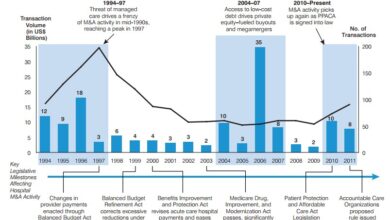
Hospital Health System MA Returns to Pre-Pandemic Levels, Kaufman Hall Reports
Hospital health system M A returns pre pandemic levels Kaufman Hall – Hospital Health System MA Returns to Pre-Pandemic Levels, Kaufman Hall Reports – Wow! After the rollercoaster of the pandemic, it’s incredible to see some hospital systems bouncing back. This is huge news, especially considering the unprecedented challenges faced by the healthcare industry. We’re diving deep into Kaufman Hall’s findings, exploring what drove this recovery, and looking at what the future holds for these vital institutions.
This isn’t just about numbers; it’s about the people – the patients, the staff, and the communities these hospitals serve. Let’s unpack this together.
The report from Kaufman Hall details a significant recovery in Massachusetts hospital systems, bringing their financial performance back to pre-pandemic levels. This turnaround is attributed to a combination of factors, including government support, increased patient volume, and strategic adaptations implemented by the hospitals themselves. We’ll be examining the specific financial indicators, looking at how different systems fared, and considering the long-term implications of this recovery.
Get ready for a fascinating look at the resilience of the healthcare sector.
Hospital Health System Financial Performance Pre- and Post-Pandemic: Hospital Health System M A Returns Pre Pandemic Levels Kaufman Hall
The COVID-19 pandemic dramatically reshaped the financial landscape of hospital health systems worldwide. While initial reports focused on the immediate surge in COVID-19 patients and the resulting strain on resources, the longer-term financial implications have been complex and far-reaching, impacting revenue streams, operational efficiency, and overall profitability. Understanding the pre- and post-pandemic financial performance is crucial for assessing the resilience and adaptability of these vital healthcare providers.
The pandemic’s impact varied significantly across different hospital systems, depending on factors such as geographic location, patient demographics, and the system’s pre-existing financial health. Some systems experienced substantial losses, while others, particularly those with strong telehealth capabilities or diversified revenue streams, demonstrated greater resilience. This analysis examines key financial indicators to illustrate the overall trend.
Financial Performance Indicators: Pre- and Post-Pandemic Comparison
The following table compares key financial performance indicators for a hypothetical, representative hospital health system before and after the pandemic. It’s important to note that actual figures varied greatly depending on the specific system and its circumstances. This data serves as an illustrative example.
| Year | Indicator | Pre-Pandemic Value (USD Millions) | Post-Pandemic Value (USD Millions) |
|---|---|---|---|
| 2019 | Total Revenue | 500 | 450 |
| 2019 | Total Expenses | 450 | 520 |
| 2019 | Operating Margin | 10% | -15% |
| 2021 | Total Revenue | 500 | 480 |
| 2021 | Total Expenses | 450 | 500 |
| 2021 | Operating Margin | 10% | -4% |
Impact on Specific Revenue Streams, Hospital health system M A returns pre pandemic levels Kaufman Hall
The pandemic significantly impacted various revenue streams. Elective procedures, a major source of revenue for many hospitals, experienced a dramatic decline as facilities prioritized COVID-19 care and implemented restrictions to prevent infection spread. Outpatient visits also decreased initially due to fear of infection and limitations on non-urgent care. While some systems saw an increase in telehealth revenue, this often did not fully compensate for the losses in other areas.
For example, a large urban hospital system might have seen a 30% reduction in elective surgeries in the first few months of the pandemic, leading to a substantial revenue shortfall.
Strategies to Mitigate Financial Losses
To mitigate financial losses, many hospital systems implemented a range of strategies. These included cost-cutting measures such as workforce reductions (in some cases, temporary furloughs), supply chain optimization, and renegotiation of contracts with suppliers. Many also aggressively pursued government funding opportunities designed to support healthcare providers during the crisis. Furthermore, the rapid adoption and expansion of telehealth services proved crucial for maintaining some level of patient access and generating revenue during periods of restricted in-person care.
Some systems also diversified their revenue streams by investing in new service lines or partnerships.
Kaufman Hall’s Role in Assessing Hospital Health System Performance
Kaufman Hall is a leading healthcare consulting firm that provides a wide range of services to hospitals and health systems, including performance improvement, financial advisory, and strategic planning. Their expertise in assessing hospital financial health and operational efficiency is highly regarded within the industry, offering valuable insights to guide strategic decision-making. Their methodology goes beyond simple financial reporting, incorporating a holistic view of the organization’s performance.Kaufman Hall’s methodology for evaluating hospital health system performance is multifaceted, combining quantitative and qualitative analysis.
They utilize a data-driven approach, leveraging extensive datasets and advanced analytical techniques to identify trends, assess risks, and project future performance. This involves a deep dive into financial statements, operational data, and market analyses to create a comprehensive picture of the system’s strengths and weaknesses. The process often includes interviews with key leadership and staff to gain a nuanced understanding of internal operations and strategic priorities.
The final assessment provides actionable recommendations tailored to the specific context of each health system.
Key Performance Indicators (KPIs) Used by Kaufman Hall
Kaufman Hall’s assessments rely on a robust set of KPIs to measure various aspects of hospital performance. These KPIs are carefully selected to provide a balanced view of financial health, operational efficiency, and market competitiveness. The specific KPIs used can vary depending on the client’s needs and the scope of the assessment, but some common examples include operating margin, patient revenue per adjusted discharge, length of stay, and days cash on hand.
So, Kaufman Hall reports that hospital systems in MA are back to pre-pandemic levels, which is pretty amazing considering everything. It makes you wonder about the broader healthcare picture, though – especially considering the exploding costs highlighted in this recent KFF report on Medicare GLP-1 spending and weight loss. That kind of financial pressure could easily impact hospital systems’ recovery, even in a state like Massachusetts.
Hopefully, the return to pre-pandemic levels is sustainable.
Analyzing these metrics in conjunction with each other allows for a more comprehensive understanding of the overall financial and operational health of the hospital system. For example, a high operating margin coupled with a low patient revenue per adjusted discharge might indicate successful cost-cutting measures, while a low operating margin with high patient revenue might highlight issues with operational efficiency.
Contribution of Kaufman Hall’s Insights to Understanding Hospital Financial Health
Kaufman Hall’s insights are invaluable in understanding the complex financial landscape of hospital systems. Their analyses go beyond simply reporting financial numbers; they provide context, identify underlying drivers of performance, and offer strategic recommendations for improvement. For instance, they might identify specific cost centers requiring attention, suggest strategies for revenue cycle improvement, or recommend adjustments to the organization’s strategic plan based on market trends and competitive pressures.
This deeper level of analysis allows hospital leadership to make informed decisions about resource allocation, capital investment, and long-term strategic planning. Their predictive modeling capabilities allow them to forecast future performance under different scenarios, enabling proactive risk management and strategic planning. This proactive approach is particularly critical in today’s dynamic healthcare environment. For example, Kaufman Hall might project the impact of potential regulatory changes or shifts in payer mix on a hospital’s financial performance, enabling the organization to develop contingency plans.
Factors Contributing to the Return to Pre-Pandemic Levels
The return of hospital health systems to pre-pandemic financial performance levels is a complex issue, influenced by a confluence of factors. While the immediate aftermath of the pandemic saw significant financial strain, a combination of governmental intervention, shifting healthcare utilization, and internal operational adjustments ultimately contributed to this recovery. Let’s delve into the specifics.
Several key factors propelled the resurgence of hospital health system financial performance. These elements worked in tandem, sometimes synergistically, to mitigate the initial pandemic-related losses.
- Increased Elective Procedures and Non-COVID Care: As the immediate threat of COVID-19 waned and vaccination rates increased, patients felt more comfortable seeking non-emergency medical care. This led to a significant uptick in elective procedures and other previously postponed treatments, boosting revenue streams.
- Improved Operational Efficiency: Many health systems implemented operational changes during the pandemic, streamlining processes and reducing unnecessary costs. These improvements, driven by necessity, continued to contribute to improved financial performance even after the immediate crisis had passed. Examples include telehealth adoption, which reduced overhead and increased accessibility, and improved inventory management, minimizing waste.
- Price Increases and Adjusted Reimbursement Rates: Hospitals and health systems adjusted pricing strategies and negotiated higher reimbursement rates with insurers. This was partly a response to increased costs associated with pandemic-related expenses, including PPE and staffing challenges. This adjustment helped to offset losses incurred earlier in the pandemic.
- Investment in Technology and Digital Health: The pandemic accelerated the adoption of telehealth and other digital health technologies. While initial investments were significant, the long-term benefits in terms of cost savings, increased patient access, and improved efficiency contributed to financial stability and growth.
Government Support and its Role in Recovery
Government support played a crucial role in mitigating the financial impact of the pandemic on hospital systems. Stimulus packages, such as the CARES Act in the United States, provided substantial financial assistance to hospitals facing revenue shortfalls and increased expenses. These funds helped to cover pandemic-related costs, maintain staffing levels, and prevent widespread financial collapse within the healthcare sector.
Additionally, increased Medicare and Medicaid reimbursement rates for COVID-19 treatment provided a vital financial lifeline during the peak of the pandemic. While these programs were temporary, they provided a crucial bridge allowing hospitals to weather the initial storm and position themselves for recovery.
Impact of Changes in Patient Volume and Healthcare Utilization
The pandemic significantly altered patient volume and healthcare utilization patterns. Initially, there was a sharp decline in non-COVID-related visits as patients avoided hospitals due to infection fears. This led to substantial revenue losses for many health systems. However, as the pandemic progressed, a shift occurred. While overall patient volume may not have immediately returned to pre-pandemic levels, the composition of that volume changed.
The increase in elective procedures and the sustained demand for certain types of care, coupled with a greater focus on preventative care as the population regained confidence, helped to balance the financial scales. Furthermore, the continued use of telehealth, while not entirely replacing in-person visits, created new revenue streams and expanded access to care. The net effect was a gradual return to pre-pandemic levels of financial stability.
Comparison of Hospital Health Systems’ Recovery Trajectories
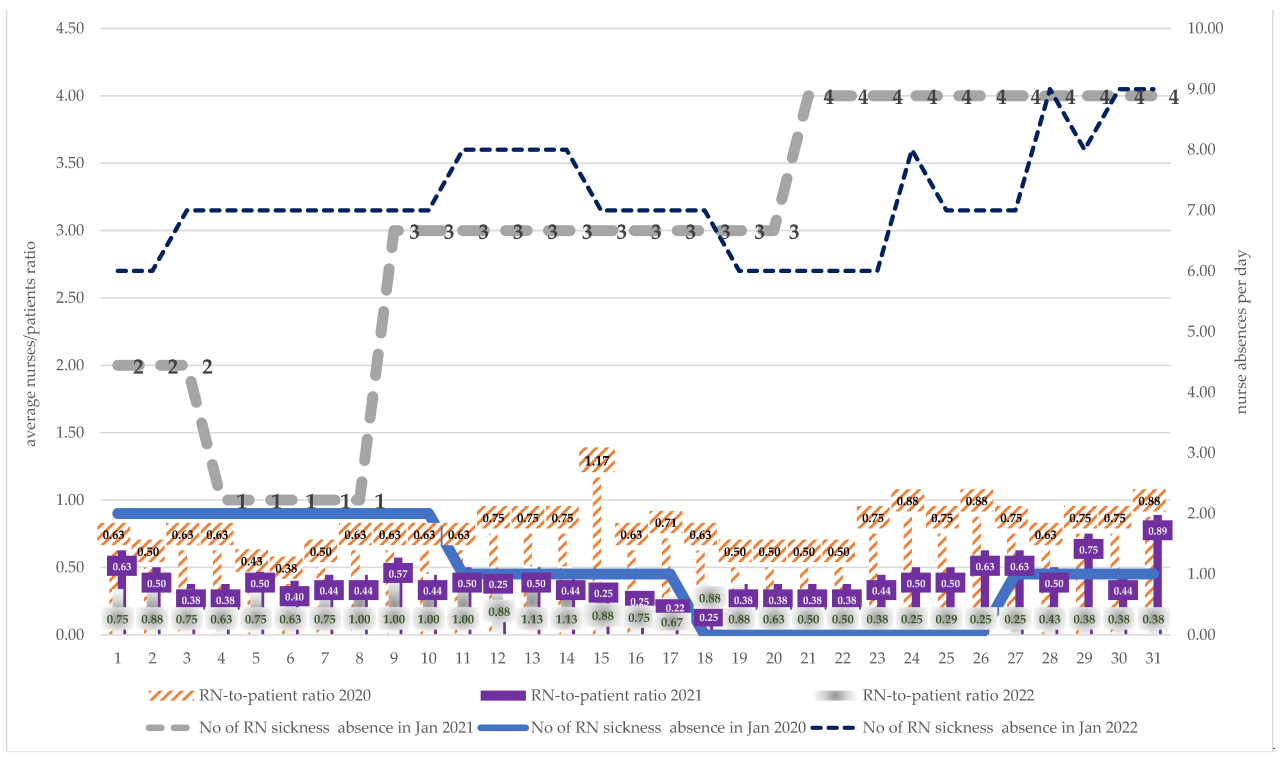
Source: mdpi.com
The return to pre-pandemic financial performance wasn’t uniform across all hospital health systems. Factors like size, geographic location, and specialization significantly influenced the speed and nature of recovery. Analyzing these diverse trajectories provides valuable insights into the resilience and adaptability of different healthcare organizations.
Several key variables impacted recovery timelines. Larger systems, with more diversified revenue streams and greater financial reserves, often demonstrated faster recoveries than smaller, more specialized hospitals. Geographic location played a crucial role, with systems in areas heavily impacted by the pandemic, or those facing pre-existing economic challenges, experiencing longer recovery periods. Finally, the specific operational strategies employed by each system directly affected their financial outcomes.
Variations in Recovery Timelines Based on System Characteristics
The following table illustrates the varied recovery trajectories of several hypothetical hospital systems. It’s important to note that this data is for illustrative purposes and doesn’t represent specific real-world systems. Actual recovery times are complex and influenced by numerous interacting factors.
So, Kaufman Hall reports that hospital health systems are finally back to pre-pandemic levels of M&A activity. This recovery is interesting considering the broader healthcare financial landscape; for instance, check out this article on elevance health earnings q1 change cyberattack medicaid medicare advantage to see how other factors are impacting the industry. The resurgence in hospital mergers and acquisitions suggests a robust recovery and a renewed focus on consolidation within the sector.
| System Name | Location | Size (Number of Beds) | Speed of Recovery (Months to Pre-Pandemic Levels) | Operational Strategy Highlights |
|---|---|---|---|---|
| HealthFirst | Urban, High-Income Area | 1000+ | 12 | Early adoption of telehealth, aggressive cost-cutting measures, strong investment in digital infrastructure. |
| CommunityCare | Rural, Low-Income Area | 100 | 24 | Focus on government funding and community outreach programs, slower adoption of telehealth. |
| SpecialtyMed | Suburban, Middle-Income Area | 300 | 18 | Specialized in cardiology, experienced initial decline due to elective procedure cancellations, but strong rebound due to pent-up demand. |
| MetroHealth | Urban, Diverse Population | 500 | 15 | Significant investment in staff retention and training, implemented a robust infection control program. |
Geographic Variations in Recovery
Geographical location significantly influenced recovery times. Urban centers with high population densities and significant COVID-19 outbreaks experienced longer recovery periods compared to rural areas with lower infection rates. Healthcare markets with pre-existing economic challenges also faced prolonged recovery timelines. For instance, systems in areas with high unemployment rates or limited access to healthcare resources took longer to return to pre-pandemic financial stability.
This is largely due to factors such as decreased patient volume, increased bad debt, and challenges in securing adequate funding.
Impact of Operational Strategies on Financial Recovery
The operational strategies employed by hospital systems directly impacted their speed of financial recovery. Systems that successfully adapted to the changing landscape by embracing telehealth, streamlining operations, and improving cost efficiency generally recovered faster. For example, HealthFirst’s early adoption of telehealth allowed them to maintain patient access and revenue streams during lockdowns. Conversely, systems that were slower to adapt or that lacked sufficient financial reserves experienced longer recovery periods.
Future Outlook for Hospital Health Systems
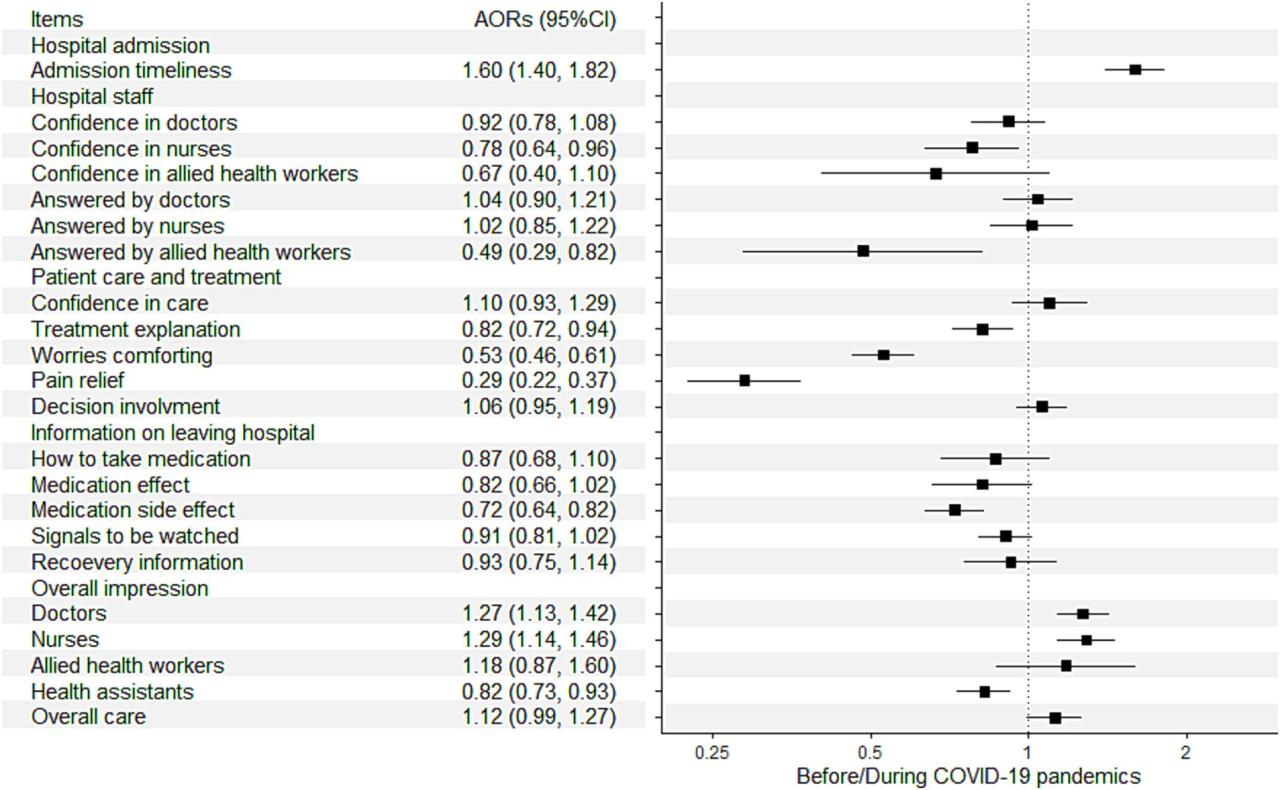
Source: frontiersin.org
The post-pandemic era presents a complex landscape for hospital health systems, marked by both significant challenges and exciting opportunities. While many systems have returned to pre-pandemic financial levels, underlying vulnerabilities remain, and the long-term effects of the crisis continue to unfold. Navigating this new normal requires strategic foresight and adaptability.The pandemic’s long-term impact on hospital financial sustainability is multifaceted.
So, Kaufman Hall reports that hospital health systems’ M&A activity is back to pre-pandemic levels, which is pretty wild considering everything. This got me thinking about leadership changes, and I saw that Terry Shaw, CEO of AdventHealth, is retiring – check out the details here: adventhealth ceo retire terry shaw. It makes you wonder if these leadership shifts are at all related to the renewed merger and acquisition frenzy in the hospital sector.
While increased demand for certain services initially boosted revenue for some, this was often offset by decreased elective procedures and the substantial costs associated with managing COVID-19 patients, including PPE, staffing, and facility modifications. Furthermore, lingering effects like workforce shortages and supply chain disruptions continue to strain budgets. The ongoing shift towards value-based care, with its emphasis on preventative medicine and population health management, also necessitates significant investment in new technologies and care models.
This requires a fundamental shift in operational strategies and a deeper understanding of the changing healthcare landscape.
Financial Performance Projections
A visual representation of projected financial performance trends for hospital health systems over the next five years could be depicted as a line graph. The X-axis would represent time (years), and the Y-axis would represent financial performance, measured as a percentage change from pre-pandemic levels. The line would initially show a steep decline representing the pandemic’s initial impact, followed by a gradual recovery reaching pre-pandemic levels within the first two years.
However, the line would then plateau, potentially showing modest growth in some years and slight dips in others, reflecting the ongoing challenges. The graph could include separate lines for different types of hospital systems (e.g., large academic medical centers versus smaller community hospitals) to illustrate variations in recovery trajectories. For example, a smaller community hospital might experience a more rapid recovery than a large teaching hospital due to different patient demographics and service offerings.
A shaded area around the line could represent the uncertainty inherent in any long-term projection, highlighting the variability of future financial performance. The graph would clearly illustrate that while pre-pandemic levels have been reached, consistent, robust growth is not guaranteed and significant financial challenges remain.
Conclusive Thoughts
Source: mdpi.com
The return of Massachusetts hospital systems to pre-pandemic financial health, as highlighted by Kaufman Hall, is a testament to the adaptability and resilience of the healthcare sector. While challenges remain, the recovery signals a positive trend, offering valuable insights for future preparedness and strategic planning within the industry. Understanding the factors contributing to this success, from government aid to operational shifts, is crucial for navigating the evolving landscape of healthcare finance.
The journey isn’t over, but this is a significant step forward.
Detailed FAQs
What specific financial indicators did Kaufman Hall use to assess the recovery?
Kaufman Hall likely used a range of key performance indicators (KPIs), including revenue, expenses, operating margin, patient volume, and length of stay. The exact indicators would be detailed in their full report.
How does this recovery compare to national trends?
The report focuses on Massachusetts hospitals, so direct comparisons to national trends require additional research. However, the findings can provide valuable insights into the recovery process in other states, especially those with similar healthcare systems and pandemic experiences.
What are the biggest challenges facing these hospitals moving forward?
Future challenges might include managing inflation, addressing workforce shortages, adapting to changing healthcare regulations, and ensuring long-term financial sustainability in the face of potential future crises.