Do All HPV Infections Lead to Cancer? Doctor Explains
Do all hpv infections lead to cancer doctor explains – Do all HPV infections lead to cancer? Doctor explains – that’s the burning question many have, and it’s a complex one. The Human Papillomavirus (HPV) is incredibly common; most sexually active people will encounter it at some point. But while many HPV infections clear up on their own, some types are linked to certain cancers. This post dives into the science behind HPV, clarifying the risks and dispelling common myths surrounding this widespread virus.
We’ll explore the different types of HPV, the cancers they can cause, and what you can do to protect yourself.
Understanding the link between HPV and cancer is crucial for informed decision-making about your health. We’ll cover the factors that influence cancer development, the role of your immune system, and the importance of vaccination and regular screenings. This isn’t about fear-mongering; it’s about empowering you with knowledge to make choices that support your well-being.
Understanding HPV and Cancer Risk
Human papillomavirus (HPV) is a common viral infection that affects the skin and mucous membranes. There are many different types of HPV, and most infections are harmless and clear up on their own without causing any health problems. However, some types of HPV can persist and lead to the development of certain cancers. Understanding the different types and their associated risks is crucial for preventative measures and early detection.HPV infections are incredibly prevalent globally.
The World Health Organization estimates that most sexually active individuals will contract at least one type of HPV at some point in their lives. The prevalence varies across demographics, with factors like age, sexual behavior, and geographic location playing significant roles. For instance, higher rates of infection are typically observed in younger populations and regions with limited access to HPV vaccination programs.
HPV Types and Cancer Risk
Not all HPV types pose the same cancer risk. HPVs are categorized as either low-risk or high-risk, based on their association with cancerous and precancerous lesions. Low-risk HPVs are usually associated with genital warts, while high-risk HPVs are linked to a greater likelihood of developing cancers, including cervical, anal, vaginal, vulvar, penile, and oropharyngeal cancers. Specific high-risk types, such as HPV 16 and 18, are responsible for the majority of HPV-related cancers.
The persistence of high-risk HPV infection is a key factor in cancer development; the longer the infection remains, the greater the risk.
Prevalence of HPV Infections
The global prevalence of HPV infection is substantial, with estimates suggesting that most sexually active individuals will be infected at some point in their lives. However, the specific prevalence rates vary widely depending on geographic location, socioeconomic factors, and screening practices. Developed nations often have better access to screening and vaccination programs, leading to lower rates of persistent HPV infections and related cancers compared to developing countries.
For example, studies in high-income countries might show lower rates of cervical cancer due to widespread cervical cancer screening programs, while data from low-income countries might reveal higher incidence rates due to limited access to such preventative measures. Understanding these disparities is critical for implementing effective public health strategies.
The Link Between HPV and Cancer
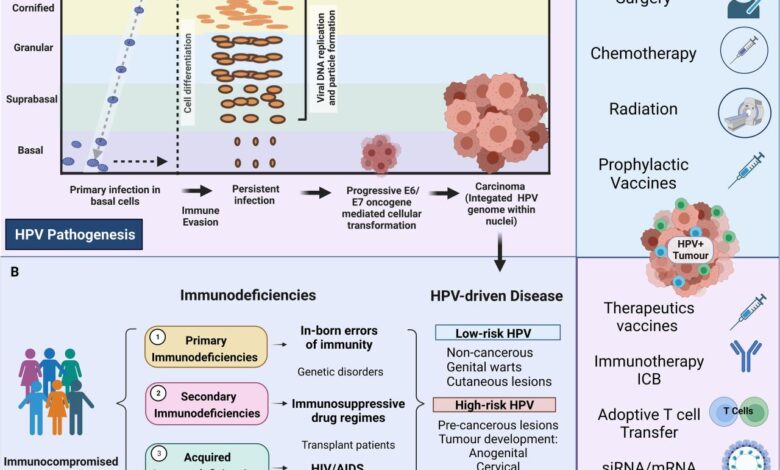
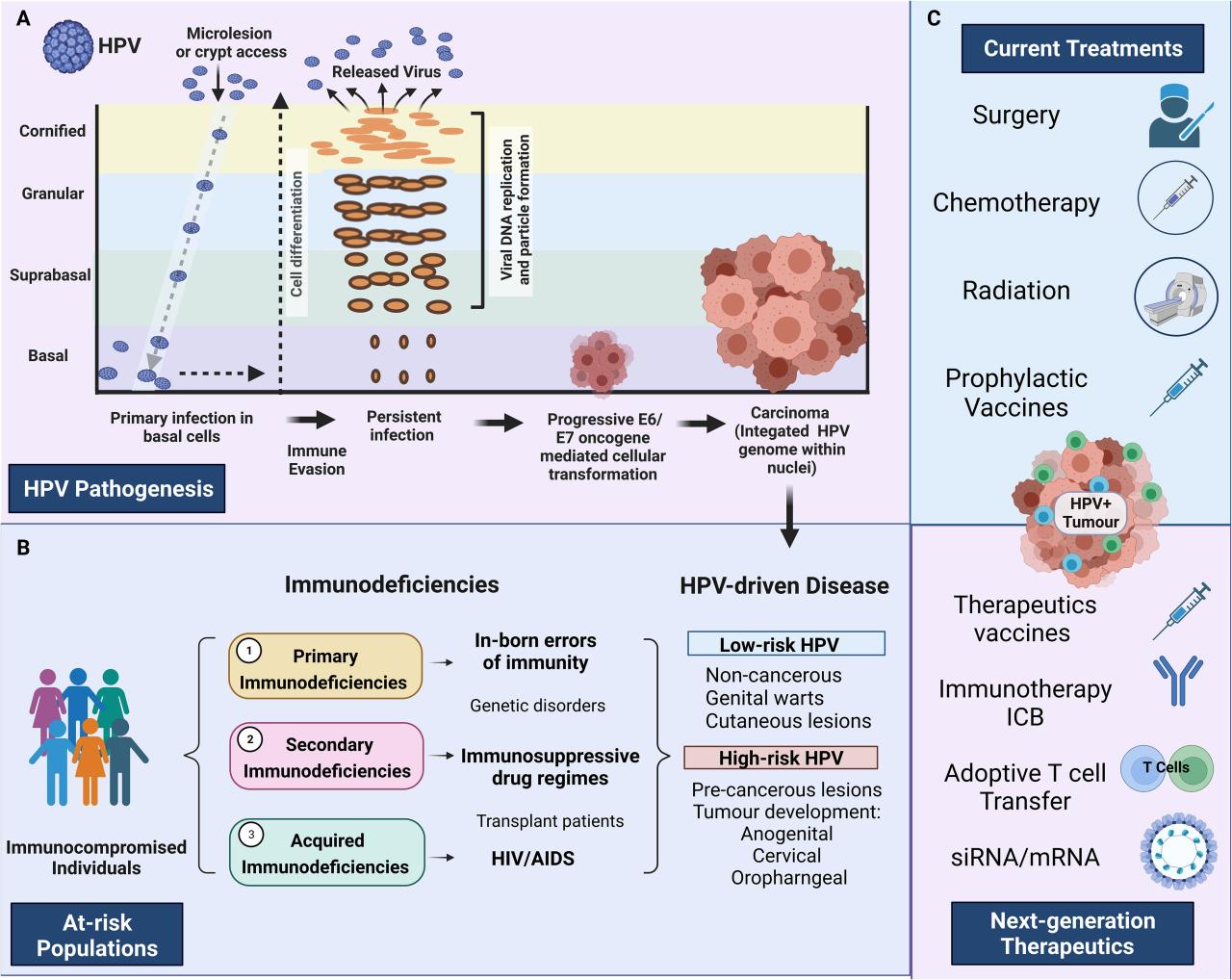
Human papillomavirus (HPV) is a common virus, with many people unknowingly carrying it at some point in their lives. While most HPV infections clear on their own without causing any health problems, some types of HPV can persist and lead to the development of certain cancers. Understanding the mechanisms behind this transformation is crucial for effective prevention and treatment strategies.HPV causes cancer through a complex process involving viral persistence, integration of the viral genome into the host cell DNA, and disruption of cellular processes that regulate cell growth and death.
Specifically, certain viral proteins, like E6 and E7, interfere with tumor suppressor genes, p53 and Rb, respectively. These genes normally control cell division and prevent uncontrolled growth. By inactivating these guardians, HPV creates an environment conducive to cancerous transformation. This process unfolds over years, and several factors influence whether an infection progresses to cancer.
Specific Cancers Linked to HPV Infection
Several types of cancer are strongly associated with persistent HPV infection. Cervical cancer is the most well-known example, with nearly all cases linked to high-risk HPV types. However, HPV is also a significant risk factor for other cancers, including anal cancer, oropharyngeal cancer (cancer of the back of the throat, including the base of the tongue and tonsils), vaginal cancer, vulvar cancer, and penile cancer.
The incidence of HPV-related cancers varies depending on factors such as geographic location, screening practices, and vaccination rates. For instance, oropharyngeal cancer rates, particularly among men, have been rising in recent years, largely attributed to an increase in oral HPV infections.
High-Risk vs. Low-Risk HPV Types
Not all HPV types pose the same cancer risk. Over 100 types of HPV exist, and they are categorized as either high-risk or low-risk based on their potential to cause cancer. High-risk HPV types, such as HPV 16 and 18, are more likely to persist and integrate into the host cell’s DNA, leading to a higher probability of cancer development.
Low-risk HPV types, such as HPV 6 and 11, are less likely to cause cancer but can still cause genital warts. The risk of cancer development is significantly higher with high-risk HPV types compared to low-risk types. For example, HPV 16 and 18 are responsible for approximately 70% of cervical cancers worldwide, highlighting the disparity in oncogenic potential between different HPV types.
While low-risk HPV types can cause benign lesions, their association with cancer is considerably less pronounced. The persistent presence of high-risk HPV is the key differentiator in cancer risk.
Factors Influencing Cancer Development
While HPV infection is a necessary cause of several cancers, it’s crucial to understand that not all HPV infections lead to cancer. Many factors influence whether an infection progresses to cancer. These factors interact in complex ways, highlighting the importance of a holistic view of cancer development.The development of HPV-related cancers is a multi-step process, influenced by both the virus itself and the individual’s characteristics and lifestyle.
Persistent infection, meaning the virus remains in the body for an extended period, is a critical factor. Other factors, like a weakened immune system, can significantly increase the risk of progression.
Persistent HPV Infection and Cancer Progression
Persistent infection with high-risk HPV types is the primary driver of cancer development. The body’s immune system usually clears HPV infections within a couple of years. However, if the immune system fails to eliminate the virus, it can persist and integrate its DNA into the host cell’s genome. This integration can disrupt normal cell function, leading to uncontrolled cell growth and ultimately, cancer.
The longer the infection persists, the greater the chance of cellular changes that could eventually become cancerous. Studies consistently demonstrate a strong correlation between persistent HPV infection and the development of cervical, anal, and other HPV-related cancers.
Role of a Weakened Immune System
A compromised immune system significantly increases the risk of persistent HPV infection and subsequent cancer development. Individuals with weakened immune systems, such as those with HIV/AIDS, organ transplant recipients taking immunosuppressant drugs, or those undergoing chemotherapy, are at higher risk. Their bodies are less effective at clearing the virus, allowing it to persist and potentially lead to cancer. This underscores the importance of maintaining a strong immune system through healthy lifestyle choices and appropriate medical care.
The Impact of Smoking
Smoking is a well-established risk factor for several cancers, including those linked to HPV. Smoking impairs the immune system’s ability to fight off infections, including HPV. Furthermore, the carcinogens in tobacco smoke can damage DNA, increasing the risk of cancerous changes in cells already infected with HPV. This synergistic effect of smoking and HPV infection dramatically elevates the risk of cancer development.
For example, women who smoke and are infected with high-risk HPV types have a significantly higher risk of developing cervical cancer compared to women who are only infected with HPV or only smoke.
Duration of HPV Infection and Cancer Risk
The duration of HPV infection is strongly correlated with cancer risk. While most HPV infections resolve spontaneously within a few years, those that persist for longer periods pose a much greater risk. The exact timeframe varies depending on the HPV type and individual factors, but prolonged infection significantly increases the likelihood of precancerous lesions and, eventually, cancer. Studies have shown that the risk of cervical cancer increases dramatically with the duration of high-risk HPV infection, emphasizing the importance of regular screenings and early detection.
HPV Infection and the Immune System
Our immune system is a complex network designed to protect us from invaders, including viruses like HPV. Understanding how this system interacts with HPV is crucial to comprehending the development of HPV-related cancers. A robust immune response is typically effective at clearing the infection before it can cause harm, but several factors can interfere with this process.The majority of HPV infections are transient, meaning they are cleared by the body’s immune system within a couple of years without any intervention.
This process involves various immune cells, including T cells, which directly attack infected cells, and antibodies, which neutralize the virus. The effectiveness of this response depends on several factors, including the individual’s overall health, the specific HPV type, and the viral load.
Immune System Clearance of HPV Infections
A healthy immune system typically mounts a targeted response to HPV. This involves the recognition of HPV-infected cells by the immune system, followed by the destruction of these cells through a process called cell-mediated immunity. Cytotoxic T lymphocytes (CTLs), a type of T cell, play a crucial role in this process by directly killing infected cells. Helper T cells also contribute by releasing cytokines, which are signaling molecules that enhance the immune response.
Additionally, antibodies produced by B cells can help neutralize the virus and prevent its spread. This coordinated effort usually leads to the successful eradication of the infection, preventing long-term persistence and reducing the risk of cancer development. The time it takes for the immune system to clear the infection varies, but it’s often within two years.
Immune System Failure to Clear HPV Infection
In some cases, the immune system fails to effectively clear the HPV infection. This can be due to several reasons. A weakened immune system, for example, due to conditions like HIV/AIDS or immunosuppressive medications, can significantly impair the body’s ability to fight off the virus. The specific HPV type also plays a role; high-risk HPV types, like HPV 16 and 18, are more likely to persist and evade immune detection compared to low-risk types.
Furthermore, factors like genetics, age, and lifestyle choices can influence the immune response and the likelihood of persistent infection. For instance, smoking can negatively impact immune function, increasing the risk of persistent HPV infection. Finally, a high viral load, meaning a large number of HPV particles, can overwhelm the immune system, making it more difficult to clear the infection.
Implications of a Compromised Immune System on HPV-Related Cancer Risk
A compromised immune system significantly increases the risk of persistent HPV infection and subsequent cancer development. Individuals with weakened immune systems, such as those with HIV/AIDS or undergoing organ transplantation, are at a much higher risk of developing HPV-related cancers. This is because their immune system is less capable of effectively clearing the infection, allowing the virus to persist and potentially lead to cellular changes that can eventually result in cancer.
The duration of persistent infection is also a critical factor; the longer the virus remains in the body, the greater the risk of cancer development. Therefore, maintaining a strong immune system is crucial in preventing HPV-related cancers. A healthy lifestyle, including a balanced diet, regular exercise, and avoidance of smoking, can contribute to a robust immune response and help reduce the risk of persistent HPV infection.
So, I was reading about whether all HPV infections lead to cancer – a doctor explains it’s far more nuanced than you might think. It got me thinking about how many health issues have similar complexities, like the increased risk of severe stroke. Understanding those risk factors that make stroke more dangerous is just as crucial as knowing the specifics of HPV and cancer prevention.
Ultimately, proactive health awareness, regardless of the condition, is key.
HPV Vaccination and Prevention
The HPV vaccine is a powerful tool in preventing infections with high-risk types of human papillomavirus (HPV), significantly reducing the risk of developing HPV-related cancers. It’s a proactive measure that offers substantial protection against a group of viruses known to cause a significant portion of cervical, anal, vaginal, vulvar, and oropharyngeal cancers. Understanding its effectiveness and recommended usage is crucial for public health.The HPV vaccine’s effectiveness lies in its ability to generate a strong immune response against specific HPV types.
Currently available vaccines target multiple high-risk HPV types, such as HPV 16 and 18, which are responsible for the majority of cervical cancers, and other types associated with other HPV-related cancers. Studies have shown a high degree of effectiveness in preventing infection with these targeted types, resulting in a substantial decrease in precancerous lesions and, consequently, cancer incidence.
The vaccine doesn’t treat existing infections, but it’s highly effective at preventing new infections. Protection levels vary depending on the vaccine type and the targeted HPV types, but generally, efficacy remains high several years after vaccination.
Recommended Age Groups for HPV Vaccination
The recommended age for HPV vaccination is typically between 11 and 12 years old, although it can be administered as early as 9 years old and up to 26 years old for individuals who have not been previously vaccinated. This age range is chosen because it is before most individuals become sexually active, maximizing the vaccine’s preventative effect. Vaccination before sexual exposure provides the best protection against HPV infection.
For individuals who did not receive the vaccine during their adolescence, catching up on the vaccine series later in life is still beneficial, though the level of protection might vary slightly compared to vaccination in pre-adolescence. The vaccination schedule involves two or three doses, depending on the vaccine type and age at vaccination. Catch-up vaccination schedules are available for those who missed their adolescent vaccination opportunity.
This highlights the importance of routine childhood vaccination programs, ensuring wide access and coverage to maximize the public health benefits.
HPV Vaccination and Cancer Incidence Reduction, Do all hpv infections lead to cancer doctor explains
Large-scale vaccination programs have demonstrated a significant impact on reducing the incidence of HPV-related cancers. For example, studies in countries with widespread HPV vaccination programs have shown a considerable decline in precancerous cervical lesions in young women, indicating a reduction in the long-term risk of cervical cancer. While the full impact of HPV vaccination on cancer incidence takes time to manifest, due to the long latency period between HPV infection and cancer development, the trend towards reduced precancerous lesions is a strong indicator of future cancer reduction.
These findings support the significant role of HPV vaccination in achieving substantial reductions in the global burden of HPV-related cancers, reinforcing its importance as a preventative healthcare strategy. Continued monitoring and analysis of vaccination programs are essential to fully assess the long-term impact on cancer rates and to guide further improvements in vaccination strategies.
HPV Testing and Screening
Regular screening is crucial for detecting HPV infections and precancerous changes before they progress to cancer. Several methods exist, each with its own strengths and limitations. Understanding these methods and their interpretation is key to effective preventative care.
Available HPV Tests and Screening Methods
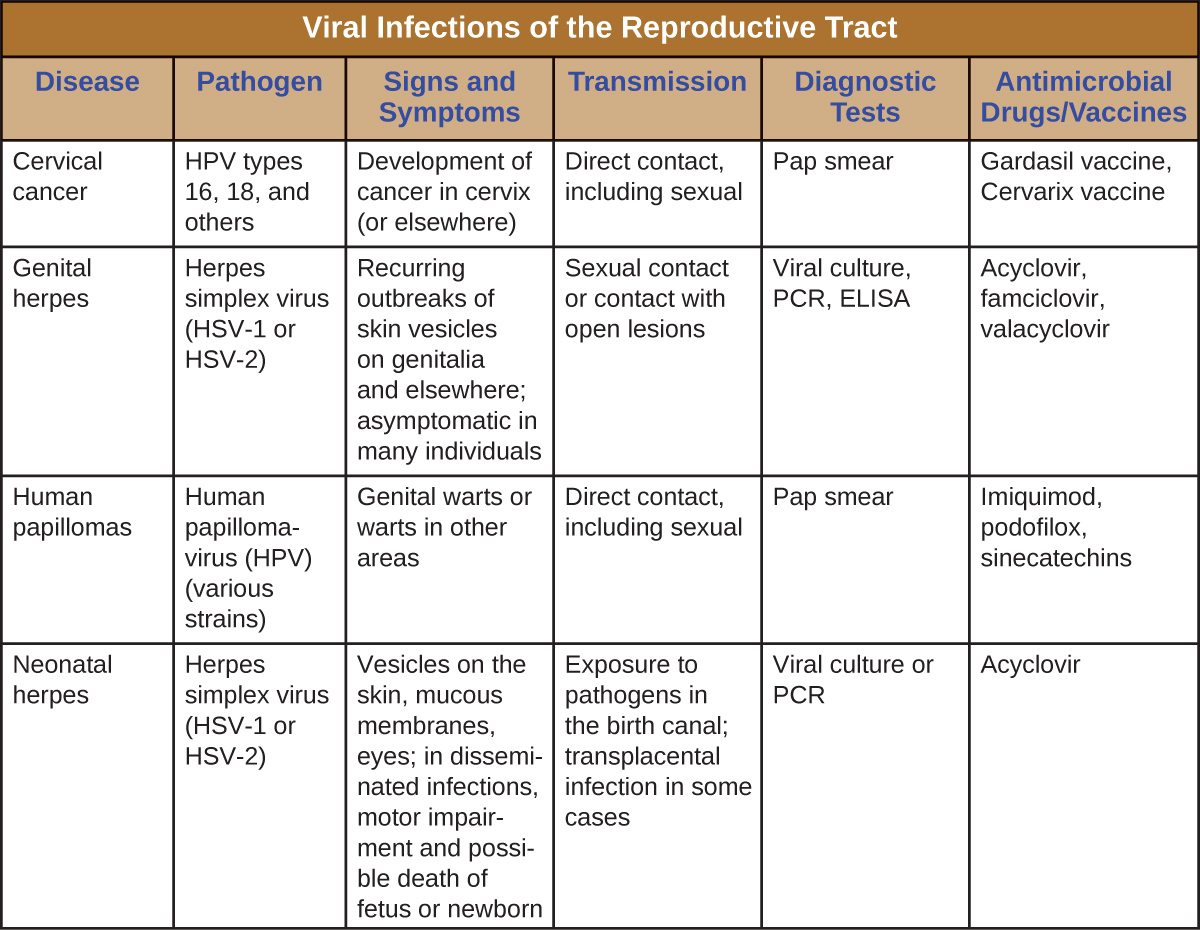
HPV testing and screening primarily involve two main methods: the Pap smear (cervical cytology) and the HPV DNA test. A Pap smear examines cells from the cervix for abnormalities, while an HPV DNA test directly detects the presence of high-risk HPV types. These tests can be used alone or in combination, depending on age, risk factors, and guidelines.
In some cases, visual inspection with acetic acid (VIA) may also be used, particularly in resource-limited settings. This involves applying acetic acid to the cervix, which causes abnormal areas to appear white.
Purpose and Interpretation of HPV Test Results
The purpose of HPV testing is to identify the presence of high-risk HPV types that are strongly linked to cervical cancer. A positive HPV DNA test result indicates the presence of these high-risk types. However, it’s crucial to remember that a positive result doesn’t automatically mean cancer. Many women with high-risk HPV infections clear the virus naturally without developing any health problems.
So, the question of whether all HPV infections lead to cancer is complex, as a doctor explained in a recent article. It’s a bit like understanding the varied presentations of neurological conditions; for example, managing Tourette Syndrome in children requires a multifaceted approach, as detailed in this helpful resource: strategies to manage Tourette syndrome in children. Similarly, HPV’s impact varies widely, highlighting the need for regular screenings and preventative measures.
Ultimately, early detection is key for both conditions.
A negative result suggests the absence of detectable high-risk HPV DNA at the time of testing. However, it doesn’t guarantee future infection. Pap smear results describe the appearance of cervical cells, identifying abnormalities that may be caused by HPV or other factors. Abnormal Pap smear results may warrant further investigation, such as HPV testing or colposcopy.
Recommended Screening Frequency
The recommended frequency of HPV testing and screening varies based on age and individual risk factors. Current guidelines generally recommend starting regular screening at age 21 with Pap smears. The frequency of Pap smears may change based on results and risk factors. HPV testing is often incorporated into screening strategies, particularly for women aged 30 and older.
Women with a history of abnormal Pap smears or HPV infections may require more frequent screening. Women with weakened immune systems or those exposed to other risk factors might also need more frequent monitoring. It’s essential to discuss individual screening needs with a healthcare provider to determine the most appropriate approach.
Comparison of Screening Methods
| Method | Accuracy | Frequency | Advantages | Disadvantages |
|---|---|---|---|---|
| Pap Smear | High for detecting precancerous changes, but lower for detecting HPV itself | Every 3 years (age 21-29), or every 5 years with HPV co-testing (age 30-65) | Widely available, relatively inexpensive, established method | Can miss some precancerous lesions, requires adequate cell sampling |
| HPV DNA Test | High for detecting high-risk HPV types | Every 5 years with Pap co-testing (age 30-65) | Directly detects high-risk HPV, can improve detection of precancerous changes | More expensive than Pap smear alone, false positives are possible |
| Co-testing (Pap Smear + HPV DNA Test) | Highest accuracy for detecting both precancerous changes and high-risk HPV | Every 5 years (age 30-65) | Combines advantages of both tests, reduces the need for more frequent testing | More expensive than Pap smear alone |
| Visual Inspection with Acetic Acid (VIA) | Moderate accuracy, highly dependent on examiner skill | Frequency varies depending on context and resources | Low cost, simple procedure, suitable for resource-limited settings | Subjective interpretation, lower sensitivity and specificity compared to other methods |
Treatment Options for HPV Infections: Do All Hpv Infections Lead To Cancer Doctor Explains
Unfortunately, there’s no cure for HPV itself. The virus can remain latent in the body for years, sometimes clearing on its own. Treatment focuses on managing symptoms, addressing precancerous changes, and preventing cancer development. The approach depends on the type of HPV and the health issues it causes.Treatment options primarily target the consequences of HPV infection, not the virus directly.
This means addressing any genital warts, precancerous lesions, or cancers that may arise. The goal is to eliminate or reduce the risk of these complications and improve the patient’s quality of life. It’s crucial to remember that treatment success varies depending on individual factors like immune system strength and the specific HPV type involved.
Treatment of Genital Warts
Genital warts, caused by certain low-risk types of HPV, are often treated with topical medications or procedures to remove the warts. These treatments aim to eliminate visible warts and alleviate symptoms like itching and discomfort. Common topical treatments include imiquimod, podofilox, and sinecatechins. Procedures like cryotherapy (freezing), laser surgery, or surgical excision may be used for larger or persistent warts.
While these treatments can effectively remove warts, they don’t eliminate the HPV virus itself; recurrence is possible.
Management of Precancerous Lesions
Precancerous lesions, also known as cervical intraepithelial neoplasia (CIN) or high-grade squamous intraepithelial lesions (HSIL), are abnormal cell growth on the cervix that can develop into cervical cancer if left untreated. Management depends on the severity of the lesion. Mild lesions may be monitored closely with regular Pap smears and HPV tests. More severe lesions may require procedures like loop electrosurgical excision procedure (LEEP), cold knife conization, or laser ablation to remove the abnormal tissue.
These procedures aim to prevent the progression to cancer. The choice of treatment is individualized and based on factors such as lesion size, grade, and patient’s overall health.
Treatment of HPV-Related Cancers
If HPV infection leads to cancer, treatment focuses on the cancer itself, using standard cancer therapies such as surgery, radiation therapy, chemotherapy, or targeted therapy. The specific treatment plan depends on the type and stage of cancer, as well as the patient’s overall health. For example, cervical cancer treatment might involve surgery to remove the cancerous tissue, followed by radiation therapy or chemotherapy to destroy any remaining cancer cells.
The aim is to remove or destroy the cancerous tissue and prevent its recurrence. The effectiveness of treatment varies greatly depending on factors like the stage of cancer at diagnosis and the patient’s response to treatment.
Potential Side Effects of HPV Treatments
Treatment for HPV-related conditions can have side effects, which vary depending on the specific treatment used. Topical treatments for genital warts may cause skin irritation, burning, or redness. Procedures to remove precancerous lesions or warts can cause bleeding, pain, scarring, and infection. Cancer treatments can have a wider range of side effects, including fatigue, nausea, hair loss, and changes in bowel or bladder function.
The severity and duration of side effects vary from person to person. Open communication with a healthcare provider is crucial to manage these side effects effectively.
Addressing Patient Concerns and Misconceptions
Source: philschatz.com
So, I was reading about whether all HPV infections lead to cancer – a doctor explains it’s not a guaranteed outcome, thankfully. It got me thinking about overall health, and I saw this article about Monali Thakur being hospitalized after breathing difficulties: monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases. It’s a reminder that maintaining good overall health, which includes preventative measures, is key, regardless of the specific health concern, whether it’s HPV or respiratory issues.
Understanding HPV and its potential link to cancer can be anxiety-inducing, leading to many questions and, unfortunately, several misconceptions. It’s crucial to address these concerns with accurate information to alleviate fears and promote informed decision-making. This section aims to clarify common misunderstandings and provide straightforward answers to frequently asked questions.Many individuals harbor inaccurate beliefs about HPV and its connection to cancer.
These misconceptions often stem from a lack of comprehensive information or from misinformation spread through unreliable sources. Addressing these directly is vital for empowering patients to make informed choices about their health.
Common Misconceptions about HPV and Cancer
It’s important to dispel several myths surrounding HPV and cancer risk. Many people believe that HPV infection automatically leads to cancer, which is simply untrue. Others underestimate the importance of vaccination or screening. Let’s address these misconceptions with factual information.
- Misconception: All HPV infections lead to cancer. Fact: The vast majority of HPV infections clear on their own within two years without causing any health problems. Only certain high-risk types of HPV are linked to cancer development, and even then, cancer development is not guaranteed. Many factors influence whether an infection progresses to cancer.
- Misconception: Only sexually active people can get HPV. Fact: While HPV is primarily transmitted through sexual contact, it’s possible to contract it through other means, although less common. For example, mother-to-child transmission during birth is a possibility.
- Misconception: HPV vaccines are only for girls/women. Fact: HPV vaccines are available and recommended for both boys and girls, as they protect against the HPV types that can cause cancers in both genders, including anal, throat, and penile cancers.
- Misconception: If I’ve had HPV, I’m immune. Fact: There are many different types of HPV, and immunity to one type doesn’t guarantee immunity to others. It’s possible to be infected with multiple types over a lifetime.
- Misconception: HPV tests are only necessary if I have symptoms. Fact: Many HPV infections are asymptomatic. Regular screening, particularly for women, is crucial for early detection and intervention, even in the absence of noticeable symptoms.
Frequently Asked Questions about HPV and Cancer
Understanding the answers to common questions can significantly reduce anxiety and improve patient compliance with preventative measures and screenings. Below are some frequently asked questions, addressed clearly and concisely.
- Question: How can I reduce my risk of getting HPV? Answer: Vaccination is the most effective preventive measure. Practicing safe sex, such as using condoms, can also help reduce the risk of transmission.
- Question: What are the symptoms of HPV? Answer: Many HPV infections have no symptoms. When symptoms do occur, they can vary widely depending on the type of HPV and the affected area. Genital warts are a common symptom of some low-risk HPV types.
- Question: How is HPV diagnosed? Answer: Diagnosis typically involves a Pap smear for women and visual inspection or other tests for men. HPV DNA testing can also be used to identify specific HPV types.
- Question: What are the treatment options for HPV? Answer: Treatment focuses on managing symptoms and preventing complications. Treatment options vary depending on the type of HPV and the presence of any related conditions, such as genital warts or precancerous lesions.
- Question: Is HPV curable? Answer: While the HPV infection itself may clear on its own, there is no cure for the virus itself. However, treatment is available to manage symptoms and prevent progression to cancer.
Illustrative Examples
Understanding the impact of HPV infection requires examining both successful immune clearance and persistent infection leading to cancer. These case studies, while fictionalized to protect patient privacy, represent the spectrum of HPV infection outcomes. It is crucial to remember that these are examples and individual experiences can vary greatly.
Persistent HPV Infection Leading to Cervical Cancer
This case study follows a 45-year-old woman, Sarah, who developed cervical cancer. Sarah had a history of multiple sexual partners and began experiencing abnormal vaginal bleeding and pelvic pain at age 43. Her risk factors included a lack of regular Pap smears and a history of smoking. A Pap smear revealed abnormal cells, and a subsequent colposcopy and biopsy confirmed the presence of high-grade squamous intraepithelial lesions (HSIL) caused by persistent HPV type 16 infection.
Over the next two years, the lesion progressed despite treatment with cryotherapy. Further biopsies confirmed invasive cervical cancer. Sarah underwent a radical hysterectomy, followed by chemotherapy and radiation therapy. While her cancer is currently in remission, she requires ongoing monitoring. This case highlights the importance of regular screenings and the potential for HPV to cause cancer even with timely intervention if the infection persists.
Successful Immune Clearance of HPV Infection
This case study focuses on a 22-year-old woman, Emily, who was diagnosed with an HPV infection following a routine Pap smear. Emily reported having one long-term sexual partner. The Pap smear showed low-grade squamous intraepithelial lesions (LSIL) associated with HPV type 6. Emily had no other significant risk factors. Her physician recommended repeat Pap smears in six months.
At the follow-up appointment, the LSIL had resolved, and the Pap smear was normal. This indicates that Emily’s immune system successfully cleared the HPV infection. This case demonstrates that many HPV infections are transient and resolve without intervention thanks to a robust immune system.
Last Point
Source: frontiersin.org
So, do all HPV infections lead to cancer? The short answer is no. While HPV is a significant risk factor for certain cancers, the vast majority of infections resolve without issue. However, understanding the different types of HPV, the role of your immune system, and the availability of preventative measures like vaccination and regular screenings are key to protecting your health.
Remember, knowledge is power, and armed with this information, you can make informed choices to minimize your risk.
Query Resolution
Can I get HPV from something other than sexual contact?
While most HPV infections are sexually transmitted, some types can be spread through skin-to-skin contact. However, the vast majority of HPV infections are acquired through sexual activity.
If I have HPV, does that mean I’ll definitely get cancer?
No. Most HPV infections clear up on their own without causing any health problems. Only certain high-risk types of HPV are linked to cancer development, and even then, cancer development is not guaranteed.
How often should I get screened for HPV?
Screening recommendations vary based on age and risk factors. Talk to your doctor to determine the appropriate screening schedule for you. Regular Pap smears and HPV tests are important tools in early detection.
Is there a cure for HPV?
There’s no cure for HPV itself, but treatments are available to manage precancerous lesions and prevent cancer development. These treatments can help eliminate the virus or the abnormal cells it causes.
