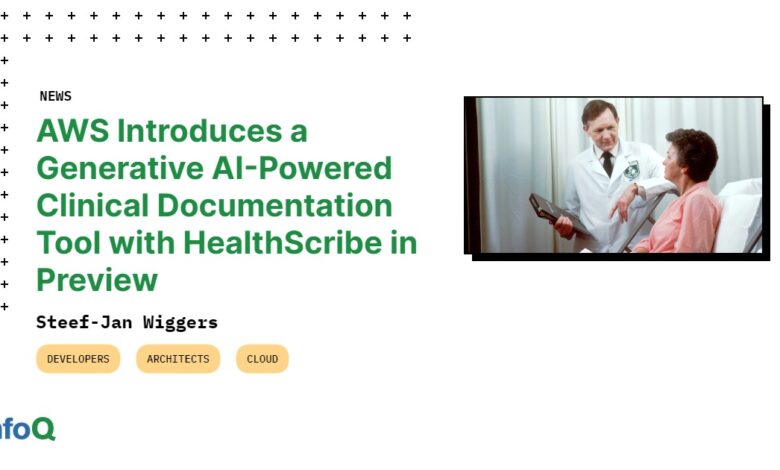
Amazon AWS Health Generative AI HealthBridge
Amazon AWS Health Generative AI HealthBridge: Imagine a future where AI assists doctors in diagnosing diseases with unprecedented accuracy, accelerates drug discovery, and personalizes patient care like never before. This is the promise of generative AI in healthcare, and Amazon Web Services (AWS) is at the forefront, providing the powerful tools and infrastructure to make it a reality. We’ll explore how AWS services, specifically tailored for healthcare’s stringent security and compliance needs, are enabling the development and deployment of cutting-edge generative AI models.
This isn’t just about technology; it’s about revolutionizing how we approach healthcare, improving outcomes, and ultimately, saving lives.
This exploration delves into the specifics of using AWS services like EC2, S3, and SageMaker to build and deploy these AI models. We’ll examine how to handle the massive datasets involved, ensuring patient privacy and data security while adhering to regulations like HIPAA. We’ll also discuss the ethical considerations and potential challenges of integrating generative AI into a real-world healthcare setting, using a hypothetical platform called HealthBridge as our example.
Get ready for a deep dive into the exciting and transformative world of AI-powered healthcare!
Amazon AWS Services Relevant to Generative AI in Healthcare: Amazon Aws Health Generative Ai Healthbridge
Developing and deploying generative AI models for healthcare presents unique challenges, demanding robust infrastructure, high security, and compliance with stringent regulations. Amazon Web Services (AWS) offers a comprehensive suite of services designed to address these needs, providing a scalable and secure platform for building innovative healthcare applications. This exploration will delve into specific AWS services crucial for this domain, highlighting their capabilities and how they contribute to a secure and compliant AI healthcare environment.
Amazon EC2, S3, and SageMaker for Generative AI in Healthcare
Amazon Elastic Compute Cloud (EC2) provides the foundational compute power needed for training and deploying large generative AI models. Researchers can choose from a wide variety of instance types, optimized for different workloads, such as those requiring high GPU processing for deep learning tasks. Amazon Simple Storage Service (S3) serves as the robust and scalable storage solution for both training data and model artifacts.
Its durability and security features are critical for protecting sensitive healthcare data. Amazon SageMaker, a fully managed machine learning service, simplifies the entire machine learning workflow, from data preparation and model building to deployment and monitoring. It offers pre-built algorithms and frameworks specifically designed for generative AI, streamlining the development process and reducing time-to-market. For example, a research team could utilize EC2 instances with powerful GPUs to train a large language model on a massive dataset stored in S3, leveraging SageMaker’s built-in tools for model optimization and deployment.
Security and Compliance Features of AWS Relevant to HIPAA and Other Healthcare Data Regulations
The security and compliance aspects are paramount when handling sensitive patient data. AWS offers a multi-layered security approach, encompassing infrastructure security, data encryption, access control, and compliance certifications. AWS services are designed to meet HIPAA requirements, allowing healthcare organizations to maintain compliance while leveraging the power of cloud computing. Features such as encryption at rest and in transit, granular access control through IAM (Identity and Access Management), and comprehensive audit trails contribute to a secure environment.
Furthermore, AWS regularly undergoes audits and certifications, including compliance with HIPAA, GDPR, and other relevant regulations, providing assurance to healthcare providers. For instance, a hospital deploying a generative AI model for diagnosis assistance can utilize AWS’s security features to ensure patient data remains confidential and secure, meeting HIPAA compliance requirements.
Comparing AWS Services for Processing Large Healthcare Datasets
Several AWS services are well-suited for processing the large, often complex, datasets common in healthcare. Amazon EMR (Elastic MapReduce) provides a managed Hadoop framework for distributed processing of massive datasets, ideal for tasks like preprocessing and feature engineering. Amazon Athena allows for querying data directly from S3 using SQL, simplifying data exploration and analysis. Amazon Redshift, a fully managed data warehouse service, is suitable for analytical queries and reporting on large datasets, supporting efficient data exploration and model evaluation.
The choice of service depends on the specific needs of the project. For instance, a large-scale genomics project might utilize EMR for distributed processing of genomic data, while a clinical trial analysis might rely on Redshift for efficient querying and reporting.
Hypothetical Architecture Diagram for a Generative AI Healthcare Application
| Service | Function | Data Flow | Notes |
|---|---|---|---|
| Amazon S3 | Data Storage (Patient Records, Medical Images) | Input to EMR, SageMaker | Secure, HIPAA-compliant storage |
| Amazon EMR | Data Preprocessing, Feature Engineering | S3 -> EMR -> S3 | Distributed processing of large datasets |
| Amazon SageMaker | Model Training, Deployment, Monitoring | S3 -> SageMaker -> S3, API Gateway | Managed machine learning platform |
| Amazon API Gateway | Secure access to the deployed model | SageMaker -> API Gateway -> Client Applications | Controls access and manages requests |
Generative AI Applications within HealthBridge
HealthBridge, a hypothetical advanced healthcare platform, stands to gain significantly from the integration of generative AI. Its potential spans across various critical areas, promising improvements in efficiency, accuracy, and ultimately, patient care. This exploration delves into specific applications, ethical considerations, and potential challenges associated with implementing generative AI within this innovative platform.
Diagnostics Enhancement with Generative AI
Generative AI models, trained on vast datasets of medical images (X-rays, CT scans, MRIs) and patient records, can assist radiologists and other specialists in identifying subtle anomalies that might be missed by the human eye. For instance, a generative model could analyze a chest X-ray and highlight potential indicators of pneumonia, generating a report that includes not only the highlighted areas but also a probability score indicating the likelihood of the diagnosis.
This enhanced diagnostic capability could lead to earlier interventions and improved patient outcomes. Furthermore, generative AI can assist in creating synthetic medical images for training purposes, addressing data scarcity issues often encountered in medical imaging. This ensures more robust and accurate AI models for future diagnostic applications.
Drug Discovery Acceleration
The process of drug discovery is notoriously lengthy and expensive. Generative AI can significantly accelerate this process by designing novel drug molecules with desired properties. By learning from existing drug databases and applying generative models, the AI can predict the efficacy and safety of potential drug candidates, significantly reducing the time and resources required for pre-clinical testing. For example, generative models have been successfully used to design new antibiotics, targeting specific bacterial mechanisms, offering a promising approach to combating antibiotic resistance.
This speeds up the time-to-market for crucial new medications.
Personalized Medicine through Generative AI
Generative AI can personalize treatment plans based on individual patient characteristics, including genetics, lifestyle, and medical history. By analyzing this complex data, the AI can generate tailored treatment recommendations, predicting the likelihood of success for different treatment options. For instance, a generative model could predict the optimal dosage and type of chemotherapy for a cancer patient based on their genetic profile and tumor characteristics, potentially improving treatment efficacy and reducing side effects.
This precision medicine approach offers a step towards more effective and individualized care.
Improving Patient Care with Generative AI in HealthBridge
The integration of generative AI within HealthBridge can lead to significant improvements in patient care through increased efficiency and accuracy. AI-powered chatbots can provide patients with immediate answers to their medical queries, freeing up human healthcare professionals to focus on more complex cases. Generative AI can also automate administrative tasks, such as scheduling appointments and generating medical reports, streamlining workflows and reducing the burden on healthcare staff.
The accuracy gains from improved diagnostics and personalized medicine contribute directly to better patient outcomes.
Ethical Implications of Generative AI in HealthBridge
The use of generative AI in healthcare raises significant ethical considerations, particularly concerning patient privacy and algorithmic bias. Robust data anonymization and security measures are crucial to protect patient information. HealthBridge must adhere to strict privacy regulations, ensuring compliance with HIPAA and other relevant legislation. Furthermore, algorithmic bias in generative AI models can lead to disparities in healthcare access and quality.
Amazon AWS Health, with its generative AI and HealthBridge, offers exciting possibilities for healthcare innovation, but robust security is paramount. Understanding the implications of the hhs healthcare cybersecurity framework hospital requirements cms is crucial for ensuring that AI solutions like HealthBridge are deployed responsibly and securely within hospital settings. This framework directly impacts how we can integrate such powerful tools into existing healthcare infrastructure.
Careful monitoring and mitigation strategies are essential to ensure fairness and equity in the application of these technologies. Regular audits and transparency in model development and deployment are crucial to address these ethical concerns.
Challenges and Risks of Implementing Generative AI in HealthBridge
Implementing generative AI in HealthBridge presents several challenges and risks that need careful consideration.
- Data Quality and Availability: Generative AI models require large, high-quality datasets for training. Acquiring and curating such datasets can be challenging and expensive.
- Model Explainability and Interpretability: Understanding how generative AI models arrive at their conclusions is crucial for building trust and ensuring accountability. The “black box” nature of some models can hinder their adoption in healthcare.
- Regulatory Compliance and Legal Issues: Navigating the complex regulatory landscape surrounding AI in healthcare requires careful planning and compliance with relevant laws and guidelines.
- Integration with Existing Systems: Seamless integration of generative AI with existing healthcare information systems is essential for effective implementation.
- Cost of Implementation and Maintenance: The development, deployment, and maintenance of generative AI systems can be expensive, requiring significant investment in infrastructure and expertise.
Data Considerations for Generative AI in Healthcare on AWS
Leveraging the power of generative AI in healthcare promises revolutionary advancements, but realizing this potential hinges critically on the quality and responsible handling of the data used to train these models. This section delves into the crucial considerations surrounding healthcare data preparation for generative AI on AWS, emphasizing data types, anonymization, security, validation, and a step-by-step preparation guide.
Amazon AWS Health’s generative AI, HealthBridge, is revolutionizing healthcare data analysis, offering incredible potential for improved patient care. This kind of advanced technology becomes even more impactful when considering large-scale healthcare integrations, like the recent Jefferson Health Lehigh Valley Health Network merger , which could benefit greatly from HealthBridge’s ability to streamline data across merged systems. Ultimately, tools like HealthBridge are crucial for navigating the complexities of modern healthcare consolidation.
Suitable Healthcare Data Types for Generative AI Model Training
The types of healthcare data suitable for training generative AI models are diverse and depend heavily on the specific application. However, some common data types include electronic health records (EHRs), medical images (X-rays, CT scans, MRIs), genomic data, clinical trial data, and wearable sensor data. The quality of this data is paramount. Inconsistent formatting, missing values, and errors can significantly impact model performance and lead to inaccurate or biased predictions.
Preprocessing steps, such as data cleaning, normalization, and feature engineering, are essential to ensure data quality and suitability for model training. For example, inconsistencies in the coding of diagnoses or procedures within EHRs need to be addressed through standardization and mapping to common terminologies like SNOMED CT or LOINC.
Anonymizing and Securing Sensitive Patient Data, Amazon aws health generative ai healthbridge
Protecting patient privacy is paramount. Before using healthcare data to train generative AI models on AWS, rigorous anonymization and security measures must be implemented. This involves techniques like de-identification, which removes or replaces identifying information such as names, addresses, and medical record numbers. Differential privacy, a method that adds carefully calibrated noise to the data, can further enhance privacy without significantly compromising the data’s utility for model training.
AWS offers a range of services to support this, including Amazon S3 for secure data storage, Amazon KMS for encryption, and Amazon Comprehend Medical for natural language processing tasks that can aid in de-identification. Implementing robust access control mechanisms, adhering to HIPAA regulations, and regularly auditing security protocols are crucial aspects of data security.
Data Validation and Reliability Assurance
Ensuring the reliability of the data used for training is critical to the trustworthiness of the resulting generative AI models. Data validation involves multiple steps, including data consistency checks, outlier detection, and plausibility checks. For instance, detecting inconsistencies between patient demographics and medical history, or identifying improbable values for vital signs, can indicate data errors. Cross-validation techniques, such as splitting the data into training, validation, and test sets, help evaluate model performance and identify potential biases.
Regular audits and quality control checks throughout the data lifecycle are essential to maintain data reliability and prevent the propagation of errors.
Step-by-Step Guide to Preparing Healthcare Data for Generative AI on AWS
Preparing healthcare data for generative AI on AWS involves a structured, multi-stage process:
- Data Acquisition and Ingestion: Gather relevant data from various sources (EHRs, image repositories, etc.) and securely transfer it to AWS using services like AWS DataSync or Snowball.
- Data Cleaning and Preprocessing: Identify and address data quality issues such as missing values, inconsistencies, and outliers. This might involve imputation, normalization, and standardization techniques.
- Data Anonymization and De-identification: Apply appropriate de-identification methods to remove or replace personally identifiable information while preserving data utility.
- Data Transformation and Feature Engineering: Transform raw data into a format suitable for model training. This may involve feature scaling, encoding categorical variables, and creating new features from existing ones.
- Data Security and Access Control: Implement robust security measures, including encryption, access control lists, and auditing, to protect sensitive patient data.
- Data Validation and Quality Control: Conduct thorough validation checks to ensure data accuracy, consistency, and reliability. Employ cross-validation techniques to assess model performance and identify potential biases.
- Data Loading and Model Training: Load the prepared data into a suitable format (e.g., Amazon S3, Amazon Redshift) and use AWS services like Amazon SageMaker to train the generative AI model.
Each stage is crucial for building a robust and reliable generative AI model that respects patient privacy and produces accurate results. Careful attention to these steps is essential for responsible and effective deployment of generative AI in healthcare.
Model Development and Deployment Strategies
Developing and deploying generative AI models for healthcare applications on AWS involves a complex but rewarding process. This process leverages the scalability and robust infrastructure of AWS to handle the large datasets and computationally intensive tasks inherent in training and deploying these sophisticated models. Careful consideration of model architecture, training techniques, and deployment strategies is crucial for success.
A Conceptual Workflow for Medical Image Analysis
Let’s consider a specific example: developing a generative AI model for medical image analysis, such as detecting cancerous lesions in mammograms. The workflow would begin with data acquisition and preprocessing. This involves collecting a large, diverse dataset of mammograms, properly labeling them, and cleaning the data to remove noise and artifacts. This preprocessed data is then used to train a chosen generative AI model, such as a convolutional neural network (CNN) or a variational autoencoder (VAE).
The model’s performance is rigorously evaluated using a separate validation dataset. Hyperparameter tuning and model architecture adjustments are made iteratively to optimize performance. Once satisfactory performance is achieved, the model is deployed to a production environment on AWS, potentially using services like SageMaker for seamless deployment and management. Continuous monitoring and retraining ensure the model remains accurate and effective over time.
Comparison of Generative AI Model Architectures
Several generative AI model architectures are suitable for various healthcare tasks. Transformers, known for their success in natural language processing, are increasingly applied to medical image analysis and genomic data analysis. Their strength lies in their ability to capture long-range dependencies within data. However, they can be computationally expensive to train and require substantial amounts of data. Generative Adversarial Networks (GANs) are another powerful architecture, particularly useful for generating synthetic medical images for data augmentation or anonymization.
Amazon AWS Health’s generative AI, HealthBridge, is revolutionizing healthcare data analysis. Imagine its potential impact on improving patient outcomes, especially when integrated with readily accessible primary care. For example, consider the expansion of convenient care options like the humana centerwell primary care centers walmart partnership; HealthBridge could analyze data from these centers to identify trends and improve preventative care strategies, ultimately leading to more efficient and effective healthcare delivery.
This makes the future of AI-driven healthcare incredibly promising.
GANs consist of two competing networks: a generator that creates synthetic data and a discriminator that distinguishes between real and synthetic data. Their weakness lies in the difficulty of training them stably and the potential for mode collapse, where the generator produces limited variations of synthetic data. Autoencoders, including VAEs, are effective for dimensionality reduction and anomaly detection in medical imaging.
They are generally less computationally demanding than transformers or GANs but may not capture as much detail. The choice of architecture depends heavily on the specific task and available resources.
Model Training, Validation, and Testing on AWS
Model training, validation, and testing are crucial steps in developing robust generative AI models. AWS provides a comprehensive suite of services to support this process. Amazon SageMaker is a fully managed service that simplifies the process of building, training, and deploying machine learning models. It offers various algorithms, including those suitable for generative AI, and allows for distributed training across multiple instances to accelerate the process.
Optimization techniques, such as hyperparameter tuning using SageMaker’s automated tuning capabilities, are essential for achieving optimal model performance. Validation is performed on a separate dataset to assess the model’s generalization ability and avoid overfitting. Rigorous testing on a held-out test dataset ensures the model meets performance requirements before deployment.
Model Deployment Strategies on AWS
Different deployment strategies on AWS cater to various needs and priorities.
| Deployment Strategy | Cost | Scalability | Latency |
|---|---|---|---|
| Amazon SageMaker endpoints | Moderate to High (depending on instance type and traffic) | High (easily scalable based on demand) | Low (milliseconds to seconds) |
| AWS Lambda | Low (pay-per-request) | High (serverless architecture) | Can be high depending on function complexity |
| Amazon Elastic Container Service (ECS) or Kubernetes (EKS) | Moderate (depending on instance type and number of containers) | High (containerized deployments allow for easy scaling) | Moderate (depends on container orchestration and instance performance) |
| Amazon EC2 instances | Low to High (depending on instance type and usage) | Moderate (manual scaling required) | Low to Moderate (depends on instance performance) |
Illustrative Examples of Generative AI in Healthcare
Source: analyticsindiamag.com
Generative AI holds immense potential to revolutionize healthcare, moving beyond simple analysis to actively create solutions and personalized approaches. Let’s explore some hypothetical yet plausible applications showcasing this transformative power.
Generative AI in Medical Imaging Analysis
This example focuses on the detection and classification of subtle anomalies in brain MRI scans indicative of early-stage Alzheimer’s disease. The input data consists of a large dataset of anonymized brain MRI scans, meticulously labeled by expert radiologists, categorized as either healthy or exhibiting early Alzheimer’s characteristics. This dataset is used to train a Generative Adversarial Network (GAN). The GAN architecture consists of two neural networks: a generator and a discriminator.
The generator attempts to create realistic MRI scans, both healthy and diseased, while the discriminator tries to differentiate between real and generated scans. Through this adversarial training process, the generator learns to produce highly realistic images, effectively capturing the subtle variations associated with Alzheimer’s. The output isn’t simply a classification; the model generates a ‘synthetic’ MRI representing the likely progression of the disease based on the input scan.
This allows for earlier and more accurate diagnosis, providing clinicians with a visual representation of potential future states, facilitating proactive treatment strategies. The image generation process involves a complex interplay between the generator and discriminator, with the generator iteratively refining its output based on the discriminator’s feedback. This results in images that are not mere copies of training data, but rather novel yet realistic representations of disease progression.
Generative AI in Drug Discovery
This application centers on the design of novel antiviral drugs targeting influenza. The process begins with a large database of known antiviral compounds and their associated molecular structures, alongside information on their binding affinities to influenza proteins. A generative model, such as a Variational Autoencoder (VAE), is trained on this data. The VAE learns the underlying latent representation of effective antiviral compounds.
The model is then prompted to generate novel molecular structures based on this learned representation, optimizing for specific desired properties like high binding affinity and low toxicity. These generated molecules are then virtually screened using molecular dynamics simulations and other computational methods to assess their efficacy and safety. The drug design process is iterative. The model generates candidate molecules, these candidates are evaluated, and feedback is used to refine the model’s generative capabilities, ultimately leading to the identification of promising drug candidates that warrant further experimental validation.
For example, the model might initially generate molecules with high binding affinity but also high toxicity. This feedback is then incorporated into subsequent iterations, guiding the model to generate molecules with improved safety profiles while maintaining high efficacy.
Personalized Treatment Plans using Generative AI
Consider a patient with type 2 diabetes. The input data comprises the patient’s medical history (blood glucose levels, weight, family history of diabetes, lifestyle factors, etc.), genetic information, and responses to previous treatments. A generative model, perhaps a recurrent neural network (RNN) or a transformer-based model, is trained on a large dataset of patient records and treatment outcomes.
This model is used to generate a personalized treatment plan, predicting the likely effectiveness of various treatment options based on the patient’s unique characteristics. The output is not just a single treatment recommendation, but rather a range of possibilities, each with an associated probability of success and potential side effects. This allows the clinician to make an informed decision, considering the patient’s preferences and risk tolerance.
The decision-making process involves a collaborative approach between the clinician and the AI system. The AI provides a probabilistic forecast of treatment outcomes, enabling the clinician to select the most suitable option, considering factors that the model might not fully capture, such as the patient’s overall well-being and lifestyle preferences. For instance, one treatment might be highly effective but require significant lifestyle changes, while another, less effective option, might be easier to integrate into the patient’s daily life.
The clinician, using the AI-generated insights, can guide the patient towards the optimal balance between efficacy and practicality.
Closure
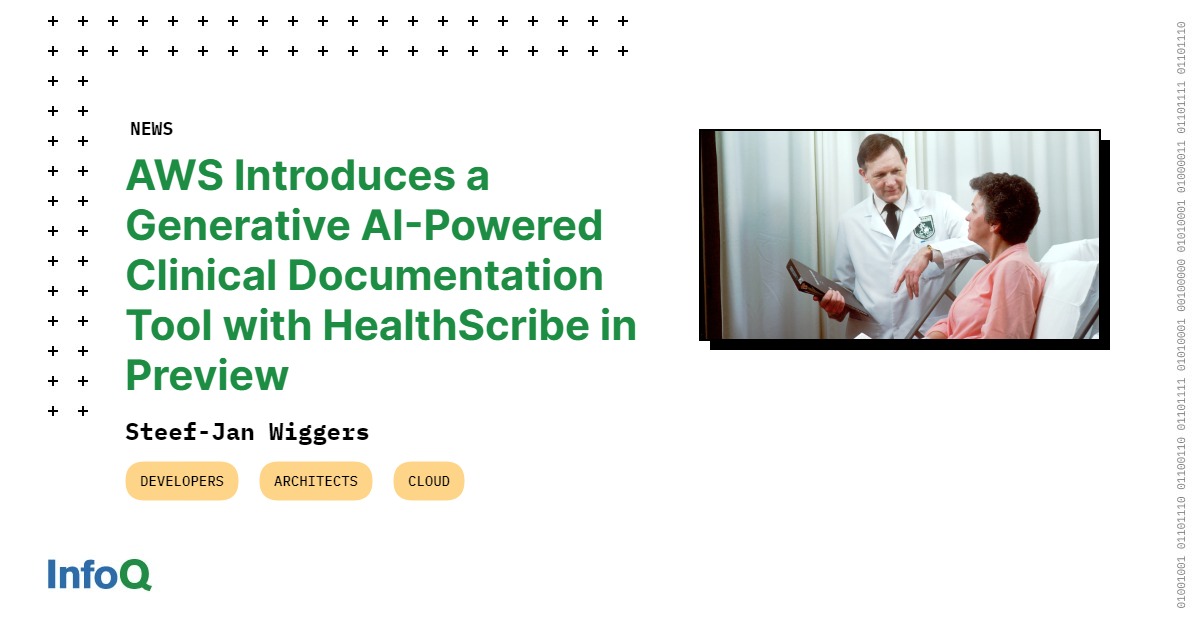
Source: infoq.com
The potential of Amazon AWS Health Generative AI HealthBridge is truly staggering. From faster diagnoses and personalized treatment plans to accelerating drug discovery, the possibilities are vast. However, responsible development and deployment are crucial. Addressing ethical concerns, ensuring data privacy, and mitigating potential biases are paramount. As we move forward, it’s vital to remember that the human element remains at the heart of healthcare.
Generative AI, powered by AWS, isn’t meant to replace doctors but to empower them, allowing them to focus on what matters most: their patients. The journey is just beginning, and the future of healthcare is being written, one line of code at a time.
Question Bank
What specific types of generative AI models are best suited for healthcare applications on AWS?
Several models excel, including transformers for natural language processing (analyzing patient records), GANs (generating synthetic medical images for training), and diffusion models (enhancing medical images).
How does AWS ensure the security and privacy of sensitive patient data used in generative AI models?
AWS employs robust security measures, including encryption at rest and in transit, access control lists, and compliance certifications like HIPAA, ensuring data protection throughout the AI lifecycle.
What are the major cost considerations when deploying generative AI models on AWS for healthcare?
Costs depend on compute resources (EC2 instances), storage (S3), and the model’s complexity. Optimizing model architecture and using cost-effective AWS services are key.
What are the potential biases in generative AI models used in healthcare, and how can they be mitigated?
Biases can stem from skewed training data. Careful data curation, bias detection techniques, and diverse datasets are crucial for mitigating these risks.





