How Focused Ultrasound Can Help in Tremors and Epilepsy
How focused ultrasound can help in tremors and epilepsy? It sounds like science fiction, right? But this non-invasive technology is making real waves in the treatment of these debilitating conditions. Imagine a future where tremors are significantly reduced and epileptic seizures are better managed, all without major surgery. This is the promise of focused ultrasound, a breakthrough that’s changing the landscape of neurological treatments.
Let’s delve into how this fascinating technology works its magic.
Focused ultrasound (FUS) uses high-intensity sound waves to precisely target specific areas of the brain. Unlike traditional surgery, it’s non-invasive, meaning there are no scalp incisions or large incisions. This precision allows doctors to treat the underlying cause of tremors and seizures without damaging surrounding healthy tissue. This post will explore the science behind FUS, its applications in treating tremors and epilepsy, and what the future holds for this revolutionary technology.
Introduction to Focused Ultrasound (FUS)
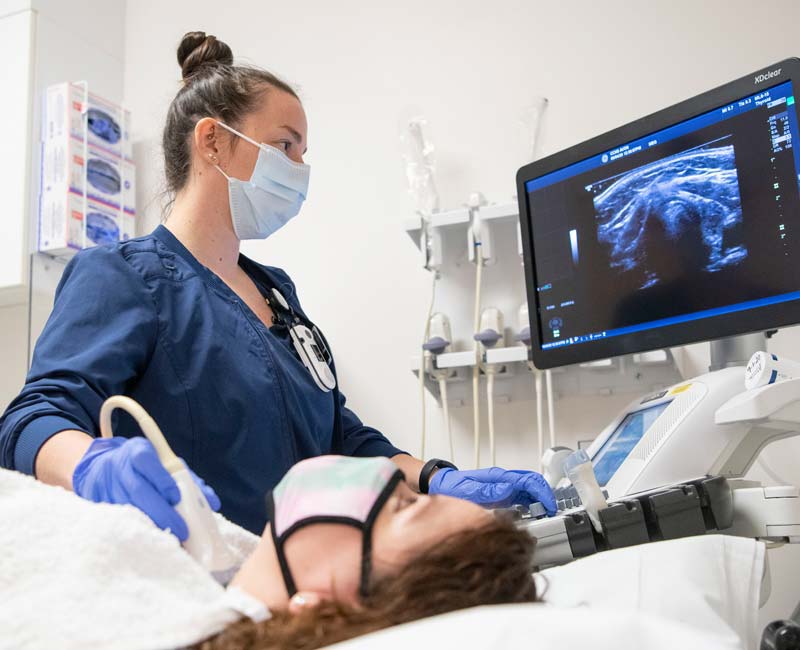
Source: clevelandclinic.org
Focused ultrasound (FUS) is a non-invasive therapeutic technique that uses high-frequency sound waves to precisely target and heat specific areas of the body. Unlike surgery, it doesn’t require incisions or general anesthesia, making it a less invasive alternative for treating various medical conditions. In the context of neurological disorders like tremors and epilepsy, FUS offers a promising approach by targeting specific brain regions responsible for these symptoms.The mechanism of FUS involves the use of a transducer array that focuses multiple ultrasound beams onto a small, predetermined target within the brain.
The focused energy causes a localized increase in temperature, leading to either the ablation (destruction) of targeted tissue or, more subtly, changes in neuronal activity. This precise targeting minimizes damage to surrounding healthy tissue, a significant advantage over more invasive surgical procedures. The interaction with brain tissue is highly dependent on the parameters of the ultrasound, such as the intensity, frequency, and duration of the sonication.
Careful planning and monitoring are crucial to ensure accurate targeting and avoid unintended consequences.
Advantages and Limitations of FUS Compared to Other Tremor and Epilepsy Treatments
FUS offers several advantages over traditional treatments for tremors and epilepsy. Compared to surgery, it is significantly less invasive, resulting in shorter recovery times and reduced risk of complications like infection or bleeding. Unlike medications, which can have systemic side effects, FUS’s effects are highly localized, minimizing the potential for adverse reactions throughout the body. Deep brain stimulation (DBS), another established treatment for these conditions, requires implantation of electrodes, a procedure that carries its own risks.
FUS offers a potential alternative that avoids this invasive step.However, FUS also has limitations. It is not suitable for all patients, and careful patient selection is crucial. The procedure requires precise targeting and sophisticated imaging techniques, making it technically challenging and potentially expensive. Furthermore, the long-term effects of FUS on brain tissue are still under investigation, and ongoing monitoring is necessary.
Not all tremor or epilepsy types are currently treatable with FUS, and research continues to expand its applicability.
History of FUS Application in Neurological Disorders
The application of FUS in neurological disorders is a relatively recent development, though the technology itself has been around for some time. Early research focused on the use of FUS for non-invasive brain surgery, and initial clinical trials explored its potential for treating essential tremor. Successful results in these early trials paved the way for further investigation into its use for other neurological conditions, including epilepsy.
Over the past two decades, there has been a significant increase in clinical trials and research studies exploring the efficacy and safety of FUS for treating various neurological disorders, with promising results emerging for specific tremor and epilepsy subtypes. The development of more sophisticated imaging techniques and improved FUS systems has significantly contributed to the increased precision and safety of the procedure, further enhancing its potential as a valuable therapeutic tool.
FUS in Tremor Treatment
Focused ultrasound (FUS) is emerging as a promising non-invasive treatment option for various types of tremors, offering a potential alternative to medications and more invasive surgical procedures. This technology uses high-intensity focused ultrasound waves to precisely target and ablate specific areas of the brain responsible for tremor generation, leading to a reduction in tremor severity.
Types of Tremors Treatable with FUS
FUS is primarily used to treat essential tremor, the most common type of tremor affecting millions worldwide. It’s characterized by rhythmic shaking that typically affects the hands, but can also involve the head, voice, and other body parts. While less common, FUS has also shown some promise in treating other types of tremors, though further research is needed to establish its efficacy in these cases.
These include tremors associated with Parkinson’s disease and some forms of dystonia. However, the selection criteria for these less common tremor types are more stringent and often require a more individualized approach.
Comparison of FUS with Other Essential Tremor Treatments
Essential tremor is often managed with medications, such as beta-blockers or primidone. These medications can be effective for some individuals, but they may not provide complete relief and can have side effects. For individuals who don’t respond well to medication or who experience intolerable side effects, surgery, such as deep brain stimulation (DBS), may be considered. DBS involves implanting electrodes into the brain, which requires a major surgical procedure with associated risks.
FUS offers a less invasive alternative, avoiding the need for brain surgery and its associated risks. While DBS often provides more significant tremor reduction, FUS offers a less invasive and potentially more tolerable approach for carefully selected patients. The choice between these options depends on individual patient factors, including tremor severity, overall health, and personal preferences.
FUS Procedure for Tremor Treatment: Patient Selection and Post-Treatment Care
The FUS procedure for tremor treatment involves using MRI guidance to precisely target the ventral intermediate nucleus (VIM) of the thalamus, a brain region implicated in tremor generation. High-intensity focused ultrasound waves are then directed at the target area, causing localized tissue ablation. Patient selection is crucial and typically involves a thorough neurological evaluation, including tremor assessment, MRI scans, and cognitive testing.
Patients must meet specific criteria, including the severity and location of their tremor, their overall health status, and their understanding of the procedure and its potential risks and benefits. Post-treatment care typically involves monitoring for any side effects and gradual adjustment of medication, if necessary. Patients may experience some temporary side effects, such as headaches or dizziness, but these usually resolve within a few days.
Regular follow-up appointments are essential to assess the long-term effectiveness of the treatment and to address any potential complications.
Comparison of Tremor Treatment Methods
| Treatment Method | Effectiveness | Side Effects | Invasiveness |
|---|---|---|---|
| Medication (e.g., Beta-blockers) | Variable; may not provide complete relief | Fatigue, dizziness, nausea, etc. | Non-invasive |
| Deep Brain Stimulation (DBS) | Generally high; significant tremor reduction | Infection, bleeding, hardware malfunction | Highly invasive (brain surgery) |
| Focused Ultrasound (FUS) | Moderate to high; less effective than DBS in some cases | Headache, dizziness, temporary weakness | Minimally invasive (non-surgical) |
FUS in Epilepsy Treatment: How Focused Ultrasound Can Help In Tremors And Epilepsy
Focused ultrasound (FUS) is emerging as a promising non-invasive treatment modality for drug-resistant epilepsy. Unlike traditional surgical approaches, FUS offers a targeted and precise method to disrupt abnormal neuronal activity responsible for seizures, minimizing damage to surrounding healthy brain tissue. This targeted approach is particularly beneficial for patients who are not suitable candidates for traditional epilepsy surgery.
FUS works by delivering highly focused ultrasound energy to specific brain regions implicated in seizure generation. This energy causes a localized increase in temperature, leading to the disruption of neural pathways involved in seizure propagation. The procedure is guided by real-time imaging, ensuring accuracy and minimizing risks. Importantly, FUS offers a minimally invasive alternative, potentially reducing recovery time and associated complications compared to open brain surgery.
Types of Epilepsy Suitable for FUS Treatment
Several types of epilepsy may benefit from FUS treatment. The ideal candidates often have focal epilepsy, where seizures originate from a specific area of the brain. This localized nature makes them particularly suitable for targeted therapies like FUS. Epilepsy syndromes involving the thalamus or hippocampus, brain regions often implicated in seizure generation, are also potential candidates. However, the suitability of FUS for each individual case is determined through careful evaluation, including detailed neurological examinations, advanced brain imaging (MRI, EEG), and consideration of the patient’s overall health and seizure characteristics.
Not all epilepsy patients are suitable candidates for FUS.
Targeting Specific Brain Regions with FUS, How focused ultrasound can help in tremors and epilepsy
The precise targeting of brain regions involved in seizure generation is crucial for the success of FUS treatment. Advanced neuroimaging techniques, such as high-resolution MRI and EEG, are used to identify the epileptogenic zone – the area of the brain responsible for initiating seizures. This information is then used to precisely guide the FUS energy delivery. The process involves meticulous planning and real-time monitoring to ensure the targeted area receives the appropriate amount of energy while minimizing the impact on surrounding healthy tissue.
The goal is to disrupt the abnormal neuronal activity within the epileptogenic zone without causing significant damage to adjacent brain structures.
Clinical Trials and Studies Demonstrating FUS Efficacy in Epilepsy Management
While still a relatively new treatment, several clinical trials and studies have explored the efficacy of FUS in epilepsy management. These studies have shown promising results in reducing seizure frequency and improving quality of life for some patients with drug-resistant epilepsy. For example, studies have investigated the use of FUS to target specific thalamic nuclei associated with absence seizures, with some showing significant reduction in seizure frequency post-treatment.
Other studies have explored the application of FUS to the hippocampus in patients with temporal lobe epilepsy. While results are variable and further research is needed, these studies provide encouraging evidence of FUS’s potential as a valuable treatment option for carefully selected patients. It’s important to note that the long-term efficacy and safety of FUS in epilepsy require further investigation through larger, long-term clinical trials.
Decision-Making Flowchart for FUS Treatment Selection in Epilepsy
A flowchart would visually represent the decision-making process. It would start with a patient presenting with drug-resistant epilepsy. The next step would involve a comprehensive evaluation including neurological examination, detailed seizure history, advanced brain imaging (MRI and EEG), and assessment of patient suitability for FUS based on location and size of epileptogenic zone, overall health, and other factors.
The flowchart would then branch into either proceeding with FUS treatment after a multidisciplinary team discussion or exploring alternative treatment options if FUS is deemed unsuitable. Following FUS treatment, the flowchart would depict ongoing monitoring and assessment of treatment efficacy and potential side effects. This detailed process ensures that FUS is only considered for appropriate candidates and that the treatment is administered safely and effectively.
Mechanisms of Action in Tremors and Epilepsy
Focused ultrasound (FUS) offers a non-invasive way to treat neurological disorders like tremors and epilepsy by precisely targeting specific brain regions. Its effectiveness stems from its ability to alter neuronal activity without the need for surgery, offering a potentially less invasive alternative to traditional treatments. Understanding the mechanisms by which FUS achieves this is crucial for optimizing its therapeutic application and expanding its use in various neurological conditions.
The precise mechanisms of FUS in treating tremors and epilepsy are still being actively researched, but several key pathways are emerging. Essentially, FUS uses focused ultrasound waves to heat targeted tissue, causing changes in the neuronal environment that ultimately modulate neuronal excitability and synaptic transmission. This targeted disruption can lead to a reduction in tremor severity or seizure frequency depending on the targeted brain area.
FUS’s Impact on Neuronal Activity in Tremors
FUS treatment for tremor typically targets the ventral intermediate nucleus (VIM) of the thalamus, a key relay station in the motor pathway. Heating this region, even subtly, disrupts the abnormal neuronal activity associated with tremor. This disruption may involve several mechanisms: direct thermal ablation of overactive neurons, alteration of synaptic connections, or modulation of neurotransmitter release. The result is a dampening of the tremor signal, leading to reduced tremor severity.
For example, studies have shown that FUS-induced lesions in the VIM can significantly reduce the amplitude and frequency of essential tremor. The precise cellular mechanisms underlying this effect are still under investigation, but the overall effect is a reduction in the aberrant neural signaling driving the tremor.
FUS’s Influence on Seizure Activity
In epilepsy, FUS treatment targets different brain regions depending on the type and location of seizures. Common targets include the hippocampus, amygdala, or cortical areas known to be seizure foci. The mechanisms by which FUS affects seizure activity are multifaceted and likely include similar mechanisms to those seen in tremor treatment, but with different consequences. By precisely heating these regions, FUS can disrupt the hyperexcitable neural networks that contribute to seizure initiation and propagation.
This disruption can involve changes in neuronal excitability, synaptic plasticity, or the modulation of neurotransmitter systems involved in seizure generation, such as GABAergic inhibition. For instance, studies are exploring the use of FUS to target epileptogenic zones in patients with medically refractory epilepsy, aiming to reduce seizure frequency and severity.
Comparison of Targeted Neural Pathways
While both tremor and epilepsy treatments utilize FUS to modulate neuronal activity, the targeted brain regions differ significantly. Tremor treatment primarily focuses on the thalamus (specifically the VIM), a key structure in motor control. Conversely, epilepsy treatment targets various regions depending on the seizure type and location, including the hippocampus, amygdala, and cortical areas. This difference reflects the distinct neural circuits involved in generating tremors and seizures.
In essence, FUS offers a targeted approach that can be adapted to the specific neural pathways implicated in each disorder.
Mechanisms of Action: A Summary
The following points summarize the known and hypothesized mechanisms of action for FUS in treating tremors and epilepsy:
- Thermal Ablation: Direct destruction of overactive neurons through targeted heating.
- Synaptic Modulation: Alteration of synaptic connections and neurotransmitter release.
- Neurotransmitter Modulation: Changes in the levels or activity of neurotransmitters, such as GABA, which influence neuronal excitability.
- Disruption of Aberrant Neural Networks: Interruption of the hyperexcitable networks responsible for tremors and seizures.
- Changes in Neuronal Excitability: Direct alteration of the threshold for neuronal firing.
Safety and Side Effects of FUS
Focused ultrasound (FUS) is a relatively new and minimally invasive treatment option for neurological conditions like tremors and epilepsy, but like any medical procedure, it carries potential risks and side effects. Understanding these potential complications is crucial for both patients and clinicians to make informed decisions about treatment. This section will explore the safety profile of FUS, discuss strategies to mitigate risks, and provide a summary of reported side effects.
While FUS is generally considered safe, it’s essential to remember that individual responses can vary. The potential for complications is dependent on several factors, including the specific target area, the patient’s overall health, and the expertise of the medical team performing the procedure. Careful pre-operative evaluation and meticulous execution of the procedure are key to minimizing risks.
Potential Side Effects of FUS
Potential side effects of FUS treatment for tremors and epilepsy can range from minor and temporary to more serious and long-lasting. These side effects are not always experienced by every patient, and their severity can vary considerably. The most commonly reported side effects are related to the localized heating effect of the ultrasound energy on the targeted brain region.
Minimizing the Risk of Complications
Several strategies are employed to minimize the risk of complications during and after FUS procedures. These include rigorous pre-operative assessment to identify patients who may be at higher risk, advanced imaging techniques (like MRI) for precise targeting of the treatment area, real-time monitoring during the procedure to ensure accurate energy delivery, and a comprehensive post-operative care plan to manage any potential side effects.
The use of ultrasound thermometry allows for real-time temperature monitoring, providing a crucial safety check during the procedure. This ensures the targeted area receives the appropriate amount of energy without causing damage to surrounding tissues.
Long-Term Safety Profile of FUS
The long-term safety profile of FUS in neurological applications is still being actively investigated, but the available data suggests a favorable outcome for most patients. Long-term follow-up studies are essential to fully understand the long-term effects and potential late-onset complications. Currently, the majority of reported side effects are temporary and resolve within a few weeks or months post-procedure.
However, ongoing research is crucial to monitor for any rare or delayed complications.
Summary of Reported Side Effects
The frequency of side effects varies significantly depending on the target area, the specific condition being treated, and the expertise of the medical team. The following table provides a general overview of reported side effects and their estimated frequency. Note that these frequencies are based on available clinical trial data and may not be representative of all patients.
| Side Effect | Frequency (Tremors) | Frequency (Epilepsy) | Severity |
|---|---|---|---|
| Headache | Common (20-40%) | Common (15-30%) | Mild to Moderate, usually transient |
| Hearing Loss (Temporary) | Rare (<5%) | Rare (<2%) | Usually resolves spontaneously |
| Facial Weakness | Rare (<2%) | Rare (<1%) | May require rehabilitation |
| Cognitive Changes (Mild) | Uncommon (5-10%) | Uncommon (3-7%) | Usually transient |
Future Directions and Research
The field of focused ultrasound (FUS) is rapidly evolving, with ongoing research pushing the boundaries of its therapeutic applications in neurological disorders beyond tremors and epilepsy. Exciting advancements are being made in both refining existing techniques and exploring entirely new avenues for treatment. This ongoing research holds immense promise for improving the lives of countless individuals suffering from debilitating neurological conditions.Current research efforts are actively exploring the use of FUS in a wide range of neurological disorders.
This includes investigating its potential in treating conditions like essential tremor, Parkinson’s disease, Alzheimer’s disease, multiple sclerosis, and even brain tumors. The versatility of FUS, its non-invasive nature, and its potential for targeted therapy are driving this expansion into new therapeutic areas.
Ongoing Clinical Trials and New Applications of FUS Technology
Many clinical trials are currently underway investigating the efficacy and safety of FUS in various neurological conditions. For example, several studies are exploring the use of FUS to modulate specific brain regions implicated in Parkinson’s disease, aiming to alleviate motor symptoms such as rigidity and bradykinesia. Other trials are investigating the potential of FUS to stimulate neurogenesis (the growth of new neurons) in patients with Alzheimer’s disease, potentially slowing disease progression.
Furthermore, research is exploring the use of FUS in combination with other therapies, such as drug delivery, to enhance treatment outcomes. These trials are providing valuable data on the effectiveness, safety, and potential limitations of FUS in a wider range of neurological disorders.
Improving FUS Technology for Enhanced Treatment Outcomes and Reduced Side Effects
Significant efforts are focused on enhancing FUS technology to improve treatment outcomes and minimize side effects. Researchers are developing more sophisticated imaging techniques to improve targeting accuracy, reducing the risk of unintended damage to surrounding tissues. Advances in transducer design are leading to more precise energy delivery, allowing for more focused treatment and minimizing off-target effects. Furthermore, research is exploring the use of real-time monitoring techniques during FUS treatment to ensure optimal energy delivery and detect any potential adverse events immediately.
These technological advancements are paving the way for safer and more effective FUS treatments.
Illustrative Image: The Future of FUS in Neurological Disorders
Imagine a futuristic image depicting a patient comfortably seated in a chair, undergoing a non-invasive FUS treatment. A sophisticated, sleek machine emits focused ultrasound waves, precisely targeted to a specific region of the brain, visualized in real-time through a high-resolution 3D brain scan displayed on a nearby monitor. The scan shows a vibrant, healthy brain with the targeted area highlighted in a soft, calming blue, indicating successful modulation of neural activity.
Surrounding the patient, a team of medical professionals monitors the treatment meticulously, ensuring optimal energy delivery and patient safety. The overall image conveys a sense of hope, technological advancement, and the potential for revolutionizing neurological care. This image represents a future where FUS is a routine and effective treatment for a wide array of neurological disorders, significantly improving the quality of life for countless individuals.
Closure
Source: ausmed.com
Focused ultrasound presents a compelling new frontier in the treatment of tremors and epilepsy. Its non-invasive nature, precision targeting, and potential for minimizing side effects offer a significant advantage over traditional methods. While still a relatively new approach, the ongoing research and clinical trials are incredibly promising. The future of FUS looks bright, with the potential to expand its applications to other neurological disorders and further improve the quality of life for countless individuals.
The journey into the world of FUS is just beginning, and the possibilities are truly exciting.
Questions Often Asked
What are the risks associated with Focused Ultrasound?
While generally safe, potential side effects can include headache, temporary dizziness, and rarely, more serious complications. These risks are carefully weighed against the potential benefits and are minimized through rigorous pre-procedure assessments and skilled clinicians.
Is Focused Ultrasound covered by insurance?
Insurance coverage for FUS varies depending on the specific condition, location, and insurance provider. It’s essential to check with your insurance company beforehand to understand your coverage options.
How long does the Focused Ultrasound procedure take?
The procedure time can vary but typically ranges from a few hours. The exact duration depends on the target area and the complexity of the treatment.
How long is the recovery time after Focused Ultrasound?
Recovery time is generally short, with most patients able to return home the same day or the following day. However, individual recovery times may vary.
