Healthcare CFOs Automation, Service Line Cuts & BDO USA
Healthcare cfos automation service line cuts bdo usa – Healthcare CFOs: Automation, Service Line Cuts & BDO USA – it sounds like a financial thriller, doesn’t it? The truth is, it’s a reality for many healthcare organizations grappling with rising costs and evolving patient needs. This post dives into the complex intersection of automation, strategic service line cuts, and the crucial role BDO USA plays in helping healthcare systems navigate these turbulent waters.
We’ll explore how automation can be a lifeline, streamlining processes and offering data-driven insights to make tough decisions about resource allocation. Get ready for a deep dive into the financial heart of modern healthcare.
We’ll examine the challenges facing healthcare CFOs, from managing increasingly complex regulations to optimizing dwindling resources. We’ll then explore how automation tools, from robotic process automation (RPA) to advanced analytics, can offer solutions. The role of BDO USA, a leading advisory firm, in guiding healthcare organizations through service line optimization and financial restructuring will be a key focus.
We’ll uncover the strategies they employ and analyze real-world case studies to illustrate their impact. Ultimately, we’ll aim to understand how these seemingly disparate elements – automation, service line cuts, and expert consulting – can work together to create a more sustainable and efficient healthcare landscape.
Healthcare CFOs and Automation
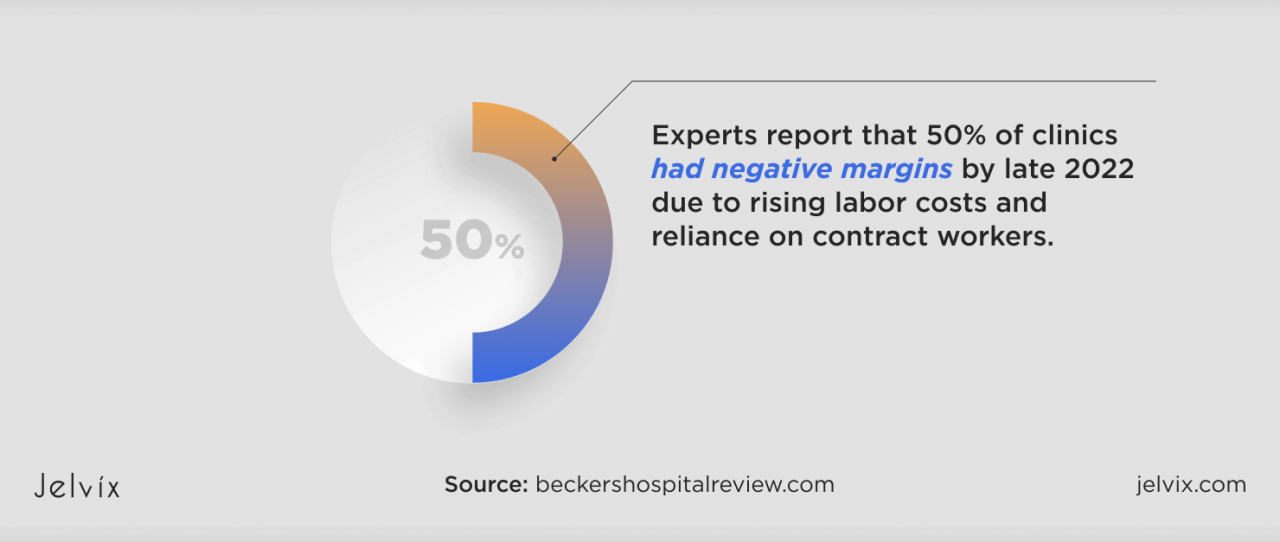
Source: jelvix.com
Healthcare CFOs are facing unprecedented challenges in today’s rapidly evolving landscape. Balancing rising costs, increasing regulatory burdens, and the need for improved patient care puts immense pressure on their financial management strategies. The sheer volume of data generated within a healthcare system, coupled with the complexity of reimbursement models and the need for accurate financial reporting, creates a perfect storm demanding innovative solutions.
Automation offers a powerful pathway to navigate these complexities and achieve greater efficiency.
Challenges Faced by Healthcare CFOs
Healthcare CFOs grapple with several key challenges. These include managing complex revenue cycles with multiple payers and intricate billing processes, ensuring regulatory compliance across a myriad of ever-changing rules and regulations (HIPAA, Medicare, Medicaid, etc.), accurately forecasting budgets and managing expenses in a volatile economic climate, and improving the accuracy and timeliness of financial reporting for internal and external stakeholders.
Data silos across different departments hinder efficient analysis, and a shortage of skilled financial professionals further exacerbates these difficulties. Legacy systems often lack the integration and functionality needed for streamlined operations, adding another layer of complexity.
Potential Benefits of Automation in Healthcare Finance
Automation offers significant benefits to healthcare finance departments. Automating repetitive tasks, such as data entry, invoice processing, and claims reconciliation, frees up valuable staff time for more strategic initiatives. This leads to increased efficiency and productivity, allowing for faster turnaround times and improved accuracy in financial reporting. Automation can significantly reduce manual errors, minimizing the risk of costly mistakes and improving the overall quality of financial data.
Advanced analytics powered by automated data collection and processing can provide valuable insights into operational efficiency, identify cost savings opportunities, and support more informed decision-making. Improved compliance through automated audit trails and data validation also reduces the risk of penalties and ensures adherence to regulations.
Comparison of Automation Solutions for Healthcare CFOs
Several automation solutions are available, each with its strengths and weaknesses. Robotic Process Automation (RPA) excels at automating repetitive, rule-based tasks, such as claims processing and data entry. Artificial Intelligence (AI) and Machine Learning (ML) offer more sophisticated capabilities, including predictive analytics for forecasting and fraud detection. Cloud-based solutions provide scalability and accessibility, while on-premise systems offer greater control over data security.
The optimal solution depends on the specific needs and resources of the healthcare organization. For example, a smaller hospital might benefit from a cloud-based RPA solution focusing on revenue cycle management, while a larger system might require a more comprehensive AI-powered platform integrating multiple financial processes.
Hypothetical Automation Strategy for a Medium-Sized Hospital System
A medium-sized hospital system could implement a phased automation strategy. Phase 1 would focus on automating high-volume, rule-based tasks within the revenue cycle, such as claims processing and payment posting using RPA. This would improve efficiency and reduce manual errors. Phase 2 would involve implementing AI-powered solutions for predictive analytics, enabling better budgeting and forecasting. This would allow for more proactive financial management and identification of potential risks.
Phase 3 could involve integrating these solutions with a cloud-based platform to enhance scalability and accessibility. This would ensure the system can adapt to future growth and changes in the healthcare landscape. Continuous monitoring and optimization are crucial throughout the process.
Return on Investment (ROI) of Automation Tools in Healthcare Finance
| Automation Tool | Implementation Cost | Annual Savings | ROI (Years) |
|---|---|---|---|
| RPA for Claims Processing | $50,000 | $25,000 | 2 |
| AI-powered Predictive Analytics | $100,000 | $50,000 | 2 |
| Cloud-based Financial Management System | $75,000 | $30,000 | 2.5 |
| Automated Accounts Payable | $25,000 | $15,000 | 1.67 |
Service Line Cuts and BDO USA’s Role

Source: medicalbillgurus.com
The healthcare industry is facing unprecedented pressure, forcing many organizations to make difficult decisions regarding service line cuts. Rising operational costs, declining reimbursements, and shifting patient demographics are all contributing factors that necessitate a thorough evaluation and potential restructuring of service offerings. BDO USA, with its deep expertise in healthcare finance and operations, plays a critical role in guiding these organizations through this complex process.Factors Contributing to Healthcare Service Line CutsSeveral interconnected factors drive the need for healthcare service line cuts.
Declining reimbursements from government and private payers often leave organizations with insufficient revenue to support all services. Simultaneously, rising operational costs, including labor, supplies, and technology, squeeze profit margins. Furthermore, shifts in patient demographics and healthcare utilization patterns necessitate a reevaluation of the demand for specific services. For example, an aging population may increase demand for geriatric care while decreasing the need for pediatric services in a specific geographic area.
Finally, increasing competition among healthcare providers forces organizations to strategically consolidate or eliminate less profitable service lines to maintain financial stability.BDO USA’s Assistance with Financial RestructuringBDO USA assists healthcare organizations undergoing financial restructuring through a multi-faceted approach. This involves a comprehensive financial assessment to identify areas of strength and weakness, followed by the development of a tailored restructuring plan.
This plan may include strategies such as cost reduction initiatives, revenue cycle optimization, and debt restructuring. BDO leverages its expertise in financial modeling and forecasting to project the impact of various restructuring scenarios, helping clients make informed decisions. They may also help negotiate with creditors and stakeholders to achieve favorable terms.Strategies for Service Line OptimizationBDO USA employs various strategies to help clients optimize their service lines.
These strategies often involve a detailed market analysis to identify areas of high demand and growth potential. This is followed by a comprehensive review of the organization’s current service offerings, evaluating their profitability, efficiency, and alignment with strategic goals. Based on this analysis, BDO may recommend streamlining operations, consolidating services, or divesting from underperforming areas. They also help clients develop robust performance metrics and reporting mechanisms to monitor the effectiveness of their optimization strategies.
This could include exploring opportunities for strategic partnerships or mergers to expand market reach or gain access to new technologies.Case Studies Demonstrating BDO USA’s ImpactWhile specific case studies from BDO USA are often confidential due to client sensitivities, the general impact of their consulting services can be observed through industry trends. For instance, BDO’s work often leads to improved operating margins for their clients, demonstrated through publicly available financial data from organizations that have disclosed such information.
Successful engagements typically show a reduction in operating expenses, improved revenue cycle management, and a more focused service line portfolio aligned with market demand. These improvements often translate to enhanced financial stability and long-term sustainability for the healthcare provider.Key Performance Indicators (KPIs) for Service Line OptimizationTo measure the success of service line optimization projects, BDO USA likely uses a range of KPIs.
BDO USA’s report on healthcare CFOs automating service lines got me thinking about resource allocation – and how that relates to individual needs. It made me wonder about the nutritional side of things; check out this fascinating article on how diets differ between the sexes: are women and men receptive of different types of food and game changing superfoods for women.
Understanding these differences might inform better healthcare resource management, particularly when considering preventative care strategies highlighted in the BDO report.
These KPIs can include:* Revenue growth: Increase in revenue generated from optimized service lines.
Operating margin Improvement in profitability of the service lines.
Patient volume Change in the number of patients served by the optimized service lines.
Patient satisfaction Assessment of patient experience with the optimized services.
Cost reduction Decrease in operational expenses associated with the service lines.
Return on investment (ROI) Measure of the financial return on investment in optimization initiatives.
Market share Change in the organization’s market share in the relevant service areas.
Healthcare CFOs are grappling with automation, service line cuts, and the fallout from BDO USA’s recent actions. These financial pressures are amplified by the shifting legal landscape, as evidenced by the Supreme Court’s decision to overturn the Chevron Doctrine, which impacts healthcare significantly, as detailed in this article: scotus overturns chevron doctrine healthcare. This ruling adds another layer of complexity for CFOs already navigating cost-cutting measures and technological advancements.
The Intersection of Automation and Service Line Optimization
Healthcare providers facing financial pressures are increasingly turning to service line optimization, a process that often involves difficult decisions about restructuring or eliminating underperforming services. Automation offers a powerful tool to navigate this complex landscape, improving efficiency and enabling data-driven decision-making throughout the process. By leveraging automation, healthcare organizations can streamline workflows, reduce costs, and ultimately improve the quality of care they deliver.
Areas Where Automation Improves Efficiency During Service Line Restructuring
Automating various aspects of service line restructuring can dramatically improve efficiency. For example, robotic process automation (RPA) can automate repetitive tasks such as data entry, claims processing, and appointment scheduling, freeing up staff to focus on more strategic initiatives. Automated reporting and analytics tools can provide real-time insights into service line performance, enabling quicker identification of areas needing attention.
Furthermore, AI-powered chatbots can handle routine patient inquiries, reducing the burden on administrative staff and improving patient satisfaction. These automation solutions collectively streamline operations, minimize manual errors, and accelerate the restructuring process.
Automation Facilitates Data Analysis for Informed Decision-Making in Service Line Cuts
Data analysis is crucial for making informed decisions during service line cuts. Automation plays a critical role here. Advanced analytics platforms, powered by machine learning, can sift through vast amounts of data – patient demographics, utilization rates, costs, and revenue – to identify trends and patterns that might be missed through manual analysis. This allows for a more objective and data-driven approach to identifying underperforming services or areas ripe for consolidation.
For example, predictive modeling can forecast the impact of potential service line cuts on patient volume and revenue, allowing for a more accurate assessment of the financial implications.
Cost and Benefit Analysis of Implementing Automation During Service Line Optimization
Implementing automation during service line optimization involves upfront costs for software, hardware, and training. However, the long-term benefits often outweigh these initial investments. Reduced labor costs, improved efficiency, minimized errors, and enhanced data-driven decision-making contribute to significant cost savings. For instance, a hospital might invest in an automated scheduling system, leading to reduced no-shows and improved resource allocation, resulting in a substantial return on investment over time.
A careful cost-benefit analysis, considering both short-term and long-term impacts, is essential before implementation. This analysis should include factors such as implementation costs, ongoing maintenance fees, staff training requirements, and the projected savings from increased efficiency and reduced errors.
Step-by-Step Process for Integrating Automation into Service Line Restructuring Projects
Integrating automation into service line restructuring requires a phased approach.
- Assessment and Planning: Identify areas ripe for automation, considering factors such as the volume of repetitive tasks, data availability, and the potential for cost savings.
- Technology Selection: Choose appropriate automation tools based on specific needs and budget constraints. This might involve RPA, AI-powered analytics platforms, or other relevant technologies.
- Implementation: Implement the chosen automation solutions, ensuring seamless integration with existing systems and workflows. This phase often involves careful planning, testing, and training.
- Monitoring and Optimization: Continuously monitor the performance of the automation solutions, making adjustments as needed to maximize efficiency and effectiveness.
- Evaluation: Regularly evaluate the impact of automation on key metrics such as cost savings, efficiency gains, and patient outcomes.
Potential Risks and Challenges Associated with Automating Service Line Optimization Processes
While automation offers numerous benefits, it also presents certain risks and challenges. The initial investment can be substantial, and there’s a risk of unforeseen technical issues or integration difficulties. Staff resistance to change is also a common hurdle. Data security and privacy concerns must be addressed carefully, particularly when dealing with sensitive patient information. Furthermore, the reliance on automation can lead to a lack of human oversight, potentially impacting the quality of care if not properly managed.
Reading about healthcare CFOs and automation-driven service line cuts at BDO USA got me thinking about the fragility of our health systems. It’s a stark reminder of how vital preventative care is, especially when you consider news like Monali Thakur’s hospitalization, as detailed in this article: monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases.
Ultimately, efficient healthcare finance is crucial, but it needs to support a system that prioritizes individual well-being and proactive health measures to avoid such crises.
Finally, the selection of inappropriate automation tools or a poorly planned implementation can lead to project failure. Therefore, a well-defined strategy, thorough planning, and careful consideration of potential risks are crucial for successful automation implementation.
Impact on Healthcare Delivery and Patient Care: Healthcare Cfos Automation Service Line Cuts Bdo Usa

Source: hubspot.com
Service line cuts, often driven by financial pressures and the implementation of automation, can significantly impact healthcare delivery and, ultimately, patient care. While automation offers potential for efficiency gains, poorly managed restructuring can lead to reduced access to care, longer wait times, and potentially compromised quality of care. Understanding these potential consequences and implementing mitigating strategies is crucial for healthcare organizations undergoing transformation.The reduction or elimination of specific service lines can directly limit patient access to specialized care.
For example, closing a dedicated cardiology unit might force patients to travel further for treatment, potentially delaying critical interventions. Similarly, cuts to mental health services could leave vulnerable populations without essential support. The impact is particularly acute for patients in rural or underserved communities with limited alternative options.
Access to Care and Service Line Reductions
Reduced access to care is a direct consequence of service line cuts. Patients may experience longer wait times for appointments, increased difficulty scheduling procedures, and potentially a decrease in the availability of specialized physicians or equipment. This is especially problematic for patients with chronic conditions requiring ongoing care or those facing urgent medical needs. For instance, a hospital system reducing its number of operating rooms might lead to significant delays in elective surgeries, impacting patient health and quality of life.
Similarly, the elimination of a specific diagnostic imaging service could lead to longer wait times for crucial tests, delaying diagnoses and treatments.
Automation’s Role in Mitigating Negative Effects on Patient Care
Automation can play a crucial role in mitigating the negative effects of service line cuts on patient care. Efficient appointment scheduling systems, electronic health records (EHRs) that streamline communication between providers, and telehealth platforms can improve access to care and reduce wait times. For example, a hospital implementing telehealth for routine follow-up appointments can free up in-person appointment slots for patients requiring more intensive care, even after reducing the number of physical clinics.
Furthermore, automated systems can improve the efficiency of administrative tasks, freeing up staff to focus on direct patient care.
Ensuring Patient Safety and Satisfaction During Service Line Changes
Maintaining patient safety and satisfaction during service line changes requires careful planning and execution. This includes thorough risk assessments, clear communication plans, and robust processes for transferring patients to alternative providers. For example, when a hospital closes a specific unit, a detailed plan must be in place to ensure seamless transfer of patient records and ongoing care to other facilities or providers.
This plan should also include mechanisms for ensuring that patients are aware of the changes and understand the implications for their care. Continuous monitoring of patient satisfaction scores and feedback mechanisms are essential to identify and address any emerging concerns.
Strategies to Maintain Quality of Care Despite Service Line Reductions
Maintaining quality of care during service line reductions requires a multi-faceted approach. This can involve optimizing existing resources, focusing on high-value care, and leveraging technology to improve efficiency. For instance, a hospital system might consolidate similar services into a single, more efficient location, reducing operational costs while maintaining or even improving the quality of care. Investing in staff training and development can also enhance the capabilities of the remaining workforce, ensuring that they are equipped to handle increased patient volume or more complex cases.
Prioritizing preventative care can reduce the need for more intensive services down the line, leading to better overall patient outcomes.
Communication Plan for Informing Patients About Changes
A clear and comprehensive communication plan is crucial for informing patients about changes resulting from service line cuts and automation. This plan should involve multiple channels, including direct mail, email, phone calls, and website updates. The messaging should be clear, concise, and empathetic, acknowledging the potential disruption to patients’ care. It is essential to provide patients with clear instructions on how to access alternative services, contact appropriate personnel, and understand the implications of the changes on their care.
Regular updates and opportunities for feedback should be incorporated to ensure that patients remain informed and their concerns are addressed promptly.
Future Trends and Predictions
The convergence of automation, data analytics, and evolving regulatory landscapes is reshaping the financial operations of healthcare organizations. Predicting the future with certainty is impossible, but by analyzing current trends and technological advancements, we can Artikel plausible scenarios for healthcare finance over the next decade. This will focus on automation’s impact, the challenges facing CFOs, and the role of emerging technologies in navigating this evolving landscape.
The healthcare finance sector is on the cusp of significant transformation. The increasing complexity of reimbursement models, coupled with the rising pressure to improve efficiency and reduce costs, is driving the adoption of automation technologies at an unprecedented rate. This adoption, however, presents both opportunities and challenges for healthcare CFOs.
Predictions for the Future of Automation in Healthcare Finance
The next five to ten years will witness a dramatic increase in the sophistication and pervasiveness of automation within healthcare finance. We can expect a shift from basic task automation to more intelligent systems capable of complex decision-making and predictive analytics. For example, robotic process automation (RPA) will handle routine tasks like invoice processing and claims submission with even greater efficiency, freeing up human resources for more strategic activities.
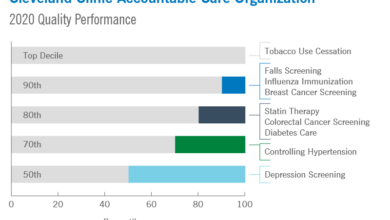
Simultaneously, the use of AI-powered tools for fraud detection and revenue cycle management will become increasingly common, leading to significant improvements in accuracy and efficiency. Hospitals like Cleveland Clinic are already leveraging AI for predictive modeling to optimize staffing and resource allocation, providing a glimpse into the future.
Future Challenges Facing Healthcare CFOs Regarding Service Line Optimization
Healthcare CFOs will face ongoing challenges in optimizing service lines, even with advanced automation. Data security and privacy will remain paramount, requiring robust cybersecurity measures and adherence to strict regulatory compliance standards like HIPAA. The integration of various automation tools and systems across different departments and healthcare systems will present significant IT challenges. Furthermore, the need to upskill and reskill the workforce to manage and utilize these new technologies will be a critical concern.
Maintaining the human element in healthcare, balancing automation with patient-centered care, will be another significant hurdle. The successful integration of automation will depend on thoughtful change management strategies and ongoing employee training.
The Role of Emerging Technologies in Healthcare Finance Automation
Artificial intelligence (AI) and machine learning (ML) will play a pivotal role in transforming healthcare finance. AI-powered systems will be able to analyze vast amounts of data to identify trends, predict future outcomes, and optimize financial processes. For instance, ML algorithms can analyze historical claims data to predict future revenue streams and identify potential areas of cost savings. Natural Language Processing (NLP) will improve the efficiency of tasks involving unstructured data, such as analyzing physician notes for coding accuracy.
The application of blockchain technology could enhance the security and transparency of healthcare transactions, streamlining payment processing and reducing fraud.
Timeline of Anticipated Developments in Healthcare Finance Automation (Next 5-10 Years)
The following timeline illustrates anticipated advancements, recognizing that the pace of technological adoption can vary across different healthcare organizations:
- Years 1-3: Widespread adoption of RPA for routine tasks; increased use of AI-powered tools for fraud detection and revenue cycle management; initial exploration of predictive analytics for resource allocation.
- Years 4-6: Integration of AI and ML into more complex financial decision-making processes; development of sophisticated predictive models for forecasting revenue and expenses; greater emphasis on data security and interoperability.
- Years 7-10: Ubiquitous use of AI-driven systems for financial planning and analysis; widespread adoption of blockchain technology for secure transactions; development of personalized financial management solutions for individual patients.
Potential Impact of Regulatory Changes on Automation and Service Line Decisions, Healthcare cfos automation service line cuts bdo usa
Regulatory changes, such as those related to data privacy and interoperability, will significantly impact the adoption and implementation of automation in healthcare. Compliance with regulations like HIPAA and the 21st Century Cures Act will necessitate robust data security measures and the development of compliant automation systems. Changes in reimbursement models will also influence service line optimization strategies, driving the need for advanced analytics and predictive modeling to adapt to evolving payment structures.
For example, value-based care models will require more sophisticated data analysis to track and measure outcomes, impacting the selection and implementation of automation tools.
Ending Remarks
Navigating the complex landscape of healthcare finance requires a strategic blend of technology and expert guidance. As we’ve explored, automation offers powerful tools to streamline processes and provide crucial data insights for healthcare CFOs facing difficult decisions about service line optimization. BDO USA’s role in this process is undeniable, providing the expertise to guide organizations through restructuring and ensure a path towards financial stability without compromising patient care.
The future of healthcare finance hinges on embracing technology and strategic partnerships to build a more resilient and efficient system. The journey may be challenging, but the potential rewards – improved financial health and enhanced patient care – make it a worthwhile endeavor.
Expert Answers
What are the biggest risks associated with automating service line optimization?
Potential risks include initial high implementation costs, integration challenges with existing systems, data security concerns, and the need for robust employee training to effectively utilize new technologies.
How does automation impact patient care during service line cuts?
While service line cuts can impact access, automation can help mitigate negative effects by streamlining processes, improving efficiency, and freeing up staff to focus on patient care. Careful planning and communication are crucial.
What types of automation solutions are best suited for healthcare CFOs?
This depends on specific needs, but solutions like RPA for repetitive tasks, predictive analytics for forecasting, and AI-powered tools for fraud detection are becoming increasingly popular.
Can automation completely replace human intervention in healthcare finance?
No. While automation streamlines many processes, human expertise remains crucial for strategic decision-making, complex problem-solving, and ensuring ethical considerations are addressed.