HHS Offers Flexibilities Medicaid Redeterminations
HHS offers flexibilities Medicaid redeterminations – that’s a mouthful, right? But it’s huge news for millions of Americans relying on Medicaid. This means the federal government is giving states some wiggle room in how they handle the process of checking if people still qualify for the program. This post dives into what these changes mean, both for states and the individuals who depend on Medicaid for their healthcare.
We’ll explore the new flexibilities, look at how different states are implementing them, and discuss the potential impacts – both positive and negative – on Medicaid beneficiaries. Get ready to unpack this complex topic in a way that’s both informative and easy to understand.
HHS Medicaid Redetermination Flexibilities

Source: army.mil
The COVID-19 pandemic significantly impacted the administration of Medicaid, leading to a continuous enrollment period and a pause on redeterminations. As the public health emergency ended, the Centers for Medicare & Medicaid Services (CMS), under the Department of Health and Human Services (HHS), implemented a phased approach to resuming eligibility renewals, offering states considerable flexibility in the process. This approach aimed to balance the need to ensure accurate enrollment with minimizing disruptions to coverage for eligible individuals.The HHS provided states with several key flexibilities regarding Medicaid redeterminations.
These flexibilities were designed to help states manage the large volume of renewals efficiently and effectively, while minimizing potential disruptions to beneficiary coverage. The flexibilities offered included extended timelines for completing redeterminations, allowing for streamlined renewal processes, and providing opportunities for states to utilize technology and innovative approaches to improve efficiency. These changes significantly altered the traditional Medicaid renewal process, providing states with greater autonomy in managing their programs.
Medicaid Redetermination Flexibility Details
States were granted extended timelines to complete redeterminations, allowing them more time to process applications and verify eligibility information. This was particularly crucial given the anticipated surge in cases needing review after the continuous enrollment period ended. Furthermore, simplified renewal processes were permitted, allowing states to use less complex methods for verifying eligibility, such as self-attestation in certain circumstances.
This helped expedite the renewal process and reduce the administrative burden on both state agencies and beneficiaries. The use of technology, including online portals and automated systems, was also encouraged to streamline the process and improve efficiency. These combined flexibilities aimed to balance the need for accurate eligibility determination with the importance of minimizing coverage disruptions for eligible individuals.
Timeline of Key Policy Announcements and Implementation
The timeline for implementing these flexibilities involved several key announcements and phases. Initially, the continuous enrollment period, preventing most Medicaid disenrollments, was extended throughout the COVID-19 public health emergency. Following the end of the public health emergency, CMS issued guidance outlining the permitted flexibilities for states to implement during the unwinding process. Specific dates for the implementation of these flexibilities varied by state, depending on their individual circumstances and administrative capabilities.
However, a general timeframe saw states begin the process of redeterminations in early 2023, with a phased approach extending through the end of 2024. The exact dates and phases were subject to continuous updates and guidance from CMS, reflecting the dynamic nature of the situation and the need for ongoing adjustments. This flexible approach allowed states to adapt their strategies based on their specific needs and resources.
Impact on State Medicaid Agencies
The recent HHS flexibilities regarding Medicaid redeterminations have presented significant challenges and opportunities for state Medicaid agencies. The sheer volume of redeterminations, coupled with the complexities of navigating new eligibility criteria and technological hurdles, has created a demanding operational environment. States are grappling with adapting their existing systems and workflows to accommodate these changes, leading to diverse implementation strategies depending on their resources and capabilities.State Medicaid agencies are facing a multitude of challenges in implementing the new flexibilities.
These include staffing shortages, needing to update outdated technology, managing increased workload, and ensuring accurate and timely processing of redeterminations to avoid disrupting coverage for eligible beneficiaries. The need for extensive outreach and communication efforts to inform beneficiaries of their responsibilities also adds a significant layer of complexity. Furthermore, ensuring compliance with federal guidelines while maintaining operational efficiency is a constant balancing act.
State Adaptation Strategies
Different states have employed various strategies to adapt their processes. Some states have invested heavily in technological upgrades, implementing new automated systems to streamline the redetermination process. Others have focused on improving their internal workflows and training staff on the new procedures. Some states have opted for a phased approach, prioritizing redeterminations for certain populations, while others have undertaken a more comprehensive, simultaneous approach.
These diverse approaches reflect the unique contexts and resources available to each state.
Resource and Technological Impacts on Implementation
States with greater resources and advanced technological capabilities have generally been able to implement the new flexibilities more smoothly. These states have often been able to invest in sophisticated case management systems and automated processes, reducing manual effort and improving efficiency. In contrast, states with fewer resources have faced greater challenges, often relying on manual processes and requiring more staff time to complete redeterminations.
This disparity highlights the need for federal support to ensure equitable implementation across all states.
| State | Approach | Challenges Faced | Outcomes |
|---|---|---|---|
| California | Phased approach, focusing on technological upgrades and outreach campaigns. | Maintaining sufficient staffing levels, managing high caseloads, ensuring timely processing. | Improved efficiency in later phases, but initial delays experienced. Significant outreach success. |
| Texas | Comprehensive, simultaneous approach with a focus on streamlining internal workflows. | Significant increase in workload, challenges with outdated technology, maintaining accuracy. | High volume of redeterminations processed, but higher error rates initially. |
| Vermont | Focused on proactive outreach and simplified application processes. | Limited resources, reliance on manual processes, challenges in reaching rural populations. | Slower processing speed, but higher beneficiary retention rate due to effective outreach. |
Impact on Medicaid Beneficiaries
The recent flexibilities offered by HHS regarding Medicaid redeterminations have significant implications for millions of beneficiaries across the United States. These changes, while intended to streamline the process and improve efficiency, could have both positive and negative consequences for those relying on Medicaid for healthcare access. Understanding these potential impacts is crucial for ensuring equitable access to vital medical services.The flexibilities aim to simplify the renewal process, potentially reducing administrative burdens on both state agencies and beneficiaries.
The HHS flexibilities for Medicaid redeterminations are a big deal, impacting millions. It’s interesting to consider this alongside the healthcare industry’s tech investments, like the recent news about Mass General Brigham’s buyout of a digital unit, as described in this article: Mass General Brigham Buyouts Digital Unit. These kinds of strategic moves highlight how healthcare providers are adapting to changing landscapes, and the Medicaid changes add another layer of complexity to their operational planning.
However, the effects on enrollment and access to care are complex and multifaceted, varying significantly depending on individual circumstances and state-level implementation.
Medicaid Enrollment and Access to Care
These flexibilities could lead to both increased and decreased Medicaid enrollment, depending on how states choose to implement them. Streamlined processes might make it easier for eligible individuals to remain enrolled, preventing unnecessary disenrollments. Conversely, simplified processes might also inadvertently lead to the disenrollment of eligible individuals who fail to meet new, less stringent documentation requirements, or who lack the resources to navigate the system.
The net effect on enrollment remains uncertain and will likely vary widely across states. Access to care could be affected similarly. Improved efficiency might lead to faster processing times and reduced administrative delays, improving access for those who remain enrolled. However, increased disenrollments could result in significant gaps in care for those who lose coverage.
Benefits and Drawbacks for Beneficiaries
Potential benefits include a smoother, less bureaucratic renewal process, reducing stress and time commitment for beneficiaries. Faster processing times could mean quicker access to needed care, preventing potential health complications from delayed treatment. However, drawbacks include the risk of unintended disenrollments, leading to loss of coverage and potential financial hardship. The simplified processes might not adequately address the unique needs of vulnerable populations, leading to disproportionate negative impacts on certain groups.
For example, those with limited digital literacy or those facing language barriers may struggle to navigate the new system, even if it is intended to be simpler.
Impact on Vulnerable Populations
The elderly, disabled, and children are particularly vulnerable to the effects of these changes. The elderly may face challenges understanding and navigating the new system, potentially leading to disenrollment. Individuals with disabilities may require more extensive documentation and support, which could be overlooked in a simplified process. Children, often reliant on their parents or guardians for enrollment, are at risk if their families struggle to meet the new requirements.
States must proactively address the unique needs of these populations through outreach and support services to minimize negative impacts.
Hypothetical Scenario
Imagine Maria, a 68-year-old woman with diabetes and limited English proficiency. Under the new flexibilities, her Medicaid renewal is handled through an online portal. While the intention is to simplify the process, Maria struggles to navigate the website and complete the necessary forms. Lacking digital literacy and support, she fails to submit the required documentation on time, leading to her disenrollment.
This results in a gap in her medication and access to crucial diabetes management services, potentially leading to serious health consequences. This scenario highlights the potential for unintended negative consequences for vulnerable populations even with simplified processes.
Data and Reporting Requirements
The increased flexibility granted to states regarding Medicaid redeterminations necessitates robust data collection and reporting to ensure accountability and transparency. This data is crucial for evaluating the effectiveness of the flexibilities in achieving their intended goals, such as minimizing disruptions to coverage and maintaining program integrity. Without rigorous data tracking, it would be impossible to assess the impact of these changes on both state agencies and Medicaid beneficiaries.The enhanced data requirements aim to provide a comprehensive picture of the redetermination process under the flexibilities.
This allows for both real-time monitoring and post-implementation analysis, informing future policy decisions and resource allocation. The data collected will also aid in identifying areas where improvements are needed, ensuring the program remains efficient and effective.
Key Metrics for State Reporting
States are required to track and report a range of key metrics to provide a holistic view of the redetermination process. These metrics fall broadly into categories assessing the efficiency of the process, the impact on beneficiary coverage, and the overall cost implications. This comprehensive data collection enables a thorough evaluation of the program’s performance under the new flexibilities.
- Number of redeterminations completed: This provides a baseline measure of the program’s throughput and identifies potential bottlenecks in the process.
- Number of individuals losing coverage: This metric directly assesses the impact of redeterminations on beneficiary access to healthcare.
- Number of individuals maintaining coverage: This metric complements the previous one, showing the success rate of retaining eligible beneficiaries.
- Average processing time per redetermination: This metric helps identify areas for process improvement and efficiency gains.
- Number of appeals filed and outcomes: This provides insights into the fairness and transparency of the redetermination process.
- State administrative costs associated with redeterminations: This allows for cost-benefit analysis of the flexibilities.
- Changes in Medicaid enrollment: This metric provides a broad overview of the overall impact on the Medicaid program.
Data Visualization for Effective Assessment, HHS offers flexibilities Medicaid redeterminations
Effective data visualization is essential for understanding the complex data generated by Medicaid redeterminations. Visual representations allow for quick identification of trends and patterns, facilitating informed decision-making. Several visualization techniques can effectively showcase the collected data.
- Bar chart showing the number of redeterminations completed per month: The x-axis would represent the months, and the y-axis would represent the number of redeterminations. This visualization would clearly illustrate monthly variations in processing volume, revealing potential seasonal effects or bottlenecks.
- Line graph illustrating the number of individuals losing coverage over time: The x-axis would represent time (months or quarters), and the y-axis would represent the number of individuals losing coverage. This visualization would highlight trends in coverage loss, allowing for the identification of periods requiring intervention or further investigation.
- Pie chart showing the proportion of individuals maintaining coverage versus losing coverage: This visualization would provide a clear and concise overview of the overall success rate of maintaining beneficiary coverage under the redetermination process.
- Scatter plot comparing processing time against the number of appeals filed: The x-axis would represent the processing time, and the y-axis would represent the number of appeals filed. This visualization would help identify any correlation between processing time and the number of appeals, potentially revealing areas where improvements could reduce appeals.
Future Implications and Considerations
The recent flexibilities granted to state Medicaid agencies regarding redeterminations have significant long-term implications for the program’s financial stability, administrative efficiency, and, most importantly, the health and well-being of millions of beneficiaries. Understanding these implications and proactively addressing potential challenges is crucial for ensuring the continued success of Medicaid in supporting vulnerable populations. Early implementation data will be key to shaping future policy and resource allocation.The impact of these flexibilities will unfold over time, influenced by factors such as state-level implementation strategies, economic conditions, and the evolving needs of the Medicaid population.
For example, the extended timeframe for redeterminations might initially reduce administrative burden, but could also lead to a delayed identification of individuals who no longer qualify, potentially resulting in increased program costs in the long run. Conversely, streamlined processes could lead to significant cost savings if effectively implemented. A thorough analysis of these competing effects is essential.
Long-Term Impacts on Medicaid Program Finances
The financial implications are multifaceted. While initial cost savings from reduced administrative overhead are possible, the delayed disenrollment of ineligible individuals could lead to increased expenditures. This risk is particularly pronounced if the economy deteriorates, leading to increased enrollment and a higher proportion of individuals who might lose eligibility if their circumstances changed. Conversely, more efficient processes could free up resources for other vital Medicaid programs.
Careful monitoring of both expenditure and enrollment data will be critical for assessing the true financial impact. For instance, states that successfully implement simplified online applications and verification processes may see significant cost savings compared to states that rely on more traditional, paper-based methods.
The HHS flexibility on Medicaid redeterminations is a big deal, especially considering the strain on healthcare systems. This is particularly relevant when you consider the challenges faced by rural hospitals, many of which are struggling to maintain essential services like labor and delivery, as highlighted in this insightful article on Rural Hospitals Labor Delivery &. Easing the Medicaid process could help alleviate some financial pressures, ultimately improving access to care in these already vulnerable communities.
The HHS changes could be a game-changer for rural healthcare access.
Policy Adjustments Based on Early Implementation
Early data analysis should focus on identifying bottlenecks and areas for improvement in the redetermination process. For example, if a particular state experiences significant delays in processing applications due to technical issues with their online portal, adjustments to the system or additional training for staff may be necessary. States should also track the number of successful and unsuccessful redeterminations, identifying any patterns or trends that might indicate areas needing refinement.
Regular feedback mechanisms with beneficiaries and providers will be crucial for identifying and addressing challenges early on. This feedback could reveal issues such as difficulty in navigating online portals or confusion regarding documentation requirements.
Areas for Further Research and Analysis
Further research should investigate the impact of these flexibilities on health outcomes for beneficiaries. Studies could compare health care utilization and health status indicators among beneficiaries who experienced streamlined redeterminations versus those who faced delays or difficulties. The impact on access to care, particularly for vulnerable populations, also warrants investigation. For example, research could examine whether certain demographic groups disproportionately experience challenges during the redetermination process.
The HHS flexibilities for Medicaid redeterminations are a huge help, streamlining the process for millions. This is especially important given the increasing complexity of healthcare administration, and tools like those described in this article on nuance integrates generative ai scribe epic ehrs could further improve efficiency. Ultimately, these technological advancements and administrative changes aim to ensure individuals maintain access to crucial healthcare coverage.
This research should also assess the impact on providers, analyzing the administrative burden associated with the changes and their effects on provider reimbursements.
Policy Recommendations for Optimizing Flexibilities
The effective use of these flexibilities requires a proactive and data-driven approach. Here are some key policy recommendations:
- Invest in robust technology infrastructure to support streamlined online applications and verification processes.
- Provide comprehensive training and support to state agency staff and beneficiaries to navigate the new system effectively.
- Implement rigorous data collection and analysis mechanisms to track key metrics, such as processing times, error rates, and beneficiary outcomes.
- Establish regular feedback loops with beneficiaries and providers to identify and address challenges proactively.
- Conduct ongoing evaluation and refinement of the redetermination process based on data analysis and stakeholder feedback.
Final Summary: HHS Offers Flexibilities Medicaid Redeterminations

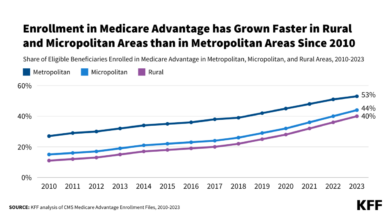
Source: kff.org
The HHS’s decision to offer flexibilities in Medicaid redeterminations is a significant development with far-reaching consequences. While the intention is to streamline the process and ensure continued access to care, the actual impact will vary greatly depending on state-level implementation and individual circumstances. Keeping a close eye on data reporting and ongoing analysis will be crucial in assessing the effectiveness of these changes and making necessary adjustments to ensure the program continues to serve its intended purpose.
It’s a dynamic situation, and we’ll continue to monitor the developments as they unfold.
Frequently Asked Questions
What happens if I don’t respond to my Medicaid redetermination request?
Failure to respond may result in the temporary or permanent loss of your Medicaid coverage. It’s crucial to respond promptly and accurately.
How long does the redetermination process take?
The timeframe varies by state and individual circumstances, but it’s generally recommended to allow ample time for processing.
Where can I find more information about my state’s specific redetermination process?
Your state’s Medicaid agency website is the best resource for detailed information and contact details.
What if I disagree with the redetermination decision?
Most states offer an appeals process. Check your state’s Medicaid website for information on how to file an appeal.