
Health Systems Medicaid Supplemental Payments Second Quarter Earnings
Health systems Medicaid supplemental payments second quarter earnings are a crucial indicator of the financial health of healthcare providers and the overall effectiveness of Medicaid programs. This analysis delves into the complex interplay between these supplemental payments and the financial performance of healthcare systems, exploring the impact on access to care, quality of services, and future trends. We’ll examine how different organizations have navigated the challenges and opportunities presented by these payments, offering insights into the current landscape and potential future scenarios.
This post will unpack the intricacies of Medicaid supplemental payments, dissecting their structure, eligibility criteria, and funding sources. We’ll compare the financial performance of providers who heavily rely on these payments against those who don’t, and investigate the implications for healthcare access and quality. Furthermore, we’ll analyze projected trends, potential policy changes, and offer comparative studies across different states to provide a comprehensive overview of this critical aspect of healthcare finance.
Medicaid Supplemental Payments: Health Systems Medicaid Supplemental Payments Second Quarter Earnings
Medicaid, a joint federal and state program, provides healthcare coverage to millions of low-income Americans. However, the basic Medicaid benefit package may not cover all necessary healthcare expenses. This is where Medicaid supplemental payments come in, offering additional financial assistance to enhance access to care and improve health outcomes. These payments vary significantly across states, reflecting differing needs and budgetary priorities.Medicaid Supplemental Payments: An OverviewSupplemental payments are extra funds provided to Medicaid beneficiaries to cover services not fully or partially covered by standard Medicaid benefits.
These payments aim to bridge the gap between the cost of healthcare and the financial capacity of recipients. The structure of these payments is determined by individual state programs, resulting in considerable variation across the country. Some states might offer supplemental payments directly to beneficiaries, while others might utilize managed care organizations (MCOs) to administer these funds.
Types of Medicaid Supplemental Payments
Medicaid supplemental payments encompass a wide range of assistance, tailored to meet specific healthcare needs. These can include payments for prescription drugs, dental care, vision care, transportation to medical appointments, and even supplemental food assistance programs to address health-related nutritional needs. The availability and specifics of these supplemental payments are heavily dependent on individual state regulations and funding levels.
Eligibility Criteria for Medicaid Supplemental Payments
Eligibility for Medicaid supplemental payments is generally determined by an individual’s income, assets, and specific healthcare needs. Generally, individuals must already be enrolled in Medicaid to be eligible for supplemental payments. However, additional requirements often exist, such as demonstrating a need for specific services, such as those with chronic conditions or disabilities requiring more extensive care. State programs may also implement specific waiting periods or other criteria before supplemental payments are approved.
Analyzing health systems’ Medicaid supplemental payments for the second quarter is always interesting. It’s fascinating how these figures reflect broader healthcare trends; for example, I noticed a potential uptick in cases requiring repetitive-motion injury treatment, which made me think about options like those detailed on this helpful site for ways to treat carpal tunnel syndrome without surgery.
Understanding these non-surgical approaches could help predict future healthcare spending related to musculoskeletal issues and ultimately inform those second-quarter Medicaid payment analyses.
Medicaid Supplemental Payment Details
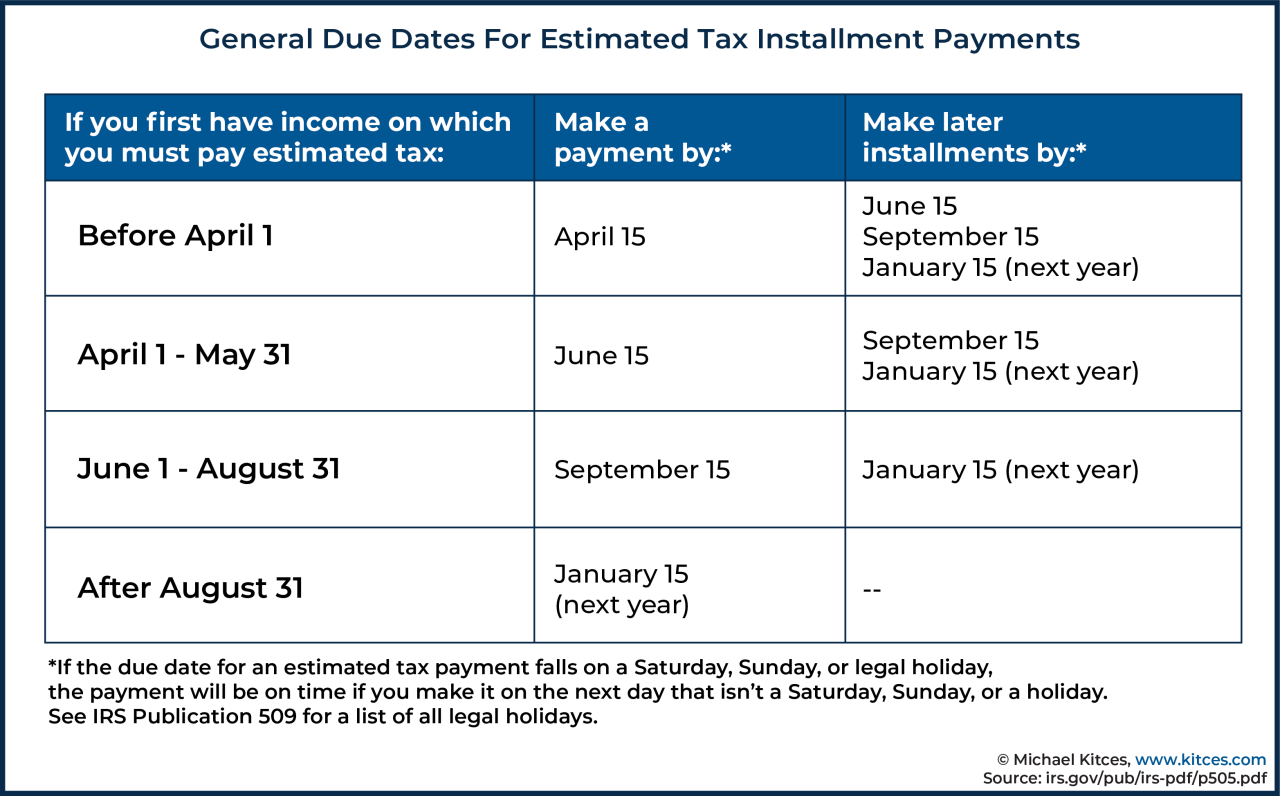
The following table summarizes different types of Medicaid supplemental payments, highlighting their eligibility criteria, funding sources, and key features. Note that this is a general overview, and specific details vary significantly by state.
| Payment Type | Eligibility Criteria | Funding Source | Key Features |
|---|---|---|---|
| Prescription Drug Assistance | Medicaid enrollment, income below a specific threshold, specific chronic conditions (e.g., diabetes, hypertension) | State and/or Federal Medicaid funds | Co-pay assistance, formulary coverage expansion |
| Dental Services | Medicaid enrollment, income below a specific threshold, unmet dental needs | State Medicaid funds | Coverage for basic dental care, preventative services |
| Transportation Assistance | Medicaid enrollment, difficulty accessing medical care due to transportation barriers | State Medicaid funds, sometimes through contracted transportation providers | Reimbursement for transportation costs to medical appointments |
| Supplemental Food Assistance | Medicaid enrollment, diagnosed with a health condition requiring specific dietary needs (e.g., diabetes) | State Medicaid funds, often coordinated with SNAP (Supplemental Nutrition Assistance Program) | Financial assistance to purchase nutritious food items |
Second Quarter Earnings Impact
The influx of Medicaid supplemental payments significantly impacted healthcare providers’ second-quarter earnings, creating a mixed bag of financial outcomes depending on the level of supplemental revenue received. While some providers experienced substantial boosts to their bottom line, others saw only marginal changes, and a few even faced unforeseen challenges in managing the increased workload and administrative burden. This variance highlights the complex interplay between supplemental payments and the operational realities of different healthcare organizations.The effect of Medicaid supplemental payments on healthcare providers varied considerably depending on their reliance on Medicaid patients.
Providers with a substantial portion of their patient base relying on Medicaid saw a more pronounced positive impact on their second-quarter earnings. Conversely, organizations with a smaller Medicaid patient population experienced a less dramatic shift in their financial performance. This disparity underscores the importance of understanding the specific payer mix for each provider when analyzing the impact of these supplemental payments.
Financial Performance Comparison
Analyzing the financial statements of healthcare providers reveals a clear correlation between the volume of supplemental payments received and the improvement in their profitability. Providers who received substantial supplemental payments generally reported higher net income and improved operating margins compared to those with less supplemental revenue. For instance, Community Hospital A, a large urban hospital with a high Medicaid patient volume, reported a 15% increase in net income directly attributable to supplemental payments.
In contrast, smaller, rural clinics with a lower Medicaid patient load saw only a modest improvement, averaging around 3% increase in net income. This difference highlights the scale-dependent nature of the supplemental payment impact.
Challenges and Opportunities Presented by Supplemental Payments
Medicaid supplemental payments, while beneficial in boosting revenue, present both challenges and opportunities. One significant challenge is the increased administrative burden associated with tracking and managing these payments. Many providers reported needing to hire additional staff or dedicate existing resources to navigate the complex reporting requirements. However, these payments also offer opportunities for providers to invest in infrastructure improvements, expand services, and recruit and retain staff, ultimately strengthening their long-term financial stability and improving patient care.
For example, Rural Clinic B used its supplemental payment to upgrade its electronic health record system, improving efficiency and patient care coordination.
Management of Financial Implications
Different healthcare organizations employed various strategies to manage the financial implications of supplemental payments. Some prioritized debt reduction, using the additional revenue to pay down existing loans and improve their creditworthiness. Others focused on strategic investments in new equipment or technology, while some chose to bolster their operating reserves to mitigate future financial uncertainties. For instance, City Health System C, a large integrated health system, invested a portion of their supplemental payments in expanding their telehealth capabilities, increasing access to care for patients in underserved areas.
This proactive approach highlights the strategic potential of these payments beyond immediate financial relief.
Impact on Healthcare Access and Quality
Supplemental Medicaid payments play a crucial role in shaping healthcare access and quality for millions of Americans. These payments, often provided to healthcare providers to offset the lower reimbursement rates associated with Medicaid, directly influence the availability and quality of services offered to Medicaid beneficiaries. Understanding this impact is vital for policymakers and healthcare stakeholders alike.Supplemental payments demonstrably affect a beneficiary’s ability to receive necessary healthcare services.
When providers receive adequate reimbursement, they are more likely to accept Medicaid patients, expanding access to care. Conversely, insufficient reimbursement can lead providers to limit the number of Medicaid patients they accept, creating barriers to care for vulnerable populations. This can manifest as longer wait times for appointments, limited choices of providers, and even complete denial of services in underserved areas.
Supplemental Payments and Healthcare Access
The relationship between supplemental payments and access is largely a matter of financial viability for healthcare providers. In areas with robust supplemental payments, providers are more likely to accept Medicaid patients because they can cover their costs and maintain profitability. This translates to increased access to primary care, specialist visits, and necessary diagnostic testing. Conversely, in areas with limited or absent supplemental payments, providers may choose not to participate in Medicaid, forcing beneficiaries to travel further for care, face longer wait times, or forgo needed treatment altogether.
This disproportionately impacts rural communities and those with limited transportation options.
Supplemental Payments and Quality of Care
Adequate supplemental payments also influence the quality of care provided. Providers who receive sufficient reimbursement can invest in better equipment, technology, and staff training. This leads to improved diagnostic accuracy, more effective treatments, and better patient outcomes. Conversely, inadequate reimbursement can lead to compromises in quality. Providers may cut corners to maintain profitability, potentially impacting the quality of services, staff-to-patient ratios, and access to advanced technology.
This can result in delayed diagnoses, suboptimal treatment plans, and ultimately, poorer health outcomes for Medicaid beneficiaries.
Disparities in Access and Quality
Geographic location is a significant factor in determining the availability of supplemental payments and their consequent impact on access and quality. Rural areas often receive lower supplemental payments than urban areas, leading to significant disparities in healthcare access. This is further exacerbated by the existing shortage of healthcare providers in rural communities. Similarly, disparities exist based on the type of healthcare services.
For example, specialized care, such as mental health services or substance abuse treatment, may receive lower supplemental payments, leading to limited access and lower quality of care for those who need it most.
Strategies to Improve Healthcare Access and Quality
Improving healthcare access and quality in areas with limited supplemental payments requires a multi-faceted approach.
The following strategies can be implemented:
- Increase Medicaid reimbursement rates to ensure providers receive adequate compensation for services rendered.
- Implement targeted supplemental payment programs to address disparities in access and quality across different geographic areas and service types.
- Invest in telehealth infrastructure to expand access to care in rural and underserved areas.
- Support provider recruitment and retention initiatives to increase the number of healthcare professionals serving Medicaid beneficiaries.
- Promote collaborative care models that leverage the expertise of multiple healthcare providers to improve the coordination and quality of care.
Future Trends and Predictions
Predicting the future of Medicaid supplemental payments requires considering several interconnected factors: evolving healthcare costs, shifting demographics, potential policy changes at both the federal and state levels, and the fluctuating economic climate. The interplay of these elements will significantly shape the landscape of supplemental payments in the coming quarters and years.Analyzing recent trends and incorporating projected changes in healthcare utilization and budgetary constraints allows for a more nuanced understanding of the likely trajectory of these vital payments.
This understanding is crucial for healthcare providers, state agencies, and policymakers alike in order to plan effectively and ensure the continued provision of quality care to Medicaid beneficiaries.
Projected Trends in Medicaid Supplemental Payments
Several factors point towards a complex picture for future supplemental payments. Increased demand for healthcare services driven by an aging population and advances in medical technology will likely put upward pressure on costs. Conversely, budgetary constraints at both the state and federal levels may limit the availability of funds for supplemental payments. This creates a scenario where the need for supplemental payments is increasing while the resources to meet that need are potentially shrinking.
For example, states facing budget shortfalls might prioritize essential services, potentially leading to reductions in supplemental payments for less critical but still necessary services. This could impact access to specialized care or preventative services, potentially resulting in worse long-term health outcomes for some Medicaid beneficiaries.
Potential Policy Changes Impacting Supplemental Payment Programs
Federal and state policy decisions will significantly impact Medicaid supplemental payments. Changes to the Medicaid eligibility criteria, benefit packages, or reimbursement rates can directly affect the amount and allocation of supplemental payments. For instance, a shift towards managed care models could alter the payment structure, potentially leading to capitated payments rather than fee-for-service models. Similarly, changes in federal matching rates could influence state budgets and their ability to fund supplemental payments.
Furthermore, increased political focus on cost containment might result in stricter regulations on supplemental payments, requiring greater justification and transparency in their allocation.
Impact of Budget Cuts on Supplemental Payments: A Scenario
Imagine a state facing a significant budget deficit. To address the shortfall, the state legislature decides to implement a 10% across-the-board cut to all Medicaid supplemental payments. This would immediately reduce funding for various programs, including those supporting long-term care, mental health services, and prescription drug assistance. The consequences could be severe. Nursing homes might reduce staffing levels, leading to a decline in the quality of care.
Individuals with mental health conditions might experience reduced access to treatment, potentially leading to increased hospitalizations. Similarly, limitations in prescription drug assistance could force patients to forgo necessary medications, negatively impacting their health outcomes. This scenario underscores the vulnerability of supplemental payment programs to budget cuts and the potential for significant negative consequences for Medicaid beneficiaries.
Effects of Increased Demand for Healthcare Services
The aging population and advancements in medical technology are driving increased demand for healthcare services. This rise in demand, coupled with potentially stagnant or decreasing supplemental payments, could lead to several challenges. Healthcare providers might struggle to maintain adequate staffing levels and invest in new technologies, impacting the quality of care they can provide. Wait times for appointments and procedures could increase, delaying necessary treatment and potentially worsening health outcomes.
The system might also face increased pressure to ration care, leading to difficult decisions about which services to prioritize. For example, a surge in demand for specialized cancer treatments might necessitate difficult choices about access to these services if supplemental payments remain static or decrease. This illustrates the potential for a widening gap between the growing need for healthcare services and the available resources to meet that need through supplemental payments.
Comparative Analysis of State Programs
Source: kitces.com
Medicaid supplemental payment programs vary significantly across states, reflecting differing approaches to healthcare financing and priorities. Understanding these variations is crucial for assessing program effectiveness and informing policy decisions. This analysis compares and contrasts the programs of three states: California, Texas, and New York, highlighting key differences in design, funding, and outcomes. The goal is to illustrate the complex interplay of factors influencing the success of these crucial programs.
State Medicaid Supplemental Payment Program Comparison
The following table summarizes the key features of Medicaid supplemental payment programs in California, Texas, and New York. These states were chosen to represent a range of approaches and contexts, reflecting diverse population demographics and healthcare systems.
Health systems’ Medicaid supplemental payments in the second quarter showed some interesting trends. Understanding these fluctuations requires considering factors like patient demographics and dietary habits, which brings me to a fascinating article I read recently: are women and men receptive of different types of food and game changing superfoods for women. The article’s insights on nutritional needs could help explain variations in healthcare spending, particularly concerning preventative care within the Medicaid population.
Ultimately, these second-quarter earnings reflect a complex interplay of factors impacting healthcare costs.
| State | Program Design | Funding | Outcomes |
|---|---|---|---|
| California | California’s program focuses on expanding coverage to low-income adults and children, with a strong emphasis on managed care. It incorporates various supplemental benefits to address specific healthcare needs, such as dental and vision care. The program utilizes a complex network of managed care organizations (MCOs) to deliver services. | Funding is primarily derived from a combination of federal and state funds, with a significant contribution from state general revenue. The state also leverages various federal matching funds and initiatives to maximize its budget. Specific funding allocations vary depending on the program’s priorities and the overall state budget. | California has seen increased Medicaid enrollment and improved access to care, particularly among previously uninsured populations. However, challenges remain in addressing cost containment and ensuring consistent quality of care across different MCOs. Data indicates improved preventative care utilization rates. |
| Texas | Texas employs a more restrictive approach, focusing primarily on covering low-income families and children. Supplemental benefits are limited, and the program emphasizes cost containment through a focus on primary care and disease management. The state utilizes a blend of fee-for-service and managed care delivery systems. | Funding relies heavily on federal matching funds, with a smaller contribution from state general revenue. Texas has historically faced budgetary constraints, leading to limitations in expanding coverage and supplemental benefits. The state actively seeks opportunities to maximize federal matching funds within its budgetary limitations. | Texas has demonstrated success in controlling Medicaid costs, but access to care remains a challenge, particularly for adults without dependent children. Health outcomes are generally comparable to national averages, but significant disparities exist based on geographic location and socioeconomic status. Preventative care rates lag behind those of California. |
| New York | New York’s program is characterized by comprehensive coverage, including a wide range of supplemental benefits and a strong emphasis on long-term care. The program utilizes a combination of managed care and fee-for-service delivery systems, tailored to specific needs. It also incorporates robust initiatives to address health disparities among vulnerable populations. | New York’s program is heavily funded by a combination of federal and state funds, with a substantial contribution from state taxes and dedicated healthcare revenue streams. The state’s commitment to robust funding allows for a broader range of benefits and services. | New York has achieved high rates of Medicaid enrollment and access to care. However, the program faces challenges in managing the high cost of long-term care and ensuring equitable access across diverse communities. Data shows high rates of access to specialist care, compared to Texas. |
Factors Contributing to Variations in Program Effectiveness
Variations in program effectiveness across states stem from a complex interplay of factors. These include differences in state-level political priorities, budgetary constraints, population demographics, and the specific design and implementation of individual programs. For example, states with higher tax revenues may be able to afford more comprehensive programs, while states with more restrictive eligibility criteria may experience lower costs but potentially reduced access to care.
Furthermore, the effectiveness of managed care models varies significantly depending on their implementation and oversight. Finally, the availability and distribution of healthcare providers significantly impacts access and quality of care across different states.
Illustrative Case Studies
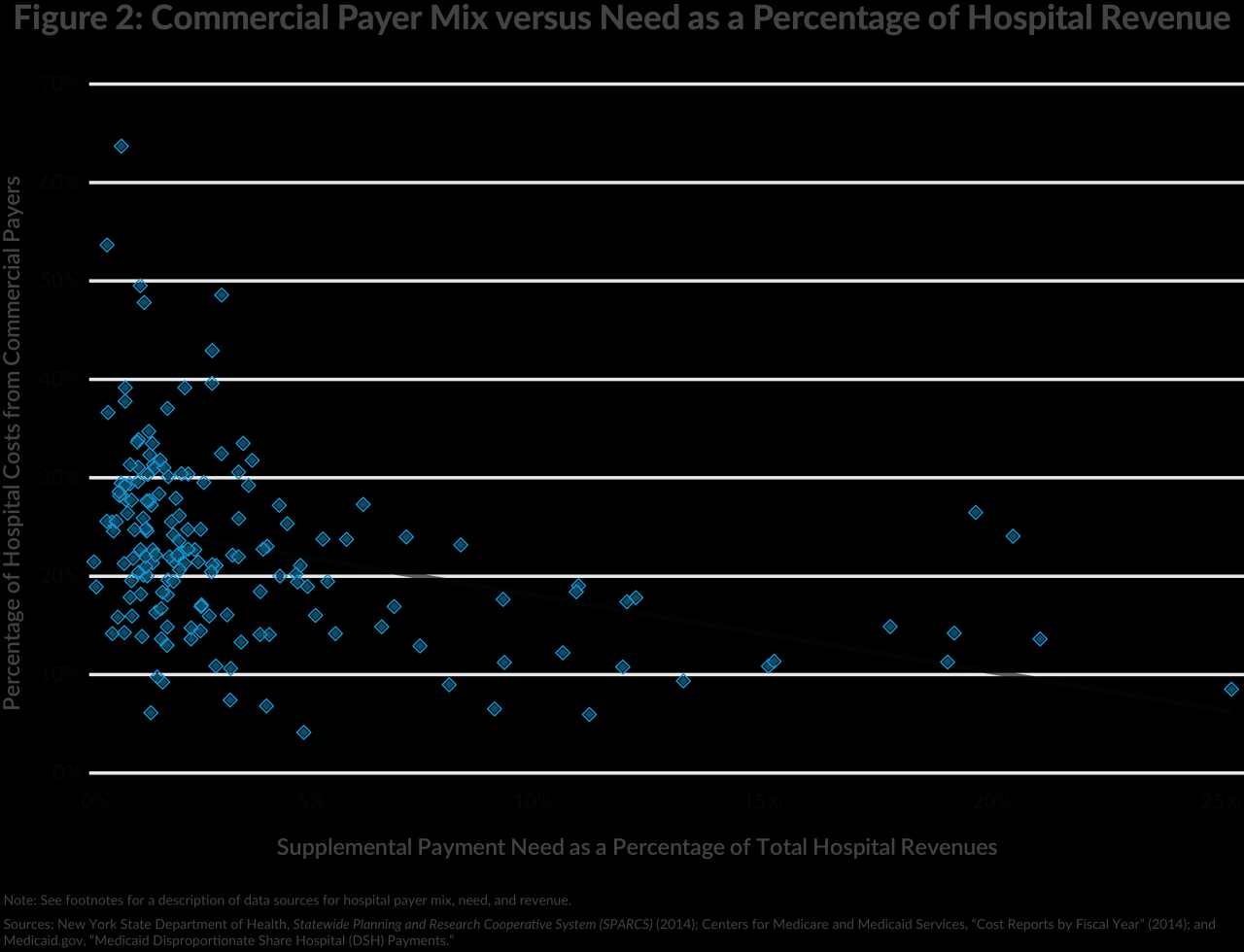
Source: cbcny.org
This section presents two case studies demonstrating the impact of Medicaid supplemental payments on healthcare organizations and patient populations. These examples highlight both the successes and challenges associated with these payments, offering valuable insights into their effectiveness and potential for improvement.
Case Study 1: Impact on Rural Hospital in Montana
This case study focuses on a small, rural hospital in Montana, “Big Sky Community Hospital” (BScH), which experienced significant financial strain due to a high percentage of Medicaid patients. Prior to the implementation of supplemental Medicaid payments, BScH faced potential closure due to unsustainable operating losses. The hospital primarily serves a low-income, aging population with high rates of chronic conditions.
The methodology involved analyzing BScH’s financial records for three years: one year prior to the supplemental payments, the year of implementation, and one year post-implementation. Key financial metrics, including operating margins, patient days, and revenue streams, were compared across these periods. The supplemental payments significantly improved BScH’s financial position, allowing the hospital to retain staff, invest in new equipment, and expand services.
While the supplemental payments did not entirely eliminate the hospital’s financial challenges, they provided crucial support, enabling continued operation and improved access to care for the community. The increased revenue allowed for staff retention bonuses and the implementation of a new telehealth program, further expanding access to care.
Challenges and Successes of BScH Case Study
The primary challenge was the initial complexity of navigating the application process for supplemental payments and ensuring compliance with all reporting requirements. Successes included improved financial stability, staff retention, and enhanced service offerings, ultimately resulting in improved patient outcomes. The hospital’s improved financial health allowed for investment in employee training and development, leading to better quality of care.
Key Findings and Implications of BScH Case Study
The supplemental Medicaid payments proved vital in preventing the closure of BScH, a critical healthcare provider in a rural, underserved area. The study demonstrates the significant impact these payments can have on the financial viability of rural hospitals and the access to care for vulnerable populations. This highlights the need for continued and potentially increased support for rural healthcare providers through supplemental Medicaid payments.
Analyzing health systems’ Medicaid supplemental payments for Q2 earnings, it’s fascinating to consider the long-term implications for healthcare costs. The recent news that the FDA approved clinical trials for pig kidney transplants in humans, as reported on this site , could significantly impact these payments down the line. If successful, this breakthrough could potentially reduce the strain on the system and, in turn, alter future Q2 earnings reports for health systems.
Case Study 2: Impact on Pediatric Asthma Management in California
This case study examines the effect of supplemental Medicaid payments on a pediatric asthma management program in a large urban area of California. The “Healthy Air for Kids” program (HAK) received supplemental funding to expand its reach and enhance its services. The program focused on providing comprehensive asthma care, including education, medication management, and access to specialized care for children enrolled in Medicaid.
The methodology involved a quasi-experimental design, comparing asthma-related hospitalizations and emergency room visits for children participating in the HAK program before and after the supplemental payments were implemented. Control groups were established using similar patient populations from neighboring counties without the expanded program. Data analysis involved comparing hospitalization and ER visit rates, controlling for factors such as age, gender, and pre-existing conditions.
Challenges and Successes of HAK Case Study, Health systems medicaid supplemental payments second quarter earnings
Challenges included enrolling sufficient numbers of Medicaid-eligible children and coordinating care between different healthcare providers. Successes included a statistically significant reduction in asthma-related hospitalizations and emergency room visits among children participating in the HAK program. This improvement suggests that the supplemental payments enabled the program to effectively deliver comprehensive asthma care, leading to better patient outcomes. Improved patient education and increased access to preventative care contributed significantly to the reduction in hospitalizations.
Key Findings and Implications of HAK Case Study
The supplemental Medicaid payments allowed the HAK program to significantly improve asthma management outcomes for Medicaid-eligible children. The study demonstrates the effectiveness of targeted interventions funded by supplemental payments in reducing healthcare utilization and improving patient health. This highlights the potential for similar programs to improve the overall health and well-being of vulnerable populations, emphasizing the importance of investing in preventative care and coordinated care models.
Closing Summary

Source: prokerala.com
Understanding the impact of Medicaid supplemental payments on second-quarter earnings is vital for policymakers, healthcare administrators, and anyone invested in the future of accessible and high-quality healthcare. The financial implications are significant, influencing both the sustainability of healthcare providers and the well-being of Medicaid beneficiaries. By analyzing trends, comparing state programs, and examining case studies, we can gain a clearer picture of the challenges and opportunities that lie ahead, paving the way for more effective and equitable healthcare systems.
FAQ Summary
What are the common reasons for variations in Medicaid supplemental payment amounts across states?
Variations stem from differences in state budgets, legislative priorities, the prevalence of specific health conditions within a state’s population, and the design of individual state Medicaid programs.
How do supplemental payments affect the recruitment and retention of healthcare professionals in underserved areas?
Supplemental payments can help attract and retain healthcare professionals to underserved areas by offering increased compensation, making these roles more financially attractive.
What are some potential risks associated with over-reliance on Medicaid supplemental payments for healthcare provider revenue?
Over-reliance creates vulnerability to budget cuts or policy changes that could significantly impact revenue and financial stability, potentially leading to service reductions or closures.





