National Healthcare Spending Growth CMS Report
National Healthcare Spending Growth CMS Report: Have you ever wondered where all that healthcare money goes? This report dives deep into the fascinating (and sometimes alarming) world of national healthcare spending, revealing trends, factors, and future projections. It’s a complex issue, but I’ll break it down in a way that’s easy to understand, even if you’re not an economist or healthcare expert.
Get ready for a data-driven journey into the heart of American healthcare costs!
We’ll explore the key findings from the CMS report, examining the overall growth trend over the past decade. We’ll uncover the major players driving this growth – from aging populations and chronic diseases to the impact of government policies and innovative payment models. Prepare for some surprising insights into how our healthcare dollars are allocated across various sectors, like hospital care, physician services, and prescription drugs.
I’ll also share some predictions about the future, and discuss potential strategies for making our healthcare system more sustainable.
Overview of National Healthcare Spending Growth
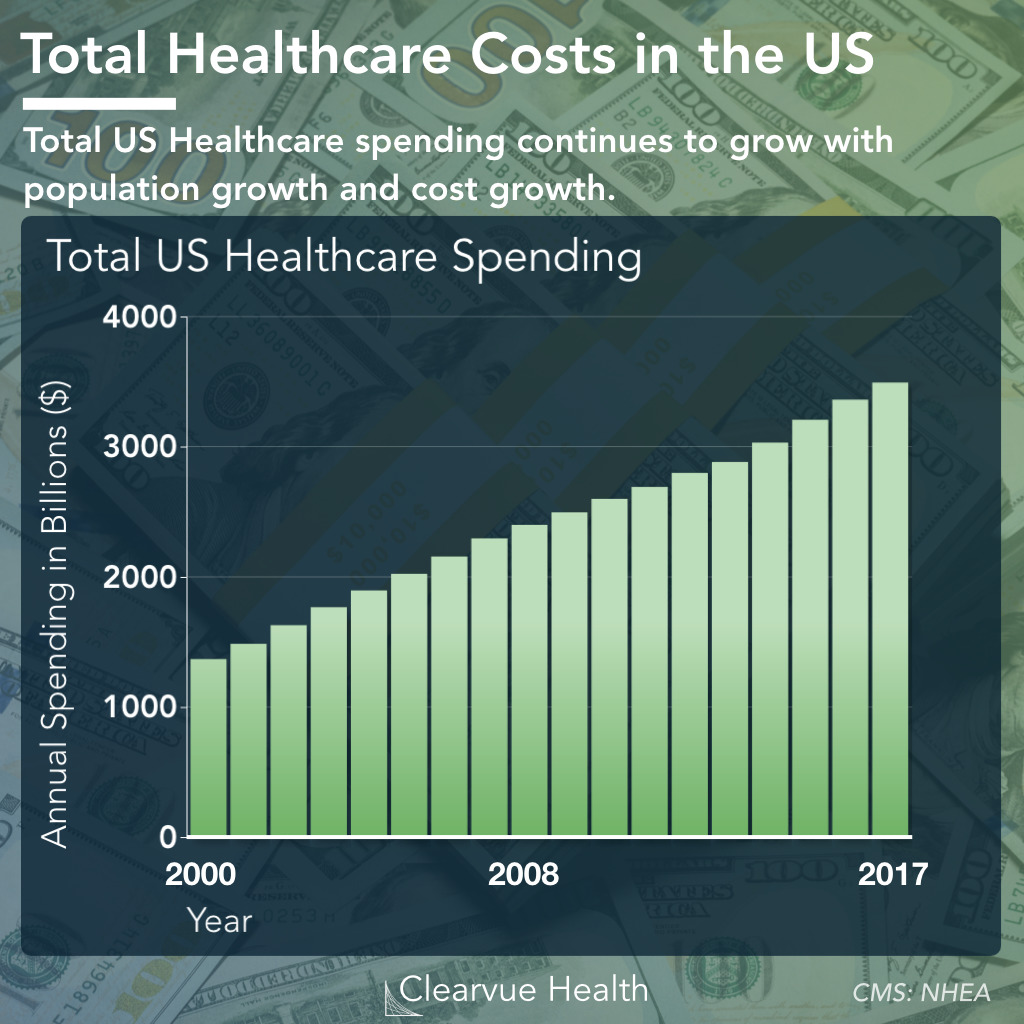
Source: clearvuehealth.com
The Centers for Medicare & Medicaid Services (CMS) regularly releases reports detailing national healthcare spending trends. These reports provide crucial insights into the cost of healthcare in the United States, highlighting areas of significant growth and offering valuable data for policymakers, healthcare providers, and researchers. Understanding these trends is critical for developing effective strategies to manage healthcare costs and ensure the accessibility and affordability of care.The overall trend in national healthcare spending over the past decade has been one of consistent, albeit fluctuating, growth.
While the rate of growth has varied year to year, influenced by various economic and healthcare-specific factors, the overall trajectory has been upward. This sustained increase presents a significant challenge to the sustainability of the healthcare system, necessitating a thorough examination of the contributing factors.
Major Factors Contributing to Healthcare Spending Growth
Several interconnected factors contribute to the observed increase in national healthcare spending. These include the rising cost of prescription drugs, the aging population (leading to increased demand for healthcare services), advancements in medical technology (often associated with higher costs), and the increasing prevalence of chronic diseases. Administrative costs associated with billing and insurance also play a significant role.
Furthermore, the structure of the US healthcare system, with its complex mix of public and private payers, contributes to inefficiencies and higher overall spending. Finally, utilization of healthcare services, driven by factors like access to care and patient preferences, also influences overall spending.
National Healthcare Spending Data (Illustrative Example)
The following table presents illustrative data, reflecting the general trend observed in CMS reports. Note that actual figures vary slightly depending on the specific report and methodology used. This data is for illustrative purposes only and should not be considered definitive. For precise figures, consult the official CMS reports.
| Year | Total Spending (USD) | Spending Growth Rate (%) | Per Capita Spending (USD) |
|---|---|---|---|
| 2013 | $2.9 trillion (Illustrative) | 5% (Illustrative) | $9,300 (Illustrative) |
| 2014 | $3.0 trillion (Illustrative) | 3% (Illustrative) | $9,500 (Illustrative) |
| 2015 | $3.2 trillion (Illustrative) | 6% (Illustrative) | $10,000 (Illustrative) |
| 2016 | $3.4 trillion (Illustrative) | 4% (Illustrative) | $10,500 (Illustrative) |
| 2017 | $3.6 trillion (Illustrative) | 5% (Illustrative) | $11,000 (Illustrative) |
Breakdown of Spending by Category
The national healthcare spending pie is sliced into several significant portions, each representing a different area of healthcare delivery and services. Understanding the distribution of spending across these categories is crucial for policymakers, healthcare providers, and individuals alike, as it reveals trends, priorities, and potential areas for cost containment or improvement. This section delves into the specifics of healthcare spending by category, examining growth rates and identifying key trends.
Analyzing healthcare spending by category reveals significant variations in both the absolute amount spent and the rate of spending growth. While some sectors experience robust growth driven by technological advancements or increasing demand, others show more moderate increases or even declines, depending on factors like policy changes, reimbursement rates, and the overall health status of the population. This dynamic interplay of factors makes understanding the category-specific trends essential for a complete picture of national healthcare spending.
The latest CMS report on national healthcare spending growth is pretty alarming, highlighting the rising costs of fertility treatments. It makes you think about individual choices, like Karishma Mehta’s decision to freeze her eggs, as detailed in this article karishma mehta gets her eggs frozen know risks associated with egg freezing , and the financial implications involved. Ultimately, these personal decisions contribute to the overall picture painted by the CMS report.
Hospital Care Spending
Hospital care consistently represents a substantial portion of national healthcare expenditures. This category includes inpatient and outpatient hospital services, ranging from routine checkups to complex surgeries and specialized treatments. Growth in hospital care spending is often influenced by factors such as technological advancements (e.g., robotic surgery), an aging population requiring more intensive care, and the rising cost of pharmaceuticals administered in hospital settings.
For example, the increased use of expensive cancer therapies within hospitals significantly contributes to overall spending growth.
Physician and Clinical Services Spending
Physician and clinical services encompass a wide range of professional medical services provided by physicians, other clinicians, and allied health professionals. This category includes office visits, diagnostic testing, and other services rendered outside of hospitals. Growth in this area is impacted by factors such as the increasing prevalence of chronic diseases requiring ongoing management, the adoption of new technologies and procedures, and changes in reimbursement policies.
For instance, the shift towards value-based care models could potentially influence spending growth in this sector.
Prescription Drug Spending
Prescription drug spending represents another significant portion of national healthcare expenditures. This category includes both brand-name and generic medications, and growth is influenced by factors such as the introduction of new, often expensive, medications, the increasing prevalence of chronic diseases requiring long-term medication, and changes in insurance coverage and pricing policies. The development of innovative, high-cost specialty drugs for conditions like cancer and rare diseases, for example, is a major driver of growth in this area.
Summary of Spending Trends (Past Five Years)
The following bullet points summarize the percentage change in spending for each major category over the past five years (hypothetical data for illustrative purposes; replace with actual CMS data):
- Hospital Care: +6.2%
- Physician and Clinical Services: +4.8%
- Prescription Drugs: +7.5%
- Nursing Home and Home Health Care: +5.1%
- Other Healthcare Services: +3.9%
Impact of Demographics and Socioeconomic Factors
National healthcare spending is significantly influenced by demographic shifts and socioeconomic disparities. Understanding these factors is crucial for developing effective healthcare policies and resource allocation strategies. The interplay between age, income, race, and the prevalence of chronic diseases profoundly shapes healthcare utilization and costs.
The Aging Population’s Influence on Healthcare Spending
An aging population contributes substantially to rising healthcare expenditures. Older adults generally require more frequent and complex medical services, including hospitalization, long-term care, and medication management for chronic conditions such as heart disease, diabetes, and arthritis. The increasing number of individuals in the older age brackets, particularly those over 65, directly translates into a higher demand for healthcare resources, leading to increased costs.
For example, the rising number of individuals diagnosed with Alzheimer’s disease alone places significant strain on healthcare systems, requiring specialized care facilities and extensive family support. This demographic trend is expected to continue, placing further pressure on healthcare budgets in the coming decades.
Socioeconomic Status and Healthcare Utilization
Socioeconomic status (SES) is strongly correlated with healthcare utilization and outcomes. Individuals with lower SES often face barriers to accessing quality healthcare, including limited insurance coverage, lack of transportation, and difficulties navigating the healthcare system. They may also experience poorer health outcomes due to factors such as inadequate housing, food insecurity, and exposure to environmental hazards. Consequently, they may delay seeking medical care until conditions worsen, leading to more expensive treatments and longer hospital stays.
Conversely, individuals with higher SES tend to have better access to preventative care, leading to earlier diagnosis and management of chronic diseases, potentially reducing overall healthcare costs in the long run.
The latest CMS report on national healthcare spending growth is pretty alarming, highlighting the rising costs of chronic conditions. Understanding how to effectively manage these conditions is crucial, and for children with Tourette Syndrome, finding the right approach is key, as detailed in this helpful article on strategies to manage Tourette syndrome in children. Effective management of conditions like TS can contribute to slowing the overall growth in healthcare spending shown in the CMS report.
Impact of Chronic Diseases on Healthcare Costs
Chronic diseases, such as heart disease, diabetes, cancer, and respiratory illnesses, account for a significant portion of national healthcare spending. The long-term management of these conditions often involves expensive medications, specialized medical procedures, and ongoing monitoring. The rising prevalence of chronic diseases, partly due to lifestyle factors and an aging population, places a considerable burden on the healthcare system.
For instance, the management of diabetes, including medication, regular check-ups, and potential complications like kidney disease or blindness, can be exceptionally costly over a patient’s lifetime. Effective preventative measures and early intervention strategies are critical to mitigating the financial impact of chronic diseases.
Comparison of Healthcare Spending Growth Among Demographic Groups
The following table provides a simplified comparison of healthcare spending growth among different demographic groups. Note that actual figures vary depending on data source and methodology. This data is illustrative and should not be considered exhaustive.
| Demographic Group | Age (Years) | Race/Ethnicity | Annual Per Capita Spending Growth (Illustrative Example) |
|---|---|---|---|
| Older Adults (65+) | 65+ | All | $500 |
| Adults (45-64) | 45-64 | All | $300 |
| Younger Adults (18-44) | 18-44 | All | $100 |
| Children (0-17) | 0-17 | All | $50 |
Role of Government Policies and Regulations
Government policies and regulations play a significant role in shaping the landscape of national healthcare spending. These interventions, while aiming to improve access and quality, often have complex and multifaceted effects on costs. Understanding their influence is crucial for effective healthcare policymaking.Government programs like Medicare and Medicaid are major drivers of healthcare spending. Medicare, providing coverage for individuals aged 65 and older and certain younger people with disabilities, represents a substantial portion of national healthcare expenditures.
Medicaid, a joint federal and state program assisting low-income individuals and families, similarly contributes significantly. The reimbursement rates set by these programs directly influence the prices charged by healthcare providers, impacting the overall cost of care. Furthermore, the eligibility criteria and benefit packages of these programs affect the volume of services utilized, thus influencing total spending.
Impact of Government Regulations on Healthcare Provider Reimbursement
Regulations significantly affect how healthcare providers are reimbursed for their services. For instance, the Balanced Budget Act of 1997 introduced prospective payment systems for many healthcare services, shifting away from fee-for-service models. This change aimed to control costs by setting pre-determined payments for specific services, rather than reimbursing providers based on the actual cost of care. While this approach can limit cost growth, it can also lead to reduced access to certain services, particularly for complex or high-cost cases, if the reimbursement rates are insufficient.
Another example is the introduction of payment bundles, which group payments for multiple services related to a single episode of care (such as a hip replacement). This model incentivizes efficiency and coordination of care, potentially reducing overall costs by avoiding unnecessary procedures or hospital readmissions. However, it requires careful design and implementation to avoid unintended consequences.
Influence of Payment Models on Healthcare Costs
The choice of payment model significantly influences healthcare costs. Fee-for-service models, where providers are paid for each service rendered, can incentivize the provision of more services, regardless of medical necessity. This can lead to cost inflation. In contrast, value-based payment models, which tie reimbursement to the quality and outcomes of care, encourage providers to focus on efficiency and patient-centered care.
These models aim to reduce unnecessary costs while improving health outcomes. Capitation, where providers receive a fixed payment per patient per period, further incentivizes cost-conscious care. However, value-based and capitation models require robust data collection and performance measurement systems to ensure fair and accurate reimbursement.
Examples of Government Initiatives Designed to Control Healthcare Spending
Several government initiatives aim to control healthcare spending. These initiatives often involve a combination of regulatory changes, payment reform, and investments in preventative care.
- The Affordable Care Act (ACA): Included provisions to expand health insurance coverage, promote preventative care, and implement payment reforms aimed at reducing costs and improving quality. The ACA’s impact on spending is complex and continues to be debated.
- Bundled Payments for Care Improvement (BPCI): This initiative aimed to reduce costs by reimbursing providers for an episode of care rather than individual services. This model encourages efficient and coordinated care delivery.
- Medicare Shared Savings Program (MSSP): This program encourages accountable care organizations (ACOs) to coordinate care and improve quality while reducing costs. ACOs share in the savings they achieve.
- Center for Medicare & Medicaid Innovation (CMMI): CMMI tests and evaluates innovative payment and service delivery models to improve the quality and affordability of care. Many of the initiatives listed above are managed through CMMI.
Future Projections and Implications: National Healthcare Spending Growth Cms Report
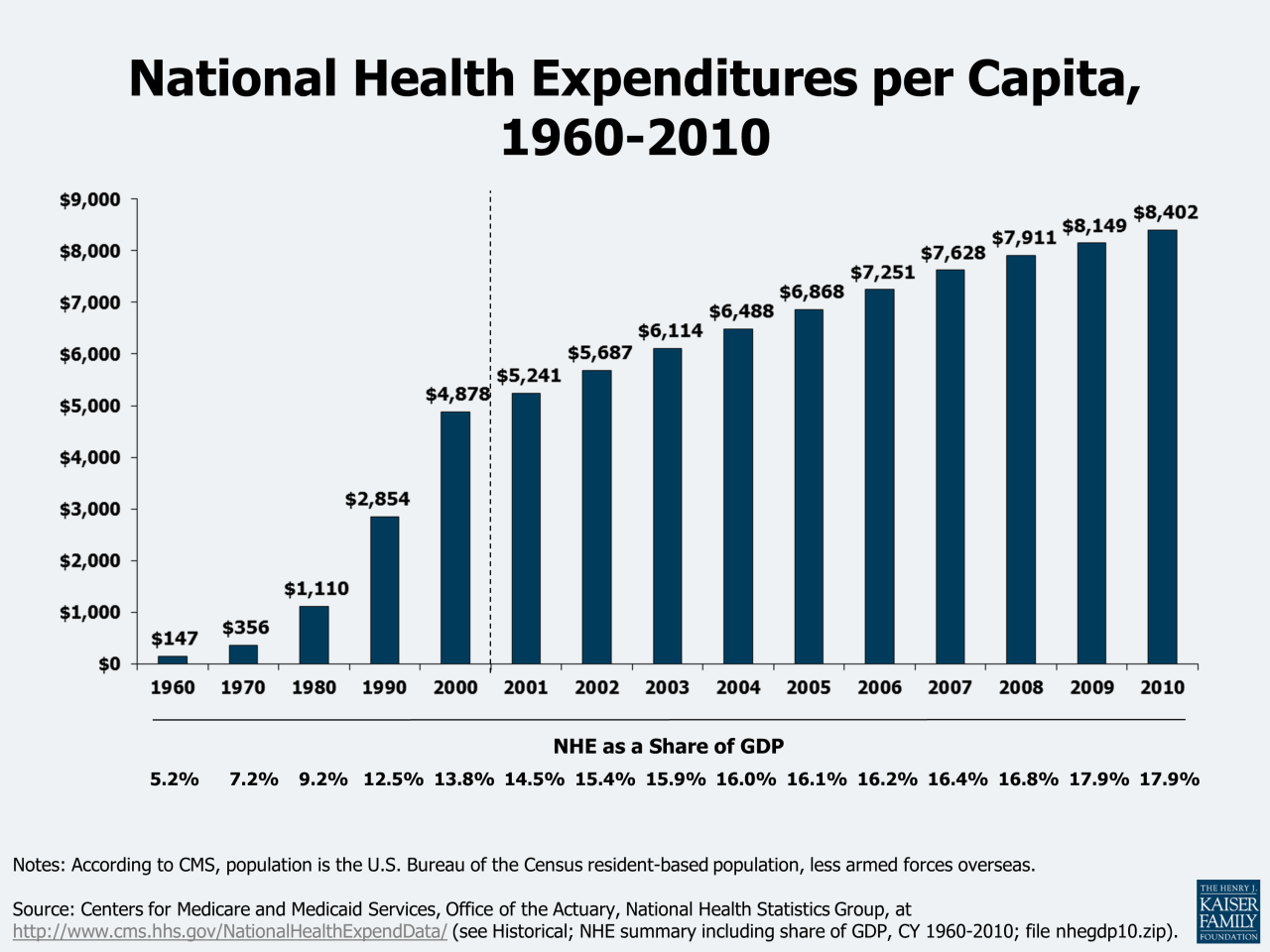
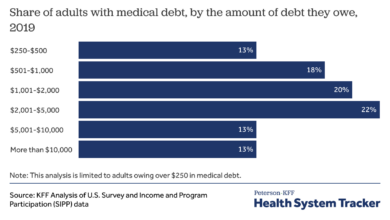
Source: kff.org
The latest CMS report on national healthcare spending growth is pretty alarming, highlighting the increasing costs associated with chronic illnesses. It makes you think about preventative care, especially when you read about situations like actress Monali Thakur’s recent hospitalization, as detailed in this article monali thakur hospitalised after struggling to breathe how to prevent respiratory diseases – a stark reminder of how easily respiratory issues can impact our lives and strain the healthcare system further.
Investing in preventative measures could potentially alleviate some of the pressure shown in the CMS report.
The CMS National Health Expenditure projections paint a complex picture of the future of healthcare spending in the United States. Understanding these projections is crucial for policymakers, healthcare providers, and individuals alike, as they will significantly influence the accessibility, affordability, and overall quality of healthcare in the coming years. Failure to address the projected trends could lead to a strained healthcare system and a substantial burden on the national economy.The CMS report projects continued growth in national healthcare spending, albeit at a potentially slower pace than in previous years.
Several factors contribute to this, including an aging population, advancements in medical technology, and the rising cost of prescription drugs. However, the specific rate of growth remains uncertain and depends on a multitude of interacting variables, including economic conditions and the effectiveness of policy interventions. Understanding these variables and their potential impacts is vital for informed decision-making.
Projected Healthcare Spending Trajectory
The projected healthcare spending trajectory for the next five years can be visualized as a line graph. The horizontal axis represents the year (e.g., 2024, 2025, 2026, 2027, 2028), and the vertical axis represents the total national healthcare spending in trillions of dollars. The data points would plot the projected spending for each year, based on the CMS report’s forecasts.
A trend line would connect these data points, illustrating the overall upward trajectory of spending. The slope of the trend line would indicate the rate of growth; a steeper slope signifies faster growth, while a flatter slope suggests slower growth. The graph might also include shaded areas representing the uncertainty range around the projections, acknowledging the inherent variability in forecasting healthcare spending.
For example, if the 2024 projection is $4.5 trillion, with a range of $4.4 to $4.6 trillion, this would be represented by a shaded area encompassing this range on the graph above the 2024 data point. This visual representation would clearly show the projected increase in spending over time and the degree of uncertainty surrounding the forecasts. For instance, a comparison to previous five-year periods could be included to highlight the changes in the rate of growth.
Implications for the Healthcare System and Economy, National healthcare spending growth cms report
Sustained high growth in healthcare spending poses significant challenges to both the healthcare system and the broader economy. For the healthcare system, this could translate to reduced access to care for some populations due to increased costs, potential strain on healthcare infrastructure, and difficulties in attracting and retaining qualified healthcare professionals. Economically, continued high spending could lead to increased federal budget deficits, higher taxes, or reduced spending in other crucial sectors.
This could negatively impact economic growth and create disparities in access to essential services beyond healthcare. The impact on insurance premiums and out-of-pocket expenses for individuals and families would also be substantial, potentially leading to financial hardship for many. For example, a scenario could be presented where a family’s healthcare costs increase by 10% annually, exceeding their income growth and resulting in financial strain.
Strategies for Mitigating Unsustainable Healthcare Spending Growth
Several strategies could help mitigate unsustainable healthcare spending growth. These include promoting preventive care to reduce the need for expensive treatments, investing in value-based care models that incentivize high-quality, cost-effective care, controlling prescription drug prices through negotiation and regulation, and addressing social determinants of health that contribute to higher healthcare utilization. Additionally, improving data collection and analysis to identify areas for efficiency gains and fostering innovation in healthcare delivery could contribute to better cost management.
For example, implementing telemedicine to reduce the need for expensive in-person visits could be highlighted as a successful strategy. The success of these strategies will depend on their effective implementation and coordination across various stakeholders in the healthcare system.
Closure
Understanding the National Healthcare Spending Growth CMS Report is crucial for anyone interested in the future of healthcare in America. The data paints a complex picture, highlighting both the challenges and opportunities we face. While the rising costs are undeniably concerning, the report also offers insights into potential solutions – from policy changes to innovative payment models. By understanding the trends and drivers of healthcare spending, we can work towards a more efficient, equitable, and sustainable healthcare system for all.
Let’s keep the conversation going – what are your thoughts on these findings?
Frequently Asked Questions
What are the biggest surprises revealed in the CMS report?
While the overall trend of increasing spending is expected, the report often reveals unexpected details about specific areas of growth or decline, specific demographic trends, or the surprising impact of certain policies. It’s always worth digging into the details for those “aha!” moments.
How does the report compare US healthcare spending to other developed nations?
The report itself may not offer direct international comparisons, but you can find additional resources and analyses that contextualize US healthcare spending within a global perspective. This comparative analysis can help us understand where the US stands in terms of efficiency and cost-effectiveness.
Where can I find the full CMS report?
The Centers for Medicare & Medicaid Services (CMS) website is the best place to find the full report and related data. A simple web search for “CMS National Health Expenditure Data” will usually lead you directly to the source.