
What Are Endocrine Disorders Symptoms, Causes, Diagnosis, Treatment
What are endocrine disorders symptoms causes diagnosis and treatment? That’s the big question, and it’s one that affects millions. Our bodies are intricate orchestras, and the endocrine system – the conductor of hormones – plays a crucial role. When this system malfunctions, the consequences can be significant, impacting everything from our energy levels to our moods and even our growth.
This post delves into the fascinating world of endocrine disorders, exploring the common symptoms, underlying causes, diagnostic methods, and available treatments. Get ready to unravel the mysteries of this vital bodily system!
We’ll cover a range of disorders, from the well-known (like diabetes and thyroid problems) to those less frequently discussed. We’ll look at how genetics, lifestyle, and environmental factors can all contribute to these conditions. Understanding the diagnostic process, from initial symptoms to advanced testing, is key to effective management. Finally, we’ll explore various treatment options, including medications, lifestyle adjustments, and surgical interventions, highlighting the importance of personalized care.
Introduction to Endocrine Disorders
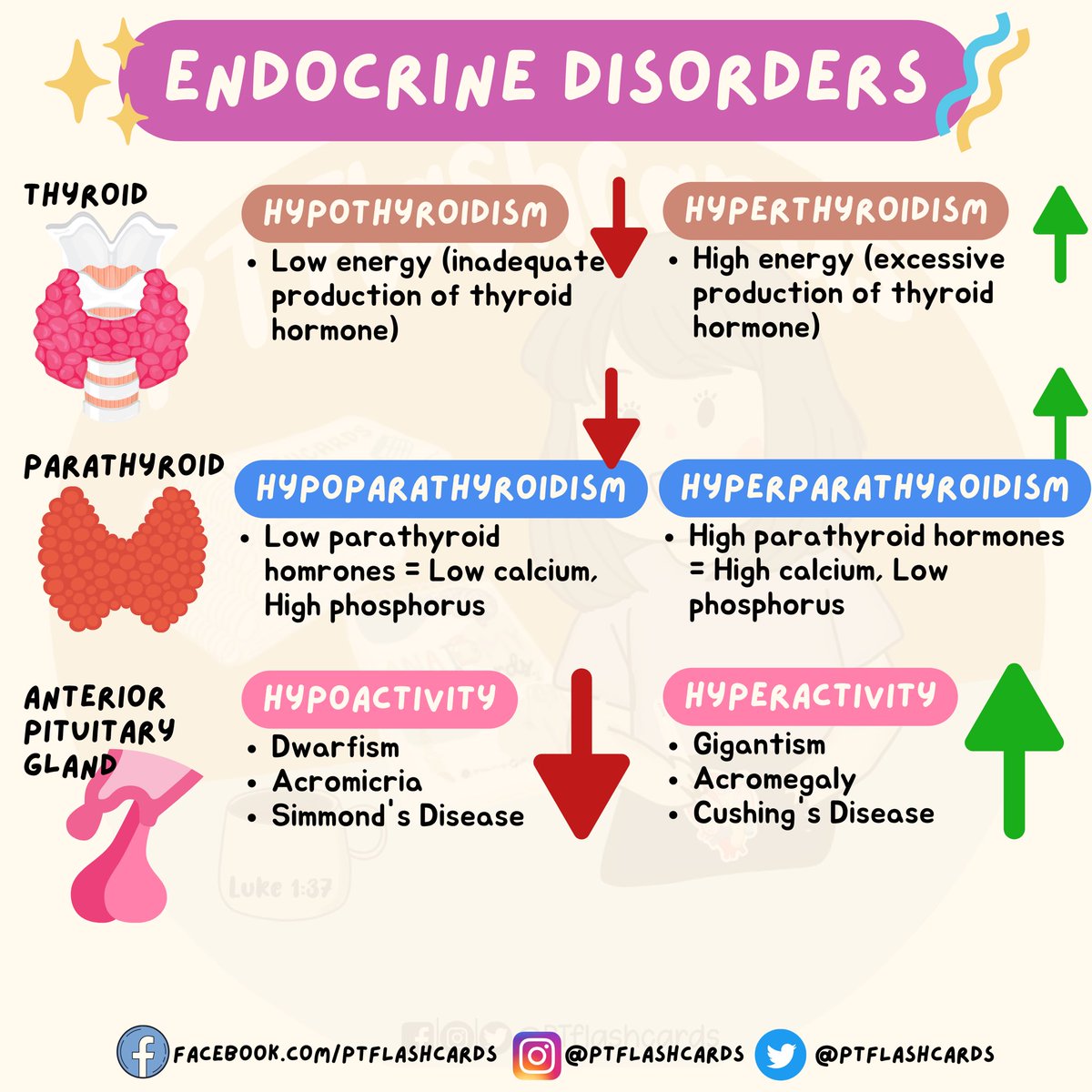
Source: twimg.com
The endocrine system is a complex network of glands that produce and release hormones directly into the bloodstream. These hormones act as chemical messengers, traveling throughout the body to regulate a vast array of functions, including metabolism, growth and development, reproduction, mood, sleep, and even our response to stress. A healthy endocrine system is crucial for maintaining overall well-being and balance within the body.
Disruptions to this delicate system can have wide-ranging and significant consequences.Endocrine disorders arise from imbalances in hormone production, action, or both. These imbalances can lead to a variety of symptoms, depending on which gland or hormone is affected and the severity of the disruption. The impact on the body can be subtle or dramatic, ranging from mild fatigue and weight changes to serious complications affecting multiple organ systems.
Effective management often requires a multi-faceted approach, involving lifestyle adjustments, medication, and sometimes surgery.
Common Endocrine Disorders
Several endocrine disorders are relatively common and affect a significant portion of the population. Understanding these conditions, their symptoms, and available treatments is essential for early detection and improved patient outcomes.
- Diabetes Mellitus: This disorder affects the body’s ability to regulate blood sugar levels. Type 1 diabetes results from the body’s immune system attacking insulin-producing cells in the pancreas. Type 2 diabetes is characterized by insulin resistance, where the body’s cells don’t respond effectively to insulin. Symptoms can include increased thirst and urination, unexplained weight loss, fatigue, and blurred vision.
Treatment often involves insulin therapy, oral medications, lifestyle modifications (diet and exercise), and regular blood sugar monitoring.
- Hypothyroidism: This condition occurs when the thyroid gland doesn’t produce enough thyroid hormone. This hormone is essential for regulating metabolism. Symptoms include fatigue, weight gain, constipation, dry skin, and intolerance to cold. Treatment typically involves hormone replacement therapy with synthetic thyroid hormone.
- Hyperthyroidism: In contrast to hypothyroidism, hyperthyroidism occurs when the thyroid gland produces too much thyroid hormone. Symptoms can include weight loss, nervousness, irritability, increased heart rate, and heat intolerance. Treatment options may include antithyroid medications, radioactive iodine therapy, or surgery.
- Cushing’s Syndrome: This disorder is caused by prolonged exposure to high levels of cortisol, a stress hormone. This can be due to various causes, including tumors in the pituitary gland or adrenal glands. Symptoms include weight gain, particularly in the face and abdomen, muscle weakness, high blood pressure, and skin thinning. Treatment focuses on addressing the underlying cause, often involving surgery or medication.
Symptoms of Endocrine Disorders
Endocrine disorders, stemming from imbalances in hormone production, can manifest in a wide array of symptoms. These symptoms are often subtle and can mimic those of other medical conditions, making diagnosis challenging. Understanding common symptoms is crucial for early detection and appropriate medical intervention. The severity and presentation of symptoms can vary significantly depending on the specific endocrine gland affected, the type and extent of the hormonal imbalance, and individual factors like age, overall health, and genetic predisposition.
Common Symptoms Across Endocrine Disorders, What are endocrine disorders symptoms causes diagnosis and treatment
Many endocrine disorders share overlapping symptoms, making it difficult to pinpoint a specific cause without proper testing. These shared symptoms often involve changes in metabolism, energy levels, and bodily functions. The following table highlights some common symptoms across various disorders. Note that not all individuals with an endocrine disorder will experience all of these symptoms, and the severity can vary greatly.
| Disorder | Symptom 1 | Symptom 2 | Symptom 3 |
|---|---|---|---|
| Hypothyroidism | Fatigue and lethargy | Weight gain | Intolerance to cold |
| Hyperthyroidism | Weight loss | Increased heart rate | Anxiety and irritability |
| Diabetes Mellitus | Increased thirst and urination | Elevated blood sugar levels | Blurred vision |
| Cushing’s Syndrome | Weight gain (particularly in the face and abdomen) | Muscle weakness | High blood pressure |
Symptom Variation and Individual Factors
The symptoms experienced by individuals with endocrine disorders are highly variable. For example, while fatigue is common in both hypothyroidism and Addison’s disease, the specific type of fatigue, its intensity, and associated symptoms can differ considerably. Similarly, weight changes can be a symptom of several endocrine disorders, but the nature of the weight change (gain or loss) and its distribution in the body can provide clues to the underlying cause.
Individual factors such as age, genetics, overall health, and the presence of other medical conditions can also significantly influence symptom presentation. A young person with hyperthyroidism may experience different symptoms and severity compared to an older adult with the same condition.
The Importance of Early Symptom Recognition
Early recognition of endocrine disorder symptoms is vital for effective management and prevention of long-term complications. Many endocrine disorders, if left untreated, can lead to serious health problems, affecting various organ systems. For instance, uncontrolled diabetes can damage the kidneys, nerves, and blood vessels, increasing the risk of cardiovascular disease, blindness, and kidney failure. Early diagnosis and treatment can significantly improve outcomes and quality of life.
If you experience persistent or unexplained symptoms such as fatigue, weight changes, changes in bowel habits, or excessive thirst or urination, it’s crucial to seek medical attention for a thorough evaluation.
Causes of Endocrine Disorders: What Are Endocrine Disorders Symptoms Causes Diagnosis And Treatment
Endocrine disorders arise from a complex interplay of genetic predisposition, environmental exposures, and lifestyle choices. Understanding these contributing factors is crucial for both prevention and effective management of these conditions. While some disorders are primarily caused by a single factor, most result from a combination of influences, making diagnosis and treatment challenging yet rewarding.
Genetic Factors in Endocrine Disorders
Many endocrine disorders have a significant genetic component. Inherited mutations in genes responsible for hormone production, receptor function, or the regulation of hormone synthesis can lead to a range of conditions. For example, certain types of diabetes, such as Maturity-Onset Diabetes of the Young (MODY), are directly linked to specific gene defects affecting insulin production or action. Similarly, some forms of congenital adrenal hyperplasia (CAH) result from inherited enzyme deficiencies affecting cortisol and aldosterone production.
Genetic testing can play a vital role in diagnosing these conditions and identifying individuals at increased risk.
Environmental Factors Contributing to Endocrine Disorders
Environmental toxins and exposures can disrupt the delicate balance of the endocrine system. Exposure to certain chemicals, such as pesticides and industrial pollutants, can mimic or block hormone action, leading to endocrine disruption. For instance, some studies suggest a link between exposure to certain pesticides and an increased risk of thyroid disorders. Furthermore, environmental factors like iodine deficiency are a major cause of hypothyroidism in regions with insufficient iodine intake.
Radiation exposure, particularly in high doses, can also damage the endocrine glands, affecting hormone production.
Understanding endocrine disorders involves looking at symptoms like fatigue and weight changes, caused by hormonal imbalances. Diagnosis often uses blood tests, and treatment might include medication or lifestyle changes, including diet. A crucial aspect of this is nutrition, which is why learning about dietary needs is so important; check out this article on how are women and men receptive of different types of food and game changing superfoods for women to tailor your approach.
Managing endocrine disorders effectively often hinges on a balanced diet and appropriate medical care.
Lifestyle Factors and Endocrine Disorders
Lifestyle choices significantly impact endocrine health. Obesity, a prevalent issue in many societies, is a major risk factor for type 2 diabetes and other endocrine disorders. Excess body fat disrupts insulin signaling and contributes to insulin resistance. Similarly, a sedentary lifestyle contributes to weight gain and exacerbates the negative effects of obesity on endocrine function. Poor diet, lacking essential nutrients like iodine or selenium, can also negatively impact hormone production and metabolism.
Chronic stress, a significant aspect of modern life, can also disrupt hormone balance, potentially contributing to various endocrine disorders.
Causes of Hypothyroidism and Hyperthyroidism
Understanding the causes of hypothyroidism and hyperthyroidism is critical for appropriate management. These conditions represent opposite ends of a spectrum of thyroid function.
The potential causes of these disorders can be summarized as follows:
- Hypothyroidism: Autoimmune thyroiditis (Hashimoto’s thyroiditis), iodine deficiency, medications (e.g., lithium, amiodarone), pituitary disorders, congenital hypothyroidism, thyroid surgery or radiation therapy.
- Hyperthyroidism: Graves’ disease (an autoimmune disorder), toxic multinodular goiter, thyroid adenoma (a benign tumor), excessive iodine intake, thyroiditis (inflammation of the thyroid gland).
Causes of Different Endocrine Disorders: A Comparison
The causes of various endocrine disorders vary significantly. Diabetes, for example, encompasses both type 1 and type 2 forms. Type 1 diabetes is an autoimmune disease where the body’s immune system attacks and destroys insulin-producing cells in the pancreas. Type 2 diabetes, on the other hand, is primarily characterized by insulin resistance, often linked to obesity and lifestyle factors.
Thyroid disorders, as discussed above, are frequently autoimmune in origin (Hashimoto’s thyroiditis and Graves’ disease), but can also result from iodine deficiency, medication side effects, or other factors. Adrenal disorders, such as Addison’s disease (adrenal insufficiency), can stem from autoimmune destruction of the adrenal glands, infections, or genetic defects. Cushing’s syndrome, conversely, involves excess cortisol production, often due to pituitary or adrenal tumors.
These examples illustrate the diversity of causes underlying different endocrine disorders.
Diagnosis of Endocrine Disorders
Diagnosing endocrine disorders can be a complex process, often requiring a combination of tests and careful clinical evaluation. The process aims to pinpoint the specific hormone imbalance and its underlying cause, guiding subsequent treatment strategies. The path to diagnosis isn’t always straightforward, and it frequently involves a collaborative effort between the patient and their healthcare team.
Diagnostic Tests and Procedures
Several tests are crucial in identifying endocrine disorders. These tests are selected based on the patient’s symptoms and the suspected endocrine gland involved. The results of these tests, taken together with the patient’s medical history and physical examination, provide a comprehensive picture of the endocrine system’s function.
- Blood Tests: These are the most common diagnostic tools, measuring hormone levels (e.g., thyroid-stimulating hormone (TSH), thyroxine (T4), triiodothyronine (T3) for thyroid disorders; cortisol for adrenal disorders; insulin and glucose for diabetes; growth hormone for growth disorders). Blood tests can also assess kidney and liver function, which are important for interpreting hormone levels and identifying potential complications.
- Urine Tests: Urine tests measure hormone levels excreted in urine, providing another perspective on hormone production and metabolism. For example, measuring cortisol levels in a 24-hour urine collection can help diagnose Cushing’s syndrome.
- Imaging Tests: These tests visualize endocrine glands to assess their size, shape, and structure. Examples include ultrasounds, computed tomography (CT) scans, and magnetic resonance imaging (MRI). These scans can detect tumors, cysts, or other abnormalities that might be affecting hormone production.
- Stimulation and Suppression Tests: These tests assess the feedback mechanisms within the endocrine system. For example, a stimulation test might involve administering a hormone and measuring the body’s response, while a suppression test might involve suppressing a hormone’s production and observing the effects. These tests help determine whether a gland is functioning properly or if there’s a problem with hormone regulation.
- Genetic Testing: In some cases, genetic testing may be used to identify genetic mutations that can cause endocrine disorders. This is particularly relevant for certain inherited conditions affecting hormone production or action.
The Diagnostic Process: A Step-by-Step Approach
The diagnostic journey typically follows a structured path. It starts with a thorough evaluation of the patient’s symptoms and medical history, followed by a physical examination. Based on this initial assessment, specific tests are ordered to confirm or rule out suspected endocrine disorders.
- Initial Consultation and History: The physician will discuss the patient’s symptoms, medical history, family history of endocrine disorders, and any medications they are taking. This step is crucial in identifying potential risk factors and narrowing down the possibilities.
- Physical Examination: A physical exam helps to identify any physical signs associated with endocrine disorders, such as goiter (enlarged thyroid gland), weight changes, changes in skin pigmentation, or other noticeable abnormalities.
- Initial Blood Tests: Based on the initial assessment, blood tests are ordered to measure hormone levels. These tests provide a baseline assessment of endocrine function.
- Further Investigations (If Necessary): If initial tests are abnormal or inconclusive, further investigations may be necessary, such as urine tests, imaging studies, or stimulation/suppression tests. These tests help to pinpoint the specific endocrine gland involved and the nature of the problem.
- Diagnosis and Treatment Plan: Once the results of all tests are reviewed and interpreted, a diagnosis is made, and a tailored treatment plan is developed. This plan may include medication, lifestyle changes, surgery, or other interventions.
Interpretation of Test Results and Treatment Decisions
Interpreting test results requires careful consideration of various factors, including the patient’s age, sex, medical history, and the results of other tests. For instance, a slightly elevated TSH level might be insignificant in a young, healthy individual but could indicate hypothyroidism in an older adult. Abnormal test results often lead to further investigations to confirm the diagnosis and rule out other possibilities.
The interpretation of test results is crucial for guiding treatment decisions. For example, high blood glucose levels in a patient with symptoms of diabetes will lead to a diagnosis of diabetes, and treatment will be initiated to manage blood sugar levels. Similarly, low levels of thyroid hormones will lead to a diagnosis of hypothyroidism, requiring hormone replacement therapy.
The specific treatment will be tailored to the individual’s needs and the severity of the disorder.
Treatment of Endocrine Disorders
Endocrine disorders require a multifaceted approach to treatment, often involving a combination of strategies tailored to the specific condition and individual patient needs. The goal is to restore hormonal balance and mitigate the symptoms, improving overall health and quality of life. Treatment options range from simple lifestyle modifications to complex medical interventions.
Medication
Pharmacological interventions form a cornerstone of endocrine disorder management. These medications aim to either supplement deficient hormones, suppress excessive hormone production, or block the effects of hormones. For instance, individuals with hypothyroidism receive synthetic thyroid hormone replacement therapy (levothyroxine), while those with hyperthyroidism may be treated with antithyroid drugs to reduce hormone production. Other medications might target specific hormone receptors or pathways to manage symptoms.
It’s crucial to remember that medication dosages are carefully adjusted based on individual responses and regular monitoring of hormone levels. Potential side effects vary depending on the specific medication but can include nausea, weight changes, and mood alterations. Close collaboration with a healthcare professional is vital for safe and effective medication management.
Lifestyle Changes
Lifestyle modifications play a significant role in managing many endocrine disorders, especially those related to metabolic issues like type 2 diabetes and obesity. Dietary adjustments, emphasizing whole foods, fruits, vegetables, and lean proteins, alongside regular physical activity, can dramatically improve glucose control, weight management, and overall health. Stress reduction techniques, such as yoga or meditation, can also positively influence hormone balance.
For example, maintaining a healthy weight can significantly improve insulin sensitivity in individuals with type 2 diabetes, reducing the need for medication or preventing the onset of the disease altogether. Quitting smoking and limiting alcohol consumption are also crucial components of a healthy lifestyle for individuals with endocrine disorders.
Surgery
In some cases, surgical intervention is necessary to address endocrine disorders. This may involve removing tumors that are causing hormone overproduction (such as in cases of pituitary adenomas or adrenal tumors), correcting anatomical abnormalities, or performing transplants for conditions like type 1 diabetes (although this is still experimental). Surgical procedures carry inherent risks, including bleeding, infection, and potential complications related to the specific surgery.
The decision to pursue surgery is made on a case-by-case basis, considering the severity of the condition, the potential benefits, and the associated risks.
Comparison of Type 1 and Type 2 Diabetes Treatment
The following table compares and contrasts the treatment options for type 1 and type 2 diabetes:
| Treatment Option | Type 1 Diabetes | Type 2 Diabetes | Comments |
|---|---|---|---|
| Insulin Therapy | Essential for survival; administered via injections or pump. | May be required if lifestyle changes and oral medications are insufficient. | Type 1 diabetes requires lifelong insulin replacement because the body does not produce insulin. |
| Oral Medications | Not effective; insulin is required. | Various options available to improve insulin sensitivity or reduce glucose production. | Metformin is a common first-line oral medication for type 2 diabetes. |
| Lifestyle Changes | Important for managing blood glucose levels and preventing complications. | Often the first-line treatment; can delay or prevent the need for medication. | Healthy diet, regular exercise, and weight management are crucial for both types. |
| Surgery | Pancreas transplant (experimental). | Bariatric surgery may be considered for individuals with severe obesity. | Surgical options are less common for diabetes management compared to medication and lifestyle changes. |
Management of Specific Endocrine Disorders and Potential Side Effects
Managing specific endocrine disorders requires a personalized approach, considering the individual’s condition, medical history, and overall health. For example, managing Cushing’s syndrome might involve medication to suppress cortisol production, surgery to remove a tumor, or both. Potential side effects of medications used to treat Cushing’s syndrome include osteoporosis, increased risk of infection, and mood changes. Similarly, managing hypoparathyroidism often involves calcium and vitamin D supplementation, with potential side effects including hypercalcemia (high blood calcium levels).
Each endocrine disorder presents its own unique challenges and treatment strategies, emphasizing the importance of close monitoring and collaboration with a healthcare professional.
Specific Endocrine Disorders
The endocrine system, a complex network of glands and hormones, is vital for maintaining bodily functions. When this system malfunctions, it can lead to a range of disorders, each with unique symptoms, causes, and treatment approaches. Let’s delve into some specific examples to illustrate the diversity and complexity of endocrine diseases.
Understanding endocrine disorders involves exploring a wide range of symptoms, from fatigue to weight changes, stemming from hormonal imbalances. Diagnosing these disorders often requires blood tests and imaging, with treatments varying from medication to lifestyle adjustments. Interestingly, some neurological conditions, like Tourette Syndrome, can sometimes present overlapping symptoms, highlighting the complexity of the human body. For effective management of Tourette Syndrome in children, check out this helpful resource: strategies to manage tourette syndrome in children.
Returning to endocrine disorders, successful treatment hinges on accurate diagnosis and a tailored approach for each individual.
Cushing’s Syndrome
Cushing’s syndrome is a hormonal disorder resulting from prolonged exposure to high levels of cortisol, a steroid hormone. This can stem from various causes, most commonly the overuse of corticosteroid medications, but also from tumors in the pituitary gland (which produces ACTH, stimulating cortisol production), adrenal glands (producing cortisol directly), or other parts of the body producing ACTH. Symptoms of Cushing’s syndrome are diverse and can be subtle initially.
They include weight gain, particularly around the midsection and face (“moon face”), thinning skin that bruises easily, muscle weakness, high blood pressure, fatigue, osteoporosis, and impaired wound healing. Women may experience menstrual irregularities, while men might notice reduced libido and erectile dysfunction. Diagnosis involves a combination of physical examination, blood tests (measuring cortisol levels and ACTH), urine tests (measuring cortisol excretion), and imaging studies (like CT or MRI scans) to locate potential tumors.
Treatment depends on the underlying cause. If it’s medication-induced, the dose can be reduced or the medication changed. Tumors may require surgery, radiation therapy, or medication to suppress their activity.
Understanding endocrine disorders involves exploring their diverse symptoms, underlying causes, diagnostic methods, and available treatments. It’s crucial to remember that certain conditions, like poorly managed diabetes, can significantly increase your risk of serious complications, including stroke. Learning about the risk factors that make stroke more dangerous is vital, as it highlights the importance of proactive healthcare management for endocrine disorders to minimize such risks.
Early diagnosis and treatment of endocrine issues are key to preventing these serious health outcomes.
Addison’s Disease
Addison’s disease, also known as primary adrenal insufficiency, is characterized by the adrenal glands’ inability to produce sufficient cortisol and aldosterone. The pathophysiology involves the destruction of the adrenal cortex, often due to autoimmune diseases (where the body’s immune system attacks the adrenal glands), infections (like tuberculosis), or inherited conditions. Less commonly, it can result from metastatic cancer or hemorrhage into the adrenal glands.The reduced cortisol levels lead to a cascade of effects.
Cortisol plays a crucial role in regulating blood sugar, metabolism, and the body’s response to stress. Its deficiency causes fatigue, weakness, weight loss, low blood pressure, darkening of the skin (hyperpigmentation), and salt craving. Aldosterone deficiency contributes to dehydration, low blood sodium, and high blood potassium, potentially leading to serious cardiovascular complications. Diagnosis involves blood tests measuring cortisol and aldosterone levels, along with a stimulation test (ACTH stimulation test) to assess the adrenal glands’ response to ACTH.
Treatment focuses on hormone replacement therapy, providing synthetic cortisol and aldosterone to compensate for the body’s deficiency. This often involves lifelong medication management. In acute adrenal crisis (a life-threatening situation with severe adrenal insufficiency), immediate intravenous cortisol is crucial.
Endocrine Disorder Comparison Table
The following table summarizes key features of three different endocrine disorders:
| Disorder Name | Key Symptoms | Common Treatments |
|---|---|---|
| Hypothyroidism | Fatigue, weight gain, constipation, cold intolerance, dry skin | Levothyroxine (synthetic thyroid hormone) |
| Hyperthyroidism | Weight loss, nervousness, irritability, heat intolerance, rapid heart rate | Antithyroid medications, radioactive iodine, surgery |
| Diabetes Mellitus (Type 1) | Frequent urination, excessive thirst, unexplained weight loss, fatigue, blurred vision | Insulin injections or pump therapy |
Lifestyle and Prevention

Source: agappe.com
Maintaining a healthy lifestyle plays a crucial role in preventing and managing endocrine disorders. Many of these conditions are influenced by factors within our control, making proactive lifestyle choices a powerful tool in safeguarding endocrine health. By focusing on diet, exercise, and managing other risk factors, individuals can significantly reduce their susceptibility to these disorders.
Diet’s Impact on Endocrine Health
A balanced diet is fundamental to endocrine health. Consuming a diet rich in fruits, vegetables, whole grains, and lean proteins provides the body with essential nutrients necessary for optimal hormone production and regulation. Conversely, a diet high in processed foods, saturated fats, and added sugars can contribute to insulin resistance, weight gain, and an increased risk of conditions like type 2 diabetes and polycystic ovary syndrome (PCOS).
For instance, a diet high in refined carbohydrates leads to rapid spikes in blood sugar, placing a significant burden on the pancreas and potentially leading to insulin resistance. Conversely, a diet rich in fiber, found in whole grains and vegetables, promotes stable blood sugar levels and supports healthy insulin function. Maintaining a healthy weight is also crucial, as obesity is linked to increased risk of several endocrine disorders.
The Role of Exercise in Endocrine Function
Regular physical activity is another cornerstone of endocrine health. Exercise improves insulin sensitivity, helps manage weight, and can reduce inflammation—all factors that positively impact hormone balance. Even moderate exercise, such as a brisk 30-minute walk most days of the week, can yield significant benefits. For example, studies have shown that regular exercise can improve glucose control in individuals with type 2 diabetes and reduce symptoms of PCOS.
The type of exercise is less critical than consistency and finding an activity one enjoys. Whether it’s swimming, cycling, or weight training, the key is to incorporate regular movement into one’s daily routine.
Modifiable Risk Factors for Endocrine Disorders
Several lifestyle factors increase the risk of developing endocrine disorders. These include smoking, excessive alcohol consumption, and chronic stress. Smoking, for example, can negatively impact thyroid hormone production and increase the risk of developing thyroid cancer. Excessive alcohol consumption can disrupt hormone balance and increase the risk of liver damage, impacting hormone production. Chronic stress elevates cortisol levels, potentially leading to long-term health problems including insulin resistance and weight gain.
Addressing these risk factors through lifestyle modifications—quitting smoking, moderating alcohol intake, and practicing stress-reduction techniques such as yoga or meditation—can significantly reduce the risk of developing endocrine disorders. For instance, stress management techniques like mindfulness meditation have been shown to reduce cortisol levels and improve overall well-being.
Final Wrap-Up
Navigating the complexities of endocrine disorders can feel overwhelming, but understanding the basics empowers you to take control of your health. Remember, early symptom recognition is crucial for effective management. This post has provided a broad overview, but always consult with your healthcare provider for personalized advice and treatment. Don’t hesitate to ask questions and advocate for your well-being.
Taking proactive steps towards understanding your body and its intricate workings is a journey worth taking, leading to a healthier and more fulfilling life.
FAQ Resource
Can endocrine disorders be prevented?
While some endocrine disorders have a strong genetic component, many can be mitigated through lifestyle choices. Maintaining a healthy weight, following a balanced diet, exercising regularly, and managing stress can significantly reduce your risk.
How long does it take to diagnose an endocrine disorder?
Diagnosis time varies greatly depending on the specific disorder and the individual’s symptoms. It can range from a few weeks to several months, as it often involves multiple tests and consultations.
Are endocrine disorders curable?
Curability depends on the specific disorder. Some, like Type 1 diabetes, are chronic conditions requiring lifelong management. Others may be treated successfully and the underlying cause resolved.
What are the long-term effects of untreated endocrine disorders?
Untreated endocrine disorders can lead to a wide range of serious health complications, including heart disease, kidney disease, nerve damage, and even death. Early diagnosis and treatment are crucial to minimize these risks.
