Health Insurer Medical Costs Climbing MA Medicaid
Health insurer medical costs climbing MA Medicaid – that’s the alarming headline grabbing everyone’s attention. Massachusetts, like many states, is facing a perfect storm of rising healthcare expenses, impacting everything from access to care to the very solvency of the state’s Medicaid program. This isn’t just about numbers on a spreadsheet; it’s about real people struggling to afford essential medical services.
We’ll dive into the factors driving this crisis, explore the challenges facing insurers and the state, and look at potential solutions to ensure everyone in Massachusetts can access the care they need.
This isn’t just a Massachusetts problem; it reflects a national trend of escalating healthcare costs. We’ll examine the specific pressures on MA Medicaid, including the largest cost drivers and how those costs translate into real-world consequences for patients. We’ll also investigate the strategies health insurers are employing to manage these costs, weighing their effectiveness against potential downsides. Ultimately, we’ll explore potential policy changes that could ease the strain on both the system and its patients.
Rising Healthcare Costs in Massachusetts
Massachusetts, like many other states, is grappling with a significant increase in healthcare costs. This rise impacts both health insurers and the state’s residents, particularly those relying on the Massachusetts Medicaid program, MassHealth. Understanding the contributing factors is crucial for developing effective strategies to mitigate these escalating expenses and ensure the long-term sustainability of the healthcare system.
Factors Contributing to Increased Medical Costs in Massachusetts
Several intertwined factors contribute to the escalating medical costs in Massachusetts. These include the rising cost of prescription drugs, the increasing complexity and cost of treating chronic diseases, and the overall aging population. The high concentration of specialized medical facilities and providers in the state also contributes to higher prices compared to other regions. Furthermore, administrative burdens and the complexities of the insurance system itself add to the overall cost.
Health insurer medical costs are skyrocketing in Massachusetts, putting a strain on Medicaid. This rising cost pressure is felt nationwide, and the recent news about hshs prevea closing Wisconsin hospitals and health centers highlights the broader challenges facing healthcare systems. These closures will likely impact access to care and potentially drive up costs even further, exacerbating the already difficult situation for Massachusetts Medicaid.
Finally, the adoption of new medical technologies, while often beneficial, frequently comes with a high price tag.
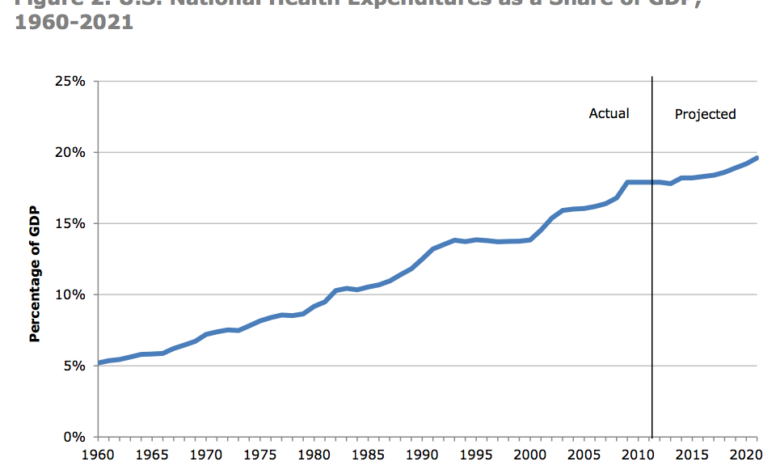
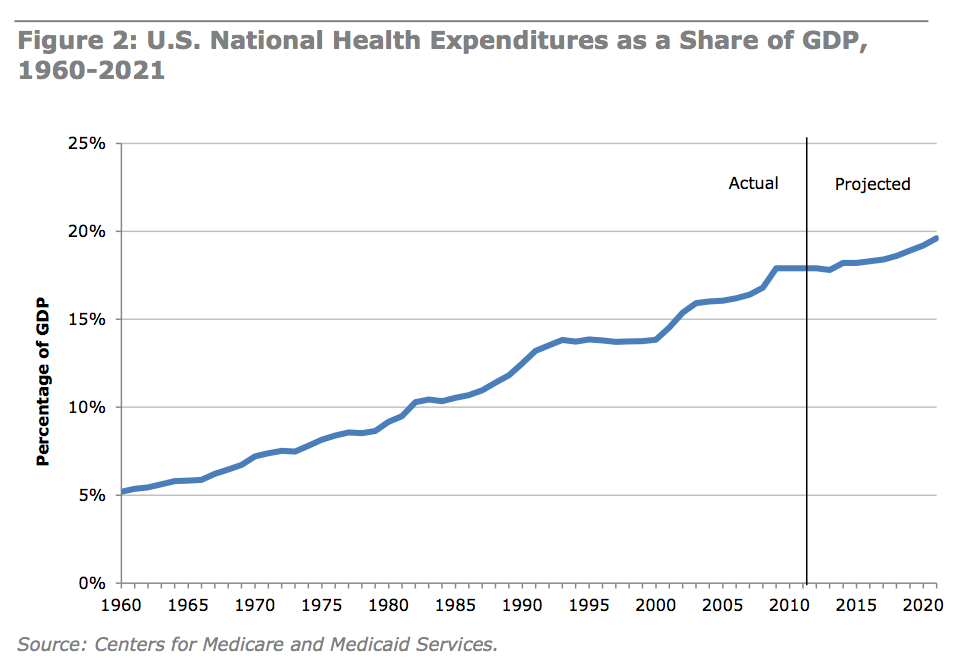
Comparison of Massachusetts Medical Cost Increases with National Averages
While precise comparisons require detailed analysis of specific data sets from various sources, it’s generally acknowledged that Massachusetts healthcare costs often exceed national averages. Several studies have shown that the rate of increase in Massachusetts healthcare spending has historically been higher than the national average, although the gap may fluctuate from year to year depending on economic conditions and policy changes.
For example, a study by the Massachusetts Health Policy Commission (MHPC) might show a specific percentage difference in the rate of increase between MA and the national average over a given period. (Note: Specific data would need to be sourced from the MHPC or similar reliable sources for accurate figures).
Largest Cost Drivers within the MassHealth System
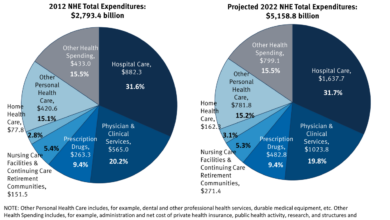
The largest cost drivers within the MassHealth system are multifaceted. Hospital care consistently accounts for a significant portion of spending, driven by factors like high utilization rates, the complexity of cases, and the cost of advanced medical technology. Physician services, including specialist consultations and procedures, also represent a substantial expense. Pharmaceutical costs, especially for specialty drugs used to treat chronic conditions, continue to climb rapidly.
Finally, the increasing prevalence of chronic diseases among the MassHealth population contributes significantly to overall spending, necessitating ongoing and expensive treatments.
Percentage Breakdown of Medicaid Spending Across Healthcare Categories, Health insurer medical costs climbing ma medicaid
The following table provides a hypothetical percentage breakdown of MassHealth spending across major categories. Actual figures vary from year to year and can be found in reports published by the Massachusetts Health Policy Commission. This table serves as an illustrative example.
| Healthcare Category | Percentage of Spending | Healthcare Category | Percentage of Spending |
|---|---|---|---|
| Hospital Care | 40% | Physician Services | 25% |
| Pharmaceuticals | 15% | Other (e.g., Long-Term Care, Home Health) | 20% |
Impact on MA Medicaid
The escalating cost of healthcare in Massachusetts presents a significant challenge to the state’s Medicaid program, MassHealth. Rising prescription drug prices, increased utilization of expensive medical technologies, and the growing number of individuals needing care all contribute to a strain on the system’s resources, potentially impacting the quality and accessibility of care for millions of low-income residents. This necessitates a careful examination of the program’s budget and the exploration of sustainable cost-containment strategies.The rising tide of medical costs directly impacts MassHealth’s ability to provide comprehensive and timely care to its beneficiaries.
Budgetary constraints force difficult choices, potentially leading to longer wait times for appointments, limited access to specialized care, and restrictions on the types of treatments covered. This creates a ripple effect, impacting not only the recipients’ health outcomes but also the overall efficiency and effectiveness of the healthcare system. The program faces immense pressure to balance the needs of its growing population with the realities of a finite budget.
Budgetary Challenges for MassHealth
MassHealth’s budget is primarily funded through a combination of state and federal dollars. However, the escalating costs of healthcare consistently outpace the growth in funding, creating a persistent budget deficit. This necessitates ongoing negotiations with the federal government to secure additional funding and the implementation of rigorous cost-control measures within the state. Failure to effectively manage these challenges could result in significant cuts to essential services or a reduction in the number of individuals eligible for coverage.
For example, the recent surge in demand for mental health services has placed considerable strain on the MassHealth budget, highlighting the need for proactive and innovative solutions.
Cost Containment Strategies for MassHealth
Implementing effective cost-containment strategies is crucial for the long-term viability of MassHealth. Strategies must focus on both improving efficiency and promoting preventative care. Negotiating lower drug prices with pharmaceutical companies, promoting the use of generic medications, and investing in preventative care programs can significantly reduce healthcare costs in the long run. Furthermore, leveraging technology to improve care coordination and reduce administrative overhead can free up resources to be directed toward patient care.
Innovative payment models, such as value-based care, can incentivize providers to focus on quality and efficiency, leading to better outcomes at a lower cost. For instance, initiatives focused on managing chronic conditions through telehealth and remote patient monitoring can be highly cost-effective and improve patient outcomes.
Potential Consequences of Uncontrolled Cost Increases
The unchecked rise in medical costs poses several severe consequences for MassHealth recipients.
- Reduced Access to Care: Longer wait times for appointments, limited access to specialists, and fewer covered services.
- Decreased Quality of Care: Compromised access to necessary medications, treatments, and preventative services.
- Increased Financial Burden: Higher out-of-pocket costs, including co-pays and deductibles, despite having insurance.
- Health Disparities: Exacerbation of existing health disparities, disproportionately affecting vulnerable populations.
- Negative Health Outcomes: Increased hospitalizations, worsening chronic conditions, and higher mortality rates due to delayed or inadequate care.
The Role of Health Insurers
Health insurers in Massachusetts play a crucial role in navigating the complex landscape of rising medical costs. Their strategies significantly impact both the affordability and accessibility of healthcare for residents, particularly those enrolled in Medicaid. Understanding their approaches is key to addressing the broader challenges facing the state’s healthcare system.Insurers employ a multifaceted approach to manage escalating medical expenses.
These strategies range from negotiating rates with providers to implementing cost-containment programs for their members. The effectiveness and impact of these methods vary, often depending on the specific insurer and the details of their contracts.
Strategies for Managing Rising Medical Costs
Health insurers in MA utilize a variety of methods to control costs. These strategies aim to balance the need to provide comprehensive coverage with the imperative to keep premiums affordable. A key element is the ongoing negotiation and contracting with healthcare providers, a process that significantly influences the overall price of medical services. Other strategies involve incentivizing preventative care, managing utilization through care management programs, and leveraging data analytics to identify and address areas of high spending.
For example, some insurers offer rewards for preventative screenings, while others employ sophisticated algorithms to identify patients at high risk of costly hospitalizations and proactively intervene with targeted interventions.
Comparison of Insurer Approaches
Different health insurers in Massachusetts adopt distinct approaches to cost management, reflecting variations in their business models, market strategies, and network structures. Some insurers, for instance, may prioritize building narrow networks of preferred providers, thereby negotiating lower rates but potentially limiting patient choice. Others might opt for broader networks, offering greater flexibility but potentially paying higher rates to providers.
The emphasis on specific cost-containment techniques also varies. Some insurers might heavily invest in disease management programs for chronic conditions like diabetes or heart disease, while others may focus more on utilization management strategies to curb unnecessary hospital admissions or procedures. This diversity in approaches reflects the competitive dynamics within the MA insurance market.
Influence of Insurer Negotiations with Healthcare Providers
Negotiations between health insurers and healthcare providers are a central determinant of medical costs. These negotiations involve setting reimbursement rates for various services, determining the scope of covered benefits, and establishing utilization management protocols. Insurers with significant market share generally have greater bargaining power, enabling them to negotiate lower rates with providers. However, overly aggressive negotiations could lead to provider shortages or limit access to specialized care.
Conversely, less stringent negotiations may lead to higher costs that are passed on to consumers through premiums. The balance between securing affordable rates and ensuring adequate access to care is a constant challenge in these negotiations.
Cost-Management Techniques Employed by Insurers
| Cost-Management Technique | Effectiveness | Potential Drawbacks | Example |
|---|---|---|---|
| Negotiating lower provider rates | High, if significant market share | Potential for provider shortages, limited access to care | Blue Cross Blue Shield negotiating lower rates with Mass General Hospital |
| Disease management programs | Moderate to high, depending on program design and patient engagement | Requires significant investment, may not be effective for all conditions | Aetna’s program for managing diabetes |
| Utilization management (pre-authorization, etc.) | Moderate, effectiveness depends on implementation | Can be burdensome for providers and patients, potential for delays in care | Prior authorization requirements for certain procedures |
| Incentivizing preventative care | High, long-term cost savings | Requires patient engagement, may not prevent all costly events | Wellness programs offering rewards for screenings |
Patient Access and Outcomes
Source: wbur.org
Rising healthcare costs in Massachusetts directly impact the accessibility and quality of care received by MA Medicaid recipients. The correlation between escalating medical expenses and diminished access to care is a significant concern, potentially leading to poorer health outcomes for a vulnerable population. This section explores this critical link, illustrating how increased costs translate into real-world challenges for patients.The increased cost of healthcare services, coupled with the often-limited financial resources of Medicaid beneficiaries, creates a precarious situation.
Even small increases in premiums, co-pays, or deductibles can represent a significant financial burden, forcing difficult choices between essential needs and healthcare. This financial strain can lead to delayed or forgone care, resulting in worsening health conditions and ultimately, higher healthcare costs in the long run. Prevention becomes less accessible, leading to more expensive treatment later.
Impact of Cost Increases on Health Outcomes
Increased healthcare costs directly impact the health outcomes of Medicaid beneficiaries. Delayed or forgone care due to financial constraints can lead to a worsening of chronic conditions, increased hospitalizations, and even premature mortality. For example, a diabetic patient who delays filling their insulin prescription due to cost concerns risks severe complications, including blindness, kidney failure, and heart disease, requiring far more extensive and expensive treatment later.
Similarly, a patient delaying necessary cancer screenings might face a later, more aggressive, and ultimately more costly diagnosis and treatment. These are not isolated incidents; they represent a systemic problem where financial barriers to care lead to significant health consequences.
Examples of Delayed or Forgone Care
Rising costs manifest in several ways, leading to delayed or forgone care. Many Medicaid recipients may delay or forgo preventative care, such as annual checkups and screenings, due to cost concerns. This can lead to the detection of serious illnesses at later, more advanced stages, resulting in more expensive and less effective treatment. Similarly, patients may postpone necessary specialist visits or opt for less expensive, but potentially less effective, treatment options.
The inability to afford prescription medications is another significant factor, often forcing patients to ration their medications or discontinue them altogether, leading to uncontrolled conditions and potential emergencies. The cumulative effect of these choices contributes to poorer overall health outcomes.
Scenario Illustrating Impact of Rising Costs
Imagine Maria, a 62-year-old MA Medicaid recipient with hypertension and diabetes. Her medication costs have recently increased, and she is struggling to afford them all. She has been experiencing chest pains, but due to her limited financial resources and high co-pays, she delays seeking medical attention. This delay in seeking care could lead to a more serious cardiovascular event, requiring hospitalization, extensive treatment, and potentially even long-term disability.
The initial cost savings from delaying care become dwarfed by the significantly higher costs associated with treating a more advanced and potentially life-threatening condition. This scenario highlights the vicious cycle of rising costs and diminished access to timely, effective healthcare.
Potential Solutions and Policy Recommendations
Source: pbs.org
Addressing the escalating medical costs within the MA Medicaid system requires a multifaceted approach encompassing policy changes, innovative cost-containment strategies, and a focus on improving healthcare delivery models. Simply put, we need a smarter, more efficient, and more equitable system. This requires a concerted effort from policymakers, healthcare providers, and insurers alike.The long-term effects of policy interventions are complex and often depend on the specific context and implementation.
However, we can analyze potential outcomes based on the experiences of other states and the principles of effective healthcare policy. For example, poorly designed programs can exacerbate existing inequalities, while well-designed programs can improve access and reduce costs in the long run. A critical factor is ensuring sufficient funding and effective oversight to prevent unintended consequences.
Soaring healthcare costs are a major concern, especially with rising MA Medicaid expenses. It makes you wonder about preventative measures, and I recently read an interesting article about how an eye test might help predict dementia risk – check it out: can eye test detect dementia risk in older adults. Early detection could potentially reduce long-term care costs, easing the burden on insurers and taxpayers alike, and hopefully helping to control the overall rise in medical spending.
Strategies for Cost Containment
Effective cost containment requires a blend of strategies targeting both the supply and demand sides of healthcare. Focusing solely on one aspect rarely yields optimal results. We need a comprehensive approach that addresses administrative inefficiencies, promotes preventative care, and incentivizes value-based care models.
- Negotiating Drug Prices: Massachusetts could explore strategies similar to those employed by other states, such as bulk purchasing agreements with pharmaceutical companies or utilizing the power of its large Medicaid population to negotiate lower prices for commonly prescribed drugs. This could significantly impact overall spending.
- Promoting Preventative Care: Investing in preventative care programs, including screenings and wellness initiatives, can reduce the need for costly treatments down the line. This requires expanding access to preventative services and addressing social determinants of health that contribute to poor health outcomes.
- Implementing Value-Based Care: Shifting from a fee-for-service model to value-based care, which rewards providers for positive patient outcomes rather than the volume of services provided, can incentivize efficiency and quality improvements. This approach requires careful design and monitoring to avoid unintended consequences.
Comparison of Cost-Containment Strategies in Other States
Several states have implemented successful cost-containment strategies. For example, Maryland’s all-payer system, which involves negotiating rates with all payers (including private insurers), has demonstrated success in controlling healthcare costs. Oregon’s Medicaid expansion, while facing challenges, has also offered insights into managing costs within a broader expansion context. Analyzing the successes and failures of these initiatives provides valuable lessons for Massachusetts.
Health insurer medical costs are skyrocketing, putting a strain on MA Medicaid and everyone involved. A big part of this problem is the increasing difficulty in processing medical claims, largely due to a shortage of skilled medical coders. One potential solution lies in exploring technological advancements, like those described in this article about the ai powered solution to the medical coding worker shortage , which could streamline the process and ultimately help control costs for MA Medicaid.
Efficient coding translates directly to quicker reimbursements and better cost management for insurers.
A comparative study of these models, focusing on their impact on access and quality, is essential for informed policymaking.
Policy Recommendations for Massachusetts
The following policy recommendations are designed to address the rising medical costs within the MA Medicaid system while ensuring equitable access to quality healthcare.
- Strengthening the State’s Negotiating Power: Empower the state to negotiate directly with pharmaceutical companies and healthcare providers to secure lower prices for medications and services.
- Investing in Preventative Care: Expand access to preventative care services and address social determinants of health that contribute to higher healthcare utilization.
- Transitioning to Value-Based Care: Implement a phased transition to value-based care models that incentivize quality and efficiency.
- Improving Data Collection and Analysis: Enhance data collection and analysis capabilities to better understand cost drivers and evaluate the effectiveness of policy interventions.
- Promoting Transparency and Accountability: Increase transparency in healthcare pricing and provider performance to improve accountability and encourage cost-conscious practices.
Last Point
The rising cost of healthcare in Massachusetts, particularly within the MA Medicaid system, presents a significant challenge. While health insurers are implementing cost-containment strategies, the problem demands a multifaceted solution involving policy changes, innovative cost-management techniques, and a renewed focus on preventative care. The ultimate goal is to ensure affordable and accessible healthcare for all residents, regardless of their ability to pay.
Ignoring this issue will only lead to worse outcomes for patients and further strain on the already burdened system. Let’s hope for proactive solutions and a future where healthcare is a right, not a privilege.
Frequently Asked Questions: Health Insurer Medical Costs Climbing Ma Medicaid
What are the biggest factors driving up healthcare costs in Massachusetts?
Several factors contribute, including the rising cost of prescription drugs, expensive hospital procedures, an aging population requiring more care, and administrative overhead.
How does Massachusetts compare to other states in terms of healthcare costs?
Massachusetts consistently ranks among the highest in the nation for healthcare spending. This is due to a combination of factors, including higher provider salaries and a higher concentration of specialized medical services.
What are the potential consequences of failing to address these rising costs?
Failure to address rising costs could lead to reduced access to care, compromised quality of care, and increased financial burden on both the state and individuals. It could also impact the overall health and well-being of Medicaid recipients.
Are there successful cost-containment strategies used in other states that could be adopted in Massachusetts?
Yes, other states have successfully implemented various strategies, such as value-based care models, increased focus on preventative care, and negotiating better drug prices. Massachusetts could learn from these examples.