CityMD COVID Settlement DOJ False Claims, Walgreens
Citymd covid settlement doj false claims walgreens – CityMD COVID settlement, DOJ false claims, and Walgreens’ involvement – it sounds like a plot from a legal thriller, doesn’t it? This massive case revolves around allegations of fraudulent billing practices related to COVID-19 testing and treatment. The Department of Justice (DOJ) accused CityMD, a large urgent care provider, of submitting false claims for reimbursement, potentially involving their partnership with Walgreens.
This investigation delves into the specifics of the allegations, the potential penalties, and the wider implications for healthcare billing transparency. Let’s unpack this complex story together.
The core issue centers around whether CityMD and Walgreens knowingly submitted inaccurate billing information to government programs for COVID-19 services. The DOJ’s lawsuit details alleged schemes involving improper testing and billing practices, potentially costing taxpayers millions. Understanding the specifics of the False Claims Act, the evidence presented, and the potential ramifications for both CityMD and Walgreens is crucial to grasping the gravity of this situation.
We’ll also explore the impact on patients and the broader healthcare system, looking at what changes might prevent similar scandals in the future.
CityMD’s Role in the COVID-19 Testing and Treatment Landscape
CityMD, a prominent urgent care provider in the New York metropolitan area and beyond, found itself thrust into the forefront of the COVID-19 pandemic response. Its pre-existing network of conveniently located clinics, coupled with its established infrastructure for handling high patient volumes, positioned it to play a significant role in the nation’s fight against the virus. Understanding CityMD’s actions during this period requires examining its operations before, during, and after the pandemic’s peak.CityMD’s operations prior to the pandemic centered around providing walk-in urgent care services for a wide range of non-life-threatening medical issues.
They held a substantial market share within their geographic areas, known for their accessibility and relatively short wait times. Their pre-existing infrastructure, including electronic health records and established billing systems, proved unexpectedly crucial in their rapid adaptation to the COVID-19 crisis.
CityMD’s Response to Increased COVID-19 Testing Demand
The rapid spread of COVID-19 created an unprecedented surge in demand for testing and treatment. CityMD responded by quickly adapting its operations to prioritize COVID-19 testing and care. This involved implementing new protocols, including drive-through testing sites and dedicated COVID-19 clinics to minimize the risk of cross-contamination. They also invested heavily in acquiring sufficient testing supplies, a challenge many healthcare providers faced during the initial stages of the pandemic.
The scale of their response involved significant increases in staffing, training, and logistical coordination. Their ability to rapidly scale operations in response to the crisis highlights their operational flexibility and responsiveness.
CityMD’s Billing Practices for COVID-19 Related Services
CityMD’s billing practices for COVID-19-related services were, like those of many healthcare providers, subject to significant scrutiny during and after the pandemic. They billed insurance companies and patients for testing, treatment, and related services according to established codes and procedures. The specifics of their billing practices and the accuracy of their claims became a central point of contention in the Department of Justice settlement.
The DOJ’s allegations focused on issues of improper billing and potential overcharging for services, resulting in a substantial financial settlement. A detailed examination of the specific billing practices and their compliance with regulations is necessary for a complete understanding of the situation.
Comparison of CityMD’s COVID-19 Protocols with Other Providers
CityMD’s approach to COVID-19 testing and treatment can be compared to that of other providers, both large and small. Some providers, like large hospital systems, may have had greater resources available for testing and treatment, potentially offering a wider range of services. Others, such as smaller clinics, may have faced greater challenges in securing testing supplies and managing increased patient volume.
A comprehensive comparison would require analyzing various factors, including access to resources, staffing levels, geographic location, and the specific types of services offered. The DOJ settlement highlights the complexities involved in ensuring accurate billing and compliance with regulations across the healthcare industry. It serves as a case study for the challenges faced by healthcare providers during public health crises and the importance of transparency and accountability in billing practices.
The Department of Justice’s Allegations Against CityMD
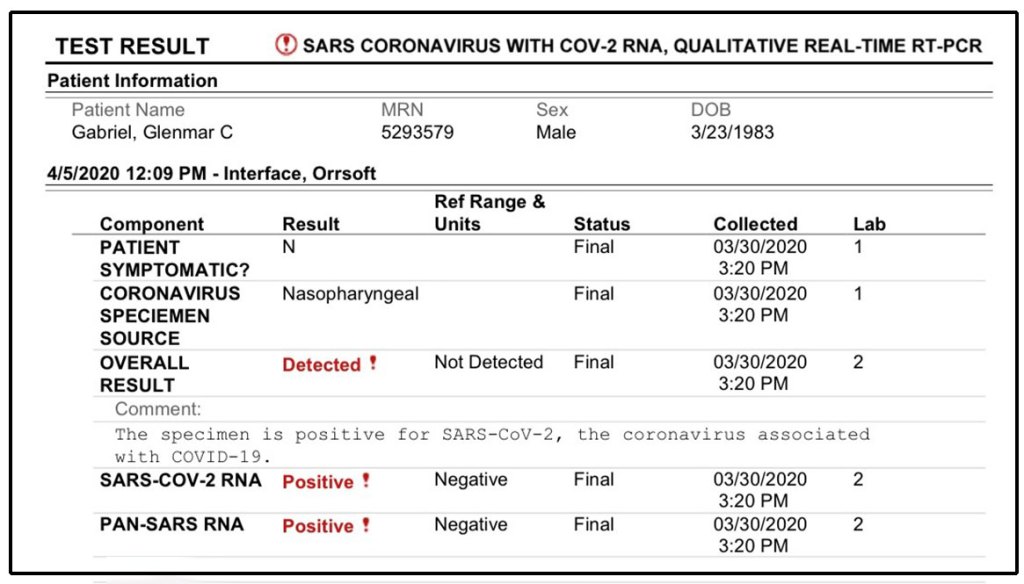
Source: nbcdfw.com
The Department of Justice (DOJ) filed a lawsuit against CityMD, alleging widespread fraud related to their COVID-19 testing and billing practices. The core of the DOJ’s case centers on accusations that CityMD knowingly submitted false claims to government healthcare programs, primarily Medicare and Medicaid, for tests and treatments that were either unnecessary, improperly coded, or not actually performed. This resulted in significant overbilling to the federal government.The DOJ’s lawsuit detailed a pattern of alleged fraudulent activity, painting a picture of a system designed to maximize profits at the expense of taxpayer dollars.
The allegations involved not just isolated incidents but a systemic approach, encompassing numerous CityMD locations and a significant period of time. The consequences of such actions are severe, potentially leading to substantial financial penalties and reputational damage for the company.
False Claims Act Violations Alleged by the DOJ
The DOJ’s lawsuit cited violations of the False Claims Act (FCA), a powerful federal law designed to combat fraud against the government. Specifically, the DOJ alleged that CityMD knowingly submitted false claims for reimbursement, violating the FCA’s prohibition against knowingly presenting false or fraudulent claims for payment. The allegations include submitting claims for tests that were not medically necessary, billing for more expensive tests than were actually performed, and upcoding services to receive higher reimbursements.
These actions, according to the DOJ, constituted a deliberate attempt to defraud the government.
The CityMD COVID settlement with the DOJ over false claims, and similar issues with Walgreens, highlights the urgent need for accessible and reliable healthcare. Reading about Monali Thakur’s hospitalization after struggling to breathe, as detailed in this article monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases , really brought home the devastating impact of respiratory illnesses.
It makes you wonder how much better preventative care could have mitigated situations like the CityMD scandal, where inadequate testing potentially contributed to the spread of illness.
Evidence Presented by the DOJ
The DOJ’s complaint detailed a range of evidence supporting their allegations. This included internal CityMD documents, such as emails and billing records, which allegedly revealed a culture that prioritized revenue over patient care. The DOJ also cited statistical analyses showing discrepancies between the volume of tests performed at certain CityMD locations and the typical rates for similar facilities.
Furthermore, whistleblower testimony likely played a significant role, providing firsthand accounts of alleged fraudulent practices within the company. The specific details of the evidence remain largely under seal, but the lawsuit clearly suggests a substantial body of evidence supporting the DOJ’s claims.
Potential Financial Penalties for CityMD
The potential financial penalties facing CityMD are substantial. Under the FCA, the government can recover treble damages (three times the amount of the false claims) plus civil penalties for each violation. Given the scale of the alleged fraud, the potential liability could run into hundreds of millions of dollars. Furthermore, CityMD could face significant legal fees and reputational damage, potentially impacting its future business prospects.
The final penalty will depend on the outcome of the legal proceedings, but the sheer volume of alleged false claims suggests a considerable financial risk for the company. For example, a similar case involving a large healthcare provider resulted in a settlement exceeding $100 million, providing a benchmark for the potential financial ramifications CityMD might face.
Walgreens’ Involvement in the Alleged Scheme

Source: cnn.com
The Department of Justice’s settlement with CityMD implicated Walgreens, highlighting a concerning partnership that allegedly facilitated fraudulent billing practices related to COVID-19 testing and treatment. Understanding Walgreens’ role requires examining their relationship with CityMD, the nature of their alleged involvement in the scheme, and the evidence presented by the DOJ.Walgreens’ relationship with CityMD during the relevant period involved the operation of CityMD testing sites within Walgreens stores.
This co-location provided CityMD with access to Walgreens’ infrastructure and potentially a wider patient base. This close proximity and operational integration created an environment where allegedly fraudulent billing practices could more easily occur, with Walgreens potentially benefiting from increased foot traffic to their stores.
The CityMD COVID settlement with the DOJ over false claims, alongside similar issues with Walgreens, highlights the importance of accurate medical billing and patient care. It makes you wonder about preventative health measures, and I was surprised to learn that, according to this article, can eye test detect dementia risk in older adults. This kind of early detection could save significant healthcare costs in the long run, contrasting sharply with the financial repercussions seen in the CityMD and Walgreens cases.
Walgreens’ Role in Alleged Fraudulent Billing
The DOJ’s allegations suggest that Walgreens’ role extended beyond simply providing space. The complaint implied that the improper billing practices, including upcoding and unnecessary testing, occurred within Walgreens locations. While the settlement did not explicitly state Walgreens was directly involved in the decision-making regarding billing practices, the physical location of the fraudulent activity within Walgreens stores and the partnership’s structure raise questions about the level of oversight and awareness on Walgreens’ part.
The proximity of Walgreens employees to CityMD’s operations necessitates a closer look at their potential knowledge of, or complicity in, the fraudulent activities.
Evidence Linking Walgreens to the Scheme
Direct evidence explicitly linking Walgreens to the fraudulent scheme might be limited in publicly available information from the DOJ settlement. However, the fact that the alleged fraudulent billing occurred within Walgreens stores constitutes circumstantial evidence. The DOJ’s investigation likely focused on financial transactions and communication records to establish the connection between CityMD’s actions and the Walgreens’ role in providing the physical location and infrastructure that facilitated the alleged scheme.
The sheer volume of fraudulent claims originating from Walgreens-based CityMD locations could be significant evidence.
Comparison with Walgreens’ Corporate Compliance Policies
Walgreens maintains a robust corporate compliance program designed to prevent and detect fraud and abuse. This program typically includes policies on provider relationships, billing practices, and internal controls. The allegations against CityMD raise questions about the effectiveness of Walgreens’ compliance program in preventing or detecting fraudulent activity within their stores. A thorough internal review of their oversight mechanisms related to the CityMD partnership would be necessary to determine if the program’s procedures were adequately followed and if any weaknesses in the system allowed the alleged fraudulent activities to occur.
A comparison of the alleged actions with Walgreens’ published compliance policies would reveal any discrepancies and potential areas for improvement in their internal controls and oversight procedures.
The False Claims Act and its Applicability
The False Claims Act (FCA) is a powerful tool used by the federal government to combat fraud against the government. It allows the government, and private citizens acting as whistleblowers (qui tam actions), to sue individuals or entities who knowingly submit false or fraudulent claims for payment to federal healthcare programs, including Medicare and Medicaid. The purpose is to protect taxpayer dollars and ensure the integrity of government programs.The FCA imposes significant penalties on those found liable, including treble damages (three times the amount of the false claims) plus civil penalties.
This substantial financial risk acts as a strong deterrent against fraudulent activities.
Elements of a False Claims Act Violation
To successfully prove a violation of the FCA, the government must demonstrate several key elements. First, a false claim must have been submitted to the government. This claim must be material, meaning it had the potential to influence the government’s decision to pay. Third, the defendant must have acted knowingly, which encompasses a range of culpability, from actual knowledge to reckless disregard for the truth or deliberate ignorance.
Finally, the false claim must have resulted in the government making a payment.
Potential Defenses for CityMD and Walgreens
CityMD and Walgreens, facing allegations under the FCA, could potentially raise several defenses. They might argue that the claims submitted were not false, perhaps contesting the accuracy of the government’s interpretation of the billing practices or the nature of the services provided. They could also challenge the materiality of any alleged misrepresentations, arguing that even if inaccuracies existed, they didn’t influence the government’s payment decisions.
The CityMD COVID settlement with the DOJ over false claims, alongside similar Walgreens issues, highlights the importance of accurate healthcare data. This is especially crucial when considering the severity of conditions like stroke; understanding the risk factors that make stroke more dangerous is vital for preventative care. Ultimately, the CityMD case underscores the need for transparency and accountability in healthcare, impacting even our understanding of stroke risk factors and effective treatment.
Another potential defense would be to dispute the “knowing” element, claiming that any errors were unintentional, made in good faith, or due to a reasonable misunderstanding of the applicable regulations. Finally, they might attempt to demonstrate that they implemented robust compliance programs to prevent fraud, mitigating their culpability.
Key Legal Precedents Related to False Claims Act Violations in Healthcare
The following table summarizes some key legal precedents that provide context for understanding FCA violations in healthcare and their potential relevance to the CityMD/Walgreens case. Note that the specific facts and circumstances of each case are crucial in determining its applicability to the current situation.
| Case Name | Court | Key Findings | Relevance to CityMD/Walgreens case |
|---|---|---|---|
| United States ex rel. Escobar v. Universal Health Services, Inc. | Supreme Court | Materiality standard clarified; a claim is material if it has a tendency to influence the government’s payment decision. | This case sets the standard for materiality, a crucial element in the government’s case against CityMD and Walgreens. The court’s definition of materiality will be heavily scrutinized. |
| United States v. AseraCare, Inc. | 11th Circuit | Affirmed that a defendant’s subjective belief in the legality of their actions is not a defense to FCA liability. | This highlights the importance of objective compliance with regulations, regardless of the defendant’s internal understanding of the rules. CityMD and Walgreens’ internal policies and training will be examined. |
| United States ex rel. Druding v. Care Alternatives | 3rd Circuit | Addresses the issue of “knowing” conduct in the context of hospice billing practices. | This case provides guidance on what constitutes “knowing” conduct in the healthcare setting, which is central to the government’s case against CityMD and Walgreens. The court’s interpretation of “knowing” conduct could significantly impact the outcome. |
| United States ex rel. Michaels v. Agape Senior Care, Inc. | 11th Circuit | The court addressed the issue of materiality and knowledge in the context of improper billing practices. | This case offers another perspective on materiality and knowledge in healthcare billing, providing further context for evaluating the government’s claims against CityMD and Walgreens. The court’s analysis of the defendant’s knowledge and intent will be relevant. |
Impact on Patients and the Healthcare System
The CityMD and Walgreens settlement regarding allegedly fraudulent COVID-19 billing practices raises serious concerns about the impact on patients and the broader healthcare system. The alleged scheme, involving unnecessary tests and inflated billing, not only defrauded government programs but also potentially harmed patients through unnecessary medical procedures and increased financial burdens. Understanding these impacts is crucial for reforming healthcare billing practices and ensuring patient trust.The potential impact on patients is multifaceted.
First, patients may have undergone unnecessary medical procedures, potentially exposing them to risks associated with those procedures without receiving any commensurate medical benefit. Secondly, patients might have faced unexpected and significant out-of-pocket costs due to inflated billing practices, even with insurance coverage. This could lead to financial hardship for some individuals and families, particularly those already struggling financially.
Finally, the erosion of trust in healthcare providers due to fraudulent billing practices undermines the patient-provider relationship, hindering access to quality care and leading to reluctance to seek timely medical attention in the future.
Financial Burden on Patients
The inflated billing practices allegedly employed by CityMD and Walgreens directly translated to increased costs for patients. Even with insurance, patients might have been left with higher co-pays, deductibles, or out-of-pocket maximums than they should have been. For example, a patient who underwent unnecessary testing might have been billed several hundred dollars more than necessary, a significant sum for many individuals.
This financial burden can disproportionately affect low-income patients, potentially delaying or preventing them from seeking essential medical care in the future. The lack of transparency in billing further exacerbates this issue, leaving patients unaware of the true cost of their care until after the fact.
Erosion of Trust in the Healthcare System
The allegations against CityMD and Walgreens severely damage public trust in the healthcare system. When large healthcare providers engage in fraudulent billing, it fuels cynicism and distrust, leading patients to question the integrity and motivations of medical professionals. This erosion of trust can have far-reaching consequences, discouraging patients from seeking necessary care, delaying diagnosis and treatment of serious conditions, and ultimately harming public health.
Restoring public trust requires transparency, accountability, and meaningful reforms to ensure that patients can rely on their healthcare providers to act ethically and in their best interests.
Potential Healthcare Reforms, Citymd covid settlement doj false claims walgreens
Preventing future instances of fraudulent billing requires a multi-pronged approach. Strengthening oversight and enforcement of existing regulations is paramount. This includes increased audits and investigations of healthcare providers’ billing practices, stricter penalties for fraud, and improved data analysis to detect patterns of potentially fraudulent activity. Additionally, promoting transparency in healthcare billing is crucial. Patients should have easier access to understandable explanations of their bills, with clear breakdowns of services rendered and associated costs.
This transparency can empower patients to identify potential billing errors or irregularities and challenge them effectively. Furthermore, improving provider education on billing compliance and ethical practices can contribute to a culture of accountability and integrity within the healthcare industry. Investing in technology that streamlines billing processes and reduces opportunities for fraud is also necessary.
Public Service Announcement: Billing Transparency in COVID-19 Testing
[Imagine a public service announcement featuring a calm, reassuring voiceover accompanied by simple, clear graphics showing a doctor and a patient discussing a bill. The graphics emphasize key information like itemized bills, contact information for billing inquiries, and resources for patients who suspect billing errors.]The voiceover states: “Were you tested for COVID-19? Understand your bill. Ask questions if anything is unclear.
Your healthcare provider should provide a detailed explanation of all charges. If you suspect billing errors or fraudulent activity, contact your insurance company or the appropriate regulatory authorities. Don’t hesitate to advocate for yourself and ensure you are being billed fairly. Your health and your finances matter.”
Financial Implications and Settlements
The Department of Justice’s allegations against CityMD and Walgreens for allegedly submitting false claims related to COVID-19 testing and treatment carry significant financial ramifications. The potential penalties, both monetary and reputational, are substantial and will depend on several factors, including the extent of the fraudulent activity, the level of culpability, and the willingness of the companies to cooperate with the investigation.
Understanding the potential financial consequences is crucial to grasping the full impact of this case.The potential financial consequences for CityMD and Walgreens could be devastating. If found liable under the False Claims Act, they face substantial fines, potentially reaching millions or even billions of dollars, depending on the number of false claims submitted and the amount of government funds involved.
Beyond the direct financial penalties, both companies risk significant reputational damage, potentially impacting future contracts, investor confidence, and patient trust. Long-term effects could include decreased market share, increased regulatory scrutiny, and difficulty attracting and retaining talent.
Potential Fines and Penalties
The size of any potential settlement will depend on a number of factors. The government will consider the number of false claims submitted, the amount of money fraudulently obtained, the degree of intent to defraud, and the level of cooperation from the companies during the investigation. A history of similar violations could also significantly increase the penalties. Furthermore, the government’s legal strategy, the strength of the evidence, and the negotiating positions of all parties involved will play a critical role in determining the final settlement amount.
Settlements in similar False Claims Act cases have ranged from hundreds of thousands to billions of dollars, demonstrating the wide spectrum of possible outcomes.
Examples of Similar Settlements
Numerous past False Claims Act cases offer insights into the potential financial consequences for CityMD and Walgreens. For example, the settlement between the United States and GlaxoSmithKline in 2012 resulted in a $3 billion payment to resolve allegations of illegal promotion of certain drugs. Similarly, the settlement between the United States and Abbott Laboratories in 2010 involved a $1.5 billion payment to resolve allegations of off-label marketing and other fraudulent activities.
These cases highlight the significant financial risks associated with violations of the False Claims Act.
Financial Implications Comparison
The following table compares the potential financial implications for CityMD, Walgreens, and the government:
| Entity | Potential Fines | Reputational Damage | Long-Term Effects |
|---|---|---|---|
| CityMD | Millions to hundreds of millions of dollars (depending on the extent of the alleged fraud) | Significant damage to brand reputation, potentially impacting patient trust and future business opportunities. | Possible loss of market share, increased regulatory scrutiny, and difficulty attracting and retaining talent. |
| Walgreens | Millions to billions of dollars (given their larger size and potential involvement) | Significant damage to brand reputation, affecting investor confidence and business relationships. | Potential loss of market share, increased regulatory scrutiny, and potential legal ramifications extending beyond the immediate settlement. |
| Government | Recovery of fraudulently obtained funds, plus additional penalties. | Improved public trust through enforcement of healthcare regulations. | Strengthened oversight mechanisms to prevent future fraudulent activities. |
Last Point
The CityMD and Walgreens case serves as a stark reminder of the importance of transparency and ethical practices within the healthcare industry. The potential financial penalties and reputational damage are substantial, highlighting the serious consequences of fraudulent billing. While the specifics of the settlement remain to be seen, this case underscores the need for robust oversight and increased accountability to protect both patients and the integrity of our healthcare system.
The ongoing fallout from this case will likely influence future billing practices and regulatory measures, hopefully leading to greater transparency and patient protection.
FAQ: Citymd Covid Settlement Doj False Claims Walgreens
What is the False Claims Act?
The False Claims Act is a U.S. law that allows the government to recover money from individuals or companies who knowingly submit false or fraudulent claims for payment to federal healthcare programs.
What role did Walgreens play?
The DOJ alleges Walgreens was involved in the fraudulent billing scheme, although the exact nature of their involvement is still under investigation.
What are the potential consequences for CityMD and Walgreens?
Potential consequences include substantial fines, reputational damage, and potential exclusion from government healthcare programs.
How might this affect patients?
Patients may experience increased scrutiny of their billing information and potentially higher costs for future healthcare services as providers adjust to stricter regulations.