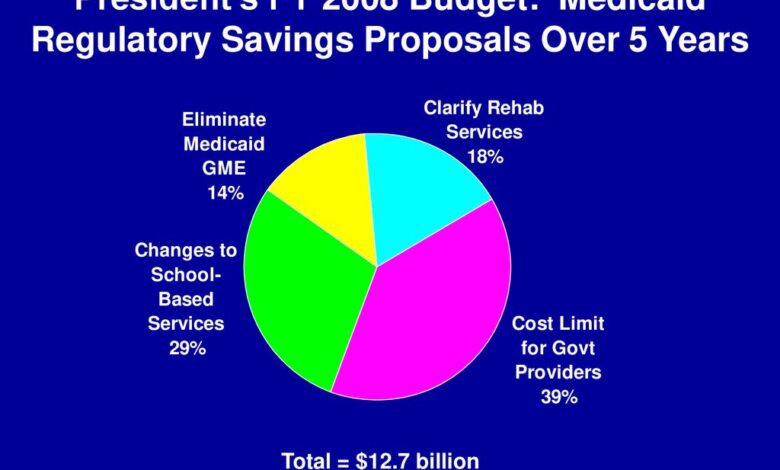
Federal Medicaid Cuts Shift Costs to Expansion States
Federal medicaid cuts shift costs expansion states – Federal Medicaid cuts shift costs to expansion states, dramatically altering the healthcare landscape. This isn’t just about numbers on a budget sheet; it’s about real people facing potential reductions in access to vital care. The shifting of financial burdens from the federal government to individual states creates a ripple effect, impacting everything from state taxes to the quality of healthcare services available to vulnerable populations.
This post dives into the complexities of this situation, exploring the consequences and the responses from states across the nation.
We’ll examine how these cuts directly impact state budgets, forcing difficult choices between essential services. We’ll look at the disproportionate effect on vulnerable groups, the innovative (and sometimes controversial) cost-saving measures states are implementing, and the long-term implications for healthcare access and affordability. Get ready for a deep dive into the intricate world of Medicaid funding and its far-reaching consequences.
Impact of Federal Medicaid Cuts on State Budgets
Federal Medicaid cuts represent a significant challenge to state governments, forcing difficult budgetary choices and potentially impacting the health and well-being of millions. The mechanism by which these cuts affect state budgets is straightforward: the federal government reduces its share of Medicaid funding, leaving states to cover a larger portion of the costs. This increased burden can strain already tight state budgets, leading to a cascade of consequences.
Mechanism of Federal Medicaid Cuts on State Budgets
Medicaid is a joint federal-state program, with the federal government traditionally covering a significant portion (typically 50% or more) of Medicaid expenditures. When federal funding is reduced, states are immediately responsible for a greater percentage of the total cost. This is not a gradual shift; it’s a direct, immediate increase in the state’s financial responsibility for providing healthcare services to its residents.
The impact varies significantly depending on a state’s existing Medicaid program structure, its population size, and the health needs of its citizens.
Comparative Budgetary Impact Across States, Federal medicaid cuts shift costs expansion states
States with larger populations and higher rates of low-income individuals, or those with higher prevalence of chronic diseases requiring expensive treatments, are disproportionately affected by federal Medicaid cuts. For instance, states like California and Texas, with their large populations, will experience substantially larger budget shortfalls than smaller states like Wyoming or Vermont, even if the percentage reduction in federal funding is uniform.
States with robust Medicaid expansion programs under the Affordable Care Act (ACA) are also more vulnerable, as they’ve incorporated more individuals into the system, increasing their overall Medicaid expenditure and, therefore, their exposure to federal cuts. Conversely, states that haven’t expanded Medicaid will experience a smaller absolute increase in their financial responsibility, but the impact on their healthcare system may still be substantial.
Increased State Taxes or Cuts to Other Essential Services
To address the increased financial burden, states are likely to explore several options. One common approach is to raise state taxes, either through broad-based tax increases or targeted taxes on specific goods or services. However, tax increases are often politically unpopular and can negatively impact economic growth. Alternatively, states may be forced to cut funding for other essential services such as education, infrastructure, or public safety.
These cuts can have far-reaching consequences, affecting the quality of life for residents and potentially hindering economic development. The specific choices made by each state will depend on its political landscape, its priorities, and the severity of the budget shortfall.
Projected Budget Shortfalls Due to Anticipated Medicaid Cuts
The following table presents projected budget shortfalls for five states, illustrating the diverse impact of anticipated Medicaid cuts. These figures are illustrative and based on hypothetical scenarios, reflecting the potential range of impacts. Actual figures will vary depending on the specifics of the federal cuts and each state’s response.
| State | Projected Shortfall | Percentage of State Budget | Planned Mitigation Strategies |
|---|---|---|---|
| California | $5 Billion | 2% | Tax increases, service reductions |
| Texas | $3 Billion | 1.5% | Program efficiency improvements, limited service reductions |
| Florida | $2 Billion | 1% | Increased provider reimbursements, budget reallocation |
| New York | $4 Billion | 2.5% | Tax increases, program redesign |
| Illinois | $1.5 Billion | 1% | Increased cost-sharing, service reductions |
Shifting Healthcare Costs to State Governments: Federal Medicaid Cuts Shift Costs Expansion States
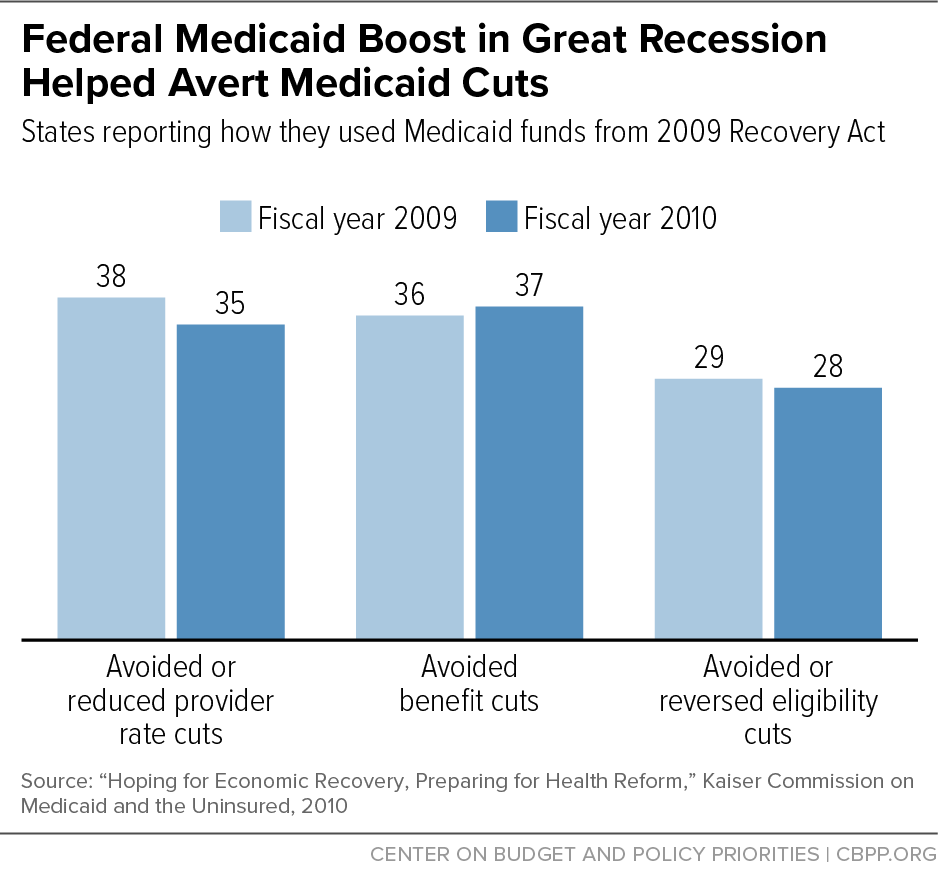
Source: cbpp.org
The looming specter of federal Medicaid cuts casts a long shadow over state budgets, forcing governors and state legislatures to grapple with the daunting task of absorbing a significantly larger portion of healthcare costs. This shift represents a fundamental change in the balance of responsibility for Medicaid, a program designed to provide healthcare for low-income individuals and families. The implications are far-reaching, impacting not only state finances but also the access to and quality of care for millions of Americans.The increased financial burden on states will necessitate difficult choices.
States will need to find creative solutions to manage increased healthcare costs while maintaining the quality of care for their most vulnerable citizens. This will likely involve a combination of cost-cutting measures, program adjustments, and, potentially, increased taxes or other revenue-generating strategies. The potential for a domino effect, impacting other state services and potentially leading to reduced access to healthcare for vulnerable populations, is a serious concern.
Federal Medicaid cuts are forcing expansion states to shoulder a disproportionate burden, impacting their budgets significantly. This financial strain is exacerbated by the recent Supreme Court decision, as detailed in this article about the scotus overturns chevron doctrine healthcare , which could further limit federal regulatory power in healthcare spending. Ultimately, these cuts and legal shifts leave expansion states grappling with immense financial pressures and uncertain futures.
Examples of State Cost-Saving Measures
Several states, anticipating these cuts, have already begun implementing cost-saving measures. For example, some states have focused on improving care coordination and reducing hospital readmissions through initiatives like enhanced care management programs and increased investment in community-based services. Others have implemented stricter eligibility requirements or focused on negotiating lower rates with healthcare providers. Arizona, for instance, has been actively pursuing managed care models to control costs and improve the efficiency of its Medicaid program.
These are proactive steps, but their long-term effectiveness and impact on patient care remain to be seen. The effectiveness of these measures will vary significantly depending on the specific context of each state.
Increased Healthcare Costs for Individuals
Reduced Medicaid coverage due to budget constraints translates directly into increased healthcare costs for many individuals. Those who previously relied on Medicaid for essential services may find themselves facing higher out-of-pocket expenses, leading to delayed or forgone care. This could exacerbate existing health disparities and negatively impact the health outcomes of vulnerable populations. For instance, individuals who delay seeking necessary care due to cost concerns might experience worsening conditions, leading to more expensive treatment in the long run.
The impact could be particularly acute for individuals with chronic conditions who require ongoing medical attention.
Federal Medicaid cuts are forcing expansion states to shoulder a heavier financial burden, impacting their healthcare systems significantly. This financial strain is highlighted by the recent news that Steward Health Care, a large hospital system, secures financing to avoid bankruptcy , a situation that underscores the precarious financial position many healthcare providers find themselves in due to these cuts.
Ultimately, these cuts threaten access to care for vulnerable populations, exacerbating the challenges faced by states already struggling to balance their budgets.
Strategies for Managing Increased Healthcare Costs
States will need to adopt a multifaceted approach to manage the increased healthcare costs resulting from federal Medicaid cuts. The following strategies represent some of the options states might employ:
- Negotiating lower rates with healthcare providers: States can leverage their purchasing power to negotiate lower rates for services from hospitals and other healthcare providers.
- Implementing managed care models: Managed care organizations (MCOs) can play a crucial role in coordinating care, managing costs, and improving the quality of care for Medicaid beneficiaries.
- Expanding telehealth services: Telehealth can provide more efficient and cost-effective access to care, particularly in rural areas.
- Investing in preventive care: Investing in preventive care can help reduce the need for more expensive treatment in the long run.
- Improving care coordination: Reducing hospital readmissions and improving care transitions can significantly lower healthcare costs.
- Targeting specific high-cost populations: Focusing on the needs of high-cost beneficiaries through tailored interventions can lead to cost savings.
- Exploring alternative payment models: Moving away from fee-for-service models towards value-based care can incentivize providers to deliver more efficient and cost-effective care.
Medicaid Expansion and Federal Funding Reductions
The Affordable Care Act (ACA) significantly altered the Medicaid landscape, offering states the option to expand their programs to cover more low-income adults. This expansion, however, came with a complex interplay of federal and state funding, creating vastly different financial realities for states depending on their decision. Federal funding reductions, regardless of expansion status, are now exacerbating these pre-existing disparities and impacting access to care across the board.The financial burdens on states that expanded Medicaid under the ACA versus those that did not are starkly different.
Expansion states initially received a significantly higher level of federal matching funds for newly eligible individuals. This lessened the immediate financial strain on state budgets. However, the current trend of federal funding reductions affects both expansion and non-expansion states, though the impact is felt differently due to the varying baseline levels of federal support. Non-expansion states, already shouldering a larger proportion of Medicaid costs, face a steeper climb in their budgetary responsibilities as federal contributions shrink.
Impact of Federal Cuts on Specific Medicaid Programs
Federal cuts are not uniformly distributed across all Medicaid programs. Areas like long-term care, behavioral health services, and home and community-based services (HCBS) are particularly vulnerable. These programs often serve the most vulnerable populations, including the elderly, individuals with disabilities, and those with serious mental illness. Reductions in funding for these areas directly translate to reduced access to crucial services, potentially leading to increased hospitalizations and higher overall healthcare costs in the long run.
For example, cuts to HCBS could force individuals needing assistance with daily living into more expensive nursing homes, increasing the overall burden on the state Medicaid budget.
Increased Wait Times and Reduced Access to Care
Decreased funding inevitably leads to reduced capacity within the Medicaid system. This translates to longer wait times for appointments with specialists, delays in obtaining necessary medical equipment or treatments, and a potential increase in the number of uninsured or underinsured individuals. For example, a state might reduce the number of contracted providers, forcing patients to travel further for care or face extended wait times for appointments.
This disproportionately affects vulnerable populations who already face barriers to accessing healthcare.
Potential Consequences of Further Federal Medicaid Cuts: A California Scenario
Consider California, a state that expanded Medicaid under the ACA. While California has a robust Medicaid program, further federal cuts could trigger a domino effect. Reduced funding could force the state to implement managed care restrictions, limiting provider choices for enrollees. The state might also be forced to reduce reimbursement rates to providers, potentially leading to provider shortages, especially in rural areas.
Federal Medicaid cuts are forcing expansion states to shoulder a heavier burden, impacting their healthcare budgets significantly. This strain is exacerbated by the ongoing medical coding worker shortage, which is further delaying reimbursements. Fortunately, there are potential solutions on the horizon, like those explored in this article on the ai powered solution to the medical coding worker shortage , which could streamline processes and ultimately alleviate some of the financial pressure on these states.
Ultimately, efficient coding is crucial to navigating these budget constraints.
This could lead to increased wait times for appointments, reduced access to specialty care, and a decline in the quality of care for millions of Californians. The state might also be forced to reduce benefits, such as dental or vision coverage, further impacting the health and well-being of its Medicaid recipients. The increased demand for services coupled with limited resources could strain the state’s healthcare infrastructure, leading to overcrowding in hospitals and emergency rooms.
Such a scenario illustrates the potential for cascading negative consequences, disproportionately affecting vulnerable communities.
Effects on Vulnerable Populations
Medicaid cuts will disproportionately harm vulnerable populations who rely heavily on the program for essential healthcare services. The consequences extend beyond simple financial strain; they represent a direct threat to the health and well-being of millions of Americans. Reduced access to care will lead to worsened health outcomes, increased health disparities, and potentially higher mortality rates among these already marginalized groups.The impact of Medicaid cuts on vulnerable populations is multifaceted and devastating.
Children, the elderly, and people with disabilities often face significant barriers to accessing healthcare even with Medicaid coverage. These barriers are exacerbated when funding is reduced, leading to longer wait times, fewer available providers, and limitations on the types of services covered. This creates a cascading effect, impacting not only their immediate health but also their long-term prospects for education, employment, and overall quality of life.
Increased Uninsured Rates
Reduced Medicaid funding directly translates to a higher number of uninsured individuals. Studies have shown that even small reductions in Medicaid eligibility can lead to a significant increase in the uninsured population, particularly among low-income families and individuals with pre-existing conditions. For example, a hypothetical 10% reduction in Medicaid funding in a state could result in an estimated 50,000 to 100,000 individuals losing coverage, depending on the state’s specific Medicaid structure and the population’s demographics.
These individuals will then be forced to navigate the complexities of the private insurance market, often without the means to afford adequate coverage, leaving them vulnerable to catastrophic medical debt and delayed or forgone care.
Negative Health Consequences
Decreased access to healthcare due to Medicaid cuts leads to a range of negative health consequences for vulnerable populations. Delayed or forgone preventative care can lead to the progression of chronic conditions, resulting in more severe illnesses and higher healthcare costs in the long run. For example, delayed cancer screenings can lead to later-stage diagnoses and reduced survival rates.
Similarly, inadequate access to mental health services can exacerbate existing conditions and lead to increased rates of suicide and self-harm. Children may experience developmental delays due to lack of access to early intervention programs, while the elderly may face increased risk of hospitalization and mortality due to untreated chronic conditions.
Increased Health Disparities
A visual representation of the increased health disparities could be a bar graph. The x-axis would represent specific health outcomes (e.g., infant mortality rate, diabetes prevalence, cancer survival rate). The y-axis would represent the percentage change in these outcomes after Medicaid cuts. Separate bars would depict the changes for different vulnerable populations (children, elderly, people with disabilities). The graph would clearly show that the negative changes are significantly larger for these vulnerable populations compared to the general population, visually demonstrating the widening gap in health outcomes.
For instance, the bar representing infant mortality rate among low-income families might show a 15% increase after the cuts, while the increase for the general population might only be 2%, highlighting the disproportionate impact on vulnerable groups. This visual would clearly demonstrate how Medicaid cuts exacerbate existing health inequalities.
State Responses to Federal Medicaid Cuts
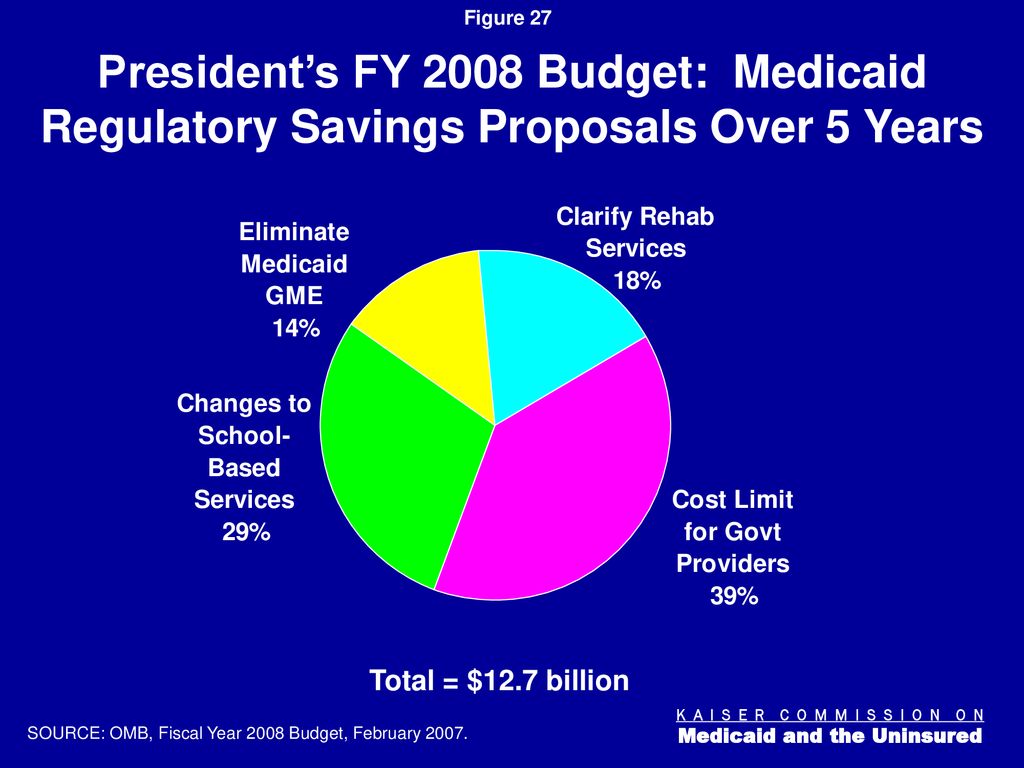
Source: slideplayer.com
The reduction in federal Medicaid funding has forced states to adopt creative and often challenging strategies to maintain essential healthcare services for their residents while navigating constrained budgets. These responses vary widely depending on a state’s pre-existing healthcare infrastructure, political climate, and the severity of the cuts imposed. The common thread, however, is a focus on increasing efficiency and maximizing the value of every healthcare dollar.
Strategies for Mitigating the Impact of Medicaid Cuts
States are employing a multi-pronged approach to mitigate the impact of federal Medicaid cuts. These strategies often involve a combination of cost-containment measures, program redesign, and increased reliance on state funds (where available). Some states are negotiating with healthcare providers to reduce reimbursement rates, while others are focusing on preventative care and disease management programs to reduce long-term healthcare costs.
A key element in many strategies involves leveraging technology to improve efficiency and streamline administrative processes. The ultimate goal is to deliver quality care while minimizing expenditure.
Examples of Successful State-Level Initiatives
Several states have implemented successful initiatives demonstrating the potential for cost savings and improved healthcare outcomes. For instance, some states have invested heavily in telehealth programs, expanding access to care in rural areas and reducing the need for expensive in-person visits. Others have successfully implemented value-based care models, which incentivize providers to focus on improving patient outcomes rather than simply increasing the volume of services provided.
These models often involve risk-sharing arrangements between providers and payers, creating a shared incentive to control costs. States have also shown success in implementing robust care coordination programs, particularly for individuals with chronic conditions, improving the efficiency and effectiveness of healthcare delivery.
Challenges in Implementing Cost-Saving Strategies
Despite the innovative approaches, states face significant challenges in implementing these strategies. Negotiating lower reimbursement rates with healthcare providers can be politically difficult and may lead to provider shortages or reduced access to care in certain areas. Implementing value-based care models requires significant upfront investment in data infrastructure and provider training, as well as the ability to accurately measure and track patient outcomes.
Furthermore, many states lack the resources to fully fund these initiatives, relying on a combination of federal and state funding that is often insufficient. The complexities of Medicaid, including its diverse population and varying needs, also pose significant challenges for effective cost management.
Comparative Analysis of State Responses
| State | Approach | Estimated Cost Savings | Potential Negative Consequences |
|---|---|---|---|
| Oregon | Focus on preventative care, increased use of telehealth, and care coordination for chronic disease management. | Varied estimates, but some reports suggest a potential for significant long-term cost savings. | Potential for increased wait times for certain services if demand outpaces capacity. Challenges in fully integrating telehealth into existing systems. |
| Vermont | Implementation of an all-payer model aimed at reducing administrative costs and improving care coordination across all payers. | Projected cost savings over the long term, but initial implementation costs were significant. | Concerns about potential provider pushback and the complexities of coordinating care across multiple payers. |
| Maryland | Negotiation of global budgets with hospitals, emphasizing value-based care and quality metrics. | Significant cost savings have been reported, but the model is highly dependent on effective monitoring and enforcement. | Risk of reduced access to care if hospitals struggle to meet the targets under the global budget. |
Final Thoughts
The ramifications of federal Medicaid cuts are far-reaching and deeply complex. While states are scrambling to find solutions, the ultimate burden often falls on the most vulnerable members of society. The debate over Medicaid funding highlights the ongoing tension between federal responsibility and state autonomy in providing crucial healthcare services. The long-term consequences remain uncertain, but one thing is clear: the fight for adequate healthcare funding is far from over.
Understanding the issues at play is crucial for advocating for change and ensuring access to healthcare for all.
Popular Questions
What specific services are most affected by Medicaid cuts?
Cuts often impact a range of services, including preventative care, mental health services, long-term care, and prescription drug coverage. The specific services affected vary by state and the nature of the cuts.
How are states attempting to mitigate the impact of these cuts on their residents?
States are employing various strategies, including negotiating lower rates with providers, implementing stricter eligibility requirements, and focusing on preventative care to reduce long-term costs. However, these measures often have unintended consequences.
What are the potential long-term consequences of continued Medicaid cuts?
Continued cuts could lead to a significant increase in the uninsured population, worsening health outcomes, and increasing healthcare disparities. It could also strain state budgets further, forcing cuts to other essential services.
Are there any legal challenges to these federal Medicaid cuts?
Yes, there have been various legal challenges to Medicaid cuts at both the state and federal levels. The outcomes of these challenges can significantly impact the implementation and effects of the cuts.





