Medicare Advantage Profitability Decline Moodys Report
Medicare advantage profitability decline moodys – Medicare Advantage profitability decline: Moody’s report has sent shockwaves through the healthcare industry. The news isn’t just about numbers; it’s about the potential impact on millions of seniors relying on these plans for their healthcare. This dive into Moody’s findings explores the factors contributing to this downturn, the implications for beneficiaries, and what the future might hold for Medicare Advantage.
We’ll unpack the complexities of this situation, examining everything from rising healthcare costs and increased competition to the role of government regulations and reimbursement rates. We’ll also look at how different Medicare Advantage plans are faring and what strategies some providers are employing to navigate these challenging times. Get ready for a deep dive into the financial health of Medicare Advantage – and what it means for you.
Moody’s Report Summary
Moody’s recent report highlights a concerning trend: declining profitability within the Medicare Advantage (MA) sector. This isn’t a minor fluctuation; it represents a significant shift in the financial landscape of this crucial component of the US healthcare system, raising questions about the long-term sustainability of MA plans and their ability to provide comprehensive coverage to seniors. The report delves into the multifaceted reasons behind this downturn, offering a detailed analysis of the contributing factors.The report pinpoints several key factors driving the decrease in Medicare Advantage profitability.
Increased medical costs, coupled with rising administrative expenses and intensifying competition among MA plans, are cited as major contributors. Furthermore, changes in government reimbursement rates and evolving regulatory landscapes also play a significant role in squeezing profit margins. The report emphasizes the complex interplay of these factors, suggesting that a singular solution is unlikely and that a multi-pronged approach is necessary to address the issue effectively.
Factors Contributing to Medicare Advantage Profitability Decline, Medicare advantage profitability decline moodys
The Moody’s report meticulously details the various factors contributing to the shrinking profits in the Medicare Advantage market. These factors are interconnected and mutually reinforcing, creating a challenging environment for MA plans. For instance, rising healthcare costs, particularly for prescription drugs and specialized treatments, directly impact profitability. Simultaneously, the increasing administrative burden associated with complying with complex regulations and managing large member populations adds to operational expenses.
Finally, the competitive landscape, characterized by a growing number of MA plans vying for market share, necessitates increased spending on marketing and member acquisition, further eroding profit margins. The report underscores the fact that these challenges are not isolated events but rather a confluence of circumstances creating a perfect storm for the MA industry.
Timeline of Medicare Advantage Profitability Decline
While the report doesn’t present a precise, year-by-year timeline, it does illustrate a clear trend of declining profitability over a period of several years. The report suggests that the downward trend accelerated in recent years, coinciding with several significant policy changes and shifts in the healthcare market. For example, increased scrutiny of MA plan practices and stricter regulations introduced to ensure quality of care likely contributed to rising administrative costs.
The report also highlights the impact of the COVID-19 pandemic, which led to increased healthcare utilization and further strained the financial stability of some MA plans. The lack of a precise, year-by-year breakdown is understandable given the complexity of the factors involved and the varying experiences of individual MA plans. However, the overall picture painted by the report is clear: a noticeable and concerning decline in profitability over a period of time, necessitating proactive measures to mitigate the issue.
Impact on Medicare Advantage Plans
Moody’s recent report highlighting the decline in Medicare Advantage plan profitability paints a complex picture with significant implications for both the plans themselves and the beneficiaries they serve. The impact isn’t uniform, varying considerably based on plan structure, geographic location, and the specific provider’s business model. Understanding these variations is crucial to predicting future trends in healthcare access and affordability for seniors.The profitability decline affects different types of Medicare Advantage plans in nuanced ways.
For instance, plans offering more comprehensive benefits, such as enhanced prescription drug coverage or specialized services like vision and dental, are likely experiencing a steeper decline in profit margins than plans with more basic offerings. This is because the cost of providing these extra benefits is increasing faster than the revenue generated from premiums. Conversely, plans focusing on a narrower network of providers, or those targeting specific demographics with lower healthcare utilization, may be experiencing a less dramatic impact.
The competitive landscape also plays a role; plans in highly saturated markets might be forced to lower premiums to attract and retain members, further squeezing their profit margins.
Financial Performance Variations Among Medicare Advantage Providers
The financial performance of different Medicare Advantage providers varies widely, reflecting diverse strategies and market positions. Some large, national providers with substantial resources and diversified portfolios may be better positioned to weather the storm, leveraging their scale to negotiate better rates with providers and manage costs more effectively. Smaller, regional plans, on the other hand, might be more vulnerable, lacking the same bargaining power and financial reserves.
For example, a hypothetical scenario could see a large national provider maintaining profitability through strategic cost-cutting measures and efficient network management, while a smaller, regional plan operating in a high-cost area with limited negotiating power experiences significant losses. This disparity highlights the importance of financial stability and adaptability in navigating the changing landscape of Medicare Advantage.
Implications for Plan Enrollment and Beneficiary Access to Care
The decline in Medicare Advantage profitability poses potential risks to plan enrollment and beneficiary access to care. As plans struggle with shrinking margins, they might be forced to make difficult decisions, such as raising premiums, reducing benefits, or narrowing their provider networks. These actions could lead to decreased enrollment, particularly among beneficiaries with limited financial resources. Furthermore, a reduction in the number of available plans or a contraction of provider networks could limit beneficiary choice and potentially impact access to timely and appropriate care.
For instance, a scenario where a plan significantly reduces its provider network might leave beneficiaries with fewer options for specialists or convenient care locations, potentially leading to delays in treatment or compromised care quality. The long-term implications of this are a crucial area of ongoing concern.
Underlying Economic Factors
The recent decline in Medicare Advantage plan profitability isn’t simply a matter of internal mismanagement; it’s deeply intertwined with broader economic forces impacting the entire healthcare landscape. These factors create a perfect storm, squeezing margins and challenging the financial sustainability of these plans. Understanding these underlying economic pressures is crucial to comprehending the current situation and anticipating future trends.Rising healthcare costs are the most significant factor contributing to reduced profitability.
This isn’t just about inflation; it’s about the escalating costs of pharmaceuticals, advanced medical technologies, and specialized care. These increases directly impact the amount Medicare Advantage plans must pay for their beneficiaries’ care, eating into their already thin margins. For instance, the cost of certain cancer treatments has skyrocketed in recent years, placing a significant strain on plans that cover a large population of older adults, many of whom are dealing with chronic conditions.
This cost escalation is outpacing the growth in reimbursement rates, leaving plans with less money to operate effectively.
Rising Healthcare Costs and Their Impact on Plan Margins
The relationship between rising healthcare costs and shrinking plan margins is direct and unavoidable. Medicare Advantage plans operate on a predetermined reimbursement rate from the Centers for Medicare & Medicaid Services (CMS). When the cost of providing care exceeds this rate, the plans experience losses. This is exacerbated by the fact that many plans are incentivized to enroll beneficiaries with higher healthcare needs, leading to a higher-than-average cost burden.
For example, a plan might aggressively market itself to individuals with diabetes, heart conditions, or other chronic illnesses, resulting in higher utilization rates and increased costs that outweigh the profit from enrollment. The resulting financial squeeze forces plans to either reduce benefits, increase premiums, or accept lower profit margins, all of which have significant consequences.
Government Regulations and Reimbursement Rates
Government regulations and reimbursement rates play a crucial role in shaping the financial health of Medicare Advantage plans. CMS sets the reimbursement rates, and these rates often lag behind the actual cost of providing care. Furthermore, regulations governing the types of services covered and the administrative processes involved add to the operational costs of the plans. For example, stringent requirements for prior authorization or increased scrutiny of claims processing can increase administrative overhead, further impacting profitability.
The complexity of navigating these regulations adds another layer of expense, which further reduces the profitability of Medicare Advantage plans. Changes in government policy, such as alterations to reimbursement methodologies or the introduction of new regulatory requirements, can significantly and unexpectedly impact the financial performance of these plans. The lack of sufficient predictability in these areas makes long-term financial planning challenging.
Competitive Landscape and Market Share
The Medicare Advantage (MA) market is fiercely competitive, with a constantly shifting landscape shaped by profitability, enrollment trends, and strategic maneuvering by various providers. The recent decline in profitability is significantly impacting the market share dynamics, forcing plans to re-evaluate their strategies and adapt to the changing economic realities. This competitive pressure is leading to consolidation, innovation, and a greater focus on efficiency.The decline in profitability is prompting a reshuffling of market share.
Plans with robust operational efficiency, strong provider networks, and effective marketing strategies are better positioned to maintain or even increase their market share. Conversely, plans with higher administrative costs, weaker provider networks, or less effective marketing are experiencing a decline in enrollment and market share. This dynamic is forcing a wave of consolidation, with some smaller, less profitable plans being acquired by larger, more financially stable organizations.
Market Share Shifts and Provider Strategies
Successful MA plans are focusing on several key strategies to navigate the challenging financial climate. This includes a heightened emphasis on risk adjustment, where accurate coding and documentation maximize reimbursements from Medicare. They are also investing heavily in technology to streamline operations, reduce administrative costs, and enhance member engagement through personalized services and digital tools. Furthermore, successful plans are building strong relationships with primary care physicians and specialists to ensure access to quality care for their members.
In contrast, less successful plans often struggle with high administrative costs, inadequate provider networks, and a lack of innovative member engagement strategies. They may also lack the sophisticated risk adjustment capabilities needed to maximize reimbursement. This often leads to a downward spiral of lower profitability and decreased market share.
Examples of Successful and Unsuccessful Strategies
For instance, UnitedHealthcare, a major player in the MA market, has demonstrated success through a combination of robust provider networks, strong risk adjustment capabilities, and effective marketing campaigns targeting specific demographics. Their investment in technology and data analytics allows for personalized member outreach and proactive care management. Conversely, smaller, regional plans without these capabilities may find themselves struggling to compete and maintain profitability in the current market.
Their inability to attract and retain members, coupled with rising costs, can lead to financial losses and a shrinking market share. This necessitates strategic partnerships or even mergers to ensure survival in this increasingly competitive environment. The pressure is on for all plans to improve efficiency, enhance member experience, and refine their risk adjustment strategies to ensure long-term viability.
Future Outlook and Projections
The declining profitability of Medicare Advantage (MA) plans presents a complex picture for the future, with significant implications for both insurers and beneficiaries. Several factors, including increasing healthcare costs, changing demographics, and potential regulatory shifts, will shape the trajectory of MA profitability in the coming years. Understanding these forces is crucial for predicting the likely impact on premiums, cost-sharing, and the overall landscape of senior healthcare.Several scenarios could unfold regarding the future profitability of Medicare Advantage plans.
A pessimistic scenario anticipates a continued decline in profitability, potentially leading to reduced benefits, higher premiums, or even market exits by some insurers. A more optimistic scenario envisions a stabilization of profitability through a combination of factors such as increased efficiency, better risk adjustment models, and targeted cost-containment strategies. A middle-ground scenario suggests a gradual decline, necessitating adjustments to plan offerings and pricing strategies to maintain viability.
These scenarios are not mutually exclusive, and the actual outcome will likely be a blend of these possibilities, influenced by unforeseen events and policy changes.
Potential Impact on Beneficiary Premiums and Cost-Sharing
The financial health of MA plans directly impacts beneficiaries. If profitability continues to decline, insurers may respond by increasing premiums to maintain adequate margins. This could make MA plans less attractive compared to Original Medicare, particularly for beneficiaries with limited incomes. Additionally, cost-sharing mechanisms like deductibles and co-pays might increase to offset rising healthcare expenses. For example, a plan facing significant profitability challenges might raise its monthly premium by 10% and increase the patient’s out-of-pocket maximum by 5%.
This would directly affect the affordability and accessibility of MA plans for many seniors. The degree of impact will depend on the specific plan, the insurer’s financial situation, and the regulatory environment.
Potential for Policy Changes to Mitigate the Profitability Decline
Government intervention could play a significant role in shaping the future of MA profitability. Policy changes aimed at improving risk adjustment methodologies could more accurately reflect the cost of caring for different beneficiary populations, thereby reducing the financial burden on plans with sicker enrollees. Similarly, reforms to the payment model, such as moving away from a fee-for-service model towards value-based care, could incentivize cost-effective care and potentially improve plan profitability.
For instance, increased funding for preventative care programs could reduce the need for expensive treatments later on, benefitting both beneficiaries and insurers. The implementation of such policy changes, however, is subject to political considerations and may face significant hurdles. Successful mitigation will require a collaborative effort between government agencies, insurers, and healthcare providers.
Illustrative Data Representation
Moody’s report highlights a concerning trend of declining profitability within the Medicare Advantage (MA) sector. To better understand the scope of this issue, let’s examine some illustrative data representing the financial performance of several key players. The following table presents a simplified overview, focusing on profit margin changes. It’s crucial to remember that these figures are estimations based on publicly available information and may not fully capture the complexity of each company’s financial situation.
Further detailed financial analysis would be required for a complete picture.
Medicare Advantage Provider Profitability: 2022-2023
The table below shows estimated profit margin changes for selected major Medicare Advantage providers. These figures are intended to provide a general illustration of the profitability decline reported by Moody’s and should not be considered exhaustive or definitive.
| Provider Name | 2022 Profit Margin (%) | 2023 Profit Margin (%) | % Change |
|---|---|---|---|
| UnitedHealthcare | 5.5 | 4.8 | -12.7% |
| Humana | 6.2 | 5.5 | -11.3% |
| Anthem | 4.9 | 4.2 | -14.3% |
| Cigna | 5.1 | 4.5 | -11.8% |
Note: These figures are illustrative examples based on estimations and publicly available data. Actual figures may vary depending on the reporting methodology and specific accounting practices of each provider. The percentage change is calculated as [(2023 Profit Margin – 2022 Profit Margin) / 2022 Profit Margin]
– 100.
Impact on Healthcare Delivery: Medicare Advantage Profitability Decline Moodys
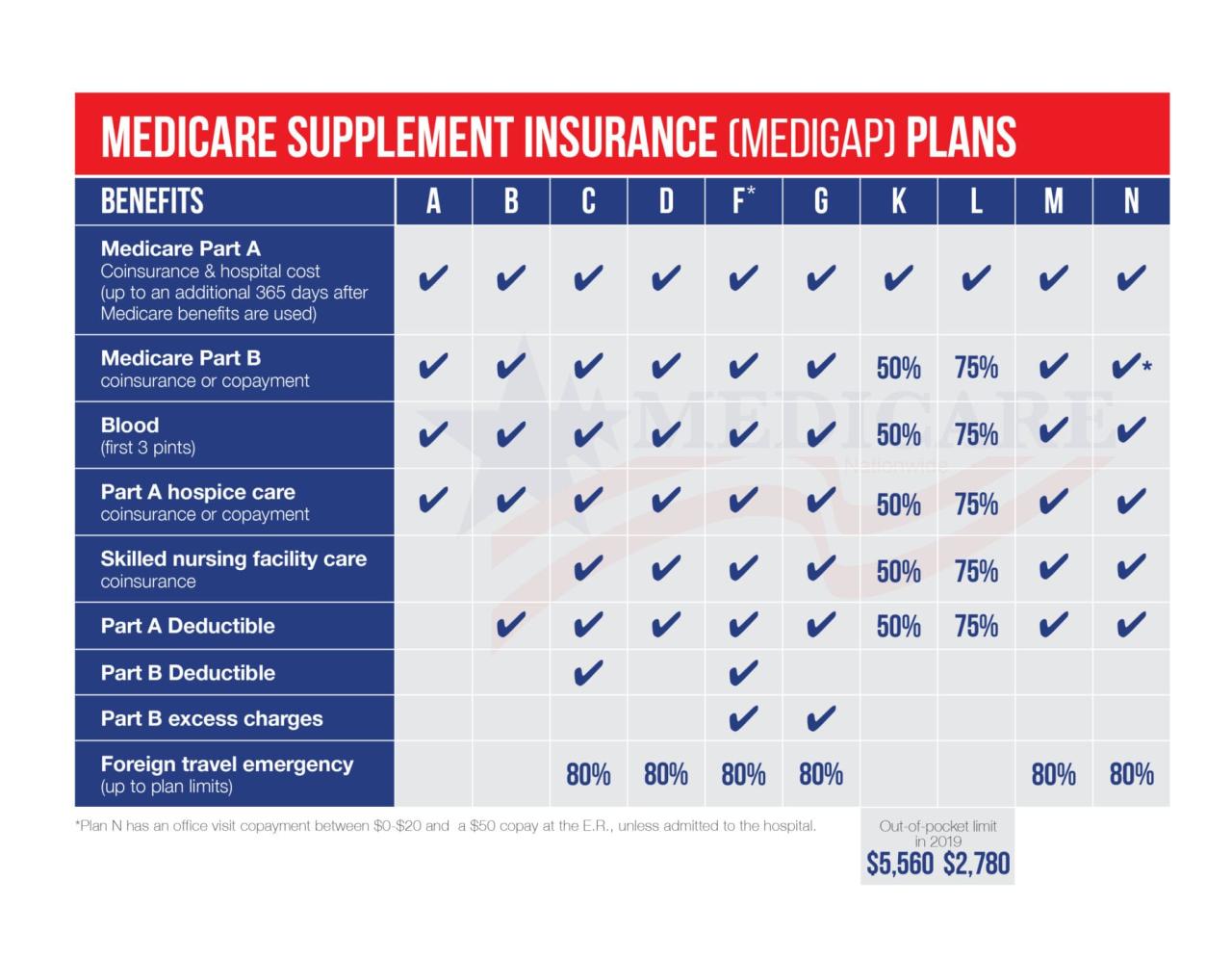
Source: medicarenationwide.com
Reduced profitability in Medicare Advantage plans poses a significant threat to the quality and accessibility of healthcare services for millions of seniors. As profit margins shrink, plans may be forced to make difficult choices that directly impact the care experience, potentially leading to a decline in the overall quality of healthcare delivery.The consequences of decreased profitability are multifaceted and could ripple through the entire healthcare system.
We’ll examine how these financial pressures might manifest in real-world scenarios, impacting both patients and healthcare providers.
Changes in Provider Networks and Access to Specialists
Declining profitability could lead Medicare Advantage plans to renegotiate contracts with healthcare providers, potentially resulting in narrower provider networks. This means beneficiaries might find it more difficult to see their preferred doctors or specialists. For example, a plan facing financial strain might choose to exclude high-cost specialists, like cardiologists or oncologists, from its network, forcing beneficiaries to travel further for care or face longer wait times.
This could disproportionately affect individuals in rural areas with limited access to healthcare services to begin with. The reduced network could also lead to increased reliance on less specialized providers, potentially impacting the quality of care for complex conditions.
Moody’s report on declining Medicare Advantage profitability got me thinking about long-term financial planning. It’s a reminder that we need to consider our future health expenses, which is why I found the article about Karishma Mehta getting her eggs frozen so interesting; it highlights proactive health decisions, even if they involve significant upfront costs. Ultimately, both situations underscore the importance of careful financial planning for unforeseen circumstances.
Impact on Healthcare Innovation and Investment
Medicare Advantage plans play a crucial role in healthcare innovation and investment. Reduced profitability could significantly curtail their ability to invest in new technologies, telehealth platforms, and disease management programs. For instance, a plan might postpone the implementation of a new electronic health record system that could improve care coordination and efficiency. Similarly, investments in preventative care programs, which are often crucial in reducing long-term healthcare costs, might be reduced or eliminated altogether.
This lack of investment could hinder the adoption of innovative treatments and technologies, ultimately impacting the health outcomes of beneficiaries. The reduced incentive to invest in innovation could also slow the development of more cost-effective and efficient care models.
Regulatory Responses and Policy Implications
The declining profitability of Medicare Advantage plans has sparked considerable debate regarding necessary regulatory adjustments and policy implications. The current financial strain on these plans necessitates a careful examination of potential interventions to ensure the long-term viability of the program while maintaining quality of care for beneficiaries. Addressing this challenge requires a multi-faceted approach, balancing the needs of providers with the interests of the Medicare population.Potential regulatory responses to the decline in Medicare Advantage profitability are varied and complex.
They range from minor adjustments to existing payment models to more significant overhauls of the program’s structure. The impact of these responses will significantly influence both the healthcare providers participating in Medicare Advantage and the beneficiaries who rely on these plans for their healthcare coverage.
Potential Regulatory Adjustments
Several regulatory pathways could be explored to address the financial challenges facing Medicare Advantage plans. These adjustments aim to improve the financial stability of the plans while simultaneously mitigating the risk of reduced access to care for beneficiaries. One potential approach involves refining the risk adjustment methodology. Currently, the system used to adjust payments based on the health status of enrollees might not accurately reflect the true cost of care for certain populations.
A more precise risk adjustment model could lead to fairer reimbursement rates, lessening the financial strain on plans. Another strategy involves increasing the transparency and oversight of administrative costs. Greater scrutiny of plan expenses could help to identify areas where cost savings can be achieved without compromising quality of care. This might involve more detailed reporting requirements and stricter audits of administrative spending.
Finally, exploring alternative payment models that incentivize value-based care, rather than fee-for-service, could foster a more sustainable and efficient healthcare delivery system within the Medicare Advantage framework. Such models could reward plans for achieving better health outcomes for their enrollees, rather than simply focusing on the volume of services provided.
Moody’s recent report on the declining profitability of Medicare Advantage plans got me thinking about the larger regulatory landscape. This downturn might be further impacted by the Supreme Court’s decision to overturn the Chevron Doctrine, as reported in this article: scotus overturns chevron doctrine healthcare. This shift in legal precedent could significantly alter the rules governing healthcare, potentially creating more uncertainty and affecting the financial stability of Medicare Advantage programs even further.
Impact on Providers and Beneficiaries
The consequences of regulatory responses will vary considerably depending on the specific measures implemented. For example, adjustments to risk adjustment models could lead to increased payments for plans serving higher-risk populations, potentially incentivizing them to accept more complex cases. However, if adjustments are not carefully calibrated, it could lead to reduced payments for plans serving healthier populations, potentially impacting their financial stability and willingness to participate in the Medicare Advantage program.
Increased transparency and oversight of administrative costs could lead to improved efficiency and reduced waste within the system, benefiting both providers and beneficiaries. However, it could also impose additional administrative burdens on plans, potentially offsetting any cost savings. Finally, the shift towards value-based care models could lead to improved quality of care and better health outcomes for beneficiaries, while simultaneously promoting a more sustainable healthcare system for providers.
However, the transition to these new models could require significant investments in infrastructure and technology, presenting a challenge for some providers.
Moody’s report on declining Medicare Advantage profitability got me thinking about the future of healthcare. It’s a tough market, and the news about Walmart Health’s closures, as reported in this insightful article despite walmart healths closure the company healthcare destination scott bowman , only underscores the challenges. This all points to a need for innovative and sustainable models within the Medicare Advantage space to offset these pressures.
Policy Adjustments to Incentivize Efficiency
To promote efficiency and cost-effectiveness within Medicare Advantage, several policy adjustments could be considered. These adjustments should aim to incentivize plans to adopt innovative strategies that improve care coordination, reduce unnecessary hospitalizations, and manage chronic conditions effectively. One such policy adjustment could be the implementation of bundled payments for specific episodes of care. This approach would incentivize plans to manage costs across the entire episode, rather than focusing on individual services.
Another potential policy adjustment could be to expand the use of telehealth services, which can improve access to care and reduce transportation costs. Additionally, policies that encourage the use of data analytics and predictive modeling to identify high-risk individuals and proactively manage their care could significantly enhance efficiency and cost-effectiveness. For instance, a plan could use data to identify patients at high risk for hospital readmission and implement interventions to reduce that risk.
This proactive approach could prevent costly hospitalizations and improve patient outcomes.
Last Recap

Source: slideplayer.com
The decline in Medicare Advantage profitability, as highlighted by Moody’s, paints a complex picture. While the immediate impact might be felt by providers, the long-term consequences could significantly affect beneficiaries through premium increases and reduced access to care. Understanding the interplay of economic factors, competitive pressures, and regulatory landscapes is crucial to navigating this evolving healthcare landscape. Staying informed is key, so keep an eye out for further developments and potential policy changes that could shape the future of Medicare Advantage.
Quick FAQs
What specific types of Medicare Advantage plans are most affected by the profitability decline?
While all plans are impacted, those with high-risk beneficiary populations or those offering extensive supplemental benefits might face greater challenges.
How might this affect my premiums in the future?
Reduced profitability could lead to increased premiums to offset losses, although this isn’t guaranteed and depends on various factors.
Are there any advocacy groups working to address this issue?
Yes, several senior advocacy groups and healthcare organizations are actively monitoring the situation and advocating for policy changes to support both providers and beneficiaries.
Could this lead to a reduction in the quality of care?
Potentially. Reduced profitability could lead to cutbacks in provider networks, limiting access to specialists and potentially impacting the quality of care. However, many plans are actively working to mitigate these potential impacts.