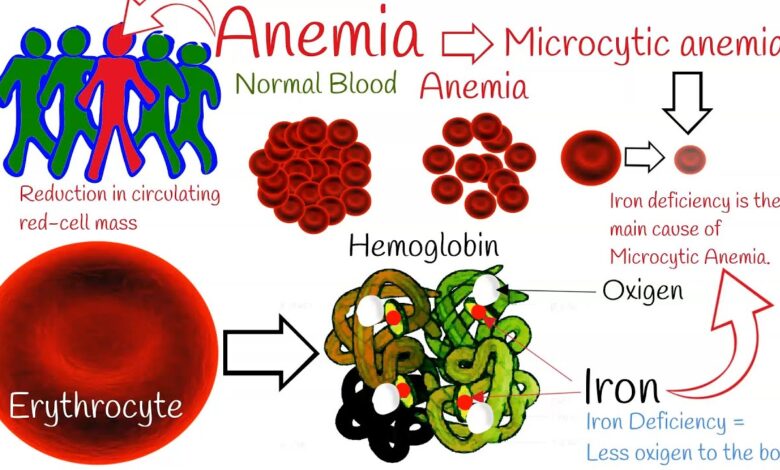
Iron Deficiency Not the Root of Indias Anemia Problem
Iron deficiency not the root cause of anaemia in india study tips to reduce the risk – Iron deficiency not the root cause of anaemia in India: study tips to reduce the risk – that’s a bold statement, right? We often hear about iron supplements as the solution to anaemia, but a closer look at India reveals a much more complex picture. This isn’t just about iron; it’s about a tangled web of nutritional deficiencies, infections, genetics, and lifestyle factors all contributing to this widespread health issue.
Let’s unravel this mystery and explore what we can do to tackle anaemia effectively.
Anemia, a condition characterized by a deficiency of red blood cells or hemoglobin, affects a staggering number of people in India. While iron deficiency plays a role, it’s often not the sole culprit. Malnutrition, particularly deficiencies in folate and vitamin B12, are significant contributors. Infectious diseases like malaria and hookworm infestations wreak havoc on red blood cell production.
Genetic factors, such as thalassemia, also play a significant part. Understanding these diverse causes is crucial for developing effective prevention and treatment strategies.
Prevalence of Anemia in India
Anemia, a condition characterized by a deficiency of red blood cells or hemoglobin, remains a significant public health challenge in India. While iron deficiency is a major contributor, a complex interplay of factors contributes to the overall high prevalence, making it crucial to understand the broader picture beyond simply focusing on iron supplementation. This necessitates a deeper dive into the various underlying causes to develop effective and targeted interventions.
Prevalence of Anemia in India and its Diverse Etiologies
The National Family Health Survey (NFHS) data consistently reveals a high prevalence of anemia across various age groups in India. NFHS-5 (2019-21) reported that nearly 57% of women aged 15-49 years and 59% of children aged 6-59 months were anemic. These figures highlight the widespread nature of the problem and the urgent need for comprehensive strategies to address its root causes.
Beyond iron deficiency, several other factors significantly contribute to anemia’s prevalence in the country. These include nutritional deficiencies (folate and vitamin B12), parasitic infections (malaria and hookworm), genetic disorders (like thalassemia), and chronic diseases (like kidney disease and cancer). Understanding the specific contribution of each factor is critical for designing effective public health interventions.
Nutritional Deficiencies Beyond Iron
Folate and vitamin B12 deficiencies are important contributors to anemia in India. Folate is essential for DNA synthesis and red blood cell production; its deficiency leads to megaloblastic anemia. Similarly, vitamin B12, crucial for the maturation of red blood cells, deficiency results in pernicious anemia. These deficiencies are often intertwined with poor dietary intake, particularly amongst populations with limited access to diverse and nutrient-rich foods.
The prevalence of these deficiencies is particularly high in pregnant women and young children, increasing their vulnerability to anemia.
Infections and Anemia
Infectious diseases, particularly malaria and hookworm infestations, are prevalent in many parts of India and significantly contribute to anemia. Malaria parasites destroy red blood cells, leading to anemia. Hookworms, intestinal parasites, cause chronic blood loss, resulting in iron deficiency anemia and other forms of anemia. The burden of these infections is often higher in impoverished communities with poor sanitation and hygiene, further exacerbating existing nutritional vulnerabilities.
Genetic Disorders and Chronic Diseases
Genetic disorders, such as thalassemia, a group of inherited blood disorders characterized by reduced or absent hemoglobin production, contribute significantly to anemia in India. Thalassemia is particularly prevalent in certain regions of the country. Furthermore, chronic diseases like kidney disease and cancer can also lead to anemia due to impaired red blood cell production or increased red blood cell destruction.
These conditions often require specialized medical care and management.
So, that recent study highlighting that iron deficiency isn’t the sole culprit behind anemia in India got me thinking about preventative health. It’s crucial to look at the bigger picture, and sometimes seemingly unrelated areas offer clues. For example, did you know that research suggests can eye test detect dementia risk in older adults ? This emphasizes the importance of comprehensive health checks, which are just as vital for preventing anemia by addressing underlying causes beyond iron levels.
Regular check-ups and a balanced diet remain key strategies to lower your risk.
Comparative Prevalence of Different Types of Anemia
While iron deficiency anemia is the most common type, it’s crucial to recognize the substantial contribution of other forms. Precise figures on the relative prevalence of different types of anemia in India are challenging to obtain due to limitations in nationwide diagnostic testing and data collection. However, studies suggest that a significant proportion of anemia cases are not solely attributable to iron deficiency.
| Type of Anemia | Potential Contributing Factors | Estimated Prevalence (Illustrative, not precise figures) | Notes |
|---|---|---|---|
| Iron Deficiency Anemia | Inadequate iron intake, poor absorption, blood loss | High (a significant majority of cases) | Often coexists with other deficiencies |
| Vitamin B12 Deficiency Anemia | Poor dietary intake, malabsorption | Moderate | More common in vegetarians and vegans |
| Folate Deficiency Anemia | Poor dietary intake, increased demand (pregnancy) | Moderate | Often overlaps with iron deficiency |
| Anemia of Chronic Disease | Kidney disease, cancer, infections | Moderate | Prevalence varies based on disease burden |
Impact of Dietary Habits on Anemia Risk
Anemia, a widespread health concern in India, is significantly influenced by dietary habits. While iron deficiency is a major contributor, understanding the complex interplay between diet and anemia requires looking beyond just iron intake. Factors like bioavailability of iron, consumption of inhibitors, and overall nutritional status play crucial roles. This section explores the impact of Indian dietary patterns on anemia risk.Dietary iron intake in India is often inadequate, especially among vulnerable populations like women and children.
Traditional diets, while rich in some nutrients, can lack sufficient bioavailable iron, leading to deficiencies. Furthermore, the prevalence of certain dietary deficiencies exacerbates the problem.
Dietary Deficiencies Contributing to Anemia in India
Several nutritional deficiencies commonly observed in India contribute to anemia. These include not only iron deficiency but also deficiencies in Vitamin B12, folate, and Vitamin C. Inadequate intake of these essential nutrients hampers the body’s ability to produce red blood cells effectively, worsening anemia. For example, a deficiency in Vitamin B12, often found in vegetarian diets lacking animal products, impairs DNA synthesis, crucial for red blood cell production.
Similarly, folate deficiency affects cell division and growth, hindering red blood cell formation. Vitamin C enhances iron absorption, so its deficiency further reduces the effectiveness of dietary iron.
Traditional Indian Diets and Iron Absorption
Many traditional Indian diets rely heavily on plant-based foods, which contain non-heme iron. Non-heme iron is less readily absorbed than heme iron (found in animal products). While foods like lentils, spinach, and rice are rich in iron, their bioavailability can be low due to the presence of phytates (found in grains and legumes) and polyphenols (found in tea and coffee), which inhibit iron absorption.
For example, consuming tea with a meal rich in iron can significantly reduce the amount of iron absorbed. Conversely, consuming iron-rich foods with Vitamin C-rich foods like citrus fruits or amla can enhance absorption.
Sample Meal Plan to Reduce Anemia Risk
A balanced diet rich in iron and other essential nutrients is crucial for preventing and managing anemia. The following sample meal plan incorporates foods rich in iron, Vitamin C, and other nutrients to enhance iron absorption and overall health. It’s important to note that this is a sample plan and individual needs may vary. Consult a doctor or registered dietitian for personalized dietary advice.
This meal plan focuses on increasing iron intake through diverse sources, while also ensuring sufficient Vitamin C and other nutrients crucial for optimal iron absorption and overall health. The inclusion of a variety of vegetables and fruits provides essential vitamins and minerals, further supporting healthy red blood cell production.
- Breakfast: Oatmeal with berries and a sprinkle of almonds. (Provides iron, fiber, and antioxidants)
- Mid-morning snack: A handful of raisins and a small orange. (Provides iron and Vitamin C)
- Lunch: Lentil soup with brown rice and a side salad with tomatoes and lemon juice. (Provides iron, fiber, and Vitamin C)
- Afternoon snack: A small bowl of chickpeas with a sprinkle of chopped cilantro. (Provides iron and other minerals)
- Dinner: Spinach and tofu curry with whole-wheat roti. (Provides iron and protein)
Infectious Diseases and Anemia

Source: healthjade.net
Anemia in India isn’t solely a nutritional deficiency; infectious diseases play a significant, often underestimated, role. Many common infections interfere with the body’s ability to produce or utilize red blood cells, leading to anemia. Understanding these infections and their mechanisms is crucial for developing effective public health strategies to combat anemia nationwide.Infections contribute to anemia through various pathways. Chronic inflammation, a common response to infection, can disrupt iron metabolism, making it harder for the body to absorb and utilize iron, even if sufficient iron is present in the diet.
Some infections directly damage bone marrow, the site of red blood cell production, reducing the number of red blood cells produced. Furthermore, certain infections cause blood loss, directly reducing red blood cell count. This complex interplay of factors highlights the importance of addressing infectious diseases as part of a comprehensive anemia control program.
Prevalent Infectious Diseases Contributing to Anemia in India
Several infectious diseases are highly prevalent in India and significantly contribute to anemia. These include malaria, hookworm infection, tuberculosis, and various other parasitic infections. The impact of these infections varies depending on factors such as the severity of the infection, the individual’s nutritional status, and access to healthcare. Addressing these infections is paramount to reducing the overall anemia burden.
Mechanisms by which Infections Cause Anemia
Malaria, caused byPlasmodium* parasites, leads to anemia through direct destruction of red blood cells by the parasite. Hookworm infections, caused by parasitic nematodes, result in chronic blood loss from the intestines. Tuberculosis (TB), a bacterial infection primarily affecting the lungs, induces chronic inflammation, which interferes with iron metabolism and red blood cell production. Many other parasitic infections, common in India, cause similar problems.
These infections create a vicious cycle; anemia weakens the immune system, making individuals more susceptible to further infections, which in turn worsen anemia.
Strategies for Preventing and Controlling Infectious Diseases to Reduce Anemia Risk
Effective prevention and control strategies for these infections are essential to reducing anemia. These include: improved sanitation and hygiene practices to reduce parasitic infections; widespread use of insecticide-treated bed nets and antimalarial drugs to control malaria; effective TB diagnosis and treatment programs; and improved access to clean water and nutritious food to bolster overall immune function. Public health initiatives focused on these areas will have a direct impact on reducing anemia prevalence.
| Infectious Disease | Mechanism of Anemia | Prevention Strategies | Control Strategies |
|---|---|---|---|
| Malaria | Direct destruction of red blood cells | Insecticide-treated bed nets, preventative medication | Early diagnosis and treatment with antimalarial drugs |
| Hookworm Infection | Chronic blood loss from intestines | Improved sanitation, regular deworming | Effective deworming programs, improved hygiene |
| Tuberculosis | Chronic inflammation, impaired iron metabolism | Vaccination (BCG), improved living conditions | Early diagnosis and treatment with anti-TB drugs |
| Other Parasitic Infections (e.g., schistosomiasis, strongyloidiasis) | Varying mechanisms, often involving blood loss or inflammation | Improved sanitation, hygiene, access to clean water | Targeted deworming programs, improved sanitation infrastructure |
Genetic Factors and Anemia
Source: ytimg.com
Anemia, characterized by a deficiency of red blood cells or hemoglobin, isn’t solely a nutritional issue. Genetic predisposition plays a significant role, particularly in India where certain inherited blood disorders are prevalent. Understanding these genetic factors is crucial for effective prevention and management strategies.Genetic variations can affect various stages of red blood cell production, leading to different types of anemia.
These variations can impact the synthesis of hemoglobin, the protein responsible for oxygen transport, or affect the structure and function of red blood cells themselves. The interplay of genetic factors with environmental influences like nutrition and infections significantly impacts the severity and manifestation of anemia.
Thalassemia in India
Thalassemia, a group of inherited blood disorders characterized by reduced or absent globin chain synthesis, is a major contributor to anemia in India. The high prevalence is linked to the high frequency of thalassemia genes within certain populations. Alpha-thalassemia, affecting the alpha-globin genes, and beta-thalassemia, affecting the beta-globin genes, are commonly observed. These conditions can range in severity from asymptomatic to life-threatening, depending on the specific genetic mutations and the number of affected genes.
Early diagnosis and management are crucial to mitigate the complications associated with these disorders.
Other Inherited Blood Disorders
Beyond thalassemia, other inherited blood disorders contribute to anemia in India. These include sickle cell anemia, characterized by abnormal hemoglobin S, and glucose-6-phosphate dehydrogenase (G6PD) deficiency, an enzyme deficiency that affects red blood cell survival. The prevalence of these disorders varies across different regions and populations within India, influenced by factors such as migration patterns and consanguineous marriages (marriages between close relatives).
These marriages increase the likelihood of inheriting two copies of a recessive gene responsible for a disorder.
Genetic Testing and Counseling
Genetic testing plays a vital role in identifying individuals at risk of developing inherited anemias. Tests such as polymerase chain reaction (PCR) and DNA sequencing can detect specific mutations associated with thalassemia and other blood disorders. Genetic counseling helps individuals and families understand the risks, inheritance patterns, and available management options. Prenatal diagnosis through chorionic villus sampling (CVS) or amniocentesis can identify affected fetuses, allowing for informed reproductive decisions.
Genetic screening programs, particularly in high-risk populations, can help reduce the incidence of these disorders.
Visual Representation of Genetic Pathways in Anemia
Imagine a flowchart. At the top, we have “Hemoglobin Synthesis.” Two branches emerge: one for “Normal Hemoglobin Synthesis” leading to “Healthy Red Blood Cells” and ultimately “No Anemia.” The other branch is “Abnormal Hemoglobin Synthesis,” which further branches into three pathways: 1. “Alpha-Thalassemia” (showing a defect in alpha-globin gene leading to reduced alpha-globin chains); 2. “Beta-Thalassemia” (showing a defect in beta-globin gene leading to reduced beta-globin chains); and 3.
“Sickle Cell Anemia” (showing a mutation in the beta-globin gene resulting in abnormal hemoglobin S). Each of these pathways ultimately leads to “Anemia” with varying degrees of severity indicated by different shades of red. A separate pathway could illustrate “G6PD Deficiency,” stemming from a different gene, also leading to “Anemia.” The flowchart visually demonstrates how different genetic defects disrupt the normal process of hemoglobin synthesis, resulting in various types of anemia.
Public Health Strategies for Anemia Reduction
Tackling anemia in India requires a multifaceted approach encompassing public health interventions, robust government policies, and widespread awareness campaigns. Success hinges on understanding the complex interplay of nutritional deficiencies, infectious diseases, and socioeconomic factors that contribute to this widespread health issue.Successful public health interventions in India have demonstrated the effectiveness of targeted strategies. These initiatives highlight the importance of integrating multiple approaches for lasting impact.
Successful Public Health Interventions in India
Several successful programs have been implemented across India to combat anemia. These programs have employed diverse strategies, ranging from large-scale supplementation programs to community-based awareness drives. The effectiveness of these interventions is often measured by changes in hemoglobin levels within targeted populations.
- National Iron Plus Initiative (NIPI): This program focuses on providing iron and folic acid supplementation to pregnant women, adolescent girls, and children. NIPI’s success is largely attributed to its widespread reach and integration within existing healthcare systems. It has demonstrated measurable improvements in hemoglobin levels in participating groups, though challenges remain in ensuring consistent adherence to the supplementation regimen.
- Poshan Abhiyaan: This national nutrition mission addresses malnutrition in all its forms, including anemia. It uses a multi-pronged approach that includes improved nutrition education, access to nutritious food, and health services. The program’s effectiveness is evaluated through regular monitoring and assessment of nutritional status indicators in target populations.
- Janani Suraksha Yojana (JSY): While primarily focused on maternal health, JSY indirectly contributes to anemia reduction by providing institutional deliveries and promoting antenatal care. This ensures pregnant women receive iron and folic acid supplements and proper medical attention, thereby reducing the risk of anemia-related complications.
Challenges in Implementing Anemia Prevention and Control Programs
Despite significant progress, challenges persist in effectively implementing anemia prevention and control programs across India. These obstacles often stem from a complex interplay of logistical, socioeconomic, and behavioral factors.
- Reaching remote and marginalized populations: Geographic barriers and socioeconomic disparities hinder access to healthcare services and supplementation programs in many regions.
- Ensuring consistent adherence to supplementation: Maintaining consistent intake of iron and folic acid supplements can be challenging due to various factors, including side effects, lack of awareness, and poor storage conditions.
- Addressing underlying causes of anemia: Simply addressing iron deficiency through supplementation may not be sufficient if underlying causes such as infections, parasitic infestations, and poor dietary diversity are not addressed concurrently.
- Resource constraints: Limited resources, including funding, trained personnel, and infrastructure, often hamper the effective implementation of anemia control programs.
The Role of Government Policies and Healthcare Initiatives
Government policies and healthcare initiatives play a crucial role in shaping the landscape of anemia prevention and control. Strong political commitment, coupled with well-defined strategies and adequate resource allocation, are essential for success.The government’s role includes developing national guidelines, implementing large-scale programs, strengthening healthcare infrastructure, and promoting research and surveillance to monitor the effectiveness of interventions. Furthermore, policies aimed at improving food security, sanitation, and access to healthcare services are vital for addressing the root causes of anemia.
A Public Health Campaign for Anemia Prevention and Treatment
A comprehensive public health campaign is crucial for raising awareness and promoting preventive measures. This campaign, titled “Healthy India, Healthy Blood,” will employ a multi-pronged approach.
- Television and Radio Advertisements: Short, impactful advertisements featuring relatable characters and clear messages about anemia symptoms, prevention, and treatment will be aired frequently across various channels.
- Community Outreach Programs: Health workers will conduct door-to-door campaigns in villages and urban slums, distributing educational materials and conducting awareness sessions.
- School-Based Education: Educational materials, including age-appropriate pamphlets and interactive sessions, will be integrated into school curricula to educate children and adolescents about anemia.
- Social Media Campaign: Utilizing platforms like Facebook, Instagram, and Twitter, the campaign will leverage the power of social media to reach a wider audience and encourage participation.
- Collaboration with NGOs and Community Leaders: Partnering with local NGOs and community leaders will facilitate better outreach and ensure culturally appropriate messaging.
Lifestyle Factors and Anemia Risk
Anemia, while often linked to dietary deficiencies, can also be significantly influenced by lifestyle choices. Understanding the impact of these factors is crucial for developing comprehensive strategies to combat anemia, especially in populations where nutritional deficiencies are prevalent. This section explores the relationship between lifestyle factors and anemia risk, highlighting how certain habits can exacerbate or mitigate the condition.Lifestyle factors such as smoking and excessive alcohol consumption can significantly contribute to the development or worsening of anemia.
These factors disrupt various physiological processes involved in red blood cell production and function, ultimately leading to lower hemoglobin levels and the characteristic symptoms of anemia.
Smoking and Anemia
Smoking negatively impacts red blood cell production in several ways. Nicotine, a primary component of cigarettes, constricts blood vessels, reducing blood flow to the bone marrow where red blood cells are produced. This reduced blood flow limits the delivery of essential nutrients and oxygen, hindering erythropoiesis (red blood cell formation). Furthermore, smoking increases oxidative stress, damaging red blood cells and shortening their lifespan.
So, that recent study showing iron deficiency isn’t the main culprit behind anemia in India got me thinking. We need to focus on broader nutritional strategies, not just iron supplements. Understanding the underlying causes is key, and that reminds me of how crucial it is to know the risk factors that make stroke more dangerous , since many share similar preventative measures like healthy diets and lifestyle choices.
Getting back to anemia, prioritizing diverse, nutrient-rich foods is the best way to combat deficiencies and boost overall health.
This leads to increased red blood cell destruction, contributing to anemia. The impact is particularly noticeable in individuals already at risk due to underlying conditions or nutritional deficiencies. For example, a smoker with a pre-existing iron deficiency will likely experience a more severe form of anemia than a non-smoker with the same deficiency.
Alcohol Consumption and Anemia, Iron deficiency not the root cause of anaemia in india study tips to reduce the risk
Excessive alcohol consumption interferes with the body’s ability to absorb essential nutrients, including iron, folate, and vitamin B12 – all crucial for red blood cell production. Alcohol also directly damages the bone marrow, impairing its function and reducing red blood cell production. Furthermore, chronic alcohol abuse can lead to liver damage, further compromising the body’s ability to process and utilize essential nutrients for red blood cell synthesis.
The type of anemia influenced by alcohol consumption can vary, ranging from macrocytic anemia (due to folate or B12 deficiency) to microcytic anemia (due to iron deficiency).
So, that recent study highlighting iron deficiency isn’t the sole culprit behind India’s anaemia problem got me thinking. We need to look at a broader picture of nutrition, and that includes understanding dietary differences between the sexes. Check out this fascinating article on are women and men receptive of different types of food and game changing superfoods for women to get a better grasp on this.
Ultimately, tailoring dietary advice based on gender might be key to tackling anaemia effectively and understanding how to boost iron absorption.
Impact of Lifestyle Factors on Anemia Types
The impact of lifestyle factors on different types of anemia varies. For instance, smoking may exacerbate iron-deficiency anemia by impairing iron absorption and increasing oxidative stress. Excessive alcohol consumption can contribute to both iron-deficiency anemia and megaloblastic anemia (due to folate or vitamin B12 deficiency) through nutrient malabsorption and bone marrow damage. It is important to note that the interaction between lifestyle factors and nutritional deficiencies can significantly worsen the severity of anemia.
Benefits of Healthy Lifestyle Choices for Anemia Prevention
Adopting healthy lifestyle choices is vital for preventing and managing anemia. These choices can significantly reduce the risk of developing anemia or lessen the severity of existing conditions.
Making positive changes to your lifestyle can significantly improve your overall health and reduce the risk of developing anemia. Here are some key lifestyle modifications:
- Quit smoking: Smoking cessation is crucial for improving overall health and reducing anemia risk. The body’s ability to produce healthy red blood cells will improve significantly after quitting.
- Moderate alcohol consumption: Limiting alcohol intake helps ensure proper nutrient absorption and prevents bone marrow damage.
- Maintain a balanced diet: A diet rich in iron, folate, vitamin B12, and other essential nutrients is essential for red blood cell production.
- Regular exercise: Physical activity promotes better circulation and overall health, indirectly supporting red blood cell production.
- Manage stress: Chronic stress can negatively impact the immune system and overall health, potentially affecting red blood cell production.
- Get enough sleep: Adequate sleep is essential for the body’s repair and regeneration processes, including red blood cell production.
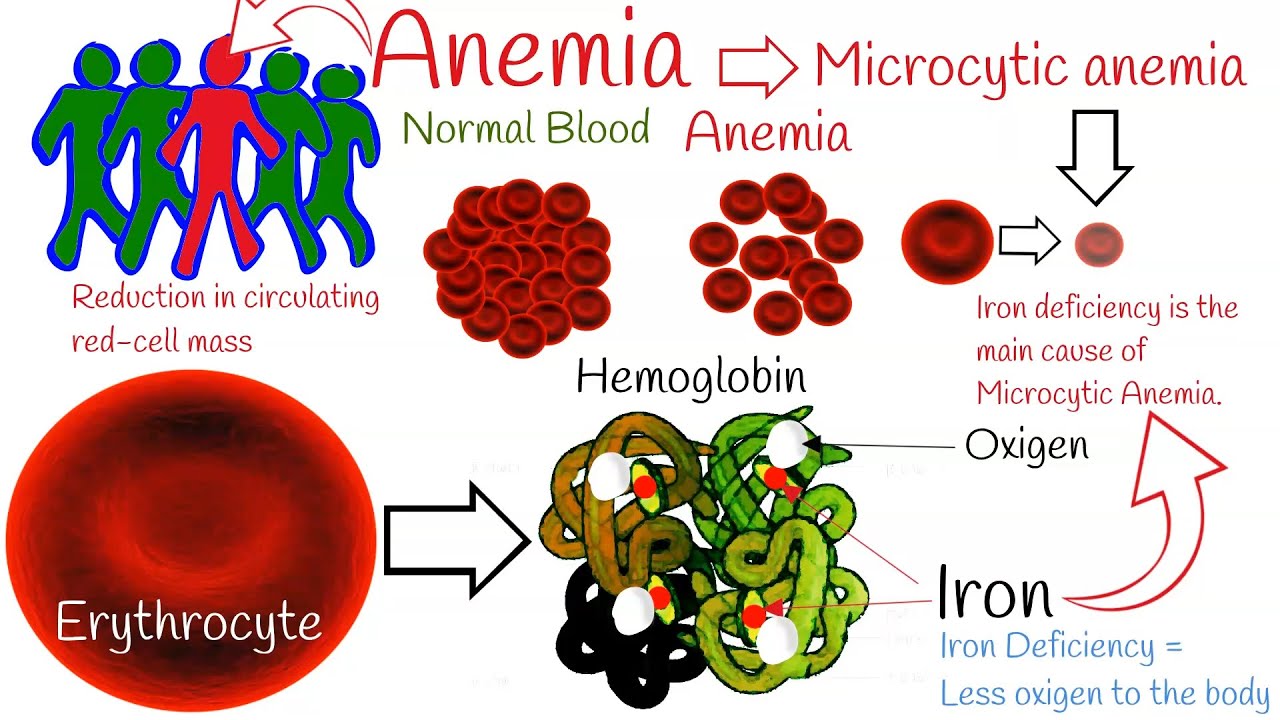
Last Point: Iron Deficiency Not The Root Cause Of Anaemia In India Study Tips To Reduce The Risk
Source: ytimg.com
So, while iron is undeniably important, addressing India’s anaemia crisis requires a holistic approach. It’s not a simple case of “take your iron pills and you’ll be fine.” We need to tackle underlying nutritional deficiencies, combat infectious diseases, address genetic predispositions, and promote healthy lifestyles. By understanding the multifaceted nature of anaemia and implementing comprehensive strategies, we can make significant strides in improving the health and well-being of millions.
Let’s work together to create a healthier India, one red blood cell at a time!
Question & Answer Hub
What are the early symptoms of anaemia?
Early symptoms can be subtle and include fatigue, weakness, pale skin, shortness of breath, and dizziness. If you experience these, it’s important to see a doctor.
Can anaemia be prevented?
Yes, to a large extent. A balanced diet rich in iron, folate, and vitamin B12, along with good hygiene practices to prevent infections, can significantly reduce your risk.
Are there any specific foods I should eat to increase my iron levels?
Leafy green vegetables, lentils, beans, red meat, and fortified cereals are all excellent sources of iron. Pairing iron-rich foods with vitamin C enhances absorption.
What if I’ve been diagnosed with anaemia? What’s the treatment?
Treatment depends on the underlying cause. It might involve iron supplements, vitamin supplements, medication to treat infections, or even blood transfusions in severe cases. Your doctor will guide you on the best course of action.





