Home Remedies for Dark Lips Due to Hyperpigmentation
Home remedies for dark lips due to hyperpigmentation offer a natural approach to addressing this common concern. Many factors contribute to dark lips, from sun exposure and dehydration to genetics and certain medical conditions. This post explores effective, at-home solutions, empowering you to regain your confidence with naturally rosy lips. We’ll delve into the science behind these remedies, discuss potential side effects, and create a simple, manageable routine you can incorporate into your daily life.
We’ll cover various natural ingredients and techniques, including gentle exfoliation and deep hydration methods, to help you understand how to address hyperpigmentation safely and effectively. Remember, while these remedies can be beneficial, it’s always best to consult a dermatologist if your condition persists or worsens.
Understanding Hyperpigmentation of the Lips
Darkened lips, often a cosmetic concern, can stem from a condition called lip hyperpigmentation. This involves an increase in melanin production in the lip tissue, leading to a darker than usual lip color. Understanding the causes and characteristics of this condition is crucial for effective treatment.
Causes of Lip Hyperpigmentation
Several factors contribute to the development of hyperpigmented lips. Genetic predisposition plays a significant role; some individuals are simply more prone to increased melanin production in their lips than others. Sun exposure is another major culprit. The delicate skin of the lips lacks the same protective melanin density as other areas of the skin, making them highly susceptible to UV damage, leading to increased melanin production and darkening.
Certain medications, particularly those containing photosensitizing agents, can also exacerbate lip hyperpigmentation when combined with sun exposure. Hormonal changes, such as those experienced during pregnancy or menopause, can influence melanin production and lead to darkening of the lips. Finally, irritation and inflammation from lip products, such as harsh chemicals or fragrances, can trigger an increase in melanin production.
Types of Lip Hyperpigmentation
While the underlying mechanism is similar – increased melanin production – lip hyperpigmentation can manifest in different ways. Post-inflammatory hyperpigmentation is a common type, resulting from lip injuries, such as burns, cold sores, or trauma. This type of hyperpigmentation usually fades over time. Melasma, a condition often associated with hormonal changes, can also affect the lips, presenting as brown patches.
Finally, some cases of lip hyperpigmentation may be linked to underlying medical conditions, though this is less common. Accurate diagnosis is crucial to determine the underlying cause and tailor treatment accordingly.
Visual Characteristics of Hyperpigmented Lips
Hyperpigmented lips typically present as a darkening of the lip color, ranging from a slightly deeper shade to a significantly darker brown or even black. The darkening can be uniform across the lips or appear in patches. The texture of the lips may remain unchanged, although in some cases, dryness or roughness might accompany the discoloration. The degree of darkening can vary depending on the underlying cause and individual factors.
For example, post-inflammatory hyperpigmentation might appear as a localized dark spot, while melasma might manifest as more diffuse patches.
Lip Hyperpigmentation Compared to Other Lip Conditions
It’s important to distinguish lip hyperpigmentation from other lip conditions. While lip hyperpigmentation primarily involves discoloration, other conditions like cheilitis (lip inflammation) may also involve changes in lip color, but are typically accompanied by other symptoms such as swelling, dryness, cracking, or bleeding. Similarly, lip lesions, such as cold sores or canker sores, might cause temporary discoloration, but their visual characteristics and associated symptoms are distinctly different.
A proper diagnosis from a dermatologist or healthcare professional is crucial to differentiate between these conditions and ensure appropriate treatment.
Natural Remedies for Dark Lips
Dark lips, often caused by hyperpigmentation, can be a concern for many. While medical treatments exist, several natural remedies offer potential solutions, working to lighten the lip color and improve overall appearance. It’s crucial to remember that results vary depending on individual factors and the underlying cause of the hyperpigmentation. Consistency and patience are key when using these methods.
Home Remedies for Lip Hyperpigmentation
Several natural ingredients possess properties that may help lighten dark lips. The following table Artikels five common remedies, their application, and potential benefits and limitations. Always perform a patch test before applying any new substance to your lips to check for allergic reactions.
| Remedy | Ingredients | Application | Expected Results |
|---|---|---|---|
| Lemon Juice | Freshly squeezed lemon juice | Apply a small amount of diluted lemon juice to lips using a cotton swab. Leave on for 5-10 minutes, then rinse thoroughly. | May gradually lighten lip color due to its bleaching properties. However, overuse can cause dryness and irritation. |
| Sugar Scrub | Granulated sugar and honey or olive oil | Mix equal parts sugar and honey/olive oil to form a paste. Gently scrub lips in circular motions for 1-2 minutes, then rinse. | Exfoliates dead skin cells, potentially revealing brighter skin underneath. Regular use may improve lip texture and reduce darkness. |
| Aloe Vera Gel | Pure aloe vera gel | Apply a thin layer of aloe vera gel to lips and leave on overnight. Rinse in the morning. | Soothes and hydrates lips, potentially reducing inflammation and improving overall lip health. May contribute to a slight lightening effect over time. |
| Beetroot Juice | Freshly squeezed beetroot juice | Apply diluted beetroot juice to lips and leave on for 15-20 minutes. Rinse thoroughly. | Beetroot contains natural pigments that may help even out lip color, though it may temporarily stain lips. It’s important to dilute the juice properly. |
| Rose Petals Paste | Dried rose petals, milk or rose water | Grind dried rose petals into a fine powder. Mix with milk or rose water to form a paste. Apply to lips and leave on for 15-20 minutes, then rinse. | Rose petals possess mild bleaching properties and can help soothe and hydrate the lips. May contribute to a gradual lightening effect. |
Benefits and Limitations of Natural Remedies
While natural remedies offer a gentler approach to lightening dark lips, it’s crucial to understand their limitations. Some remedies, like lemon juice, can cause dryness and irritation if overused. Others, such as beetroot juice, may temporarily stain lips. The effectiveness of these remedies also varies significantly depending on the individual and the underlying cause of the hyperpigmentation.
For significant hyperpigmentation, professional medical advice is recommended.
Scientific Basis of Effectiveness
The effectiveness of these natural remedies is often based on anecdotal evidence and traditional practices. Lemon juice’s bleaching effect is attributed to its citric acid content, which can lighten skin pigmentation. Sugar scrubs help exfoliate dead skin cells, revealing brighter skin underneath. Aloe vera’s soothing and hydrating properties can improve overall lip health. The effectiveness of beetroot and rose petals is less scientifically established, but their use is rooted in traditional practices for skin lightening and soothing.
Step-by-Step Guide: Using a Sugar Scrub
This guide details the application of a sugar scrub for lip exfoliation. Remember to always perform a patch test before full application.
- Gather Ingredients: Mix equal parts granulated sugar and honey (or olive oil).
- Prepare the Scrub: Create a paste-like consistency. The paste should be thick enough to stay on the lips but not so thick it’s difficult to apply.
- Apply the Scrub: Gently apply the sugar scrub to your lips using your fingertip. Use circular motions to exfoliate.
- Massage Gently: Massage your lips for 1-2 minutes. Avoid harsh scrubbing, as this can irritate your lips.
- Rinse Thoroughly: Rinse your lips with lukewarm water to remove the scrub completely.
- Moisturize: Apply a lip balm or moisturizer to hydrate your lips after exfoliating.
Precautions and Potential Side Effects, Home remedies for dark lips due to hyperpigmentation
While generally safe, using sugar scrubs can lead to irritation if used too frequently or aggressively. Avoid using this remedy if you have cuts or sores on your lips. Excessive exfoliation can lead to dryness and chapped lips. If you experience any irritation or adverse reactions, discontinue use immediately.
Lifestyle Factors and Lip Health
Source: healthcareplaning.org
Darker lips aren’t always a sign of a serious problem, but several lifestyle choices can contribute to hyperpigmentation and negatively impact overall lip health. Understanding these factors is crucial for developing an effective approach to improving lip color and maintaining healthy lips. This section explores the connection between lifestyle and lip pigmentation, emphasizing preventative measures and healthy habits.
Numerous lifestyle factors can influence lip pigmentation. Sun exposure, smoking, and certain dietary deficiencies all play a role in the development or worsening of dark lips. Addressing these factors is key to achieving a healthier lip color and overall well-being.
Sun Protection for Lip Health
Sun exposure is a significant contributor to lip hyperpigmentation. The delicate skin on our lips lacks the same protective melanin as the skin on the rest of our face, making them highly susceptible to sun damage. Prolonged exposure to ultraviolet (UV) radiation from the sun can lead to increased melanin production, resulting in darkening of the lips. This damage can also contribute to dryness, chapping, and even an increased risk of lip cancer.
So, I’ve been researching home remedies for dark lips caused by hyperpigmentation, trying out things like lemon juice and honey. It’s amazing how much you can learn about the body’s intricacies! It got me thinking about other health markers, like how fascinating it is that, according to this article, can eye test detect dementia risk in older adults.
Back to my lips though – I’m hoping to see some improvement soon with these natural remedies!
Therefore, protecting lips from the sun is paramount for maintaining their health and color.
Recommendations for a Healthy Lip Care Routine
A consistent lip care routine is essential for maintaining healthy, naturally colored lips. This routine should incorporate several key elements:
A daily lip care routine should include gentle exfoliation to remove dead skin cells, hydration with a lip balm containing SPF, and avoidance of harsh chemicals or irritants. This holistic approach promotes healthy lip tissue and minimizes hyperpigmentation.
- Gentle Exfoliation: Once or twice a week, gently exfoliate your lips using a soft-bristled toothbrush or a sugar scrub. This removes dead skin cells, revealing smoother, healthier lip tissue. Be sure to be gentle, avoiding harsh scrubbing.
- Hydration: Keep your lips moisturized throughout the day using a lip balm containing SPF 15 or higher. This protects your lips from sun damage and prevents dryness, which can exacerbate hyperpigmentation.
- Avoid Irritants: Limit exposure to harsh chemicals and irritants found in certain lipsticks, lip glosses, and other lip products. Choose products with natural ingredients and avoid those known to cause allergic reactions or irritation.
The Role of Diet and Hydration in Maintaining Healthy Lip Color
Diet and hydration play a vital role in overall health, including lip health. A balanced diet rich in antioxidants and vitamins can contribute to healthy lip color. Adequate hydration is crucial for maintaining the plumpness and suppleness of the lips. Dehydration can lead to dryness and cracking, making lips appear dull and darker.
A diet rich in fruits and vegetables, particularly those high in antioxidants like vitamins C and E, can help protect against oxidative stress and promote healthy skin cell turnover. Staying well-hydrated by drinking plenty of water helps maintain the natural plumpness and hydration of the lips, preventing dryness and chapping which can worsen the appearance of dark lips.
Maintaining adequate hydration is key. Aim for at least 8 glasses of water per day.
Using Exfoliation and Hydration for Lip Pigmentation: Home Remedies For Dark Lips Due To Hyperpigmentation
Dark lips due to hyperpigmentation can often benefit from a consistent routine incorporating both exfoliation and hydration. Exfoliation helps remove dead skin cells that can contribute to a dull and uneven lip tone, revealing brighter, healthier skin underneath. Simultaneously, hydration keeps lips plump and moisturized, promoting a smoother, more even texture and potentially reducing the appearance of pigmentation. This combination is key to achieving a more even lip color naturally.
Exfoliation Methods for Lips
Regular exfoliation is crucial for removing dead skin cells, allowing for better absorption of hydrating products and revealing brighter skin. However, it’s important to be gentle, as the lip skin is delicate. Over-exfoliation can lead to irritation and dryness.
- Sugar Scrub: Mix a small amount of granulated sugar (preferably fine-grained) with a touch of honey or olive oil to create a gentle paste. Gently massage this onto your lips in circular motions for about a minute, then rinse thoroughly. The sugar acts as a mild abrasive, while the honey or olive oil provides moisturizing benefits.
- Honey and Baking Soda Scrub: Combine a teaspoon of baking soda with enough honey to form a paste. Baking soda is slightly more abrasive than sugar, so use this method sparingly and only if your lips aren’t sensitive. Apply gently and rinse thoroughly.
- Lip Balm Exfoliation: Many lip balms contain gentle exfoliating ingredients like tiny sugar crystals. These are less abrasive than homemade scrubs and are generally safe for daily use. Simply apply and gently massage the balm into your lips.
- Soft-Bristled Toothbrush: Gently brushing your lips with a soft-bristled toothbrush after cleansing can help remove dead skin cells. Be extremely gentle to avoid irritation. This method is best used sparingly and only if your lips are not already dry or chapped.
Hydration’s Role in Lip Color Improvement
Hydrated lips appear fuller, smoother, and more even in color. When lips are dehydrated, they become dry, cracked, and more prone to pigmentation. Adequate hydration plumps the lips, reducing the appearance of uneven texture and dark spots. This improved texture allows for a more even distribution of lip color, resulting in a more natural and vibrant appearance.
Natural Hydrating Agents for Lips
Several natural ingredients effectively hydrate and nourish the lips.
- Shea Butter: Rich in vitamins and fatty acids, shea butter deeply moisturizes and protects lips from environmental damage.
- Coconut Oil: A natural emollient, coconut oil softens and hydrates, creating a protective barrier against dryness.
- Aloe Vera: Known for its soothing and healing properties, aloe vera gel can help soothe irritated or chapped lips while providing hydration.
- Honey: A natural humectant, honey attracts and retains moisture, keeping lips soft and supple.
Sample Weekly Lip Care Routine
This routine balances gentle exfoliation with consistent hydration.
- Monday: Exfoliate gently using a sugar scrub. Apply a thick layer of shea butter or coconut oil before bed.
- Tuesday-Friday: Apply a hydrating lip balm throughout the day, reapplying as needed.
- Saturday: Gently exfoliate using a soft-bristled toothbrush. Apply a hydrating lip mask (e.g., a thick layer of honey or aloe vera gel) for 15-20 minutes, then remove.
- Sunday: Apply a generous layer of coconut oil or your preferred hydrating lip balm before bed.
Important Considerations and Precautions

Source: ytimg.com
While natural remedies can be beneficial for addressing lip hyperpigmentation, it’s crucial to approach them with caution and awareness. Not all remedies are suitable for everyone, and some may even cause adverse reactions. Understanding potential risks and when to seek professional help is essential for safe and effective treatment.Potential allergic reactions to home remedies are a significant concern. Many natural ingredients, even those commonly considered safe, can trigger allergic contact dermatitis in sensitive individuals.
This can manifest as redness, itching, swelling, or even blistering around the lips. A patch test on a small area of skin before applying any new remedy to the lips is strongly recommended. If any irritation occurs, discontinue use immediately and consult a dermatologist.
Allergic Reactions and Patch Testing
Before applying any new home remedy, perform a patch test. Apply a small amount of the remedy to an inconspicuous area of skin, such as the inner arm, and wait 24-48 hours to observe for any reaction. If redness, itching, or swelling occurs, avoid using the remedy on your lips. Common allergens found in lip treatments include essential oils (like peppermint or cinnamon), certain fruits (like berries), and honey.
Always opt for products with minimal ingredients, and carefully review the ingredient list before use.
When Professional Medical Advice is Necessary
While home remedies can be helpful for mild lip hyperpigmentation, certain situations necessitate professional medical attention. If your lip discoloration is severe, accompanied by pain, significant swelling, or bleeding, consult a dermatologist or other qualified healthcare professional immediately. Persistent hyperpigmentation despite trying home remedies for several weeks also warrants a visit to a dermatologist. They can properly diagnose the underlying cause of the hyperpigmentation and recommend appropriate treatment, which might include prescription creams, chemical peels, or laser therapy.
Additionally, if you suspect your lip discoloration might be related to an underlying medical condition, seeking professional medical advice is crucial.
Preventing Lip Hyperpigmentation
Preventing lip hyperpigmentation involves a multi-pronged approach focused on protection and hydration. Consistent use of a broad-spectrum SPF 30 or higher lip balm with UVA and UVB protection is paramount. This shields the lips from harmful sun rays, a major contributor to hyperpigmentation. Avoid excessive sun exposure, especially during peak hours. Staying hydrated by drinking plenty of water helps maintain the overall health of your lips and prevents dryness, which can exacerbate hyperpigmentation.
A balanced diet rich in antioxidants can also contribute to healthy lip tissue.
Correct Application of Lip Balms and Treatments
Proper application of lip balms and treatments is crucial for maximizing their effectiveness. Start with clean, dry lips. Gently exfoliate your lips beforehand to remove dead skin cells, allowing better penetration of the treatment. Apply a thin, even layer of lip balm or treatment, avoiding excessive rubbing or pressure. Reapply lip balm frequently, especially after eating, drinking, or exposure to sun or wind.
For targeted treatments like lip serums or oils, apply only the recommended amount. Be patient and consistent with your application; results typically take time to become noticeable.
Visual Aids
Source: ytimg.com
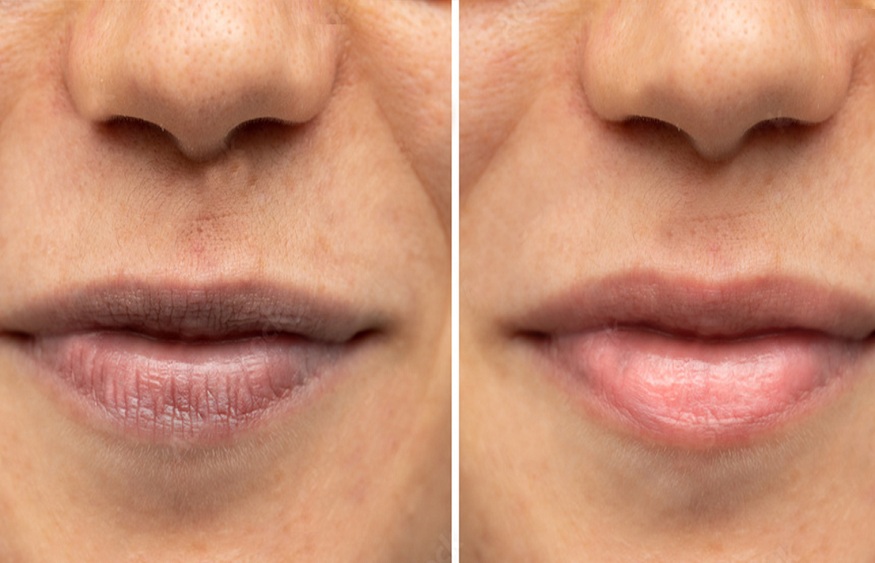
Seeing is believing, and when it comes to addressing dark lips, visual aids can be incredibly helpful in understanding the transformation. Before-and-after illustrations, while not directly shown here, can vividly depict the changes that occur with consistent application of home remedies for lip hyperpigmentation. These visuals offer a powerful way to track progress and stay motivated throughout the treatment process.Before treatment, lips affected by hyperpigmentation may appear noticeably darker than the surrounding skin.
The color can range from a deep brown to a grayish-black hue, depending on the severity of the condition. The texture might feel rough or uneven, possibly with a slightly dry or flaky appearance. Overall, the lips might look dull and lack the natural rosy vibrancy associated with healthy lips. The darkness might be uniform across the lip surface or concentrated in patches.
Expected Appearance After Treatment
After consistent use of home remedies, a gradual lightening of the lip color is typically observed. The intensity of the color change varies depending on the individual, the severity of the hyperpigmentation, and the effectiveness of the chosen remedies. The texture of the lips also improves, becoming smoother and more supple. The lips will appear more hydrated and plump, and the overall appearance will be brighter and more even-toned.
For example, someone with dark brown lips might notice a noticeable lightening to a light brown or even a natural pink shade over several weeks or months of consistent treatment. It is important to note that complete reversal of hyperpigmentation may not always be achievable, but significant improvement is often possible.
Timeline for Visible Results
The timeline for seeing visible results from home remedies varies considerably. Factors such as the severity of hyperpigmentation, the individual’s skin type, the consistency of treatment, and the specific remedies used all play a role. Some individuals may start to see a noticeable difference within a few weeks, while others might require several months of consistent use to achieve significant improvement.
Patience and consistency are key. For instance, a person using a gentle lip scrub and a hydrating lip balm might see subtle improvements in lip texture and color within two to four weeks, while a more significant lightening of pigmentation might take several months. It’s crucial to manage expectations and understand that results are gradual and not instantaneous.
Regular application and a commitment to the chosen home remedies are crucial for achieving the desired outcome.
Final Thoughts
Taking control of your lip health is within reach! By understanding the causes of lip hyperpigmentation and implementing a consistent routine of gentle exfoliation, deep hydration, and sun protection, you can significantly improve the appearance of your lips. Remember that patience is key, and consistent effort will yield the best results. While home remedies can be incredibly effective, don’t hesitate to seek professional advice if you have concerns or experience any adverse reactions.
Embrace your natural beauty and enjoy the journey to healthier, brighter lips!
FAQ Resource
How long does it take to see results from home remedies for dark lips?
Results vary depending on the individual and the severity of hyperpigmentation. You might see subtle improvements within a few weeks, but significant changes usually take several months of consistent treatment.
Can I use these remedies if I have sensitive lips?
Always perform a patch test on a small area of skin before applying any new remedy to your lips. If you experience irritation, discontinue use. Choose gentle ingredients and avoid harsh scrubs.
Are there any foods that can worsen lip hyperpigmentation?
While no specific foods directly cause hyperpigmentation, a diet lacking in essential nutrients can negatively impact overall skin health, potentially affecting lip color. Focus on a balanced diet rich in fruits, vegetables, and antioxidants.
What should I do if a home remedy causes a reaction?
Stop using the remedy immediately and wash the area thoroughly. If the reaction is severe (e.g., significant swelling, blistering), seek medical attention.