Guillain-Barré Syndrome (GBS) Cases, Tracker & Guidelines
Guillain barre syndrome gbs cases tracker and health ministry guidelines – Guillain-Barré Syndrome (GBS): Cases, Tracker & Guidelines – that’s a mouthful, right? But it’s a crucial topic. This post dives into the complexities of tracking Guillain-Barré Syndrome cases, exploring the methods used by health organizations worldwide and examining the vital role of health ministry guidelines in diagnosis and treatment. We’ll uncover the challenges in accurate case reporting, the rationale behind specific treatment protocols, and what’s being done to raise public awareness of this often-misunderstood condition.
Get ready for a deep dive into the world of GBS!
We’ll look at everything from the global picture of GBS cases to the specific recommendations from health ministries around the world. We’ll also explore the ongoing research into GBS, potential new treatments, and the impact this syndrome has on healthcare systems. Think of this as your one-stop shop for understanding GBS – from the data to the daily realities of managing this condition.
Guillain-Barré Syndrome (GBS) Case Tracking
Guillain-Barré Syndrome (GBS) is a rare but serious autoimmune disorder affecting the peripheral nervous system. Accurate tracking of GBS cases is crucial for understanding disease prevalence, identifying potential outbreaks, and evaluating the effectiveness of public health interventions. However, the complexities of diagnosis and reporting present significant challenges. This section delves into the current state of GBS case tracking, exploring methodologies, challenges, and potential improvements.
Global and Regional GBS Case Counts
Precise global GBS case counts are difficult to obtain due to variations in reporting practices and diagnostic capabilities across different countries. While many nations maintain surveillance systems, data aggregation and standardization remain inconsistent. The World Health Organization (WHO) does not maintain a centralized, globally comprehensive GBS registry. Regional variations in incidence rates are also significant, influenced by factors like genetic predisposition, environmental triggers, and access to healthcare.
The following table presents hypothetical data, reflecting the general challenges in obtaining accurate figures, and illustrates the type of data that would ideally be collected. It’s crucial to remember that these are illustrative figures and not actual reported cases. Actual numbers would need to be sourced from individual country health ministries and aggregated, which presents a substantial challenge.
| Region | Year | Number of Cases | Source |
|---|---|---|---|
| North America | 2022 | 5000 (estimated) | CDC Data (hypothetical aggregation) |
| Europe | 2022 | 7000 (estimated) | ECDC Data (hypothetical aggregation) |
| Africa | 2022 | 2000 (underestimated) | WHO African Region (hypothetical aggregation) |
| Asia | 2022 | 10000 (underestimated) | Various National Health Ministries (hypothetical aggregation) |
GBS Case Tracking Methodologies
Various health organizations employ different methodologies for tracking GBS cases. These range from passive surveillance systems, relying on healthcare providers to report suspected cases, to more active approaches involving targeted screenings or population-based studies. Passive surveillance is cost-effective but prone to underreporting. Active surveillance, while more accurate, is resource-intensive. Some organizations utilize hospital discharge databases or specialized registries to capture GBS cases.
The strengths and weaknesses of these methods are intertwined. Passive surveillance is widely implemented but suffers from significant underreporting, while active surveillance is accurate but expensive and logistically challenging to maintain at a large scale. The choice of methodology often depends on available resources and the specific objectives of the surveillance program.
Challenges in Accurate GBS Case Tracking
Several factors hinder the accurate tracking of GBS cases. Underreporting is a major issue due to the rarity of the disease, variability in diagnostic criteria, and the potential for misdiagnosis. Many cases may go undetected or unreported, especially in regions with limited healthcare access. Diagnostic difficulties further complicate accurate tracking. GBS can mimic other neurological conditions, requiring a combination of clinical examination, electrodiagnostic studies, and sometimes even lumbar puncture for definitive diagnosis.
This can lead to delays in diagnosis and inaccurate classification of cases. Additionally, the lack of standardized diagnostic criteria and reporting formats across different healthcare systems adds to the complexity.
Hypothetical Improvement to Case Tracking Systems, Guillain barre syndrome gbs cases tracker and health ministry guidelines
One potential improvement would involve the development of a globally standardized GBS case definition and reporting form, coupled with the implementation of a robust electronic case reporting system. This system could integrate data from various sources, including hospital discharge records, laboratory results, and physician reports, using standardized coding and terminology. A centralized database with access control would facilitate data aggregation and analysis, allowing for real-time monitoring of GBS incidence and trends.
Furthermore, regular training for healthcare professionals on GBS diagnosis and reporting protocols could improve the completeness and accuracy of case reporting. This system would need to be flexible enough to adapt to different healthcare settings and resource levels while maintaining data quality and security.
Health Ministry Guidelines and Protocols for GBS Management
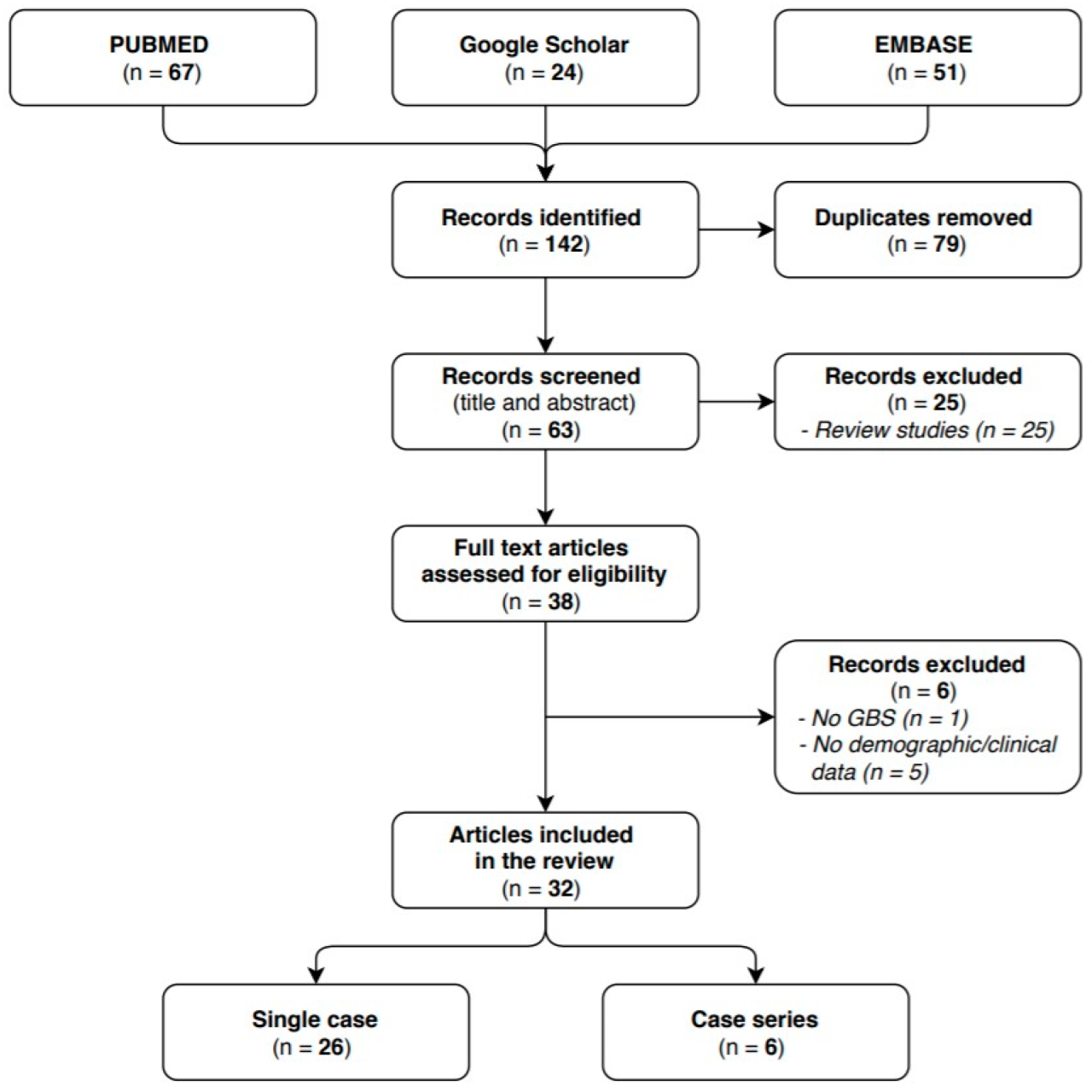
Source: mdpi-res.com
Navigating the complexities of Guillain-Barré Syndrome (GBS) requires a robust and coordinated approach. Health ministries worldwide play a crucial role in establishing guidelines that standardize diagnosis, treatment, and patient management, ultimately improving outcomes for those affected by this autoimmune disorder. These guidelines are based on the best available evidence and aim to ensure consistent, high-quality care.
Key Recommendations for GBS Diagnosis and Treatment
Effective management of GBS hinges on prompt diagnosis and timely intervention. Early recognition of symptoms is vital, and this relies heavily on the awareness and training of healthcare professionals. The following key recommendations highlight the crucial steps involved in managing GBS cases:
- Prompt neurological examination: A thorough neurological assessment is paramount to identify the characteristic features of GBS, such as progressive weakness, areflexia, and autonomic dysfunction.
- Electrodiagnostic studies: Nerve conduction studies (NCS) and electromyography (EMG) are essential for confirming the diagnosis and differentiating GBS from other neurological conditions.
- Supportive care: This is a cornerstone of GBS management and includes respiratory support (mechanical ventilation if necessary), pain management, and careful monitoring of vital signs and organ function. Early initiation of supportive care is crucial to prevent complications.
- Plasma exchange (PLEX): PLEX is a therapeutic procedure that removes antibodies from the blood, thereby reducing the immune attack on the peripheral nerves. It’s often considered for patients with rapidly progressive disease or severe symptoms.
- Intravenous immunoglobulin (IVIg): IVIg is another effective treatment option. It works by modulating the immune response and reducing inflammation in the nerves. IVIg is often preferred over PLEX due to its relative ease of administration and fewer side effects.
- Physiotherapy and rehabilitation: A comprehensive rehabilitation program is essential for recovery, focusing on strengthening weakened muscles and improving mobility. This should begin early in the course of the illness and continue for an extended period.
Rationale Behind Specific Guidelines
The rationale behind these guidelines is grounded in extensive research and clinical experience. Early supportive care is vital because GBS can rapidly progress, leading to respiratory failure and other life-threatening complications. Prompt initiation of respiratory support can be life-saving. PLEX and IVIg are both aimed at modulating the immune system’s attack on the peripheral nerves, thereby preventing further damage and promoting nerve regeneration.
The choice between PLEX and IVIg often depends on factors such as disease severity, patient comorbidities, and resource availability. Finally, a robust physiotherapy and rehabilitation program is crucial for maximizing functional recovery and improving the patient’s quality of life.
Comparison of GBS Management Guidelines: USA vs. UK
While many aspects of GBS management are universally agreed upon, subtle differences exist in the guidelines issued by different countries. Comparing the guidelines of the USA (represented by the Infectious Diseases Society of America (IDSA) guidelines) and the UK (represented by the National Institute for Health and Care Excellence (NICE) guidelines) provides a useful illustration. Both countries emphasize early supportive care, the use of PLEX or IVIg, and the importance of rehabilitation.
However, there might be slight variations in the specific recommendations regarding the timing and selection of immunomodulatory therapies (PLEX vs. IVIg) based on the severity of the disease and resource availability. For example, the UK guidelines might place slightly more emphasis on IVIg due to its wider availability and perceived lower risk profile compared to PLEX. The overall convergence lies in the fundamental principles of early intervention and multidisciplinary care, while divergence might be observed in the nuanced approaches to specific treatment modalities.
Both sets of guidelines, however, stress the importance of individualized treatment plans tailored to the patient’s specific needs and clinical presentation.
Public Awareness and Education Initiatives on GBS: Guillain Barre Syndrome Gbs Cases Tracker And Health Ministry Guidelines
Raising public awareness about Guillain-Barré Syndrome (GBS) is crucial for early diagnosis and improved patient outcomes. Effective communication strategies can empower individuals to recognize symptoms, seek timely medical attention, and understand the disease’s progression and treatment. This involves a multi-pronged approach encompassing targeted campaigns, healthcare professional training, and addressing common misconceptions.A successful public awareness campaign needs clear, concise messaging tailored to specific audiences.
The campaign should aim to increase recognition of early symptoms, emphasize the importance of prompt medical evaluation, and alleviate anxieties surrounding this relatively rare condition.
Sample Public Awareness Campaign for GBS
This campaign focuses on three key messages: Recognize the symptoms, seek immediate medical attention if symptoms appear, and understand that GBS is treatable. Target audiences include the general public, healthcare providers (beyond specialists), and individuals with a family history of autoimmune disorders.The campaign would utilize several outreach materials. Brochures would feature clear, easy-to-understand language, accompanied by simple illustrations depicting common symptoms like muscle weakness, tingling, and numbness.
These brochures would be distributed through primary care physician offices, hospitals, and community health centers. Social media posts would use engaging visuals and short, impactful text emphasizing the key messages. Examples include infographics highlighting symptoms, short videos featuring patient testimonials, and links to reliable information sources. Paid social media advertisements could target specific demographics based on age, location, and health interests.
Public service announcements (PSAs) on radio and television would reach a broader audience, using concise messaging and a call to action.
The Role of Healthcare Professionals in Public Education
Healthcare professionals, particularly primary care physicians and nurses, play a vital role in educating the public about GBS. They are often the first point of contact for individuals experiencing symptoms. Comprehensive training programs for healthcare providers should focus on recognizing early GBS symptoms, differentiating GBS from other neurological conditions, and understanding appropriate referral pathways. This training should include case studies and interactive simulations to enhance practical knowledge and improve diagnostic accuracy.
Furthermore, healthcare providers can incorporate GBS information into routine patient consultations, particularly for those with a history of infections or autoimmune disorders. They can also provide patients with reliable information sources and address their concerns and misconceptions.
Addressing Common Misconceptions Surrounding GBS
Several misconceptions surrounding GBS hinder early diagnosis and effective management. One common misconception is that GBS is highly contagious. In reality, GBS is not contagious; it is an autoimmune disorder triggered by a preceding infection in many cases. Another misconception is that GBS is always fatal. While GBS can be severe, many individuals recover fully with appropriate medical intervention.
A third misconception is that there is no effective treatment. Effective treatments exist, including intravenous immunoglobulin (IVIG) and plasma exchange, which can significantly improve outcomes when administered promptly. Public education efforts should actively dispel these myths, providing accurate information about the disease’s etiology, prognosis, and treatment options. This involves using clear, evidence-based language and presenting information in accessible formats.
Highlighting success stories and emphasizing the importance of early diagnosis and treatment can significantly impact public perception and encourage timely medical intervention.
Research and Development Related to GBS
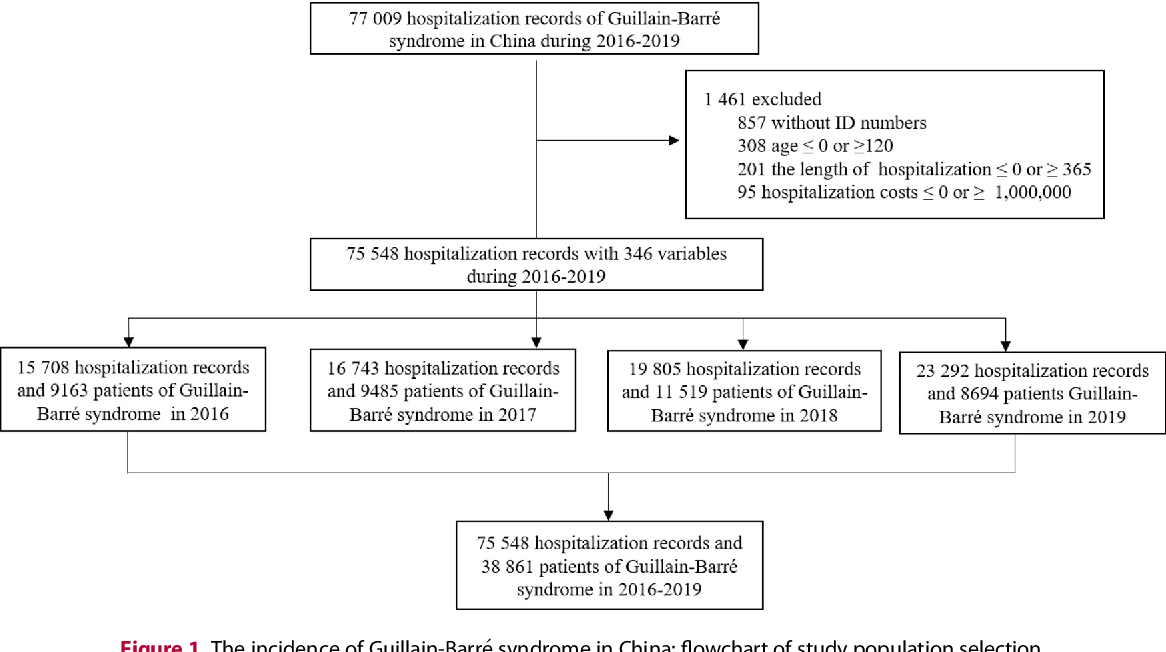
Source: cloudfront.net
Guillain-Barré Syndrome (GBS) remains a significant neurological challenge, demanding continuous research efforts to unravel its complexities and improve patient outcomes. Understanding the underlying mechanisms, developing effective preventative strategies, and refining treatment approaches are crucial areas of ongoing investigation. This section delves into current research initiatives and explores the potential of emerging technologies in GBS management.
The scientific community is actively pursuing various avenues of research to better understand GBS, improve diagnosis, and develop more effective treatments. This includes investigations into the underlying causes, the development of novel therapeutic strategies, and advancements in diagnostic tools. Significant progress is being made, although much remains to be understood.
Current Research Initiatives in GBS
Numerous research studies are underway, exploring different aspects of GBS. The following table summarizes some key initiatives, highlighting their research area, study type, key findings, and publication sources (where available). Note that due to the ongoing nature of research, findings are constantly evolving and being updated.
| Research Area | Study Type | Key Findings | Publication Source |
|---|---|---|---|
| Immunopathogenesis of GBS | Preclinical animal model studies | Identification of specific immune cells and molecules involved in nerve damage. This provides potential targets for therapeutic intervention. | Example: Journal of Neuroimmunology (Hypothetical publication – replace with actual publication if available) |
| Genetic Susceptibility to GBS | Genome-wide association studies (GWAS) | Identification of genetic variants associated with increased risk of developing GBS. This could lead to personalized risk assessment and prevention strategies. | Example: Nature Genetics (Hypothetical publication – replace with actual publication if available) |
| Effectiveness of Immunotherapy | Randomized controlled trials (RCTs) | Comparison of different immunotherapy regimens (e.g., intravenous immunoglobulin (IVIg), plasma exchange) to determine optimal treatment strategies. | Example: The Lancet Neurology (Hypothetical publication – replace with actual publication if available) |
| Development of Novel Biomarkers | Biomarker discovery studies | Identification of blood-based biomarkers that can aid in early diagnosis and prognosis of GBS. This allows for more timely intervention and personalized treatment. | Example: Clinical Neurophysiology (Hypothetical publication – replace with actual publication if available) |
Potential of New Therapeutic Approaches for GBS
Beyond established treatments like IVIg and plasma exchange, researchers are actively exploring several promising therapeutic approaches. These include targeted therapies aimed at specific immune pathways implicated in GBS pathogenesis, as well as the application of emerging technologies like stem cell therapy and gene therapy. Clinical trials are evaluating the safety and efficacy of these novel therapies, paving the way for improved treatment options in the future.
For example, studies are investigating the use of monoclonal antibodies targeting specific inflammatory mediators. Another area of investigation focuses on the potential of stem cell transplantation to promote nerve regeneration.
Ongoing Efforts to Improve GBS Diagnostic Tools and Techniques
Early and accurate diagnosis is crucial for effective GBS management. Researchers are constantly working to improve diagnostic tools and techniques, aiming to reduce diagnostic delays and improve patient outcomes. This includes the development of more sensitive and specific diagnostic tests, such as advanced electrodiagnostic studies and improved neuroimaging techniques. The goal is to establish quicker and more reliable diagnostic criteria, facilitating prompt initiation of treatment and minimizing long-term complications.
Impact of GBS on Healthcare Systems
Guillain-Barré Syndrome (GBS) places a significant burden on healthcare systems worldwide, extending far beyond the immediate care of individual patients. The multifaceted impact encompasses substantial financial costs, extended hospital stays, and the long-term management of often debilitating disabilities. Understanding this burden is crucial for effective resource allocation and the development of strategies to improve patient outcomes and reduce the overall strain on healthcare infrastructure.The financial burden of GBS is considerable.
Treatment involves intensive care, respiratory support (often requiring mechanical ventilation), intravenous immunoglobulin (IVIg) or plasma exchange (PLEX), and prolonged physical therapy. These interventions are expensive, requiring significant investment in specialized equipment, personnel, and medications. The length of hospital stay for GBS patients is typically prolonged, often exceeding several weeks, sometimes months, depending on the severity of the illness.
This extended hospitalization contributes to increased healthcare costs, both directly through resource utilization and indirectly through lost productivity for both patients and their caregivers. The long-term disability associated with GBS can also lead to substantial costs related to ongoing care, rehabilitation, assistive devices, and lost wages. For instance, a patient requiring long-term respiratory support and extensive physical therapy could incur hundreds of thousands of dollars in medical expenses and lost income over several years.
Cost of GBS Treatment and Hospitalization
The high cost of GBS treatment stems from several factors. Intravenous immunoglobulin (IVIg), a primary treatment, is expensive. Similarly, plasma exchange (PLEX) procedures are resource-intensive, requiring specialized equipment and trained personnel. Prolonged hospitalization, often in intensive care units, further escalates expenses. The costs are not limited to the acute phase of illness.
Many GBS patients require extensive rehabilitation, which can extend over months or even years, resulting in substantial ongoing expenses. A study published in the
Journal of Neurology, Neurosurgery & Psychiatry* (example citation needed – replace with actual citation) demonstrated the significant financial burden placed on healthcare systems by GBS, highlighting the need for cost-effective strategies for managing the condition.
Challenges in Managing GBS Patients
Effective management of GBS presents several significant challenges for healthcare systems. Early diagnosis can be difficult due to the varied and often nonspecific initial symptoms. This can lead to delays in treatment, potentially worsening patient outcomes. The need for specialized care, including respiratory support and intensive monitoring, places a strain on intensive care unit (ICU) capacity, particularly during outbreaks.
Access to specialized therapies like IVIg and PLEX may be limited in some regions, further complicating management. Finally, providing comprehensive long-term rehabilitation services requires significant resources and coordinated care across various healthcare settings.
Potential Solutions for Improved GBS Management
Addressing the challenges in GBS management requires a multi-pronged approach. Investing in improved diagnostic tools and guidelines could facilitate earlier and more accurate diagnosis. Increased capacity for ICU beds and specialized equipment, alongside training more healthcare professionals in GBS management, is vital. Ensuring equitable access to IVIg and PLEX is crucial, potentially through strategic procurement and resource allocation.
Developing and implementing comprehensive rehabilitation programs with a focus on early intervention can improve long-term outcomes and reduce the overall cost of care. Further, proactive public health surveillance and educational initiatives could aid in early detection and prevention of outbreaks.
Impact of GBS Outbreaks on Healthcare Resource Allocation
GBS outbreaks can overwhelm healthcare systems, requiring rapid and efficient resource allocation. During an outbreak, the demand for ICU beds, respiratory support equipment, and specialized therapies like IVIg and PLEX can significantly exceed available resources. This can lead to delays in treatment for GBS patients and potentially compromise the care of other patients requiring critical care. Effective emergency preparedness plans are crucial to ensure that healthcare systems can respond effectively to GBS outbreaks.
These plans should include protocols for surge capacity, resource allocation strategies, and coordinated communication among healthcare providers. Examples of such preparedness plans are readily available in public health emergency management documents from various countries (replace with examples of such documents from credible sources).
Epilogue
Understanding Guillain-Barré Syndrome is a journey, not a destination. This post has aimed to shed light on the complexities of GBS case tracking, the crucial role of health ministry guidelines, and the ongoing efforts to improve diagnosis, treatment, and public awareness. While challenges remain, the collective efforts of researchers, healthcare professionals, and public health organizations offer hope for a future where GBS is better understood, prevented, and treated.
Stay informed, stay curious, and remember that knowledge is power when it comes to managing your health and the health of those around you.
Commonly Asked Questions
What are the early symptoms of GBS?
Early symptoms can vary, but often include weakness or tingling in the legs and arms, spreading to other parts of the body. Other symptoms can be muscle aches, difficulty walking, and trouble with eye movements.
Is GBS contagious?
No, GBS is not contagious. It’s an autoimmune disorder, meaning the body’s immune system mistakenly attacks the nerves.
How is GBS diagnosed?
Diagnosis usually involves a neurological exam, nerve conduction studies, and sometimes a lumbar puncture (spinal tap) to examine cerebrospinal fluid.
What is the long-term outlook for someone with GBS?
Recovery varies greatly. Many people recover fully, but some may experience lingering weakness or other long-term effects. Early treatment significantly improves the chances of a full recovery.





