PE Ownership Impacts Healthcare Quality, Increases Costs
PE ownership impacts healthcare quality increases costs – a statement that’s sparking intense debate. This isn’t just about dollars and cents; it’s about the very fabric of our healthcare system. We’re diving deep into how private equity’s involvement shapes the quality of care we receive, the prices we pay, and the accessibility of treatment for everyone. Get ready for a no-nonsense look at the complexities of this crucial issue.
From examining different investment strategies employed by private equity firms in healthcare to analyzing the potential trade-offs between profitability and patient well-being, we’ll explore the multifaceted effects of this increasingly prevalent business model. We’ll look at real-world examples, both positive and negative, to paint a clearer picture of this complex landscape. This isn’t just about numbers; it’s about the human impact of these financial decisions on our lives and the lives of our loved ones.
Private Equity Ownership in Healthcare
Private equity (PE) firms have significantly reshaped the healthcare landscape, impacting everything from access to care to the overall cost of treatment. Understanding the various ways PE firms engage with healthcare organizations is crucial to analyzing their influence. This discussion will delve into the different investment strategies employed by PE firms, the types of healthcare providers they typically acquire, and the resulting differences in business models compared to non-PE-owned facilities.
Private Equity Investment Strategies in Healthcare
Private equity firms utilize several strategies to invest in healthcare. These strategies vary in their approach to ownership and management, ranging from passive investments to active operational restructuring. Some common strategies include leveraged buyouts (LBOs), where the PE firm acquires a controlling stake using debt financing; minority investments, where they acquire a smaller stake without controlling influence; and growth equity investments, focusing on providing capital to expand existing businesses.
Another important strategy is the creation of platforms, where a PE firm acquires multiple smaller companies within a specific niche to create a larger, more competitive entity. These different strategies reflect the diverse goals and risk appetites of various PE firms.
Types of Healthcare Providers Acquired by Private Equity Firms, Pe ownership impacts healthcare quality increases costs
PE firms invest across a broad spectrum of healthcare providers. Common targets include physician practices (such as cardiology or dermatology groups), ambulatory surgery centers, dental practices, home health agencies, hospitals (both large and small), and long-term care facilities. The choice of target often depends on market trends, the PE firm’s investment strategy, and perceived opportunities for growth and cost optimization.
Private equity ownership’s impact on healthcare is a complex issue; often, increased profits lead to cutbacks that negatively affect quality. One example illustrating this tension is the model employed by the humana centerwell primary care centers walmart , which raises questions about accessibility and affordability despite potentially increased efficiency. Ultimately, the balance between profit and patient care remains a crucial concern in the ongoing debate about PE ownership’s effects on healthcare costs and quality.
For example, the increasing demand for outpatient care has led to significant PE investment in ambulatory surgery centers and physician practices.
Comparison of Business Models: PE-Owned vs. Non-PE-Owned Healthcare Facilities
The business models of PE-owned and non-PE-owned healthcare facilities often differ significantly. PE-owned facilities frequently prioritize efficiency and profitability, often through measures such as streamlining operations, consolidating services, and implementing cost-cutting strategies. This focus can sometimes lead to concerns about reduced patient care quality or increased patient burdens. In contrast, non-PE-owned facilities, such as those operated by non-profit organizations or government entities, may place a greater emphasis on community benefit and access to care, potentially at the expense of short-term profitability.
However, this is a generalization, and the actual practices vary greatly depending on the specific organization and its leadership.
Key Characteristics of PE-Owned and Non-PE-Owned Healthcare Providers
| Provider Type | Ownership Structure | Profitability Metrics | Patient Satisfaction Scores |
|---|---|---|---|
| Ambulatory Surgery Center | PE-owned: Typically focused on high volume, low cost procedures. | PE-owned: Higher profit margins, often driven by efficiency gains. | PE-owned: May vary depending on cost-cutting measures and staff retention. |
| Physician Practice (Cardiology) | Non-PE-owned: Often part of a larger hospital system or independent. | Non-PE-owned: Profitability varies greatly depending on payer mix and patient volume. | Non-PE-owned: Can be high due to focus on patient relationships. |
| Hospital (Rural) | PE-owned: May experience operational improvements but potential for reduced services. | PE-owned: Potential for improved financial performance through cost reduction. | PE-owned: Potentially lower scores if cost-cutting impacts staffing levels. |
| Long-Term Care Facility | Non-PE-owned: Often non-profit or government-run, focused on patient well-being. | Non-PE-owned: Lower profit margins, emphasis on quality of care over profit maximization. | Non-PE-owned: Generally high, although staffing shortages can impact scores. |
Impact of PE Ownership on Healthcare Quality
Private equity (PE) firms’ involvement in healthcare is a complex issue, sparking considerable debate regarding its impact on the quality of care. While PE investment can potentially streamline operations and introduce innovative technologies, concerns exist about prioritizing profit maximization over patient well-being. This section delves into both the potential benefits and drawbacks of PE ownership on healthcare quality, offering examples to illustrate the nuanced reality.
Positive Impacts of PE Investment on Healthcare Quality
PE firms often bring significant capital and operational expertise to healthcare organizations. This influx of resources can facilitate improvements in various aspects of care delivery. Strategic investments in technology, infrastructure upgrades, and staff training can enhance efficiency and patient outcomes. Furthermore, PE firms may implement best practices learned from managing other healthcare businesses, leading to improved processes and standardization of care.
This can translate to reduced wait times, improved diagnostic accuracy, and better overall patient experience.
Negative Impacts of PE Investment on Healthcare Quality
The pursuit of profitability inherent in PE investment models can sometimes lead to cost-cutting measures that negatively affect healthcare quality. This may involve reductions in staffing levels, limiting access to specialized services, or delaying necessary equipment upgrades. The focus on short-term returns can incentivize quick fixes rather than long-term investments in patient care infrastructure and staff development. Furthermore, a heightened emphasis on financial performance can potentially compromise the quality of care provided, especially for vulnerable patient populations.
Examples of PE Ownership’s Impact on Healthcare Quality
The impact of PE ownership on healthcare quality is not uniform; it varies greatly depending on the specific PE firm, the target organization, and the prevailing market conditions. To illustrate this variability, consider the following examples:
- Improved Quality: A PE firm’s investment in a regional hospital system led to a significant upgrade in their electronic health record (EHR) system, resulting in improved data management, reduced medical errors, and enhanced patient communication.
- Diminished Quality: In another instance, a PE-owned nursing home chain faced criticism for understaffing and insufficient training, leading to reports of substandard care and increased patient safety incidents.
- Mixed Results: A PE-backed home health agency implemented new technology to improve scheduling and patient monitoring. While this enhanced efficiency, it also resulted in reduced face-to-face time with patients, raising concerns about the quality of personalized care.
Hypothetical Scenario: Dual Impact of PE Investment
Imagine a struggling rural hospital facing closure. A PE firm invests, providing capital for much-needed equipment upgrades and attracting experienced administrators. This leads to improved diagnostic capabilities and reduced wait times, positively impacting patient outcomes. However, to meet profitability targets, the PE firm also implements cost-cutting measures, such as reducing staff in non-critical areas, potentially impacting patient support services and potentially leading to longer wait times for non-urgent appointments.
So, we’re talking about how private equity ownership impacts healthcare – often leading to increased costs and questionable quality improvements. This is especially concerning when you consider the serious health implications, like the increased risk of stroke. Understanding the risk factors, like those outlined in this helpful article on risk factors that make stroke more dangerous , is crucial.
Ultimately, the cost-cutting measures driven by PE ownership can indirectly affect access to preventative care and timely treatment, potentially worsening outcomes for conditions like stroke.
This scenario highlights the potential for both positive and negative consequences of PE investment in healthcare, underscoring the need for careful oversight and regulatory mechanisms.
The Influence of PE Ownership on Healthcare Costs
Private equity (PE) firms’ increasing involvement in healthcare has sparked considerable debate regarding its impact on costs. While PE firms often claim to improve efficiency and reduce expenses, concerns persist about potential cost increases for patients and insurers. Understanding the complex interplay of cost-cutting strategies and potential cost drivers is crucial for a balanced assessment.
Mechanisms of Cost Reduction by PE Firms in Healthcare
PE firms typically aim to boost profitability through various cost-cutting strategies. These often involve streamlining operations, negotiating lower prices from suppliers, and implementing technological solutions to enhance efficiency. For instance, a PE-owned hospital might consolidate administrative functions, reducing redundant staff and optimizing resource allocation. They might also leverage their purchasing power to negotiate bulk discounts on medical supplies and equipment.
The implementation of electronic health records (EHRs) and other digital health technologies can also contribute to cost savings by improving workflow and reducing administrative overhead. However, the success of these strategies often depends on the specific circumstances and the firm’s approach.
Comparison of Pricing Strategies
PE-owned healthcare providers might employ different pricing strategies compared to their non-PE-owned counterparts. While some PE firms may focus on cost reduction to maintain competitive pricing, others might prioritize maximizing profits through higher prices, particularly if they operate in markets with limited competition. This can lead to increased costs for patients and insurers, potentially impacting access to care.
For example, a PE-owned chain of urgent care clinics might charge higher fees than independently owned clinics, especially if they have established a dominant market position. Conversely, a PE firm might acquire a struggling hospital system and implement cost-cutting measures that allow them to offer more competitive pricing, potentially benefiting consumers in the short term. The long-term implications, however, depend on the firm’s overall strategic goals and the regulatory environment.
Hierarchical Structure of Cost Drivers Associated with PE Ownership
Understanding the various factors influencing healthcare costs under PE ownership requires a structured approach. The following hierarchical structure illustrates the key cost drivers:
- Increased Prices and Reduced Services:
- Higher Prices for Services: Driven by profit maximization strategies, potentially leading to reduced patient affordability and increased insurer expenses.
- Reduction in Service Availability: Cost-cutting measures might involve reducing services, such as eliminating less profitable departments or reducing staff, which can negatively impact patient care and access.
- Increased Administrative Costs:
- Debt Servicing: High levels of debt incurred during acquisitions can lead to increased financial burdens and pressure to maximize profits to meet debt obligations.
- Management Fees: PE firms often charge significant management fees, diverting resources away from direct patient care.
- Reduced Investment in Infrastructure and Staff:
- Deferred Maintenance: Cost-cutting measures might lead to delayed or inadequate maintenance of facilities and equipment, potentially impacting patient safety and the quality of care.
- Staffing Shortages: Pressure to reduce labor costs can lead to understaffing, increasing workload on existing employees and potentially compromising the quality of care.
PE Ownership and Access to Healthcare: Pe Ownership Impacts Healthcare Quality Increases Costs

Source: bain.com
Private equity (PE) firms’ increasing influence on the healthcare industry raises significant concerns about access to care, especially for vulnerable populations. The pursuit of profit maximization inherent in the PE model can lead to decisions that prioritize financial returns over patient needs, potentially impacting the availability and affordability of essential healthcare services. This section examines how PE ownership affects access to care, focusing on its consequences for specific communities and the healthcare workforce.PE-driven consolidation often results in reduced access to healthcare services, particularly in underserved areas.
The closure of smaller, independent clinics or hospitals following acquisitions by larger PE-backed systems can leave communities with limited options for care, increasing travel distances and potentially delaying or preventing necessary treatment. This is especially problematic for individuals with limited transportation resources, low incomes, or pre-existing health conditions requiring frequent care.
Impact of PE Consolidation on Geographic Access
The consolidation of healthcare providers under PE ownership frequently leads to the closure of facilities in rural or underserved areas. For example, the acquisition of a small, rural hospital by a large PE-backed healthcare system might result in the hospital’s closure due to perceived financial inefficiencies or a strategic shift towards more profitable urban markets. This leaves residents of the rural area with significantly reduced access to essential services like emergency care, primary care, and specialized treatments, forcing them to travel long distances to reach alternative providers.
In some cases, these long distances create insurmountable barriers to care, particularly for elderly or disabled individuals. Another example is the closure of smaller, independent physician practices after being acquired by larger PE-backed hospital systems. This can limit patient choice and increase reliance on a single, potentially less convenient or more expensive provider network.
PE Ownership and Healthcare Workforce
PE ownership can negatively impact healthcare workforce recruitment and retention. Cost-cutting measures implemented by PE firms to boost profits, such as reducing staffing levels or lowering wages, can lead to decreased morale and increased burnout among healthcare professionals. This can make it difficult to attract and retain qualified staff, especially in already understaffed areas, ultimately impacting the quality and availability of care.
The focus on short-term profits can also discourage investment in training and development programs, further hindering workforce retention and potentially reducing the overall skill level of the healthcare workforce. For instance, a PE-owned nursing home might cut staffing levels to increase profitability, leading to higher patient-to-nurse ratios and potentially compromising patient safety and quality of care.
Visual Representation: The Ripple Effect of Reduced Access
Imagine a concentric circle diagram. The central circle represents a rural community with a small, independent hospital. The next circle outward represents the surrounding area dependent on that hospital for primary and emergency care. The third circle represents more distant communities that may rely on the hospital for specialized services. If the hospital closes due to PE-driven consolidation (indicated by a large X over the central circle), the second and third circles become progressively darker, representing a decrease in access to care.
The darkness intensifies as distance increases, highlighting the disproportionate impact on those furthest from alternative healthcare options. The outer edges of the diagram could show individuals forced to forgo care altogether due to the distance and logistical barriers. This visual demonstrates how the closure of a single facility, driven by PE ownership, creates a ripple effect, diminishing access to care for a broad geographic area and exacerbating health disparities.
Private equity ownership’s impact on healthcare is a hot topic, often linked to increased costs and potentially reduced quality. But improving care is crucial, and that’s where innovative solutions come in, like those explored in this fascinating article on reimagining collaboration in senior care a technology driven approach. Ultimately, better collaboration, even with technology’s help, might be key to mitigating the negative consequences of PE ownership on patient care and costs.
Regulatory and Ethical Considerations

Source: journalistsresource.org
Private equity (PE) investment in healthcare presents a complex landscape, raising significant regulatory and ethical concerns. The pursuit of profit within a sector fundamentally focused on human well-being necessitates careful consideration of potential conflicts of interest and the impact on patient care. Existing regulations aim to mitigate some of these risks, but significant challenges remain.Existing Regulations Aimed at Mitigating Negative Consequences of PE Ownership in HealthcareSeveral regulations attempt to address the potential negative consequences of PE ownership in healthcare.
These regulations vary across jurisdictions but generally focus on transparency, antitrust concerns, and patient safety. For instance, in the United States, the Federal Trade Commission (FTC) and the Department of Justice (DOJ) scrutinize mergers and acquisitions in the healthcare sector to prevent anti-competitive practices. These agencies assess whether a proposed merger would substantially lessen competition, leading to higher prices or reduced quality of care.
Furthermore, state-level regulations often address issues such as licensing, certificate of need requirements, and oversight of healthcare facilities. These regulations, however, often struggle to keep pace with the rapid evolution of PE investment strategies and the complex structures employed by PE firms. The effectiveness of these regulations is frequently debated, with critics arguing that they are insufficient to adequately protect patients and the public interest.
Ethical Dilemmas Raised by Profit Pursuit in Healthcare by PE Firms
The inherent tension between profit maximization and the ethical obligations of healthcare providers creates significant ethical dilemmas. PE firms, by their nature, are driven by financial returns. This focus can lead to decisions that prioritize profit over patient care, such as cost-cutting measures that compromise quality, reduced staffing levels, or deferral of necessary investments in equipment or infrastructure. The prioritization of short-term financial gains over long-term patient well-being raises serious ethical questions about the fiduciary responsibilities of PE firms operating within the healthcare sector.
This conflict is further exacerbated by the often opaque nature of PE transactions, making it difficult to assess the true impact on patients and the community. The potential for conflicts of interest is substantial, particularly when PE firms exert influence over clinical decision-making.
Case Study: Ethical Concerns in PE-Owned Healthcare Facilities
A notable example illustrating these concerns involves the acquisition of a chain of nursing homes by a PE firm. Following the acquisition, cost-cutting measures were implemented, leading to reductions in staffing levels and a decline in the quality of care provided. Reports surfaced detailing instances of inadequate staffing, leading to increased patient falls and injuries, as well as delayed or inadequate medical attention.
This case highlights the potential for PE ownership to negatively impact patient outcomes when financial incentives outweigh the ethical obligation to provide quality care. While specific details of the case may vary due to confidentiality concerns, the underlying issues – the tension between profit and patient well-being – are commonly observed in similar scenarios across the healthcare landscape.
The subsequent legal battles and negative publicity surrounding the case underscore the need for stronger regulatory oversight and ethical guidelines in the industry.
Policy Recommendations for Responsible PE Investment in Healthcare
To ensure responsible integration of private equity investment in healthcare, several policy recommendations are crucial. Increased transparency regarding PE ownership and investment strategies is paramount. This includes mandatory disclosure of financial performance metrics, cost-cutting measures, and their impact on patient care. Strengthened regulatory oversight, including more robust enforcement of existing regulations and the development of new regulations tailored to the specific challenges posed by PE ownership, is also essential.
Independent oversight bodies could be established to monitor PE-owned healthcare facilities and ensure compliance with ethical standards and quality of care requirements. Finally, greater emphasis should be placed on the development of ethical guidelines specific to PE investment in healthcare, explicitly addressing conflicts of interest and promoting a patient-centered approach. These guidelines could be incorporated into licensing requirements and used as a framework for assessing the ethical implications of PE transactions.
Conclusive Thoughts
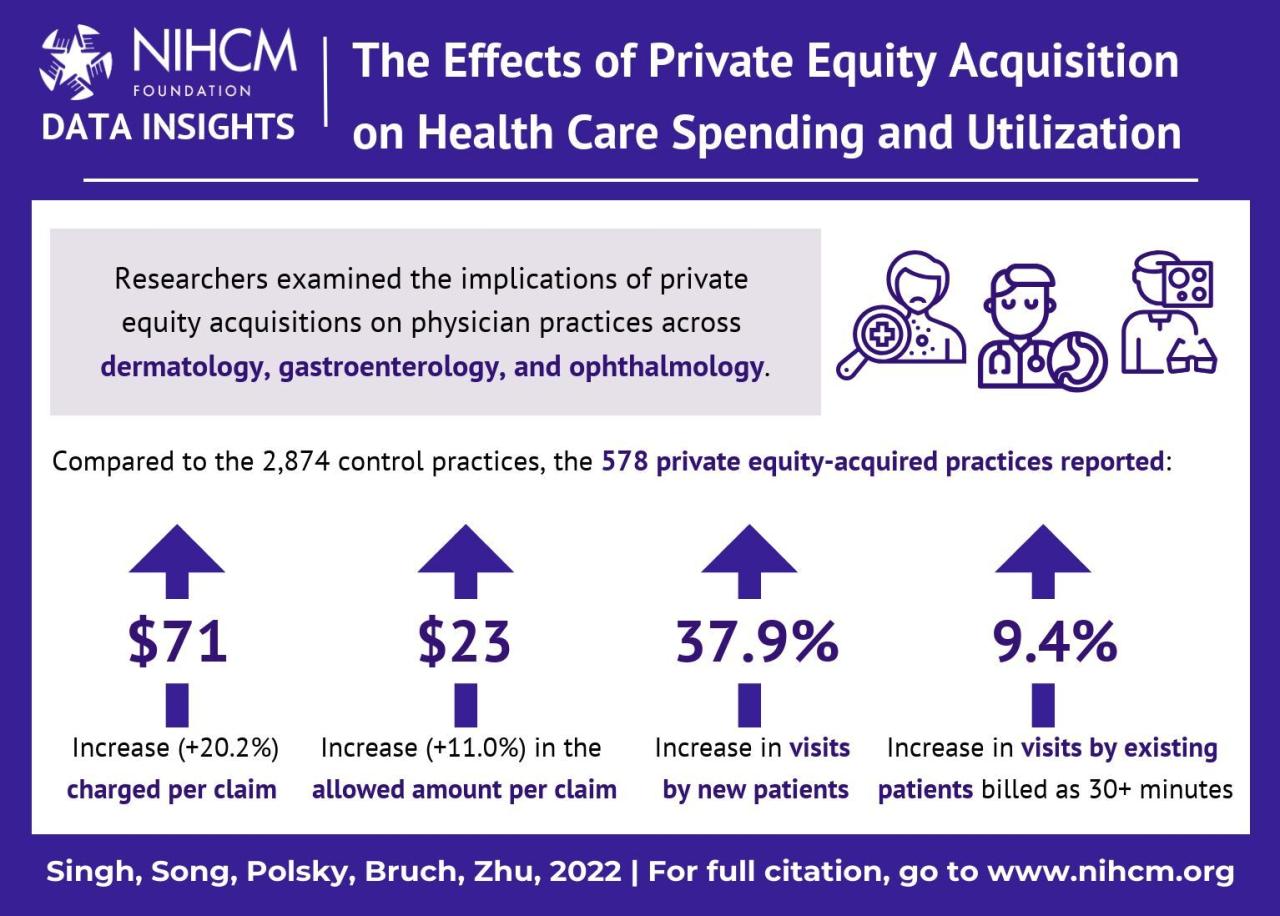
Source: nihcm.org
So, where does this leave us? The impact of private equity on healthcare is undeniably complex. While potential benefits like improved efficiency and technology upgrades exist, the potential downsides—increased costs, compromised quality of care, and reduced access—cannot be ignored. Ultimately, a thoughtful and balanced approach is crucial, one that prioritizes patient well-being above all else while acknowledging the role of financial considerations.
The conversation needs to continue, demanding greater transparency and accountability from all stakeholders to ensure a healthier future for everyone.
FAQ Section
What are some common criticisms of PE ownership in healthcare?
Critics often point to cost-cutting measures that may compromise patient care, a focus on short-term profits over long-term investments, and potential reductions in access to care, particularly for vulnerable populations.
How does PE ownership affect healthcare workers?
PE ownership can impact healthcare workers through changes in staffing levels, compensation, and benefits, potentially leading to burnout and difficulties in recruitment and retention.
Are there any regulations in place to address the concerns surrounding PE ownership in healthcare?
Yes, several regulations exist at various levels (local, state, and federal), but their effectiveness in mitigating negative impacts is a subject of ongoing debate and requires stronger enforcement.
What are some examples of successful PE investments in healthcare?
Some PE investments have led to improved technology, enhanced efficiency, and expansion of services, resulting in better patient outcomes. However, these successes are not universally applicable and often depend on the specific circumstances and the PE firm’s approach.