Pharmacy Benefits Manager House Hearing Drug Costs
Pharmacy benefits manager house hearing drug costs – that’s a mouthful, isn’t it? But it’s a seriously important topic affecting millions. We’re talking about the House hearing that delved into the murky world of prescription drug pricing, specifically the role of Pharmacy Benefit Managers (PBMs). These companies, essentially middlemen between drug manufacturers and patients, have a huge impact on what we pay at the pharmacy counter.
This hearing aimed to shed light on their practices and explore ways to lower those often exorbitant costs.
The hearing brought together key players: pharmaceutical companies defending their pricing strategies, PBMs explaining their negotiation tactics, and patient advocacy groups fighting for affordable medications. The testimony highlighted concerns about opaque PBM practices, rebates, and fees, all of which contribute to the escalating price of drugs. The debate touched upon potential legislative changes and reforms aimed at bringing more transparency and accountability to the system.
It’s a complex issue with no easy answers, but understanding the players and their roles is the first step towards finding solutions.
The Role of Pharmacy Benefit Managers (PBMs) in Drug Pricing
Pharmacy Benefit Managers (PBMs) are intermediaries in the pharmaceutical supply chain, acting as negotiators between pharmaceutical manufacturers, insurance companies, and patients. Their influence on drug pricing is substantial, making understanding their role crucial to addressing the high cost of medications. They manage prescription drug benefits for health plans, negotiating discounts and rebates with drug manufacturers, and establishing formularies (lists of covered drugs).
Functions of PBMs in the Pharmaceutical Supply Chain
PBMs perform several key functions. They process prescription claims, manage formularies, negotiate drug prices, and provide clinical services such as drug utilization review. Their role in negotiating prices significantly impacts what patients ultimately pay at the pharmacy counter. This negotiation process involves complex strategies and contractual agreements, often resulting in significant savings for health plans, but also raising concerns about potential conflicts of interest and their impact on patient access to medications.
The House hearing on pharmacy benefits managers and their impact on drug costs was intense! So many questions about price gouging and transparency remain. It’ll be interesting to see how this plays out, especially considering Robert F. Kennedy Jr. cleared a key hurdle in his bid to become HHS Secretary, as reported here: rfk jr clears key hurdle on path to hhs secretary.
His potential influence on drug pricing policies could significantly shift the landscape of the PBM debate.
The intricate relationships between PBMs, manufacturers, and insurers contribute to the overall complexity of drug pricing.
Methods of Negotiating Drug Prices
PBMs employ various strategies to negotiate lower drug prices. These include leveraging their large purchasing power to secure volume discounts, negotiating rebates based on market share, and employing sophisticated data analytics to identify cost-saving opportunities. They also use their influence to encourage manufacturers to offer lower prices for drugs included in their formularies. The effectiveness of these negotiation tactics varies depending on the drug, the manufacturer, and the specific market conditions.
For example, a PBM might negotiate a lower price for a widely used generic drug but have less leverage for a newly launched specialty medication.
Types of Rebates and Fees
PBMs receive various forms of compensation from pharmaceutical manufacturers. These include rebates, which are discounts off the list price of a drug, and administrative fees for processing claims. They may also receive spread pricing, where they charge the plan a higher price than they pay the pharmacy, keeping the difference as profit. The complexity of these arrangements makes it difficult to fully understand the overall impact on drug prices.
For instance, a rebate might initially appear to lower the cost, but the PBM might simultaneously increase its administrative fees, offsetting the savings. Transparency in these financial arrangements is essential for evaluating the true cost of prescription drugs.
Comparison of Major PBM Business Models
The business models of major PBMs vary, leading to different approaches to drug pricing and negotiations. While the core functions are similar, the specific strategies and financial arrangements can differ significantly.
| PBM | Ownership | Key Business Strategies | Notable Characteristics |
|---|---|---|---|
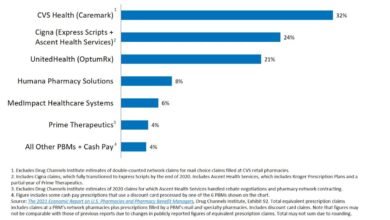
| Express Scripts | Cigna | Large scale negotiations, formulary management, specialty pharmacy services | One of the largest PBMs, significant market share |
| CVS Caremark | CVS Health | Integrated pharmacy network, focus on retail pharmacy, clinical programs | Vertically integrated model, strong retail presence |
| OptumRx | UnitedHealth Group | Data analytics driven pricing, focus on integrated care models | Strong data analytics capabilities, emphasis on cost management |
| Prime Therapeutics | Blue Cross Blue Shield plans | Cooperative model, serving Blue Cross Blue Shield plans | Member-owned, focus on serving its member plans |
House Hearing Focus and Key Concerns
Source: noworldborders.com
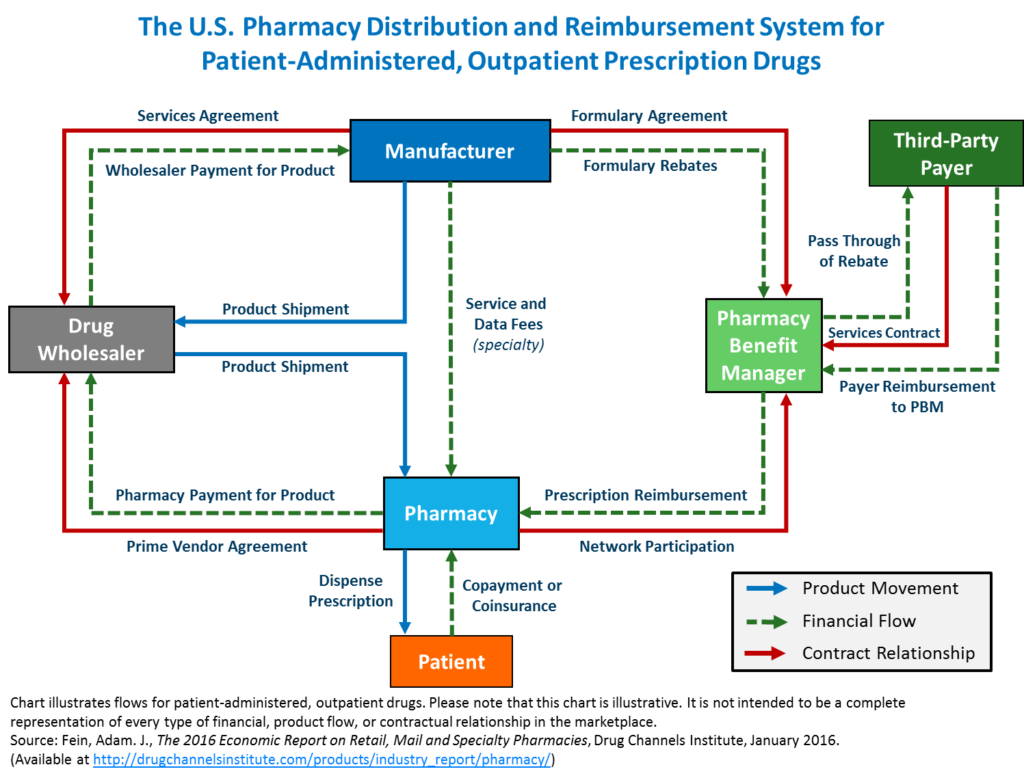
The recent House hearing on drug pricing brought to light a complex web of issues surrounding the affordability and accessibility of prescription medications. The hearing served as a platform for various stakeholders—pharmaceutical companies, Pharmacy Benefit Managers (PBMs), and patient advocacy groups—to voice their concerns and perspectives on the role PBMs play in shaping drug costs. The overarching theme revolved around the need for greater transparency and accountability within the PBM industry to ensure fair pricing and equitable access to essential medications for all Americans.The hearing extensively examined the opaque nature of PBM practices and their potential impact on patient out-of-pocket costs.
Specific concerns raised included the lack of transparency regarding rebate negotiations between PBMs and pharmaceutical manufacturers, the use of spread pricing (the difference between what PBMs pay pharmacies and what they charge insurers), and the impact of prior authorization requirements on patient access to timely and necessary treatment. These practices, it was argued, contribute to the rising cost of prescription drugs, ultimately burdening patients and hindering access to life-saving medications.
Testimony from Key Stakeholders
Pharmaceutical companies largely argued that the current system allows PBMs to negotiate excessive rebates, leading to reduced manufacturer profits and ultimately hindering research and development of new drugs. They presented data illustrating the substantial rebates they provide to PBMs, arguing that these rebates do not always translate into lower prices for patients. Conversely, PBM representatives defended their practices, emphasizing their role in managing drug costs for health plans and ultimately benefiting consumers through lower premiums.
They cited their use of formularies and other management tools as ways to control costs and ensure the efficient use of healthcare resources. Patient advocacy groups, however, painted a stark picture of the impact of high drug prices on patients. They shared compelling testimonials from individuals struggling to afford their medications, highlighting the real-world consequences of the current system on patient health and well-being.
They emphasized the need for greater transparency and regulation to protect patients from exploitative PBM practices.
Concerns Regarding PBM Practices and Patient Access
A significant concern raised during the hearing centered on the lack of transparency surrounding PBM rebate negotiations. The secretive nature of these negotiations makes it difficult to determine whether the rebates ultimately benefit patients or simply line the pockets of PBMs and insurers. The use of spread pricing, where PBMs profit from the difference between what they pay pharmacies and what they charge insurers, also drew considerable criticism.
This practice, critics argued, incentivizes PBMs to negotiate lower reimbursement rates for pharmacies, potentially leading to pharmacy closures, especially in underserved areas, thus limiting patient access to medications. Furthermore, the increasing use of prior authorization requirements, which require patients to obtain pre-approval from their insurer before receiving certain medications, was cited as a significant barrier to timely access to care.
This process often involves delays and added administrative burden for both patients and healthcare providers.
Legislative Proposals and Policy Recommendations
Several legislative proposals and policy recommendations were discussed during the hearing, aiming to address the concerns raised. These included increased transparency requirements for PBM rebate negotiations, limitations on spread pricing, and reforms to prior authorization processes. Some proposals called for the establishment of a public PBM to increase competition and drive down prices. Others focused on strengthening consumer protections and empowering patients with more information about their drug costs and PBM practices.
The specific details of these proposals varied, but the common thread was a desire to create a more transparent, accountable, and patient-centered system for managing prescription drug costs. For example, one proposed bill would require PBMs to publicly disclose their rebate negotiations and spread pricing practices, while another would limit the use of prior authorizations to specific, clinically justified circumstances.
Impact of PBM Practices on Patients and Healthcare Providers
Pharmacy Benefit Managers (PBMs) play a significant role in the prescription drug market, impacting not only drug prices but also patient access and healthcare provider choices. Their practices, while aiming for cost-efficiency, often lead to unintended consequences for patients and providers alike. Understanding these effects is crucial for developing effective policies to improve the healthcare system.
Patient Out-of-Pocket Costs
PBMs’ influence on patient out-of-pocket costs is multifaceted. Their negotiation strategies with pharmaceutical manufacturers, while potentially lowering overall costs for payers, can lead to higher patient cost-sharing through increased co-pays, deductibles, and coinsurance. The use of tiered formularies, where drugs are categorized based on cost and efficacy, often places more expensive, newer medications in higher tiers, resulting in significantly higher out-of-pocket expenses for patients.
Additionally, the spread pricing model, where PBMs profit from the difference between the negotiated price and the reimbursement price paid by insurers, can indirectly increase patient costs by inflating the overall price of drugs. For example, a patient prescribed a brand-name drug might face a significantly higher copay than if the PBM negotiated a lower price directly with the manufacturer, leading to a direct increase in the patient’s out-of-pocket expenses.
Medication Formularies and Prior Authorization Requirements
PBMs exert considerable control over medication formularies, the lists of drugs covered by a health plan. The inclusion or exclusion of specific drugs on these formularies significantly impacts patient access to needed medications. This is further complicated by prior authorization requirements, which necessitate physician pre-approval before a patient can receive a specific medication. These requirements often involve time-consuming paperwork and delays, potentially disrupting treatment and causing unnecessary frustration for both patients and healthcare providers.
For instance, a patient needing a specific medication for a chronic condition might find that medication excluded from their formulary, forcing them to try alternative, potentially less effective treatments, or navigate the often-complex prior authorization process. This can create significant hurdles, especially for patients with complex medical needs.
Impact on Healthcare Provider Prescribing Practices
PBM practices can directly influence the medications healthcare providers can prescribe. The restrictive nature of formularies and prior authorization requirements can limit provider choices, potentially forcing them to prescribe less effective or more expensive alternatives. This interference can compromise the physician-patient relationship and limit access to optimal treatments. Physicians might find themselves spending significant time justifying their prescribing decisions to PBMs, diverting their attention from patient care.
This administrative burden adds to the overall stress and inefficiency within the healthcare system. A physician might prefer to prescribe a specific medication based on their clinical judgment and the patient’s specific needs, but if that medication is not on the formulary or requires extensive prior authorization, the physician may be forced to choose a less suitable alternative.
Barriers to Patient Access to Affordable Medications
The combined effect of high out-of-pocket costs, restrictive formularies, and burdensome prior authorization requirements creates significant barriers to affordable medication access. Patients facing financial constraints might be forced to forgo necessary medications or skip doses, jeopardizing their health outcomes. This is particularly true for patients with chronic conditions requiring ongoing medication, where the cumulative cost of these barriers can become overwhelming.
For example, a patient with diabetes might find that their preferred insulin is not covered by their plan, or that obtaining it requires navigating a complex prior authorization process, ultimately leading to inconsistent treatment and poorer health management. These situations illustrate how PBM practices can exacerbate existing health disparities and negatively impact patient well-being.
Transparency and Accountability in PBM Operations
The lack of transparency in Pharmacy Benefit Manager (PBM) operations is a significant contributor to the high cost of prescription drugs. The complex web of rebates, fees, and administrative practices makes it difficult to understand how PBM profits are generated and how these profits impact the final price paid by patients and insurers. Increased transparency and robust accountability measures are crucial to ensuring fair pricing and equitable access to essential medications.The opaque nature of PBM operations obscures the true cost of prescription drugs and hinders efforts to control escalating healthcare expenses.
This lack of visibility creates an environment where PBM practices can inadvertently, or intentionally, inflate drug prices without sufficient oversight. Addressing this issue requires a multifaceted approach involving greater transparency in PBM financial dealings and improved regulatory oversight.
PBM Rebates and Fee Structures Lack Transparency
The intricate system of rebates and fees negotiated between PBMs, pharmaceutical manufacturers, and health plans is largely shrouded in secrecy. Manufacturers offer rebates to PBMs in exchange for favorable formulary placement, which influences which drugs are covered by insurance plans and at what cost-sharing level. However, the details of these negotiations—including the size of the rebates and how they are used—are often kept confidential.
This lack of transparency makes it difficult to determine whether rebates are actually passed on to patients in the form of lower out-of-pocket costs or whether they simply inflate PBM profits. For example, a manufacturer might offer a large rebate to a PBM, but the PBM might only pass a small portion of that rebate on to the patient, keeping the remainder as profit.
This opaque system makes it hard to determine if the system is working as intended. Similarly, the various fees charged by PBMs to pharmacies and health plans are often unclear, making it challenging to assess their reasonableness and impact on drug costs.
Methods for Improving PBM Accountability and Oversight, Pharmacy benefits manager house hearing drug costs
Improving accountability and oversight of PBM activities requires a multi-pronged approach. One crucial step is mandating greater transparency in PBM financial reporting. This could involve requiring PBMs to publicly disclose their revenue streams, including rebates and fees, as well as their profit margins on specific drugs. Additionally, independent audits of PBM practices could help ensure that their operations align with the interests of patients and healthcare providers.
Strengthening state and federal regulations governing PBM practices is also essential. This might involve implementing stricter requirements for disclosure of rebates and fees, as well as establishing clearer guidelines on formulary management practices. A standardized reporting format could ensure consistency and comparability across different PBMs.
Framework for Enhanced Regulatory Oversight of PBMs
A robust framework for enhanced regulatory oversight of PBMs is essential to ensure fair pricing and patient access to medications. This framework should include the following elements: First, mandatory public disclosure of all rebates, fees, and administrative costs associated with drug pricing. Second, independent audits of PBM operations to verify the accuracy of reported data and identify potential conflicts of interest.
Third, the establishment of clear guidelines on formulary management practices to prevent PBMs from manipulating drug selection to maximize their profits. Fourth, stronger enforcement mechanisms to penalize PBMs for non-compliance with regulations. Fifth, the creation of a central database to track PBM activities and facilitate analysis of their impact on drug prices and patient access. Such a framework, modeled perhaps on existing regulations for other sectors with similar complexities, would provide a level of transparency and accountability that is currently lacking and would allow for better oversight of the PBM industry.
For instance, the framework could incorporate elements similar to those used in regulating financial institutions, where regular reporting and audits are mandated to maintain transparency and prevent fraudulent activities.
Alternative Models for Drug Pricing and PBM Reform
The current system of drug pricing and PBM operation has generated considerable controversy, leading to calls for significant reform. Several alternative models are being debated, each with its own set of potential benefits and drawbacks for patients, providers, manufacturers, and PBMs themselves. These models represent a range of approaches, from incremental adjustments to the existing system to more radical overhauls.
Understanding these different approaches is crucial for informed policymaking.
Government Negotiation of Drug Prices
This model proposes allowing the government, either at the federal or state level, to directly negotiate drug prices with pharmaceutical manufacturers, similar to the approach used by other developed countries. This could lead to lower prices for taxpayers and patients, particularly for high-cost medications. However, it also raises concerns about potential limitations on pharmaceutical innovation due to reduced profitability, as well as potential political influence on drug selection.
For example, the potential for political interference in drug selection could prioritize cheaper options over those that offer superior efficacy. Furthermore, manufacturers might shift production away from the US market, reducing domestic competition and innovation. The impact on patients would depend on the negotiation’s effectiveness and whether the savings are passed on fully.
Increased PBM Transparency and Regulation
This approach focuses on enhancing transparency and accountability within the PBM industry through stricter regulations and reporting requirements. This could include mandating the disclosure of rebates, fees, and other financial arrangements between PBMs, manufacturers, and pharmacies. The goal is to curb practices that drive up costs without providing commensurate value to patients or the healthcare system. Increased regulation could lead to more predictable pricing and fairer competition, benefiting patients and providers.
However, it might also increase administrative burdens and potentially stifle innovation if overly restrictive. A real-world example would be requiring PBMs to publicly disclose the spread between what they pay manufacturers and what they charge insurers, which could expose excessive profit margins.
Reference Pricing Models
Reference pricing models compare the prices of a drug across different countries or regions to establish a benchmark. This benchmark then serves as a basis for negotiating or setting prices domestically. This approach aims to leverage international price differences to control drug costs. While this could lead to lower prices, it also risks limiting access to newer, more expensive drugs, particularly those with limited availability in countries with lower drug prices.
The House hearing on pharmacy benefits managers and their impact on drug costs is heating up! With the potential for significant changes to the system, it’ll be interesting to see how things play out, especially considering the recent news that rfk jr confirmed hhs secretary robert f kennedy jr , which could significantly influence healthcare policy, including drug pricing regulations.
This new administration might prioritize tackling the issues raised at the hearing in a more decisive way.
The impact on pharmaceutical innovation is a significant concern, as it could disincentivize investment in new drugs if prices are capped too low.
Public Option for Drug Insurance
The creation of a public drug insurance option, similar to Medicare, could introduce competition into the private insurance market, potentially leading to lower prices and improved coverage. This could provide greater access to medications for uninsured or underinsured individuals. However, the implementation of such a program would require significant government investment and careful design to avoid unintended consequences, such as market disruption or excessive administrative costs.
The success of such a model would depend heavily on its design and funding mechanisms.
Market-Based Reforms Focused on Competition
These reforms aim to foster greater competition within the pharmaceutical industry and the PBM sector. This might involve reducing barriers to entry for generic drug manufacturers or promoting greater transparency in drug development costs. Increased competition could theoretically lead to lower drug prices. However, the effectiveness of this approach hinges on the ability to create a genuinely competitive market, which is challenging in an industry characterized by high barriers to entry and complex regulatory hurdles.
Visual Representation of Key Findings: Pharmacy Benefits Manager House Hearing Drug Costs

Source: bannerbear.com
The House hearing on pharmacy benefits managers and their impact on drug costs got me thinking about healthcare leadership in general. It’s a complex issue, and the news about AdventHealth CEO Terry Shaw’s retirement highlights how much pressure these leaders face navigating such challenges. Ultimately, finding solutions to lower drug prices requires collaboration across the entire healthcare system, from CEOs to PBMs.
The following visualizations aim to clarify the complex relationship between Pharmacy Benefit Manager (PBM) practices and the escalating cost of prescription drugs, as well as the impact on patient access. These are simplified representations for illustrative purposes and do not encompass the full nuance of the issue.The data presented is hypothetical, representing general trends observed in the industry and should not be taken as precise, verifiable figures.
Specific data points would require extensive research and analysis from multiple sources.
PBM Practices and Drug Costs
This bar graph illustrates the potential influence of various PBM practices on the final cost of a prescription drug. The X-axis represents different PBM practices, such as rebates, spread pricing, and administrative fees. The Y-axis represents the increase in drug cost to the consumer. Each bar represents a specific PBM practice, and its height corresponds to the estimated percentage increase in drug cost attributed to that practice.
For example, a tall bar for “Spread Pricing” would indicate a significant contribution of this practice to increased drug costs. A shorter bar for “Rebates” might show that while rebates exist, their impact on lowering the final cost for the consumer is less than the impact of other practices that inflate costs. This visualization would clearly demonstrate which PBM practices are most strongly correlated with higher drug prices.
Impact of PBM Practices on Patient Access to Medications
This pie chart visually represents the proportion of patients facing challenges in accessing medications due to different PBM practices. The chart is divided into segments, each representing a specific barrier. For example, one segment could represent patients facing high out-of-pocket costs due to formulary restrictions or prior authorization requirements. Another segment could illustrate patients unable to afford medications due to high co-pays or lack of financial assistance programs.
A third segment could show patients experiencing delays in medication access due to prior authorization processes. The size of each segment directly reflects the percentage of patients affected by that particular barrier. This visual clearly highlights the significant impact of PBM practices on patient access, allowing for a clear understanding of the extent to which different aspects of PBM operations affect patient ability to receive necessary medications.
End of Discussion
The House hearing on pharmacy benefits manager drug costs left a lasting impression, not just for its detailed examination of PBM practices, but also for the stark contrast between the perspectives of different stakeholders. While the hearing didn’t offer immediate solutions, it undeniably spurred crucial conversations about transparency, accountability, and the urgent need for reform. The path forward remains unclear, but the spotlight shone on this critical issue, hopefully paving the way for meaningful change and more affordable medications for everyone.
Query Resolution
What exactly
-are* Pharmacy Benefit Managers (PBMs)?
PBMs are third-party administrators of prescription drug programs for insurance companies and employers. They negotiate drug prices with manufacturers, manage formularies (lists of covered drugs), and process prescription claims.
How do PBMs profit from high drug prices?
PBMs receive rebates and fees from drug manufacturers, often tied to the volume of prescriptions filled. Some critics argue this incentivizes them to steer patients towards more expensive drugs, even if cheaper alternatives exist.
What are some examples of PBM practices that increase costs?
Examples include spread pricing (keeping the difference between what they pay and what they charge insurers), restrictive formularies limiting patient choices, and complex prior authorization processes delaying access to necessary medications.