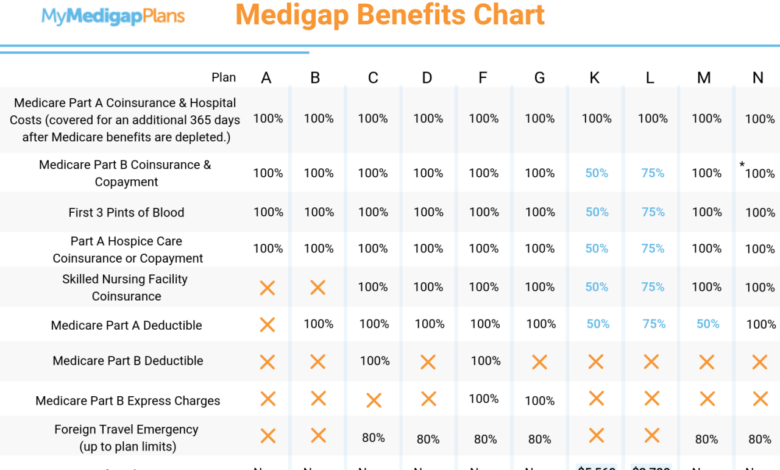
Medicare Advantage Beneficiaries Lower Acute Spending
Medicare Advantage beneficiaries chronic conditions lower acute utilization spending – that’s a headline that grabs attention, right? It hints at a fascinating story about how proactive chronic disease management within Medicare Advantage plans can actually lead to significant cost savings. We’re diving into the details of how this works, exploring the different types of plans, the prevalent chronic conditions, and the programs designed to keep beneficiaries healthy and out of the hospital.
Get ready to uncover the surprising connection between managing chronic illnesses and reducing healthcare costs!
This isn’t just about numbers; it’s about real people living healthier lives. We’ll look at how various Medicare Advantage plans incentivize preventative care, the role of patient adherence, and the impact of socioeconomic factors on healthcare utilization. We’ll also examine the effectiveness of different care coordination models, showing how a holistic approach can make a world of difference. Think of it as a peek behind the curtain of Medicare Advantage, revealing how smart planning and proactive care can translate into both better health and significant cost savings.
Medicare Advantage Plan Structure and Chronic Disease Management: Medicare Advantage Beneficiaries Chronic Conditions Lower Acute Utilization Spending
Source: verywellhealth.com
Medicare Advantage (MA) plans offer an alternative to Original Medicare, providing comprehensive coverage through private insurance companies. These plans play a significant role in managing chronic conditions, offering various approaches tailored to individual needs and health status. Understanding the different plan types and their features is crucial for beneficiaries seeking effective chronic disease management.
It’s fascinating how proactive management of chronic conditions in Medicare Advantage beneficiaries leads to lower acute care spending. This highlights the importance of preventative care, and I was thinking about this in relation to the news about Mass General Brigham’s buyout of a digital health unit, Mass General Brigham Buyouts Digital Unit. Perhaps such acquisitions will help further improve remote patient monitoring and chronic disease management, ultimately contributing to even greater savings in acute care costs for Medicare Advantage plans.
Types of Medicare Advantage Plans and Their Approaches to Chronic Condition Management
Medicare Advantage plans are categorized into several types, each with a unique approach to healthcare delivery and chronic disease management. These include Health Maintenance Organizations (HMOs), Preferred Provider Organizations (PPOs), Point-of-Service (POS) plans, and Special Needs Plans (SNPs). HMOs typically require beneficiaries to choose a primary care physician (PCP) within the plan’s network and obtain referrals for specialist care.
This structured approach can facilitate proactive chronic disease management through regular checkups and coordinated care. PPOs offer more flexibility, allowing beneficiaries to see specialists without referrals, but often at a higher cost. POS plans combine elements of both HMOs and PPOs, offering some flexibility while maintaining a PCP-centered approach. SNPs cater to specific populations, such as those with chronic conditions or specific geographic locations, and often provide specialized care coordination and management programs for their enrolled members.
Benefits and Limitations of Medicare Advantage Plans in Relation to Chronic Condition Care
The benefits of MA plans for chronic disease management include coordinated care, preventative services, and potentially lower out-of-pocket costs. The coordinated care offered by many MA plans, particularly HMOs and SNPs, can lead to improved adherence to treatment plans and better overall health outcomes. Many plans actively incentivize preventative care, such as screenings and vaccinations, which are crucial for managing chronic conditions.
However, limitations exist. Network restrictions in HMOs and POS plans can limit access to specialists or preferred providers. Some MA plans may have higher premiums or deductibles than Original Medicare, particularly for those with complex health needs. The benefit packages can vary significantly between plans, so careful comparison is crucial.
Incentivizing Preventative Care for Beneficiaries with Chronic Conditions
Medicare Advantage plans employ several strategies to incentivize preventative care among beneficiaries with chronic conditions. These include providing coverage for preventative screenings and services at no cost to the beneficiary, offering wellness programs and health coaching, and using disease management programs to support adherence to treatment plans. For example, many plans cover annual wellness visits, diabetes self-management education, and cardiac rehabilitation programs.
These initiatives are designed not only to improve health outcomes but also to reduce the likelihood of costly hospitalizations and emergency room visits associated with poorly managed chronic conditions. The cost savings from preventing complications often outweigh the initial investment in preventative care.
Cost-Sharing Structures of Different Medicare Advantage Plans for Chronic Disease Management
The cost-sharing structures for Medicare Advantage plans can vary significantly, impacting the overall cost of chronic disease management. The following table illustrates potential cost differences:
| Plan Type | Monthly Premium | Annual Deductible | Copay (Doctor Visit) |
|---|---|---|---|
| HMO | $0 – $50 | $0 – $700 | $0 – $40 |
| PPO | $20 – $100 | $0 – $1000 | $20 – $60 |
| POS | $10 – $75 | $0 – $800 | $10 – $50 |
| SNP (Chronic Condition Focused) | Variable | Variable | Variable |
*Note: These are example ranges and actual costs vary widely depending on the specific plan, location, and individual circumstances.*
Impact of Chronic Conditions on Healthcare Utilization
Chronic conditions significantly impact healthcare utilization among Medicare Advantage beneficiaries, driving up costs and influencing the overall health of the population. Understanding the prevalence of these conditions, their associated healthcare resource use, and how they compare to traditional Medicare beneficiaries is crucial for effective healthcare planning and resource allocation. This section will delve into these aspects, providing a clearer picture of the challenges and opportunities presented by chronic disease management within the Medicare Advantage system.
Prevalence of Chronic Conditions Among Medicare Advantage Beneficiaries
The most prevalent chronic conditions among Medicare Advantage beneficiaries mirror those seen in the general elderly population, but their impact is amplified due to the age and often multiple comorbidities present. Heart disease, including coronary artery disease and heart failure, consistently ranks high. Similarly, diabetes, both type 1 and type 2, poses a substantial burden. Chronic obstructive pulmonary disease (COPD), encompassing conditions like emphysema and chronic bronchitis, is another major player.
Hypertension (high blood pressure) and arthritis, affecting joints and mobility, are also extremely common. Finally, many beneficiaries struggle with multiple conditions simultaneously, leading to complex care needs and increased healthcare utilization.
Healthcare Resource Utilization Associated with Chronic Conditions
These prevalent chronic conditions significantly impact healthcare resource utilization. For instance, individuals with heart failure frequently require hospitalizations for exacerbation management, along with numerous physician visits for ongoing monitoring and medication adjustments. Similarly, uncontrolled diabetes can lead to hospitalizations due to complications like diabetic ketoacidosis or infections, alongside frequent visits to endocrinologists and primary care physicians. COPD patients often experience acute respiratory exacerbations necessitating emergency room visits and hospital admissions.
The cumulative effect of these conditions results in substantial utilization of resources, including inpatient hospital stays, emergency department visits, and physician office visits. While precise quantification varies based on the specific condition and study methodology, the overall trend is consistently upward. For example, a study by the Centers for Medicare & Medicaid Services (CMS) might show that individuals with multiple chronic conditions have X number of hospital readmissions within Y timeframe compared to those without chronic conditions.
Comparison of Acute Care Utilization Rates
Comparing acute care utilization rates between Medicare Advantage beneficiaries with chronic conditions and those enrolled in traditional Medicare reveals interesting patterns. While direct comparisons are complex due to differing populations and benefit structures, studies often suggest that Medicare Advantage plans, through their emphasis on preventative care and care coordination, may achieve slightly lower rates of hospitalization and emergency room visits for certain chronic conditions.
This difference may be attributed to proactive management strategies employed by many Medicare Advantage plans, such as disease management programs and telehealth initiatives. However, this is not universally true, and variations exist depending on the specific plan and the beneficiary’s individual circumstances. For example, a comparative analysis of hospitalization rates for heart failure patients might show a marginal reduction in Medicare Advantage versus traditional Medicare, but this would need to be analyzed further, controlling for other factors like socioeconomic status and access to care.
Relationship Between Severity of Chronic Conditions and Acute Care Utilization
A visual representation of this relationship could be a scatter plot. The x-axis would represent the severity of chronic conditions, perhaps measured by a composite score incorporating multiple factors like the number of conditions, their severity, and the presence of complications. The y-axis would represent the rate of acute care utilization, measured by the number of hospitalizations, emergency room visits, or a combined metric.
The plot would likely show a positive correlation, with increasing severity of chronic conditions associated with a higher rate of acute care utilization. Points clustered in the upper right quadrant would represent individuals with severe chronic conditions and high acute care utilization, while points in the lower left would represent individuals with less severe conditions and lower utilization.
This visualization would clearly illustrate the direct link between the burden of chronic disease and the demand for acute care services.
Cost Savings Associated with Chronic Condition Management Programs
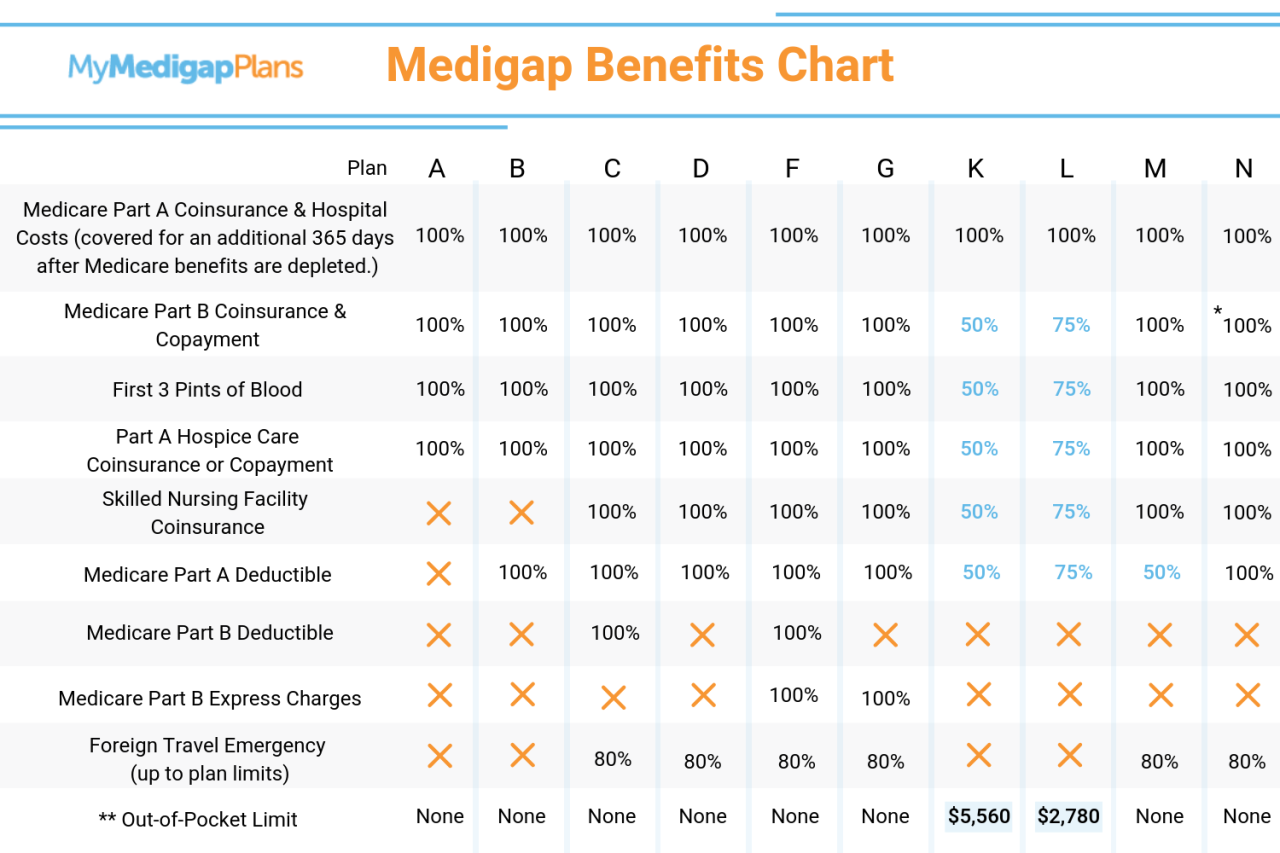
Source: mymedigapplans.com
Medicare Advantage (MA) plans are increasingly incorporating comprehensive chronic disease management programs to improve beneficiary health and, importantly, reduce healthcare costs. These programs recognize that proactive management of chronic conditions like diabetes, heart disease, and hypertension can significantly lessen the need for expensive emergency room visits and hospitalizations. By focusing on preventative care and early intervention, MA plans aim to shift the healthcare paradigm from reactive treatment to proactive wellness.The various programs offered by MA plans aim to reduce acute care utilization through several strategies.
These include regular check-ups, medication management support, telehealth consultations, and health education initiatives designed to empower beneficiaries to actively participate in their own care. This proactive approach not only improves health outcomes but also leads to substantial cost savings for both the individual and the healthcare system.
Chronic Disease Management Programs Offered by Medicare Advantage Plans
Medicare Advantage plans offer a wide array of chronic disease management programs tailored to specific conditions. These programs often include personalized care plans developed in collaboration with the beneficiary’s primary care physician. For example, a diabetes management program might include regular blood glucose monitoring, nutritional counseling, and medication adherence support. Similarly, a heart failure management program could focus on weight management, medication optimization, and regular monitoring of vital signs.
These programs are frequently delivered through a combination of in-person visits, telehealth appointments, and educational materials. The goal is to equip beneficiaries with the knowledge and resources necessary to effectively manage their conditions and prevent complications.
Cost Savings Demonstrated Through Effective Chronic Condition Management
Numerous studies have demonstrated the significant cost savings associated with effective chronic condition management within the Medicare Advantage framework. These savings stem from reduced hospitalizations, emergency room visits, and overall healthcare utilization. The precise savings vary depending on the specific program, the condition being managed, and the population being served. However, the overall trend is clear: proactive management of chronic conditions translates into significant cost reductions.
It’s fascinating how proactive management of chronic conditions in Medicare Advantage beneficiaries leads to lower acute care costs. This makes me wonder about the resource allocation challenges faced by rural hospitals, especially considering the complexities of providing care like labor and delivery, as highlighted in this insightful article on Rural Hospitals Labor Delivery &. Perhaps similar preventative strategies could help alleviate some of the financial strain on these vital community institutions, ultimately benefiting both Medicare Advantage patients and rural healthcare systems.
Examples of Cost Savings by Program Type and Condition
The following bullet points illustrate the potential cost savings achieved through various chronic disease management programs:
- Diabetes Management: Studies have shown reductions in hospitalizations of up to 20% and a decrease in emergency room visits by 15% in Medicare Advantage beneficiaries participating in structured diabetes management programs. This translates to substantial savings, potentially ranging from hundreds to thousands of dollars per beneficiary annually, depending on the severity of the condition and the intensity of the intervention.
- Heart Failure Management: Effective heart failure management programs can reduce hospital readmissions by 25-30%, resulting in considerable cost savings. Reduced hospital stays directly translate to lower costs associated with inpatient care, medications, and rehabilitation.
- Hypertension Management: Programs focused on blood pressure control can significantly reduce the risk of stroke and heart attack, leading to fewer hospitalizations and long-term cost savings. These savings can be substantial, particularly considering the high cost of treating stroke and cardiovascular events.
It is important to note that these figures represent averages and the actual cost savings can vary significantly depending on factors such as the individual’s health status, adherence to the program, and the specific design of the program. However, the consistent trend across numerous studies demonstrates the clear financial benefits of investing in comprehensive chronic disease management programs within the Medicare Advantage system.
It’s fascinating how proactive management of chronic conditions in Medicare Advantage beneficiaries leads to lower acute care spending. This highlights the importance of efficient documentation, and that’s where technology like Nuance’s generative AI scribe, now integrated with Epic EHRs as detailed in this article, nuance integrates generative ai scribe epic ehrs , comes into play. Improved documentation could streamline care coordination, ultimately impacting those lower acute utilization rates we’re seeing in the Medicare Advantage population.
Factors Influencing Acute Care Utilization
Understanding the factors that drive acute care utilization among Medicare Advantage beneficiaries with chronic conditions is crucial for developing effective interventions and improving overall healthcare outcomes. High rates of acute care visits often indicate gaps in preventative care and chronic disease management, leading to increased costs and reduced quality of life for patients. This section explores several key factors contributing to this issue.
Patient Adherence to Treatment Plans
Patient adherence, or the extent to which individuals follow their prescribed treatment plans, plays a significant role in preventing acute care needs. Poor adherence to medication regimens, dietary restrictions, and lifestyle modifications can lead to disease exacerbations and ultimately necessitate emergency room visits or hospitalizations. For example, a diabetic patient who inconsistently manages their blood sugar levels is at a much higher risk of experiencing hyperglycemic crises requiring urgent medical attention.
Conversely, strong adherence to treatment plans, supported by effective communication from healthcare providers and access to resources like medication assistance programs, can significantly reduce acute care utilization. Studies consistently demonstrate a strong correlation between treatment adherence and lower rates of hospital readmissions and emergency department visits.
Socioeconomic Factors Contributing to Higher Acute Care Utilization
Socioeconomic disparities significantly influence access to healthcare and the management of chronic conditions. Medicare Advantage beneficiaries facing financial constraints may struggle to afford prescribed medications, healthy food options, or transportation to medical appointments. Lack of health literacy, coupled with limited access to reliable information and culturally competent healthcare services, further complicates the situation. For instance, individuals living in areas with limited access to public transportation might find it difficult to attend regular check-ups or participate in chronic disease management programs, leading to delayed care and increased risk of acute events.
These factors disproportionately impact vulnerable populations, resulting in higher rates of hospitalization and emergency room visits.
Effectiveness of Different Care Coordination Models
Various care coordination models aim to improve the management of chronic conditions and reduce acute care utilization. These models vary in their approaches, ranging from basic case management to more complex, integrated models that involve multiple healthcare professionals and community resources. For example, a patient-centered medical home (PCMH) model emphasizes proactive care, regular check-ups, and coordination of care across multiple providers.
Accountable care organizations (ACOs) incentivize providers to manage the care of a defined population, promoting coordinated care and reducing unnecessary hospitalizations. Comparative studies show that integrated care models, involving proactive outreach, remote patient monitoring, and strong patient-provider communication, generally demonstrate greater success in reducing hospitalizations and emergency room visits compared to traditional models of care. The effectiveness of each model depends on several factors, including the specific needs of the patient population, the resources available, and the level of provider engagement.
Flowchart Illustrating Chronic Condition Management within a Medicare Advantage Plan
The following describes a flowchart illustrating the process of managing a chronic condition within a Medicare Advantage plan. The flowchart begins with a patient diagnosis. The next step is a comprehensive assessment of the patient’s needs, including physical, social, and emotional factors. This is followed by the development of a personalized care plan, involving the patient in the decision-making process.
Regular monitoring of the patient’s health status is crucial, utilizing tools like telehealth and remote patient monitoring. This monitoring allows for early detection of potential problems and timely intervention. If complications arise, appropriate adjustments to the care plan are made, potentially involving referral to specialists or other healthcare professionals. Points of potential intervention to reduce acute care needs are highlighted throughout the process, including patient education, medication adherence support, and access to community resources.
Finally, the process concludes with ongoing evaluation and adjustment of the care plan as needed, ensuring the plan remains relevant and effective. The overall goal is to proactively manage the chronic condition, prevent exacerbations, and minimize the need for acute care services.
Data Sources and Research Methodology
Understanding the relationship between chronic conditions and acute care utilization among Medicare Advantage beneficiaries requires a robust research methodology grounded in reliable data sources. This analysis leverages a multi-faceted approach, combining large-scale administrative datasets with careful statistical techniques to uncover meaningful trends and patterns.The primary data source for this study is Medicare claims data. This rich dataset provides detailed information on medical services received by Medicare Advantage beneficiaries, including diagnoses, procedures, and the associated costs.
Specifically, we utilize Part A (hospital insurance) and Part B (medical insurance) claims to capture both inpatient and outpatient acute care utilization. These claims are linked to beneficiary demographic and enrollment information, allowing for a comprehensive analysis stratified by age, gender, and chronic condition prevalence. To gain a more nuanced understanding of the patient experience and potential mediating factors, we supplement the claims data with publicly available data on socioeconomic factors and access to care in different geographic areas.
This helps to contextualize the findings and identify potential disparities in healthcare access and outcomes.
Data Analysis Methods
The analysis employs a combination of descriptive and analytical statistical techniques. Descriptive statistics, such as frequencies, means, and standard deviations, are used to summarize the characteristics of the study population and their healthcare utilization patterns. More sophisticated methods, such as regression analysis, are employed to investigate the relationship between the presence of specific chronic conditions (e.g., diabetes, heart failure, chronic obstructive pulmonary disease) and the likelihood of acute care utilization (e.g., hospital admissions, emergency department visits).
We use multivariable regression models to adjust for potential confounding factors, such as age, gender, socioeconomic status, and the presence of multiple chronic conditions. This allows us to isolate the independent effect of each chronic condition on acute care utilization.
Limitations of Data and Methods, Medicare Advantage beneficiaries chronic conditions lower acute utilization spending
While Medicare claims data offer a comprehensive picture of healthcare utilization, certain limitations must be acknowledged. Claims data may not capture the full spectrum of a patient’s health status, as it primarily reflects diagnosed and treated conditions. Unreported or undiagnosed conditions could influence acute care utilization but remain undetected in the claims data. Furthermore, the data may not fully capture the quality of care received, limiting our ability to assess the impact of interventions aimed at improving chronic disease management.
Finally, the observational nature of the study design prevents us from establishing definitive causal relationships between chronic conditions and acute care utilization. We can identify associations, but we cannot definitively conclude that one causes the other.
Study Design and Steps
A comprehensive study on this topic would involve several key steps:
- Define the study population: Specify the inclusion and exclusion criteria for Medicare Advantage beneficiaries (e.g., age range, enrollment duration, presence of specific chronic conditions).
- Data acquisition and cleaning: Obtain Medicare claims data and other relevant datasets. Clean the data to address missing values, inconsistencies, and errors.
- Variable creation and selection: Create variables representing chronic conditions, acute care utilization measures, and potential confounding factors. Select the relevant variables for the analysis.
- Descriptive analysis: Summarize the characteristics of the study population and their healthcare utilization patterns.
- Statistical modeling: Employ appropriate statistical methods (e.g., regression analysis) to investigate the relationship between chronic conditions and acute care utilization, adjusting for confounding factors.
- Sensitivity analysis: Conduct sensitivity analyses to assess the robustness of the findings to different assumptions and model specifications.
- Interpretation and reporting: Interpret the results in the context of existing literature and report the findings clearly and concisely.
Final Review
So, there you have it – the compelling case for proactive chronic disease management within Medicare Advantage. We’ve seen how different plans approach this, the impressive cost savings achieved, and the crucial role of patient engagement. It’s clear that investing in preventative care and effective chronic condition management isn’t just good for the individual; it’s a smart financial strategy for the entire system.
The future of healthcare is undoubtedly intertwined with this proactive approach, and understanding its implications is more important than ever.
Popular Questions
What are the most common chronic conditions among Medicare Advantage beneficiaries?
Diabetes, hypertension, heart disease, and chronic obstructive pulmonary disease (COPD) are among the most prevalent.
How do Medicare Advantage plans incentivize preventative care?
Many plans offer wellness programs, preventive screenings at no cost, and potentially lower premiums for healthy behaviors.
Can I switch Medicare Advantage plans if I’m not satisfied with my current plan’s chronic disease management?
Yes, you can typically switch plans during the annual open enrollment period (generally October 15th to December 7th).
What if I can’t afford the cost-sharing associated with my Medicare Advantage plan?
You may be eligible for extra help with Medicare costs based on your income and resources. Contact your State Medicaid office for more information.





