Early Signs of Osteopenia & Osteoporosis Prevention Tips
Early signs of osteopenia and tips to prevent osteoporosis – it’s a topic that might seem a bit dry, but trust me, it’s incredibly important! We all want strong, healthy bones, right? This isn’t just about avoiding fractures later in life; it’s about maintaining your independence and enjoying an active life for as long as possible. This post will delve into the subtle signs of weakening bones, explore the risk factors, and most importantly, give you practical steps to protect your skeletal system.
Let’s get started!
Understanding the difference between osteopenia and osteoporosis is crucial. Osteopenia is essentially a precursor to osteoporosis – a condition where your bones become less dense, making them more prone to fractures. Osteoporosis, on the other hand, is a more severe stage characterized by significantly weakened bones and a heightened risk of breaks. While both conditions often share similar symptoms like back pain and decreased height, osteoporosis typically presents more severe symptoms and a greater risk of fractures.
Early detection and intervention are key to slowing or even reversing bone loss. We’ll explore the tell-tale signs, risk factors, and lifestyle changes you can implement to protect your bone health.
Understanding Osteopenia and Osteoporosis
Osteopenia and osteoporosis are both conditions characterized by low bone mass, increasing the risk of fractures. However, they represent different stages in the bone loss process, with osteoporosis signifying a more severe and advanced state. Understanding the distinctions between these two conditions is crucial for effective prevention and management.Osteopenia and Osteoporosis: A Detailed Comparison
Bone Density and Fracture Risk
Osteopenia is defined as bone mineral density (BMD) that’s lower than normal but not yet low enough to be classified as osteoporosis. Think of it as a warning sign – your bones are weaker than they should be, but not critically so. Osteoporosis, on the other hand, is characterized by significantly lower BMD, making bones considerably more fragile and susceptible to fractures even from minor falls or bumps.
The fracture risk is substantially higher in osteoporosis compared to osteopenia. For example, a person with osteopenia might have a slightly increased risk of a wrist fracture, while someone with osteoporosis faces a significantly higher risk of hip, spine, and wrist fractures.
Progression from Osteopenia to Osteoporosis
Osteopenia often precedes osteoporosis. It’s a gradual process where bone loss accumulates over time. If bone loss continues unchecked, osteopenia can progress to osteoporosis. Several factors influence this progression, including genetics, lifestyle choices (diet, exercise, smoking), and hormonal changes. For instance, a post-menopausal woman with osteopenia might develop osteoporosis if she doesn’t take steps to protect her bone health.
The transition isn’t always linear; some individuals with osteopenia may maintain their bone density, while others may progress to osteoporosis at varying rates.
Symptoms of Osteopenia and Osteoporosis
Both osteopenia and osteoporosis often have no noticeable symptoms in their early stages. The first indication is frequently a fracture, particularly a vertebral fracture (in the spine) which might present as back pain or a loss of height. As osteoporosis advances, more significant fractures may occur, leading to pain, deformity, and reduced mobility. Osteopenia rarely causes symptoms unless a fracture occurs.
The absence of symptoms in the early stages highlights the importance of regular bone density screenings, especially for individuals at higher risk.
Comparison of Osteopenia and Osteoporosis
| Bone Density | Fracture Risk | Symptoms | Treatment |
|---|---|---|---|
| Lower than normal, but not severely low | Increased, but lower than in osteoporosis | Often asymptomatic; fractures may be the first sign | Lifestyle modifications, medication in some cases |
| Significantly lower than normal | Substantially increased, especially for hip, spine, and wrist fractures | Often asymptomatic until a fracture occurs; pain, deformity, and reduced mobility may occur with advanced disease | Lifestyle modifications, medication (bisphosphonates, denosumab, etc.) |
Early Signs and Symptoms of Osteopenia

Source: slidesharecdn.com
Osteopenia, a condition characterized by bone mineral density lower than normal but not yet low enough to be classified as osteoporosis, often presents subtly. Many individuals experience no noticeable symptoms in the early stages, making early detection crucial. Understanding the potential signs, however slight, can empower individuals to take proactive steps toward bone health.Osteopenia’s primary manifestation is decreased bone strength and increased bone fragility.
This translates to a heightened risk of fractures, even from seemingly minor impacts. The body’s ability to repair micro-fractures, common occurrences in daily life, is also compromised. This progressive weakening can lead to significant bone loss and eventually osteoporosis if left unaddressed.
Subtle Signs of Osteopenia Often Overlooked
Many individuals dismiss early symptoms of osteopenia as normal age-related changes. However, persistent aches, pains, and stiffness, especially in the back or hips, warrant attention. A slight decrease in height over time, often unnoticed unless compared to old photographs, can also be an indicator. Furthermore, a persistent feeling of fatigue or weakness, unrelated to other health conditions, might be linked to bone loss.
These subtle cues should not be ignored, especially in individuals with risk factors for osteopenia, such as family history or hormonal imbalances.
Decreased Bone Strength and Increased Bone Fragility
The reduced bone density associated with osteopenia directly impacts bone strength and increases fragility. This translates into a higher likelihood of fractures, even from relatively minor falls or bumps. For example, a simple stumble could result in a wrist fracture in someone with osteopenia, whereas a healthy individual might only experience minor bruising. Similarly, a seemingly insignificant strain during exercise or daily activities might cause a stress fracture.
The decreased ability to withstand everyday stresses is a key indicator of the condition’s progression. This increased fragility isn’t always apparent until a fracture occurs, highlighting the importance of preventative measures and regular bone density screenings.
Examples of Osteopenia Symptom Manifestation
Consider a 60-year-old woman who experiences increasing back pain, initially attributing it to aging. This pain, however, doesn’t respond to over-the-counter pain relievers and worsens with activity. Another example is a 55-year-old man who notices he’s become shorter over the past few years, a change he initially dismisses. These scenarios, while seemingly minor, could indicate underlying osteopenia.
In both cases, a visit to a healthcare professional for a bone density scan is recommended to rule out or confirm the diagnosis. Early detection through proactive screening and attention to subtle symptoms can significantly impact the management and prevention of more serious bone loss.
Importance of Early Detection in Preventing Further Bone Loss
Early detection of osteopenia is critical because it allows for timely intervention. Lifestyle modifications, such as increased calcium and vitamin D intake, regular weight-bearing exercise, and smoking cessation, can significantly slow or even reverse bone loss. In some cases, medication may be prescribed to help improve bone density. The earlier these interventions are implemented, the more effective they are in preventing the progression to osteoporosis, a condition associated with significantly increased fracture risk and associated health complications.
Delaying treatment can lead to more severe bone loss, increasing the risk of debilitating fractures and reducing quality of life.
Risk Factors for Osteopenia and Osteoporosis
Understanding the risk factors for osteopenia and osteoporosis is crucial for prevention and early intervention. These conditions, characterized by decreased bone density and increased fracture risk, are influenced by a complex interplay of genetic predispositions and lifestyle choices. Identifying and managing these risk factors can significantly improve bone health and reduce the likelihood of developing these debilitating diseases.
Categorization of Risk Factors
Risk factors for osteopenia and osteoporosis are broadly categorized into age-related factors, gender-related factors, family history, medical conditions, and lifestyle factors. These factors often interact, meaning that the presence of multiple risk factors significantly increases the overall risk. For example, a postmenopausal woman with a family history of osteoporosis and a sedentary lifestyle faces a much higher risk than a younger, active woman with no family history.
Age and Gender as Risk Factors
Age is a significant risk factor, with bone density naturally declining with age in both men and women. However, the rate of decline and the overall impact are more pronounced in women, particularly after menopause due to the significant drop in estrogen levels. This hormonal shift accelerates bone loss, increasing the risk of osteoporosis. Men also experience bone loss with age, though typically at a slower rate.
This age-related bone loss starts subtly in the 30s and 40s, becoming more significant after 50.
Family History and Genetic Predisposition
A family history of osteoporosis significantly increases an individual’s risk. This suggests a genetic component influencing bone density and strength. If a close family member (parent or sibling) has experienced an osteoporotic fracture, the risk is heightened. Genetic factors influence bone metabolism and the body’s ability to absorb and utilize calcium.
Medical Conditions Affecting Bone Health
Several medical conditions can increase the risk of osteopenia and osteoporosis. These include endocrine disorders like hypothyroidism and hyperparathyroidism, which directly affect calcium metabolism. Gastrointestinal diseases that interfere with nutrient absorption, such as Crohn’s disease and celiac disease, can also impair bone health. Long-term use of certain medications, such as corticosteroids, can also weaken bones.
Lifestyle Factors Influencing Bone Density
Lifestyle plays a significant role in bone health. A diet lacking in calcium and vitamin D can impair bone formation and strength. Insufficient physical activity, particularly weight-bearing exercise, reduces bone density. Smoking is another major risk factor, as it impairs bone formation and increases bone resorption. Excessive alcohol consumption can also negatively impact bone health.
Infographic Description
The infographic would use a circular design, with “Bone Health Risk Factors” in the center. Radiating outwards would be six sections, each representing a major risk factor category (age, gender, family history, medical conditions, diet, and lifestyle). Each section would use a different color, with lighter shades representing lower risk and darker shades representing higher risk. Data visualization would involve icons representing each risk factor (e.g., a calendar for age, a figure for gender, a family tree for family history) within each section, with the size of the icons correlating to the relative risk.
Catching early signs of osteopenia, like decreased bone density, is crucial for preventing osteoporosis later in life. Regular weight-bearing exercise and a calcium-rich diet are key preventative measures. Interestingly, managing underlying conditions can also impact bone health; for instance, understanding the challenges faced by families dealing with children’s health issues, such as those outlined in this helpful article on strategies to manage Tourette syndrome in children , highlights the importance of holistic well-being.
This holistic approach extends to bone health, too, emphasizing the need for consistent healthy habits from a young age to build strong bones.
The overall design would be clean and easy to understand, using clear fonts and minimal text.
Prioritized List of Risk Factors
The following list prioritizes risk factors based on their impact, acknowledging that the interaction of multiple factors significantly increases overall risk.
- Age (especially post-menopause in women): The natural decline in bone density accelerates significantly with age, especially after menopause due to hormonal changes.
- Family History of Osteoporosis: A strong genetic component influences bone density and fracture risk.
- Medical Conditions (e.g., endocrine disorders, gastrointestinal diseases): These conditions directly impact calcium metabolism and nutrient absorption.
- Lifestyle Factors (e.g., poor diet, lack of exercise, smoking, excessive alcohol consumption): These modifiable factors significantly influence bone health.
- Gender (female): Women are at a significantly higher risk due to hormonal changes after menopause.
Diagnostic Methods for Osteopenia: Early Signs Of Osteopenia And Tips To Prevent Osteoporosis
Diagnosing osteopenia involves assessing bone mineral density (BMD) to determine if it’s lower than normal for your age and sex. Several methods exist, each with its strengths and weaknesses. Understanding these methods is crucial for effective management and prevention of osteoporosis.
Bone Density Scans (DEXA)
Dual-energy X-ray absorptiometry (DEXA) is the gold standard for measuring bone density. This non-invasive test uses low-dose X-rays to measure BMD in the hip and spine, the areas most prone to fractures. The procedure is quick and painless, taking only about 10-20 minutes. A DEXA scan provides a T-score, which compares your BMD to the average BMD of a healthy young adult of the same sex.
A T-score between -1.0 and -2.5 indicates osteopenia, while a T-score of -2.5 or lower suggests osteoporosis. The Z-score compares your BMD to the average BMD of people your age and sex. This helps to identify individuals who have lower than expected bone density for their age, even if their T-score is within the normal range.
Interpretation of Bone Density Scan Results and the T-score
The T-score is the key indicator in interpreting DEXA results. It’s calculated by comparing your BMD to the peak bone mass of a healthy 30-year-old. A T-score of -1.0 to -2.5 indicates osteopenia, meaning your bone density is lower than normal but not yet at the level of osteoporosis. A T-score of -2.5 or lower signifies osteoporosis, a more severe condition characterized by significantly weakened bones.
Catching osteopenia early is crucial, often showing up as subtle back pain or decreased bone density. Preventing osteoporosis requires a proactive approach, focusing on diet and exercise. Understanding nutritional needs is key, which is why I found this article on are women and men receptive of different types of food and game changing superfoods for women so insightful.
Knowing which superfoods are best for bone health, especially for women, can make a huge difference in preventing future bone problems.
For example, a T-score of -1.8 suggests osteopenia, indicating a need for lifestyle changes and possibly medication to prevent further bone loss and reduce fracture risk. A T-score of -3.0 would be indicative of severe osteoporosis. It’s important to remember that the T-score is just one factor considered in assessing bone health; your medical history, risk factors, and overall health are also important.
Comparison of Diagnostic Techniques
While DEXA is the preferred method due to its accuracy and low radiation exposure, other techniques exist. Conventional X-rays can sometimes reveal fractures or severe bone loss, but they are not as sensitive as DEXA for detecting early stages of osteopenia. Quantitative computed tomography (QCT) provides more detailed information about bone structure, but it exposes patients to higher levels of radiation.
Therefore, DEXA remains the most commonly used and recommended method for diagnosing osteopenia due to its balance of accuracy, safety, and cost-effectiveness.
Step-by-Step Procedure for a Typical Bone Density Scan (DEXA)
1. Preparation No special preparation is usually required for a DEXA scan. You may be asked to remove any jewelry or metal objects that could interfere with the scan.
2. Positioning You will lie on a padded table while the DEXA machine scans your hip and spine. The procedure is painless and takes approximately 10-20 minutes.
3. The Scan The machine emits low-dose X-rays that pass through your bones. A computer then analyzes the X-ray absorption to calculate your BMD.
4. Results Your doctor will review your results and discuss your T-score and Z-score, along with your risk factors, to determine the best course of action.
Preventive Measures and Lifestyle Modifications
Osteopenia and osteoporosis, while often associated with aging, are conditions that can be significantly influenced by lifestyle choices. Taking proactive steps to maintain bone health is crucial, not just for preventing osteoporosis, but also for slowing the progression of osteopenia and improving overall quality of life. By adopting a holistic approach encompassing diet, exercise, and lifestyle changes, we can significantly reduce our risk and build stronger, healthier bones.
Calcium and Vitamin D Intake for Bone Health
Adequate calcium and vitamin D intake are fundamental to bone health. Calcium is the primary building block of bone, while vitamin D facilitates calcium absorption in the gut. A deficiency in either nutrient can significantly impair bone mineralization and increase the risk of bone loss. The recommended daily allowance of calcium varies depending on age and other factors, but generally ranges from 1000 to 1200 mg.
Good dietary sources of calcium include dairy products (milk, yogurt, cheese), leafy green vegetables (kale, spinach), and fortified foods (cereals, plant milks). Vitamin D, often obtained through sunlight exposure, is also crucial. However, insufficient sunlight exposure or limited dietary intake may necessitate supplementation. Many foods are fortified with vitamin D, and supplements are readily available. Consulting a doctor to determine the appropriate calcium and vitamin D intake based on individual needs is always recommended.
The Role of Exercise in Bone Strengthening
Regular weight-bearing and resistance training exercises are vital for maintaining bone density and strength. These exercises stimulate bone cells (osteoblasts) to build new bone tissue, counteracting the natural bone loss that occurs with age. Weight-bearing exercises involve activities where the bones and muscles work against gravity, such as walking, jogging, dancing, climbing stairs, and hiking. Resistance training, on the other hand, involves using weights or resistance bands to strengthen muscles and bones.
Both types of exercise are crucial for optimal bone health. For instance, a study published in the “Journal of Bone and Mineral Research” demonstrated a significant increase in bone mineral density in postmenopausal women who participated in a regular weight-bearing exercise program.
Sample Weekly Exercise Plan
A balanced exercise plan should incorporate both weight-bearing and resistance training activities. This sample plan is a suggestion and should be adjusted based on individual fitness levels and any pre-existing health conditions. Always consult your doctor before starting any new exercise program.
Monday: 30 minutes brisk walking
Tuesday: Resistance training (focus on legs and arms) – 3 sets of 10-12 repetitions for each exercise. Examples include squats, lunges, push-ups, bicep curls, and tricep extensions.
Wednesday: Rest or light activity like yoga or swimming.
Thursday: 30 minutes of dancing or other enjoyable aerobic activity.
Friday: Resistance training (focus on core and back) – 3 sets of 10-12 repetitions for each exercise. Examples include planks, back extensions, and rows.
Catching osteopenia early is key; look out for subtle bone pain and increased fragility. Preventing osteoporosis requires a healthy diet rich in calcium and vitamin D, regular weight-bearing exercise, and avoiding smoking. Interestingly, learning about reproductive health choices, like in this article on karishma mehta gets her eggs frozen know risks associated with egg freezing , reminds us that proactive health decisions span our entire lifespan.
Building strong bones early on is just as crucial as other aspects of well-being.
Saturday: Hiking or another outdoor weight-bearing activity.
Sunday: Rest or light stretching.
Dietary Recommendations for Bone Health
Building strong bones and preventing osteoporosis requires a proactive approach to nutrition. A balanced diet rich in specific nutrients plays a crucial role in maintaining bone density and overall skeletal health throughout your life. This section will explore the dietary components vital for strong bones and provide a practical example of a bone-healthy meal plan.
Calcium-Rich Foods and Their Importance, Early signs of osteopenia and tips to prevent osteoporosis
Calcium is the primary building block of bones. Adequate calcium intake is essential for bone growth and maintenance, particularly during childhood, adolescence, and adulthood. Dairy products like milk, yogurt, and cheese are excellent sources of calcium. However, many non-dairy options also provide significant amounts, including leafy green vegetables (kale, spinach, collard greens), fortified plant milks (soy, almond, oat), canned sardines (with bones), and tofu.
Choosing a variety of these foods ensures you meet your daily calcium needs. The recommended daily allowance of calcium varies depending on age and other factors, so consulting a healthcare professional or registered dietitian is advisable for personalized guidance.
Vitamin D’s Role in Calcium Absorption
Vitamin D isn’t just important for bone health; it’s crucial for calcium absorption. Without sufficient vitamin D, your body struggles to utilize the calcium you consume, leading to weaker bones. Exposure to sunlight is a primary source of vitamin D, but dietary sources are also important. Fatty fish (salmon, tuna, mackerel), egg yolks, and fortified foods (milk, cereals, orange juice) are good choices.
Supplementation might be necessary, especially for individuals with limited sun exposure or those at higher risk of vitamin D deficiency.
Benefits of Vitamin K2 and Magnesium for Bone Health
While calcium and vitamin D often take center stage, vitamin K2 and magnesium are equally important for optimal bone health. Vitamin K2 helps direct calcium to the bones, preventing its deposition in soft tissues like arteries. Leafy green vegetables, fermented foods, and some cheeses are good sources. Magnesium plays a vital role in bone mineralization and calcium metabolism.
Good sources include nuts, seeds, legumes, and whole grains.
Sample Bone-Healthy Weekly Meal Plan
This meal plan provides a balanced intake of calcium, vitamin D, and other bone-supporting nutrients. Remember to adjust portion sizes based on your individual caloric needs and activity level.
| Day | Breakfast | Lunch | Dinner |
|---|---|---|---|
| Monday | Yogurt with berries and almonds | Salad with grilled salmon and a side of steamed broccoli | Lentil soup with whole-wheat bread |
| Tuesday | Oatmeal with milk and a sprinkle of chia seeds | Tuna salad sandwich on whole-wheat bread with a side of carrots and celery | Chicken stir-fry with brown rice and plenty of leafy greens |
| Wednesday | Scrambled eggs with spinach and whole-wheat toast | Leftover chicken stir-fry | Baked cod with roasted vegetables (broccoli, sweet potatoes) |
| Thursday | Smoothie with spinach, banana, milk, and protein powder | Quinoa salad with chickpeas, feta cheese, and cucumbers | Vegetarian chili with cornbread |
| Friday | Whole-wheat pancakes with fruit and a side of yogurt | Leftover vegetarian chili | Pizza on whole-wheat crust with lots of vegetables and low-fat cheese |
| Saturday | Breakfast burrito with scrambled eggs, black beans, and salsa | Salad with grilled chicken and a side of mixed greens | Pasta with marinara sauce and a side salad |
| Sunday | French toast with fruit and a side of bacon | Leftover pasta | Roast chicken with roasted potatoes and green beans |
Negative Impacts of Excessive Sodium and Caffeine
Excessive sodium intake can increase calcium excretion through urine, potentially reducing bone density over time. High caffeine consumption may also interfere with calcium absorption and increase calcium excretion. Moderation is key; limiting processed foods high in sodium and controlling caffeine intake can help protect bone health. For example, aiming for less than 2,300 milligrams of sodium per day and limiting caffeine to moderate amounts is a reasonable goal for most adults.
Medical Interventions and Treatments
Osteopenia and osteoporosis, while sharing a common thread of decreased bone density, require different approaches to treatment depending on the severity of bone loss and individual risk factors. Treatment aims to slow bone loss, prevent fractures, and in some cases, increase bone density. This often involves a combination of lifestyle changes and medication.
Pharmacological Interventions for Osteoporosis
Several medications are available to treat osteoporosis, each working through different mechanisms to improve bone health. The choice of medication depends heavily on factors like the patient’s age, overall health, risk of fractures, and tolerance to potential side effects. Bisphosphonates, for example, are a widely used class of drugs that inhibit bone resorption, the process by which bone is broken down.
They are highly effective in reducing fracture risk. Other medications, like denosumab, target a different aspect of bone remodeling, offering an alternative for patients who cannot tolerate bisphosphonates. Selective estrogen receptor modulators (SERMs) provide an option for postmenopausal women, offering some of the bone-protective effects of estrogen without the associated risks of hormone replacement therapy. Finally, monoclonal antibodies like denosumab and teriparatide, a parathyroid hormone analog, can also be used, often for patients with severe osteoporosis or high fracture risk.
Comparison of Osteoporosis Medications
| Medication Class | Mechanism of Action | Efficacy | Common Side Effects |
|---|---|---|---|
| Bisphosphonates (alendronate, risedronate) | Inhibit bone resorption | High; significantly reduces fracture risk | Esophageal irritation, gastrointestinal upset |
| Denosumab | Inhibits RANKL, reducing bone resorption | High; comparable to bisphosphonates | Increased risk of infection |
| SERMs (raloxifene) | Mimic some effects of estrogen on bone | Moderate; reduces vertebral fractures | Hot flashes, leg cramps, increased risk of blood clots |
| Teriparatide | Stimulates bone formation | High; increases bone density | Hypercalcemia (high blood calcium) |
Tailoring Treatment to Individual Needs
Treatment decisions are not one-size-fits-all. A 70-year-old woman with a history of vertebral fractures will likely require a different treatment approach than a 55-year-old woman with osteopenia and no fracture history. Factors such as age, bone density, fracture risk, other medical conditions, and personal preferences all play a role in determining the most appropriate treatment strategy. For instance, a patient with a history of gastrointestinal problems might be unsuitable for bisphosphonates, necessitating an alternative like denosumab.
Similarly, patients with a high risk of blood clots might not be candidates for SERMs.
Selecting an Appropriate Treatment Plan
The process of selecting a treatment plan begins with a thorough evaluation by a doctor, typically an endocrinologist or rheumatologist. This involves a comprehensive medical history, bone density testing (DEXA scan), and assessment of fracture risk. The doctor will discuss the various treatment options, weighing the benefits and risks of each in the context of the patient’s individual circumstances.
Shared decision-making is key, ensuring the patient understands their options and feels comfortable with the chosen approach. Regular monitoring of bone density and overall health is crucial to ensure the effectiveness of the treatment and to make adjustments as needed. This collaborative approach ensures that the treatment plan is tailored to the specific needs and preferences of the individual, maximizing the benefits while minimizing potential side effects.
Outcome Summary
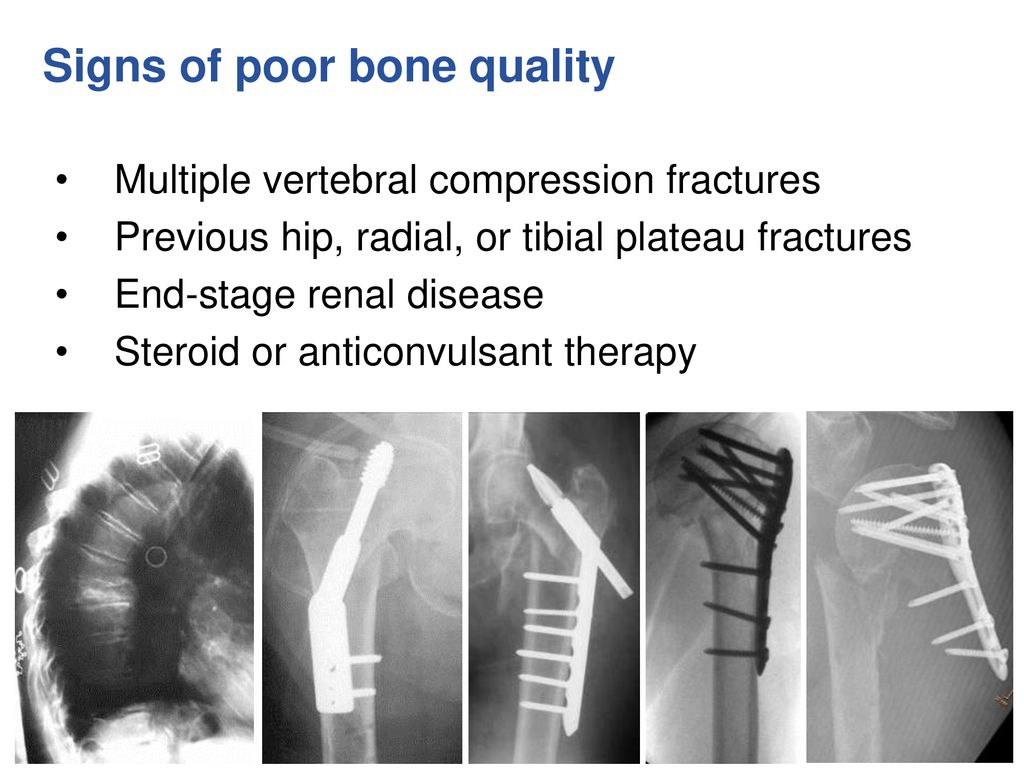
Source: slideplayer.com
Taking care of your bone health is a marathon, not a sprint. While there’s no magic bullet, proactively addressing risk factors and making conscious lifestyle choices can significantly reduce your chances of developing osteopenia or osteoporosis. Remember, early detection is key. Don’t hesitate to schedule a bone density scan if you have concerns, and always consult with your doctor before making any significant dietary or exercise changes.
By understanding the early warning signs and taking proactive steps, you can empower yourself to maintain strong, healthy bones throughout your life. Let’s work together to build a stronger, healthier future, one bone at a time!
FAQ Guide
What are some subtle signs of osteopenia that might be easily overlooked?
Subtle signs can include unexplained aches and pains, particularly in the back, a slight decrease in height over time, and a gradual loss of posture. These can be easily dismissed as part of aging, so it’s important to pay attention to any persistent or unusual changes.
Is there a specific age when I should start worrying about osteopenia?
While risk increases with age, it’s not about a specific age. Family history, lifestyle choices, and certain medical conditions play a huge role. Talk to your doctor about your individual risk factors and when they recommend a bone density scan.
Can I reverse osteopenia?
While you can’t completely reverse bone loss, you can often slow or even stop its progression through lifestyle changes, diet, and in some cases, medication. The earlier you intervene, the better the outcome.
What if I’m already diagnosed with osteopenia? What’s next?
Your doctor will likely recommend lifestyle changes, including diet and exercise, and may prescribe medication to help slow bone loss. Regular follow-up appointments are crucial to monitor progress.
