Fitch Says 1-2 Year Operating Margins Will Be the Challenge for Some Nonprofit Hospitals
For some nonprofit hospitals fitch says 1 2 operating margins will be the – For some nonprofit hospitals, Fitch says 1-2 year operating margins will be the biggest hurdle they face. It’s a tough reality check for these vital institutions, and understanding the factors at play is crucial. This post dives into Fitch’s assessment, exploring the economic headwinds, operational challenges, and strategic choices impacting these hospitals’ bottom lines. We’ll look at everything from inflation and reimbursement rates to staffing optimization and technological investments – all in the context of providing high-quality care.
Fitch Ratings, a leading credit rating agency, recently released its analysis of nonprofit hospital operating margins. Their projections paint a complex picture, highlighting the interplay between macroeconomic factors, operational efficiency, and healthcare policy. This analysis goes beyond simple numbers; it reveals the vulnerabilities and resilience within the nonprofit hospital sector, and offers valuable insights into the strategies needed to navigate these challenging times.
Fitch Ratings’ Assessment of Nonprofit Hospital Operating Margins: For Some Nonprofit Hospitals Fitch Says 1 2 Operating Margins Will Be The
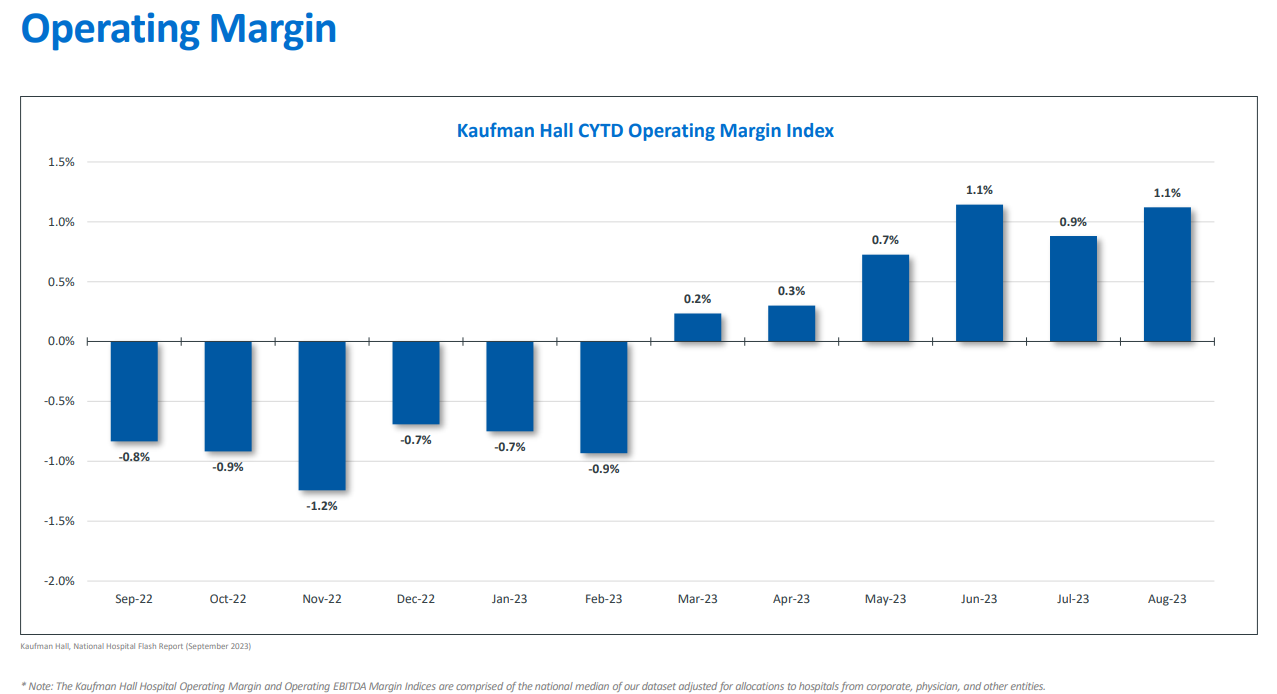
Source: migasolutions.com
Fitch Ratings, a leading credit rating agency, plays a crucial role in evaluating the financial health of nonprofit hospitals. Their assessment of operating margins provides valuable insights into the sector’s performance and future prospects, influencing investment decisions and strategic planning for these institutions. Understanding Fitch’s methodology and the factors they consider is vital for stakeholders across the healthcare landscape.Fitch’s Methodology for Assessing Nonprofit Hospital Operating MarginsFitch employs a comprehensive, multi-faceted approach to assess the operating margins of nonprofit hospitals.
This involves a thorough review of financial statements, operational data, and market conditions. The process is not simply a numerical calculation; it considers the qualitative aspects of a hospital’s performance and its strategic positioning within the competitive healthcare market. The analysis incorporates both historical performance and projected future trends, offering a forward-looking perspective on the hospital’s financial viability.
Factors Considered in Predicting 1-2 Year Operating Margins
Fitch’s prediction of 1-2 year operating margins for nonprofit hospitals considers a range of factors, each weighted according to its perceived influence. These factors are intertwined and often influence one another. For instance, a hospital’s payer mix significantly impacts its revenue cycle, which in turn affects its operating margin.
- Payer Mix and Reimbursement Rates: The proportion of patients covered by Medicare, Medicaid, commercial insurance, and self-pay significantly impacts revenue. Changes in reimbursement rates from government payers or private insurers directly influence profitability. For example, a hospital heavily reliant on Medicare payments might experience margin pressure if Medicare reimbursement rates are reduced.
- Operating Efficiency and Cost Management: Fitch assesses a hospital’s efficiency in managing its expenses, including labor costs, supplies, and administrative overhead. Hospitals with strong cost-control measures are generally better positioned to maintain healthy margins, even in a challenging reimbursement environment. A hospital implementing innovative cost-saving technologies, such as telemedicine, would be viewed favorably.
- Volume and Service Mix: The volume of patients served and the types of services provided (e.g., high-margin specialty services versus low-margin inpatient care) are crucial determinants of revenue. A shift towards higher-volume, lower-margin services could negatively impact operating margins. For example, a hospital seeing a decline in elective procedures due to economic downturn would experience margin pressure.
- Market Position and Competition: Fitch evaluates a hospital’s market share, the intensity of competition, and its ability to attract and retain patients. Hospitals in highly competitive markets may face pressure to reduce prices, potentially impacting their margins. A hospital in a rural area with limited competition may have more pricing power.
- Debt Levels and Capital Structure: High levels of debt can significantly strain a hospital’s finances and reduce its operating margin. Fitch assesses a hospital’s debt burden and its ability to service its debt obligations. A hospital with a high debt-to-equity ratio would be viewed less favorably.
Key Performance Indicators (KPIs) Used in Fitch’s Analysis
Fitch’s analysis relies on a variety of KPIs to gauge the financial health and operational efficiency of nonprofit hospitals. These KPIs are not used in isolation but are considered holistically to develop a comprehensive view.
- Operating Margin: This is a fundamental KPI, representing the percentage of revenue remaining after deducting operating expenses. A consistently strong operating margin is a key indicator of financial health.
- Days Cash on Hand: This metric indicates a hospital’s liquidity and its ability to meet its short-term obligations. A higher number of days suggests greater financial stability.
- Debt Service Coverage Ratio: This KPI measures a hospital’s ability to service its debt obligations. A ratio significantly below 1.0 indicates a potential risk of default.
- Revenue per Adjusted Discharge: This measures the average revenue generated per patient discharge, reflecting the hospital’s pricing power and efficiency in managing patient care costs.
- Patient Days: This indicates the volume of inpatient care provided and can be used to assess trends in patient demand.
Comparison with Other Rating Agencies’ Perspectives
While Fitch Ratings provides a valuable perspective, it’s important to note that other rating agencies, such as Moody’s and S&P Global Ratings, also assess nonprofit hospitals. While their methodologies may differ slightly in terms of specific KPIs or weighting of factors, the overall goal remains the same: to evaluate the creditworthiness and financial stability of these institutions. A comparison of ratings from multiple agencies can offer a more comprehensive understanding of a hospital’s financial standing.
However, it’s important to understand that each agency has its own specific criteria and scoring models.
Impact of Macroeconomic Factors on Nonprofit Hospital Margins
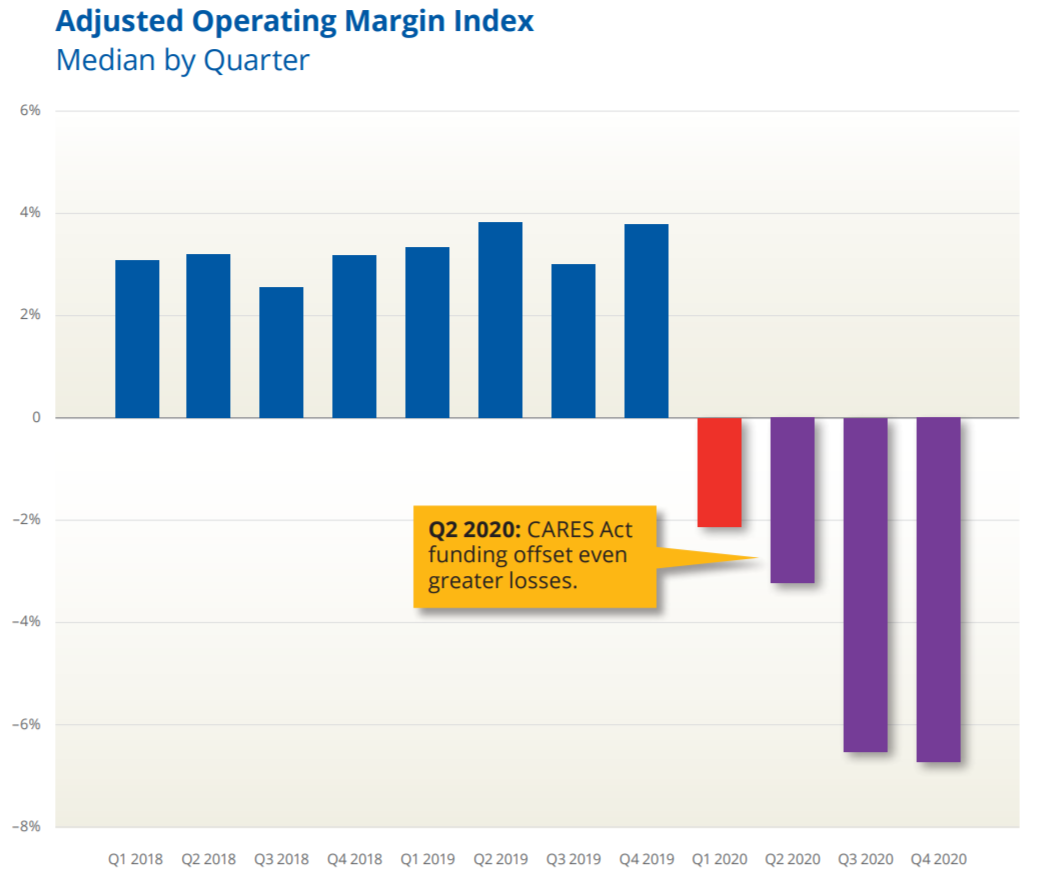
Source: cloudfront.net
Nonprofit hospitals, while dedicated to community health, are not immune to the pressures of the broader economy. Their financial health, reflected in operating margins, is significantly influenced by macroeconomic trends that affect both their costs and revenue streams. Understanding these influences is crucial for predicting future performance and developing effective strategies for financial stability.Inflation’s impact on nonprofit hospital margins is multifaceted.
Rising prices for supplies, medications, and labor directly increase operating costs. Simultaneously, the ability to increase revenue to match these cost increases is often constrained by fixed reimbursement rates from government programs like Medicare and Medicaid, and negotiated rates with private insurers. This squeeze between rising costs and relatively stagnant revenue is a significant threat to profitability.
Inflation’s Influence on Costs and Revenue
Inflation erodes the purchasing power of hospitals’ budgets. For example, a 5% inflation rate on medical supplies necessitates a 5% increase in spending just to maintain the same level of service. Simultaneously, hospitals may struggle to negotiate commensurate increases in reimbursement rates from payers, leading to reduced margins. This effect is amplified when coupled with staff shortages, forcing hospitals to offer higher wages to attract and retain qualified personnel, further straining budgets.
Fitch’s prediction of 1-2% operating margins for some nonprofit hospitals is sobering. It makes me think about the challenges of managing complex situations, much like the difficulties parents face in supporting children with Tourette Syndrome; finding effective strategies is crucial, as highlighted in this helpful article on strategies to manage Tourette syndrome in children. Ultimately, both scenarios require careful planning and resource allocation to navigate difficult financial and healthcare landscapes.
The pressure on nonprofit hospitals to maintain services under these margins is immense.
Conversely, inflation can, in some instances, slightly increase revenue if hospitals are able to successfully adjust their charges for services, although this is often limited by contractual obligations and payer negotiations.
Changes in Healthcare Reimbursement Rates
Changes in healthcare reimbursement rates are a major determinant of hospital profitability. Reductions in reimbursement rates, often implemented by government agencies or private insurers to control healthcare costs, directly decrease hospital revenue. This can be particularly damaging for hospitals heavily reliant on government funding, forcing them to cut costs or accept lower margins. Conversely, increases in reimbursement rates can improve margins, but these increases are often insufficient to offset rising costs, especially during periods of high inflation.
For instance, a decrease in Medicare reimbursement for a specific procedure would directly impact the profitability of hospitals providing that service.
Economic Downturns and Their Impact on Nonprofit Hospital Margins
Economic downturns create a perfect storm of negative impacts on nonprofit hospital margins. During recessions, unemployment rises, leading to a decrease in the number of insured individuals and an increase in patients seeking charity care. Simultaneously, private insurers may tighten their reimbursement policies, further reducing revenue. Additionally, charitable donations, a crucial source of funding for many nonprofit hospitals, often decline during economic hardship.
This combination of reduced revenue and increased demand for uncompensated care severely strains hospital finances.
Examples of Macroeconomic Trends and Their Impact on Operating Margins
The following table illustrates how specific macroeconomic factors influence nonprofit hospital margins:
| Factor | Impact on Costs | Impact on Revenue | Overall Margin Effect |
|---|---|---|---|
| High Inflation | Increased costs for supplies, labor, and utilities | Potential for slight revenue increases through price adjustments, but often limited | Reduced margins due to cost exceeding revenue growth |
| Decreased Medicare Reimbursement Rates | No direct impact | Significant reduction in revenue for Medicare patients | Reduced margins |
| Economic Recession | Increased demand for charity care | Decreased patient volume, reduced private insurance reimbursements, lower charitable donations | Significantly reduced margins, potential for financial losses |
| Staff Shortages (driven by labor market dynamics) | Increased labor costs due to competition for qualified personnel and higher wages | Potentially increased revenue if higher staffing levels lead to improved efficiency and patient volume, but often offset by higher costs | Variable impact, but often leads to reduced margins due to higher labor expenses |
Operational Efficiency and Cost Management in Nonprofit Hospitals
Nonprofit hospitals, while dedicated to providing care, face increasing pressure to maintain financial stability. Efficient operations and robust cost management are crucial for sustaining their mission and ensuring long-term viability, particularly in light of the macroeconomic factors already discussed. Optimizing various aspects of hospital operations can significantly impact operating margins, allowing these vital institutions to continue serving their communities effectively.
Efficient Supply Chain Management and Operating Margins
Effective supply chain management directly influences a hospital’s bottom line. Negotiating favorable contracts with medical suppliers, implementing inventory management systems to minimize waste and storage costs, and utilizing group purchasing organizations (GPOs) to leverage collective buying power are key strategies. For example, a hospital adopting a just-in-time inventory system could drastically reduce storage costs and minimize the risk of expired or obsolete medical supplies.
This translates directly into improved operating margins. Implementing a robust tracking system to monitor usage and predict future needs allows for more accurate ordering, further reducing waste and optimizing spending.
Optimizing Staffing Levels for Improved Profitability
Staffing is a major expense for hospitals. Strategies for optimization involve careful analysis of patient volume, acuity levels, and staffing needs. This includes leveraging data analytics to predict fluctuations in demand and adjust staffing levels accordingly. Implementing flexible staffing models, such as utilizing temporary or per-diem staff during peak periods, can help control labor costs without compromising patient care.
Furthermore, investing in staff training and development can improve efficiency and reduce errors, indirectly leading to cost savings. For instance, a hospital might implement a training program to improve the efficiency of nurses, leading to faster patient turnover and reduced overtime costs.
Methods to Reduce Administrative Expenses
Administrative expenses often represent a significant portion of a hospital’s budget. Reducing these costs requires a multi-pronged approach. This includes streamlining administrative processes, leveraging technology to automate tasks, and negotiating better rates with vendors for services like IT support and printing. Centralizing administrative functions, consolidating departments where possible, and carefully reviewing contracts for unnecessary services can also yield substantial savings.
For instance, switching to electronic health records (EHRs) can reduce paper costs and improve efficiency in billing and patient management.
Best Practices for Revenue Cycle Management to Enhance Margins
Revenue cycle management (RCM) encompasses all processes involved in capturing and collecting payments for services rendered. Optimizing RCM involves improving patient registration and billing processes, minimizing claim denials, and accelerating the payment collection cycle. Implementing automated billing systems, employing skilled billing and coding specialists, and proactively addressing denials can significantly improve cash flow and boost operating margins. A hospital might implement a system that automatically verifies insurance coverage at registration, reducing the number of denied claims due to incomplete information.
Investing in advanced analytics to identify bottlenecks and areas for improvement within the RCM process can also contribute to substantial cost savings.
Financial Strategies for Maintaining Profitability
Nonprofit hospitals face increasing pressure to maintain profitability in a challenging healthcare landscape. Balancing the need to provide high-quality care with the financial realities of operating a hospital requires a multi-pronged approach encompassing strategic funding acquisition, responsible debt management, efficient cost control, and leveraging technology. This section explores key financial strategies to ensure long-term sustainability.
Securing Funding and Grants
Diversifying revenue streams is crucial for nonprofit hospitals. This involves actively pursuing various funding opportunities beyond traditional patient revenue. Strategies include aggressively applying for federal and state grants, focusing on grants targeting specific initiatives like community health programs or telehealth expansion. Building strong relationships with philanthropic organizations and individual donors is also essential. Successful fundraising campaigns often hinge on clearly articulating the hospital’s mission, demonstrating the impact of donations, and providing transparent financial reporting.
For example, a hospital might secure a grant from the Centers for Medicare & Medicaid Services (CMS) to implement a new electronic health record (EHR) system, improving efficiency and patient care. Simultaneously, they could launch a capital campaign focused on building a new cancer center, attracting significant donations from individuals and foundations committed to cancer research and treatment.
Debt Management Strategies
Effective debt management is critical for maintaining financial stability. Strategies include refinancing existing debt at lower interest rates when market conditions are favorable. This can significantly reduce long-term interest payments. Another strategy is to prioritize debt reduction through careful budgeting and increased revenue generation. For example, a hospital might consolidate multiple loans into a single, lower-interest loan, simplifying repayment and reducing overall debt burden.
So, Fitch is predicting razor-thin operating margins for some non-profit hospitals – we’re talking 1-2%! This makes me think about the fragility of the healthcare system, and how even small unexpected events can create huge problems. For example, a stroke, and the often significant long-term care it requires, is drastically impacted by risk factors that make stroke more dangerous , leading to higher hospital costs and further squeezing those already tight margins for hospitals.
This really highlights the precarious financial position of many non-profit hospitals.
Additionally, implementing a proactive approach to debt monitoring and forecasting can help identify potential problems early and allow for timely intervention. A well-structured debt repayment plan, combined with prudent financial planning, ensures the hospital’s long-term financial health and ability to invest in critical infrastructure and services.
Cost-Cutting Measures
Implementing cost-cutting measures without compromising the quality of patient care requires careful planning and strategic decision-making. This could involve streamlining administrative processes, negotiating better rates with suppliers, and optimizing staffing levels through improved scheduling and workforce management. Investing in technology to improve efficiency can also reduce costs in the long run. For example, a hospital might reduce its reliance on expensive disposable supplies by transitioning to reusable alternatives, or implement a centralized inventory management system to reduce waste and optimize supply chain efficiency.
Another example could be negotiating bulk discounts with pharmaceutical companies to lower medication costs. These measures, when implemented strategically, can generate significant cost savings without compromising the quality of care provided.
Investment in Technology
Technology plays a vital role in improving operational efficiency and reducing costs in nonprofit hospitals. Investing in advanced electronic health record (EHR) systems can streamline administrative tasks, reduce medical errors, and improve patient outcomes. Telehealth technologies can expand access to care, particularly in underserved communities, while reducing the need for expensive in-person visits. Implementing data analytics tools can help hospitals identify areas for improvement in operational efficiency, resource allocation, and cost management.
For example, a hospital investing in a robust EHR system can automate billing processes, reducing administrative overhead and improving revenue cycle management. The use of telehealth can also reduce travel costs for both patients and healthcare providers, leading to overall cost savings. Furthermore, predictive analytics can help hospitals anticipate surges in patient volume, enabling them to optimize staffing levels and avoid costly overtime expenses.
Patient Demographics and Healthcare Utilization

Source: qtxasset.com
The aging population and shifting demographics are profoundly impacting nonprofit hospitals, forcing a reassessment of resource allocation and financial strategies. Understanding these demographic trends and their influence on healthcare utilization is crucial for maintaining profitability and ensuring the delivery of quality care. This section will explore the complex interplay between patient demographics, healthcare utilization, and the financial health of nonprofit hospitals.
Impact of an Aging Population on Hospital Resource Allocation and Profitability
The increasing proportion of elderly individuals in the population significantly impacts hospital resource allocation. Older adults generally require more intensive and frequent healthcare services, leading to increased demand for specialized care units, geriatric specialists, and long-term care facilities. This heightened demand can strain hospital resources, potentially increasing operational costs and impacting profitability if not managed effectively. For example, a hospital might need to invest in additional geriatric beds, hire more specialized nurses, and purchase advanced medical equipment to cater to the growing elderly patient population.
This increased investment can impact the hospital’s operating margin unless appropriately offset by increased revenue or cost-cutting measures. Hospitals might explore strategies like telehealth to manage some aspects of elderly care more efficiently, mitigating the impact on resources.
Fitch’s prediction of 1-2% operating margins for some nonprofit hospitals is sobering, especially considering the massive healthcare costs involved. This makes breakthroughs like the recent FDA approval of clinical trials for pig kidney transplants in humans, as reported by this article , even more significant. Such advancements could potentially reduce long-term healthcare expenses, ultimately impacting the financial stability of hospitals in the future.
Relationship Between Changes in Patient Demographics and Hospital Operating Margins
Changes in patient demographics directly influence hospital operating margins. A shift towards an older population, for instance, can lead to higher average costs per patient due to increased complexity of care. Conversely, a younger, healthier population might result in lower overall costs and potentially higher operating margins, assuming demand for services remains consistent. The impact, however, is not solely determined by age.
Factors like the prevalence of chronic diseases within specific demographic groups also play a significant role. A population with high rates of chronic conditions like diabetes or heart disease will necessitate more extensive and costly treatment, negatively impacting margins. Conversely, a population with lower rates of chronic disease will likely result in lower costs and improved margins.
Trends in Healthcare Utilization and Their Effect on Hospital Financial Performance
Trends in healthcare utilization are dynamic and significantly affect hospital financial performance. The increasing prevalence of chronic diseases, coupled with advances in medical technology, leads to higher healthcare utilization rates. This means more patients seeking treatment, longer hospital stays, and increased demand for specialized procedures. While this increased utilization can lead to higher revenue, it also significantly increases operational costs, potentially squeezing operating margins if not managed efficiently.
For example, the rising prevalence of obesity and its associated complications is placing considerable strain on hospital resources, requiring more extensive care and impacting the bottom line. Conversely, preventive care initiatives and public health programs aimed at reducing chronic disease prevalence can positively influence hospital financial performance by reducing the overall burden of disease.
Financial Impact of Treating Different Patient Populations
The financial impact of treating different patient populations varies significantly due to differences in the complexity and cost of care.
The following bullet points Artikel different patient populations and their associated cost implications:
- Elderly Patients (65+): Often require more extensive and prolonged care, leading to higher costs due to increased frequency of hospitalizations, longer stays, and greater need for specialized services. This can include higher medication costs, rehabilitation services, and ongoing monitoring.
- Patients with Chronic Conditions (e.g., diabetes, heart disease, cancer): These patients frequently require ongoing management and treatment, leading to higher overall costs compared to patients with acute conditions. This includes medications, specialist consultations, and potentially extensive procedures.
- Uninsured or Underinsured Patients: These patients often delay seeking care, resulting in more severe health problems requiring more extensive and costly treatments. Hospitals may also experience challenges in collecting payments from these patients, further impacting their financial performance.
- Patients Requiring Specialized Care (e.g., organ transplants, complex surgeries): These patients necessitate highly specialized medical equipment, skilled personnel, and prolonged hospital stays, leading to significantly higher costs.
Regulatory and Policy Impacts on Nonprofit Hospitals
Navigating the complex landscape of healthcare regulation and policy is a significant challenge for nonprofit hospitals. These external forces exert considerable influence on operating costs, reimbursement rates, and ultimately, the financial stability of these vital institutions. Understanding these impacts is crucial for effective strategic planning and ensuring continued service to the community.Government regulations significantly impact hospital operating costs and reimbursement.
Compliance with regulations related to patient safety, staffing ratios, electronic health records (EHR) implementation, and environmental protection necessitates substantial investments in infrastructure, technology, and personnel. These costs, often mandated with limited or no direct reimbursement, can squeeze already tight operating margins. Simultaneously, government reimbursement policies, such as those set by Medicare and Medicaid, influence the revenue hospitals receive for services provided.
Changes in reimbursement rates, often tied to value-based care models or bundled payments, can directly affect a hospital’s profitability. For instance, a reduction in Medicare reimbursement for a specific procedure can lead to a significant decrease in revenue, impacting the hospital’s ability to cover its expenses.
Government Regulations and Hospital Operating Costs
The implementation and maintenance of EHR systems, for example, represent a substantial capital investment and ongoing operational expense for hospitals. While EHRs offer potential benefits in terms of efficiency and care coordination, the initial costs and the need for ongoing training and technical support place a significant burden on hospital budgets. Similarly, regulations concerning patient safety, such as those related to infection control and medication administration, necessitate significant investment in training, equipment, and protocols, all of which impact operating costs.
The compliance burden extends beyond direct financial costs; it also demands significant administrative time and resources, diverting staff from direct patient care.
Impact of Healthcare Policy Changes on Financial Stability
Healthcare policy changes, such as the shift towards value-based care, can dramatically alter the financial landscape for nonprofit hospitals. Value-based care models, which emphasize quality of care and patient outcomes over volume, require hospitals to invest in data analytics, care coordination programs, and population health management initiatives. While these investments can lead to improved patient outcomes in the long run, they represent significant upfront costs that may not be immediately recouped through increased reimbursement.
Furthermore, policy changes related to Medicaid expansion or the Affordable Care Act (ACA) can impact the patient population served by nonprofit hospitals, potentially increasing the proportion of patients with limited or no insurance coverage, thereby affecting revenue streams. For example, a reduction in federal funding for Medicaid could lead to a decrease in reimbursements for hospitals treating a high volume of Medicaid patients.
Regulatory Challenges and Potential Solutions
One significant regulatory challenge is the complexity and ever-changing nature of healthcare regulations. Keeping abreast of these changes and ensuring compliance can be a daunting task, requiring significant investment in legal and compliance expertise. Potential solutions include investing in robust compliance programs, fostering strong relationships with regulatory agencies, and actively participating in industry advocacy efforts to influence policy development.
Another challenge is the potential for regulatory inconsistencies across different jurisdictions, creating complexities for hospitals operating in multiple states. Strategies to address this include developing standardized compliance protocols and engaging in collaborative efforts with other hospitals to share best practices and resources.
Impact of Different Healthcare Payment Models, For some nonprofit hospitals fitch says 1 2 operating margins will be the
Fee-for-service models, where hospitals are reimbursed for each service provided, can incentivize high-volume care, potentially leading to increased costs and reduced efficiency. In contrast, value-based care models, such as bundled payments and accountable care organizations (ACOs), reward hospitals for achieving positive patient outcomes and managing costs effectively. The shift towards value-based care presents both challenges and opportunities for nonprofit hospitals.
While it requires significant investment in infrastructure and care coordination, it also offers the potential for long-term financial sustainability by incentivizing efficiency and quality improvement. For example, a hospital participating in a bundled payment program for hip replacements would be incentivized to reduce complications and readmissions, leading to cost savings and improved patient outcomes.
Outcome Summary
The financial health of nonprofit hospitals is more than just a balance sheet; it’s directly tied to the well-being of our communities. Fitch’s forecast underscores the urgent need for proactive strategies to address the challenges ahead. From embracing innovative cost-cutting measures and optimizing resource allocation to advocating for policy changes that support fair reimbursement, the path to sustainability requires a multi-pronged approach.
By understanding the complexities of the current landscape, nonprofit hospitals can better position themselves to continue providing essential care while maintaining financial stability. The future isn’t just about survival; it’s about thriving, and this requires strategic planning and decisive action.
Answers to Common Questions
What specific KPIs does Fitch use in its analysis?
Fitch likely uses a range of KPIs, including debt-to-equity ratios, operating income margins, days cash on hand, and patient days. The exact mix will vary depending on the specific hospital and its financial profile.
How do these projections compare to other rating agencies?
While Fitch’s projections are valuable, it’s important to compare them to assessments from Moody’s and S&P to get a more holistic view. Different agencies may use slightly different methodologies, leading to varying conclusions.
What role does philanthropy play in mitigating these margin challenges?
Philanthropic donations can significantly buffer the impact of shrinking margins. Successful fundraising strategies are critical for maintaining financial stability and investing in necessary upgrades.