How Are Acid Reflux, Fatty Liver, and Inflammation Linked to Chronic Diseases?
How are acid reflux fatty liver and inflammation linked to chronic diseases – How are acid reflux, fatty liver, and inflammation linked to chronic diseases? That’s a question that’s been burning in my mind lately, and I’m diving deep to uncover the connections. We’re talking about a trio of seemingly separate issues that, when examined closely, reveal a surprising interconnectedness with far-reaching health consequences. This isn’t just about heartburn and a slightly enlarged liver; it’s about understanding how these conditions can contribute to the development of serious, long-term illnesses.
Get ready to explore the intricate web of inflammation, metabolic dysfunction, and chronic disease risk.
This post will unravel the complex relationships between acid reflux, fatty liver disease (specifically NAFLD), and chronic inflammation. We’ll explore how chronic acid reflux can trigger systemic inflammation, potentially contributing to a cascade of health problems. Then, we’ll delve into the inflammatory pathways in fatty liver disease and its link to insulin resistance and the progression to more serious liver conditions.
Finally, we’ll connect these seemingly disparate conditions, examining how they interact to increase the risk of chronic diseases like type 2 diabetes and cardiovascular disease. Prepare for a fascinating journey into the body’s intricate systems!
Acid Reflux and its Role in Chronic Disease Development
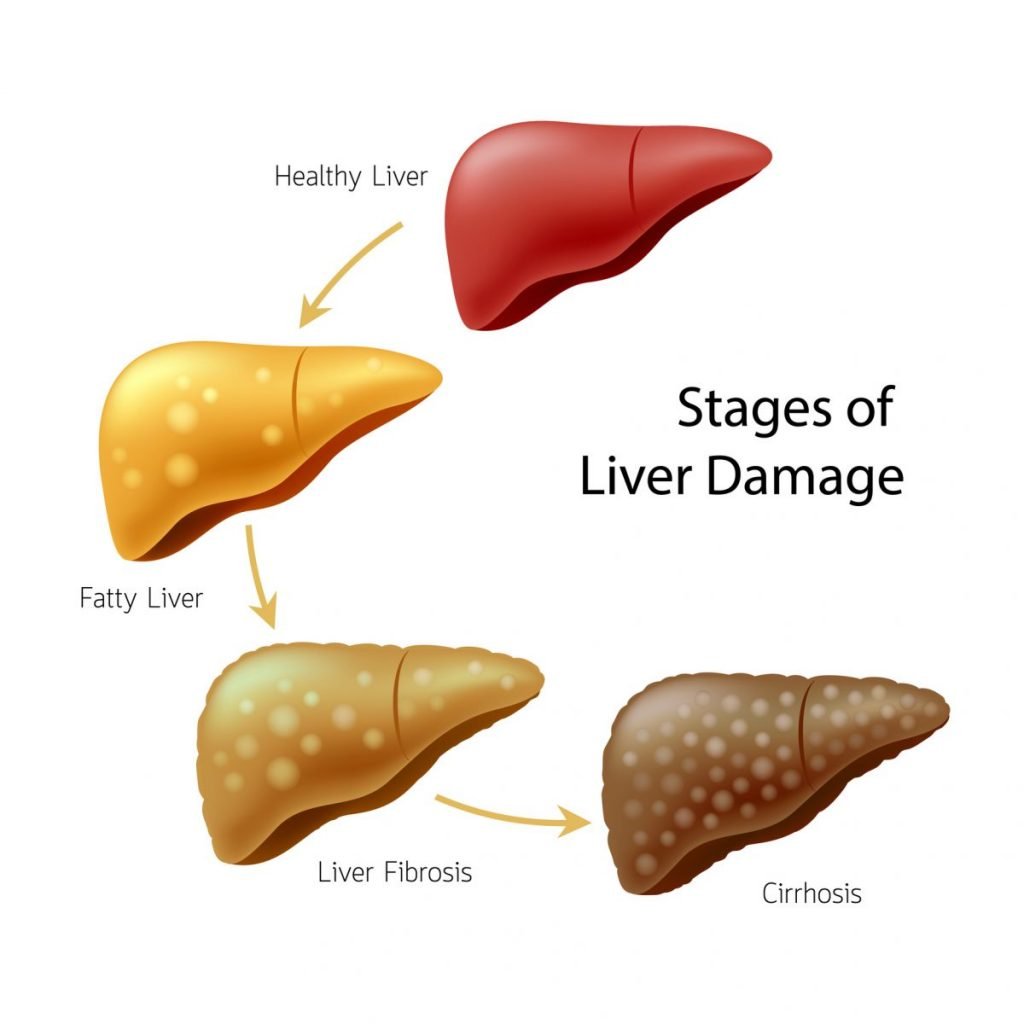
Source: mblycdn.com
Acid reflux, or gastroesophageal reflux disease (GERD), is more than just heartburn; it’s a chronic condition that, if left untreated, can significantly impact overall health and increase the risk of developing several serious diseases. The persistent exposure of the esophagus to stomach acid triggers a cascade of inflammatory responses throughout the body, ultimately contributing to a higher risk of various chronic illnesses.
Mechanisms of Chronic Acid Reflux-Induced Systemic Inflammation
Chronic acid reflux leads to persistent inflammation in the esophagus, initially manifesting as esophagitis. This inflammation isn’t localized; it triggers the release of inflammatory cytokines and other signaling molecules into the bloodstream. These molecules travel throughout the body, promoting systemic inflammation, a process implicated in the development of numerous chronic diseases like cardiovascular disease, type 2 diabetes, and even certain cancers.
So, we’re talking about how acid reflux, fatty liver, and chronic inflammation are all interconnected, paving the way for serious health problems down the line. It’s all about that low-grade, persistent inflammation affecting various systems. Thinking about long-term health got me reading about Karishma Mehta getting her eggs frozen and the risks involved , which highlights how proactive health choices are crucial at every stage of life.
Ultimately, managing inflammation through diet and lifestyle is key to preventing these interconnected chronic diseases.
The constant irritation and injury to the esophageal lining further exacerbate the inflammatory response, creating a vicious cycle that perpetuates and amplifies the systemic effects. The body’s attempt to heal the damaged esophageal tissue also contributes to the overall inflammatory burden.
Untreated Acid Reflux and Esophageal Cancer Risk
The link between untreated GERD and esophageal cancer, specifically adenocarcinoma, is well-established. Chronic exposure of the esophageal lining to stomach acid causes long-term damage and cellular changes. Over time, these changes can lead to the development of precancerous lesions known as Barrett’s esophagus. Barrett’s esophagus significantly increases the risk of developing esophageal adenocarcinoma. Regular monitoring and prompt treatment of GERD are crucial to minimizing this risk.
While not everyone with GERD will develop esophageal cancer, the risk is demonstrably higher in individuals with long-standing, untreated reflux.
Lifestyle Modifications to Mitigate Acid Reflux and Inflammation
Several lifestyle changes can significantly reduce acid reflux symptoms and the associated inflammation. These modifications target the underlying causes of reflux, such as dietary triggers and lifestyle habits.
Examples of effective strategies include:
- Maintaining a healthy weight: Obesity increases intra-abdominal pressure, contributing to reflux.
- Dietary adjustments: Avoiding trigger foods like fatty or spicy foods, chocolate, caffeine, and alcohol can reduce symptoms.
- Elevating the head of the bed: This can help prevent stomach acid from flowing back into the esophagus.
- Eating smaller, more frequent meals: This reduces the volume of food in the stomach at any given time.
- Quitting smoking: Smoking weakens the lower esophageal sphincter, increasing reflux.
- Stress management: Stress can exacerbate acid reflux symptoms.
Comparison of Acid Reflux Medications and Potential Side Effects
Different medications are available to treat acid reflux, each with its own mechanism of action and potential side effects. Choosing the right medication depends on the severity of the condition and individual patient factors.
| Medication Type | Mechanism of Action | Common Side Effects | Serious Side Effects (Rare) |
|---|---|---|---|
| Antacids | Neutralize stomach acid | Constipation, diarrhea | Metabolic alkalosis (with excessive use) |
| H2 Blockers (e.g., ranitidine, famotidine) | Reduce stomach acid production | Headache, dizziness, constipation | Severe allergic reactions, liver damage |
| Proton Pump Inhibitors (PPIs) (e.g., omeprazole, lansoprazole) | Significantly reduce stomach acid production | Headache, diarrhea, nausea | Increased risk of bone fractures, kidney problems, Clostridium difficile infection |
Fatty Liver Disease and its Inflammatory Pathways
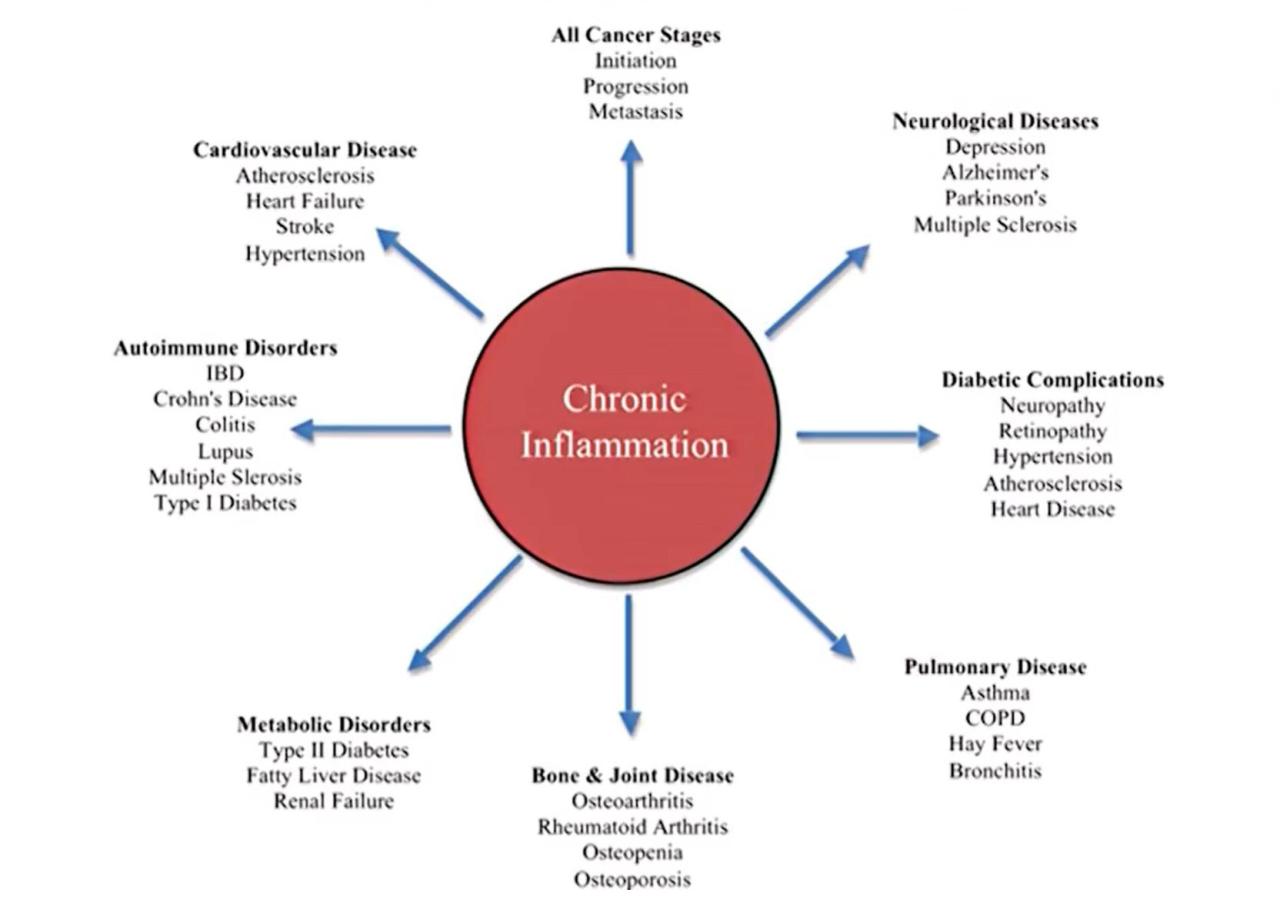
Source: somaticmovementcenter.com
Fatty liver disease, particularly non-alcoholic fatty liver disease (NAFLD), is a significant health concern globally, often linked to metabolic syndrome and a silent contributor to chronic inflammation. Understanding its inflammatory pathways is crucial for developing effective prevention and treatment strategies. This section delves into the intricate relationship between NAFLD, insulin resistance, hepatic inflammation, and the progression to more severe liver diseases.
NAFLD and Insulin Resistance
NAFLD is strongly associated with insulin resistance, a condition where the body’s cells don’t respond effectively to insulin, leading to elevated blood sugar levels. Insulin resistance promotes the accumulation of fat in the liver, initiating the development of NAFLD. The exact mechanisms are complex but involve impaired insulin signaling in hepatocytes (liver cells), leading to increased lipogenesis (fat synthesis) and decreased fatty acid oxidation (fat breakdown).
This imbalance results in the build-up of triglycerides within the liver, causing hepatocyte damage and triggering an inflammatory response. Studies have shown a clear correlation between higher levels of insulin resistance, as measured by HOMA-IR (Homeostasis Model Assessment of Insulin Resistance), and the severity of NAFLD. For instance, individuals with type 2 diabetes, a condition characterized by significant insulin resistance, have a much higher prevalence of NAFLD.
Hepatic Inflammation in NAFLD Progression
Hepatic inflammation, or inflammation within the liver, plays a central role in the progression of NAFLD. The accumulation of fat in the liver activates various immune cells, including Kupffer cells (resident macrophages in the liver) and inflammatory cytokines, such as TNF-α (Tumor Necrosis Factor-alpha) and IL-6 (Interleukin-6). These inflammatory mediators damage liver cells, leading to fibrosis (scarring) and ultimately cirrhosis and liver failure.
The chronic inflammatory state in NAFLD disrupts liver architecture and function, potentially contributing to the development of hepatocellular carcinoma (liver cancer). The severity of inflammation, often assessed through liver biopsies and blood tests measuring inflammatory markers, correlates with the stage and prognosis of NAFLD.
Chronic inflammation, often stemming from issues like acid reflux and fatty liver disease, significantly increases the risk of developing serious health problems. These conditions can weaken the body’s defenses, making it more susceptible to respiratory illnesses, as highlighted by the recent news of Monali Thakur’s hospitalization after struggling to breathe; you can read more about preventing respiratory diseases here: monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases.
Ultimately, managing inflammation through diet and lifestyle changes is crucial in preventing a cascade of chronic diseases.
Dietary Changes and Reduction of Inflammation in Fatty Liver
Research consistently demonstrates the positive impact of dietary changes on reducing inflammation associated with fatty liver disease. A diet rich in fruits, vegetables, and whole grains, while limiting saturated and trans fats, refined carbohydrates, and excessive sugar intake, can significantly improve liver health. Studies have shown that the Mediterranean diet, characterized by its emphasis on plant-based foods, olive oil, and fish, is particularly effective in reducing liver fat content and improving liver enzyme levels, thereby mitigating inflammation.
Specifically, the consumption of foods rich in antioxidants, such as polyphenols found in berries and green tea, can help combat oxidative stress and reduce inflammation. Weight loss, even modest weight loss, through dietary modification and increased physical activity, is crucial in improving insulin sensitivity and reducing hepatic inflammation. For example, a meta-analysis of multiple studies showed a significant reduction in liver fat and inflammation in individuals with NAFLD who adopted a weight-loss diet.
Stages of NAFLD and Associated Inflammatory Markers
The following flowchart illustrates the progression of NAFLD and the associated inflammatory markers:[Flowchart Description: The flowchart would visually represent the stages of NAFLD, starting with Simple Steatosis (fat accumulation without inflammation), progressing to Non-alcoholic Steatohepatitis (NASH, characterized by fat accumulation and inflammation), then Fibrosis (scarring), Cirrhosis (severe scarring), and finally Hepatocellular Carcinoma (liver cancer). Each stage would be linked to specific inflammatory markers, such as ALT (Alanine aminotransferase), AST (Aspartate aminotransferase), TNF-α, IL-6, and others.
The increase in the levels of these markers would be visually represented as the disease progresses. Arrows would connect the stages, illustrating the progression of the disease.]
Inflammation as a Common Link
Acid reflux and fatty liver disease, while seemingly disparate conditions, share a significant commonality: chronic inflammation. This pervasive inflammatory response isn’t just localized to the esophagus or liver; it creates a systemic inflammatory state that significantly increases the risk of developing a range of chronic diseases. Understanding the inflammatory pathways involved is crucial to grasping the interconnectedness of these conditions and their broader health implications.The inflammatory process in both conditions involves a complex interplay of immune cells and signaling molecules called cytokines.
These cytokines act as messengers, amplifying and coordinating the inflammatory response. However, the specific triggers and the nature of the inflammation differ depending on the organ involved.
Key Inflammatory Cytokines in Acid Reflux and Fatty Liver Disease
Both acid reflux and fatty liver disease involve a complex cascade of inflammatory cytokines. In acid reflux, the esophageal lining’s exposure to stomach acid triggers the release of pro-inflammatory cytokines like TNF-α (tumor necrosis factor-alpha), IL-1β (interleukin-1 beta), and IL-6 (interleukin-6). These cytokines promote inflammation and tissue damage in the esophagus, contributing to symptoms like heartburn and esophageal damage.
Similarly, in fatty liver disease, the accumulation of fat in the liver triggers the release of these same cytokines, along with others like IL-8 and IL-18. This leads to liver inflammation (steatohepatitis), fibrosis, and ultimately, cirrhosis and liver failure. The precise balance and levels of these cytokines vary depending on the severity and stage of each disease.
Comparison of Inflammatory Responses in the Esophagus and Liver
While both the esophagus and liver utilize similar inflammatory pathways involving TNF-α, IL-1β, and IL-6, the context and consequences differ significantly. In acid reflux, inflammation is primarily a reaction to direct chemical injury from stomach acid. The inflammatory response is largely localized to the esophageal lining, although severe cases can lead to systemic effects. In fatty liver disease, inflammation is a more complex process driven by multiple factors, including lipotoxicity (fatty acid toxicity), oxidative stress, and gut dysbiosis (imbalance of gut microbiota).
This leads to a more diffuse and prolonged inflammatory response within the liver, with potential for significant systemic repercussions. The chronic nature of the liver inflammation distinguishes it from the often episodic inflammation seen in acid reflux.
Chronic Inflammation and Systemic Disease
Chronic, low-grade inflammation, whether originating in the esophagus, liver, or other organs, doesn’t stay confined to the initial site. It creates a systemic inflammatory environment, impacting various bodily functions and increasing susceptibility to a wide range of chronic diseases. The persistent release of inflammatory cytokines into the bloodstream can trigger widespread damage, affecting blood vessels, promoting oxidative stress, and disrupting metabolic processes.
This systemic inflammation is a major driver of many chronic illnesses.
Chronic Diseases Linked to Systemic Inflammation
Chronic systemic inflammation is a significant risk factor for a multitude of diseases. The following list highlights some key examples and shared risk factors:
- Cardiovascular Disease: Inflammation damages blood vessels, leading to atherosclerosis (plaque buildup) and increasing the risk of heart attacks and strokes. Shared risk factors include obesity, diabetes, and high blood pressure.
- Type 2 Diabetes: Inflammation impairs insulin signaling and contributes to insulin resistance, a hallmark of type 2 diabetes. Shared risk factors include obesity, unhealthy diet, and lack of exercise.
- Rheumatoid Arthritis: This autoimmune disease is characterized by chronic inflammation in the joints. Shared risk factors include genetic predisposition and environmental triggers.
- Neurodegenerative Diseases (Alzheimer’s and Parkinson’s): Inflammation plays a role in the neurodegeneration seen in these conditions. Shared risk factors are not fully understood but may include aging, genetic factors, and environmental exposures.
- Certain Cancers: Chronic inflammation can create an environment that promotes tumor growth and metastasis. Shared risk factors vary depending on the specific cancer type but can include smoking, exposure to carcinogens, and chronic infections.
Interconnectedness of Acid Reflux, Fatty Liver, and Inflammation: How Are Acid Reflux Fatty Liver And Inflammation Linked To Chronic Diseases
Source: draxe.com
The relationship between acid reflux, fatty liver disease (FLD), and chronic inflammation isn’t simply a case of three separate conditions existing in the same body. Instead, compelling evidence suggests a complex interplay, where each condition can exacerbate the others, creating a vicious cycle that significantly increases the risk of developing serious chronic diseases. Understanding these interconnected pathways is crucial for developing effective preventative and therapeutic strategies.The potential causal pathways are multifaceted and not fully elucidated, but several mechanisms are increasingly understood.
For instance, chronic inflammation, a hallmark of both acid reflux (gastroesophageal reflux disease or GERD) and FLD, can trigger and sustain the progression of each other. The constant irritation of the esophagus from refluxed stomach acid can lead to chronic inflammation, potentially impacting the gut microbiome and increasing systemic inflammation. This systemic inflammation, in turn, can contribute to the development of FLD by promoting fat accumulation in the liver and impairing its function.
So, acid reflux, fatty liver, and inflammation – they’re a nasty trio often paving the way for chronic illnesses like heart disease and diabetes. Understanding how to manage these issues is crucial, and that’s where diet plays a huge role. It’s fascinating to learn more about how nutritional needs differ between the sexes, as highlighted in this article on are women and men receptive of different types of food and game changing superfoods for women , because choosing the right foods can significantly impact inflammation and liver health, ultimately affecting your risk of chronic diseases.
Conversely, FLD’s inflammatory state can further increase the likelihood of GERD through hormonal and metabolic changes.
Metabolic Syndrome as a Linking Factor
Metabolic syndrome, a cluster of conditions including obesity, high blood pressure, high blood sugar, and abnormal cholesterol levels, acts as a significant bridge connecting acid reflux, fatty liver disease, and the increased risk of chronic diseases like type 2 diabetes, cardiovascular disease, and certain cancers. Individuals with metabolic syndrome often experience increased visceral fat accumulation, which is strongly linked to both GERD and FLD.
The excess fat in the abdominal cavity can increase intra-abdominal pressure, contributing to acid reflux. Simultaneously, this visceral fat releases inflammatory cytokines, further fueling the inflammatory processes driving both GERD and the progression of FLD to non-alcoholic steatohepatitis (NASH). For example, a study published in the
Journal of Hepatology* demonstrated a strong correlation between the severity of metabolic syndrome and the risk of developing NASH.
Gut Microbiota Dysbiosis and Systemic Inflammation
The gut microbiome, the complex community of bacteria and other microorganisms residing in the digestive tract, plays a pivotal role in maintaining overall health. Dysbiosis, an imbalance in the gut microbiota composition, is increasingly recognized as a significant contributor to inflammation in multiple organ systems. In the context of acid reflux, FLD, and their associated chronic diseases, dysbiosis can exacerbate the inflammatory cascade in several ways.
For example, an altered gut microbiome can increase intestinal permeability (“leaky gut”), allowing bacterial components and toxins to enter the bloodstream, triggering systemic inflammation. This systemic inflammation can worsen both GERD symptoms and promote the development and progression of FLD. Furthermore, specific bacterial species have been linked to increased production of inflammatory molecules, which can contribute to the development of both conditions.
A study in
Gut* showed a significant association between specific bacterial species and the severity of NASH.
Potential Therapeutic Targets for Reducing Inflammation
The interconnected nature of acid reflux, fatty liver disease, and inflammation suggests that therapeutic strategies should focus on addressing the underlying inflammatory processes. A multi-pronged approach is often necessary, tailored to the individual’s specific condition and overall health.
- Lifestyle Modifications: Weight loss, regular exercise, and a balanced diet low in saturated and trans fats are crucial first steps in managing inflammation and improving both GERD and FLD. These changes can improve insulin sensitivity, reduce visceral fat, and promote a healthier gut microbiome.
- Dietary Interventions: Specific dietary components, such as polyphenols found in fruits and vegetables, have demonstrated anti-inflammatory properties and may help manage both GERD and FLD. Eliminating trigger foods that exacerbate GERD symptoms is also important.
- Pharmacological Approaches: Proton pump inhibitors (PPIs) are commonly used to reduce stomach acid production in GERD, but long-term use may have side effects. Other medications, such as those targeting specific inflammatory pathways or improving gut microbiome composition, are being actively researched and developed.
- Probiotics and Prebiotics: The use of probiotics (live beneficial bacteria) and prebiotics (food for beneficial bacteria) can help restore gut microbiome balance and reduce inflammation. However, more research is needed to determine the optimal strains and dosages for specific conditions.
Illustrative Examples of Disease Progression
Understanding the interconnectedness of acid reflux, fatty liver disease, and inflammation requires examining how these conditions interact to contribute to chronic diseases. Let’s explore a case study illustrating this complex interplay.
Case Study: Progression from Acid Reflux and Fatty Liver to Type 2 Diabetes
Consider a 55-year-old male, Mr. Jones, with a history of long-standing gastroesophageal reflux disease (GERD). He experienced frequent heartburn, especially after meals, and occasionally woke up at night with a burning sensation in his chest. He self-medicated with over-the-counter antacids but rarely sought medical attention. Over the years, his symptoms worsened, and he started noticing abdominal bloating and discomfort.
He also gained significant weight, leading to obesity. Routine blood work revealed elevated liver enzymes, prompting further investigation which diagnosed him with non-alcoholic fatty liver disease (NAFLD). Over the next few years, Mr. Jones developed increased thirst and frequent urination, along with fatigue and blurred vision. Further testing confirmed a diagnosis of type 2 diabetes.
His physician explained that the chronic inflammation associated with both GERD and NAFLD likely contributed to insulin resistance, a key factor in the development of type 2 diabetes. The constant inflammation in his body, stemming from both his gut and liver, negatively impacted his body’s ability to regulate blood sugar effectively.
Microscopic Changes in Liver Tissue Associated with NAFLD Progression, How are acid reflux fatty liver and inflammation linked to chronic diseases
In the early stages of NAFLD, microscopic examination of liver tissue reveals an accumulation of fat droplets within hepatocytes (liver cells). These fat droplets appear as clear vacuoles within the cytoplasm of the cells. As the disease progresses, inflammation becomes evident. Inflammatory cells, such as macrophages and lymphocytes, infiltrate the liver tissue. These cells release cytokines and other inflammatory mediators, contributing to liver damage.
Advanced NAFLD (NASH, or non-alcoholic steatohepatitis) is characterized by hepatocyte ballooning (swelling of liver cells), lobular inflammation, and the formation of Mallory-Denk bodies (protein aggregates within damaged hepatocytes). Fibrosis, the formation of scar tissue, is also a hallmark of advanced NASH, potentially leading to cirrhosis and liver failure. The liver architecture becomes distorted, with the normal hepatic lobules replaced by fibrous septa.
Physiological Changes in the Esophageal Lining Caused by Chronic Acid Reflux
Chronic acid reflux leads to significant physiological changes in the esophageal lining. Normally, the esophagus is lined with stratified squamous epithelium, a protective layer of cells resistant to acid. However, prolonged exposure to stomach acid causes damage to this protective lining. Initially, this damage manifests as inflammation (esophagitis), characterized by redness, swelling, and erosion of the epithelial cells.
Microscopic examination shows an influx of inflammatory cells into the esophageal mucosa. With persistent reflux, the damage can progress to more severe conditions, such as Barrett’s esophagus. Barrett’s esophagus involves metaplasia, a change in the type of cells lining the esophagus. The normal squamous epithelium is replaced by columnar epithelium, similar to the lining of the intestine.
This change is considered precancerous, increasing the risk of esophageal adenocarcinoma. The microscopic appearance of Barrett’s esophagus shows the presence of intestinal metaplasia, with goblet cells and absorptive cells characteristic of the intestinal lining. The presence of dysplasia (abnormal cell growth) further indicates an increased risk of cancer.
Summary
So, there you have it – a glimpse into the complex interplay between acid reflux, fatty liver disease, and chronic inflammation. While these conditions might seem isolated, their interconnectedness is undeniable, significantly impacting the risk of developing serious chronic diseases. Understanding these relationships is crucial for proactive health management. By addressing underlying inflammation and adopting lifestyle changes like diet and exercise, we can potentially mitigate the risks and improve our overall well-being.
Remember, this is a complex area, and consulting with healthcare professionals is vital for personalized advice and treatment plans. Let’s prioritize our health and take steps towards a healthier, more informed future!
Question & Answer Hub
Can stress worsen acid reflux and fatty liver disease?
Yes, stress can exacerbate both conditions. Stress hormones can increase stomach acid production and impair liver function, leading to inflammation and worsening symptoms.
Are there specific foods to avoid if I have both acid reflux and fatty liver?
Fatty, fried foods, processed foods, sugary drinks, and excessive alcohol should be limited as they worsen both conditions. Focus on a balanced diet rich in fruits, vegetables, and lean protein.
How often should I get checked for fatty liver if I have acid reflux?
Regular checkups with your doctor, including liver function tests, are recommended, especially if you have risk factors like obesity or diabetes.
What are the long-term consequences of ignoring acid reflux and fatty liver?
Ignoring these conditions can lead to serious complications, including esophageal cancer (acid reflux), cirrhosis or liver failure (fatty liver), and increased risk of other chronic diseases.
