Medicaid Funding Reduction Redeterminations CMS Rule
Medicaid Funding Reduction Redeterminations CMS Rule: This new rule is shaking up the healthcare landscape, and frankly, it’s causing a lot of anxiety. We’re talking about potential cuts to Medicaid, impacting millions who rely on this vital program for healthcare access. This post dives into the details, exploring the implications for beneficiaries, states, and the future of healthcare funding in America.
It’s a complex issue, but I’ll break it down in a way that’s hopefully easy to understand.
The rule’s core changes involve stricter eligibility checks for Medicaid recipients, leading to potential disenrollments. The timeline for implementation varies by state, but the projected impact on state budgets and individual access to care is significant. We’ll be looking at how different states are reacting, the financial pressures they face, and the legal challenges the rule is already encountering.
Get ready for a deep dive into the complexities of this crucial healthcare policy shift.
Overview of the CMS Rule on Medicaid Funding Reduction and Redeterminations
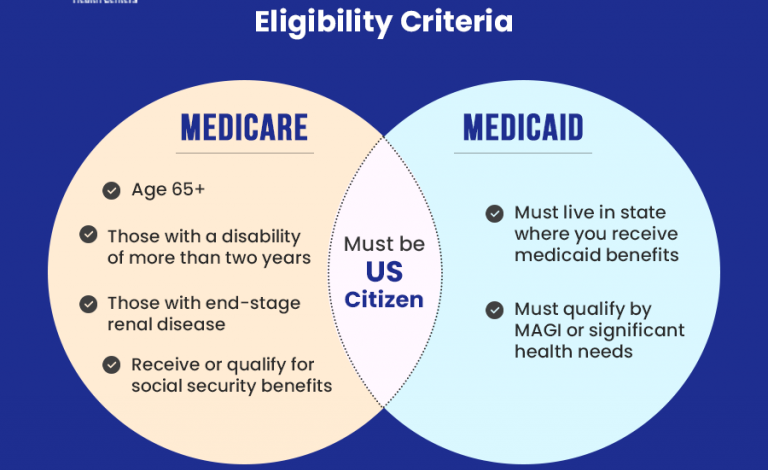
The Centers for Medicare & Medicaid Services (CMS) recently issued a rule impacting Medicaid eligibility and funding. This rule significantly alters the process of determining who qualifies for Medicaid, potentially leading to substantial changes in enrollment and state budgets. The core of the rule focuses on a renewed emphasis on verifying eligibility, leading to a projected decrease in Medicaid enrollment and a shift in financial responsibility between the federal and state governments.The key provisions of the CMS rule center around redeterminations of Medicaid eligibility.
Previously, continuous coverage was a hallmark of the Affordable Care Act’s expansion of Medicaid. This rule reinstates a more frequent review process, requiring states to verify eligibility more regularly. This includes confirming income, household size, and citizenship status for current enrollees. The rule also sets forth new requirements for states regarding timely processing of applications and appeals, aiming to streamline the process while simultaneously increasing scrutiny.
Failure to comply with these new standards can result in financial penalties for states. Furthermore, the rule Artikels specific procedures for handling disenrollment, including providing ample notification to individuals facing potential loss of coverage.
Timeline for Implementation of the Rule’s Provisions
The implementation timeline for the rule is phased, beginning with states submitting updated plans to CMS detailing how they intend to comply. This initial phase involves significant planning and logistical adjustments for state Medicaid agencies. The subsequent phases involve the actual implementation of the redetermination process, starting with a gradual rollout across different demographics and gradually encompassing the entire Medicaid population.
States are given a certain amount of time to implement the changes, with specific deadlines varying depending on the specific provision and the state’s individual circumstances. However, the overall timeline is relatively tight, necessitating a rapid and efficient response from state agencies. Failure to meet these deadlines could lead to financial penalties or loss of federal funding.
The Medicaid funding reduction and redeterminations CMS rule is causing a lot of anxiety, especially for those with pre-existing conditions. For example, many people with carpal tunnel syndrome rely on affordable healthcare options, and the new rules might impact access to treatment. If you’re struggling with carpal tunnel, check out this helpful resource on ways to treat carpal tunnel syndrome without surgery to explore non-surgical options.
Ultimately, the impact of these CMS changes on access to care remains a significant concern.
For example, some states anticipate completing their redetermination processes within 12-18 months, while others may require a longer timeframe.
The Medicaid funding reduction redeterminations CMS rule is causing a lot of upheaval, impacting hospitals already stretched thin. This financial strain adds another layer of complexity, especially when considering the stringent new cybersecurity regulations; understanding the hhs healthcare cybersecurity framework hospital requirements CMS is crucial for compliance. Failing to meet these standards could further jeopardize already vulnerable hospital budgets, exacerbating the issues created by the Medicaid funding cuts.
Expected Impact on State Medicaid Programs
The expected impact of this rule on state Medicaid programs is multifaceted and potentially significant. One major consequence is the projected decrease in Medicaid enrollment. The stricter eligibility verification process is expected to lead to a reduction in the number of individuals receiving Medicaid benefits, as some individuals may no longer meet the eligibility criteria. This reduction in enrollment will, in turn, affect state budgets.
While the federal government shares the cost of Medicaid, states bear a portion of the financial burden. A decrease in enrollment could lead to a decrease in federal funding, but it could also potentially lead to reduced state expenditures. The net effect on state budgets remains uncertain and will vary considerably depending on the state’s specific circumstances, including its initial Medicaid enrollment rate and its ability to efficiently implement the new requirements.
For example, states with larger proportions of low-income individuals might experience a more substantial drop in enrollment and a corresponding shift in financial responsibilities.
Impact on Medicaid Beneficiaries

Source: dreamstime.com
The CMS rule’s changes to Medicaid funding and redetermination processes will undoubtedly have a significant impact on millions of Americans relying on this crucial safety net. The stricter eligibility requirements and increased frequency of redeterminations will likely lead to a decrease in Medicaid enrollment, with potentially devastating consequences for those who lose coverage. This section will explore these potential effects in detail.
The rule’s changes will affect access to vital healthcare services for eligible individuals. The increased administrative burden on both beneficiaries and state Medicaid agencies could lead to delays in processing applications and renewals, leaving individuals without coverage during critical periods. Furthermore, the heightened scrutiny of eligibility criteria could result in the disenrollment of individuals who, despite meeting the requirements, struggle to navigate the complex application process or provide the necessary documentation.
Groups Most Affected by Medicaid Redeterminations
Several groups are particularly vulnerable to the impacts of the rule’s changes. Individuals experiencing homelessness, those with disabilities, people with limited English proficiency, and those living in rural areas with limited access to technology or transportation will face significant challenges in navigating the redetermination process. These groups often lack the resources and support needed to successfully maintain their Medicaid coverage.
For example, a homeless individual might struggle to provide a stable address, a critical piece of information required for renewal, while someone with a cognitive disability might find the application process overwhelming. The added administrative burden will disproportionately affect these vulnerable populations, leading to higher disenrollment rates.
Consequences of Medicaid Disenrollment
Loss of Medicaid coverage can have severe consequences for individuals and families. Without access to affordable healthcare, individuals may delay or forgo necessary medical care, leading to worsening health conditions and increased healthcare costs in the long run. This can manifest in various ways, from untreated chronic illnesses to delayed diagnoses of serious conditions. For example, someone with diabetes might forgo insulin due to cost, leading to potentially life-threatening complications.
Furthermore, disenrollment can result in financial instability, as medical bills accumulate and individuals struggle to afford treatment. The ripple effect extends to families, impacting their financial security and overall well-being.
Comparison of Pre- and Post-Rule Beneficiary Access to Care
| Feature | Pre-Rule Scenario | Post-Rule Scenario | Potential Impact |
|---|---|---|---|
| Eligibility Determination | Relatively streamlined process; less frequent redeterminations. | More stringent requirements; increased frequency of redeterminations. | Increased risk of disenrollment for eligible individuals; delays in accessing care. |
| Access to Care | Relatively easy access to a wide range of healthcare services. | Reduced access to care for those disenrolled or facing delays in renewal. | Increased healthcare costs for individuals; potential worsening of health conditions. |
| Administrative Burden | Lower burden for both beneficiaries and state agencies. | Increased burden for both beneficiaries and state agencies due to increased paperwork and verification processes. | Potential delays in processing applications and renewals; increased stress and frustration for beneficiaries. |
| Financial Stability | Reduced financial burden for healthcare costs. | Increased risk of medical debt and financial hardship for those losing coverage. | Potential for increased poverty and financial instability among vulnerable populations. |
State-Level Responses to the Rule
The CMS rule on Medicaid redeterminations has created a patchwork of responses across the United States, with states employing diverse strategies to navigate the complex challenges it presents. The variations reflect differing political climates, existing administrative capacities, and the unique demographics of each state’s Medicaid population. This leads to a wide range of outcomes for beneficiaries and significant disparities in access to care.
Categorization of State Responses
States’ responses to the Medicaid redetermination rule can be broadly categorized into three approaches: proactive engagement, reactive adaptation, and limited intervention. These categories are not mutually exclusive, and many states exhibit elements of multiple approaches. The choice of approach often reflects a state’s existing infrastructure, resources, and political priorities.
- Proactive Engagement: These states have implemented comprehensive strategies to minimize disruptions to coverage. This often involves significant investments in outreach and technology, proactive communication with beneficiaries, and streamlined application processes. Examples include states that have leveraged technology to automate much of the redetermination process, allowing for faster processing and more effective communication with beneficiaries.
- Reactive Adaptation: States in this category are primarily reacting to the rule’s requirements, implementing changes as needed but without a large-scale, proactive strategy. This approach often leads to longer processing times, higher error rates, and increased difficulties for beneficiaries in navigating the system. These states may rely heavily on existing resources and may struggle to keep up with the increased workload.
- Limited Intervention: Some states have adopted a more limited approach, focusing on fulfilling the minimum requirements of the rule without significant additional investment. This often results in increased disenrollment rates and potentially greater challenges for vulnerable populations. This approach is often associated with states facing budgetary constraints or those with less robust administrative systems.
Examples of Innovative Strategies
Several states are employing innovative strategies to mitigate the rule’s negative impacts. For example, some states are using predictive modeling to identify beneficiaries at high risk of disenrollment, allowing for targeted outreach and assistance. Others are partnering with community organizations to provide in-person assistance with the redetermination process. The use of multi-lingual outreach materials and culturally competent staff is also proving vital in ensuring equitable access to information and assistance.
Challenges Faced by States
Implementing the rule’s requirements presents numerous challenges for states. These include: the sheer volume of redeterminations required; the need for significant investment in technology and staff; the difficulty in reaching vulnerable populations; and ensuring accuracy and fairness in the process. Many states are grappling with staffing shortages, outdated technology, and a lack of funding to adequately support the increased workload.
The complexity of the rule itself and the varying eligibility criteria across states further exacerbate these challenges. Furthermore, the unpredictable nature of beneficiary responses and the logistical hurdles of contacting individuals who have moved or changed contact information add significant complexity to the process. This can lead to significant delays and increased administrative costs.
Financial Implications for States: Medicaid Funding Reduction Redeterminations Cms Rule
The CMS rule on Medicaid funding reduction and redeterminations will significantly impact state budgets, forcing difficult choices and potentially straining already stretched resources. The magnitude of the impact varies considerably depending on factors such as the state’s Medicaid enrollment, the proportion of beneficiaries likely to lose coverage, and the state’s existing fiscal capacity. Understanding these financial implications is crucial for policymakers and healthcare providers alike.The projected financial impact on state budgets is substantial and multifaceted.
Direct losses from reduced federal matching funds are a primary concern. States will also face increased administrative costs associated with the redetermination process, including outreach efforts to beneficiaries, processing applications, and managing appeals. Furthermore, a potential surge in uninsured individuals could lead to increased demand for uncompensated care at state-funded hospitals and clinics, further straining state resources.
The exact figures remain uncertain, as the actual number of disenrolled individuals is still unfolding. However, early estimates suggest billions of dollars in potential losses across the nation.
State Funding Sources to Offset Reductions
States will likely explore several avenues to offset the anticipated Medicaid funding reductions. Increased state general fund appropriations represent a straightforward, though potentially politically challenging, approach. However, this option is often limited by existing budgetary constraints and competing priorities. Other potential sources include reallocating funds from other state programs, potentially impacting services in other areas. States might also seek additional revenue through tax increases, though this is also politically sensitive.
Finally, some states might explore innovative financing mechanisms or seek federal waivers to modify their Medicaid programs to mitigate the financial burden. The feasibility and political viability of these options will vary greatly across states.
Resource Allocation Trade-offs
The financial pressures imposed by the CMS rule will necessitate difficult trade-offs in resource allocation. States may be forced to reduce funding for other critical programs, such as education, infrastructure, or public safety, to maintain Medicaid coverage levels. Alternatively, they might prioritize certain Medicaid benefits over others, potentially leading to reductions in coverage or access to specific services.
For example, states might choose to reduce funding for optional Medicaid benefits, such as dental or vision care, to maintain coverage for essential services like hospitalization. This decision-making process requires careful consideration of the potential consequences for various populations and services.
Potential Financial Burden on Various States
The following table illustrates the potential financial burden on several states, based on estimated Medicaid enrollment and projected disenrollment rates (these are illustrative examples and should not be considered definitive projections; actual figures will vary considerably). These figures are hypothetical and should be interpreted cautiously, highlighting the potential range of impact rather than providing precise predictions.
| State | Estimated Medicaid Enrollment (Millions) | Projected Disenrollment Rate (%) | Estimated Annual Funding Loss (Millions) |
|---|---|---|---|
| California | 14 | 5 | $700 |
| Texas | 5 | 7 | $350 |
| Florida | 5 | 6 | $300 |
| New York | 7 | 4 | $280 |
Legal Challenges and Policy Debates
The CMS rule on Medicaid redeterminations has sparked significant controversy, leading to numerous legal challenges and intense policy debates. These challenges stem from concerns about the rule’s potential impact on access to healthcare, its fairness, and the ethical implications of its implementation. The arguments are complex and involve a range of stakeholders, from individual beneficiaries to state governments and advocacy groups.
Potential Legal Challenges to the Rule
Several legal challenges to the rule are anticipated, primarily focusing on whether it complies with federal law and the requirements of the Medicaid Act. Arguments will likely center on whether the rule’s expedited processes adequately protect beneficiaries’ due process rights, particularly concerning procedural fairness and access to legal representation. Plaintiffs might argue that the shortened timelines for redetermination violate the spirit and intent of the Medicaid Act, which aims to provide healthcare access to vulnerable populations.
Another key area of legal contention could be the rule’s impact on states’ ability to administer their Medicaid programs effectively and efficiently, potentially raising constitutional concerns about federal overreach. For example, states might argue that the rule’s rigid timelines don’t account for variations in administrative capacity across different states, leading to unequal application of the rule.
Policy Debates Surrounding the Rule’s Effectiveness and Fairness
The rule’s effectiveness and fairness are central to the ongoing policy debates. Critics argue that the streamlined redetermination process will lead to a significant number of eligible individuals losing their Medicaid coverage due to procedural hurdles, administrative errors, or a lack of awareness. This could disproportionately affect vulnerable populations, exacerbating existing health disparities. Conversely, proponents argue that the rule is necessary to ensure the efficient allocation of limited Medicaid funds and to prevent fraud and abuse.
They contend that the rule’s expedited processes will streamline the system and improve accuracy in determining eligibility. The debate revolves around balancing the need for fiscal responsibility with the imperative of ensuring access to essential healthcare services for vulnerable individuals. The effectiveness of the rule will ultimately depend on its implementation and the extent to which states effectively support their beneficiaries through the redetermination process.
Ethical Considerations Raised by the Rule’s Implementation
The implementation of the rule raises significant ethical considerations, particularly regarding fairness, equity, and access to healthcare. The potential for increased disenrollment of vulnerable populations raises concerns about health equity and the potential for worsening health outcomes among those who lose coverage. Ethical questions arise concerning the balance between fiscal responsibility and the moral obligation to provide healthcare access to those in need.
The rule’s design and implementation should prioritize minimizing harm to vulnerable individuals and ensuring that the process is transparent, fair, and accessible to all. Concerns also exist about the potential for increased administrative burden on state Medicaid agencies and the ethical implications of prioritizing efficiency over individual needs.
Scenario: A Potential Legal Challenge
Imagine a hypothetical case where a state, let’s call it “Example State,” implements the CMS rule in a way that disproportionately affects its elderly population due to a flawed online portal for redetermination. Many elderly individuals lack sufficient technological literacy to navigate the portal, leading to a high rate of disenrollment among this vulnerable group. A coalition of advocacy groups representing the elderly could file a lawsuit against the federal government and Example State, arguing that the rule’s implementation in Example State violates the Medicaid Act’s mandate to provide equitable access to healthcare for all eligible individuals.
The plaintiffs could argue that Example State’s failure to provide adequate support and alternative methods for redetermination for its elderly population constitutes a violation of due process and creates an unreasonable barrier to accessing essential healthcare services. The legal challenge would center on whether the rule, as implemented by Example State, adheres to the spirit and intent of the Medicaid Act, considering the specific needs and vulnerabilities of the elderly population.
Data and Information Sources
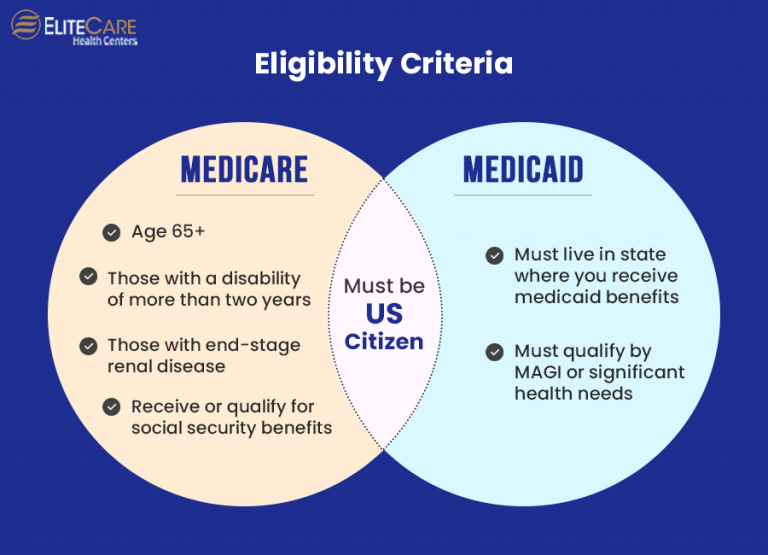
Source: elitecarehc.com
Understanding the impact of the CMS rule on Medicaid funding reduction and redeterminations requires careful examination of various data sources and analytical methods. Accessing and interpreting this information is crucial for policymakers, researchers, and advocates seeking to assess the rule’s consequences and propose effective solutions. The data landscape is complex, however, presenting challenges in terms of accessibility, consistency, and potential biases.Reliable sources for information about the CMS rule and its implementation include government websites, academic research, and reports from non-profit organizations.
These sources offer a range of perspectives and data types, enabling a more comprehensive understanding.
Government Websites and Publications
The Centers for Medicare & Medicaid Services (CMS) website is the primary source for official information regarding the rule, including the final rule text, fact sheets, and implementation guidance. State Medicaid agencies also publish reports and data related to their implementation of the redetermination process. The Congressional Research Service (CRS) provides non-partisan analyses of the rule’s potential impacts and policy implications.
These government sources offer a foundation for understanding the official policy and its implementation, but they may not always reflect the full picture of real-world effects. For example, while CMS may publish aggregate data on disenrollments, state-level data may provide a more nuanced understanding of the impact on specific populations.
Academic Research and Reports
Academic journals and policy research organizations frequently publish studies analyzing the impact of Medicaid policy changes. These studies often utilize a variety of data sources and methodologies to assess the rule’s effects on access to care, health outcomes, and state budgets. Examples include research from organizations like the Kaiser Family Foundation (KFF) and the Urban Institute. These sources offer valuable insights but may be limited by the availability of data and the time it takes to conduct thorough research and analysis.
For example, studies analyzing long-term effects of the rule will take time to emerge.
Data Types for Assessing the Rule’s Impact
Several types of data are crucial for evaluating the rule’s impact. Administrative data from state Medicaid agencies provides information on enrollment changes, disenrollment rates, and reasons for disenrollment. Survey data, collected through household surveys or provider surveys, can capture the experiences of beneficiaries and providers. Claims data offers insights into healthcare utilization patterns before and after the rule’s implementation.
Finally, qualitative data, such as interviews with beneficiaries and state officials, provides valuable contextual information. Combining these different data sources allows for a more robust and comprehensive assessment of the rule’s effects. For example, a decline in enrollment numbers (administrative data) can be contextualized by information from beneficiary surveys (survey data) regarding reasons for disenrollment.
Data Collection and Analysis Methods
Data collection methods vary depending on the type of data. Administrative data is typically collected through automated systems, while survey data requires direct interaction with respondents. Claims data is extracted from electronic health records. Qualitative data is collected through interviews and focus groups. Data analysis methods include descriptive statistics, regression analysis, and qualitative thematic analysis.
For example, regression analysis can be used to assess the relationship between the rule’s implementation and changes in healthcare utilization, while qualitative analysis can reveal the lived experiences of those affected by the rule. The selection of appropriate methods depends on the research question and the type of data available.
Limitations of Available Data and Potential for Bias
Data limitations and potential biases must be considered when interpreting the results. Administrative data may not always capture the full extent of the rule’s impact, as it may not reflect individuals who lose coverage without formally disenrolling. Survey data can be subject to sampling bias and response bias. Claims data may not fully capture the use of healthcare services outside of the formal healthcare system.
Finally, the design of data collection and analysis methods can introduce biases. Researchers must carefully address these limitations and biases to ensure the accuracy and reliability of their findings. For instance, if a survey only targets those who have lost coverage, it may overrepresent the negative experiences and underestimate the neutral or positive experiences. This is a crucial consideration in ensuring the integrity of the research.
Long-Term Effects and Predictions
The CMS rule’s impact on Medicaid extends far beyond the immediate budgetary concerns. Its long-term consequences will ripple through the healthcare system, affecting access to care, health outcomes, and the financial stability of state Medicaid programs. Predicting the precise effects is challenging, but analyzing historical trends and current conditions allows for informed estimations of potential long-term scenarios.Predicting the precise long-term consequences of the rule is inherently difficult, as the actual impact will depend on a complex interplay of factors including state-level implementation strategies, economic conditions, and the responses of healthcare providers.
However, several key areas deserve close scrutiny.
Impact on Access to Care
The redetermination process, while intended to ensure program integrity, risks significantly reducing access to care for eligible individuals. Increased administrative burden and confusion surrounding the process could lead to delays in renewals, resulting in temporary or permanent loss of coverage for many. This is particularly concerning for vulnerable populations like the elderly, disabled, and those with chronic conditions, who rely heavily on Medicaid for essential healthcare services.
The CMS rule on Medicaid funding reduction redeterminations is causing major ripples, impacting millions. It’s fascinating to see how this plays out against the backdrop of major healthcare players like Elevance Health, whose Q1 earnings were recently impacted by a cyberattack, as reported in this article: elevance health earnings q1 change cyberattack medicaid medicare advantage. The financial strain on these large companies could further complicate the already challenging situation created by the Medicaid funding cuts.
The experience of states that have previously implemented stricter eligibility verification processes suggests a potential increase in the uninsured rate, leading to delayed or forgone care and worsened health outcomes. For example, a study in [State Name] following a similar eligibility tightening showed a [Percentage]% increase in uninsured individuals within the first year.
Changes in Health Outcomes Among Medicaid Beneficiaries
Reduced access to preventative and ongoing care, resulting from disenrollment or delays in renewal, will likely lead to a deterioration in the health status of some Medicaid beneficiaries. Delayed or missed medical appointments, coupled with difficulties accessing medications, could result in a rise in preventable hospitalizations and emergency room visits. This is likely to place additional strain on already overburdened healthcare systems.
Furthermore, the loss of continuous coverage can disrupt ongoing treatment plans for chronic conditions, potentially leading to complications and exacerbating existing health issues. We can expect to see an increase in preventable hospital readmissions and potentially a rise in mortality rates among certain vulnerable populations. A parallel can be drawn to similar policies in other countries, where reductions in healthcare access have been directly linked to declines in population health indicators.
Financial Implications for States and the Federal Government, Medicaid funding reduction redeterminations cms rule
While the rule aims to reduce federal spending, the long-term financial implications are less clear. While some short-term savings may be achieved through reduced enrollment, the potential increase in uncompensated care costs borne by hospitals and other providers could offset these savings. States may also face increased administrative costs associated with the intensified verification process. The long-term effect could be a shift in the cost burden from the federal government to state budgets, potentially straining state resources and forcing difficult choices in other areas of public spending.
The possibility of increased legal challenges and the costs associated with defending those challenges also add to the financial uncertainty. Similar policy changes in other states have shown a pattern of initial savings followed by increased costs in subsequent years, particularly due to increased hospital readmissions and emergency room visits.
Adaptation and Adjustments to the Rule
Given the potential for significant negative consequences, it is likely that the rule will undergo adjustments and modifications over time. This could involve changes to the redetermination process to streamline the administrative burden, targeted outreach programs to assist vulnerable populations in navigating the process, or even a reconsideration of the eligibility criteria. The extent of these adaptations will depend on the extent and nature of the observed negative consequences, the political climate, and the availability of resources.
Pressure from advocacy groups, healthcare providers, and affected individuals will likely play a significant role in shaping any future modifications. The history of similar Medicaid policies demonstrates a pattern of iterative adjustments based on feedback and evaluation of real-world outcomes.
Final Review
The Medicaid Funding Reduction Redeterminations CMS rule is a game-changer, forcing states to navigate tricky financial and ethical dilemmas. While some states are innovating to mitigate the negative impacts, many face significant challenges. The long-term consequences remain uncertain, but it’s clear this rule will redefine access to healthcare for millions of Americans. Staying informed is crucial, so keep an eye on further developments and advocate for policies that ensure equitable healthcare for all.
Quick FAQs
What is the main goal of the CMS rule?
The primary goal is to reduce Medicaid spending by tightening eligibility requirements and removing individuals no longer deemed eligible.
How will this affect my doctor visits?
If you’re currently on Medicaid and lose eligibility due to the rule, you may face significant barriers to accessing necessary healthcare, potentially leading to delays or inability to receive care.
What are the potential legal challenges?
Several legal challenges are anticipated, focusing on arguments of fairness, equity, and the rule’s potential to disproportionately impact vulnerable populations.
Where can I find more information about my state’s response?
Your state’s Medicaid agency website is the best place to start. You can also search for news articles and reports specific to your state’s implementation of the rule.





