Hospital Margins to Stabilize Below Pre-Pandemic Levels
Hospital margins to stabilize below pre pandemic levels – Hospital margins to stabilize below pre-pandemic levels – a sobering reality check for the healthcare industry. The COVID-19 pandemic threw hospitals into a financial whirlwind, forcing them to grapple with unprecedented surges in patients, skyrocketing expenses, and strained resources. While some government aid cushioned the blow, the long-term effects are still unfolding, leaving many hospitals struggling to regain their pre-pandemic financial footing.
This post dives into the challenges and strategies shaping the future of hospital finances.
From plummeting patient volumes and the increased costs of PPE to persistent staffing shortages and inflation, the road to recovery has been far from smooth. We’ll explore the factors hindering a return to pre-pandemic profitability, examining everything from reimbursement rates and supply chain issues to the innovative solutions hospitals are employing to navigate these turbulent waters. We’ll also look ahead, forecasting potential trajectories for hospital margins in the coming years and considering the impact of evolving healthcare models.
Pre-Pandemic Hospital Margins
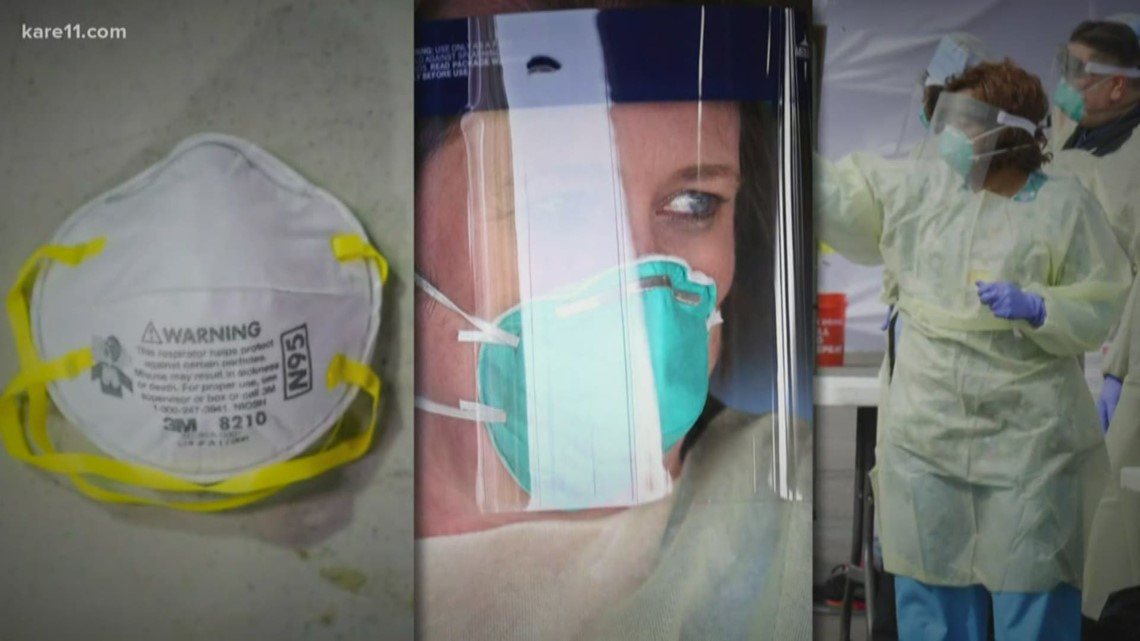
Source: kare11.com
The financial landscape for hospitals before the COVID-19 pandemic was characterized by a complex interplay of revenue streams and cost pressures, resulting in varying levels of profitability across different hospital types. While overall profitability was generally positive, margins were often described as thin, and the sector faced ongoing challenges related to reimbursement rates, rising operational costs, and increasing demand for services.
Understanding this pre-pandemic baseline is crucial for evaluating the impact of the pandemic and assessing the long-term trajectory of hospital finances.
Average Operating Margins and Profitability Metrics
Pre-pandemic, hospital operating margins varied considerably, influenced by factors like location, size, and the types of services offered. While precise figures fluctuate depending on the source and methodology used, a reasonable estimate would place the average operating margin for hospitals in the range of 2-5%. This indicates that for every dollar of revenue generated, hospitals were typically retaining only a small percentage as profit after covering operating expenses.
Other key profitability metrics, such as return on assets (ROA) and return on equity (ROE), also reflected this relatively low margin environment. For example, a 2019 report from the American Hospital Association (AHA) might have shown ROA figures averaging in the low single digits for many hospitals. The financial health of individual hospitals, however, varied significantly.
Hospital Revenue and Cost Structures
Hospitals generate revenue from a variety of sources, with the relative importance of each stream differing based on the hospital’s specific characteristics. A typical pre-pandemic revenue structure might look like this:
| Major Revenue Source | Percentage Contribution to Total Revenue | Major Cost Category | Percentage of Total Expenses |
|---|---|---|---|
| Inpatient Services | 35-45% | Salaries and Benefits | 50-60% |
| Outpatient Services | 30-40% | Supplies and Pharmaceuticals | 15-20% |
| Government Reimbursement (Medicare/Medicaid) | 20-30% | Depreciation and Amortization | 5-10% |
| Other (e.g., Private Insurance, Philanthropy) | 5-15% | Other Operating Expenses | 10-15% |
Note that these percentages are approximate and can vary significantly depending on the specific hospital. The high percentage allocated to salaries and benefits reflects the labor-intensive nature of hospital operations.
Financial Health of Different Hospital Types
Teaching hospitals, often affiliated with medical schools and research institutions, generally had more complex cost structures due to research expenses and educational programs. Their revenue streams might also be more diversified, including research grants and endowments. As a result, their profitability could differ from other hospital types, potentially exhibiting higher expenses but also potentially greater revenue diversification. In contrast, rural hospitals often faced challenges related to lower patient volumes, limited access to specialized services, and higher uncompensated care costs.
This frequently translated to lower operating margins and greater financial vulnerability compared to their urban counterparts. The pre-pandemic financial landscape highlighted the diverse financial realities faced by hospitals across different settings and service models.
Impact of the Pandemic on Hospital Margins
The COVID-19 pandemic dramatically reshaped the financial landscape of hospitals worldwide, causing unprecedented disruptions and significantly impacting their margins. The initial shockwaves, followed by prolonged challenges, created a complex interplay of decreased revenue and increased expenses, leaving many healthcare systems struggling to maintain financial stability. Understanding these impacts is crucial to comprehending the current state of hospital finances.The pandemic’s immediate effect on hospital revenue was a sharp decline.
This was primarily due to a significant drop in patient volume, as elective procedures and non-urgent care were postponed or canceled to prioritize COVID-19 patients and conserve resources. Simultaneously, the payer mix shifted, with a higher proportion of patients relying on government assistance programs like Medicaid, which typically reimburse hospitals at lower rates compared to private insurance. This double whammy of reduced volume and altered payer mix created a substantial revenue shortfall for many hospitals.
Increased Hospital Expenses During the Pandemic
The pandemic led to a substantial increase in hospital expenses across several key areas. These added costs significantly strained already tight budgets and contributed heavily to the erosion of hospital margins. The following points highlight the most impactful expense increases:
- Personal Protective Equipment (PPE): The demand for PPE, including masks, gowns, gloves, and face shields, skyrocketed. Hospitals faced shortages and had to pay significantly inflated prices to secure adequate supplies for their staff and patients, leading to substantial additional costs.
- Staffing Costs: Hospitals experienced increased demand for healthcare professionals, particularly nurses and respiratory therapists, to manage the influx of COVID-19 patients. This heightened demand led to increased overtime pay, recruitment bonuses, and agency staffing costs, significantly impacting labor expenses. Burnout and attrition further exacerbated the situation, necessitating additional investment in training and recruitment.
- Treatment Costs: The treatment of COVID-19 patients was expensive, requiring specialized care, prolonged hospital stays, and often, intensive care unit (ICU) admission with mechanical ventilation. These patients frequently required prolonged oxygen therapy and other resource-intensive treatments, contributing to significantly higher overall treatment costs.
- Facility Modifications and Upgrades: Many hospitals had to invest in facility modifications to create dedicated COVID-19 units, including negative pressure rooms to prevent the spread of the virus. These renovations, along with investments in improved ventilation systems and other infection control measures, added substantial capital expenses.
Government Support Measures and Their Impact
Governments worldwide implemented various support measures to mitigate the financial strain on hospitals during the pandemic. These included direct financial aid, increased Medicare and Medicaid reimbursements, and loan programs. For example, the CARES Act in the United States provided significant funding to hospitals to offset losses and support COVID-19 related expenses. While these measures provided crucial relief to many healthcare systems, the support often fell short of the actual financial burden, and the distribution of funds was not always equitable across all hospitals.
Furthermore, the temporary nature of many of these programs meant that hospitals faced renewed financial challenges as the support ended.
Hospital margins are slowly recovering, but it’s a tough climb back to pre-pandemic levels. The healthcare industry is seeing a lot of shifts, with even major players like NextGen Healthcare reportedly exploring a sale, as reported by Reuters nextgen exploring sale reuters. This kind of market activity highlights the financial pressures facing the entire sector, further emphasizing the challenge hospitals face in stabilizing their margins.
Factors Hindering Margin Recovery
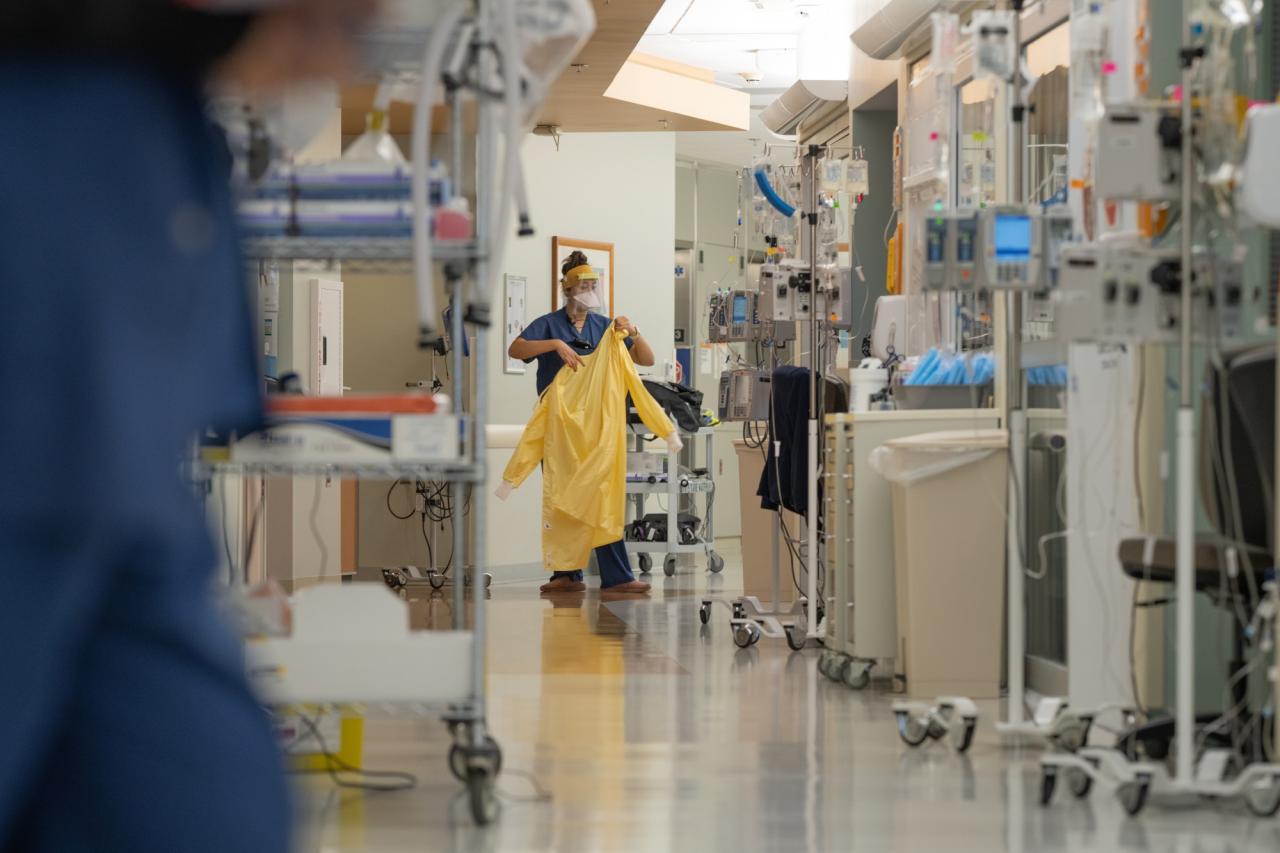
Source: bwbx.io
Hospitals are facing a perfect storm of challenges that are preventing them from returning to pre-pandemic profit levels. While the immediate crisis of COVID-19 has subsided, the lingering effects are compounded by broader economic headwinds, creating a complex and persistent obstacle to financial recovery. This section will delve into the key factors hindering this recovery.The combination of inflation, supply chain disruptions, and persistent labor shortages is significantly impacting hospital finances.
Inflation drives up the cost of everything from medications and medical supplies to utilities and staff salaries, squeezing margins. Simultaneously, supply chain issues lead to delays and increased costs for essential equipment and pharmaceuticals. The ongoing labor shortage, particularly for nurses and other healthcare professionals, forces hospitals to increase wages to attract and retain staff, further impacting profitability.
These challenges are interconnected, creating a cascading effect that intensifies the pressure on hospital budgets.
Inflation’s Impact on Hospital Expenses
Inflation has significantly increased the cost of goods and services for hospitals. For example, the price of certain medications has risen dramatically, impacting pharmacy budgets. Similarly, the cost of disposable medical supplies, like gloves and gowns, has increased significantly, adding to operational expenses. These increased costs are not always offset by corresponding increases in reimbursement rates, leading to a reduction in profit margins.
Hospitals are finding themselves in a difficult position, balancing the need to provide high-quality care with the pressure to control costs in an inflationary environment. One example is the significant increase in the cost of fuel, impacting transportation costs for supplies and patient transport.
Reimbursement Rates and Their Impact
Current reimbursement rates from various payers – Medicare, Medicaid, and private insurers – lag behind the rising costs faced by hospitals. While some private insurers have adjusted their rates, the increases often fail to keep pace with inflation and the escalating cost of labor and supplies. Medicare and Medicaid reimbursement rates, notoriously slow to adjust, remain a significant source of concern.
The discrepancy between the rising cost of care and the relatively stagnant reimbursement rates from these major payers creates a substantial financial strain on hospitals, making it difficult to achieve pre-pandemic profit levels. A specific example could be comparing the reimbursement rate for a specific procedure in 2019 versus 2023, highlighting the insufficient increase to cover inflation and rising costs.
Improving Operational Efficiency to Enhance Margins
Increasing operational efficiency is crucial for improving hospital margins. This involves streamlining processes, reducing waste, and optimizing resource allocation. Implementing technologies like electronic health records (EHRs) can improve administrative efficiency, reduce medical errors, and improve patient flow. Adopting data-driven decision-making can help hospitals identify areas for cost reduction and improvement. A scenario could involve a hospital implementing a new inventory management system to reduce waste and optimize supply chain logistics.
This system could lead to a 5% reduction in supply costs, a measurable improvement in operational efficiency directly translating to improved margins. Another example might be the implementation of telehealth services, reducing the need for costly in-person visits for certain types of care. This would free up resources and potentially reduce overhead costs.
Strategies for Margin Stabilization
Hospital margins, battered by the pandemic, require a multifaceted approach to recovery and stabilization. This involves not only addressing lingering effects of the past but also proactively implementing strategies to improve financial performance and ensure long-term sustainability. This section explores several key strategies hospitals are employing to achieve this goal.
Telehealth Adoption and Revenue Cycle Management Improvements
The expansion of telehealth services offers a significant opportunity for margin improvement. By reducing reliance on costly in-person visits, hospitals can increase patient access while simultaneously lowering operational expenses. This is particularly effective for routine follow-ups and chronic disease management, freeing up valuable resources for more complex cases. Simultaneously, streamlined revenue cycle management (RCM) processes are crucial.
This involves optimizing billing and coding practices, improving claims processing efficiency, and reducing denials. Implementing advanced analytics and automation within RCM can significantly reduce administrative costs and accelerate revenue collection, leading to improved cash flow and ultimately, higher margins. For example, a hospital system in Ohio reported a 15% reduction in denials after implementing a new RCM platform, translating directly into improved profitability.
Effective Cost Management
Effective cost management is the cornerstone of margin stabilization. This involves a comprehensive review of all operational expenses, identifying areas for potential savings without compromising the quality of care. This includes negotiating better rates with suppliers, optimizing staffing levels through improved scheduling and workforce management technologies, and reducing energy consumption through energy-efficient infrastructure upgrades. Furthermore, a focus on supply chain optimization can yield substantial savings.
Hospitals can leverage group purchasing organizations (GPOs) to negotiate bulk discounts on medical supplies and equipment, significantly reducing procurement costs. For instance, a large hospital system in California reported annual savings of over $10 million by implementing a comprehensive supply chain optimization program. This demonstrates the substantial impact that even seemingly minor cost-saving measures can have on overall margins when implemented systematically.
Strategic Partnerships and Collaborations
Strategic partnerships and collaborations offer a powerful mechanism for improving financial sustainability. By sharing resources, expertise, and infrastructure, hospitals can achieve economies of scale and reduce operational redundancies. This can include joint ventures in areas such as telehealth, specialized services, or research and development. Furthermore, partnerships can facilitate access to new technologies and innovative care delivery models, improving both quality of care and financial performance.
Hypothetical Case Study: Successful Partnership, Hospital margins to stabilize below pre pandemic levels
Consider two rural hospitals, Hospital A and Hospital B, both facing declining patient volumes and financial challenges. Hospital A excels in cardiology, while Hospital B has a strong oncology program. By forming a strategic partnership, they establish a shared telehealth platform, allowing specialists from each hospital to remotely consult with patients in both locations. This expands access to specialized care, attracting more patients and generating additional revenue for both hospitals.
They also jointly negotiate contracts with suppliers, leveraging their combined purchasing power to secure better pricing on medical supplies and equipment. The result is improved patient access, increased revenue streams, and reduced operational costs, leading to improved financial stability for both partners. This demonstrates the synergistic benefits that can be achieved through strategic collaboration.
Long-Term Outlook for Hospital Margins
Predicting the future of hospital margins is a complex undertaking, requiring consideration of numerous intertwined factors. Over the next 3-5 years, a multitude of economic and policy shifts will significantly influence hospital profitability, potentially leading to a range of outcomes. While a complete return to pre-pandemic margins within this timeframe seems unlikely for many institutions, the trajectory will depend heavily on the successful implementation of strategic initiatives and the broader healthcare landscape.The next few years will be a period of significant adjustment for hospitals.
Hospital margins are still struggling to recover to pre-pandemic levels, a situation exacerbated by rising labor costs. The recent news of a new york nurse strike deal reached Mount Sinai Montefiore highlights the intense pressure hospitals face. These significant wage increases, while deserved by the hardworking nurses, will undoubtedly put further strain on already thin margins, making a return to pre-pandemic profitability a longer, tougher road.
Several interconnected forces—shifting reimbursement models, evolving patient demographics, and persistent workforce shortages—will continue to exert pressure on margins. However, innovative strategies and a proactive approach to cost management could mitigate some of these challenges. A nuanced understanding of these interacting forces is crucial for accurate forecasting.
Projected Hospital Margin Trends
A visual representation of projected hospital margins over the next five years would show a gradual, uneven recovery. The graph would use a line chart, with the x-axis representing the years (2024-2028) and the y-axis representing hospital operating margins (expressed as a percentage). The line would initially show a slow upward trend, reflecting some recovery from the pandemic’s immediate impact.
However, the line would not reach pre-pandemic levels (let’s say, a consistent 5% margin) within the five-year period. Instead, it would fluctuate, showing a slight dip around 2025 (possibly due to a temporary economic downturn or policy changes) before resuming a slow upward climb. Specific data points could be included, illustrating projected margins for each year (e.g., 3% in 2024, 3.5% in 2025, 4% in 2026, 4.5% in 2027, and 5% in 2028).
The pre-pandemic margin level (5%) would be shown as a horizontal dashed line for comparison. The graph would clearly indicate that while a recovery is expected, a complete return to pre-pandemic profitability is likely a longer-term goal, contingent on numerous variables. For example, a hypothetical scenario illustrating the impact of a successful value-based care implementation could be represented by a steeper upward trend from 2026 onwards, demonstrating the potential for accelerated margin improvement through this model.
Hospital margins are finally stabilizing, but unfortunately, they’re still below pre-pandemic levels. This lingering financial strain is partly due to the lingering effects of the COVID-19 crisis, a period that officially ended with the covid 19 public health emergency ends announcement. The recovery process is slow, and many hospitals are still grappling with the financial fallout, impacting their ability to fully recover to pre-pandemic profitability.
Impact of Value-Based Care on Hospital Profitability
The transition to value-based care (VBC) presents both opportunities and challenges for hospital profitability. While VBC initially requires significant upfront investment in infrastructure, technology, and workforce training, the long-term potential for improved efficiency and reduced costs can lead to enhanced margins. Hospitals successfully implementing VBC models often see reduced readmission rates and improved patient outcomes, leading to lower overall healthcare expenditures.
This can translate into improved reimbursement rates and a more sustainable revenue stream. However, the success of VBC hinges on the hospital’s ability to effectively manage population health, coordinate care across multiple settings, and demonstrate measurable improvements in patient outcomes. Hospitals that fail to adapt to VBC models may face decreased reimbursement and struggle to compete in a changing healthcare landscape.
For example, a hypothetical case study could be presented showcasing a hospital that successfully transitioned to a VBC model and saw a 2% increase in margins within three years due to a 15% reduction in readmissions.
End of Discussion: Hospital Margins To Stabilize Below Pre Pandemic Levels
The journey back to financial stability for hospitals is a marathon, not a sprint. While the immediate crisis may have passed, the lingering effects of the pandemic continue to impact hospital margins. The strategies discussed – from improved revenue cycle management and strategic partnerships to embracing telehealth and cost-cutting measures – are crucial for long-term sustainability. The future of hospital finance hinges on adaptability, innovation, and a proactive approach to navigating the ever-changing landscape of healthcare.
The outlook is complex, but with careful planning and strategic execution, hospitals can not only stabilize their margins but also build a stronger, more resilient future.
FAQ Resource
What specific government aid programs helped hospitals during the pandemic?
Several programs offered financial assistance, including the Coronavirus Relief Fund, Provider Relief Fund, and increased Medicare and Medicaid reimbursements. The specifics varied by program and location.
How are supply chain disruptions affecting hospital margins?
Disruptions lead to increased costs for essential medical supplies, equipment, and pharmaceuticals, squeezing profit margins.
What role does telehealth play in stabilizing hospital margins?
Telehealth can increase access to care, reduce overhead costs associated with in-person visits, and potentially improve efficiency.
Are all types of hospitals experiencing the same financial challenges?
No, rural hospitals, for example, often face greater challenges due to lower patient volumes and limited resources compared to larger urban hospitals.