IBS Constipation, Diarrhea, and Management
How can ibs cause both constipation and diarrhoea and management measures – IBS: Constipation, Diarrhea, and Management – it sounds like a paradox, right? How can one condition cause both agonizing constipation and debilitating diarrhea? This isn’t some medical mystery; it’s a common reality for many living with Irritable Bowel Syndrome (IBS). This post delves into the fascinating (and sometimes frustrating!) mechanisms behind this duality, exploring the science, offering practical management strategies, and providing a glimmer of hope for those navigating this challenging condition.
We’ll unpack the gut-brain connection, discuss dietary tweaks, lifestyle changes, and medical interventions that can make a real difference.
Understanding IBS starts with recognizing its varied faces. While some experience primarily constipation (IBS-C), others battle mainly diarrhea (IBS-D), and many, like myself, experience a frustrating mix of both (mixed IBS). This fluctuating bowel behavior stems from a complex interplay of factors including gut motility issues, visceral hypersensitivity, gut microbiome imbalances, and even stress. We’ll examine each of these contributing elements to provide a clearer picture of how this perplexing condition works.
Understanding IBS and its Diverse Symptoms
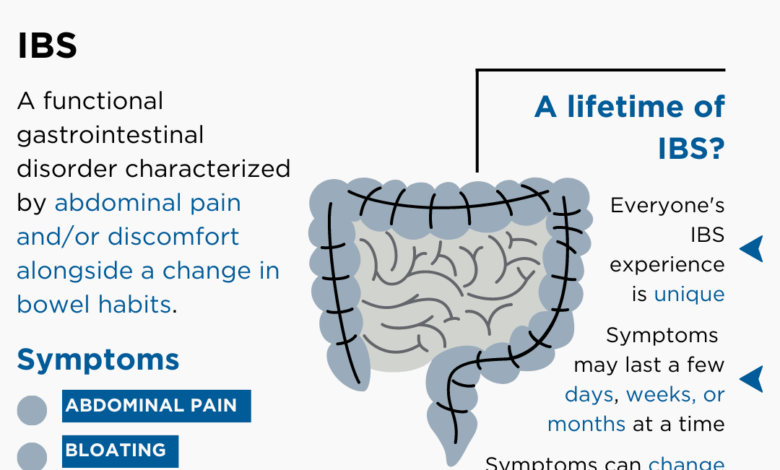
Irritable Bowel Syndrome (IBS) is a chronic gastrointestinal disorder affecting millions worldwide. Characterized by abdominal pain and altered bowel habits, its complexity stems from a poorly understood interplay of factors, making it a challenging condition to diagnose and manage. This section delves into the physiological mechanisms behind IBS, explores its various subtypes, and examines the crucial role of the gut-brain axis.The physiological mechanisms underlying IBS remain an area of active research.
However, several factors are implicated. Visceral hypersensitivity, an increased sensitivity to stimuli in the gut, is a key feature. This heightened sensitivity leads to amplified perception of normal gut sensations, resulting in pain and discomfort. Abnormal gut motility, referring to the contractions that move food through the digestive system, also plays a significant role. In some individuals, motility is slowed (constipation), while in others it’s accelerated (diarrhea).
Furthermore, alterations in gut microbiota, the community of bacteria and other microorganisms residing in the gut, are increasingly recognized as contributors to IBS symptoms. Changes in the composition and function of the gut microbiota can influence inflammation, gut permeability, and overall digestive function. Finally, psychological factors, such as stress and anxiety, significantly impact IBS symptoms through the gut-brain axis.
IBS Subtypes
IBS is classified into subtypes based on predominant bowel habits. These include constipation-predominant IBS (IBS-C), diarrhea-predominant IBS (IBS-D), and mixed IBS, where both constipation and diarrhea occur. Mixed IBS represents a significant portion of IBS cases, highlighting the fluctuating nature of the condition and the complex interplay of physiological factors involved. Patients with mixed IBS might experience periods of constipation followed by diarrhea, or even alternating episodes within a short timeframe.
This variability underscores the need for individualized treatment approaches.
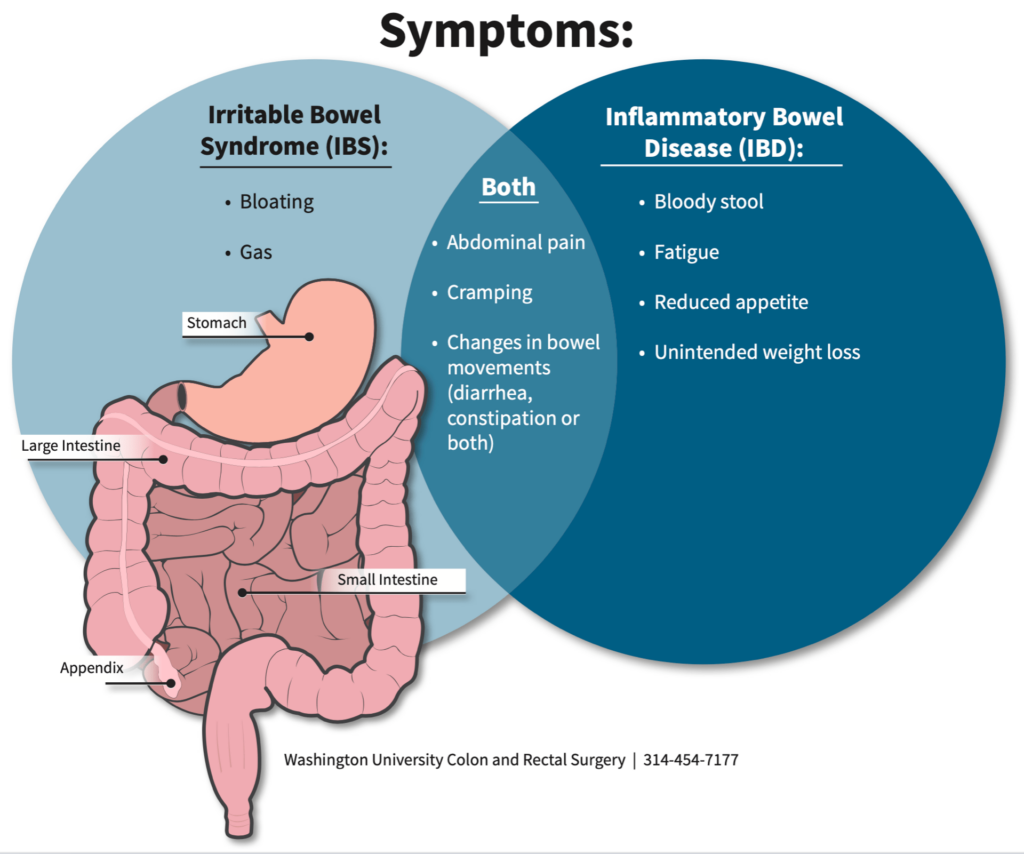
Comparison of IBS-C and IBS-D Symptoms
IBS-C is characterized by infrequent bowel movements, hard stools, and straining during defecation. Individuals with IBS-C often experience a feeling of incomplete evacuation, abdominal bloating, and discomfort. In contrast, IBS-D is marked by frequent loose or watery stools, urgency, and abdominal cramping. Patients with IBS-D may experience mucus in their stools and a sense of incomplete evacuation.
While distinct, these subtypes share overlapping symptoms such as abdominal pain, bloating, and fatigue. The variability in symptoms between individuals, even within the same subtype, highlights the need for personalized approaches to diagnosis and management.
The Gut-Brain Axis and IBS
The gut-brain axis refers to the bidirectional communication pathway between the gut and the brain. This complex network involves the nervous system, endocrine system, and immune system, all interacting to influence gut function and behavior. In IBS, this communication pathway is disrupted. Stress, anxiety, and other psychological factors can trigger changes in gut motility, visceral sensitivity, and gut microbiota composition, leading to symptom exacerbation.
Conversely, gut disturbances can also influence brain function, contributing to mood disorders and other psychological symptoms. Understanding the gut-brain axis is crucial for developing effective therapies that address both the physical and psychological aspects of IBS. For example, stress management techniques like mindfulness or cognitive behavioral therapy (CBT) can help regulate the gut-brain axis and improve IBS symptoms.
Similarly, changes in diet and lifestyle can influence gut microbiota composition and reduce inflammation, ultimately impacting the gut-brain communication.
The Paradox of Constipation and Diarrhea in IBS
Irritable bowel syndrome (IBS) is famously perplexing because it can manifest with seemingly contradictory symptoms: constipation and diarrhea. This isn’t simply a matter of alternating between the two; many IBS sufferers experience both within the same week, even the same day, creating significant challenges in managing their condition. Understanding this paradox requires looking at the underlying mechanisms within the gut.Visceral Hypersensitivity’s Dual Role in IBS Bowel HabitsVisceral hypersensitivity, a heightened sensitivity to sensations in the gut, is a hallmark of IBS.
This increased sensitivity isn’t just about pain; it impacts motility and the perception of bowel movements. In some individuals, heightened sensitivity leads to a perception of fullness and discomfort even with minimal bowel content, resulting in constipation. The gut muscles contract less frequently and with less force, leading to slower transit times and harder stools. Conversely, in others, the same hypersensitivity triggers more frequent, stronger contractions, causing the gut to expel contents too quickly, resulting in diarrhea.
The brain’s interpretation of gut signals, further complicated by the visceral hypersensitivity, plays a critical role in this process.Altered Gut Motility: The Engine of Inconsistent Bowel HabitsThe rhythmic contractions of the intestinal muscles, known as gut motility, are crucial for moving food through the digestive tract. In IBS, this motility is often disrupted. Some individuals experience slow transit constipation, where the movement is sluggish, leading to infrequent, hard stools.
Others experience accelerated transit diarrhea, where the food moves through the system too quickly, resulting in loose, frequent stools. The irregular patterns observed in IBS aren’t simply a case of one extreme or the other; rather, there’s often a mix of both slow and fast transit phases, contributing to the unpredictable nature of IBS symptoms. This inconsistency is further complicated by the varying responses to different foods and situations.The Impact of Gut Microbiota Dysbiosis on IBS Bowel HabitsThe gut microbiome, the vast community of bacteria and other microorganisms living in our intestines, plays a significant role in gut health.
In IBS, an imbalance in this microbiome, known as dysbiosis, is frequently observed. This dysbiosis can influence both constipation and diarrhea. For example, a reduction in beneficial bacteria that produce short-chain fatty acids (SCFAs), crucial for gut health and motility, can contribute to constipation. Conversely, an overgrowth of certain bacteria can trigger inflammation and increased motility, leading to diarrhea.
The exact mechanisms are complex and still under investigation, but the impact of dysbiosis on bowel habits in IBS is undeniable.Food Triggers: Exacerbating Both Constipation and DiarrheaMany IBS sufferers identify specific foods that worsen their symptoms. These triggers can vary greatly from person to person. For instance, high-fat foods might trigger diarrhea in one individual by stimulating gut motility, while in another, they could cause constipation due to slowing down transit time.
Similarly, certain fruits and vegetables containing high amounts of fiber, while generally beneficial, can exacerbate diarrhea in some IBS patients due to increased gas production and osmotic effects. Conversely, low-fiber diets can worsen constipation in others by reducing stool bulk. Identifying individual food triggers through careful dietary tracking is often crucial for managing IBS symptoms effectively. The impact of these triggers is further intensified by the already altered gut motility and visceral hypersensitivity present in IBS.
Dietary Management Strategies for IBS: How Can Ibs Cause Both Constipation And Diarrhoea And Management Measures

Source: dakotagi.com
Managing Irritable Bowel Syndrome (IBS) often involves a significant dietary overhaul. Since IBS can manifest as both constipation and diarrhea, a tailored approach is crucial, focusing on balancing fiber intake, hydration, and the gut microbiome. This requires careful consideration of what you eat and drink to alleviate symptoms and improve overall digestive health.
Sample Meal Plan for Managing IBS Symptoms
A balanced diet is key to managing both constipation and diarrhea associated with IBS. The following sample meal plan demonstrates a focus on easily digestible foods, adequate fiber, and hydration. Remember, individual needs vary, and this is just a guide. Consulting a registered dietitian or gastroenterologist is highly recommended for personalized dietary advice.
| Meal | Food Items | Fiber Content (approx.) | Potential Impact on IBS Symptoms |
|---|---|---|---|
| Breakfast | Oatmeal (1/2 cup) with berries (1/2 cup) and a sprinkle of nuts (1/4 cup) | 5-7g | Provides soluble fiber for stool softening (berries, oats) and some insoluble fiber for bulk (nuts). May help with both constipation and diarrhea depending on individual tolerance. |
| Lunch | Lentil soup (1.5 cups) with a side of whole-wheat bread (1 slice) | 10-12g | Lentils are a good source of soluble fiber, aiding in stool formation. Whole-wheat bread provides additional fiber but may need to be adjusted based on individual tolerance. |
| Dinner | Baked salmon (4oz) with roasted vegetables (1 cup) like carrots, zucchini, and squash | 4-6g | Lean protein and easily digestible vegetables. Provides some fiber without being overly harsh on the digestive system. |
| Snacks | Plain yogurt (1 cup), banana (1 medium), or a small handful of almonds | 2-4g (varies depending on snack) | Yogurt contains probiotics beneficial for gut health. Bananas provide potassium, and almonds offer healthy fats and fiber. |
Foods to Avoid
Certain foods commonly trigger or worsen both constipation and diarrhea in individuals with IBS. Avoiding these can significantly improve symptom management.
It’s important to note that food sensitivities are highly individual. Keeping a food diary can help identify personal triggers.
- Dairy products (milk, cheese, ice cream): Lactose intolerance is common in IBS and can lead to both diarrhea and gas.
- High-FODMAP foods (onions, garlic, wheat, beans, apples): These are fermentable carbohydrates that can exacerbate IBS symptoms.
- Processed foods, fried foods, and excessive amounts of fat: These can slow down digestion and worsen constipation.
- Highly caffeinated beverages (coffee, tea, soda): These can stimulate bowel movements and worsen diarrhea.
- Alcohol: This can irritate the digestive system and contribute to both constipation and diarrhea.
- Artificial sweeteners: Some individuals experience digestive issues with certain artificial sweeteners.
Hydration and IBS Management
Adequate hydration is crucial for regular bowel movements and overall digestive health. Dehydration can worsen constipation, while sufficient water intake helps to soften stools and prevent constipation and diarrhea.
Aim for at least 8 glasses (64 ounces) of water per day. You may need more depending on activity level, climate, and other factors.
The Role of Probiotics and Prebiotics
Probiotics are live microorganisms (bacteria) that, when consumed in adequate amounts, confer a health benefit. Prebiotics are non-digestible food ingredients that promote the growth of beneficial bacteria in the gut. Both can play a significant role in improving gut health and managing IBS symptoms.
So, IBS can be a real rollercoaster – one day constipation, the next diarrhoea! It’s all about the gut’s messed-up communication. Managing it often involves dietary changes, and understanding that can be tricky, especially since, as this article points out, are women and men receptive of different types of food and game changing superfoods for women , influencing what works best for individual IBS management.
Finding the right diet, combined with stress management and potentially medication, is key to navigating this unpredictable condition.
Probiotics may help restore the balance of gut microbiota, reducing inflammation and improving symptoms. Prebiotics provide nourishment for beneficial bacteria already present in the gut. Many foods naturally contain prebiotics (such as bananas, onions, garlic – although these should be consumed cautiously in IBS due to potential high-FODMAP content).
Lifestyle Modifications for IBS Symptom Relief
Source: askthenurseexpert.com
Living with IBS can feel like navigating a minefield, but thankfully, lifestyle changes can significantly impact symptom management. Beyond diet, focusing on movement, stress reduction, sleep hygiene, and addressing potential allergies or intolerances can make a world of difference in your overall well-being and IBS control. These changes aren’t quick fixes, but consistent effort can lead to lasting improvements.
Regular Physical Activity and IBS
Regular physical activity offers numerous benefits for IBS sufferers, going beyond general health improvements. Exercise stimulates gut motility, helping to regulate bowel movements and reduce both constipation and diarrhea. It also helps to reduce stress, a major IBS trigger. Aim for at least 150 minutes of moderate-intensity aerobic activity per week, such as brisk walking, swimming, or cycling.
Incorporating strength training twice a week can also be beneficial for overall health and potentially gut function. Gentle exercises like yoga and Pilates, which focus on mindful movement and breathing, can be particularly helpful in managing stress and improving gut motility.
Stress Management Techniques for IBS
Stress significantly exacerbates IBS symptoms. Chronic stress can disrupt the gut-brain axis, leading to increased inflammation and altered bowel function. Mindfulness practices, such as yoga and meditation, have been shown to be effective in reducing stress and improving IBS symptoms. Yoga, with its combination of physical postures, breathing techniques, and meditation, can promote relaxation and reduce visceral hypersensitivity, a common feature of IBS.
Meditation, focusing on deep breathing and present moment awareness, can help calm the nervous system and reduce stress-induced gut issues. Regular practice, even for short periods (10-15 minutes daily), can lead to noticeable improvements.
Maintaining a Regular Sleep Schedule for Gut Health
Sleep deprivation negatively impacts gut health and worsens IBS symptoms. Aim for 7-9 hours of quality sleep per night. A consistent sleep schedule, even on weekends, helps regulate your body’s natural circadian rhythm, which influences gut motility and hormone production. Establishing a relaxing bedtime routine, such as taking a warm bath, reading a book, or listening to calming music, can signal to your body that it’s time to wind down.
Creating a dark, quiet, and cool sleep environment will also contribute to better sleep quality. If you struggle with insomnia, consult your doctor or a sleep specialist to rule out underlying medical conditions and explore potential treatment options.
Identifying and Managing Food Intolerances or Allergies
Food intolerances and allergies can significantly worsen IBS symptoms. Common triggers include dairy, gluten, fructose, and certain other foods. Keeping a detailed food diary can help identify potential triggers by tracking your diet and symptoms. Working with a registered dietitian or gastroenterologist can help develop an elimination diet to pinpoint specific triggers and develop a personalized management plan.
While completely eliminating all potential triggers may not be necessary, reducing consumption of identified problem foods can substantially alleviate IBS symptoms. It’s important to note that eliminating food groups should be done under professional guidance to ensure nutritional adequacy.
So, IBS can be a real rollercoaster – one day you’re constipated, the next you’re rushing to the bathroom! It’s all about the gut’s inconsistent muscle contractions. Managing it often involves dietary changes and stress reduction. Interestingly, understanding the complexities of managing chronic conditions like IBS can shed light on other neurological challenges; for instance, learning about effective strategies for managing a child’s Tourette Syndrome, like those outlined in this helpful article: strategies to manage tourette syndrome in children , highlights the importance of tailored approaches and consistent support.
Returning to IBS, finding the right balance of fiber and fluids, alongside stress management techniques, is key to finding some relief.
Medical Management of IBS
Managing Irritable Bowel Syndrome (IBS) often involves a multi-pronged approach, and medication plays a significant role for many individuals. While lifestyle changes and dietary adjustments form the cornerstone of IBS management, medications can help alleviate specific symptoms and improve overall quality of life. It’s crucial to remember that medication is most effective when used in conjunction with other management strategies.
Pharmacological Interventions for IBS
Several medications are available to target the diverse symptoms of IBS. These medications work through different mechanisms, addressing either diarrhea or constipation, or focusing on pain relief. Choosing the right medication depends on the individual’s specific IBS subtype (IBS-C or IBS-D) and the predominant symptoms.
| Medication Type | Mechanism of Action | Use in IBS-C/IBS-D | Common Side Effects |
|---|---|---|---|
| Antispasmodics (e.g., hyoscyamine, dicyclomine) | Reduce intestinal muscle spasms, relieving abdominal pain and cramping. | Both IBS-C and IBS-D | Dry mouth, blurred vision, constipation (especially with IBS-D), drowsiness. |
| Antidiarrheals (e.g., loperamide) | Slows down bowel movements by affecting the gut’s motility. | IBS-D | Constipation, drowsiness, nausea. |
| Laxatives (e.g., polyethylene glycol, lubiprostone) | Increase stool frequency and soften stool consistency. Different types work through different mechanisms (osmotic, stimulant, lubricant). | IBS-C | Abdominal bloating, cramping (especially with stimulant laxatives), dehydration (with osmotic laxatives). |
| Antidepressants (e.g., tricyclic antidepressants, selective serotonin reuptake inhibitors) | Affect neurotransmitters in the gut, reducing pain perception and improving bowel function. Low doses are typically used. | Both IBS-C and IBS-D | Drowsiness, dry mouth, constipation, weight gain (variable depending on the specific antidepressant). |
| Rifaximin | A non-absorbable antibiotic that may alter the gut microbiota, reducing symptoms in some individuals. | IBS-D with diarrhea-predominant symptoms | Generally well-tolerated, but mild nausea and headache may occur. |
The Role of Psychological Therapies
Psychological factors significantly impact IBS symptoms. Stress, anxiety, and depression can exacerbate IBS symptoms, leading to a vicious cycle of pain, discomfort, and emotional distress. Cognitive Behavioral Therapy (CBT) is a highly effective psychological therapy for IBS. CBT helps individuals identify and modify negative thought patterns and behaviors that contribute to their IBS symptoms. Techniques such as relaxation exercises, stress management strategies, and dietary habit modification are integrated into CBT to address the interplay between psychological and physiological factors in IBS.
For instance, a patient learning to manage stress through mindfulness techniques might experience a reduction in IBS-related abdominal pain and discomfort.
So, IBS can be a real rollercoaster – one day constipation, the next diarrhoea! It’s all about the gut’s messed-up communication. Managing it involves diet changes, stress reduction, and sometimes medication. Interestingly, while researching gut health, I stumbled upon this fascinating article about how an eye test might predict dementia risk – can eye test detect dementia risk in older adults – which got me thinking about the connections between different body systems.
Anyway, back to IBS, finding the right management strategy is key to a more comfortable life.
Integrated Management of IBS Symptoms, How can ibs cause both constipation and diarrhoea and management measures
Effective IBS management relies on a holistic approach that combines dietary changes, lifestyle modifications, and, when necessary, medication. For example, a patient with IBS-C might benefit from increased fiber intake, regular exercise, stress management techniques, and the use of a mild osmotic laxative as needed. Similarly, a patient with IBS-D might find relief through a low-FODMAP diet, stress reduction strategies, and the use of an antidiarrheal medication for acute episodes.
This integrated approach allows for targeted symptom relief while addressing the underlying factors contributing to IBS.
Importance of Regular Follow-Up
Regular follow-up appointments with a healthcare professional are crucial for ongoing IBS management. These appointments allow for monitoring of symptom control, medication effectiveness, and adjustment of treatment plans as needed. It also provides an opportunity to discuss any new symptoms or concerns, ensuring the management strategy remains appropriate and effective over time. This ongoing communication is vital for optimizing treatment and maintaining a good quality of life.
Illustrative Examples of IBS Management
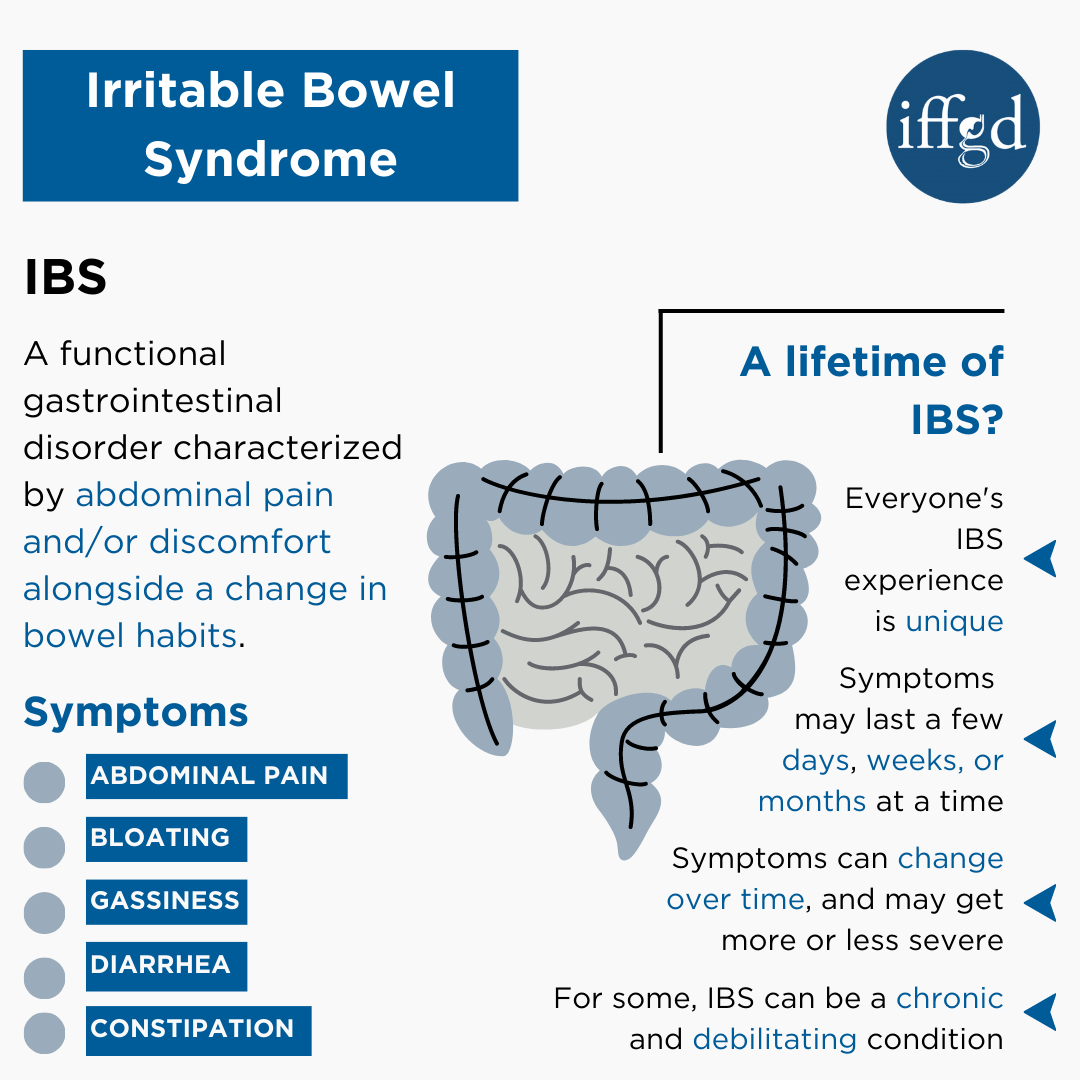
Source: aboutibs.org
Successfully managing Irritable Bowel Syndrome (IBS) requires a holistic approach, tailoring treatment to the individual’s specific symptoms and needs. This often involves a combination of dietary changes, lifestyle adjustments, and, in some cases, medication. The following examples illustrate how a multi-faceted approach can lead to significant improvements in IBS symptoms.
Case Study: Successful Management of Mixed IBS Symptoms
Sarah, a 32-year-old woman, presented with a history of fluctuating bowel habits characterized by both constipation and diarrhea, abdominal pain, and bloating for the past five years. Her symptoms significantly impacted her quality of life, affecting her work and social interactions. Initial assessment revealed a diagnosis of mixed IBS. Her treatment plan involved several key components. First, a low FODMAP diet was implemented to identify and eliminate trigger foods.
This was coupled with regular exercise, including daily 30-minute walks, and stress-reduction techniques such as mindfulness meditation (practiced for 15 minutes daily). After four weeks, Sarah experienced a noticeable reduction in bloating and abdominal pain. However, constipation persisted. Her physician then introduced a fiber supplement, psyllium husk, to promote regular bowel movements. After eight weeks, Sarah reported significant improvement in both constipation and diarrhea, experiencing regular, comfortable bowel movements.
She also reported a reduction in stress levels and improved overall well-being. This demonstrates how a combination of dietary modifications, lifestyle changes, and medication can effectively manage even the most challenging IBS symptoms.
Infographic: The Interplay of Diet, Lifestyle, and Medication in IBS Management
This infographic would visually represent the interconnectedness of dietary choices, lifestyle factors, and medication in managing IBS. A central image could depict a balanced scale representing symptom control. On one side of the scale, we would see icons representing potential IBS triggers: high FODMAP foods (e.g., onions, garlic, wheat), processed foods, caffeine, alcohol, and stress. The other side of the scale would showcase positive influences: low FODMAP foods (e.g., rice, quinoa, carrots), regular exercise, stress-management techniques (yoga, meditation), and medications (e.g., antispasmodics, fiber supplements, antidepressants).
Arrows would connect these elements, demonstrating how dietary changes, lifestyle modifications, and medications can all contribute to achieving a balance and reducing IBS symptoms. The infographic could include brief descriptions of each element and their impact on IBS, highlighting the importance of a holistic approach. For instance, a section on diet could explain the benefits of a low FODMAP diet and provide examples of suitable foods.
The lifestyle section could emphasize the role of regular physical activity and stress reduction techniques, and the medication section would list common IBS medications and their mechanisms of action. Finally, a small section could illustrate how the combination of these elements creates a synergistic effect, leading to better symptom control and an improved quality of life for individuals with IBS.
Last Point
Living with IBS, particularly the mixed type, can feel like an uphill battle. But remember, you’re not alone, and effective management is absolutely possible. By understanding the underlying mechanisms of IBS and adopting a holistic approach encompassing dietary adjustments, lifestyle modifications, and when necessary, medical interventions, you can significantly improve your quality of life. This journey requires patience, self-awareness, and potentially, professional guidance.
Don’t hesitate to reach out to your doctor or a registered dietitian to create a personalized plan that addresses your specific needs. The path to better gut health is achievable – one step, one mindful meal, one stress-reducing technique at a time.
FAQs
What are some common food triggers for both constipation and diarrhea in IBS?
Common triggers vary by individual, but frequently include dairy products (lactose intolerance), gluten (for those with gluten sensitivity), high-FODMAP foods (fructose, lactose, etc.), and highly processed foods. Keeping a food diary can help identify your personal triggers.
How long does it typically take to see improvement after implementing IBS management strategies?
This varies greatly depending on the individual and the severity of their symptoms. Some people see improvements within weeks, while others may require several months to experience significant relief. Consistency with the chosen management plan is key.
Is there a specific test to diagnose mixed IBS?
There isn’t one definitive test. Diagnosis usually involves a combination of symptom evaluation, physical examination, and possibly stool tests to rule out other conditions. A gastroenterologist can help determine the most appropriate course of action.