Nonprofit Hospitals Labor Stabilizing Fitch Ratings
Nonprofit hospitals labor stabilizing Fitch ratings: It’s a headline that might sound dry, but behind it lies a fascinating story of balancing budgets, employee relations, and maintaining financial credibility. This isn’t just about numbers; it’s about the people who keep these vital institutions running – the doctors, nurses, and support staff – and the complex interplay between their compensation, the hospital’s financial health, and the all-important rating agencies like Fitch.
We’ll delve into the challenges and successes, exploring how effective labor management directly impacts a hospital’s bottom line and its creditworthiness.
From understanding the factors influencing nonprofit hospital finances – like labor costs and debt – to navigating the intricacies of union negotiations and employee retention strategies, we’ll unpack the key elements that contribute to a stable and sustainable future. We’ll also examine how Fitch Ratings assesses these hospitals, the criteria they use, and the consequences of a good or bad rating.
Think of it as a behind-the-scenes look at the financial acrobatics required to keep these essential community pillars thriving.
Nonprofit Hospital Financial Stability
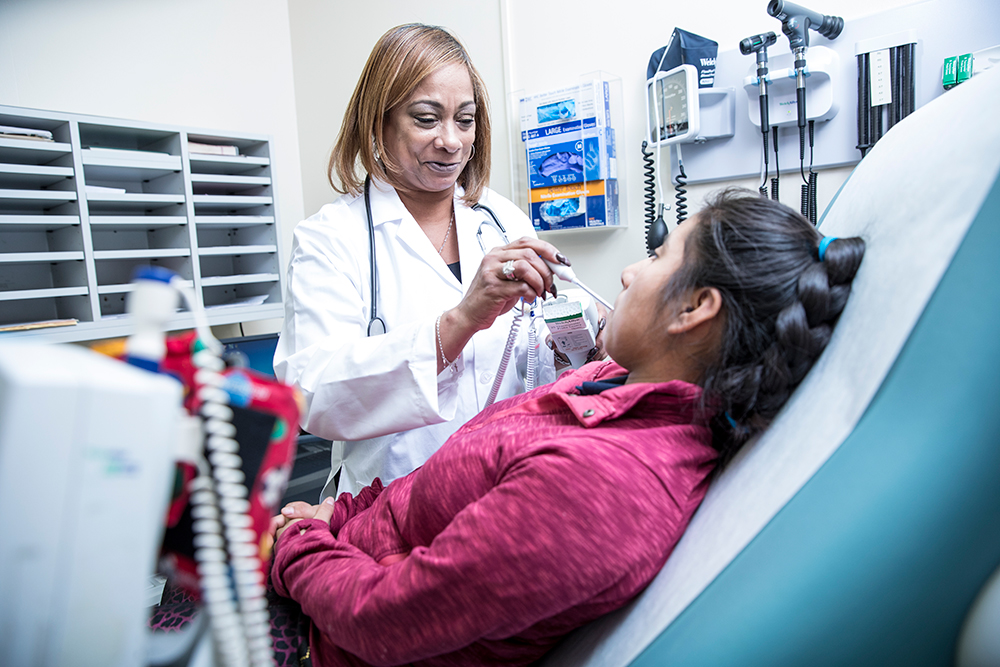
Source: windows.net
The financial health of nonprofit hospitals is a complex issue, crucial for ensuring access to quality healthcare for communities. Maintaining financial stability allows these institutions to invest in facilities, technology, and staff, ultimately benefiting patients. Several interconnected factors contribute to their overall financial well-being, and understanding these factors is vital for effective management and policy decisions.
Factors Influencing Nonprofit Hospital Financial Health
A multitude of factors influence the financial health of nonprofit hospitals. Reimbursement rates from government programs like Medicare and Medicaid are significant, often falling short of actual costs. The increasing prevalence of high-deductible health plans shifts more financial responsibility to patients, potentially impacting revenue streams. Competition from for-profit hospitals and other healthcare providers also plays a crucial role, impacting patient volume and market share.
Operational efficiency, effective cost management, and philanthropic support are further key contributors to a hospital’s financial standing. Finally, the overall economic climate and its impact on patient demographics and insurance coverage also exerts a significant influence.
Impact of Labor Costs on Nonprofit Hospital Budgets
Labor costs represent a substantial portion of a nonprofit hospital’s operating budget, often exceeding 50%. Salaries, benefits, and staffing levels directly impact the bottom line. The ongoing shortage of nurses and other healthcare professionals drives up wages, further straining already tight budgets. Negotiating competitive compensation packages to attract and retain qualified staff is essential, yet this can be challenging given the financial constraints faced by many nonprofit institutions.
Strategies for managing labor costs include optimizing staffing models, leveraging technology to improve efficiency, and investing in employee training and retention programs to reduce turnover.
Financial Performance Comparison: Nonprofit vs. For-Profit Hospitals
While direct comparisons are complex due to differing accounting practices and reporting requirements, some general observations can be made. For-profit hospitals, driven by shareholder value, may prioritize profitability over certain community benefits. This could lead to higher operating margins in some cases, but potentially at the expense of uncompensated care or investment in community health initiatives. Nonprofit hospitals, however, often prioritize community benefit, potentially leading to lower operating margins but higher levels of uncompensated care and community investment.
Ultimately, both models play vital roles in the healthcare system, and their comparative performance varies widely based on specific market conditions and management strategies.
Financial Strategies for Maintaining Stability
Nonprofit hospitals employ a variety of strategies to maintain financial stability. These include diversifying revenue streams through outpatient services, telehealth initiatives, and strategic partnerships. Cost-cutting measures, such as streamlining administrative processes and negotiating favorable contracts with suppliers, are also implemented. Philanthropic fundraising and endowment management are crucial for supplementing operational budgets and supporting capital improvements. Furthermore, effective debt management, including refinancing existing debt at lower interest rates, is essential for maintaining a healthy financial position.
Finally, proactive financial planning and budgeting, coupled with regular financial performance monitoring, are critical for navigating the complexities of the healthcare landscape.
Key Financial Ratios of High- and Low-Performing Nonprofit Hospitals
The following table presents a simplified comparison, highlighting that actual ratios vary widely based on hospital size, location, and services offered. This data is illustrative and not representative of all nonprofit hospitals.
| Hospital Name | Debt-to-Equity Ratio | Operating Margin | Fitch Rating |
|---|---|---|---|
| High-Performing Hospital A | 0.8 | 5% | AA- |
| High-Performing Hospital B | 0.7 | 6% | A+ |
| Low-Performing Hospital C | 1.5 | -2% | BB+ |
| Low-Performing Hospital D | 1.2 | 1% | BBB- |
Labor Relations in Nonprofit Hospitals
Navigating the complex landscape of labor relations is a significant challenge for nonprofit hospitals, particularly given their dual mission of providing quality care and operating within budgetary constraints. The unique characteristics of this sector, including a high proportion of unionized workers and a reliance on public funding, create a distinct set of hurdles compared to for-profit healthcare organizations. Balancing the needs of employees with the financial realities of the organization requires a delicate and strategic approach.
Challenges of Managing Labor Relations in Nonprofit Hospitals
Nonprofit hospitals face a multifaceted set of challenges in managing labor relations. These include balancing the often competing demands of providing high-quality patient care, maintaining financial stability, and ensuring fair treatment of employees. The high-stress environment of hospital work, coupled with the emotional toll of caring for sick and injured patients, can lead to higher rates of burnout and turnover, creating staffing shortages and increasing pressure on existing employees.
Furthermore, the increasing complexity of healthcare regulations and the constant pressure to improve efficiency add to the challenges of managing a workforce effectively. Negotiating contracts with unions, managing employee grievances, and ensuring compliance with labor laws all demand significant resources and expertise. For example, a hospital might face difficulties in negotiating wage increases that are both competitive and sustainable within their budget, particularly if facing reduced government funding or increased operating costs.
Impact of Unionization on Nonprofit Hospital Finances
Unionization significantly impacts the financial health of nonprofit hospitals. Union contracts often stipulate higher wages, enhanced benefits packages, and stricter grievance procedures than non-unionized settings. While these provisions can improve employee morale and retention, they inevitably increase labor costs. For instance, a union contract might mandate higher minimum staffing levels, leading to increased payroll expenses. Similarly, the implementation of comprehensive grievance procedures can result in increased administrative costs associated with handling disputes.
However, it is important to note that unionized hospitals may also experience reduced turnover rates and improved productivity, potentially offsetting some of the increased labor costs. The overall financial impact is a complex equation dependent on various factors, including the specific terms of the union contract, the hospital’s overall financial health, and the effectiveness of labor relations management. A well-managed union relationship, however, can actually contribute to a more stable and productive workforce.
Common Labor Disputes in Nonprofit Hospitals and Their Resolutions
Common labor disputes in nonprofit hospitals often revolve around wages, benefits, staffing levels, and working conditions. Disagreements over wage increases, especially during periods of economic uncertainty or budget constraints, are frequently a source of conflict. Similarly, disputes can arise regarding the adequacy of healthcare benefits, retirement plans, and paid time off. Staffing levels are another major area of contention, with unions often advocating for increased staffing ratios to ensure patient safety and reduce employee workload.
Disputes are frequently resolved through negotiations, mediation, or arbitration. Negotiations between hospital management and union representatives aim to reach a mutually agreeable settlement. If negotiations fail, mediation involves a neutral third party facilitating communication and assisting in finding common ground. Arbitration, a more formal process, involves a neutral arbitrator making a binding decision. For example, a dispute over staffing ratios might be resolved through a negotiated agreement that increases staffing levels gradually over a set period, while a dispute over wages could be settled through arbitration based on comparable compensation in similar healthcare settings.
Approaches to Employee Compensation and Benefits in Nonprofit Hospitals
Nonprofit hospitals employ various approaches to employee compensation and benefits, often balancing financial constraints with the need to attract and retain qualified staff. Some hospitals offer competitive salaries and comprehensive benefits packages comparable to those in for-profit settings, while others rely on a combination of competitive salaries and a strong emphasis on mission-driven work to attract employees. Some hospitals may also offer unique benefits such as tuition reimbursement, loan forgiveness programs, or flexible work schedules to enhance their appeal to potential employees.
For instance, a hospital might offer a competitive salary structure benchmarked against regional averages while also providing generous benefits like health insurance and retirement plans. In contrast, another hospital might offer a slightly lower salary but emphasize the positive impact of working in a mission-driven environment, potentially including opportunities for professional development or community engagement.
Hypothetical Employee Retention Strategy for a Nonprofit Hospital Facing Labor Shortages
A nonprofit hospital facing significant labor shortages might implement a multi-pronged retention strategy. This strategy could involve a combination of competitive compensation adjustments, improved benefits packages (including enhanced health insurance options, expanded paid time off, and robust retirement plans), and investments in employee well-being initiatives. These initiatives might include offering on-site wellness programs, employee assistance programs, and stress management training.
Additionally, creating clear career progression pathways, offering opportunities for professional development (like tuition reimbursement or specialized training), and fostering a supportive and collaborative work environment can significantly impact retention rates. Finally, improving communication channels and actively soliciting employee feedback to address concerns proactively is vital. For example, a hospital could offer a signing bonus to new hires to incentivize recruitment, while simultaneously implementing a mentorship program for existing employees to enhance job satisfaction and reduce burnout.
By combining financial incentives with a strong focus on employee well-being and career development, the hospital could significantly improve its ability to attract and retain skilled healthcare professionals.
So, Fitch ratings for nonprofit hospitals are looking a bit more stable regarding labor costs, which is great news. This stability is crucial, especially considering the increasing complexity of healthcare. It makes you wonder about the long-term health of our aging population, and I recently read an interesting article about how an eye test might detect dementia risk in older adults – check it out: can eye test detect dementia risk in older adults.
Understanding these risks helps us plan for future healthcare needs, impacting everything from hospital staffing to overall financial stability of places like nonprofit hospitals.
Fitch Ratings and Nonprofit Hospitals: Nonprofit Hospitals Labor Stabilizing Fitch Ratings
Fitch Ratings, a globally recognized credit rating agency, plays a crucial role in assessing the financial health and creditworthiness of nonprofit hospitals. Understanding how Fitch evaluates these institutions is vital for hospital administrators, investors, and anyone interested in the financial stability of the healthcare sector. Their ratings directly impact a hospital’s ability to secure financing, influencing everything from bond issuance to operational budgets.
Fitch’s Assessment Methodology for Nonprofit Hospitals
Fitch employs a comprehensive methodology to assess the creditworthiness of nonprofit hospitals. This involves a detailed analysis of various financial and operational factors, ultimately assigning a rating that reflects the perceived risk of default on debt obligations. The process is rigorous, combining quantitative data analysis with qualitative assessments of management quality and market position. The goal is to provide a clear and objective picture of the hospital’s long-term financial sustainability.
Key Criteria Used by Fitch in Rating Nonprofit Hospitals
Several key criteria heavily influence Fitch’s rating decisions. These include the hospital’s financial performance, including operating profitability, liquidity, and debt levels. Crucially, Fitch also considers the hospital’s market position, analyzing its competitive landscape, market share, and patient volume. Management quality and governance structures are assessed, examining the hospital’s strategic planning, operational efficiency, and financial management practices. Finally, the regulatory environment and the hospital’s compliance with relevant laws and regulations are taken into account.
Factors Positively and Negatively Impacting Fitch Ratings
A strong operating margin, consistently positive cash flow, and a low debt-to-equity ratio are all positive factors that can significantly improve a nonprofit hospital’s Fitch rating. A diverse and robust payer mix, demonstrating resilience to changes in reimbursement policies, is also viewed favorably. Conversely, negative factors include declining patient volumes, operating losses, high levels of debt, and weak liquidity.
Significant reliance on government funding, coupled with potential changes in healthcare policy, can also negatively impact a hospital’s rating. For example, a hospital experiencing a sudden decrease in Medicare reimbursements might see its rating downgraded if it doesn’t have sufficient reserves or alternative revenue streams.
Fitch’s Rating Categories and Their Implications
Fitch uses a letter-based rating system, with ‘AAA’ representing the highest credit quality and ‘D’ indicating default. Each rating category carries specific implications for a nonprofit hospital. A higher rating translates to lower borrowing costs, greater access to capital markets, and improved investor confidence. Conversely, a lower rating can lead to higher interest rates, limited access to financing, and potentially increased scrutiny from regulators and stakeholders.
For instance, a hospital rated ‘AA’ would likely have easier access to capital and better interest rates compared to a hospital rated ‘BBB’.
Hypothetical Case Study: Improving a Nonprofit Hospital’s Fitch Rating, Nonprofit hospitals labor stabilizing fitch ratings
Let’s consider a hypothetical case of “Community General Hospital,” currently rated ‘BBB+’. The hospital is experiencing declining patient volumes in its emergency department and has a relatively high debt-to-equity ratio. To improve its Fitch rating, Community General could implement several strategies. First, it could invest in marketing and outreach programs to attract more patients to its emergency department, potentially diversifying services to attract a broader patient base.
Secondly, the hospital could implement cost-reduction measures to improve its operating margin and strengthen its financial performance. This could involve streamlining administrative processes, negotiating better contracts with suppliers, and improving workforce efficiency. Finally, Community General could explore refinancing options to reduce its debt burden and improve its debt-to-equity ratio. By implementing these strategies, the hospital could demonstrate improved financial performance and stability, potentially leading to an upgrade in its Fitch rating to ‘A-‘ or higher.
The Interplay of Labor, Finances, and Fitch Ratings

Source: windows.net
Nonprofit hospitals operate in a complex environment where balancing high-quality patient care with fiscal responsibility is paramount. A significant factor influencing their financial health and creditworthiness is the relationship between labor costs, overall financial performance, and the resulting Fitch ratings. Understanding this interplay is crucial for ensuring the long-term sustainability of these vital institutions.
Labor Costs and Financial Performance
Labor costs represent a substantial portion of a nonprofit hospital’s operating budget. Salaries, benefits, and other employee-related expenses directly impact the bottom line. High labor costs, particularly when not effectively managed, can lead to reduced operating margins and decreased financial flexibility. Conversely, efficient labor management, including optimized staffing levels and competitive compensation packages that attract and retain qualified personnel, can contribute to improved operational efficiency and better financial outcomes.
It’s interesting to see how Fitch ratings for nonprofit hospitals are being impacted by labor issues. The stability of these ratings is crucial, and recent events like Steward Health Care securing financing to emerge from bankruptcy, as reported here: steward health care secures financing bankruptcy , highlight the financial pressures facing the healthcare sector. This instability ultimately impacts the labor market and the overall stability of nonprofit hospital ratings.
For example, a hospital successfully implementing a program to reduce staff turnover through improved employee engagement might see significant savings in recruitment and training costs, thereby positively impacting its financial statements and ultimately, its credit rating.
Consequences of a Low Fitch Rating
A low Fitch rating signifies increased financial risk for a nonprofit hospital. This can make it more difficult to secure loans at favorable interest rates, limiting access to capital needed for necessary upgrades, expansions, or even day-to-day operations. It can also impact the hospital’s ability to attract philanthropic donations and recruit top talent, as potential donors and employees may perceive increased risk.
A downgraded rating can further lead to higher insurance premiums and potentially restrict the hospital’s ability to participate in certain government programs or partnerships. For instance, a hospital with a low rating might face challenges securing funding for a much-needed new wing or technological upgrades, hindering its ability to provide optimal patient care.
Effective Labor Management and Improved Financial Stability
Effective labor management is a critical component of a nonprofit hospital’s financial health. Strategies such as implementing robust workforce planning, negotiating favorable collective bargaining agreements, investing in employee training and development, and fostering a positive work environment can significantly reduce labor costs while improving employee productivity and retention. By reducing staff turnover, hospitals minimize recruitment and training expenses, saving considerable sums.
Furthermore, a positive work environment leads to increased employee morale and improved patient care, potentially attracting more patients and generating higher revenue. These factors cumulatively contribute to enhanced financial stability and a more favorable outlook for Fitch rating agencies.
Strategies to Mitigate Risk of Negative Fitch Ratings
Proactive strategies are essential to mitigate the risk of negative Fitch ratings related to labor issues. This involves meticulous financial planning that incorporates realistic labor cost projections, diligent contract negotiations, and continuous monitoring of key performance indicators (KPIs) related to staffing levels, employee satisfaction, and turnover rates. Implementing a data-driven approach to workforce management allows for more accurate forecasting and proactive adjustments to staffing levels, avoiding both overstaffing and understaffing scenarios.
So, Fitch’s ratings for nonprofit hospitals are looking a bit more stable regarding labor costs lately, which is good news. However, the stress on hospital staff can indirectly impact patient care; for example, a rushed environment increases the risk of misdiagnosis, especially for conditions like stroke, where understanding risk factors that make stroke more dangerous is crucial for timely intervention.
Ultimately, a healthier workforce contributes to better patient outcomes, further strengthening the financial stability of these hospitals.
Regular audits of labor practices and compliance with all relevant regulations further minimize potential liabilities and contribute to a stronger financial profile.
Best Practices for Maintaining Strong Labor Relations and Financial Health
To maintain strong labor relations and financial health, leading to favorable Fitch ratings, nonprofit hospitals should adopt several best practices:
- Develop a comprehensive workforce plan that aligns with the hospital’s strategic goals and anticipates future staffing needs.
- Invest in employee training and development to enhance skills and improve productivity.
- Foster a culture of open communication and collaboration between management and employees.
- Implement competitive compensation and benefits packages to attract and retain qualified personnel.
- Regularly monitor and analyze labor costs and KPIs to identify areas for improvement.
- Establish robust grievance procedures and conflict resolution mechanisms.
- Ensure compliance with all relevant labor laws and regulations.
- Regularly review and update labor contracts to reflect changing market conditions.
Case Studies

Source: twimg.com
This section delves into real-world examples of nonprofit hospitals navigating the complex interplay between labor relations, financial performance, and Fitch ratings. We’ll examine both successful and less successful cases, highlighting key strategies and their impact on creditworthiness.
Successful Navigation of Labor Challenges: Example of Memorial Healthcare System
Memorial Healthcare System (MHS), a large nonprofit hospital system in South Florida, provides a compelling case study of successful labor relations management. Facing increasing labor costs and a competitive job market, MHS implemented a multifaceted strategy. This included proactive investments in employee training and development programs, leading to increased staff retention and reduced recruitment costs. They also negotiated competitive compensation packages, incorporating performance-based incentives and benefits that addressed employee needs and priorities, thereby mitigating potential labor disputes.
Simultaneously, MHS implemented robust cost-containment measures in other areas of operations, such as supply chain management and administrative efficiency improvements, ensuring that increased labor costs did not unduly strain the system’s overall financial health. These combined strategies helped MHS maintain strong financial performance and a consistently high Fitch rating. The system’s commitment to its workforce and its strategic financial planning created a virtuous cycle, leading to improved patient care and a strong credit profile.
Financial Difficulties Due to Labor Issues: Example of St. Jude’s Regional Hospital
In contrast, St. Jude’s Regional Hospital, a smaller nonprofit hospital in a rural area, faced significant financial difficulties stemming from unresolved labor disputes. A protracted nurses’ strike, resulting from failed contract negotiations concerning wages and staffing levels, significantly disrupted operations and led to a decline in patient volume. The strike resulted in substantial financial losses, including lost revenue, increased temporary staffing costs, and legal fees.
These challenges negatively impacted St. Jude’s financial ratios, leading to a downgrade in its Fitch rating. The hospital’s response involved implementing a new labor relations strategy focusing on improved communication and collaborative problem-solving with its unions. They also sought financial assistance through state and federal programs, while simultaneously implementing cost-cutting measures to address the immediate financial crisis.
While St. Jude’s is working to recover, this case illustrates the significant and potentially long-lasting negative consequences of unresolved labor disputes on a nonprofit hospital’s financial stability and credit rating.
Visual Representation of Labor Costs, Financial Performance, and Fitch Ratings
The visual representation would be a dual-line graph. The x-axis would represent time (e.g., years). The y-axis would have three scales: one for labor costs (percentage of operating budget), one for operating margin (percentage), and one for Fitch rating (e.g., AAA, AA, A, etc.). For the “successful hospital” (e.g., a hypothetical “Wellspring Hospital”), the labor cost line would show a moderate increase over time, reflecting competitive compensation.
The operating margin line would remain relatively high and stable, indicating strong financial performance. The Fitch rating line would remain consistently high (e.g., AA or AAA).For the “struggling hospital” (e.g., a hypothetical “County General”), the labor cost line would show a sharp increase, potentially due to unsustainable wage increases or high turnover requiring costly recruitment. The operating margin line would show a sharp decline, reflecting financial strain.
The Fitch rating line would show a downward trend, reflecting the deterioration of the hospital’s creditworthiness. This visual clearly illustrates how sustainable labor cost management directly impacts financial performance and ultimately influences a hospital’s Fitch rating. The contrasting trajectories of the two hypothetical hospitals would emphasize the importance of proactive labor relations management in ensuring long-term financial stability and a strong credit profile.
Conclusion
Ultimately, the story of nonprofit hospitals, their labor forces, and their Fitch ratings is a story of resilience, adaptation, and the constant search for equilibrium. It highlights the critical need for strong financial management, effective labor relations, and a clear understanding of the factors that influence creditworthiness. By understanding these interconnected elements, nonprofit hospitals can better position themselves for long-term success, ensuring they can continue providing vital care to their communities.
It’s a complex puzzle, but one with a solution that benefits everyone involved.
Detailed FAQs
What are the potential consequences of a low Fitch rating for a nonprofit hospital?
A low Fitch rating can make it harder for a nonprofit hospital to secure loans, obtain favorable insurance rates, and attract investors. It can also damage their reputation and make it more difficult to recruit and retain top talent.
How can a nonprofit hospital improve its employee retention rates?
Strategies include competitive compensation and benefits packages, opportunities for professional development, a positive work environment, and recognition programs to boost morale and job satisfaction.
Are there specific legal considerations for labor relations in nonprofit hospitals?
Yes, nonprofit hospitals must still comply with all relevant labor laws, including those related to wages, hours, working conditions, and unionization. The specifics vary by location and jurisdiction.