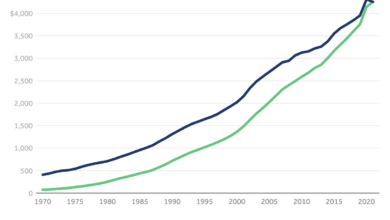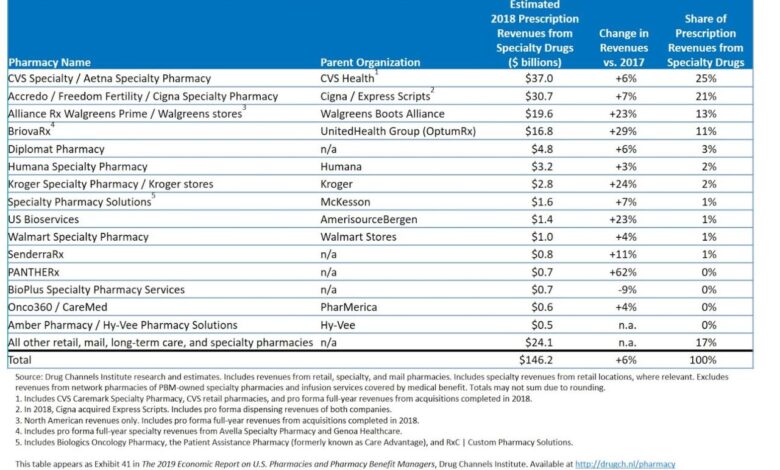
FTC Second PBM Report Caremark, Express Scripts, UnitedHealth
Ftc second pharmacy benefit manager report caremark express scripts unitedhealth – FTC second pharmacy benefit manager report Caremark, Express Scripts, and UnitedHealth – the title alone screams drama, right? This report isn’t just another government document; it’s a deep dive into the murky world of prescription drug pricing and the massive power held by three pharmaceutical giants. We’re talking about allegations of anti-competitive practices, inflated prices, and potentially limited access to essential medications.
Get ready to unravel the complexities and discover how these PBMs impact your healthcare costs.
The Federal Trade Commission’s (FTC) second report on Pharmacy Benefit Managers (PBMs) has sent shockwaves through the healthcare industry. Caremark, Express Scripts, and UnitedHealth, three of the biggest names in the PBM game, are squarely in the crosshairs. The report alleges a range of anti-competitive practices, from manipulating drug rebates to controlling pharmacy networks, ultimately driving up costs for consumers.
This isn’t just about big corporations; it’s about the everyday impact on individuals struggling to afford their prescriptions. We’ll break down the key findings, analyze the implications, and explore potential solutions.
FTC Report Overview
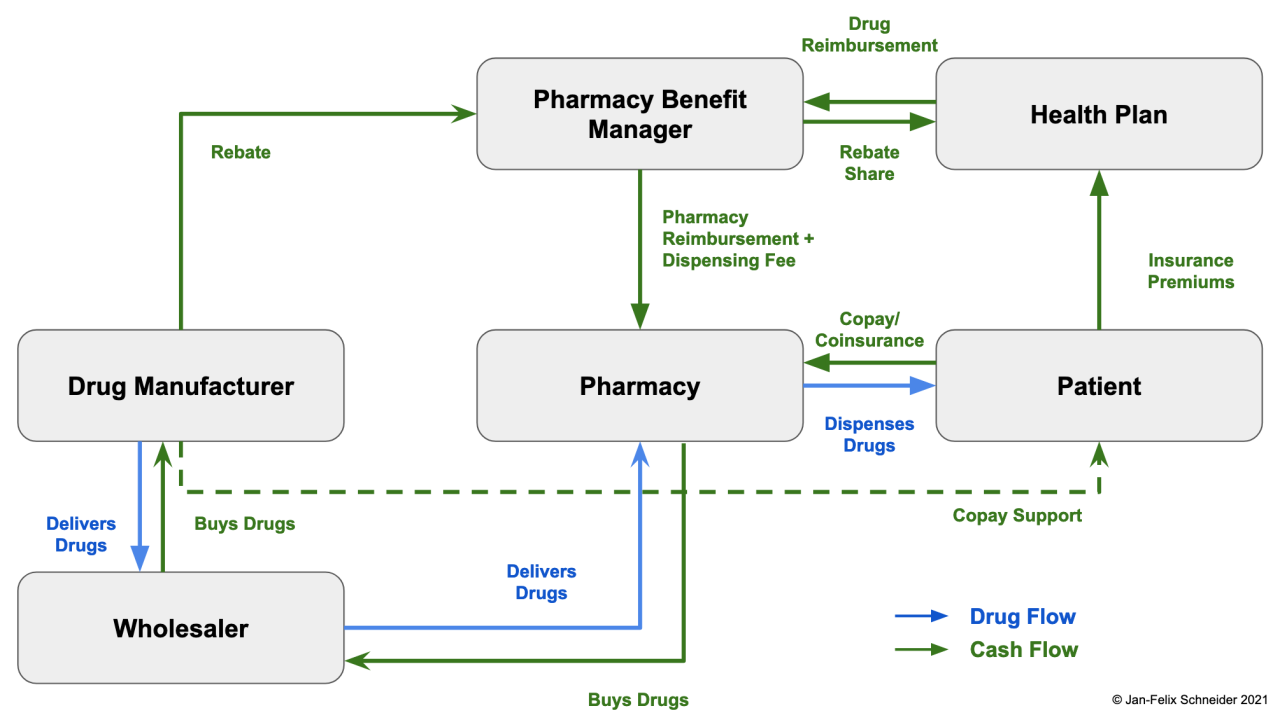
Source: substackcdn.com
The Federal Trade Commission’s (FTC) second report on Pharmacy Benefit Managers (PBMs) delves into the practices of three dominant players: Caremark, Express Scripts, and UnitedHealth. This report builds upon previous investigations, offering a more detailed analysis of their market influence and potential anti-competitive behaviors. The findings paint a picture of a system where these PBMs wield significant power, potentially impacting both healthcare providers and consumers.
The FTC’s second Pharmacy Benefit Manager report on Caremark, Express Scripts, and UnitedHealth is raising serious concerns about drug pricing. This highlights the need for streamlined, efficient healthcare processes, and that’s where technology steps in; check out this article on the ai powered solution to the medical coding worker shortage to see how automation can help.
Ultimately, improving healthcare efficiency, even in areas seemingly unrelated to PBM’s, could help address the larger issues highlighted in the FTC report.
Key Findings of the FTC Report
The FTC’s report highlights several key concerns regarding the operations of Caremark, Express Scripts, and UnitedHealth. These concerns center around the potential for these PBMs to use their market dominance to suppress competition, manipulate drug prices, and ultimately harm consumers. The report suggests that the current regulatory framework may be inadequate to address these concerns, leaving patients vulnerable to higher costs and limited access to medications.
The report meticulously Artikels specific instances where these companies allegedly engaged in practices that stifle competition and inflate prices.
Criticisms of Caremark, Express Scripts, and UnitedHealth
The report levels specific criticisms against each of the three PBMs. Caremark, for instance, faces scrutiny over its alleged use of spread pricing, a practice where the difference between what the PBM pays a pharmacy and what it charges the plan sponsor is kept by the PBM, often exceeding the actual cost of dispensing. Express Scripts has been criticized for its network design, which some argue limits patient access to preferred pharmacies and increases costs.
UnitedHealth, with its integrated model encompassing both insurance and PBM operations, faces concerns regarding potential conflicts of interest and anti-competitive practices related to its own internal drug pricing and network management.
Comparison of PBM Business Practices
While all three PBMs operate in a similar market, their business practices and alleged anti-competitive strategies differ in their specifics. Caremark’s emphasis on spread pricing contrasts with Express Scripts’ focus on network control. UnitedHealth’s vertically integrated structure presents a unique set of challenges regarding potential conflicts of interest not directly mirrored by the other two. The FTC’s report examines these differences, highlighting how each PBM leverages its market position to potentially gain an unfair advantage.
Alleged Anti-Competitive Practices
| PBM Name | Alleged Practice | Impact on Consumers | FTC Recommendation |
|---|---|---|---|
| Caremark | Spread Pricing; Lack of transparency in rebate negotiations | Higher prescription drug costs; Limited pharmacy choices | Increased transparency; Regulatory reforms to limit spread pricing |
| Express Scripts | Restrictive network design; Favoritism towards certain drug manufacturers | Reduced access to pharmacies; Higher drug prices due to limited competition | Greater network neutrality; Enhanced scrutiny of manufacturer relationships |
| UnitedHealth | Potential conflicts of interest due to vertical integration; Anti-competitive practices related to internal pricing | Higher costs for consumers; Reduced choice in health plans | Structural separation of insurance and PBM operations; Stricter oversight of internal pricing |
Impact on Drug Pricing
The FTC’s report on Caremark, Express Scripts, and UnitedHealth’s pharmacy benefit manager (PBM) practices reveals a complex system significantly impacting prescription drug prices for consumers. The report suggests that these PBMs, through their negotiating power and various operational practices, may be contributing to higher, rather than lower, drug costs for patients. This impact extends beyond simple price fluctuations; it involves intricate relationships between manufacturers, PBMs, and insurance companies, ultimately affecting the affordability and accessibility of essential medications.The PBMs’ influence on drug pricing operates through several mechanisms detailed in the FTC report.
For instance, their substantial market share allows them to negotiate deeply discounted prices from drug manufacturers. While this might seem beneficial, the report raises concerns that these discounts aren’t always passed on fully to consumers in the form of lower co-pays or premiums. Instead, the PBMs may retain a significant portion of these discounts as profit, leading to a situation where both the manufacturer and the PBM profit at the expense of the consumer.
Furthermore, practices like spread pricing (the difference between what the PBM reimburses the pharmacy and what it charges the insurer) and rebates tied to market share can also inflate costs.
Specific Drug Price Impacts, Ftc second pharmacy benefit manager report caremark express scripts unitedhealth
The report doesn’t isolate specific drugs and their price changes in a direct, quantifiable way. However, the FTC’s investigation suggests that the practices of these three PBMs likely influence the pricing of a wide range of medications. The lack of transparency in PBM operations makes it difficult to pinpoint precise examples, but it’s reasonable to assume that commonly prescribed drugs across various therapeutic classes, including those for chronic conditions like diabetes, hypertension, and high cholesterol, are affected.
For example, a drug with a high market share might be subject to significant rebate negotiations that don’t translate to lower consumer costs, while a newer drug with less competition might face less pressure on its pricing from the PBMs.
Increased Healthcare Costs
The cumulative effect of PBM practices described in the report can significantly contribute to increased healthcare costs. The lack of transparency regarding rebates and discounts, combined with spread pricing and other strategies, creates a system where the actual cost of a medication is obscured from consumers. This opacity makes it difficult for patients, physicians, and policymakers to assess the true value and cost-effectiveness of different medications and treatment plans.
Consequently, the increased overall cost of prescription drugs contributes to higher insurance premiums, increased out-of-pocket expenses for patients, and ultimately, a heavier burden on the healthcare system as a whole.
Visual Representation of Drug Pricing Flow
Imagine a flowchart. It begins with the Pharmaceutical Manufacturer, who sets a list price for a drug. An arrow points to the Pharmacy Benefit Manager (PBM), representing the negotiation process where the PBM negotiates a discounted price with the manufacturer. A significant portion of this discount remains with the PBM as profit (represented by a branching arrow showing a portion of the money flowing to the PBM’s profit).
Another arrow points from the PBM to the Health Insurance Plan, representing the price the PBM charges the insurer. The insurer then sets premiums based on this price, plus administrative fees and other costs (represented by an arrow showing a flow of money from the insurer to the PBM and an increase in the cost). A final arrow points from the Health Insurance Plan to the Consumer, representing the consumer’s co-pay or out-of-pocket expense.
The visual clearly illustrates how the PBM sits between the manufacturer and the consumer, influencing the final price paid by the consumer despite potentially receiving substantial discounts from the manufacturer.
Market Domination and Competition
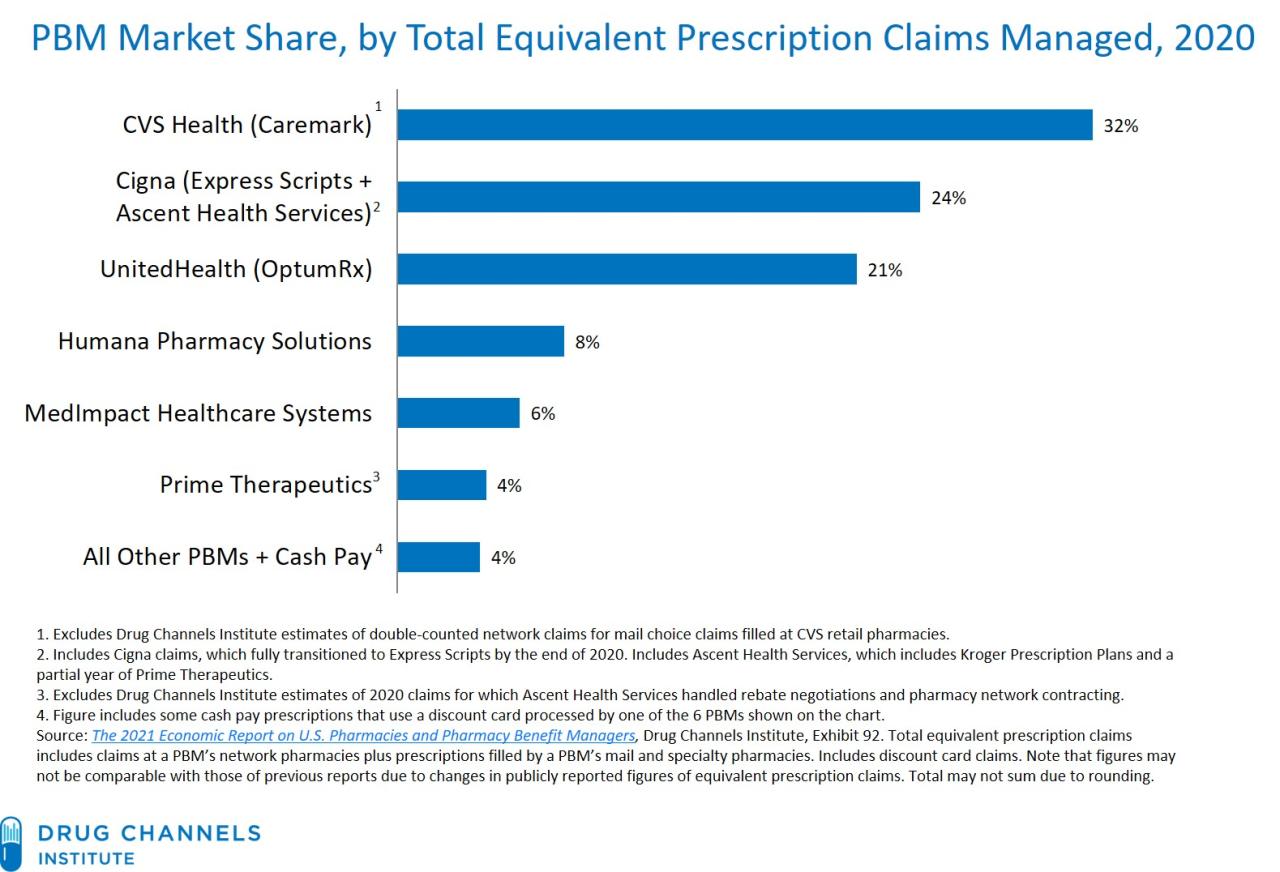
Source: blogspot.com
The pharmaceutical benefit manager (PBM) industry, dominated by Caremark, Express Scripts, and UnitedHealth, presents a compelling case study in market concentration and its impact on drug pricing. The sheer size and influence of these three giants raise significant concerns about competition and its effect on both consumers and pharmaceutical manufacturers. Understanding their market share and the implications of this concentration is crucial to assessing the overall health of the pharmaceutical marketplace.The immense market share held by these three PBMs significantly impacts the competitive landscape.
Their negotiating power with pharmaceutical companies is unparalleled, allowing them to dictate prices and terms in a way that smaller PBMs simply cannot. This imbalance of power can lead to reduced competition and ultimately, higher costs for consumers.
The FTC’s second report on pharmacy benefit managers like Caremark, Express Scripts, and UnitedHealth is raising serious questions about drug pricing. It makes you wonder about the broader healthcare landscape, especially considering Walmart’s recent healthcare setbacks; check out this article on despite Walmart health’s closure, the company healthcare destination, Scott Bowman , for a different perspective. Ultimately, the FTC’s findings on these PBMs and their impact on patient access and affordability are critical to understanding the bigger picture of healthcare costs.
Market Share and Concentration
Precise market share figures fluctuate, and publicly available data often lags. However, it’s widely acknowledged that Caremark, Express Scripts, and UnitedHealth collectively control a substantial majority of the PBM market. Their combined market share is often estimated to be well over 70%, leaving a relatively small portion for numerous smaller competitors. This high concentration limits the choices available to health plans and employers, potentially reducing the incentives for PBMs to compete on price or service quality.
The lack of robust competition allows these large players to maintain higher profit margins, potentially at the expense of lower drug prices for consumers.
Implications of Market Concentration on Competition
The concentrated nature of the PBM market significantly dampens competition within the broader pharmaceutical market. The large PBMs’ considerable leverage allows them to negotiate significantly lower reimbursement rates from pharmaceutical manufacturers. This, in turn, can reduce the profitability of drug development and innovation, potentially slowing down the introduction of new and improved medications. Furthermore, this concentrated power can lead to limited choices for consumers and employers when selecting pharmacy benefits, potentially leading to less favorable terms and conditions.
Comparison of Market Power
The market power wielded by Caremark, Express Scripts, and UnitedHealth dwarfs that of their smaller competitors. Smaller PBMs often lack the scale and negotiating power to secure favorable contracts with pharmaceutical manufacturers or health plans. They may struggle to compete on price, leading to a limited ability to expand their market share. This disparity in market power can create a barrier to entry for new players, further reinforcing the dominance of the “Big Three.” This situation ultimately restricts innovation and potentially limits the development of alternative PBM models that could offer greater value to consumers.
Strategies to Increase Competition in the PBM Sector
Increasing competition in the PBM sector requires a multi-pronged approach. The following strategies could help foster a more competitive and dynamic marketplace:
The need for increased competition is clear. These strategies, while not exhaustive, represent a starting point for addressing the issues of market concentration and its effects on drug pricing and overall market health.
- Strengthening antitrust enforcement: More rigorous scrutiny of mergers and acquisitions within the PBM industry could prevent further consolidation and maintain a more diverse competitive landscape.
- Promoting transparency in PBM pricing and practices: Greater transparency would allow for better comparison-shopping and could encourage greater competition among PBMs.
- Supporting the development of independent PBMs: Government incentives or other support mechanisms could help smaller, independent PBMs gain a foothold in the market and offer alternatives to the large players.
- Empowering consumers and employers with more choices: Providing consumers and employers with more information and options regarding their pharmacy benefits can encourage PBMs to compete more aggressively on price and service.
- Encouraging the development of alternative PBM models: Exploring and supporting innovative models that prioritize patient care and cost-effectiveness over profit maximization could foster a more competitive and consumer-centric market.
Reimbursement Practices and Patient Access
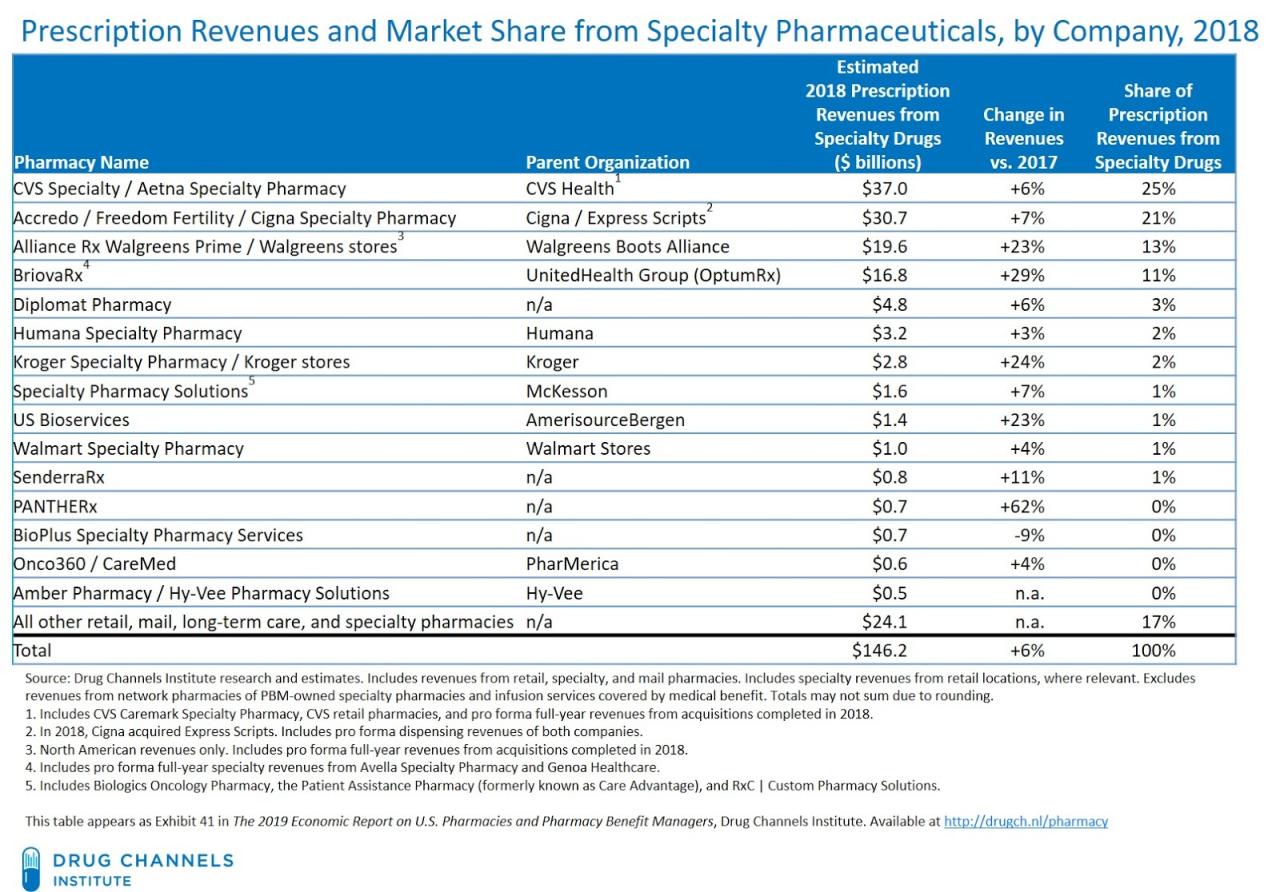
Source: blogspot.com
The way Pharmacy Benefit Managers (PBMs) like Caremark, Express Scripts, and UnitedHealth reimburse pharmacies significantly impacts both the pharmacies themselves and, ultimately, patient access to medications. Understanding these reimbursement methods is crucial to comprehending the complexities of the pharmaceutical supply chain and its effect on healthcare costs and patient care. Different reimbursement models, coupled with other PBM practices, can create a system where patients face barriers to accessing needed prescriptions.
PBMs utilize a variety of reimbursement methods, often involving complex negotiations and contractual agreements with pharmacies. These methods typically fall under a few broad categories: direct and indirect remuneration (DIR) fees, maximum allowable costs (MAC), and various forms of rebates and discounts. The intricacies of these methods, however, often leave pharmacies operating on razor-thin margins, forcing difficult decisions that can impact patient care.
PBM Reimbursement Methods and Their Impact on Pharmacies
The three major PBMs employ variations on these common reimbursement models. For example, DIR fees, which are payments deducted from pharmacies’ reimbursementsafter* the dispensing of a medication, can be unpredictable and significantly reduce a pharmacy’s profit. MAC pricing sets a maximum amount a PBM will reimburse for a drug, regardless of the pharmacy’s acquisition cost. This can force pharmacies to absorb losses when drug costs rise.
Rebates and discounts, while seemingly beneficial, are often negotiated between PBMs and manufacturers, with pharmacies receiving only a portion of the savings, if any. This opaque system creates a lack of transparency and makes it difficult for pharmacies to accurately assess their profitability and plan for the future. The cumulative effect of these practices can be devastating for independent pharmacies, which lack the bargaining power of large chains.
Examples of How Reimbursement Practices Limit Patient Access
These reimbursement practices can directly impact patient access. Imagine a scenario where a small, independent pharmacy faces extremely low reimbursement rates for a particular medication due to MAC pricing. To remain profitable, the pharmacy might be forced to limit the quantity of this medication they stock, potentially resulting in patients experiencing delays or being unable to obtain their necessary prescriptions.
Similarly, unpredictable DIR fees can lead pharmacies to limit their formularies, meaning they might not carry a specific medication, especially if it’s a low-profit item. This can disproportionately affect patients who rely on specific medications or have limited transportation options to access larger chain pharmacies.
Impact on Independent versus Large Chain Pharmacies
Independent pharmacies are particularly vulnerable to these reimbursement practices. Lacking the scale and negotiating power of large chains, they are more likely to absorb losses due to low reimbursement rates and unpredictable DIR fees. This can lead to closures of independent pharmacies, reducing competition and potentially limiting patient choice and access, particularly in underserved areas. Large chain pharmacies, on the other hand, can often negotiate better terms with PBMs due to their volume and market share.
They are also better equipped to absorb losses and remain financially viable despite these challenging reimbursement structures.
PBM Reimbursement Policies and Medication Adherence: A Hypothetical Scenario
Consider a patient with chronic hypertension requiring daily medication. Due to low reimbursement rates, their local independent pharmacy stops carrying the patient’s preferred brand-name medication. The PBM’s formulary only allows for a generic alternative, which the patient finds less effective and less tolerable. This leads to poor medication adherence, potentially resulting in worsening health outcomes, increased healthcare costs associated with managing complications, and reduced quality of life for the patient.
This scenario highlights the indirect, but significant, consequences of PBM reimbursement policies on patient health and the overall healthcare system.
Potential Regulatory Responses
The FTC’s report on Caremark, Express Scripts, and UnitedHealth’s dominance in the pharmacy benefit manager (PBM) market has significant implications. The findings, if substantiated, could lead to a range of regulatory actions aimed at increasing competition and protecting consumers. The effectiveness and consequences of these actions will depend on their scope and enforcement.The potential regulatory responses fall broadly into several categories, each with its own set of advantages and disadvantages, and precedents in other countries’ healthcare systems.
Considering the complexities of the PBM market and its impact on drug pricing and patient access, a nuanced approach is crucial.
The FTC’s second report on pharmacy benefit managers like Caremark, Express Scripts, and UnitedHealth is raising serious questions about drug pricing. It’s interesting to consider this in light of soaring Medicare spending on GLP-1 medications, as highlighted in this insightful KFF report: medicare glp1 spending weight loss kff. The rising costs of these weight-loss drugs, coupled with the PBM’s influence on drug access and pricing, paint a complex picture of healthcare costs that the FTC’s investigation needs to address.
Antitrust Actions
The FTC could pursue antitrust actions, such as filing lawsuits alleging violations of antitrust laws like the Sherman Act or the Clayton Act. These actions could aim to break up the large PBMs, force divestitures of certain assets, or impose structural changes to prevent anti-competitive behavior. Successful antitrust actions could lead to increased competition, potentially lowering drug prices and improving patient access.
However, such lawsuits are lengthy, complex, and uncertain in their outcome. Furthermore, proving anti-competitive intent can be challenging. The European Union, for example, has employed similar antitrust measures against pharmaceutical companies engaging in anti-competitive practices, leading to significant fines and behavioral changes. Conversely, the US has seen mixed results in antitrust cases related to healthcare, highlighting the challenges involved.
Price Controls and Transparency Measures
Regulatory responses could also involve implementing price controls or greater transparency measures. Price controls could directly limit the amount PBMs can charge for their services, potentially reducing overall healthcare costs. However, such controls could stifle innovation and lead to reduced quality of services. Increased transparency, such as requiring PBMs to publicly disclose their rebate and pricing practices, could empower consumers and payers to make more informed decisions.
This approach, while less intrusive than price controls, relies on the market’s ability to respond effectively to greater transparency. Several countries in Europe have implemented various forms of price regulation and transparency measures in their pharmaceutical markets with varying degrees of success, often leading to trade-offs between affordability and access.
Increased Oversight and Regulation
Strengthening regulatory oversight of PBMs could involve creating new agencies or expanding the authority of existing ones to monitor PBM practices more closely. This approach could include stricter enforcement of existing regulations and the introduction of new rules governing rebates, pricing, and other key aspects of PBM operations. Increased oversight can help ensure compliance with existing laws and prevent future anti-competitive behavior.
However, excessive regulation could increase bureaucratic burden and stifle innovation. Canada, for instance, has a more robust regulatory framework for its pharmaceutical industry compared to the US, resulting in greater government oversight and control over drug pricing.
Potential Long-Term Consequences of Different Regulatory Approaches
The long-term consequences of different regulatory approaches are complex and depend on numerous factors. Here’s a summary:
- Antitrust Actions: Increased competition, potentially lower drug prices, but lengthy legal battles and uncertain outcomes.
- Price Controls and Transparency Measures: Lower drug costs, but potential for reduced innovation and quality of services.
- Increased Oversight and Regulation: Improved compliance and prevention of future anti-competitive behavior, but increased bureaucratic burden and potential for stifling innovation.
- No Action: Continued market concentration, potential for higher drug prices, and limited patient access.
Ending Remarks: Ftc Second Pharmacy Benefit Manager Report Caremark Express Scripts Unitedhealth
The FTC’s second PBM report paints a concerning picture of market dominance and questionable practices by Caremark, Express Scripts, and UnitedHealth. While the report details serious allegations, the ultimate impact on consumers and the pharmaceutical landscape remains to be seen. The potential regulatory responses, ranging from stricter oversight to antitrust actions, will significantly shape the future of prescription drug pricing and access.
One thing is certain: this isn’t the end of the story. This report is a catalyst for change, and the ongoing debate promises to be both fascinating and crucial for the future of healthcare.
Answers to Common Questions
What exactly are Pharmacy Benefit Managers (PBMs)?
PBMs are middlemen between drug manufacturers, insurance companies, and pharmacies. They manage prescription drug benefits for insurance plans, negotiating drug prices and creating formularies (lists of covered drugs).
How does this report affect me personally?
The alleged practices highlighted in the report could lead to higher prescription drug costs, limited access to certain medications, and less choice in pharmacies. The outcome of potential regulatory changes will directly impact your out-of-pocket expenses and healthcare experience.
What are some examples of alleged anti-competitive practices?
The report alleges practices such as steering patients to more expensive drugs, manipulating rebates to favor certain manufacturers, and using their market power to suppress competition among pharmacies.
What can I do to help?
Stay informed about the ongoing discussions and regulatory developments. Contact your elected officials to express your concerns and support policies aimed at promoting fair competition and affordable prescription drugs.