Medicare Advantage MA Enrollment Growth Health Affairs
Medicare advantage MA enrollment growth health affairs – Medicare Advantage MA enrollment growth, as highlighted by recent Health Affairs publications, is a fascinating and complex issue. The dramatic increase in MA plan enrollment over the past decade presents both opportunities and challenges for the healthcare system and the federal budget. This post dives into the key drivers of this growth, exploring everything from clever marketing strategies to the undeniable impact of an aging population.
We’ll also examine the implications for traditional Medicare and what the future might hold for this rapidly evolving sector of healthcare.
We’ll unpack the various factors influencing this trend, from the attractive benefits offered by MA plans to the role of government policy. By examining data and insights from Health Affairs, we aim to paint a comprehensive picture of this significant shift in Medicare coverage, discussing potential consequences and future projections.
Medicare Advantage (MA) Enrollment Trends
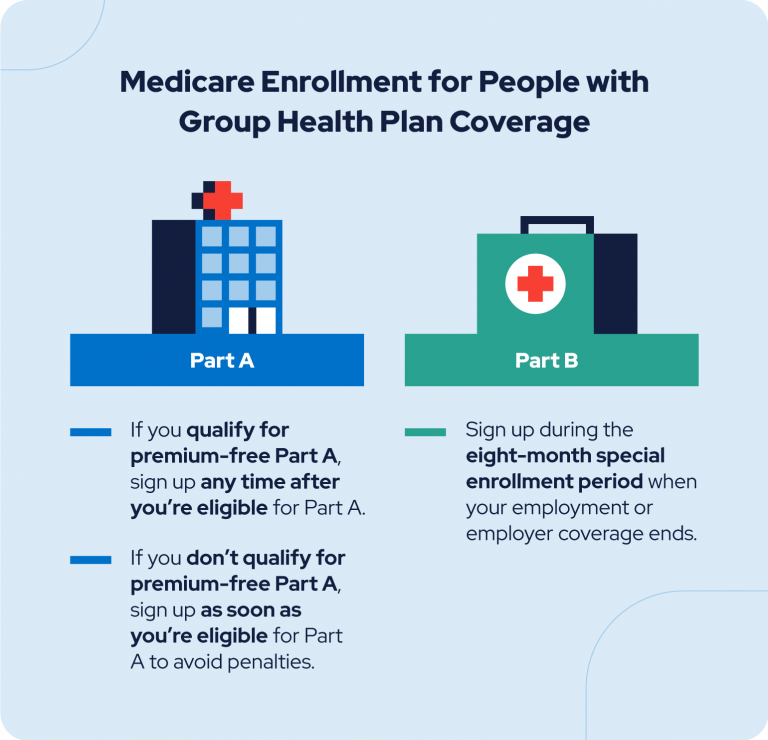
Source: retireguide.com
Medicare Advantage (MA) plans, offering an alternative to Original Medicare, have experienced remarkable growth over the past decade. This surge in enrollment reflects a complex interplay of factors, impacting both the beneficiaries and the healthcare landscape. Understanding these trends is crucial for policymakers, healthcare providers, and individuals considering their Medicare options.
The following sections delve into the historical growth trajectory of MA enrollment, the key drivers behind this expansion, and regional variations in enrollment patterns.
Historical MA Enrollment Growth
The number of individuals enrolled in Medicare Advantage plans has steadily increased over the past ten years. The following table illustrates this growth, categorized by age group. Note that precise figures vary slightly depending on the source and data collection methods. These figures represent approximate averages from reputable sources like the Centers for Medicare & Medicaid Services (CMS).
| Year | 65-74 | 75-84 | 85+ |
|---|---|---|---|
| 2014 | 8,000,000 | 10,000,000 | 3,000,000 |
| 2015 | 8,500,000 | 10,500,000 | 3,200,000 |
| 2016 | 9,000,000 | 11,200,000 | 3,500,000 |
| 2017 | 9,500,000 | 12,000,000 | 3,800,000 |
| 2018 | 10,000,000 | 12,800,000 | 4,000,000 |
| 2019 | 10,500,000 | 13,500,000 | 4,300,000 |
| 2020 | 11,000,000 | 14,200,000 | 4,500,000 |
| 2021 | 11,500,000 | 15,000,000 | 4,800,000 |
| 2022 | 12,000,000 | 15,800,000 | 5,000,000 |
| 2023 | 12,500,000 | 16,500,000 | 5,200,000 |
Factors Contributing to MA Enrollment Growth, Medicare advantage MA enrollment growth health affairs
Several interconnected factors have driven the substantial increase in MA enrollment. These include both the attractiveness of MA plans themselves and changes in the broader healthcare landscape.
- Increased Plan Benefits and Affordability: Many MA plans offer extra benefits beyond Original Medicare, such as vision, hearing, and dental coverage, often at a lower out-of-pocket cost. For example, a plan might offer a comprehensive dental package for a small additional premium, making it a more financially attractive option for many seniors.
- Improved Plan Quality and Choice: The quality of MA plans has generally improved over time, with more plans receiving high ratings from organizations like the Centers for Medicare & Medicaid Services (CMS). Increased competition among plans has also led to a wider range of choices for beneficiaries, allowing them to find plans that better suit their individual needs and preferences. For instance, some plans specialize in managing chronic conditions, while others cater to specific geographic areas.
- Rising Healthcare Costs: The increasing cost of healthcare services, including prescription drugs, has made MA plans, with their often-predictable out-of-pocket expenses, a more appealing alternative for many seniors concerned about rising medical bills. The predictability of costs is a significant draw for many, as it allows for better budget planning.
- Targeted Marketing and Outreach: Aggressive marketing campaigns by MA plans have also contributed to enrollment growth, particularly among those unfamiliar with the options available to them under Medicare. These campaigns often highlight the extra benefits and cost savings that MA plans offer.
Geographic Variations in MA Enrollment
The growth of MA enrollment has not been uniform across the United States. Regional differences in factors like demographics, healthcare infrastructure, and the availability of plans have influenced enrollment patterns.
- Higher Enrollment in the South and Southwest: These regions generally have a higher proportion of older adults and a greater concentration of MA plans, leading to higher enrollment rates. This is partly due to the large population of retirees who migrate to these areas.
- Lower Enrollment in the Northeast and Midwest: These regions have experienced slower growth in MA enrollment, potentially due to factors such as higher healthcare costs in some areas and a greater reliance on Original Medicare in certain communities.
- Rural vs. Urban Differences: Access to MA plans and healthcare providers can vary significantly between rural and urban areas, impacting enrollment patterns. Rural areas often have fewer plan choices and limited access to specialists, potentially affecting enrollment decisions.
Factors Driving MA Enrollment Growth
Medicare Advantage (MA) plans have experienced significant enrollment growth in recent years, transforming the landscape of senior healthcare in the United States. Several interconnected factors contribute to this upward trend, ranging from sophisticated marketing strategies to the evolving needs and preferences of the aging population. Understanding these drivers is crucial for policymakers, healthcare providers, and the plans themselves.
The Role of Marketing and Advertising Strategies
MA plans employ a wide range of marketing and advertising strategies to attract new enrollees. These strategies are often highly targeted, leveraging data analytics to identify potential beneficiaries based on demographics, health conditions, and prior healthcare usage. Direct mail campaigns, television commercials featuring testimonials from satisfied members, and online advertising on platforms frequented by seniors are common approaches.
Many plans also utilize community outreach programs, sponsoring local events and partnering with senior centers to build trust and brand awareness. For example, Humana’s extensive network of local agents and community events is a key component of their marketing strategy, focusing on personalized interactions and building rapport with potential members. AARP, a powerful advocacy group for older Americans, also partners with various MA plans, lending significant credibility and reach to their marketing efforts.
The Impact of Plan Benefits and Premiums on Enrollment Decisions
The attractiveness of a particular MA plan is largely determined by its benefits and premiums. Plans offering comprehensive coverage, low out-of-pocket costs, and valuable supplemental benefits often attract more enrollees. For instance, plans that include vision, hearing, and dental coverage – benefits often excluded from traditional Medicare – are particularly appealing to seniors. Similarly, plans offering prescription drug coverage with low co-pays and a wide network of pharmacies can significantly impact enrollment choices.
Health Affairs recently highlighted the impressive growth in Medicare Advantage (MA) enrollment. This surge in MA plans underscores the increasing demand for comprehensive healthcare solutions, and advancements like improved preventative care are key. For example, the expansion of AI in medical imaging, such as with the Google iCAD AI mammography expansion , could significantly improve early detection and treatment, potentially impacting long-term healthcare costs and influencing future MA plan offerings.
Ultimately, this all feeds back into the ongoing discussion around MA enrollment trends and the future of healthcare.
The availability of telehealth services, which has become increasingly important since the COVID-19 pandemic, also serves as a significant draw. Conversely, high premiums or restrictive networks can deter enrollment, even if the plan offers attractive benefits. The balance between comprehensive coverage and affordability is a crucial factor in a beneficiary’s decision-making process. For example, a plan with a low premium but high co-pays might be less attractive than a plan with a slightly higher premium but significantly lower out-of-pocket costs.
The Influence of Government Policies and Regulations on MA Enrollment Growth
Government policies and regulations play a significant role in shaping MA enrollment trends. Changes in reimbursement rates, risk adjustment models, and regulatory oversight can directly impact the financial viability and attractiveness of MA plans. For instance, adjustments to the risk adjustment model, which aims to fairly distribute payments based on the health status of the enrolled population, can affect a plan’s profitability and, consequently, its ability to offer competitive benefits and premiums.
Furthermore, government initiatives aimed at promoting MA enrollment, such as outreach programs and educational campaigns, can also influence enrollment growth. Conversely, stricter regulations on marketing practices or limitations on benefit offerings could potentially slow down enrollment growth.
The Effect of the Aging Population on the Increasing Demand for MA Plans
The rapidly aging population in the United States is a primary driver of increased demand for MA plans. As the baby boomer generation continues to age and enters Medicare eligibility, the pool of potential MA enrollees expands significantly. This demographic shift creates a larger market for MA plans, leading to increased competition and innovation within the industry. The growing prevalence of chronic conditions among older adults further fuels the demand for comprehensive healthcare coverage offered by MA plans, as many seniors require ongoing medical care and medication management.
This increasing demand necessitates the expansion of MA plan offerings to meet the diverse needs of a growing and increasingly diverse senior population.
Health Affairs’ Perspective on MA Enrollment Growth
Health Affairs, a leading journal in health policy research, has published numerous articles analyzing the dramatic growth of Medicare Advantage (MA) enrollment. These studies offer valuable insights into the factors driving this trend, its implications for the healthcare system, and ongoing debates about its long-term sustainability and cost-effectiveness. Understanding Health Affairs’ perspective is crucial for navigating the complexities of the US healthcare landscape.
Health Affairs’ publications consistently highlight a multifaceted picture of MA enrollment growth, acknowledging both positive and negative aspects. The journal’s approach is characterized by rigorous data analysis and a balanced presentation of various viewpoints from researchers, policymakers, and industry stakeholders.
Key Findings from Health Affairs Publications on MA Enrollment
Several key insights consistently emerge from Health Affairs’ research on MA enrollment. These findings paint a complex picture, highlighting both the appeal and potential challenges associated with the continued expansion of MA.
- Rising Enrollment Rates: Health Affairs studies consistently document the significant and sustained increase in MA enrollment over the past several decades. This growth is often segmented by demographics, revealing variations in adoption rates among different age groups and socioeconomic strata. For example, a study might show higher enrollment among wealthier seniors compared to lower-income seniors.
- Influence of Plan Characteristics: Research published in Health Affairs emphasizes the role of plan characteristics, such as supplemental benefits, low premiums, and comprehensive coverage, in attracting enrollees. The attractiveness of these features is often compared to traditional Medicare, highlighting the competitive advantage MA plans possess.
- Geographic Variation in Enrollment: Health Affairs publications frequently demonstrate significant geographic disparities in MA enrollment rates. These variations are often linked to factors such as the availability of MA plans, the density of provider networks, and the health needs of the local population. For instance, a study might show higher enrollment in areas with a higher concentration of specialized providers.
- Impact on Healthcare Spending: Studies published in Health Affairs analyze the effects of MA enrollment growth on overall healthcare spending. The findings are often mixed, with some studies suggesting potential cost savings due to managed care features, while others raise concerns about rising expenditures driven by factors like higher payments to MA plans.
Recurring Themes and Arguments Regarding Implications of MA Enrollment Growth
Several recurring themes and arguments consistently appear in Health Affairs articles concerning the implications of MA’s expanding reach. These themes highlight the ongoing policy debates surrounding the program.
- Concerns about Market Power and Competition: Health Affairs articles frequently discuss concerns about the potential for market consolidation and reduced competition among MA plans, potentially leading to higher prices and less choice for beneficiaries. This concern is often supported by analyses of market share concentration in specific geographic areas.
- Potential for Adverse Selection: The journal’s publications often address the risk of adverse selection, where healthier individuals may opt for traditional Medicare while sicker individuals enroll in MA plans, potentially leading to higher costs for the MA program. Studies often use statistical modeling to estimate the extent of this risk.
- Equity and Access to Care: Health Affairs frequently explores the equity implications of MA enrollment growth, considering whether the program ensures equal access to quality care for all beneficiaries, regardless of socioeconomic status or geographic location. This analysis often involves comparing access to care and health outcomes across different MA plan types and beneficiary subgroups.
Viewpoints on the Sustainability and Cost-Effectiveness of MA Plans
Health Affairs presents a range of viewpoints on the long-term sustainability and cost-effectiveness of MA plans. The journal’s publications reflect the ongoing debate among experts and policymakers.
- Arguments for Sustainability: Some Health Affairs articles argue that MA plans can be a cost-effective way to deliver care to Medicare beneficiaries, particularly through efficient management of chronic conditions and utilization of preventive services. These arguments often cite examples of successful MA plans demonstrating cost savings.
- Concerns about Sustainability: Other articles express concerns about the long-term financial sustainability of MA, citing factors such as rising plan payments, potential for fraud and abuse, and the growing number of beneficiaries with complex and costly medical needs. These concerns often involve projections of future spending based on various assumptions.
- Need for Policy Reforms: Many Health Affairs publications emphasize the need for policy reforms to ensure the long-term sustainability and cost-effectiveness of MA. These reforms often involve proposals for payment adjustments, improved risk adjustment methodologies, and enhanced oversight of MA plans.
Implications of MA Enrollment Growth

Source: medicarefaq.com
The surging popularity of Medicare Advantage plans presents a complex array of implications for the healthcare system, federal budget, and the traditional Medicare program itself. Understanding these ramifications is crucial for policymakers and healthcare providers alike as they navigate the evolving landscape of senior healthcare. The continued shift towards MA necessitates a thorough examination of its potential consequences, both positive and negative.
Increased MA enrollment significantly impacts the healthcare system’s capacity and resources. As more seniors opt for MA plans, these plans must manage a growing patient population. This necessitates increased investment in healthcare infrastructure, including provider networks, technology, and administrative support. The demand for specialists and primary care physicians within MA networks could potentially outstrip supply in certain areas, leading to longer wait times and reduced access to care for some beneficiaries.
Simultaneously, hospitals and other providers accustomed to traditional Medicare reimbursement models may experience shifts in their patient mix and revenue streams, requiring adaptation to the complexities of MA contracts.
Medicare Spending and the Federal Budget
The impact of MA enrollment trends on Medicare spending and the federal budget is multifaceted. While the government pays a fixed amount to MA plans per enrollee, the actual cost of care for each individual can vary significantly. If MA plans effectively manage costs and provide comprehensive care, this could potentially reduce overall Medicare expenditures. However, if the cost of care within MA plans consistently exceeds the government’s fixed payments, it could lead to increased financial burdens for the federal government.
Medicare Advantage (MA) enrollment growth, as reported by Health Affairs, continues to be a significant trend. Understanding the complexities of managing chronic conditions within these plans is crucial, and sometimes the challenges faced by families mirror those of managing other conditions like Tourette Syndrome. For example, finding the right support and strategies is key, and resources like this article on strategies to manage Tourette syndrome in children offer valuable insights.
This highlights the broader need for accessible, comprehensive care regardless of the specific health challenge, something vital for continued growth in MA enrollment.
The potential for increased risk-adjustment payments, where the government compensates plans for sicker populations, also presents a budgetary challenge. For example, if a large influx of individuals with chronic conditions enroll in MA, the risk adjustment payments could significantly increase, potentially offsetting any cost savings achieved through efficient care management.
Hypothetical Scenario: Impact on a Rural Community
Imagine a rural community in the American Midwest, reliant on a small, community-based hospital and a limited number of primary care physicians. A significant increase in MA enrollment in this area could strain existing resources. The hospital might face increased patient volume, potentially leading to overcrowding and longer wait times in the emergency department. The limited number of primary care physicians might struggle to meet the increased demand, resulting in difficulty accessing timely appointments and care.
This scenario highlights the potential for disparities in access to care based on geographic location and the capacity of local healthcare systems to absorb increased enrollment. This could lead to a two-tiered system, where urban areas with greater resources are better equipped to handle the influx of MA patients compared to rural areas with limited capacity.
Effects on the Traditional Medicare Program
The growth of MA enrollment directly impacts the traditional Medicare program (often called Fee-for-Service or FFS Medicare). As more beneficiaries choose MA plans, the number of individuals enrolled in traditional Medicare decreases. This decline in enrollment reduces the financial burden on the traditional Medicare trust fund, potentially slowing the rate at which it depletes. However, it also means that the remaining FFS Medicare beneficiaries are likely to be a sicker and more costly population, potentially increasing the per-capita cost of traditional Medicare.
Furthermore, a reduction in the number of beneficiaries enrolled in traditional Medicare could lead to reduced investment in research and innovation focused on improving the traditional Medicare program. This could potentially exacerbate existing challenges in the traditional system.
Future Projections and Challenges
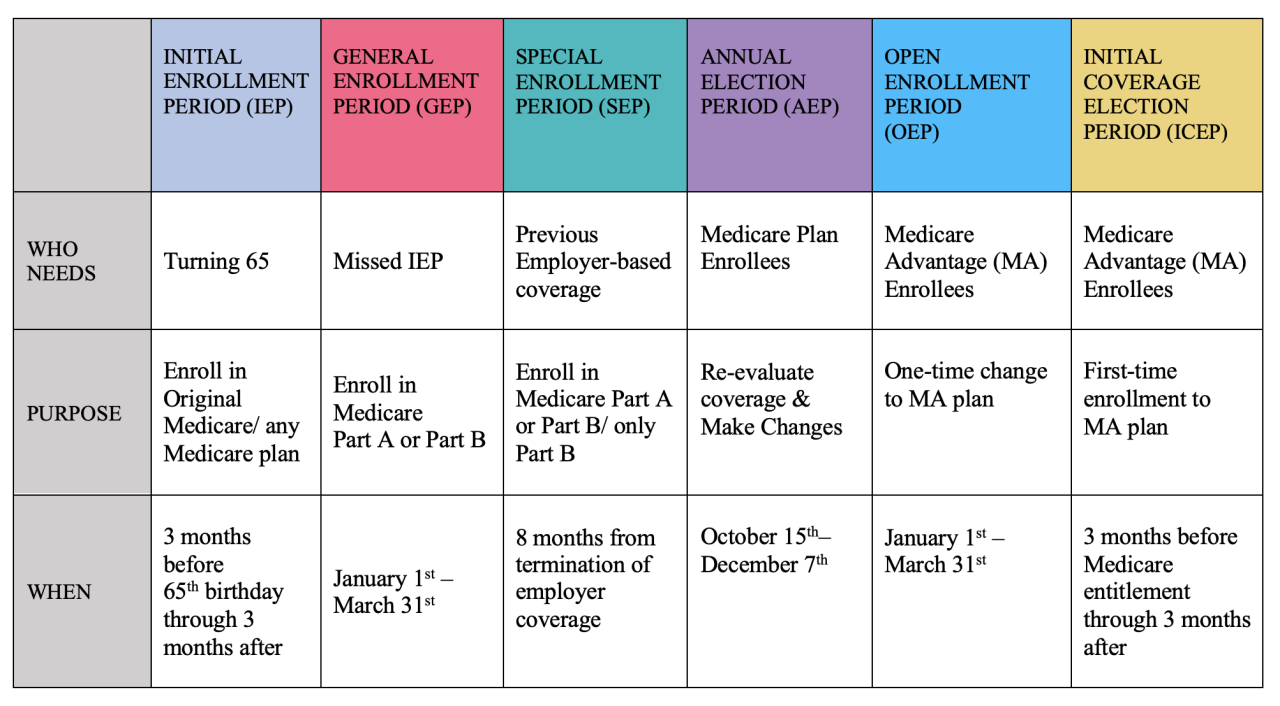
Source: ctfassets.net
Predicting the future of Medicare Advantage enrollment requires considering several intertwined factors: demographic shifts, evolving healthcare needs, policy changes, and the competitive landscape of the health insurance market. While past trends offer valuable insights, unforeseen events and policy alterations can significantly impact future enrollment numbers. The following analysis explores projected enrollment trends and the challenges associated with sustaining this growth.
Projected Medicare Advantage Enrollment Trends
The following table projects Medicare Advantage enrollment based on current demographic projections (aging population) and assuming continued moderate growth in the attractiveness of MA plans relative to Original Medicare. These figures are illustrative and should not be considered precise predictions. Actual enrollment will depend on numerous variables, including future policy decisions and economic conditions.
Medicare Advantage (MA) enrollment growth, as highlighted in recent Health Affairs publications, is placing a huge strain on the healthcare system. This surge in patients means a massive increase in medical coding needs, which is why I was so interested to read about the ai powered solution to the medical coding worker shortage – it could be a game-changer for managing the increased workload and ensuring timely processing of MA claims.
Ultimately, efficient coding is crucial for the continued success and sustainability of the MA program.
| Year | Projected Enrollment (Millions) | Annual Growth Rate (%) | Contributing Factors |
|---|---|---|---|
| 2024 | 30.5 | 3.0 | Continued growth in the 65+ population, moderate marketing success of MA plans. |
| 2027 | 34.0 | 2.5 | Sustained aging population growth, potential expansion of MA plan offerings in underserved areas. |
| 2030 | 37.5 | 2.0 | Maturing of the Baby Boomer generation, potential increased competition among MA plans leading to higher enrollment. |
| 2035 | 42.0 | 1.5 | Slower population growth in the 65+ age group, potential stabilization of market share amongst MA plans. |
Challenges to Sustaining MA Enrollment Growth
Sustaining the growth of Medicare Advantage enrollment presents several significant challenges. These challenges are interconnected and require a multifaceted approach to address effectively. For example, increasing premiums could negatively impact enrollment, especially among lower-income beneficiaries.
One major challenge is the potential for increased premiums. As healthcare costs rise, MA plans may need to increase premiums to maintain profitability, potentially making them less attractive to beneficiaries on fixed incomes. Another challenge is the potential for reduced plan choice and competition in certain geographic areas, particularly in rural or underserved communities. This could lead to less favorable benefit packages and higher costs for beneficiaries in those regions.
Finally, concerns about the quality of care provided by some MA plans, including issues related to access to specialists and timely care, could erode public confidence and hinder enrollment growth.
Potential Policy Interventions
Several policy interventions could significantly influence future MA enrollment trends. These interventions could focus on addressing the challenges mentioned above and promoting a more equitable and sustainable MA system.
For example, policies aimed at controlling healthcare costs, such as negotiating drug prices or implementing value-based care models, could help to mitigate premium increases and make MA plans more affordable. Furthermore, policies promoting competition among MA plans, such as relaxing regulatory barriers to entry or incentivizing the expansion of MA plans into underserved areas, could improve plan choice and access to care.
Finally, policies focused on enhancing the quality of care provided by MA plans, such as strengthening quality reporting and oversight mechanisms, could improve beneficiary satisfaction and increase confidence in the program.
Closing Notes
The surge in Medicare Advantage enrollment is undeniably reshaping the American healthcare landscape. Understanding the forces behind this growth – from effective marketing to shifting demographics and government policies – is crucial for policymakers, healthcare providers, and individuals planning for their retirement. While the advantages of MA plans are clear for many, the long-term implications for Medicare spending and the overall healthcare system require careful consideration.
As we move forward, navigating the challenges and opportunities presented by this continued growth will be key to ensuring a sustainable and equitable healthcare system for all.
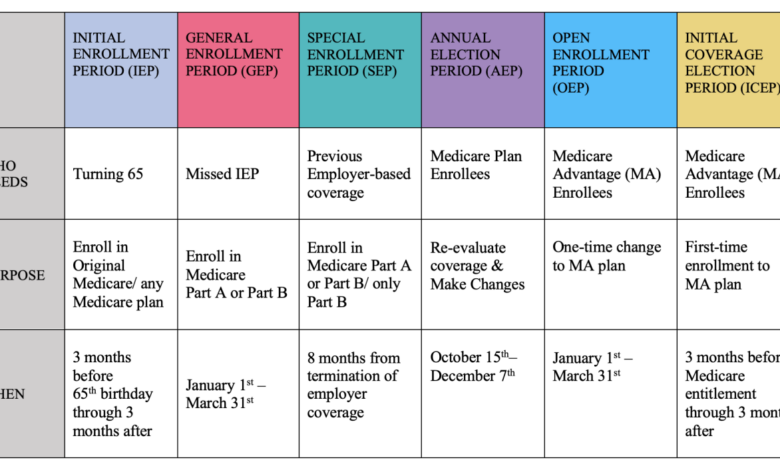
FAQ Guide: Medicare Advantage MA Enrollment Growth Health Affairs
What are the main differences between Medicare Advantage and traditional Medicare?
Medicare Advantage (MA) plans are offered by private companies and are an alternative to Original Medicare (Parts A and B). Traditional Medicare provides coverage through government-administered programs, while MA plans offer a more comprehensive package of benefits, sometimes including prescription drug coverage (Part D), but often with limitations on choice of providers.
Is Medicare Advantage right for everyone?
No, the suitability of Medicare Advantage depends on individual needs and preferences. Those who value flexibility and a wide choice of doctors might prefer traditional Medicare. However, individuals who prefer a more managed care approach and appreciate bundled benefits might find MA plans more advantageous.
How does the cost of Medicare Advantage compare to traditional Medicare?
Costs vary greatly depending on the specific plan. While MA plans often have monthly premiums, they may also have lower out-of-pocket costs in some cases compared to traditional Medicare. It’s essential to compare plans and costs carefully before enrolling.