
Mayo Clinic Income Cut in Half Labor Costs
Mayo clinic income cut in half labor costs – Mayo Clinic income cut in half due to labor costs? It’s a headline that’s sent shockwaves through the healthcare industry, raising serious questions about the future of one of the world’s most prestigious medical institutions. This isn’t just about numbers on a spreadsheet; it’s about the potential impact on patient care, research, and the dedicated professionals who make the Mayo Clinic what it is.
Let’s dive into the details and explore what this means for the future of healthcare.
The Mayo Clinic, renowned for its exceptional medical care and groundbreaking research, finds itself facing an unprecedented financial challenge. A significant reduction in income, attributed largely to escalating labor costs, has forced the institution to re-evaluate its operational strategies. This situation raises crucial questions about the sustainability of high-quality healthcare in the face of rising expenses and potential cost-cutting measures.
We’ll examine the contributing factors, the implemented cost-reduction strategies, and the potential long-term consequences for both the Mayo Clinic and the broader healthcare landscape.
Mayo Clinic’s Financial Situation

Source: infraon.io
The Mayo Clinic, a renowned non-profit medical practice, recently announced a significant reduction in its operating income, prompting concerns about its financial health and the broader implications for healthcare systems. While the clinic remains financially stable, the challenges it faces highlight the evolving pressures on even the most established healthcare providers.The reported income reduction is multifaceted, stemming from a confluence of factors impacting both revenue and expenditure.
A key element is the shift in healthcare reimbursement models, moving away from fee-for-service towards value-based care. This transition requires significant investments in infrastructure and technology, impacting short-term profitability while aiming for long-term sustainability. Additionally, rising operational costs, including staffing, supplies, and technology upgrades, have significantly impacted the bottom line. The increase in uninsured and underinsured patients also contributes to the financial strain, as these patients often require extensive care with limited reimbursement potential.
Mayo Clinic’s Revenue Streams and Performance
The Mayo Clinic’s revenue is derived from a variety of sources, primarily patient care services. This includes inpatient and outpatient visits, surgical procedures, diagnostic testing, and other medical services. Revenue also comes from research grants, philanthropic donations, and educational activities. While specific financial data is not publicly released in granular detail due to its non-profit status, recent reports indicate a decline in overall revenue growth compared to previous years.
This slower growth is attributed to the aforementioned factors, including the shift to value-based care and the increasing cost of providing care. The performance of individual revenue streams varies; for example, while outpatient visits may remain relatively strong, the reimbursement rates for certain procedures may have decreased, impacting overall revenue.
Comparison to Similar Healthcare Organizations
The Mayo Clinic’s financial performance needs to be considered within the context of the broader healthcare landscape. Many large healthcare systems, both for-profit and non-profit, are experiencing similar financial pressures. The shift to value-based care, rising operational costs, and increasing numbers of uninsured patients are universal challenges. However, direct comparisons are difficult due to variations in reporting standards, accounting practices, and the specific services offered by different organizations.
Some institutions might focus on specialized areas, leading to different revenue streams and financial profiles. Furthermore, geographic location plays a significant role, with varying reimbursement rates and healthcare regulations affecting financial outcomes. While a comprehensive comparative analysis requires detailed financial statements from multiple institutions, it’s safe to say the Mayo Clinic’s struggles are reflective of broader industry trends.
Labor Costs at Mayo Clinic
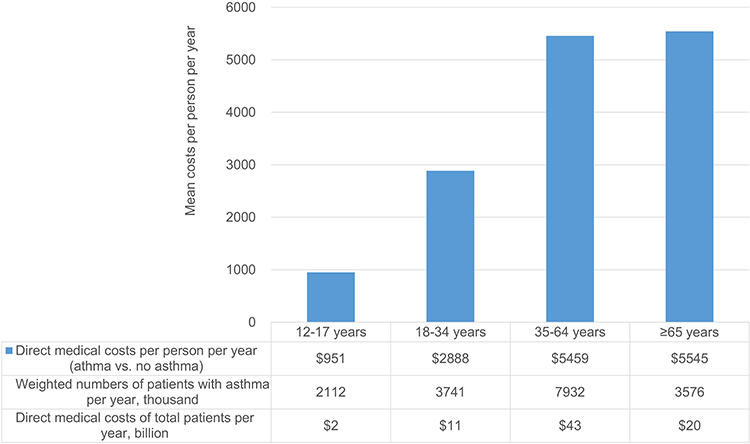
Source: dovepress.com
Mayo Clinic, like any large healthcare organization, faces significant challenges in managing its labor costs. These costs represent a substantial portion of its overall expenses, and recent financial adjustments have necessitated a closer look at how these funds are allocated and utilized. Understanding the composition of these costs and the strategies employed for reduction is crucial to comprehending the clinic’s current financial situation.The composition of Mayo Clinic’s labor costs is complex, encompassing far more than just salaries.
Hearing about the Mayo Clinic’s income cut due to halved labor costs got me thinking about the future of healthcare. It’s a stark reminder of rising expenses, but maybe solutions lie in innovative tech like AI. Check out this article on the exciting advancements at UPMC, ai most exciting healthcare technology center connected medicine upmc , which could potentially address these cost concerns.
Perhaps embracing AI could help organizations like the Mayo Clinic navigate these financial challenges more effectively.
It includes a wide range of expenses related to employing its extensive workforce of physicians, nurses, technicians, administrative staff, and support personnel. Salaries, of course, constitute the largest component. However, significant portions are also dedicated to employee benefits, including health insurance, retirement plans, paid time off, disability insurance, and professional development opportunities. These benefits are essential for attracting and retaining top talent within a highly competitive healthcare market.
Furthermore, costs associated with training, recruitment, and ongoing professional development programs also contribute to the overall labor expense.
Areas of Labor Cost Reduction
Mayo Clinic’s efforts to reduce labor costs have likely targeted multiple areas. Given the size and complexity of the organization, a comprehensive strategy would involve a multifaceted approach rather than a single drastic measure. Areas potentially affected include workforce optimization, potentially through attrition and strategic hiring freezes in less critical areas. Negotiations with unions regarding compensation and benefits packages may have also been undertaken to achieve cost savings.
Furthermore, streamlining administrative processes and improving operational efficiency could contribute to reducing the overall labor burden.
Examples of Cost-Cutting Measures
Specific examples of cost-cutting measures are difficult to definitively state without access to internal Mayo Clinic documents. However, based on industry trends and common practices in large healthcare organizations, some plausible examples include: implementing more efficient scheduling systems to minimize overtime and optimize staffing levels; re-evaluating the need for certain positions and potentially consolidating roles where feasible; negotiating more favorable contracts with vendors providing employee benefits; and investing in technology to automate certain tasks and reduce the need for manual labor.
These are all common strategies employed by organizations facing budgetary constraints.
Hearing about the Mayo Clinic cutting labor costs to halve its income loss got me thinking about the pressures on healthcare leadership. It’s a tough situation, and the news about AdventHealth CEO Terry Shaw’s retirement, as reported here adventhealth ceo retire terry shaw , highlights the intense challenges facing hospital systems. Perhaps these drastic measures at Mayo Clinic are a sign of things to come for other organizations struggling with similar financial burdens.
Impact on Employee Morale and Retention
The implementation of labor cost reduction measures inevitably carries the risk of negatively impacting employee morale and retention. Reductions in salaries, benefits, or job security can lead to decreased job satisfaction and increased employee turnover. This can, in turn, lead to increased recruitment costs, loss of institutional knowledge, and a potential decline in the quality of patient care.
To mitigate these risks, Mayo Clinic would likely need to carefully communicate its financial challenges to its employees, emphasizing the necessity of these measures and the steps being taken to minimize negative impacts on the workforce. This could involve providing transparent explanations of the cost-cutting strategies, offering additional support services to employees, and maintaining open communication channels to address concerns.
The long-term success of any cost-cutting strategy will depend heavily on its ability to balance financial needs with the well-being and retention of its valuable workforce.
Impact of Reduced Income on Services: Mayo Clinic Income Cut In Half Labor Costs
A 50% cut in Mayo Clinic’s income, largely attributed to reduced labor costs, presents a significant challenge to the organization’s ability to maintain its current level of services. This reduction will inevitably impact various aspects of the Clinic’s operations, from the range of services offered to the pace of research and development. Understanding these potential consequences is crucial for both the Clinic’s administration and the patients it serves.The ripple effect of reduced income will be far-reaching.
A decrease in funding necessitates difficult choices about resource allocation, potentially leading to a scaling back of certain programs and services. This could affect not only the breadth of care offered but also the accessibility and quality of that care.
Impact on Service Range and Patient Access
The reduction in income will likely force the Mayo Clinic to prioritize its services. This could mean scaling back less frequently used or less profitable specialized services. For example, experimental treatments or niche procedures might be temporarily suspended or limited to only the most critical cases. This prioritization could lead to longer wait times for appointments, especially for non-emergency procedures and less urgent conditions.
Patients might experience increased difficulty scheduling appointments, longer wait times in clinics, and potentially reduced access to certain specialists or diagnostic tests. A real-world example is the reduction of elective surgeries during periods of financial strain seen in other healthcare systems. These temporary suspensions are common and demonstrate the direct link between funding and service availability.
Hearing about the Mayo Clinic’s income being cut in half due to labor costs got me thinking about the larger picture of healthcare finances. It’s a tough situation, and the news that HSHS Prevea is closing Wisconsin hospitals and health centers, as reported here: hshs prevea close wisconsin hospitals health centers , only highlights how precarious the financial stability of many healthcare systems is.
This makes the Mayo Clinic’s struggles seem less isolated and more like a symptom of a wider problem facing healthcare providers nationwide.
Impact on Research and Development
Research and development are vital components of Mayo Clinic’s mission. However, funding cuts will likely translate to reduced investment in these areas. This could manifest in several ways: fewer research grants awarded, smaller research teams, delays in launching new studies, and a potential slowdown in the development of innovative treatments and technologies. This would have long-term consequences, potentially hindering the Clinic’s ability to remain at the forefront of medical innovation and impacting future patient care.
For instance, a delay in cancer research funding could directly impact the development of new therapies, potentially leading to poorer patient outcomes in the future.
Summary of Impacts and Mitigation Strategies, Mayo clinic income cut in half labor costs
| Service Area | Impact on Service | Impact on Patients | Mitigation Strategies |
|---|---|---|---|
| Specialized Services | Potential reduction or elimination of less frequently used services. | Reduced access to specialized care; potential increase in wait times for appointments. | Prioritization of services based on clinical need and cost-effectiveness; exploring partnerships or collaborations to share resources. |
| Diagnostic Testing | Potential delays in access to certain tests due to budget constraints. | Increased wait times for test results; potential delays in diagnosis and treatment. | Optimizing testing protocols; exploring less expensive alternatives while maintaining quality; improving scheduling efficiency. |
| Research and Development | Reduced funding for research projects; potential delays or cancellations of studies. | Slower development of new treatments and technologies; potential impact on future patient care. | Prioritization of high-impact research projects; seeking alternative funding sources; streamlining research processes to maximize efficiency. |
| Patient Access | Longer wait times for appointments; potential limitations on access to certain specialists. | Increased inconvenience and potential delays in receiving necessary care. | Improved appointment scheduling systems; expanding telehealth options; optimizing clinic workflows. |
Strategies for Financial Recovery
Mayo Clinic faces a significant challenge in restoring its financial stability after a 50% income cut. A multi-pronged approach, focusing on revenue generation, operational efficiency, and strategic cost management, is crucial for its recovery. This plan Artikels key strategies to navigate this difficult period and ensure the continued provision of high-quality healthcare.
The core of the recovery plan hinges on a balanced approach: increasing revenue streams while simultaneously optimizing operational efficiency and managing costs effectively. A holistic strategy is needed, addressing both the immediate financial pressures and the long-term sustainability of the institution.
Revenue Generation Strategies
Diversifying revenue streams is essential to reduce reliance on traditional sources. The following strategies can significantly boost Mayo Clinic’s income.
- Expand Telemedicine Services: Leverage existing telehealth infrastructure to offer a wider range of virtual consultations and remote patient monitoring services. This can reach geographically dispersed patients and increase accessibility, leading to higher patient volume and revenue.
- Strategic Partnerships and Joint Ventures: Collaborate with pharmaceutical companies, medical device manufacturers, and other healthcare providers on research initiatives, clinical trials, and shared service agreements. This can generate revenue through licensing agreements, research grants, and shared resources.
- Enhanced Pricing Strategies: Implement a more nuanced pricing model that accounts for the complexity and value of Mayo Clinic’s services. This could involve value-based pricing, bundled payments, and tiered pricing based on patient needs and insurance coverage.
- Focus on High-Margin Services: Prioritize services with high profit margins, such as specialized procedures, advanced diagnostics, and complex surgeries. This requires careful analysis of service profitability and allocation of resources accordingly.
- Develop and Market New Services: Identify unmet healthcare needs in the community and develop innovative services to address them. This could include new specialized clinics, wellness programs, or preventative care initiatives.
Improved Operational Efficiency
Optimizing operational efficiency can significantly reduce costs and free up resources for reinvestment. This requires a systematic approach to identifying and eliminating waste.
- Streamline Administrative Processes: Implement advanced technology and automation to reduce administrative overhead. This could involve electronic health records (EHR) optimization, automated billing systems, and improved workflow management.
- Optimize Supply Chain Management: Negotiate better contracts with suppliers, implement inventory management systems, and reduce waste in the supply chain. This can lead to significant savings on medical supplies and equipment.
- Improve Resource Allocation: Analyze resource utilization across different departments and allocate resources more effectively to optimize service delivery and reduce idle time.
- Data-Driven Decision Making: Use data analytics to identify areas for improvement in operational efficiency. This involves tracking key performance indicators (KPIs) and using data to inform strategic decisions.
Cost Management Approaches
Effective cost management is crucial for regaining financial stability. Different approaches need to be considered, balanced against their impact on service quality.
- Targeted Cost Reduction: Focus on areas with high potential for cost savings without compromising patient care. This might involve renegotiating contracts, streamlining processes, and reducing unnecessary spending.
- Strategic Workforce Management: Implement strategies to optimize staffing levels, improve employee productivity, and reduce employee turnover. This could include training programs, improved work-life balance initiatives, and competitive compensation packages.
- Technology Investment: Investing in technology can lead to long-term cost savings through automation, improved efficiency, and reduced errors. However, careful evaluation of ROI is essential before making significant investments.
Long-Term Implications

Source: medpagetoday.net
The 50% income cut at the Mayo Clinic presents a multifaceted challenge with profound long-term implications, extending far beyond the immediate financial crisis. The ripple effects will impact its reputation, ability to attract and retain talent, and its overall contribution to the healthcare landscape. Understanding these implications is crucial for charting a path towards sustainable recovery.The most significant long-term concern is the potential erosion of Mayo Clinic’s prestigious reputation.
A reduction in services, even temporary, could damage public perception and erode patient trust. This is especially true given the Clinic’s history of excellence and its status as a global leader in healthcare. Any perceived decline in quality of care, whether due to staff reductions or limitations in research funding, could have lasting consequences.
Impact on Talent Acquisition and Retention
Reduced income inevitably impacts the ability to attract and retain top medical talent. Highly skilled physicians, researchers, and nurses are in high demand, and Mayo Clinic will face increased competition from institutions with more stable financial positions. Salaries and benefits packages might need to be adjusted, potentially leading to staff departures and difficulty in filling crucial positions. This brain drain could further compromise the quality of care and hinder research initiatives.
For example, a competing hospital system offering significantly higher compensation packages and state-of-the-art facilities could easily lure away key personnel. The loss of experienced staff would translate into a decline in expertise and potentially longer wait times for patients.
Effect on the Overall Healthcare Landscape
Mayo Clinic’s financial struggles have implications that extend beyond its own walls. As a major player in the healthcare industry, its difficulties could signal broader systemic issues. If a renowned institution like Mayo Clinic is struggling with financial sustainability, it highlights the vulnerabilities within the healthcare system as a whole. This could impact the availability and affordability of high-quality care nationwide, especially for specialized treatments and research.
For instance, a reduction in Mayo’s research output could delay breakthroughs in disease treatment and prevention, impacting the broader healthcare community. Furthermore, if Mayo is forced to reduce or eliminate certain services, other healthcare providers may be overwhelmed by the increased demand.
Future Scenarios for Mayo Clinic
Several potential future scenarios exist, all depending on the interplay of income, labor costs, and service provision. In a best-case scenario, Mayo Clinic successfully implements cost-cutting measures, diversifies its revenue streams, and secures additional funding. This would allow it to maintain a high standard of care and retain its top talent. However, a worst-case scenario involves a prolonged period of financial instability, leading to significant staff reductions, service limitations, and a decline in its reputation.
This could result in a diminished role for Mayo Clinic in the healthcare landscape, possibly impacting its research capabilities and ability to compete with other leading institutions. A more moderate scenario involves a gradual recovery, where Mayo Clinic implements strategic changes to improve efficiency and adapt to the changing healthcare environment. This might involve a shift in focus towards certain specialties or a greater emphasis on telehealth and preventative care.
The ultimate outcome will hinge on the Clinic’s ability to effectively manage its resources, adapt to evolving market conditions, and maintain its commitment to providing high-quality patient care.
Final Conclusion
The Mayo Clinic’s struggle to balance its budget amidst rising labor costs highlights a critical issue facing many healthcare providers. The potential impact on patient care, research, and employee morale is significant, and the path to financial recovery requires a multi-faceted approach. While cost-cutting measures are necessary, maintaining the high standards of care that define the Mayo Clinic is paramount.
The long-term implications will depend on the effectiveness of their recovery strategies and the broader shifts in the healthcare industry. This is a story that will continue to unfold, and its outcome will have far-reaching consequences.
Query Resolution
Will this impact the quality of care at the Mayo Clinic?
The Mayo Clinic aims to mitigate the impact on patient care through strategic cost-cutting and efficiency improvements. However, some service adjustments are possible.
What specific cost-cutting measures have been implemented?
Specific details are limited, but likely include streamlining administrative processes, negotiating better contracts with suppliers, and potentially workforce adjustments.
How does this compare to other major healthcare systems?
Many large healthcare systems face similar financial pressures due to rising labor and operational costs. The Mayo Clinic’s situation highlights the broader challenges in the industry.
What are the long-term implications for Mayo Clinic employees?
The long-term effects on employees are uncertain and depend on the success of the financial recovery plan. Potential impacts range from job security concerns to changes in benefits.





