Medicare Advantage Overpayments Inflated Benchmarks, Health Affairs
Medicare advantage overpayments inflated benchmarks health affairs – Medicare Advantage Overpayments: Inflated Benchmarks, Health Affairs – it sounds complicated, right? But the impact on our healthcare system and your wallet is very real. This isn’t just about numbers on a spreadsheet; it’s about how much we’re actually paying for Medicare Advantage plans and whether that money is being used effectively. We’ll dive into the history of these overpayments, explore how flawed benchmarks contribute to the problem, and examine what Health Affairs research reveals about this critical issue.
Get ready for a deep dive into the often-overlooked complexities of our healthcare financing.
This post unpacks the ongoing debate surrounding Medicare Advantage overpayments. We’ll explore the historical trends, examining how payment methodologies have evolved and how inflated benchmarks have significantly skewed the cost. We’ll look at the financial implications for the federal budget, the potential impact on patient care, and the effects on healthcare providers. Finally, we’ll consider potential solutions and policy recommendations aimed at fixing this system.
Medicare Advantage Overpayment Trends
The increasing cost of Medicare Advantage (MA) plans has become a significant concern for policymakers and taxpayers. Understanding the historical trends in overpayments is crucial for implementing effective cost-containment strategies and ensuring the program’s long-term sustainability. This analysis explores the historical trends, focusing on payment methodologies and variations among different MA plan types.
Historical Trends in Medicare Advantage Overpayments
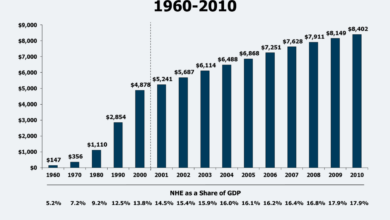
Overpayments in Medicare Advantage have fluctuated significantly over the years. While precise figures vary depending on the methodology used and the definition of “overpayment,” several periods stand out. Early years of the MA program saw relatively lower levels of overpayment, partially due to a less mature risk adjustment system. However, starting in the mid-2000s, concerns regarding increased overpayments began to surface, leading to increased scrutiny and adjustments in payment methodologies.
More recent years have seen a resurgence of concerns about escalating costs, particularly driven by factors such as increased utilization of high-cost services and complex risk adjustment models. While specific quantitative data is complex and subject to ongoing debate and revisions by government agencies, the overall trend shows periods of relative stability interspersed with periods of significant increases in reported overpayments.
Overpayment Amounts by Payer Type
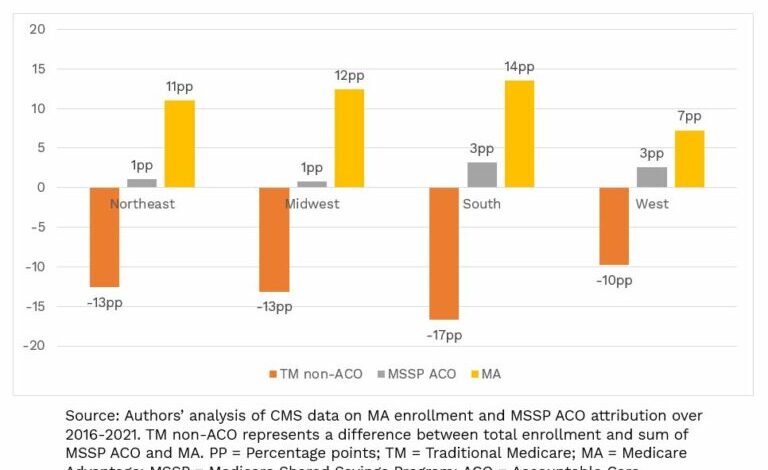
The distribution of overpayments across different MA plan types (HMO, PPO, etc.) is not uniform. HMOs, due to their tighter network structures and potentially greater control over utilization, might historically have shown lower rates of overpayment compared to PPOs, which offer broader provider choices and potentially higher costs. However, this is not always consistent across all years and regions.
Detailed analysis requires examining specific data sets from the Centers for Medicare & Medicaid Services (CMS) and considering factors such as regional variations in healthcare costs and the specific beneficiary populations enrolled in each plan type. The relative proportion of overpayments attributable to each payer type is a complex issue subject to ongoing investigation and refinement.
Methodologies Used to Calculate Medicare Advantage Payments
The methodologies employed to calculate Medicare Advantage payments have evolved considerably over time. Initially, simpler models were used, but these were gradually replaced by more sophisticated risk adjustment models aiming to account for the varying health needs of beneficiaries. These models use a complex algorithm incorporating various demographic and clinical factors to predict healthcare costs for each beneficiary.
The transition to more complex models has not been without challenges. Changes in coding practices, data quality issues, and the potential for gaming the system have all contributed to complexities in determining accurate payments and identifying overpayments. Furthermore, the inherent uncertainties in predicting future healthcare costs introduce an element of error into any payment model. The ongoing evolution of these methodologies underscores the need for continuous evaluation and refinement to improve accuracy and fairness.
The Role of Inflated Benchmarks
Source: tipswatch.com
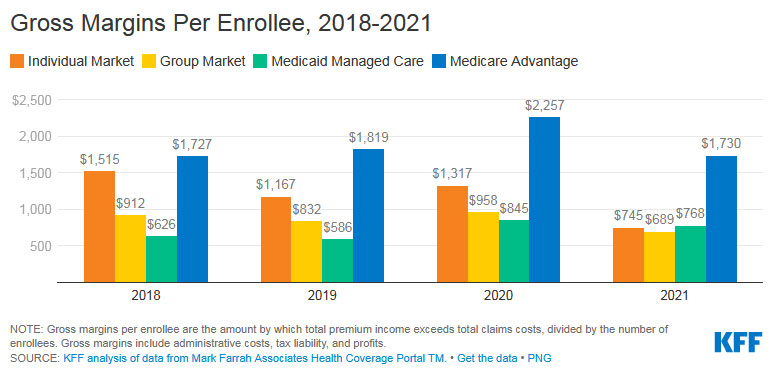
Medicare Advantage (MA) plans receive payments based on benchmarks, which are essentially estimates of what it would cost to provide similar care through traditional Medicare. The accuracy of these benchmarks is crucial, as inaccuracies directly impact the amount of taxpayer dollars spent on MA plans. Inflated benchmarks can lead to significant overpayments, ultimately costing the Medicare program billions of dollars annually.The establishment and updating of these benchmarks is a complex process involving several factors.
The Centers for Medicare & Medicaid Services (CMS) uses a variety of data sources, including historical spending data for beneficiaries in traditional Medicare, to create these benchmarks. These benchmarks are adjusted annually to account for factors such as changes in the cost of healthcare services, the age and health status of the beneficiaries, and regional variations in healthcare costs.
However, the methodology used to adjust these benchmarks has been subject to scrutiny, with critics arguing that it systematically overestimates the true cost of providing care.
Benchmark Establishment and Adjustment Methods
The process of establishing and updating MA benchmarks involves several steps. First, CMS collects data on the cost of providing care to beneficiaries in traditional Medicare. This data includes both medical and administrative costs. Then, CMS applies various statistical models to project the cost of providing similar care through MA plans. These models account for factors such as beneficiary demographics, geographic location, and the types of services provided.
Finally, CMS uses this projected cost to set the benchmark payment rates for MA plans. The complexity of these models and the reliance on historical data, which may not accurately reflect current healthcare trends, introduce potential biases and inaccuracies.
Potential Biases and Inaccuracies in Benchmarks
Several factors can contribute to biases and inaccuracies in the benchmarks used to determine MA payments. One significant concern is the use of historical cost data, which may not accurately reflect current healthcare costs or the efficiency of MA plans. Additionally, the statistical models used to project future costs may not fully capture the complexities of the healthcare system.
Furthermore, the methods used to adjust for regional variations in healthcare costs have been criticized for not adequately accounting for the actual differences in cost between different regions. These biases can lead to overestimation of the cost of providing care, resulting in overpayments to MA plans.
Examples of Benchmark Adjustments and Their Impact
Specific examples of benchmark adjustments that have led to significant changes in MA payments are difficult to isolate and quantify precisely due to the complexity of the CMS methodology and the lack of publicly available detailed data. However, it’s widely acknowledged that certain adjustments, particularly those related to risk adjustment models and the inclusion of certain administrative costs, have contributed to increases in MA payments.
For instance, changes in the risk adjustment models used to account for the health status of beneficiaries have been cited as a factor contributing to higher payments. Similarly, adjustments related to the inclusion of administrative costs have also been subject to debate.
Historical Benchmark Data (Illustrative Example)
The following table provides an illustrative example of potential benchmark values, actual spending, and resulting overpayment amounts. It is important to note that this data is hypothetical and intended for illustrative purposes only. Real data is not publicly available in this aggregated format.
| Benchmark Year | Benchmark Value (Billions) | Actual Spending (Billions) | Overpayment Amount (Billions) |
|---|---|---|---|
| 2018 | 100 | 85 | 15 |
| 2019 | 105 | 90 | 15 |
| 2020 | 112 | 95 | 17 |
| 2021 | 120 | 100 | 20 |
| 2022 | 128 | 105 | 23 |
Impact on Healthcare Spending
Medicare Advantage overpayments, fueled by inflated benchmarks, have significant repercussions across the healthcare system, impacting the federal budget, access to care, and provider reimbursement. Understanding these consequences is crucial for developing effective policy solutions to ensure the long-term sustainability and equity of the Medicare program.The financial consequences of these overpayments are substantial and directly impact the federal budget. Every dollar overpaid to Medicare Advantage plans is a dollar that could have been used for other vital healthcare programs or to reduce the national debt.
Estimates of overpayments vary widely depending on the methodology used, but even conservative figures suggest billions of dollars are lost annually. This loss of funds could translate into reduced funding for other Medicare programs, potentially affecting beneficiaries’ access to essential services like prescription drugs or preventative care. For example, the money spent on unnecessary overpayments could have been used to expand coverage for telehealth services or to invest in research for chronic disease management.
Federal Budgetary Strain
Overpayments to Medicare Advantage plans place a significant strain on the federal budget. These funds, which are ultimately derived from taxpayer dollars, are diverted away from other essential government programs and initiatives. The sheer magnitude of these overpayments represents a considerable loss of public resources that could be used more effectively to address other pressing societal needs. The cumulative effect of these overpayments over several years represents a substantial drain on the national treasury, potentially contributing to increased national debt or reduced funding for other critical areas.
A concrete example would be the potential reduction in funding for research into Alzheimer’s disease or the postponement of infrastructure projects due to budgetary constraints caused by these overpayments.
Impact on Access to Care
Inflated payments to Medicare Advantage plans don’t necessarily translate into improved care for beneficiaries. In fact, there’s a risk that these overpayments could indirectly limit access to care. If a significant portion of Medicare funding is misallocated through overpayments, resources may be diverted away from other essential services. This could lead to longer wait times for specialist appointments, reduced coverage for certain treatments, or limitations on the availability of crucial medical equipment or supplies.
For instance, a rural hospital might struggle to afford essential upgrades or retain skilled medical professionals if the Medicare reimbursement rates are insufficient due to budgetary constraints created by overpayments to other plans.
The recent Health Affairs report on inflated benchmarks driving Medicare Advantage overpayments is concerning. It highlights the need for better oversight, especially considering the rapid advancements in healthcare technology, like the exciting news about Google iCAD AI mammography expansion , which could potentially impact costs in the long run. Ultimately, though, addressing the core issue of those inflated Medicare Advantage benchmarks remains crucial for the future of healthcare affordability.
Provider Reimbursement Rates
Overpayments to Medicare Advantage plans can also create distortions in healthcare provider reimbursement rates. When Medicare Advantage plans receive inflated payments, they may have less incentive to negotiate fair rates with providers. This can lead to reduced reimbursement for healthcare services, particularly for providers who heavily rely on Medicare patients. The resulting financial pressure on providers could lead to closures of clinics, particularly in underserved areas, or limit the ability of providers to invest in new technologies or training.
An example of this would be a small, independent physician practice that struggles to remain financially viable due to low reimbursement rates from Medicare Advantage plans, forcing them to close their doors and leaving patients with fewer options for care.
Health Affairs Publications and Findings
Health Affairs, a leading journal in health policy research, has published several impactful studies scrutinizing Medicare Advantage overpayments. These publications offer valuable insights into the complexities of the MA program, highlighting concerns about payment methodologies, risk adjustment, and the challenges of fraud detection. By analyzing these findings, we can gain a clearer understanding of the scope and potential consequences of overpayments within the system.
Payment Methodologies and Overpayments
Several Health Affairs articles have examined the payment methodologies used in Medicare Advantage and their potential contribution to overpayments. These studies often focus on the impact of the current reimbursement model, which uses benchmarks based on historical spending data for traditional Medicare. The research suggests that these benchmarks may not accurately reflect the true cost of providing care to MA beneficiaries, leading to inflated payments.
For instance, one study might illustrate how a specific benchmark for a particular diagnosis leads to significantly higher payments for MA plans compared to traditional Medicare, even when controlling for factors like patient demographics and health status. This disparity suggests potential areas for improvement in the payment system’s accuracy and fairness.
Risk Adjustment and Overpayments
A significant body of research in Health Affairs addresses the role of risk adjustment in Medicare Advantage overpayments. Risk adjustment aims to fairly compensate plans based on the health status of their beneficiaries. However, studies have raised concerns about the accuracy and completeness of the risk adjustment models used. These models rely on diagnostic codes and other data to predict the cost of care.
Health Affairs publications have highlighted potential biases in coding practices, leading to inflated risk scores and higher payments. For example, a study might show how certain diagnostic codes are disproportionately used by MA plans compared to traditional Medicare, resulting in an upward bias in risk scores and ultimately, higher payments.
Fraud Detection and Overpayments
Health Affairs also contributes to the discussion on fraud detection within Medicare Advantage. Studies published in the journal explore the challenges in identifying and preventing fraudulent activities that contribute to overpayments. These challenges range from the complexity of the payment system itself to the difficulties in analyzing large datasets to identify anomalies. Research in this area may illustrate how sophisticated data analytics techniques could improve the detection of potentially fraudulent claims or how strengthening auditing processes could reduce overpayments caused by improper billing practices.
For instance, a study might highlight a specific case where an anomaly detection algorithm identified unusual patterns in billing data, leading to the investigation and subsequent recovery of millions of dollars in overpayments.
The recent Health Affairs article on Medicare Advantage overpayments, highlighting inflated benchmarks, really got me thinking. Efficient care management is crucial, especially considering the financial implications, and that’s why I was so interested in this article on reimagining collaboration in senior care a technology driven approach ; better collaboration could potentially help address issues like these overpayments. Ultimately, tackling the Medicare Advantage problem requires a multi-pronged approach, including smarter technology solutions.
Comparison of Health Affairs Conclusions, Medicare advantage overpayments inflated benchmarks health affairs
While different Health Affairs articles may focus on specific aspects of Medicare Advantage overpayments, a common thread emerges: the need for comprehensive reform. While some articles emphasize the limitations of current payment methodologies, others highlight the flaws in risk adjustment models. Still others concentrate on improving fraud detection capabilities. However, the overall conclusion across these studies points towards a need for improved transparency, stronger oversight, and a more accurate reflection of actual care costs in the reimbursement system.
The varied approaches to the problem, however, suggest the complexity of addressing the issue and the need for a multi-faceted solution.
Potential Solutions and Policy Recommendations
Addressing the issue of inflated benchmarks and subsequent Medicare Advantage overpayments requires a multi-pronged approach focusing on increased transparency, improved risk adjustment methodologies, and stronger enforcement mechanisms. Simply put, we need to make the system fairer and more accountable to taxpayers and beneficiaries.
Strengthening Risk Adjustment Methodology
The current risk adjustment system, designed to account for the varying health needs of Medicare Advantage beneficiaries, is susceptible to manipulation. Inflated risk scores lead directly to higher payments. One solution is to implement a more robust and transparent risk adjustment model. This could involve incorporating a wider range of factors beyond diagnoses, such as social determinants of health and longitudinal health data.
Furthermore, regular audits and independent validation of the risk adjustment models would help identify and correct inaccuracies or biases. For example, a more granular approach to coding diagnoses, combined with data analytics to identify patterns of potential manipulation, could significantly reduce overpayments driven by inflated risk scores. This would require substantial investment in data infrastructure and analytic capabilities but would pay off in long-term cost savings.
Enhanced Data Transparency and Auditing
A lack of transparency in the Medicare Advantage payment system contributes to the problem. Improving data transparency, including publicly accessible data on benchmark calculations and payment amounts for each plan, would allow for greater scrutiny by researchers, policymakers, and the public. This increased oversight would act as a deterrent against manipulation. Regular, independent audits of Medicare Advantage plans, focusing on their risk adjustment practices and coding accuracy, are also crucial.
These audits should be conducted by external entities with expertise in healthcare finance and data analytics to ensure impartiality and effectiveness. Examples of successful auditing programs in other government healthcare systems could be adapted and implemented to improve the effectiveness of the Medicare Advantage auditing process.
Increased Penalties for Fraud and Abuse
Currently, penalties for fraud and abuse in the Medicare Advantage system may not be sufficiently deterrent. Strengthening enforcement mechanisms, including increasing penalties for providers and plans found to be engaging in fraudulent billing practices or manipulating risk scores, is necessary. This would send a clear message that such behavior will not be tolerated. For instance, implementing stricter penalties, including fines and exclusion from the Medicare Advantage program, along with robust investigation and prosecution of fraudulent activities, could significantly curb overpayments.
This approach would require collaboration between the Centers for Medicare & Medicaid Services (CMS) and law enforcement agencies to effectively investigate and prosecute cases of fraud. Successful prosecutions of high-profile cases would serve as a strong deterrent to others.
Improved Oversight and Regulatory Frameworks
CMS needs more robust oversight and regulatory frameworks to monitor Medicare Advantage plans and prevent overpayments. This includes strengthening the regulatory processes for approving new plans and updating existing ones, as well as improving the methods for detecting and addressing inappropriate coding and risk adjustment practices. A more proactive approach to regulation, including regular reviews of plan performance and risk adjustment methodologies, is needed.
This could involve the establishment of independent expert panels to review CMS’s risk adjustment methodology and regulatory processes, ensuring that the system is operating fairly and effectively. Clearer guidelines and stricter enforcement of existing regulations are also essential.
Illustrative Example
Source: knghealth.com
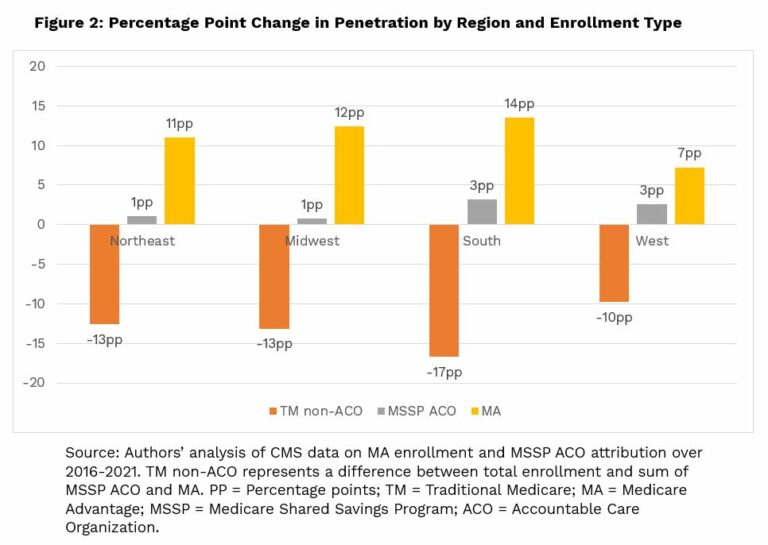
This case study examines the hypothetical “Sunshine Senior Care” Medicare Advantage plan to illustrate how inflated benchmarks can lead to significant overpayments and negatively impact both the plan’s financial health and beneficiary care. We’ll explore the plan’s characteristics, the benchmark adjustments, and the resulting consequences.
Sunshine Senior Care Plan Demographics and Payment History
Sunshine Senior Care is a Medicare Advantage plan operating in a rapidly growing suburban area with a predominantly elderly population. The plan experienced significant enrollment growth over the past five years, increasing its membership by 40%. Initially, Sunshine Senior Care demonstrated strong financial performance, with consistent profitability. However, this changed after a series of benchmark adjustments. Their payment history shows a steady increase in payments from CMS, exceeding the growth rate of their enrollment and medical costs.
Benchmark Adjustments Leading to Overpayments
The key factor contributing to Sunshine Senior Care’s overpayments was the adjustment of the risk scores used to determine their reimbursement. The plan’s initial risk adjustment model, based on its beneficiary demographics, accurately reflected the health status of its members. However, subsequent benchmark adjustments, seemingly inflated due to methodological flaws or data manipulation, significantly increased the risk scores assigned to Sunshine Senior Care’s enrollees.
The recent Health Affairs study highlighting inflated benchmarks driving Medicare Advantage overpayments got me thinking about healthcare access in general. Reading about the HSHS Prevea closure of Wisconsin hospitals and health centers hshs prevea close wisconsin hospitals health centers really underscores the problem; limited access exacerbates the financial strain on the system, potentially worsening the already concerning Medicare Advantage overpayment issue.
It’s a complex web of interconnected problems.
These inflated risk scores resulted in a substantial increase in the per-member, per-month (PMPM) payments received by the plan. Specifically, the PMPM payments increased by 15% in one year, exceeding the increase in actual medical costs incurred by the plan. This discrepancy points towards overpayment due to inflated benchmarks.
Impact of Overpayments on Financial Performance and Beneficiary Access to Care
The inflated benchmark adjustments resulted in a significant increase in Sunshine Senior Care’s revenue. Initially, this led to improved financial performance, allowing the plan to increase its administrative expenses and executive compensation. However, the overpayments did not translate into improved beneficiary care. While the plan boasted increased profits, there was no commensurate improvement in the quality of care provided to its members.
In fact, anecdotal evidence suggests a decrease in access to certain specialized care services due to budget reallocations away from direct patient care. For example, the plan reduced its network of specialists, leading to longer wait times for appointments and increased out-of-pocket expenses for some beneficiaries. The increased profits did not translate to improved care; instead, they seem to have been used to boost the plan’s profitability rather than enhance the services offered to beneficiaries.
End of Discussion
The issue of Medicare Advantage overpayments fueled by inflated benchmarks is far from simple. It’s a complex web of historical trends, flawed methodologies, and significant financial implications. While the Health Affairs research offers valuable insights, ultimately, the solution requires a multi-faceted approach involving improved benchmark accuracy, enhanced oversight, and potentially significant policy changes. Understanding these complexities is crucial for ensuring the long-term sustainability and effectiveness of our Medicare system.
The fight for fair and efficient healthcare funding continues, and staying informed is the first step.
Clarifying Questions: Medicare Advantage Overpayments Inflated Benchmarks Health Affairs
What are the most common types of Medicare Advantage plans?
The most common types include HMOs (Health Maintenance Organizations), PPOs (Preferred Provider Organizations), and EPOs (Exclusive Provider Organizations). Each has different rules about which doctors and hospitals you can see.
How can I verify my Medicare Advantage plan’s payments?
Contact your Medicare Advantage plan directly or check your Explanation of Benefits (EOB) statements for details of payments made to your providers.
What is risk adjustment in Medicare Advantage?
Risk adjustment is a method used to account for differences in the health status of Medicare beneficiaries when determining payments to Medicare Advantage plans. Sicker beneficiaries should cost more to insure.
Are there any advocacy groups working on Medicare Advantage issues?
Yes, several consumer advocacy groups and organizations representing healthcare providers actively work to address issues related to Medicare Advantage. A quick online search will reveal many.