mergers that substantially lessen competition.
These laws aim to maintain a competitive marketplace where consumers benefit from a range of choices and reasonable prices. State attorneys general have a crucial role in enforcing these laws within their respective jurisdictions. The specific concerns raised, and the level of involvement, vary depending on the individual attorney general and the geographic market affected by the merger.
Attorney General Involvement and Specific Concerns
While the exact details of each state attorney general’s involvement may not be fully public due to ongoing investigations, it’s known that several states where Northwell and Nuvance operate have initiated reviews. These reviews are typically confidential until a decision is reached, but public statements and documents may be released if and when the investigations conclude. For instance, the New York Attorney General’s office, given Northwell’s significant presence in New York, is likely heavily involved, scrutinizing the potential impact on hospital pricing and service availability within the state.
Similarly, attorneys general in Connecticut and other states where Nuvance operates would be examining potential anti-competitive effects within their borders. Concerns may center on reduced competition leading to higher healthcare costs, limited access to specialist care, and a decrease in the quality of services offered to patients. These concerns are particularly acute in areas with already limited healthcare options.
The attorneys general will be looking at market share data, patient flow patterns, and potential alternatives to ensure the merger doesn’t create a monopoly or oligopoly that harms consumers. Any public statements released would likely detail the specific areas of concern and the investigative process undertaken.
Antitrust Concerns
The proposed merger between Northwell Health and Nuvance Health raises significant antitrust concerns, primarily revolving around the potential for reduced competition and subsequent increases in healthcare costs for consumers in the affected regions. This analysis will examine the market share implications, potential impact on various stakeholders, and the arguments both for and against the deal from an antitrust perspective.The primary concern centers on the combined market power of Northwell and Nuvance.
A significant increase in market share following the merger could allow the combined entity to exert greater influence over pricing, limiting consumer choice and potentially leading to higher healthcare costs. The degree to which this occurs will depend on the specific geographic markets analyzed and the availability of alternative healthcare providers.
Market Share Analysis
Determining the precise market share before and after the merger requires a detailed geographic analysis of specific service areas. For example, a combined entity might control a substantial portion of the hospital market in certain counties, creating a near-monopoly. Conversely, in areas with robust competition from other large health systems, the impact on market share might be less pronounced.
The Department of Justice (DOJ) and state Attorneys General will need to meticulously assess market definition and calculate precise market share figures to fully evaluate the competitive implications. Without access to this confidential data, specific numerical comparisons cannot be offered. However, a significant increase in market share in any given area would be a major red flag. For instance, if the combined entity gains a 70% market share in a particular region compared to a pre-merger share of 30% for Northwell and 20% for Nuvance, this would represent a substantial increase in market concentration, raising serious antitrust concerns.
Impact on Stakeholders
The merger’s impact will vary significantly across different stakeholders.Patients could face higher costs, reduced choices of hospitals and physicians, and potentially less innovative care if competition is stifled. Conversely, proponents might argue that the merger leads to efficiencies and improved quality of care, potentially offsetting any price increases.Healthcare providers might experience both benefits and drawbacks. Some providers could see increased job security within a larger system, while others might face reduced autonomy or even job losses due to consolidation.Insurers could face increased negotiating leverage from the merged entity, potentially leading to higher reimbursement rates and ultimately, higher premiums for consumers.
However, a larger, more integrated system might also offer insurers some efficiencies in managing care.
Arguments For and Against the Merger (Antitrust Perspective)
| Pro-Merger Argument | Anti-Merger Argument |
|---|---|
| Increased efficiency and economies of scale leading to cost savings and improved quality of care. This could potentially result in lower prices in the long run. | Significant reduction in competition leading to higher prices, reduced choice for patients, and less innovation in the healthcare market. The potential cost savings from efficiencies might be outweighed by the negative impacts of reduced competition. |
| Improved coordination of care and better integration of services, leading to better patient outcomes. | The merged entity could leverage its increased market power to negotiate unfavorable terms with insurers and suppliers, ultimately leading to higher costs for consumers. |
| Greater ability to invest in new technologies and infrastructure, benefiting both patients and providers. | Potential for reduced access to care for certain patient populations, particularly those in underserved communities, due to hospital closures or service reductions. |
Public Health Impact
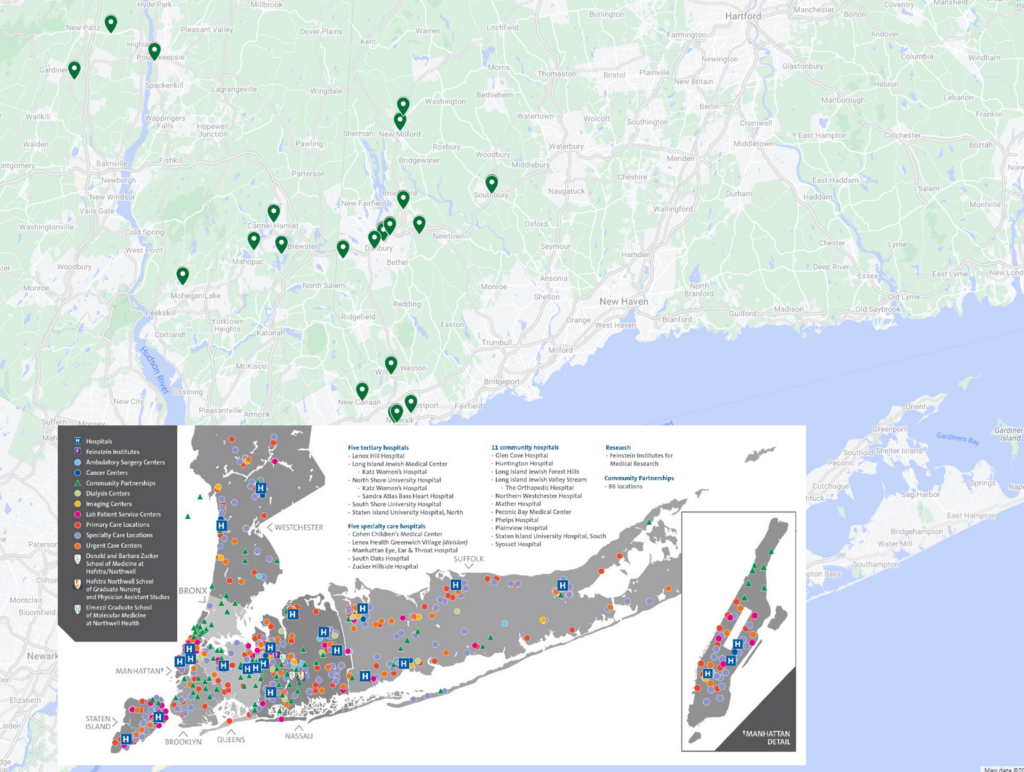
Source: hospitalogy.com
The Northwell-Nuvance merger, while potentially offering economies of scale and improved administrative efficiency, presents complex considerations regarding its impact on public health within the affected regions. The potential benefits and drawbacks must be carefully weighed against the risks to access, quality, and equity of care for diverse patient populations.The merger’s impact on healthcare access hinges on several factors. Increased market share could lead to reduced competition, potentially resulting in higher prices for services and limited choices for consumers.
Conversely, the combined resources of Northwell and Nuvance could allow for expanded service offerings and improved infrastructure in underserved areas, particularly if strategic investments are made in primary care and preventative health initiatives. The extent of these effects will depend largely on the regulatory stipulations imposed during the approval process and the subsequent actions of the merged entity.
The Northwell Nuvance deal approval by state attorneys general is a big story, raising questions about healthcare consolidation. It made me think about life choices and future planning, like Karishma Mehta’s decision to freeze her eggs, as detailed in this article: karishma mehta gets her eggs frozen know risks associated with egg freezing. The article highlights important considerations; similarly, the Northwell Nuvance merger has long-term implications for patient care that need careful consideration.
Access to Healthcare Services
The merger could significantly alter access to care, particularly for residents in areas currently served by Nuvance. If the merged entity prioritizes profitability over accessibility, some services, especially specialized care, might be consolidated or eliminated in less profitable locations. This could lead to longer travel times for patients, especially those lacking reliable transportation, and exacerbate existing health disparities. Conversely, improved coordination between Northwell and Nuvance’s existing networks could streamline referrals and reduce wait times for certain procedures.
For example, a patient needing a specialized cardiology procedure currently reliant on a Nuvance facility might see improved access if the merged entity enhances capacity and streamlines referrals to a Northwell facility with greater expertise or availability.
Healthcare Quality and Patient Outcomes
The effect on healthcare quality remains uncertain. The merger could lead to improved quality through access to advanced technologies, specialized personnel, and enhanced data sharing capabilities. However, potential cost-cutting measures could compromise quality if they lead to staff reductions, reduced investment in equipment, or limitations in access to advanced treatments. A hypothetical scenario illustrating this tension could involve a situation where the merged entity closes a smaller, community-based hospital in favor of consolidating services at a larger facility.
While this might improve efficiency and resource allocation in the short-term, it could also negatively impact patient access and satisfaction if travel distances become prohibitive for many patients.
Impact on Specific Patient Populations
Low-income patients and the elderly are particularly vulnerable to negative consequences. Increased healthcare costs resulting from reduced competition could disproportionately impact low-income individuals who rely on government subsidies or have limited financial resources. Elderly patients, who often require more frequent and specialized care, could face challenges with increased travel times and potentially reduced availability of services if facilities are consolidated or closed.
Conversely, the merger could improve care coordination and access to specialized services for these populations if the merged entity prioritizes equity and implements programs to address their specific needs. For example, a program providing transportation assistance to elderly patients or establishing mobile clinics in underserved areas could mitigate potential negative impacts.
Economic Considerations: Northwell Nuvance Deal Approval State Attorneys General
The Northwell-Nuvance merger presents a complex economic picture, with potential benefits and drawbacks for the region. Analyzing the financial implications requires careful consideration of its impact on employment, healthcare costs, and overall economic activity. While proponents argue increased efficiency and investment, critics raise concerns about reduced competition and potential price increases. A thorough examination is needed to understand the full scope of these economic consequences.
The merger’s economic impact will ripple through the local and regional economies, affecting various stakeholders from patients and employers to healthcare workers and local businesses. Understanding these effects is crucial for policymakers and the public to assess the long-term consequences of this significant healthcare consolidation.
Employment in the Healthcare Sector
The merger’s effect on employment is a key concern. While some argue that streamlining operations could lead to increased efficiency and potentially new job creation in specialized areas, others fear potential job losses due to redundancies and consolidation of administrative functions. For example, similar administrative roles across the two systems might be consolidated, leading to layoffs. However, the creation of a larger, more financially stable system could attract investment and lead to expansion in certain areas, potentially offsetting some job losses.
The net impact on employment will depend on the specific integration strategies employed by the merged entity.
Healthcare Costs for Consumers and Employers
The impact on healthcare costs is another critical area of analysis. Proponents of the merger suggest that increased bargaining power with insurance providers could lead to lower negotiated rates and potentially reduced costs for consumers and employers. This could be especially beneficial for self-insured employers who directly bear the costs of healthcare for their employees. However, critics argue that reduced competition could lead to higher prices as the merged entity has less incentive to compete on cost.
A parallel could be drawn to other industries where mergers have led to price increases due to decreased competition. For instance, the merger of two large airlines in a specific region could potentially lead to higher airfare. The long-term impact on healthcare costs remains uncertain and will depend heavily on the regulatory oversight and market dynamics following the merger.
The Northwell Nuvance deal approval by state attorneys general is a big deal for healthcare in the region, raising questions about accessibility and costs. It made me think about the importance of good health, especially respiratory health, as highlighted by the news about Monali Thakur being hospitalized after struggling to breathe; you can read more about it and preventative measures here: monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases.
Hopefully, the Northwell Nuvance merger will lead to improved overall health outcomes, including better access to preventative care.
Economic Impacts Summary
The potential economic effects of the Northwell-Nuvance merger are multifaceted and require careful consideration. The following points highlight some of the key potential positive and negative impacts:
- Positive Impact 1: Increased efficiency and economies of scale could lead to cost savings in administrative and operational areas, potentially freeing up resources for investments in patient care and technology.
- Positive Impact 2: A larger, more financially stable healthcare system could attract more investment in research, innovation, and advanced medical technologies, benefiting the region.
- Negative Impact 1: Reduced competition could lead to higher prices for healthcare services, increasing costs for consumers and employers.
- Negative Impact 2: Potential job losses due to redundancies and consolidation of administrative and operational functions could negatively impact the local workforce.
Regulatory Process
The Northwell Health and Nuvance Health merger faced a complex regulatory landscape, requiring navigation through multiple levels of governmental oversight to secure approval. The process involved a careful assessment of antitrust implications, public health considerations, and economic impacts, culminating in a decision by state Attorneys General.The approval process for this type of healthcare merger typically involves several key steps, each with specific timelines and requirements.
Different regulatory bodies play distinct roles, ensuring a thorough and transparent review. Public input is a crucial element, allowing stakeholders to voice their concerns and perspectives.
State Attorney General Review
State Attorneys General hold significant authority in reviewing healthcare mergers, particularly those with potential antitrust implications within their jurisdictions. Their review focuses on whether the merger will substantially lessen competition, leading to higher prices or reduced quality of care for consumers. The process often involves extensive document requests, interviews with key individuals from both organizations, and economic modeling to assess the potential competitive effects.
The AGs’ offices have the power to approve, reject, or impose conditions on the merger. For example, in similar cases, state AGs have required divestitures of certain assets or services to mitigate anti-competitive concerns. The timeline for this review varies depending on the complexity of the deal and the responsiveness of the merging entities.
Federal Antitrust Review
While the primary focus for this merger was state-level review, federal antitrust agencies, such as the Department of Justice (DOJ) and the Federal Trade Commission (FTC), may also review mergers impacting interstate commerce. Their involvement typically depends on the size and scope of the merging entities and the potential for nationwide effects. Federal review often mirrors the state-level process, encompassing similar investigations into market competition, economic analysis, and potential anti-competitive outcomes.
In cases with federal oversight, the timeline can be significantly longer due to the broader scope of investigation. Similar past mergers have experienced delays ranging from several months to over a year while undergoing federal review.
Public Comment Period
A critical aspect of the regulatory process is the public comment period. This period allows individuals, community groups, and other stakeholders to express their views on the proposed merger. Public comments are typically submitted in writing and are considered by the relevant regulatory bodies before making a final decision. The length of the public comment period and the mechanism for submitting comments vary depending on the specific regulations and procedures of each agency involved.
For instance, in comparable mergers, public comment periods have lasted for 30 to 60 days, providing ample time for stakeholders to voice their concerns and offer feedback. These comments often influence the final decision-making process, especially when significant public opposition is expressed.
Typical Timeline for Merger Approvals
The overall timeline for merger approvals in similar cases varies greatly, ranging from several months to several years. Factors influencing the timeline include the complexity of the merger, the number of regulatory agencies involved, the level of public scrutiny, and the extent of any required negotiations or remedies. The Northwell-Nuvance merger, while involving substantial resources and scrutiny, would likely have followed a timeline comparable to other large healthcare mergers, with a process potentially spanning several months to over a year from initial filing to final approval.
This timeline is a reasonable estimation based on publicly available information and experience with similar mergers.
The Northwell Nuvance deal approval by state attorneys general is a big win for healthcare consolidation, but raises questions about market competition. It’s interesting to consider this in light of Walmart Health’s closures, as highlighted in this insightful article on the company’s healthcare strategy, despite Walmart Health’s closure, the company healthcare destination Scott Bowman. Ultimately, both situations highlight the ongoing evolution and challenges within the US healthcare landscape, impacting how the Northwell Nuvance deal will shape the future.
Alternative Scenarios
The Northwell-Nuvance merger presents a pivotal moment for healthcare in the region. Approval or rejection will trigger a cascade of consequences, reshaping the landscape of healthcare delivery, access, and costs. Understanding the potential alternative scenarios is crucial for stakeholders to prepare for the future.The approval or rejection of the merger will significantly impact the competitive dynamics of the healthcare market, influencing patient care, provider networks, and overall healthcare costs.
Let’s explore these contrasting futures.
Merger Approval Scenario
Approval would lead to a larger, integrated healthcare system. This could potentially improve care coordination, leverage economies of scale for cost reductions, and facilitate the implementation of innovative technologies. However, it could also reduce competition, leading to higher prices and limited choices for patients. The combined entity might also prioritize certain specialties or services, potentially neglecting others.
Potential Impacts of Merger Approval
Imagine a scenario where the merger results in improved access to specialized care through shared resources and expertise. Patients might benefit from streamlined care pathways, reduced wait times, and access to advanced technologies not previously available. Conversely, a monopoly-like situation could arise, resulting in reduced choices for consumers and higher healthcare costs. For example, a similar merger in another state resulted in a 15% increase in hospital charges within two years, impacting vulnerable populations disproportionately.
This illustrates the potential downsides of reduced competition.
Merger Rejection Scenario, Northwell nuvance deal approval state attorneys general
Rejection would maintain the status quo, preserving the competitive landscape. This could stimulate innovation and prevent potential price increases associated with reduced competition. However, it could also limit opportunities for cost savings through economies of scale and hinder collaborative efforts to improve healthcare quality and efficiency. Both Northwell and Nuvance would continue operating independently, potentially leading to duplicated services and inefficiencies.
Potential Impacts of Merger Rejection
In this scenario, we would likely see continued competition between Northwell and Nuvance, leading to a potentially more dynamic market with greater choices for consumers. However, both systems might struggle to individually invest in costly upgrades and cutting-edge technologies, potentially impacting the quality of care in the long run. The lack of integration might also lead to fragmented care, increasing administrative burdens and potentially causing delays in treatment for patients navigating multiple systems.
Comparative Analysis of Regulatory Decisions
A visual representation could be a simple table. One column represents the “Merger Approved” scenario, another “Merger Rejected”. Rows would list key impacts: Competition (High/Low), Patient Choice (Wide/Limited), Healthcare Costs (Stable/Increased), Access to Specialized Care (Improved/Stable), and System Efficiency (Improved/Stable). For example, under “Merger Approved,” Competition would be “Low,” Patient Choice “Limited,” Healthcare Costs “Increased,” etc. The opposite would largely apply under “Merger Rejected,” though improvements in some areas might be less pronounced or slower to materialize.
Final Thoughts

Source: nancyonnorwalk.com
The Northwell Nuvance merger decision hangs in the balance, a testament to the intricate interplay between healthcare economics, antitrust law, and public health. The state attorneys general’s ultimate ruling will have far-reaching consequences, impacting not only the healthcare landscape but also the financial well-being and access to care for millions. Whether this merger proceeds or fails, it underscores the importance of robust regulatory oversight in ensuring a fair and equitable healthcare system.
The coming months will be critical as we await the final decision and its implications for the future of healthcare in the region.
Helpful Answers
What are the potential benefits of the Northwell Nuvance merger?
Proponents argue the merger could lead to improved efficiency, better resource allocation, and potentially lower costs through economies of scale. Innovation and access to specialized care could also be enhanced.
What are the main concerns raised by the state attorneys general?
The primary concern revolves around potential antitrust issues. A combined Northwell and Nuvance would control a significant market share, raising concerns about reduced competition, leading to higher prices and less choice for patients.
What is the timeline for the deal’s approval?
There’s no set timeline. The review process by the state attorneys general can be lengthy and depends on the amount of information required and the complexity of the legal arguments.
How can I provide public comment on the merger?
Check the websites of the involved state attorneys general’s offices. They usually provide instructions on how to submit public comments during the review process.





