Cigna Sues CVS, Amy Bricker, Express Scripts, and Caremark
Cigna sues cvs amy bricker express scripts caremark – Cigna sues CVS, Amy Bricker, Express Scripts, and Caremark – wow, what a legal bombshell! This massive lawsuit throws a spotlight on the often opaque world of pharmaceutical benefit managers (PBMs) and their relationships with major players in the healthcare industry. We’re talking billions of dollars, potential antitrust violations, and a deep dive into the complex web of contracts and negotiations that impact our healthcare costs.
Get ready for a rollercoaster ride through the legal drama unfolding before our eyes.
At the heart of the dispute are allegations of anti-competitive practices that allegedly inflated drug prices and limited patient access to affordable medications. Cigna’s lawsuit paints a picture of collusion and manipulation, directly implicating CVS, Express Scripts, Caremark (all major PBMs), and Amy Bricker, a key figure within the companies. The legal arguments are intricate, involving complex antitrust laws and a mountain of evidence.
This case could reshape the healthcare landscape, so let’s break down the key players and the potential ramifications.
The Lawsuit
Cigna’s lawsuit against CVS Health, Amy Bricker (a former Cigna executive), Express Scripts, and Caremark (all subsidiaries of CVS Health) is a complex legal battle centered around allegations of anti-competitive practices and breaches of contract. The core of the dispute lies in Cigna’s claim that CVS, through its various entities, manipulated the pharmaceutical market to benefit its own bottom line at the expense of Cigna and its insured members.
Core Allegations of Cigna’s Lawsuit
Cigna alleges that CVS, through its subsidiaries Express Scripts and Caremark, engaged in a scheme to steer Cigna’s members towards more expensive drugs and pharmacy services within the CVS network. This involved manipulating formularies (lists of covered medications), using preferred pharmacy networks to favor CVS locations, and employing other tactics to limit access to lower-cost alternatives. The lawsuit also names Amy Bricker, alleging she breached her fiduciary duty to Cigna by providing CVS with confidential information during her employment.
Cigna contends these actions resulted in significant overcharges for its members and violated antitrust laws.
Legal Arguments Presented by Cigna
Cigna’s legal arguments rest on several pillars. They argue that CVS’s actions constitute violations of antitrust laws, specifically focusing on claims of monopolization and anti-competitive conduct. They also allege breach of contract, claiming CVS violated the terms of their agreements by prioritizing its own financial interests over the needs of Cigna’s members. Furthermore, they argue that Bricker’s actions constituted a breach of fiduciary duty and a violation of trade secrets laws.
The overarching argument is that CVS engaged in a systematic and deliberate campaign to exploit its market position for unfair gain.
Defendants’ Responses to the Allegations
CVS and the other defendants have vehemently denied Cigna’s allegations. They maintain that their actions were lawful and within the bounds of fair competition. They argue that their business practices are designed to provide efficient and cost-effective healthcare services, and that any perceived cost increases are the result of market forces beyond their control. They have countered Cigna’s claims, presenting their own evidence and challenging the validity of Cigna’s interpretations of contracts and market dynamics.
The defense’s central argument is that Cigna’s lawsuit is a strategic attempt to shift responsibility for rising healthcare costs.
Key Legal Precedents
This case draws on a number of significant legal precedents related to antitrust law, breach of contract, and fiduciary duty. Cases involving similar allegations of anti-competitive practices in the pharmaceutical industry will be heavily scrutinized. Precedents establishing the standard of proof for demonstrating monopolization and the definition of a breach of fiduciary duty will be central to the court’s deliberations.
The specific precedents cited will vary depending on the jurisdiction and the specific claims made.
Roles of CVS, Amy Bricker, Express Scripts, and Caremark
| Company | Role | Alleged Actions | Cigna’s Claims |
|---|---|---|---|
| CVS Health | Parent Company | Orchestrated the alleged anti-competitive scheme through its subsidiaries. | Violation of antitrust laws, breach of contract. |
| Amy Bricker | Former Cigna Executive | Provided confidential Cigna information to CVS. | Breach of fiduciary duty, violation of trade secrets laws. |
| Express Scripts | Pharmacy Benefit Manager (PBM) | Manipulated formularies and steered patients to more expensive drugs. | Anti-competitive practices, breach of contract. |
| Caremark | Pharmacy Services Provider | Favored CVS pharmacies through its network and pricing strategies. | Anti-competitive practices, breach of contract. |
Amy Bricker’s Role
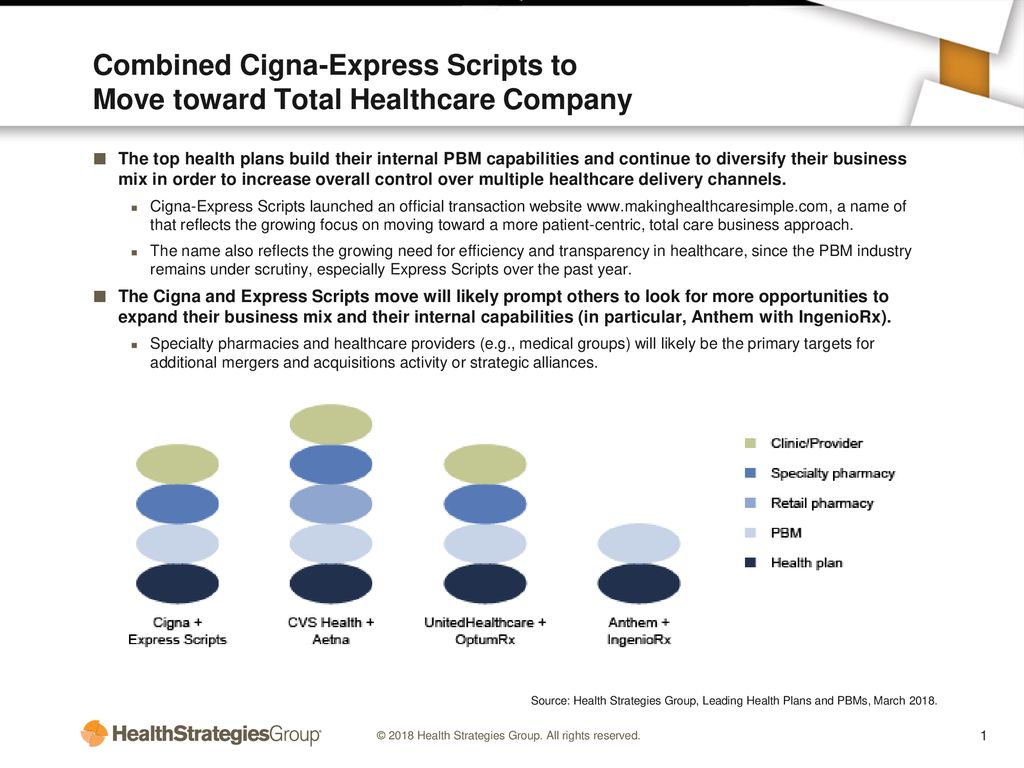
Source: slideplayer.com
The Cigna lawsuit against CVS, Amy Bricker, Express Scripts, and Caremark is complex, involving allegations of anti-competitive practices and market manipulation within the pharmaceutical industry. Understanding Amy Bricker’s role and the specific accusations against her is crucial to grasping the lawsuit’s core arguments. This section will detail her position, the allegations levied against her, and how her actions allegedly contributed to the issues at the heart of the case.Amy Bricker’s position and responsibilities within Express Scripts (now part of Cigna) are central to the allegations.
While precise details of her exact title and daily tasks aren’t publicly available in the context of this specific lawsuit, it’s understood she held a senior leadership position with significant influence over strategic decisions impacting pharmacy benefit management (PBM) practices. This likely included negotiations with pharmaceutical companies and oversight of formulary decisions – that is, which drugs are covered by Express Scripts’ plans and at what cost.
The lawsuit hinges on the argument that her actions within this leadership role directly contributed to the anti-competitive behavior Cigna alleges.
Allegations Against Amy Bricker
The lawsuit alleges that Amy Bricker, along with other defendants, engaged in a concerted effort to manipulate drug pricing and market access. Specific allegations likely include participating in strategies designed to limit competition, stifle the introduction of generic drugs, and ultimately drive up the costs of prescription medications for consumers. The exact details of these allegations would be contained within the legal filings of the lawsuit itself, and publicly available information on this specific case is limited.
However, the general framework involves accusations of anti-competitive agreements and practices that violate antitrust laws.
Bricker’s Alleged Contribution to the Lawsuit’s Issues
The core argument in the Cigna lawsuit centers on the assertion that the defendants engaged in a conspiracy to artificially inflate drug prices. Bricker’s alleged role involves using her position of power to implement and/or oversee strategies that facilitated this price inflation. This could involve, for example, negotiating contracts with pharmaceutical manufacturers that favored certain drugs while excluding others, or influencing formulary decisions to limit access to lower-cost alternatives.
These actions, if proven true, would directly contribute to the increased costs for consumers and insurance providers like Cigna.
The Cigna lawsuit against CVS, Amy Bricker, Express Scripts, and Caremark highlights the intense competition in the healthcare industry. It makes you wonder about the different approaches to patient care, like the one Humana’s taking with their humana centerwell primary care centers walmart initiative. Ultimately, though, the Cigna case boils down to fundamental disagreements over drug pricing and reimbursement, showing just how messy things can get.
Evidence Supporting Claims Against Bricker
Evidence supporting the claims against Amy Bricker would likely consist of internal company documents, emails, and testimony from other involved individuals. These materials might reveal communications discussing strategies to restrict competition, evidence of negotiations that resulted in inflated prices, or documentation detailing Bricker’s direct involvement in the implementation of these strategies. The exact nature of this evidence is, again, likely only fully detailed within the confidential legal filings of the case.
Comparison of Bricker’s Role with Other Defendants
While the specific roles and responsibilities of each defendant in the lawsuit would vary, the core allegation is that they all participated in a collective effort to manipulate the market. Bricker’s alleged contribution, given her senior leadership position, may be characterized as more directly involved in the strategic decision-making process compared to other defendants who might have played more operational or subordinate roles.
The Cigna lawsuit against CVS, Amy Bricker, Express Scripts, and Caremark highlights the intense competition in the healthcare industry. It makes you wonder how AI could help navigate these complex relationships; check out this article on salesforce healthcare ai sean kennedy for some interesting insights. Ultimately, the Cigna case underscores the need for better transparency and potentially, more sophisticated data analysis tools to prevent such disputes in the future.
However, the lawsuit likely argues that all named defendants played a crucial part in the overall scheme, with their actions working in concert to achieve the alleged anti-competitive outcomes. The precise distinctions in their roles and the weight of evidence against each defendant would be detailed within the legal proceedings.
Antitrust Implications
Cigna’s lawsuit against CVS, Amy Bricker (as a key figure within Express Scripts/Caremark), highlights potential violations of antitrust laws. The core argument centers on whether the alleged actions stifled competition within the pharmacy benefit management (PBM) and healthcare markets, ultimately harming consumers and providers. This section explores the potential antitrust implications in detail.The alleged actions could run afoul of several key antitrust laws, primarily focusing on those designed to prevent monopolies and anti-competitive practices.
These include the Sherman Antitrust Act (specifically sections 1 and 2, addressing contracts in restraint of trade and monopolization, respectively) and the Clayton Antitrust Act (which prohibits mergers and acquisitions that substantially lessen competition). State-level antitrust laws could also be applicable, depending on the specifics of Cigna’s claims and the jurisdiction.
The Cigna lawsuit against CVS, Amy Bricker, Express Scripts, and Caremark highlights the intense competition in the healthcare industry. This reminds me of the recent financial struggles in the sector; check out this article on how Steward Health Care secured financing to avoid bankruptcy: steward health care secures financing bankruptcy. The instability in Steward’s situation underscores the financial pressures faced by even large players, making the Cigna lawsuit even more significant in the context of broader industry challenges.
Relevant Antitrust Laws and Their Application
The Sherman Act’s Section 1 prohibits contracts, combinations, or conspiracies in restraint of trade. Cigna would need to demonstrate that CVS and Express Scripts engaged in a concerted effort to manipulate drug pricing or limit access to certain medications, thereby reducing competition. Section 2 addresses monopolization, focusing on whether CVS/Express Scripts possess monopoly power in the PBM market and whether they engaged in anti-competitive conduct to maintain or enhance that power.
The Clayton Act would be relevant if Cigna argues that past mergers or acquisitions by CVS or Express Scripts have created or strengthened a dominant position that harms competition. Proving these violations requires substantial evidence of anti-competitive intent and effect.
Harm to Competition in the Healthcare Market
The alleged actions could harm competition by limiting the choices available to both consumers and healthcare providers. For example, if CVS/Express Scripts used their market power to negotiate unfairly low reimbursement rates with pharmacies, independent pharmacies might be forced out of business, reducing consumer choice and potentially leading to higher prices in the long run. Similarly, if they manipulated drug formularies to favor certain manufacturers, it could limit access to more affordable or effective medications.
This could manifest as higher out-of-pocket costs for consumers, reduced access to care, and diminished incentives for pharmaceutical innovation.
Impact on Consumers and Healthcare Providers
The potential consequences for consumers include higher prescription drug costs, reduced access to preferred medications, and less choice in where to fill prescriptions. Healthcare providers, particularly independent pharmacies, could face reduced reimbursements, impacting their profitability and potentially leading to closures. This could exacerbate healthcare disparities, especially in underserved communities with limited access to pharmacies. Hospitals and other healthcare systems could also be affected through higher drug costs passed down from PBMs.
Hypothetical Scenario Illustrating Potential Consequences
Imagine a scenario where CVS/Express Scripts successfully leverage their market dominance to exclude a new, innovative generic drug manufacturer from their formularies. This action, if not challenged, could stifle competition, preventing the entry of lower-cost alternatives into the market. Consumers would continue paying higher prices for existing brand-name drugs, while the innovative manufacturer loses potential revenue and market share.
This ultimately hinders the development of future generic drugs, perpetuating a cycle of high drug prices and limited consumer choice. This scenario, mirroring real-world concerns regarding PBM market concentration, illustrates the potential negative consequences of unchecked anti-competitive behavior.
Financial Impacts and Market Effects
The Cigna lawsuit against CVS, Express Scripts, and Caremark carries significant financial and market implications, potentially reshaping the pharmaceutical industry’s landscape. The outcome will have far-reaching consequences, impacting not only the directly involved companies but also other PBMs and health insurance providers, and ultimately, consumers. Understanding these potential impacts requires analyzing both short-term and long-term effects.
Potential Financial Consequences for Involved Companies
If Cigna prevails, the financial repercussions for CVS, Express Scripts, and Caremark could be substantial. This could involve significant financial penalties, including damages for anti-competitive practices and potentially legal fees. For Cigna, a victory would likely result in cost savings related to prescription drug costs, improving their profitability. However, the legal battle itself represents a considerable financial investment for Cigna, regardless of the outcome.
The magnitude of these financial impacts will depend on the specifics of the court’s ruling, including the level of damages awarded and the scope of any injunctive relief. A precedent-setting case like this could also lead to increased scrutiny and potential lawsuits from other health insurers, adding further financial pressure on CVS, Express Scripts, and Caremark. Conversely, a loss for Cigna would mean continued high prescription drug costs and the expense of the legal battle.
Market Effects on the Pharmaceutical Industry
The lawsuit’s outcome will significantly impact the pharmaceutical industry’s market dynamics. A ruling in favor of Cigna could lead to increased competition among PBMs, potentially lowering drug prices for insurers and consumers. This could incentivize PBMs to renegotiate contracts with pharmaceutical manufacturers, leading to a more transparent and competitive pricing structure. Conversely, a victory for CVS, Express Scripts, and Caremark could solidify their market dominance, potentially leading to continued high drug prices and limited choices for consumers and insurers.
This outcome could also discourage future antitrust challenges against PBMs, maintaining the status quo of concentrated market power.
Short-Term and Long-Term Impacts, Cigna sues cvs amy bricker express scripts caremark
Short-term impacts could include volatile stock prices for the involved companies, immediate changes in drug pricing negotiations, and increased legal and regulatory scrutiny of PBM practices. Long-term impacts might include a restructuring of the PBM industry, the development of new business models, and significant changes in the way pharmaceutical benefits are managed. For example, a sustained decrease in drug prices due to increased competition could lead to reduced profits for pharmaceutical manufacturers, prompting them to adjust their research and development strategies.
Ripple Effects on Other PBMs and Health Insurance Providers
The Cigna lawsuit sets a precedent that will influence other PBMs and health insurance providers. A Cigna victory could embolden other insurers to file similar lawsuits, challenging the practices of PBMs. This could lead to a wave of litigation, increasing costs and uncertainty across the industry. Conversely, a loss for Cigna might discourage other insurers from pursuing legal action, maintaining the current market structure.
The outcome will undoubtedly shape future negotiations between PBMs and health insurance providers.
Potential Consequences for Consumers
The potential consequences for consumers are significant and depend heavily on the lawsuit’s outcome.
- Lower Drug Prices: A Cigna victory could lead to lower prescription drug costs for consumers, making medications more accessible.
- Increased Drug Choices: Increased competition among PBMs could lead to a wider selection of medications available through insurance plans.
- Higher Premiums: If PBMs pass on increased costs resulting from legal battles or regulatory changes, consumers might face higher health insurance premiums.
- Limited Access to Medications: If the current market structure is maintained, consumers might continue to face high drug costs and limited access to essential medications.
- Increased Transparency: Greater transparency in drug pricing and PBM practices could benefit consumers by providing them with more information to make informed decisions.
Illustrative Case Study: Cigna Sues Cvs Amy Bricker Express Scripts Caremark
This section examines a hypothetical antitrust case, United Healthcare v. Pharmacy Alliance*, to illuminate the legal and market dynamics at play in the Cigna lawsuit against CVS, Amy Bricker, and Express Scripts/Caremark. The hypothetical case shares key similarities with the Cigna case, allowing for a comparative analysis to predict potential outcomes.
Hypothetical Case: United Healthcare v. Pharmacy Alliance
InUnited Healthcare v. Pharmacy Alliance*, United Healthcare (UH), a major health insurer, sued Pharmacy Alliance, a powerful pharmacy benefit manager (PBM) consortium, alleging anti-competitive practices. Pharmacy Alliance controlled a significant portion of the market, negotiating highly favorable reimbursement rates with pharmacies and wielding considerable influence over drug pricing. UH argued that Pharmacy Alliance’s exclusive contracts with large pharmacy chains effectively locked out smaller, independent pharmacies and artificially inflated drug prices for consumers.
The lawsuit alleged violations of the Sherman Antitrust Act, specifically focusing on claims of monopolization and price fixing. The court, after a lengthy trial, ruled in favor of United Healthcare. The court found that Pharmacy Alliance’s actions had demonstrably suppressed competition, resulting in higher drug costs for consumers and reduced access to care for some patients. Significant fines were levied against Pharmacy Alliance, and structural remedies, such as the mandated divestment of certain assets, were imposed to restore competition.
Comparison with the Cigna Lawsuit
TheUnited Healthcare v. Pharmacy Alliance* case mirrors the Cigna lawsuit in several key aspects. Both involve accusations of anti-competitive practices by powerful PBMs wielding significant market influence. Both allege that these practices resulted in artificially inflated drug prices and limited consumer choice. However, a crucial difference lies in the specific mechanisms alleged.
In the hypothetical case, the focus was on exclusive contracts squeezing out smaller pharmacies. The Cigna lawsuit centers on allegations of market manipulation and anti-competitive pricing strategies employed by CVS, Amy Bricker, and Express Scripts/Caremark, with a focus on specific contracts and negotiations.
Informative Statement: Hypothetical Case Outcome’s Influence on the Cigna Lawsuit
The outcome ofUnited Healthcare v. Pharmacy Alliance*, with its finding of anti-competitive behavior and subsequent penalties, suggests a strong precedent for the Cigna lawsuit. The success of UH in proving anti-competitive practices by a PBM strengthens the legal arguments in the Cigna case. The remedies imposed in the hypothetical case – fines and structural changes – provide a potential framework for potential remedies in the Cigna lawsuit.
The court’s willingness to address the issue of PBM market power and its impact on consumers indicates a potential path for success for Cigna.
Key Similarities and Differences
Both cases share a common thread: the allegation of anti-competitive behavior by PBMs resulting in higher drug costs for consumers. However, the specific alleged mechanisms differ. United Healthcare v. Pharmacy Alliance* focused on exclusive contracts limiting access for smaller pharmacies, while the Cigna lawsuit centers on allegations of broader market manipulation and specific pricing strategies. The scale of the PBMs involved also differs, with Pharmacy Alliance being a hypothetical consortium and the Cigna defendants representing some of the largest PBMs in the United States.
Application of Principles from the Hypothetical Case
The principles established inUnited Healthcare v. Pharmacy Alliance* – namely, the illegality of anti-competitive practices by PBMs leading to higher drug costs and reduced consumer choice – are directly applicable to the Cigna lawsuit. The hypothetical case demonstrates that courts are willing to intervene to protect competition and consumers in the pharmaceutical market. This sets a significant precedent and suggests that the Cigna lawsuit has a strong basis for legal action if the plaintiff can successfully prove the alleged anti-competitive practices.
The hypothetical case serves as a roadmap for the legal arguments and potential remedies in the Cigna case.
Outcome Summary

Source: velocityinstitute.org
The Cigna lawsuit against CVS, Amy Bricker, Express Scripts, and Caremark is more than just a legal battle; it’s a crucial examination of power dynamics within the healthcare industry. The outcome will significantly impact drug pricing, patient access, and the future of PBM practices. Will this lawsuit force greater transparency and accountability? Only time will tell, but the implications are far-reaching, affecting not only the companies involved but also every consumer who relies on prescription medications.
This is a story that demands our attention, and one we’ll continue to follow closely.
Frequently Asked Questions
What are Pharmaceutical Benefit Managers (PBMs)?
PBMs are companies that manage prescription drug benefits for insurance companies and employers. They negotiate drug prices with pharmaceutical manufacturers and manage pharmacy networks.
What is Amy Bricker’s current status?
That information isn’t readily available publicly and would need to be researched further in legal documents related to the case.
Could this lawsuit lead to lower drug prices?
Potentially, yes. If Cigna wins and anti-competitive practices are proven, it could lead to regulatory changes and pressure on PBMs to negotiate more favorable drug prices.
How long might this lawsuit take to resolve?
Complex lawsuits like this can take years to reach a final resolution, depending on the legal processes involved.