Congress Healthcare Hearings Medicare, PBMs, Hospitals
Congress healthcare hearings medicare advantage pbms hospitals – the very phrase conjures images of intense debate, powerful lobbying, and the very real impact on millions of Americans. These hearings are a crucial battleground where the future of healthcare access and affordability is being fought. We’re diving deep into the complexities of Medicare Advantage plans, the often-opaque role of Pharmaceutical Benefit Managers (PBMs), and the crucial role hospitals play in this intricate system.
Expect to uncover potential conflicts of interest, surprising cost drivers, and the ongoing struggle to balance patient care with budgetary constraints. This is a story about power, politics, and the very real consequences for those relying on Medicare.
This post will break down the key issues raised in recent congressional hearings, exploring the criticisms leveled against Medicare Advantage, the influence of PBMs on drug pricing, and the financial incentives shaping hospital participation. We’ll examine the potential impact on patient access and healthcare costs, and delve into proposed legislative solutions. Get ready for a comprehensive overview of a system desperately needing reform.
Medicare Advantage Plans & Congressional Hearings
Medicare Advantage (MA) plans have become a significant point of contention in recent years, sparking numerous congressional hearings and raising concerns about their effectiveness and fairness. These plans, an alternative to Original Medicare, offer a different way for seniors to access healthcare coverage, but their complexities and potential pitfalls have drawn considerable scrutiny. Understanding the structure, function, and criticisms surrounding MA plans is crucial for anyone involved in or affected by the healthcare system.
Medicare Advantage Plan Structure and Function
Medicare Advantage plans are offered by private insurance companies that contract with Medicare to provide Part A (hospital insurance) and Part B (medical insurance) benefits. Instead of receiving these benefits directly from Medicare, beneficiaries enroll in an MA plan, which typically bundles these benefits with additional coverage, such as prescription drugs (Part D), vision, hearing, and dental. These plans operate under a capitated payment system, meaning the insurance company receives a fixed amount per enrollee per month from Medicare, regardless of the actual healthcare services used.
This incentivizes cost-containment strategies, but also raises concerns about potential limitations on access to care. The structure involves a complex interplay between Medicare, the private insurance companies, and the beneficiaries themselves, making oversight and regulation challenging.
Key Issues Raised in Congressional Hearings Regarding Medicare Advantage
Recent congressional hearings have focused on several key issues surrounding Medicare Advantage plans. One major concern is the practice of “upcoding,” where providers bill for more expensive services than were actually rendered. This inflates the costs paid by Medicare, ultimately affecting taxpayer dollars. Another critical area of investigation has been the restrictive network of providers often associated with MA plans.
Beneficiaries may find that their preferred doctors or specialists are not included in the plan’s network, limiting their access to care. Furthermore, concerns have been raised about the marketing practices of some MA plans, with allegations of misleading or confusing information provided to potential enrollees. The lack of transparency regarding plan performance and cost-effectiveness has also been a significant point of debate.
The recent Congress healthcare hearings on Medicare Advantage, PBMs, and hospitals got me thinking about overall health. It’s crucial to consider preventative care, and that’s where nutrition plays a huge role. I was reading this fascinating article about dietary differences between the sexes – are women and men receptive of different types of food and game changing superfoods for women – which highlights how individual needs can impact healthcare costs long-term.
Understanding these nuances could inform better healthcare policy decisions regarding the very issues being debated in those hearings.
Finally, the complexities of navigating the MA system, particularly for beneficiaries with limited health literacy, have been highlighted as a major challenge.
Comparison of Different Types of Medicare Advantage Plans
Several types of Medicare Advantage plans exist, each with its own features and coverage options. HMO (Health Maintenance Organization) plans typically require beneficiaries to select a primary care physician (PCP) and obtain referrals for specialist care. PPO (Preferred Provider Organization) plans offer more flexibility, allowing beneficiaries to see specialists without referrals, but usually at a higher cost if they go outside the network.
POS (Point of Service) plans combine features of both HMO and PPO plans, offering a balance between cost and flexibility. Special Needs Plans (SNPs) cater to specific populations, such as those with chronic conditions or those residing in specific geographic areas. The choice of plan depends heavily on individual health needs, preferences for flexibility, and budget considerations. The coverage offered by each plan type varies considerably, affecting both the cost-sharing and the range of services available to the enrollee.
Criticisms of Medicare Advantage Plans
| Criticism | Source | Impact | Proposed Solutions |
|---|---|---|---|
| Upcoding and inflated billing | Government Accountability Office (GAO) reports, Congressional hearings | Increased Medicare costs, potential for fraud | Increased audits and stricter enforcement of billing practices, improved data analysis to detect anomalies. |
| Restrictive provider networks | Beneficiary testimonials, patient advocacy groups | Limited access to care, reduced choice of providers | Regulations to ensure adequate network adequacy, increased transparency regarding network composition. |
| Misleading marketing practices | Consumer complaints, state insurance departments | Enrollee confusion, inappropriate plan selection | Stricter regulations on marketing materials, improved consumer education and resources. |
| Lack of transparency and accountability | Congressional reports, academic research | Difficulty in comparing plans, limited ability to assess value | Improved data reporting requirements, standardized plan comparison tools, increased public access to performance data. |
Pharmaceutical Benefit Managers (PBMs) and Their Role
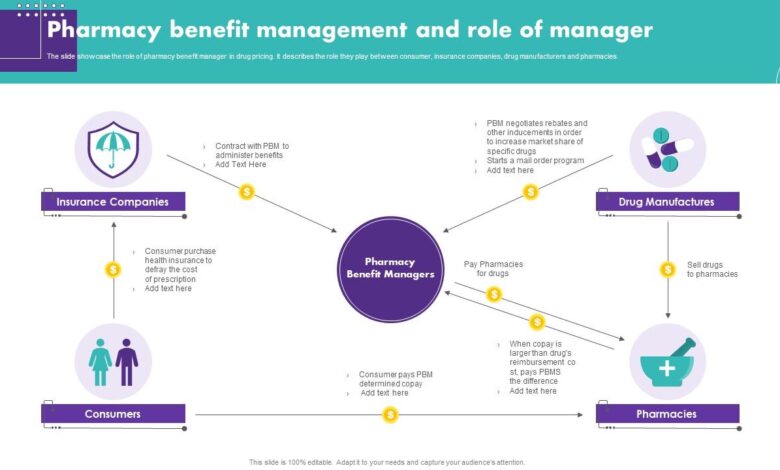
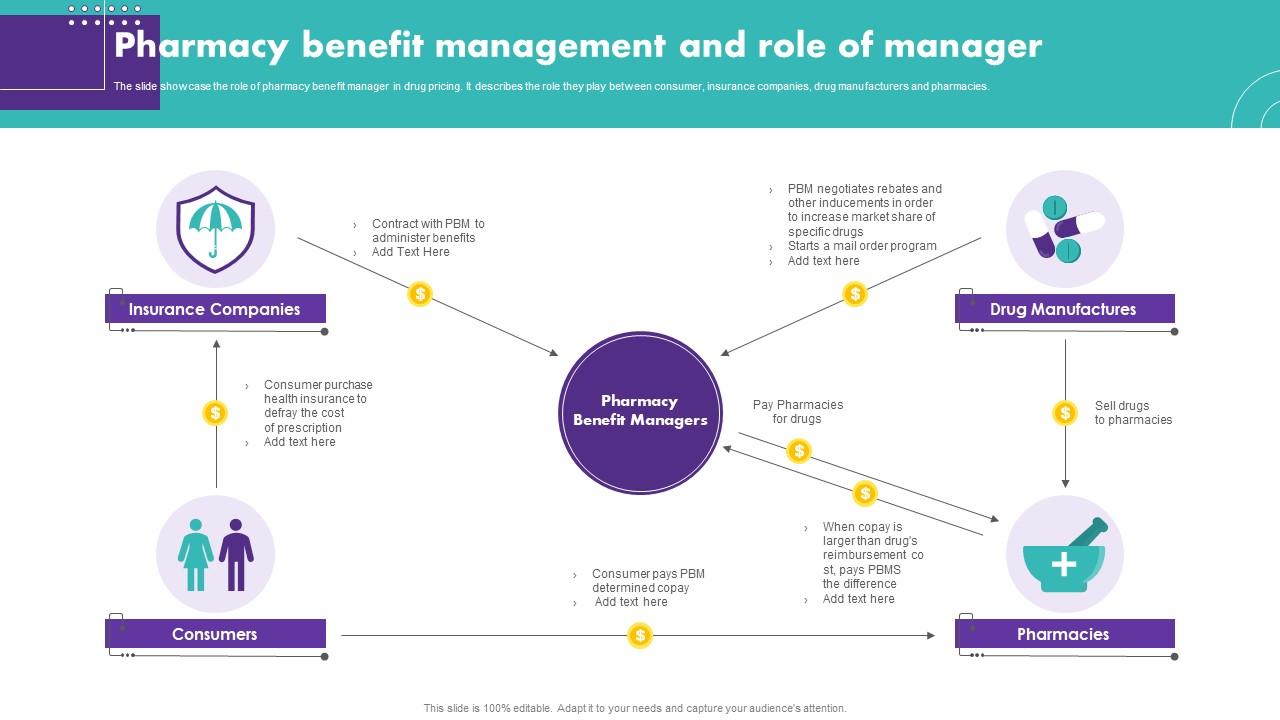
Pharmaceutical Benefit Managers (PBMs) are middlemen in the prescription drug supply chain, acting as intermediaries between pharmaceutical manufacturers, health insurance plans (including Medicare Advantage), and pharmacies. Their role is multifaceted, encompassing negotiating drug prices, developing formularies (lists of covered drugs), processing claims, and managing drug utilization. However, their significant influence on drug pricing and patient access has led to increasing scrutiny.PBMs’ involvement in the Medicare Advantage system is extensive.
Many Medicare Advantage plans contract with PBMs to manage their prescription drug benefits. This means the PBM negotiates prices with drug manufacturers, determines which drugs are covered under the plan’s formulary, and processes claims for prescription drugs filled by beneficiaries. The complexity of these arrangements, and the often opaque nature of PBM practices, is a key area of concern.
Potential Conflicts of Interest Associated with PBM Practices
PBMs operate under a complex web of financial relationships that can create significant conflicts of interest. For example, PBMs may receive rebates from drug manufacturers in exchange for favorable formulary placement of their drugs. This can incentivize PBMs to prioritize higher-reimbursed drugs, even if less expensive or clinically equivalent alternatives exist. Furthermore, some PBMs also own or operate pharmacies, creating a potential conflict of interest when deciding which pharmacies are included in their networks.
This can limit patient choice and potentially lead to higher out-of-pocket costs. The lack of transparency in these rebate arrangements makes it difficult to assess their overall impact on drug costs and patient care.
Impact of PBM Negotiations on Drug Pricing and Patient Access
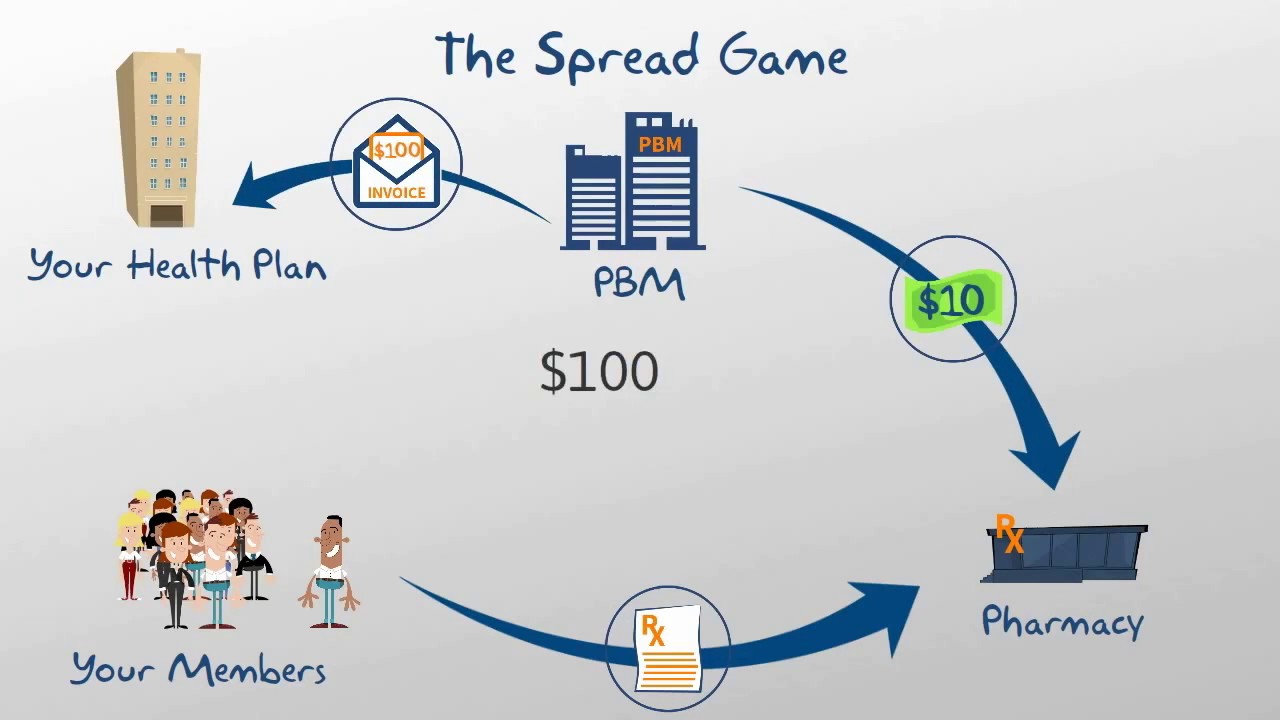
PBM negotiations significantly influence drug pricing and patient access. While PBMs claim to negotiate lower prices for drugs, the actual impact is often debated. Critics argue that the opaque nature of rebate negotiations makes it difficult to determine whether the savings are passed on to consumers or absorbed by the PBMs and health plans. Furthermore, the practice of “spread pricing,” where PBMs charge insurers more than they pay pharmacies, is a major source of concern.
This practice can inflate drug costs for insurers and ultimately contribute to higher premiums for patients. Restrictions on patient access to certain medications due to formulary restrictions, driven by PBM negotiations, further compound these issues. The net effect can be higher drug costs for patients, despite the claimed savings from PBM negotiations.
PBM Practices Under Congressional Scrutiny
Several PBM practices have drawn significant congressional scrutiny. These include:
- Spread Pricing: The practice of PBMs charging health plans more for drugs than they reimburse pharmacies.
- Rebates and Lack of Transparency: The opaque nature of rebates received from drug manufacturers and how those rebates affect drug prices and patient costs.
- Pharmacy Network Restrictions: Limiting the number of pharmacies in their networks, potentially reducing patient choice and access to care.
- Formulary Design and Drug Tiers: Manipulating formulary design and drug tiers to favor certain drugs, often those with higher rebates.
- Administrative Fees and Pass-Through Charges: The lack of transparency in administrative fees and other pass-through charges imposed on health plans and patients.
Hospital Participation in Medicare Advantage
Source: ytimg.com
The relationship between hospitals and Medicare Advantage (MA) plans is complex, shaped by financial incentives, reimbursement structures, and the ultimate impact on patient care. Understanding this dynamic is crucial for ensuring access to quality healthcare for seniors. This section will explore the key aspects of hospital participation in MA, focusing on the financial drivers, effects on patient care, and comparisons with traditional Medicare.
Financial Incentives for Hospital Participation in Medicare Advantage Networks
Hospitals are incentivized to participate in MA networks primarily through the promise of patient volume and predictable revenue streams. MA plans negotiate rates with hospitals, often resulting in lower reimbursement rates compared to traditional Medicare. However, the potential for increased patient volume, especially in regions with a high concentration of MA beneficiaries, can offset these lower rates. Furthermore, MA plans often offer bundled payments or value-based care arrangements that can incentivize hospitals to improve efficiency and quality of care to maximize their earnings.
This can lead to a shift in hospital focus towards managing the overall cost of care for their MA patient population. The stability and predictability of MA contracts can also be attractive to hospitals, especially in contrast to the fluctuating reimbursements and potential for bad debt under traditional Medicare.
Hospital Participation’s Effects on Patient Care and Access, Congress healthcare hearings medicare advantage pbms hospitals
The impact of hospital participation in MA on patient care and access is multifaceted. Increased participation generally improves access for MA beneficiaries to in-network hospitals, streamlining the process of receiving care and reducing out-of-pocket expenses. However, reduced reimbursement rates under MA contracts could potentially lead to hospitals prioritizing efficiency over certain aspects of patient care, especially if they face financial constraints.
This might manifest in reduced staffing levels, limited access to advanced technologies or specialized services, or longer wait times for appointments or procedures. The level of impact varies greatly depending on the specific hospital, the MA plan’s reimbursement model, and the local healthcare market. For example, a rural hospital with limited resources might face significant challenges if it cannot secure favorable MA contracts.
Reimbursement Models: Traditional Medicare vs. Medicare Advantage
Traditional Medicare (fee-for-service) uses a retrospective payment system, where hospitals are reimbursed for services rendered after they are provided. This system can lead to unpredictable revenue streams for hospitals and potential for higher costs. In contrast, MA plans typically use prospective payment systems, such as capitation or bundled payments. Under capitation, hospitals receive a fixed payment per member per month, regardless of the services provided.
Bundled payments involve a single payment for a specific episode of care, incentivizing hospitals to manage costs effectively within that episode. These prospective payment models shift the financial risk from the government to the hospitals, potentially leading to cost-saving measures, but also potentially limiting access to certain services if costs exceed the pre-negotiated payments.
Hypothetical Scenario: Reduced Hospital Participation in Medicare Advantage
Imagine a scenario where a major metropolitan area experiences a significant reduction in hospital participation in MA networks due to disagreements over reimbursement rates. This could lead to a shortage of in-network hospitals for MA beneficiaries, forcing them to seek care at out-of-network facilities, resulting in higher out-of-pocket expenses and potentially impacting access to timely and necessary care. Elderly patients reliant on MA plans might find it more difficult to receive treatment, leading to increased emergency room visits and potentially poorer health outcomes.
Furthermore, this could exacerbate existing disparities in access to care, particularly impacting vulnerable populations. This scenario underscores the critical importance of striking a balance between cost containment and ensuring sufficient hospital participation in MA networks to maintain adequate access to quality healthcare for beneficiaries.
Impact on Patient Access and Healthcare Costs
Source: slideteam.net
Medicare Advantage (MA) plans, while offering potentially lower premiums, present a complex picture regarding patient access to care and overall healthcare costs. The interplay between MA plans, Pharmaceutical Benefit Managers (PBMs), and hospital participation significantly influences beneficiaries’ experiences and expenses. This section delves into the impact of these factors on patient access and the ultimate cost of healthcare.
Medicare Advantage’s Influence on Patient Access to Care
The impact of Medicare Advantage on patient access is multifaceted. While MA plans often offer a wider network of physicians than traditional Medicare, the reality is more nuanced. Network restrictions, prior authorization requirements, and the steering of patients towards specific providers within the network can limit patient choice and potentially delay or prevent access to necessary care. For instance, a beneficiary needing a specialist might find that their preferred specialist is not in their MA plan’s network, forcing them to choose from a smaller pool of options or face significant out-of-pocket costs.
Additionally, the increasing prevalence of narrow networks in MA plans, designed to control costs, can restrict access to care, especially for individuals with complex medical needs requiring specialized services. Studies have shown a correlation between narrow networks and reduced access to specialists and certain types of care.
The Relationship Between PBM Practices and Prescription Drug Costs
Pharmaceutical Benefit Managers (PBMs) play a crucial role in negotiating drug prices and managing prescription drug benefits within MA plans. However, their practices have been a subject of scrutiny, with concerns raised about their impact on drug costs for beneficiaries. PBMs’ use of rebates and spread pricing, where they keep the difference between the negotiated price and the reimbursement from the plan, can lead to higher costs for beneficiaries despite the PBM’s claims of negotiating lower prices.
Furthermore, the lack of transparency in PBM operations makes it difficult to determine the actual impact of their practices on drug prices. For example, a PBM might negotiate a lower price with a pharmaceutical company, but then increase the patient’s copay or impose prior authorization requirements, ultimately increasing the cost for the beneficiary.
Congressional Oversight and Healthcare Costs for Medicare Advantage Beneficiaries
Congressional oversight plays a vital role in shaping the cost of healthcare for Medicare Advantage beneficiaries. Investigations and hearings into PBM practices, network adequacy, and the overall performance of MA plans can lead to policy changes aimed at improving transparency, increasing competition, and protecting beneficiaries from excessive costs. For example, legislation mandating greater transparency in PBM rebate negotiations could lead to lower drug costs for beneficiaries.
Similarly, increased scrutiny of MA plan network adequacy could encourage plans to expand their networks, improving patient access to care. However, the effectiveness of congressional oversight depends on the political will to implement meaningful reforms and the ability to overcome lobbying efforts from powerful industry players.
So, Congress is grilling everyone from Medicare Advantage plans to PBMs and hospitals about rising healthcare costs. It’s a huge mess, and honestly, sometimes I feel like I need a break from all the political drama. I just read about Karishma Mehta’s decision to freeze her eggs – check out the article on the risks associated with that here: karishma mehta gets her eggs frozen know risks associated with egg freezing – and it makes me realize that personal health decisions are equally complex, even outside the political sphere.
It’s all connected, really; the pressure on the healthcare system affects us all, in ways big and small.
Key Findings on Patient Access and Healthcare Costs
| Finding | Supporting Evidence |
|---|---|
| Narrow MA networks restrict patient access to specialists and preferred providers. | Studies showing a correlation between narrow networks and reduced access to care; anecdotal evidence from beneficiaries facing difficulties accessing specialists. |
| PBM practices, including spread pricing and lack of transparency, can increase prescription drug costs for beneficiaries. | Reports from government agencies and watchdog groups highlighting concerns about PBM practices; evidence of higher beneficiary cost-sharing despite negotiated lower drug prices. |
| Congressional oversight can influence healthcare costs through policy changes addressing PBM practices and MA plan performance. | Examples of legislation aimed at increasing transparency and accountability in the healthcare industry; impact assessments of past legislative actions. |
Legislative Proposals and Policy Recommendations
The ongoing debate surrounding Medicare Advantage has spurred numerous legislative proposals aimed at improving the program’s efficiency, transparency, and patient outcomes. These proposals reflect a range of concerns, from rising costs and inadequate provider reimbursement to issues with beneficiary access to care and potential conflicts of interest involving PBMs and hospitals. Understanding these proposals and their potential consequences is crucial for stakeholders across the healthcare landscape.The impact of these legislative changes on hospitals, PBMs, and beneficiaries will vary considerably depending on the specific proposal.
Some aim to increase payments to providers, potentially benefiting hospitals struggling with shrinking Medicare Advantage reimbursements. Others focus on greater transparency and regulation of PBMs, potentially altering their profit margins and influencing drug pricing. Finally, some proposals aim to improve beneficiary protections, ensuring access to needed care and preventing misleading marketing practices.
Key Legislative Proposals Targeting Medicare Advantage
Several key legislative proposals are currently under consideration. One example focuses on increasing transparency regarding Medicare Advantage plan payments and the use of funds. This aims to address concerns about potentially excessive administrative costs and profits siphoned away from patient care. Another significant proposal involves strengthening the oversight of PBMs, limiting their ability to steer beneficiaries toward more expensive medications or restrict access to preferred providers.
Finally, proposals exist to enhance the appeals process for beneficiaries who have been denied coverage or services, providing better recourse for patients facing denials.
Potential Impacts of Proposed Legislation
The potential impact of these proposals is complex and multifaceted. For example, increased transparency regarding plan payments could lead to adjustments in how Medicare Advantage plans operate, potentially impacting both hospitals (through changes in reimbursement) and PBMs (through scrutiny of their practices). Strengthened PBM oversight could lead to lower drug prices for beneficiaries, but it might also reduce PBM profitability, potentially affecting their investment in other programs.
Improved beneficiary appeals processes could increase administrative burdens but simultaneously lead to better patient outcomes and satisfaction. Consider the case of a hypothetical scenario where stricter regulations on PBM formularies result in increased access to preferred medications for patients with chronic illnesses. This could significantly reduce hospital readmissions and improve overall health outcomes, despite the potential for initial cost increases.
Congress is grilling everyone from Medicare Advantage providers to PBMs and hospitals in these healthcare hearings. It’s a mess trying to untangle the complexities, but to get a better grasp on the underlying data issues, I highly recommend checking out this insightful podcast: podcast inside healthcare apis. Understanding the APIs involved could shed light on some of the opaque pricing and administrative hurdles fueling these hearings.
Comparison of Policy Recommendations
Different policy recommendations exist for addressing concerns about Medicare Advantage. Some advocate for a more regulatory approach, involving increased government oversight and stricter rules for plans, PBMs, and hospitals. Others favor a market-based approach, relying on greater competition among plans and improved consumer choice to drive down costs and improve quality. For instance, proposals promoting greater competition could involve reducing barriers to entry for new Medicare Advantage plans or increasing transparency regarding plan performance metrics.
Conversely, proposals for stronger regulation might involve implementing stricter penalties for plans that engage in questionable billing practices or limiting the influence of PBMs in medication selection.
Potential Unintended Consequences of Proposed Legislative Changes
A careful consideration of unintended consequences is crucial when evaluating legislative proposals.
- Increased administrative burden on providers and plans, potentially leading to delays in processing claims and increased costs.
- Reduced participation by Medicare Advantage plans, potentially limiting beneficiary choices and access to care in certain areas.
- Unforeseen effects on drug pricing and availability, potentially leading to shortages or higher costs for some medications.
- Increased litigation and legal challenges, leading to higher costs for taxpayers and healthcare systems.
- Disruptions to the healthcare delivery system, potentially impacting the quality of care for beneficiaries.
Final Summary: Congress Healthcare Hearings Medicare Advantage Pbms Hospitals
The congressional hearings on Medicare Advantage, PBMs, and hospitals have illuminated a complex and often troubling picture. The system, as it currently stands, presents significant challenges for both patients and providers. From concerns about patient access and rising drug costs to potential conflicts of interest among key players, the need for reform is undeniable. While legislative solutions are being debated, the ultimate outcome will significantly impact the future of healthcare in America.
This is an ongoing story, and we’ll continue to follow the developments with keen interest.
FAQ Compilation
What are the main criticisms of Medicare Advantage plans?
Common criticisms include inadequate coverage for certain services, restrictive provider networks limiting patient choice, and complex billing practices leading to confusion and higher out-of-pocket costs for beneficiaries.
How do PBMs profit from their role in Medicare Advantage?
PBMs profit through rebates from drug manufacturers, administrative fees charged to plans, and spread pricing (the difference between what they pay pharmacies and what they charge plans).
What are some examples of legislative proposals aimed at reforming Medicare Advantage?
Proposals include increased transparency in PBM practices, stronger oversight of Medicare Advantage plans, and expanding access to care by allowing greater provider choice for beneficiaries.





