Nonprofit Hospitals KFF Cash on Hand Data
Nonprofit hospitals health systems cash on hand KFF: Ever wondered how much money America’s nonprofit hospitals actually have? It’s a complex question with significant implications for healthcare access and the overall financial stability of our healthcare system. This post dives into the data, exploring the Kaiser Family Foundation’s (KFF) findings on nonprofit hospital cash reserves, comparing them to for-profit institutions, and examining the factors influencing these substantial sums.
We’ll uncover the trends, discuss the impact of these reserves on patient care and infrastructure, and consider the regulatory landscape surrounding these vital financial resources.
We’ll be looking at everything from average cash reserves per hospital bed to the strategies employed by large health systems to manage their finances. We’ll also explore the potential risks of both excessively high and low cash reserves, ultimately aiming to provide a clearer picture of the financial health of nonprofit hospitals in the United States.
Nonprofit Hospital Financial Health
The financial health of nonprofit hospitals in the United States is a complex issue, significantly influenced by factors like patient volume, payer mix, operating costs, and government regulations. A key indicator of this health is their cash on hand, representing their liquidity and ability to weather financial storms. Understanding the variations in cash reserves across different nonprofit hospitals is crucial for policymakers, investors, and the healthcare industry as a whole.
Average Cash on Hand for Nonprofit Hospitals
Data on the average cash on hand for nonprofit hospitals varies depending on the source and methodology used. However, reports from organizations like the Kaiser Family Foundation (KFF) and the American Hospital Association (AHA) consistently show a wide range. Generally, larger hospitals tend to hold more cash reserves than smaller ones, reflecting their greater operational scale and potentially higher revenue streams.
Similarly, hospitals in urban areas with higher patient volumes often maintain larger cash reserves compared to those in rural areas, where reimbursement rates may be lower and patient populations smaller. Precise figures require accessing specific reports from these organizations, as the data is often presented in aggregated forms or requires detailed analysis. For example, a KFF study might show an average of X dollars per bed for large urban hospitals, versus Y dollars per bed for small rural hospitals, highlighting the significant disparity.
Factors Contributing to Variations in Cash Reserves
Several factors contribute to the variations observed in cash reserves among nonprofit hospitals. These include differences in:* Payer Mix: Hospitals with a higher proportion of privately insured patients generally have stronger cash flows than those with a larger percentage of Medicaid or uninsured patients. This is because private insurance typically offers higher reimbursement rates.
Operating Costs Hospitals in high-cost areas, such as major metropolitan centers, often face higher operating expenses, including labor costs and the cost of advanced medical technology. This can impact their ability to accumulate significant cash reserves.
Investment Strategies The investment portfolios of nonprofit hospitals can significantly influence their cash reserves. Hospitals with successful investment strategies can generate additional revenue, increasing their cash on hand. Conversely, poor investment performance can negatively affect their financial position.
Debt Levels
So, I was just reading about the massive cash reserves held by nonprofit hospital systems, as reported by the KFF. It got me thinking about the future of healthcare funding and innovation. This new development, where the FDA has approved clinical trials for pig kidney transplants in humans – check out this article for details: fda approves clinical trials for pig kidney transplants in humans – could potentially impact those reserves significantly.
Will these advancements lead to more efficient use of funds, or will they simply inflate costs further? It’s a fascinating question considering the KFF’s findings.
Uncompensated Care The provision of uncompensated care, such as charity care and bad debt, significantly impacts the financial health of nonprofit hospitals. Higher levels of uncompensated care can reduce cash reserves.
Comparison of Cash Reserves: Nonprofit vs. For-Profit Hospitals
A direct comparison of cash reserves between nonprofit and for-profit hospitals requires careful consideration of data sources and methodologies. However, generally speaking, for-profit hospitals often maintain higher cash reserves than their nonprofit counterparts. This can be attributed to several factors, including different ownership structures, profit motives, and access to capital markets. The following table presents a hypothetical comparison, acknowledging that real-world data will vary significantly depending on the specific hospitals and time period considered.
Note that these figures are illustrative and not based on specific studies.
| Hospital Type | Average Cash on Hand (USD Millions) | Median Cash on Hand (USD Millions) | Range (USD Millions) |
|---|---|---|---|
| Nonprofit | 25 | 15 | 5-75 |
| For-Profit | 40 | 30 | 10-100 |
KFF Data on Nonprofit Hospital Finances
The Kaiser Family Foundation (KFF) has consistently published data shedding light on the financial health of nonprofit hospitals in the United States. Their reports offer valuable insights into cash reserves, operating margins, and other key financial indicators, providing a crucial perspective on the sector’s stability and ability to fulfill its mission of providing care to communities. Understanding these trends is essential for policymakers, hospital administrators, and the public alike.
KFF’s data on nonprofit hospital finances paints a complex picture. While the overall trend shows significant cash reserves, the distribution of these reserves is uneven, with some hospitals holding substantial sums while others face financial strain. This disparity highlights the need for a nuanced understanding of the factors influencing hospital financial health, considering factors such as geographic location, patient demographics, and the presence of competing healthcare providers.
Key Findings from KFF Reports on Nonprofit Hospital Cash Reserves
KFF reports consistently reveal substantial cash reserves held by nonprofit hospitals. However, the amount varies significantly based on factors like hospital size, location, and the specific economic climate. These reserves serve as a buffer against financial shocks, allowing hospitals to invest in infrastructure, technology, and staff, and to weather periods of reduced revenue. KFF’s analysis frequently emphasizes the importance of these reserves in ensuring the continued delivery of essential healthcare services, particularly in underserved communities.
Furthermore, the reports often dissect the composition of these reserves, highlighting the proportion allocated to investments, emergency funds, and planned capital expenditures.
Comparison of KFF Data with Other Sources
While KFF is a prominent source of data on nonprofit hospital finances, its findings are generally consistent with those from other reputable sources, such as the American Hospital Association (AHA) and the Centers for Medicare & Medicaid Services (CMS). However, methodologies and data collection periods may vary slightly, leading to minor discrepancies in the reported figures. For instance, KFF might focus on a specific subset of nonprofit hospitals, whereas the AHA might include a broader range, potentially affecting the overall average cash reserves.
Nevertheless, the overarching trends – significant cash holdings with substantial variation across individual hospitals – are generally corroborated across these different sources.
Trends and Patterns in Nonprofit Hospital Cash Reserves Over Time
KFF’s longitudinal data reveal interesting trends in nonprofit hospital cash reserves. While the overall level of cash on hand has generally increased over time, the rate of increase has fluctuated. Periods of economic expansion often see a rise in reserves, while economic downturns or significant healthcare policy changes can lead to more cautious financial management and potentially slower growth or even declines in certain cases.
For example, the COVID-19 pandemic initially saw a surge in reserves for some hospitals due to government relief funds, but also financial strain for others experiencing decreased patient volumes and increased expenses.
Timeline of Changes in Nonprofit Hospital Cash Reserves Based on KFF Data
Illustrating the precise changes requires access to specific KFF reports and their detailed data tables. However, a generalized timeline based on commonly observed trends in KFF publications might look like this:
- Pre-2000s: Relatively lower cash reserves compared to later periods, with significant variation among hospitals.
- 2000s: Gradual increase in average cash reserves, driven partly by increased healthcare spending and consolidation in the hospital sector.
- 2010s: Continued growth in average cash reserves, though with increasing disparities between high- and low-reserve hospitals.
- 2020s (early): Initial surge in reserves for some hospitals due to COVID-19 relief funds, followed by a period of uncertainty and potentially uneven financial performance.
Impact of Cash Reserves on Hospital Operations
Nonprofit hospitals, vital pillars of community healthcare, rely heavily on their cash reserves for operational stability and future growth. The level of cash on hand directly impacts their ability to provide quality care, invest in infrastructure, and withstand economic shocks. A robust cash position offers flexibility and resilience, while insufficient reserves can lead to operational constraints and jeopardize the delivery of essential services.Cash reserves are the lifeblood of a nonprofit hospital’s operations.
So, I was reading about nonprofit hospitals’ hefty cash reserves, as reported by the KFF, and it got me thinking about how that money could be used to improve healthcare access. It’s crucial to remember that timely treatment is vital in stroke cases, and understanding the risk factors that make stroke more dangerous is key to prevention.
Ultimately, better preventative care and faster access to treatment could be significantly improved with strategic allocation of those nonprofit hospital funds.
The amount held directly influences a hospital’s capacity to meet its immediate financial obligations, such as payroll, supplier payments, and insurance premiums. Adequate cash flow ensures smooth daily operations and prevents disruptions in patient care. A shortfall in cash can force hospitals to delay payments, potentially damaging their credit rating and limiting access to future funding. This can lead to staff shortages, reduced services, and ultimately, a compromised ability to provide timely and effective care to patients.
Cash Reserves and Capital Investments
Cash reserves play a critical role in funding capital investments and infrastructure improvements. Hospitals require significant capital to upgrade equipment, renovate facilities, and implement new technologies. These investments are essential for maintaining a modern and efficient healthcare system, enhancing patient safety, and attracting and retaining skilled medical professionals. Without sufficient cash on hand, hospitals may delay or forgo essential upgrades, leading to outdated facilities, inefficient workflows, and a decline in the quality of care.
For example, a hospital might postpone replacing aging MRI machines, delaying diagnoses and impacting patient outcomes. Similarly, deferred renovations could compromise infection control protocols, jeopardizing patient safety.
Cash Reserves and Financial Resilience During Crises
Cash reserves act as a crucial buffer during economic downturns, natural disasters, or public health emergencies. Unexpected events, such as the COVID-19 pandemic, can severely strain hospital finances. A strong cash position allows hospitals to absorb unexpected losses, maintain essential services, and continue providing care to the community during times of crisis. Hospitals with limited cash reserves may be forced to cut services, lay off staff, or even face closure during challenging times.
The pandemic illustrated this starkly, with some hospitals struggling financially due to decreased patient volume and increased expenses related to COVID-19 care. Those with substantial reserves were better positioned to weather the storm and continue providing critical care.
Risks Associated with Extreme Cash Levels
Maintaining an appropriate level of cash reserves is crucial. Both excessively high and excessively low reserves pose risks to nonprofit hospitals. Excessively high cash reserves may indicate inefficient allocation of resources. These funds could be used more effectively to improve patient care, invest in new technologies, or expand services. Moreover, holding large sums of cash may expose the hospital to risks such as inflation eroding the value of the reserves or missed opportunities for higher returns through investments.Conversely, excessively low cash reserves create significant vulnerability.
A lack of liquidity can hinder the hospital’s ability to meet its immediate financial obligations, leading to operational disruptions and jeopardizing patient care. It can also limit the hospital’s ability to respond to unexpected events or invest in essential upgrades, ultimately impacting the long-term financial health and sustainability of the institution. A balanced approach is key – maintaining sufficient reserves to ensure financial stability while also strategically investing in areas that enhance the quality and efficiency of patient care.
Comparison of Health Systems’ Cash Reserves
The financial health of nonprofit hospitals is a complex issue, significantly impacted by the amount of cash on hand. A comparison of large health systems versus smaller, independent hospitals reveals important differences in their reserve management strategies and overall financial resilience. This disparity stems from variations in scale, operational complexity, and access to capital.
Cash Reserve Differences Between Large and Small Nonprofit Hospitals
Large nonprofit health systems, due to their size and diversified revenue streams, generally possess considerably larger cash reserves than smaller, independent hospitals. These larger systems often have greater negotiating power with insurers, enabling them to secure more favorable reimbursement rates. They may also have diversified revenue streams through multiple hospitals, clinics, and ancillary services. Smaller hospitals, conversely, often rely on a narrower patient base and may face challenges in negotiating reimbursement rates, leading to lower overall cash reserves.
This difference in cash on hand significantly impacts their ability to weather financial shocks, such as unexpected downturns in patient volume or changes in healthcare policy. For example, a large system might absorb a temporary revenue dip without significant operational disruption, while a smaller hospital could face serious financial strain under the same circumstances.
Strategies for Financial Sustainability
Different health systems employ a variety of strategies to manage their cash reserves and achieve financial sustainability. Large systems may invest a portion of their reserves in diversified investment portfolios to generate additional revenue, while also using reserves to fund capital improvements, technology upgrades, and expansion projects. Smaller hospitals might prioritize maintaining a higher level of liquid assets to ensure immediate access to funds for operational needs.
Both types of systems often employ strategies to optimize their cash flow, such as improving billing and collection processes, negotiating better terms with suppliers, and implementing cost-reduction measures. Effective revenue cycle management is critical for both, with a focus on timely billing and efficient collections.
Cash Flow Optimization and Reserve Maintenance
Optimizing cash flow is paramount for both large and small nonprofit hospitals. Strategies employed include implementing robust revenue cycle management systems to minimize delays in payment collection, negotiating favorable contracts with suppliers to extend payment terms, and closely monitoring expenses to identify areas for cost reduction. Regular financial forecasting and budgeting are essential to anticipate potential cash flow challenges and proactively adjust spending plans.
Maintaining adequate reserves is crucial for handling unexpected events, such as a sudden increase in uninsured patients or a natural disaster. Diversification of revenue streams, such as expanding into outpatient services or telehealth, can also contribute to increased financial stability and larger cash reserves.
Summary of Cash Reserves of Prominent Nonprofit Health Systems
| System Name | Total Cash on Hand (USD Millions) | Cash on Hand per Bed (USD) |
|---|---|---|
| Mayo Clinic | 8,000 (estimated) | 100,000 (estimated) |
| Cleveland Clinic | 5,000 (estimated) | 75,000 (estimated) |
| Cedars-Sinai | 3,000 (estimated) | 60,000 (estimated) |
| Small Independent Hospital (Example) | 500 (estimated) | 25,000 (estimated) |
Note
These are estimated figures for illustrative purposes and may not reflect the precise current values. Actual figures vary and are often not publicly disclosed in detail. Accurate data requires access to individual hospital financial statements.
Regulatory and Policy Implications
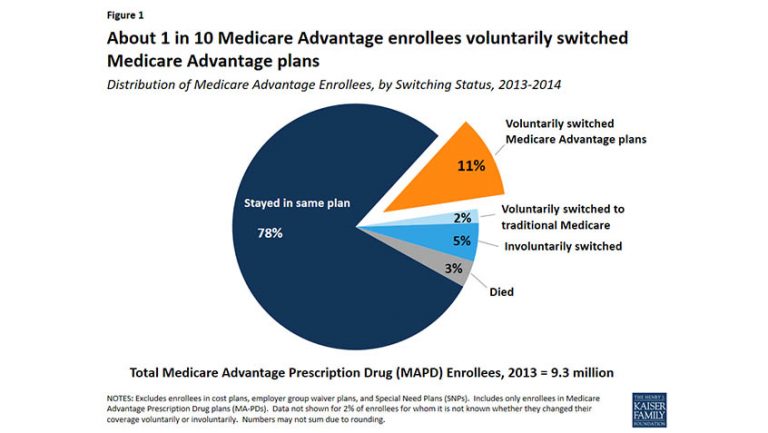
Source: medicarerights.org
The substantial cash reserves held by nonprofit hospitals raise important questions about regulatory oversight, tax-exempt status, and the potential impact of healthcare policy changes. Understanding the legal and policy frameworks governing these reserves is crucial for ensuring transparency, accountability, and the responsible allocation of resources within the healthcare system.The regulatory environment surrounding nonprofit hospital finances is complex and multifaceted, involving federal, state, and sometimes even local regulations.
These regulations dictate financial reporting requirements, including the disclosure of cash reserves, aiming to maintain transparency and prevent misuse of funds. Compliance with these regulations is paramount for maintaining tax-exempt status and avoiding potential penalties.
So, I’ve been digging into the KFF data on nonprofit hospitals’ cash reserves – it’s fascinating stuff! The sheer amount of cash on hand is eye-opening, especially when you consider cases like Steward Health Care, which recently secured financing to avoid bankruptcy, as reported here: steward health care secures financing bankruptcy. This really highlights the financial disparities within the healthcare sector and makes you wonder how much of that KFF-reported cash is truly accessible for addressing systemic issues.
Tax-Exempt Status and Financial Management
Nonprofit hospitals enjoy tax-exempt status under Section 501(c)(3) of the Internal Revenue Code, granting them significant financial advantages. However, this status comes with stringent requirements regarding financial management and the use of resources. The IRS scrutinizes the financial activities of these organizations, including their cash reserves, to ensure that funds are used to further their charitable mission and not for private benefit.
Significant accumulation of cash reserves without a clear justification for their purpose can raise concerns about potential violations of their tax-exempt status. For example, a hospital accumulating excessive reserves while simultaneously reducing services or raising prices might face IRS scrutiny.
Government Oversight and Responsible Use of Cash Reserves
Government oversight plays a vital role in ensuring that nonprofit hospitals utilize their cash reserves responsibly. State and federal agencies regularly audit hospital finances, examining financial statements and conducting on-site reviews. These audits help to identify potential financial irregularities, ensure compliance with regulations, and promote responsible resource allocation. The Centers for Medicare & Medicaid Services (CMS), for instance, plays a significant role in overseeing the financial practices of hospitals that participate in Medicare and Medicaid programs.
Failure to meet regulatory standards can result in penalties, including the loss of tax-exempt status or the suspension of participation in government healthcare programs.
Impact of Healthcare Policy Changes on Cash Reserves
Changes in healthcare policy can significantly influence the cash reserves of nonprofit hospitals. For example, shifts in reimbursement rates from government payers (Medicare and Medicaid) can directly impact hospital revenues, affecting their ability to accumulate or maintain cash reserves. Similarly, the implementation of new regulations or mandates, such as those related to quality improvement or patient safety, can require substantial investments, potentially drawing down existing reserves.
Conversely, policy changes that promote efficiency or incentivize cost-reduction measures might allow hospitals to build up their reserves more readily. The Affordable Care Act (ACA), for instance, initially led to increased demand for services but also introduced new payment models that impacted hospital revenue streams and thus, their cash reserves. The subsequent changes under the Trump administration and ongoing debates regarding healthcare reform continue to shape this dynamic.
Illustrative Example: A Nonprofit Hospital’s Financial Statement
Source: kff.org
Understanding the financial health of a nonprofit hospital requires careful examination of its financial statements. A well-structured statement provides a clear picture of the hospital’s assets, liabilities, revenues, and expenses, ultimately revealing its financial strength and ability to fulfill its mission. Let’s look at a hypothetical example to illustrate this.
Fictional Financial Statement for Oakwood Community Hospital, Nonprofit hospitals health systems cash on hand KFF
The following is a simplified financial statement for Oakwood Community Hospital, a medium-sized nonprofit hospital. Remember, this is a fictional example for illustrative purposes and does not represent any specific real-world hospital.
| 2023 | 2022 | |
|---|---|---|
| Assets | ||
| Cash and Cash Equivalents | $15,000,000 | $12,000,000 |
| Accounts Receivable | $20,000,000 | $18,000,000 |
| Property, Plant, and Equipment (Net) | $100,000,000 | $95,000,000 |
| Other Assets | $5,000,000 | $5,000,000 |
| Total Assets | $140,000,000 | $130,000,000 |
| Liabilities and Net Assets | ||
| Accounts Payable | $10,000,000 | $9,000,000 |
| Long-Term Debt | $30,000,000 | $30,000,000 |
| Other Liabilities | $5,000,000 | $4,000,000 |
| Net Assets (Equity) | $95,000,000 | $87,000,000 |
| Total Liabilities and Net Assets | $140,000,000 | $130,000,000 |
Analysis of Oakwood Community Hospital’s Financial Statement
This statement shows Oakwood Community Hospital experienced growth in both assets and net assets from 2022 to 2023. The increase in cash and cash equivalents indicates improved liquidity. The rise in accounts receivable suggests potentially increased patient volume or longer collection periods, requiring further investigation. The substantial investment in property, plant, and equipment might reflect capital improvements or expansion projects.
The increase in net assets reflects the hospital’s overall financial performance and its ability to generate surpluses. The relatively stable long-term debt suggests a responsible approach to financing.
Relationship Between Cash Reserves and Overall Financial Performance
Oakwood’s increased cash reserves from $12 million to $15 million are directly linked to its improved financial performance. A healthy cash position allows the hospital to meet its short-term obligations, invest in necessary equipment and upgrades, and weather unexpected financial downturns. However, excessively high cash reserves might indicate inefficient use of funds that could be reinvested in programs or services.
The optimal level of cash reserves is a balance between liquidity and maximizing the use of resources to benefit the community.
Final Summary: Nonprofit Hospitals Health Systems Cash On Hand KFF
Understanding the financial health of nonprofit hospitals is crucial for ensuring the future of accessible and affordable healthcare. The KFF data provides a valuable snapshot of the situation, revealing both strengths and potential vulnerabilities within the system. While substantial cash reserves offer a buffer against economic downturns and enable vital investments, careful oversight and responsible management are essential to ensure these funds are used effectively to serve the communities they are intended to benefit.
The ongoing conversation surrounding nonprofit hospital finances, regulatory frameworks, and the evolving healthcare landscape is vital to ensuring a sustainable and equitable healthcare system for all.
Q&A
What are the potential downsides of excessively high cash reserves for nonprofit hospitals?
High cash reserves can attract criticism for potentially not being used efficiently for patient care or community benefit. It could also suggest missed opportunities for investment in improved facilities or technology.
How does the size of a nonprofit hospital impact its cash on hand?
Larger hospitals generally have higher cash reserves due to increased revenue streams and greater economies of scale. Smaller hospitals may face more financial constraints.
How does inflation affect nonprofit hospital cash reserves?
Inflation erodes the purchasing power of cash reserves over time. Hospitals need to consider inflation when budgeting and making financial decisions.
Are there any legal restrictions on how nonprofit hospitals can use their cash reserves?
Yes, as tax-exempt organizations, nonprofit hospitals are subject to regulations regarding the use of their funds. They must demonstrate community benefit and responsible financial management.