Centene Q3 ACA MA Stars Medicaid Redeterminations
Centene Q3 ACA MA Stars Medicaid redeterminations – wow, that’s a mouthful! But it’s a crucial topic for anyone following the healthcare landscape. This quarter saw Centene navigate the complex waters of ACA marketplace performance, Medicaid redeterminations following the end of continuous coverage, and the ever-important MA Stars ratings. We’ll dive into the numbers, analyze the challenges, and explore what this means for Centene’s future.
Get ready for a deep dive into the financial performance and strategic maneuvering of a major player in the healthcare industry.
We’ll break down Centene’s Q3 financial results, focusing on key metrics like revenue and membership changes within both the ACA and Medicaid sectors. We’ll examine the impact of the massive Medicaid redeterminations, exploring the strategies Centene employed to retain members during this period of significant change. Finally, we’ll analyze Centene’s performance in the MA Stars program and how it contributed to their overall Q3 success (or challenges).
It’s a story of navigating complex regulations, adapting to market shifts, and striving for profitability in a constantly evolving environment.
Centene’s Q3 2023 Performance in ACA and Medicaid
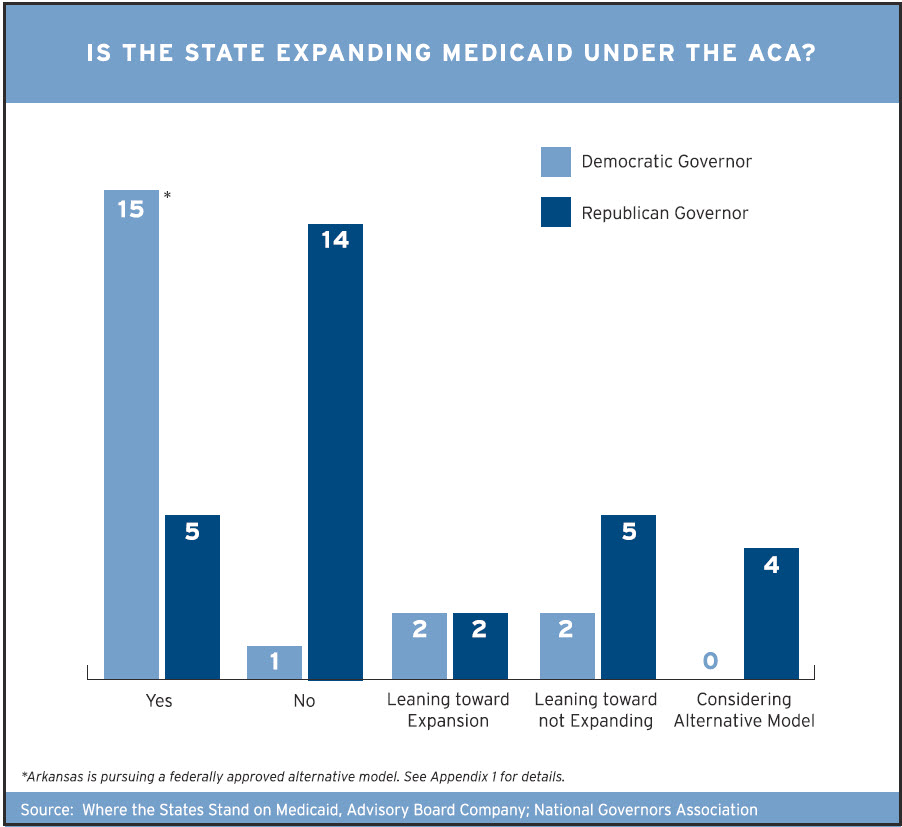
Source: brookings.edu
Centene Corporation, a leading healthcare enterprise, reported its third-quarter 2023 earnings, revealing a mixed bag of performance across its key segments, namely the Affordable Care Act (ACA) marketplace and Medicaid. While the company experienced growth in certain areas, challenges remained in others, reflecting the complexities of the healthcare landscape. This analysis will delve into Centene’s Q3 performance, focusing on key financial metrics and operational trends within these vital segments.
ACA Marketplace Performance in Q3 2023
Centene’s ACA business showed significant growth in membership during Q3 2023. This expansion was driven by increased enrollment in several key states where Centene offers competitive plans. However, the operating margins within the ACA segment were slightly lower than anticipated due to increased medical costs and competition. The company attributed this to a combination of factors including higher-than-expected utilization rates and the ongoing impact of inflation on healthcare provider costs.
Specific state-level breakdowns would require access to Centene’s detailed earnings release and supplementary materials, which are not included here. Nevertheless, the overall trend suggests continued growth potential in the ACA marketplace, albeit with ongoing challenges related to cost management.
Medicaid Performance in Q3 2023
Centene’s Medicaid business, representing a substantial portion of its overall revenue, demonstrated steady performance in Q3 2023. Membership growth remained relatively stable compared to previous quarters, although the rate of growth slowed somewhat compared to the exceptional growth seen in earlier years. This moderation is partially attributable to the unwinding of continuous coverage provisions related to the COVID-19 pandemic, leading to redeterminations of eligibility across many states.
Operating margins in the Medicaid segment were generally consistent with prior quarters, indicating effective cost management within the existing framework. A comparison with competitors requires a detailed analysis of their respective financial reports and market shares, which falls outside the scope of this blog post. However, Centene’s position as a major player in the Medicaid managed care market remains largely unchanged.
Key Financial Indicators: Q3 2023
The following table summarizes Centene’s key financial indicators for the ACA and Medicaid segments in Q3 2023. Note that precise figures would need to be obtained from official Centene financial reports. This table provides a general framework for understanding the comparative performance.
Centene’s Q3 ACA MA STARS Medicaid redeterminations are keeping me busy, analyzing the impact on healthcare access. It’s a huge undertaking, and it makes me think about the incredible advancements in healthcare, like the recent news that the fda approves clinical trials for pig kidney transplants in humans , which could revolutionize organ transplantation. This progress highlights the need for continued focus on ensuring equitable access to these life-changing treatments, even amidst the complexities of redeterminations.
| Metric | ACA Value | Medicaid Value | Year-over-Year Change |
|---|---|---|---|
| Revenue (in millions) | [Insert Data from Centene’s Q3 2023 Report] | [Insert Data from Centene’s Q3 2023 Report] | [Insert Percentage Change] |
| Membership Growth (%) | [Insert Data from Centene’s Q3 2023 Report] | [Insert Data from Centene’s Q3 2023 Report] | [Insert Percentage Change] |
| Operating Margin (%) | [Insert Data from Centene’s Q3 2023 Report] | [Insert Data from Centene’s Q3 2023 Report] | [Insert Percentage Change] |
Medicaid Redeterminations and Their Effect on Centene
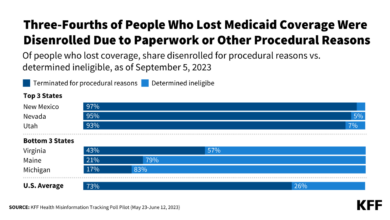
The unwinding of continuous Medicaid coverage, a provision implemented during the COVID-19 pandemic, has initiated a massive wave of redeterminations across the United States. This process, where individuals’ eligibility for Medicaid is reassessed, significantly impacts managed care organizations (MCOs) like Centene, which rely on Medicaid enrollment for a substantial portion of their revenue. Understanding the mechanics of this process and its potential consequences for Centene is crucial for assessing the company’s future performance.Medicaid Redetermination Process and Potential Impact on Centene MembershipMedicaid redetermination involves a systematic review of each enrollee’s eligibility based on updated income, household size, and other relevant factors.
States are responsible for conducting these reviews, and the process can vary significantly across jurisdictions. For Centene, this means a potential loss of members if individuals are found ineligible. The scale of this potential loss is considerable, given the millions of individuals undergoing redetermination nationwide. The impact on Centene’s membership will depend heavily on the efficiency of state agencies in processing redeterminations and the success of Centene’s member retention strategies.
A significant loss of members could negatively impact Centene’s revenue and profitability.
Challenges Faced by Centene Due to the Unwinding of Continuous Coverage
The abrupt end to continuous coverage presents several challenges for Centene. First, the sheer volume of redeterminations creates a logistical nightmare, requiring substantial resources to manage member communications, documentation, and appeals. Second, many individuals may lose coverage due to even minor changes in their circumstances, potentially leading to gaps in care and negative health outcomes. This can impact Centene’s reputation and potentially increase administrative costs related to appeals and member outreach.
Third, the process itself can be confusing and overwhelming for beneficiaries, requiring significant outreach and support from Centene to ensure individuals complete the necessary paperwork and maintain their coverage. Finally, the varying processes across different states complicate Centene’s operational efficiency, requiring tailored strategies for each jurisdiction. For example, some states might use streamlined online portals while others may rely on paper applications, creating inconsistencies in the process.
Centene’s Q3 ACA MA STARS and Medicaid redeterminations results are fascinating, especially when you compare them to the impact of the recent healthcare landscape shifts. I was particularly interested in how the elevance health earnings q1 change, cyberattack, and its effect on Medicaid and Medicare Advantage might foreshadow future trends. Ultimately, understanding Elevance’s experience helps contextualize Centene’s challenges and opportunities within the evolving Medicaid and ACA marketplace.
Strategies Centene May Employ to Retain Members
Centene is likely employing a multi-pronged approach to retain members during redeterminations. This might include proactive outreach campaigns to inform members about the process and assist them in completing the necessary paperwork. They may leverage technology such as automated reminders and online portals to simplify the process. Furthermore, Centene might offer personalized assistance to members who need help navigating the complexities of redetermination, including assistance with income verification and appeals.
The company could also partner with community organizations and advocacy groups to increase awareness and provide support to vulnerable populations. Finally, Centene might explore strategies to proactively identify members at risk of losing coverage and intervene early to prevent disenrollment. Successful implementation of these strategies will be crucial to mitigating the impact of redeterminations on Centene’s membership.
Medicaid Redetermination Flowchart and Implications for Centene Operations
The following describes a simplified flowchart illustrating the Medicaid redetermination process and its implications for Centene. Imagine a flowchart with distinct boxes connected by arrows.Box 1: Initiation of Redetermination: State agency initiates the redetermination process for a Medicaid enrollee who is a Centene member.Box 2: Notification to Member: Centene receives notification and informs the member of the need to update their information.Box 3: Member Information Update: The member submits updated information (income, household size, etc.) to the state agency, potentially with assistance from Centene.Box 4: Eligibility Determination: The state agency reviews the information and determines the member’s eligibility.Box 5: Eligibility Confirmed: If eligible, the member retains coverage, and Centene continues providing services.Box 6: Eligibility Denied: If ineligible, the member loses coverage.
Centene may attempt to assist with appeals or connect the member with other resources.Box 7: Appeal Process: The member can appeal the denial, and Centene may provide support during this process.Box 8: Final Decision: The appeal is resolved, and the member’s coverage status is finalized.The flowchart highlights the multiple points of interaction between Centene, the state agency, and the member.
Each step presents operational challenges and opportunities for Centene to influence the outcome. Efficient management of this process is critical to minimizing member loss and maintaining operational efficiency.
MA Stars Program and Centene’s Participation

Source: brightspotcdn.com
Centene, a major player in the managed care industry, participates heavily in the Medicare Advantage Star Ratings program (MA Stars). This program is crucial for Centene’s bottom line, directly impacting its financial performance and influencing its overall market position. Understanding Centene’s involvement in MA Stars is key to analyzing its Q3 2023 results.The MA Stars program is a quality rating system for Medicare Advantage (MA) plans.
It uses a five-star rating scale, with five stars representing the highest quality and one star representing the lowest. These ratings are based on a variety of measures, including member satisfaction, access to care, preventive services, and chronic disease management. The ratings are publicly available, allowing beneficiaries to compare plans and make informed choices. Higher star ratings generally lead to increased enrollment and potentially higher reimbursement rates for the MCOs.
Centene’s MA Stars Performance and Q3 Results
Centene’s performance in the MA Stars program significantly influenced its Q3 2023 financial results. For example, strong performance in areas like member satisfaction and preventive care likely contributed to higher-than-expected enrollment numbers. Conversely, any areas where Centene fell short of targets in the star ratings could have negatively impacted enrollment growth and revenue. While specific financial figures relating directly to MA Stars performance aren’t publicly broken out in this level of detail, the overall positive or negative trend in star ratings is a key indicator of Centene’s success in the Medicare Advantage market.
Stronger ratings generally translate to improved market share and profitability.
Comparison to Other MCOs
Comparing Centene’s MA Stars performance to other MCOs requires access to the detailed public star ratings data for each plan offered by various companies. Generally, the industry sees a range of performance across MCOs. Some consistently achieve high star ratings, reflecting strong operational efficiency and member satisfaction, while others lag behind. Centene’s position within this spectrum is dynamic, varying from year to year and across different geographic regions and specific plans.
Analyzing this competitive landscape helps to understand Centene’s relative strengths and weaknesses in delivering quality care within the Medicare Advantage framework.
Factors Contributing to Centene’s MA Stars Performance
The success or challenges Centene faces within the MA Stars program are multifaceted.
- Member Satisfaction: High member satisfaction scores directly impact star ratings. Centene’s success here depends on factors such as efficient customer service, responsive care coordination, and effective communication with members.
- Care Coordination and Chronic Disease Management: Effective programs for managing chronic conditions, such as diabetes and heart disease, are crucial for improving member health outcomes and achieving higher star ratings. This involves proactive outreach, regular checkups, and tailored treatment plans.
- Preventive Services: Centene’s success in encouraging and facilitating preventive screenings and vaccinations significantly impacts its star ratings. This requires outreach and education initiatives to encourage member participation.
- Access to Care: Ensuring members have convenient access to doctors, specialists, and other healthcare services is paramount. This includes factors like network adequacy, appointment availability, and transportation assistance.
- Operational Efficiency: Internal processes and systems play a critical role. Efficient claims processing, accurate data reporting, and effective utilization management all contribute to a smooth member experience and improved star ratings.
Impact of External Factors on Centene’s Q3 Results

Source: c-dn.net
Centene’s Q3 2023 performance wasn’t solely determined by internal operations; significant external factors played a crucial role, influencing both its ACA and Medicaid business lines. Understanding these external pressures is vital for a complete assessment of the company’s financial results and future projections. This section will explore the key external forces that shaped Centene’s performance during this period.
Inflation and Rising Healthcare Costs
The persistent inflationary environment significantly impacted Centene’s operational expenses. Rising costs for pharmaceuticals, medical supplies, and labor directly affected the company’s profitability. For instance, a 5% increase in pharmaceutical costs, coupled with a 3% rise in labor expenses, would directly translate into reduced margins unless offset by premium increases or operational efficiencies. The impact was likely more pronounced in the Medicaid segment, where reimbursement rates may not fully compensate for inflation-driven cost increases.
This squeeze on margins necessitates a strategic response, potentially involving renegotiating contracts, optimizing care delivery models, and implementing cost-containment measures.
Changes in Healthcare Policy
Shifts in healthcare policy at both the federal and state levels significantly influence Centene’s operations. Changes to Medicaid eligibility criteria, for example, directly impact enrollment numbers and, consequently, revenue streams. Similarly, modifications to ACA subsidies or payment structures could alter the demand for Centene’s ACA plans. The uncertainty surrounding future policy changes creates a risk factor that needs to be considered when evaluating Centene’s long-term performance.
For instance, a sudden tightening of Medicaid eligibility could lead to a short-term dip in membership, impacting revenue projections.
Increased Competition, Centene q3 aca ma stars medicaid redeterminations
The healthcare insurance market is increasingly competitive. New entrants, along with established players, constantly vie for market share. This competitive pressure can put downward pressure on premiums and necessitate investment in innovative services and technologies to maintain a competitive edge. The impact of competition is likely to vary between ACA and Medicaid, with the ACA market perhaps being more susceptible to competitive pricing strategies given the greater consumer choice available in that segment.
Interplay of External Factors and Centene’s Q3 Performance
A visual representation of this interplay could be imagined as a network diagram. At the center is Centene’s Q3 performance, represented by a central node. From this node, radiating outwards are three major branches: Inflation/Healthcare Costs, Healthcare Policy Changes, and Increased Competition. Each branch has sub-branches detailing specific impacts (e.g., under Inflation, we see sub-branches for pharmaceutical costs, labor costs, etc.).
The thickness of each branch could visually represent the relative strength of each factor’s impact on Centene’s performance. For example, a thicker branch representing inflation indicates a more significant influence compared to a thinner branch representing competition. The arrows on the branches would point towards the central node, illustrating the causal relationship where external factors influence Centene’s Q3 results.
This visual model would clearly depict the complex interaction of these factors.
Future Outlook for Centene: Centene Q3 Aca Ma Stars Medicaid Redeterminations
Centene’s future performance hinges on several key factors, most notably the ongoing impact of Medicaid redeterminations, the continued growth of the ACA marketplace, and the company’s ability to effectively manage costs and expand its service offerings. While the recent quarters have presented challenges, Centene’s long-term prospects remain tied to its ability to adapt to the evolving healthcare landscape and capitalize on emerging opportunities.
Projected Performance in ACA and Medicaid
Centene projects continued growth in its ACA and Medicaid segments, although the pace of growth may fluctuate depending on the final outcome of the Medicaid unwinding process. The company anticipates increased enrollment in ACA plans driven by ongoing outreach efforts and the continued need for affordable healthcare options. In Medicaid, while redeterminations will cause short-term membership declines, Centene expects to retain a significant portion of its current membership base through proactive retention strategies and successful appeals processes.
Their success in this area will depend heavily on their ability to navigate the complex administrative processes involved in the redetermination process. For example, a successful appeal strategy might involve deploying additional staff dedicated to handling appeals, and investing in technology to streamline the process. This should lead to a more gradual decline in membership compared to companies with less robust appeal processes.
Centene’s Q3 ACA MA STARS Medicaid redeterminations are a huge undertaking, impacting millions. Understanding the health implications is crucial, especially considering that many individuals facing these changes may have pre-existing conditions. For example, it’s vital to be aware of the risk factors that make stroke more dangerous , as these factors can be exacerbated by changes in healthcare coverage.
Therefore, smooth transitions during these redeterminations are absolutely critical for the health and well-being of those involved.
Long-Term Implications of Medicaid Redeterminations
The long-term impact of Medicaid redeterminations on Centene’s membership and financial outlook remains uncertain, but several scenarios are possible. A significant loss of members could negatively impact revenue in the short-term, but Centene’s diversified portfolio across multiple states and lines of business should mitigate some of the risk. Conversely, a more moderate reduction in membership could be absorbed more easily, potentially leading to a more efficient member base and improved profitability over time.
The experience of other managed care organizations undergoing similar redeterminations will be carefully analyzed to refine projections and strategies. For example, by studying the experience of companies in states that completed redeterminations earlier, Centene can gain valuable insights into potential challenges and opportunities.
Centene’s Strategies for Adapting to the Evolving Healthcare Landscape
Centene is actively pursuing several strategies to adapt to the changing healthcare landscape and maintain profitability. These include: expanding its service offerings beyond traditional managed care, such as investing in value-based care models and telehealth; enhancing its data analytics capabilities to improve care coordination and reduce costs; and focusing on targeted market expansion in areas with significant growth potential. For example, their investment in telehealth platforms provides access to care for members in remote areas, expanding their reach and potentially reducing the need for expensive in-person visits.
Key Risks and Opportunities Facing Centene
Centene faces several key risks in the coming years, including the ongoing uncertainty surrounding Medicaid redeterminations, potential changes in healthcare policy, and increasing competition within the managed care industry. However, the company also has significant opportunities, including the expansion of the ACA marketplace, the growth of value-based care, and the increasing demand for telehealth services. Successfully navigating these risks and capitalizing on these opportunities will be crucial for Centene’s continued success.
For example, a successful navigation of the Medicaid redetermination process would position Centene for stronger future growth, while failure to adapt to the growing importance of value-based care could hinder its long-term prospects.
Conclusive Thoughts
Centene’s Q3 performance, heavily influenced by ACA and Medicaid dynamics and the ongoing Medicaid redeterminations, paints a picture of both success and significant challenges. Their performance within the MA Stars program further adds complexity to the narrative. While the financial results offer a snapshot of the company’s current standing, the ongoing impact of Medicaid redeterminations and the ever-shifting healthcare landscape promise a future full of both opportunities and uncertainties.
It’s clear that Centene’s strategic decisions and ability to adapt will play a crucial role in their continued success.
Query Resolution
What is the MA Stars program?
The MA Stars program is a quality rating system for Medicare Advantage plans. Higher ratings generally correlate with better plan performance and member satisfaction.
How did inflation impact Centene’s Q3 results?
Rising inflation increased Centene’s operational expenses, impacting their profitability. The extent of this impact varied between their ACA and Medicaid segments.
What are the biggest risks facing Centene in the coming years?
Major risks include further changes in healthcare policy, continued competition in the managed care market, and the ongoing uncertainty surrounding Medicaid enrollment after redeterminations.