
Healthcare Worker Exodus Physician Burnout Definitive
Healthcare worker exodus physician burnout definitive: It’s a crisis unfolding before our eyes, a silent emergency threatening the very fabric of our healthcare system. We’re facing a mass exodus of physicians, fueled by crippling burnout, leaving patients stranded and the future of medicine uncertain. This isn’t just about numbers; it’s about the human cost – the exhausted doctors, the overwhelmed nurses, and the patients caught in the crossfire.
This post dives deep into the heart of the problem, exploring the causes, consequences, and potential solutions to this devastating trend.
From the sheer scale of the physician shortage and its geographical disparities to the specialties hardest hit, we’ll examine the contributing factors – excessive administrative burdens, inadequate compensation, and a relentless pressure cooker environment. We’ll also explore the devastating impact on patient care, the escalating healthcare costs, and the urgent need for systemic change. We’ll look at policy interventions, successful retention strategies, and the role of medical education reform in shaping a more sustainable future for healthcare professionals.
Defining the Healthcare Worker Exodus
The healthcare worker exodus, particularly among physicians, represents a significant and growing crisis impacting the accessibility and quality of healthcare globally. This mass departure from the profession is not merely a localized phenomenon but a widespread trend with profound implications for patients and healthcare systems alike. Understanding the scope and contributing factors is crucial to developing effective solutions.
The Scope and Scale of the Physician Shortage
The current physician shortage is substantial and varies considerably depending on specialty and geographic location. Estimates from the Association of American Medical Colleges (AAMC) project a shortfall of between 37,800 and 124,000 physicians by 2034 in the United States alone. This shortage is not limited to the US; many developed and developing nations are facing similar challenges, driven by factors ranging from aging populations and increased demand for care to burnout and unsustainable working conditions.
The healthcare worker exodus, fueled by physician burnout, is a definitive crisis. Finding solutions is crucial, and initiatives like the one detailed in this article, cms launches primary care medicare model aco , which aims to improve primary care access, might offer a piece of the puzzle. Ultimately, addressing burnout and improving working conditions are key to stemming the tide of departures and ensuring better patient care.
The sheer number of unfilled positions translates to longer wait times for appointments, reduced access to specialist care, and potentially compromised patient outcomes. For example, rural communities often experience a disproportionately higher physician shortage compared to urban areas, leading to significant healthcare disparities.
Geographical Variations in the Exodus
The geographical distribution of the physician shortage is uneven. Rural and underserved areas consistently experience the most significant deficits. These regions often face challenges in attracting and retaining physicians due to lower compensation, limited access to resources, and a lack of social support. Conversely, major metropolitan areas, while still experiencing shortages in certain specialties, generally have a more robust physician workforce, although even these areas are feeling the pressure of increased demand and burnout.
For instance, states like Mississippi and West Virginia consistently report higher rates of physician shortages compared to states like California and New York, despite population density differences. This disparity highlights the complex interplay of factors beyond simple population density.
Specialties Most Affected by the Exodus
The exodus isn’t uniform across all medical specialties. Primary care physicians, particularly family medicine and general internal medicine, are facing significant shortages. This is concerning because these physicians provide the foundation of healthcare, acting as gatekeepers to the system and addressing the majority of patient needs. However, shortages are also impacting specialized fields such as surgery, anesthesiology, and psychiatry.
The increasing complexity of medical practice, coupled with administrative burdens and malpractice concerns, contributes to the attrition in these high-demand specialties. For example, the rising rates of physician burnout in specialties like emergency medicine are directly linked to high patient volumes, long hours, and exposure to traumatic events.
Comparison to Historical Trends in Physician Workforce
While physician shortages have occurred periodically throughout history, the current situation presents a unique set of challenges. Past shortages were often related to specific events or localized factors. The current crisis, however, is characterized by a confluence of long-term systemic issues, including an aging physician population, increasing demand for care due to an aging global population, and unsustainable working conditions.
Furthermore, the rate of physician attrition is accelerating, exceeding the rate of new physician entry into the workforce in many regions. This unsustainable trend indicates a systemic failure to address the underlying causes of the exodus.
Contributing Factors to the Healthcare Worker Exodus
| Factor | Description | Impact | Example |
|---|---|---|---|
| Burnout and Stress | High workload, long hours, administrative burden, emotional toll | Reduced job satisfaction, increased turnover | A surgeon leaving practice due to chronic fatigue and emotional exhaustion. |
| Compensation and Benefits | Low salaries, inadequate insurance, lack of retirement benefits | Reduced incentive to enter or remain in the profession | A family physician choosing a higher-paying job outside of healthcare. |
| Administrative Burden | Excessive paperwork, electronic health record (EHR) issues, insurance complexities | Reduced time for patient care, increased frustration | A physician spending more time on documentation than patient interaction. |
| Work-Life Balance | Lack of flexibility, unpredictable schedules, limited time off | Decreased job satisfaction, difficulty in maintaining personal relationships | A pediatrician leaving the profession due to inability to balance work and family responsibilities. |
Physician Burnout
The exodus of healthcare workers is a multifaceted crisis, and physician burnout plays a significant role. Burnout, characterized by emotional exhaustion, depersonalization, and a reduced sense of personal accomplishment, is not simply a matter of individual resilience; it’s a systemic problem stemming from flawed working conditions and unsustainable demands within the healthcare system. Understanding its causes and consequences is crucial to addressing this critical issue.
Working Conditions and Burnout Rates
A strong correlation exists between challenging working conditions and high physician burnout rates. Long working hours, inadequate staffing levels, and excessive administrative burdens are consistently cited as major contributors. Studies have shown a direct link between increased patient loads and higher burnout scores, particularly in specialties with high acuity and demanding patient populations, such as emergency medicine and intensive care.
Similarly, hospitals with a culture of overwork and insufficient support systems tend to experience higher rates of physician attrition and burnout. The lack of control over one’s schedule, coupled with constant pressure to meet performance metrics, further exacerbates the problem.
The Impact of Administrative Burden on Physician Well-being
The ever-increasing administrative burden placed on physicians is a significant driver of burnout. Physicians spend a substantial portion of their workday on tasks unrelated to direct patient care, such as completing electronic health records (EHRs), dealing with insurance claims, and navigating complex regulatory requirements. This administrative burden detracts from time spent with patients, reduces job satisfaction, and contributes to feelings of frustration and inefficiency.
For instance, the time spent on EHR documentation often surpasses the time spent directly interacting with patients, leading to a sense of disconnect from the core purpose of their profession. This administrative overload is particularly detrimental to physicians’ mental health and contributes to feelings of being undervalued and overwhelmed.
Effective Stress Management Strategies for Physicians
Implementing effective stress management techniques is crucial for mitigating the effects of burnout. Mindfulness practices, such as meditation and deep breathing exercises, can help physicians manage stress and improve emotional regulation. Regular physical exercise, a balanced diet, and sufficient sleep are also vital components of a healthy lifestyle. Seeking support through peer networks, mentorship programs, or professional counseling can provide valuable emotional support and guidance.
Furthermore, establishing clear boundaries between work and personal life is essential to prevent burnout. Engaging in hobbies and activities outside of work helps maintain a sense of balance and perspective.
Strategies to Improve Work-Life Balance for Healthcare Professionals
Improving work-life balance for physicians requires a multi-pronged approach involving both individual and systemic changes. Hospitals and healthcare systems need to implement policies that promote reasonable working hours, adequate staffing levels, and reduced administrative burdens. This could include investing in technology to streamline administrative tasks, providing dedicated administrative support staff, and promoting a culture that values work-life integration.
Physicians themselves can actively prioritize their well-being by setting boundaries, delegating tasks when possible, and utilizing available resources such as wellness programs. Flexible work arrangements, such as compressed workweeks or telecommuting options where appropriate, can also help improve work-life balance.
Common Symptoms of Physician Burnout
Physician burnout manifests in various ways, both physically and emotionally. Common symptoms include persistent fatigue and exhaustion, cynicism and detachment from work, feelings of inefficacy and low self-esteem, increased irritability and impatience, difficulty concentrating, physical ailments such as headaches and gastrointestinal problems, and substance abuse. These symptoms often accumulate over time, gradually impacting not only the physician’s well-being but also their ability to provide quality patient care.
Early recognition of these symptoms is crucial for effective intervention and prevention of more severe consequences.
Financial Implications of the Exodus: Healthcare Worker Exodus Physician Burnout Definitive
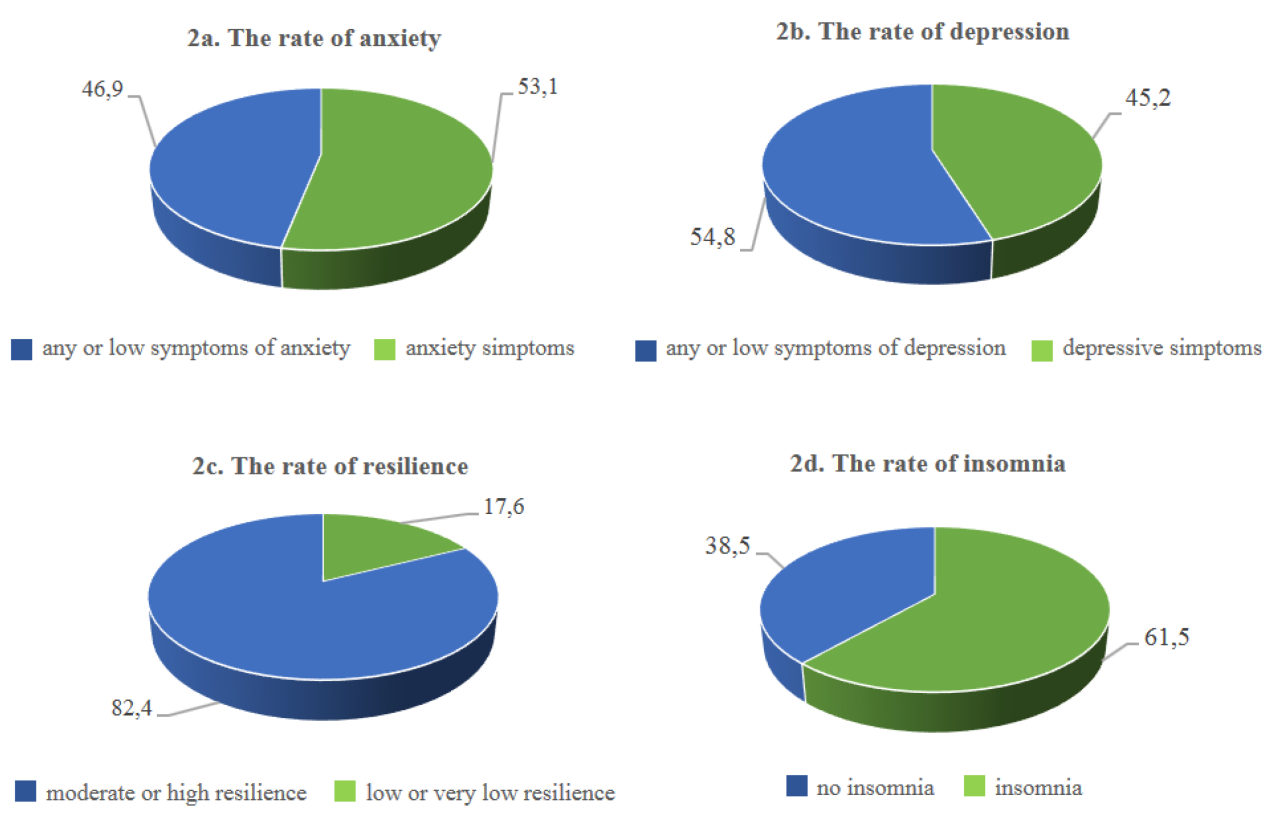
Source: mdpi-res.com
The mass exodus of healthcare workers, particularly physicians, isn’t just a human resources crisis; it’s a significant economic catastrophe with far-reaching consequences for healthcare systems, patients, and the overall economy. The financial implications are multifaceted and demand immediate attention, impacting everything from hospital budgets to patient access and the quality of care delivered.The economic consequences of physician shortages are severe and multifaceted.
Reduced physician availability directly translates to decreased hospital revenue, as fewer procedures are performed and fewer patients are seen. This impacts not only hospital profitability but also their ability to invest in infrastructure upgrades, new technologies, and staff training. Furthermore, the need to recruit and retain physicians through higher salaries and signing bonuses places a considerable strain on already stretched healthcare budgets.
Economic Consequences for Healthcare Systems
Physician shortages lead to a domino effect of financial challenges for healthcare systems. Hospitals and clinics face increased costs associated with recruitment and retention, including higher salaries, relocation packages, and signing bonuses to attract qualified physicians. Simultaneously, they experience decreased revenue due to reduced patient volume and a potential increase in malpractice insurance premiums, given the increased workload on remaining physicians.
This financial strain can limit investment in crucial areas like medical equipment upgrades, research, and employee development. For example, a rural hospital struggling to attract family doctors might have to curtail services or even face closure, leading to substantial economic losses for the entire community.
Impact on Patient Access and Quality of Care
The shortage of physicians directly impacts patient access to care. Longer wait times for appointments, limited availability of specialists, and potential delays in receiving necessary treatments are all common consequences. This reduced access disproportionately affects vulnerable populations, including the elderly, low-income individuals, and those living in rural or underserved areas. Furthermore, the increased workload on remaining physicians can negatively impact the quality of care.
Physician burnout, stemming from excessive hours and administrative burdens, can lead to decreased diagnostic accuracy, increased medical errors, and a decline in patient satisfaction. A study published in the
Journal of the American Medical Association* showed a direct correlation between physician burnout and increased medical errors.
Effect of Physician Burnout and Turnover on Healthcare Costs
Physician burnout and high turnover rates significantly contribute to increased healthcare costs. The costs associated with recruiting and training new physicians far exceed the costs of retaining experienced ones. Additionally, the indirect costs of burnout, including medical errors, increased hospital readmissions, and decreased patient satisfaction, add to the financial burden. For instance, a single medical error resulting from physician fatigue can lead to substantial costs associated with legal fees, additional treatment, and potential loss of patient trust.
The cumulative effect of these costs across numerous healthcare institutions is substantial.
Financial Incentives and Disincentives for Physicians
The current healthcare landscape presents a complex interplay of financial incentives and disincentives for physicians. High salaries and lucrative specialization opportunities are strong incentives, but these are often counterbalanced by the increasing administrative burden, high malpractice insurance premiums, and the emotional toll of burnout. The significant student loan debt many physicians carry also contributes to financial strain, making it challenging to maintain a healthy work-life balance and potentially discouraging younger generations from entering the profession.
Conversely, initiatives such as loan forgiveness programs and increased government funding for medical education could serve as significant incentives.
Potential Cost-Saving Measures
Addressing the physician exodus requires a multifaceted approach involving cost-saving measures. These measures should focus on both attracting new physicians and retaining existing ones.
- Investing in robust physician wellness programs to reduce burnout and improve job satisfaction.
- Reducing administrative burdens on physicians through streamlined processes and electronic health record (EHR) optimization.
- Implementing innovative models of care, such as telehealth and team-based care, to improve efficiency and reduce workload.
- Increasing government funding for medical education and residency programs to expand the physician workforce.
- Offering loan forgiveness programs and other financial incentives to attract and retain physicians, particularly in underserved areas.
- Promoting work-life balance initiatives to enhance physician well-being and reduce turnover.
Policy and Systemic Responses

Source: m3.com
The healthcare worker exodus and physician burnout crisis demand comprehensive policy interventions and systemic changes. Addressing this requires a multi-pronged approach focusing on improving working conditions, reforming medical education, and leveraging technological advancements. Simply put, we need to make being a doctor less stressful and more rewarding.
Policy Interventions to Address Physician Burnout, Healthcare worker exodus physician burnout definitive
Effective policy interventions must target the root causes of burnout, including excessive administrative burden, long working hours, and inadequate compensation. One key strategy is to implement policies that limit administrative tasks and streamline billing processes. This could involve leveraging technology to automate administrative functions and reducing the reliance on outdated paper-based systems. Additionally, policies promoting fair compensation and benefits packages, including paid time off and mental health support, are crucial for attracting and retaining physicians.
Finally, implementing stricter regulations on physician work hours and promoting a culture of work-life balance are essential steps. These changes aren’t just about improving the lives of doctors; they directly impact patient care by preventing burnout-related errors and ensuring a more engaged and effective workforce.
Examples of Successful Initiatives to Improve Physician Retention
Several successful initiatives demonstrate the positive impact of targeted interventions. For example, the Mayo Clinic’s focus on physician well-being has included programs promoting mindfulness, stress management, and access to mental health services. This proactive approach has led to improved physician satisfaction and reduced burnout rates. Similarly, some hospitals have successfully implemented shared decision-making models, empowering physicians to participate in policy decisions affecting their work environment.
The healthcare worker exodus and physician burnout are definitive crises, impacting patient care and system stability. Understanding the financial pressures on major players like Elevance Health is crucial; check out their Q1 earnings report and the impact of their recent cyberattack on Medicaid and Medicare Advantage programs here. These financial strains ultimately contribute to the underlying issues fueling burnout and the ongoing exodus of healthcare professionals.
This increased autonomy has fostered a sense of ownership and improved job satisfaction. These initiatives highlight the importance of a holistic approach that considers both the professional and personal well-being of physicians.
The Role of Medical Education Reform in Mitigating the Exodus
Medical education reform plays a vital role in mitigating the exodus. Curriculum changes should prioritize teaching resilience, stress management techniques, and effective communication skills. Furthermore, integrating interprofessional education and collaborative practice models can foster a more supportive and collaborative work environment, reducing feelings of isolation and overwhelm often associated with burnout. By equipping future physicians with the necessary coping mechanisms and collaborative skills, medical schools can contribute significantly to reducing burnout and improving physician retention.
This preventative approach addresses the problem at its source, cultivating a healthier and more sustainable medical workforce.
Regulatory Changes to Improve the Work Environment
Regulatory changes can significantly improve the work environment for physicians. Strengthening regulations regarding physician work hours, particularly reducing the number of on-call shifts and ensuring adequate rest periods, is crucial. Similarly, implementing stricter regulations on administrative burdens, including simplifying billing processes and reducing unnecessary paperwork, can free up physicians’ time to focus on patient care. Finally, creating regulatory frameworks that promote fair compensation and protect physicians from harassment and discrimination contribute to a more supportive and respectful work environment.
These regulatory interventions create a system that values physicians’ well-being and fosters a more sustainable medical workforce.
The Potential Impact of Telehealth on Addressing the Shortage
Telehealth offers significant potential for addressing the physician shortage and mitigating burnout. By expanding access to care in underserved areas and providing alternative care models, telehealth can reduce the pressure on existing physicians. Furthermore, telehealth can facilitate remote consultations and monitoring, reducing the need for in-person visits and freeing up physicians’ time for more complex cases. However, successful implementation of telehealth requires addressing issues such as equitable access to technology, reimbursement policies, and regulatory frameworks.
If implemented effectively, telehealth can become a valuable tool in both alleviating the physician shortage and improving the work-life balance of existing physicians, reducing burnout.
The Patient Perspective
The healthcare worker exodus and physician burnout are not abstract problems; they have a very real and often devastating impact on patients. The consequences ripple outwards, affecting access to care, the quality of treatment, and ultimately, patient health outcomes. Understanding the patient perspective is crucial for addressing this multifaceted crisis.
The shortage of healthcare professionals translates directly into a diminished patient experience. Longer wait times for appointments, difficulty accessing specialists, and a general feeling of being rushed during consultations are becoming increasingly common. This erosion of trust and the feeling of being undervalued can significantly impact a patient’s overall well-being, adding further stress to already challenging health situations.
Impact of Physician Shortages on Patient Experience and Satisfaction
Reduced access to timely and quality care is a direct result of physician shortages. Patients face longer wait times for appointments, potentially delaying diagnosis and treatment for serious conditions. This can lead to increased anxiety, frustration, and a decline in overall satisfaction with the healthcare system. The feeling of being rushed during consultations, a common consequence of physician burnout and high patient loads, further diminishes the patient experience, leaving individuals feeling unheard and undervalued.
Examples of Patient Impact from Long Wait Times and Limited Access
Many patients report significant delays in receiving necessary care. For example, a patient with a suspected heart condition might experience weeks-long delays in getting a cardiologist appointment, increasing the risk of complications. Similarly, patients with chronic conditions might struggle to secure regular check-ups, leading to worsening symptoms and potential health crises. The inability to access specialized care, due to a shortage of specialists, can also force patients to travel long distances or rely on less qualified providers.
Consequences of Physician Burnout on the Quality of Patient Care
Physician burnout significantly compromises the quality of patient care. Exhausted and stressed physicians are more prone to making errors, overlooking crucial details, and providing less empathetic and effective care. The emotional toll of burnout can manifest in reduced communication, leading to misunderstandings and a lack of trust between doctor and patient. This negatively impacts treatment adherence and overall patient outcomes.
The healthcare worker exodus and physician burnout are definitive crises, impacting patient care across the board. This is further underscored by the recent news that Kaiser Permanente nixes 500m Seattle bed tower capital spending , a decision likely influenced by staffing shortages and escalating operational costs. Ultimately, this highlights the urgent need to address the root causes of burnout to prevent further deterioration of our healthcare system.
Stories Illustrating the Impact of Physician Shortages on Patient Health Outcomes
My mother waited three months to see a specialist for her persistent back pain. By the time she finally got an appointment, the condition had significantly worsened, requiring more extensive and invasive treatment than would have been necessary with timely intervention. The delay caused her immense suffering and added considerable financial burden.
I had to wait over six weeks to get an appointment with my primary care physician for a routine check-up. By the time I saw him, I was already experiencing symptoms of a urinary tract infection that could have been easily treated earlier if I had access to a timely appointment. The delay meant I suffered unnecessarily and required a stronger course of antibiotics.
Visual Representation of the Patient’s Perspective
Imagine a crowded emergency room, overflowing with patients on stretchers and in waiting chairs. The scene is chaotic and stressful, with overworked nurses rushing between patients and a visibly exhausted physician trying to attend to everyone. The image depicts a feeling of helplessness and vulnerability, with patients looking anxious and frustrated. The colors are muted and somber, reflecting the stress and anxiety of the situation.
A single, brightly lit figure of a physician, barely visible in the background, symbolizes the overwhelming shortage of healthcare workers and the immense pressure they face. The overall impression is one of overwhelming demand and insufficient resources, leaving patients feeling neglected and at risk.
End of Discussion
The healthcare worker exodus and physician burnout are not merely isolated problems; they are interconnected crises demanding immediate and comprehensive solutions. Ignoring this issue will have far-reaching and devastating consequences for both healthcare professionals and the patients they serve. While the challenges are significant, there’s hope. By addressing systemic issues, promoting physician well-being, and implementing innovative strategies, we can begin to stem the tide of this exodus and create a healthcare system that values and supports its most precious resource: its people.
The future of healthcare depends on it.
Quick FAQs
What are some common signs of physician burnout that patients might observe?
Patients might notice increased wait times, rushed appointments, less personalized care, or a seeming lack of empathy from their physician. Changes in demeanor, like increased irritability or detachment, can also be indicators.
How does physician burnout affect medical innovation and advancements?
Burnout can significantly hamper medical innovation. Exhausted physicians have less time and energy for research, professional development, and staying abreast of the latest medical advancements, ultimately slowing progress in healthcare.
Are there specific support systems available for physicians struggling with burnout?
Yes, many organizations offer peer support groups, mentorship programs, and access to mental health professionals specifically trained to address the unique challenges faced by healthcare workers. Many hospitals and medical practices are also beginning to implement wellness programs.
