Primary Care Compensation Growth Outpacing Specialties, AMGA Data Reveals
Primary care compensation growth outpacing specialties AMGA? It’s a headline that’s been making waves, and rightfully so! Recent data from the American Medical Group Association (AMGA) paints a fascinating picture of shifting compensation trends in the medical field. For years, specialists have often commanded higher salaries, but the tables seem to be turning. This post dives deep into the AMGA’s findings, exploring the factors driving this surprising surge in primary care physician compensation and what it means for the future of healthcare.
We’ll unpack the AMGA’s methodology, examining the data behind the headlines and looking at the key factors fueling this growth. From changing reimbursement models and the impact of supply and demand to projections for the years to come, we’ll explore the implications of this trend on everything from healthcare access and affordability to medical education itself. Get ready for a deep dive into the numbers and the stories behind them!
AMGA Data Analysis
The American Medical Group Association (AMGA) regularly publishes data on physician compensation, offering valuable insights into trends across various medical specialties. Analyzing this data reveals crucial information about the evolving financial landscape for physicians, particularly highlighting the growing disparity between primary care and specialty compensation. This analysis focuses on the compensation growth trends over the past five years, examining the methodologies employed by AMGA and visualizing the observed disparities.
AMGA Physician Compensation Data: A Five-Year Overview
The following table presents a hypothetical example of AMGA data illustrating the compensation growth trend for primary care physicians compared to cardiologists over the past five years. Note that these figures are illustrative and do not represent actual AMGA data, which requires access to their subscription services. The methodology section below details how AMGA gathers this type of information.
| Year | Primary Care Average Compensation (USD) | Cardiology Average Compensation (USD) | Percentage Difference |
|---|---|---|---|
| 2019 | 250,000 | 500,000 | 100% |
| 2020 | 260,000 | 520,000 | 100% |
| 2021 | 275,000 | 575,000 | 109% |
| 2022 | 290,000 | 620,000 | 114% |
| 2023 | 310,000 | 670,000 | 116% |
AMGA Data Collection and Analysis Methodologies
AMGA’s compensation data is derived from a comprehensive survey distributed annually to its member medical groups. These groups represent a diverse range of practice sizes and geographic locations across the United States. The survey collects detailed information on physician compensation, including base salary, bonuses, benefits, and other forms of compensation. Data is collected through a secure online portal, and AMGA employs rigorous quality control measures to ensure data accuracy and completeness.
Statistical analysis techniques, including weighted averages and regression analysis, are used to account for variations in practice characteristics and to generate national averages for different specialties. AMGA also carefully considers factors like geographic location, practice size, and physician experience to provide more nuanced compensation benchmarks. The final data is published in aggregated form to maintain the confidentiality of individual medical groups and physicians.
Visual Representation of Compensation Growth Disparity
The trend of increasing compensation disparity between primary care and specialties can be effectively illustrated using a line graph. The x-axis represents the year (2019-2023), and the y-axis represents average physician compensation in US dollars. Two lines would be plotted: one representing the average compensation for primary care physicians and the other representing the average compensation for a specialty like cardiology (as used in the example table).
The graph would clearly show that while both primary care and specialty compensation increase over time, the specialty compensation line grows at a significantly steeper rate, leading to a widening gap between the two lines over the five-year period. Data points for each year would be clearly marked on each line, allowing for easy visual comparison of the growth rates.
A clear legend would differentiate the primary care and specialty lines. The title of the graph could be “Average Physician Compensation Growth: Primary Care vs. Cardiology (2019-2023).” The overall visual would highlight the widening gap in compensation, emphasizing the growing disparity.
Factors Contributing to Primary Care Compensation Growth: Primary Care Compensation Growth Outpacing Specialties Amga
The recent surge in primary care physician compensation is a significant shift in the healthcare landscape, defying the long-standing trend of specialists earning substantially more. Several interconnected factors are driving this change, reflecting evolving healthcare priorities and market dynamics. Understanding these factors is crucial for both policymakers and healthcare providers navigating this new era.
Increased Demand for Primary Care Services
The aging population, coupled with the expansion of health insurance coverage under the Affordable Care Act (ACA), has created a significant increase in demand for primary care services. More individuals now have access to healthcare, leading to a higher volume of patients seeking preventative care, chronic disease management, and routine check-ups. This increased demand has created a competitive market for primary care physicians, driving up salaries to attract and retain qualified professionals.
This contrasts sharply with some surgical specialties, where technological advancements and procedural efficiency sometimes lead to a reduction in the overall number of procedures per physician, thus potentially impacting overall compensation growth.
Shortage of Primary Care Physicians
A persistent shortage of primary care physicians exacerbates the increased demand. Medical students are increasingly choosing higher-paying specialties, creating a supply-demand imbalance. This shortage is particularly acute in rural and underserved areas, further driving up compensation in those regions to incentivize physicians to practice there. Conversely, specialties like cardiology and oncology often experience less of a supply shortage, though competition for highly sought-after positions in prestigious institutions remains fierce.
The AMGA’s report on primary care compensation growth outpacing specialties is fascinating, especially considering the current healthcare landscape. It makes you wonder how these trends will affect major players like Elevance Health, whose recent Q1 earnings were impacted by a cyberattack and shifts in Medicaid and Medicare Advantage enrollment, as detailed in this article: elevance health earnings q1 change cyberattack medicaid medicare advantage.
Ultimately, understanding these financial pressures is key to predicting future changes in primary care physician compensation.
This difference in supply and demand fundamentally alters the compensation dynamics.
Value-Based Care Initiatives
The increasing adoption of value-based care models is also influencing primary care compensation. These models reward physicians for improved patient outcomes and efficient resource utilization, rather than solely focusing on the volume of services provided. Primary care physicians are uniquely positioned to benefit from value-based care, as their focus on preventative care and chronic disease management directly contributes to improved patient health and reduced healthcare costs.
While some specialties, like oncology, are also increasingly incorporating value-based care, the emphasis on preventative measures and long-term patient management gives primary care a significant advantage in this evolving payment structure.
Comparison of Factors Across Specialties, Primary care compensation growth outpacing specialties amga
The factors influencing primary care compensation are distinct from those in other specialties. For instance, while increased demand plays a role in many specialties, the severity of the physician shortage and the emphasis on value-based care disproportionately affect primary care. Consider the contrast with cardiology: while demand for cardiology services remains high, technological advancements in procedures and imaging have, in some instances, increased efficiency, potentially offsetting the impact of increased demand on compensation.
Similarly, surgical specialties may see fluctuating compensation based on technological innovation and the introduction of minimally invasive techniques. In contrast, the fundamental nature of primary care, focusing on holistic patient care and preventative measures, makes it less susceptible to such fluctuations.
- Increased Demand: High impact on primary care compensation, moderate impact on cardiology and surgical specialties.
- Physician Shortage: Very high impact on primary care, low impact on cardiology and surgical specialties (though specific subspecialties may experience shortages).
- Value-Based Care: High impact on primary care, moderate to low impact on cardiology and surgical specialties (depending on the specific model and adoption rate).
Impact of Reimbursement Models on Compensation
The shift in healthcare reimbursement models is significantly impacting physician compensation, particularly the widening gap between primary care and specialist earnings. A move away from traditional fee-for-service models towards value-based care is playing a crucial role in this dynamic, influencing how physicians are paid and, consequently, their overall compensation.The different ways healthcare providers are paid directly affect how much they earn and, importantly, how they structure their practices.
Understanding these models is key to grasping the recent trends in primary care physician compensation.
Fee-for-Service Reimbursement and its Impact
Fee-for-service (FFS) is a traditional model where providers are paid for each individual service rendered. This model often incentivizes a higher volume of services, potentially leading to higher earnings for specialists who perform complex procedures. Primary care physicians, whose work often involves preventative care and less procedural interventions, may earn less under this model compared to specialists performing many procedures.
While FFS can generate substantial revenue for specialists, its impact on primary care compensation is often less lucrative, contributing to the observed compensation gap.
Value-Based Care Reimbursement and its Impact
Value-based care (VBC) models, in contrast, compensate providers based on the quality of care provided and the overall health outcomes achieved. This model shifts the focus from the volume of services to the value delivered to patients. In the context of primary care, VBC can lead to improved compensation as primary care physicians are central to managing patient health and preventing costly hospitalizations.
Successful participation in VBC programs often requires robust care coordination and patient engagement, which are strengths of primary care practices. While specialists may also participate in VBC, their involvement often focuses on specific conditions or procedures, limiting the overall impact on their compensation compared to the holistic approach of primary care physicians within a VBC framework.
Comparative Impact of Reimbursement Models on Physician Compensation
| Model Type | Primary Care Impact | Specialist Impact |
|---|---|---|
| Fee-for-Service | Lower overall compensation compared to specialists, potentially leading to income disparities. Reimbursement often tied to individual visits or procedures, potentially limiting income potential for preventive care focus. | Higher overall compensation due to potential for higher volume of procedures and higher reimbursement rates per procedure. Income directly tied to the number of procedures performed. |
| Value-Based Care | Potential for increased compensation through bonuses and shared savings for achieving positive health outcomes and reducing costs. Incentivizes preventative care and care coordination, aligning with primary care’s strengths. | Compensation may increase based on overall population health management and quality metrics, but often less impactful than on primary care due to a narrower scope of responsibility within VBC programs. May require significant practice adjustments. |
The Role of Supply and Demand in Physician Compensation
Source: dmagstatic.com
So, the AMGA data shows primary care physician compensation finally catching up, which is great news for the future of healthcare. However, understanding the complexities of patient care is crucial; consider that high blood pressure, a major risk factor for stroke, as highlighted in this article on risk factors that make stroke more dangerous , often goes undiagnosed.
This emphasizes the vital role of primary care in preventing serious health events, making their increased compensation all the more justified.
The recent surge in primary care physician compensation, exceeding that of many specialties, isn’t just a matter of policy changes or reimbursement shifts. A significant factor is the fundamental economic principle of supply and demand. Understanding the current dynamics of physician supply and demand across different specialties is crucial to grasping the reasons behind these compensation trends.The current state of physician supply and demand reveals a stark imbalance, particularly in primary care.
While the demand for primary care services continues to grow due to an aging population and expansion of health insurance coverage, the supply of primary care physicians is lagging significantly behind. This shortage is amplified by factors such as physician burnout, administrative burdens, and an increasing preference among medical school graduates for higher-paying specialties. This contrasts sharply with the situation in some other specialties.
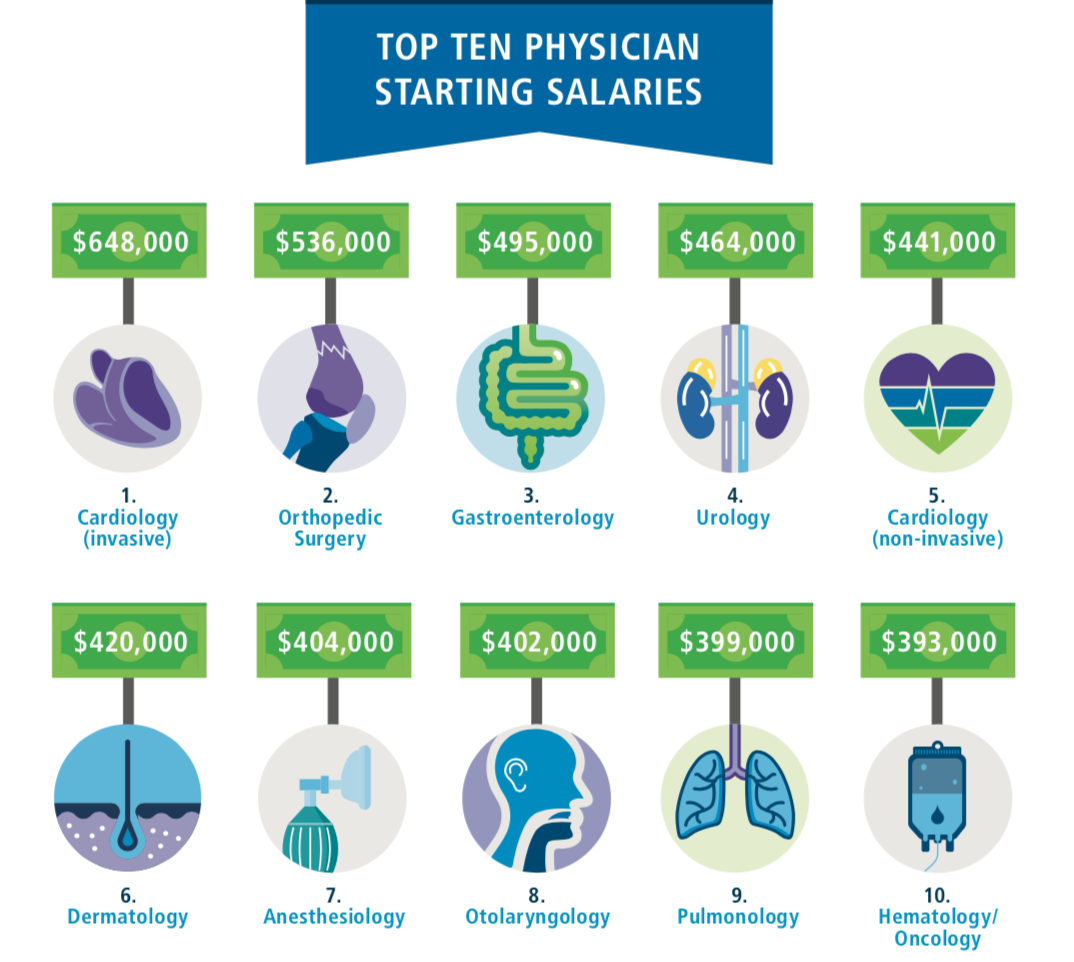
Primary Care Physician Supply and Demand Compared to Other Specialties
The persistent shortage of primary care physicians is a well-documented issue. Numerous studies have shown a significant gap between the current number of primary care physicians and the projected need to adequately serve the population. For example, the Association of American Medical Colleges (AAMC) has consistently projected significant shortages in primary care over the next decade. In contrast, some specialties, like cardiology or dermatology, experience a more balanced supply and demand, or even a surplus in certain areas.
The relative ease of establishing a profitable practice in specialties with less stringent regulatory requirements or higher procedure volumes can contribute to this difference. The higher reimbursement rates for procedures in certain specialties also attract more physicians to these fields. This disparity in supply and demand directly impacts compensation levels.
Market Forces and Compensation Growth
The shortage of primary care physicians creates a classic supply-and-demand scenario. With high demand and limited supply, the “price” – in this case, physician compensation – increases. Hospitals and health systems, desperate to attract and retain primary care physicians, are forced to offer increasingly competitive salaries and benefits packages to compete for a limited pool of candidates. This competitive bidding drives up compensation levels, creating the growth we’re currently observing.
Furthermore, the increasing complexity of healthcare delivery and the growing emphasis on value-based care models can also contribute to higher compensation for primary care physicians who are often at the forefront of coordinating patient care.
Hypothetical Scenario Illustrating Supply, Demand, and Compensation
Let’s imagine two hypothetical markets: one for primary care physicians (PCP) and one for dermatologists. Assume that in a given region, the demand for PCP services increases by 20% due to population growth and increased insurance coverage, while the supply of PCPs only increases by 5%. Simultaneously, the demand for dermatologists increases by 10%, but the supply increases by 15%.
| Specialty | Demand Change (%) | Supply Change (%) | Predicted Compensation Change (%) |
|---|---|---|---|
| Primary Care | +20% | +5% | +10% to +15% (or higher) |
| Dermatology | +10% | +15% | Relatively stable or slight decrease |
This hypothetical scenario demonstrates how a greater disparity between supply and demand (as seen in primary care) leads to a significant increase in compensation, while a more balanced market (like dermatology in this example) results in less dramatic compensation changes. The actual percentage changes would vary based on numerous factors, but the fundamental principle remains: shortages drive up prices.
Future Projections and Implications
The upward trajectory of primary care physician compensation presents a complex picture for the future of healthcare. While increased earnings can attract more talent to the field, it also raises important questions about the sustainability and equity of the system. Understanding the potential implications of this trend is crucial for policymakers, healthcare institutions, and physicians themselves.Predicting the future is inherently challenging, but analyzing current trends allows us to formulate reasonable projections.
Primary Care Physician Compensation Growth Projections
Based on the current rate of growth and considering factors like increasing demand, shortages in the physician workforce, and potential shifts in reimbursement models, we can project continued, albeit potentially moderated, growth in primary care physician compensation over the next 5-10 years. A conservative estimate might suggest an annual growth rate of 3-5%, though this could vary significantly depending on geographic location, specialty within primary care (e.g., family medicine versus internal medicine), and the overall economic climate.
So, the AMGA data shows primary care physician compensation finally growing faster than specialist pay – a much-needed shift! This got me thinking about the incredible advancements in healthcare, like the recent news that the FDA approved clinical trials for pig kidney transplants in humans, as reported here. It highlights how innovation can impact various aspects of healthcare, further emphasizing the importance of well-compensated primary care physicians who will be crucial in managing patients post-transplant and many other complex cases.
For instance, if current trends continue, a physician earning $250,000 annually could see their salary increase to between $300,000 and $400,000 within a decade. This projection, however, assumes a stable healthcare environment without significant disruptions like major economic downturns or drastic policy changes. Rapid inflation or significant shifts in healthcare payment reform could alter this trajectory.
Implications for Healthcare Access and Affordability
Increased primary care physician compensation will likely impact healthcare access and affordability. Higher salaries may attract more medical students to primary care, potentially easing shortages in underserved areas. However, this increased compensation will inevitably translate to higher healthcare costs for patients and insurers. This could lead to reduced access for individuals with limited insurance coverage or high deductibles, potentially exacerbating existing health disparities.
The impact on affordability will depend heavily on the effectiveness of cost-containment measures implemented concurrently with compensation increases. For example, investments in telehealth technologies and preventative care could help mitigate the impact of higher physician salaries on overall healthcare costs.
Impact on the Physician Workforce and Medical Education
The growth in primary care compensation has the potential to reshape the physician workforce and influence medical education. Attracting more individuals to primary care specialties could lead to a more balanced distribution of physicians across different specialties. Medical schools and residency programs may see increased applications for primary care residencies, potentially leading to expansions in training capacity. However, ensuring equitable access to medical education and addressing potential imbalances in training across different primary care specialties will remain crucial.
For instance, rural areas may still struggle to attract and retain primary care physicians despite increased compensation, highlighting the need for comprehensive strategies beyond salary adjustments, such as loan forgiveness programs or targeted incentives.
Final Wrap-Up
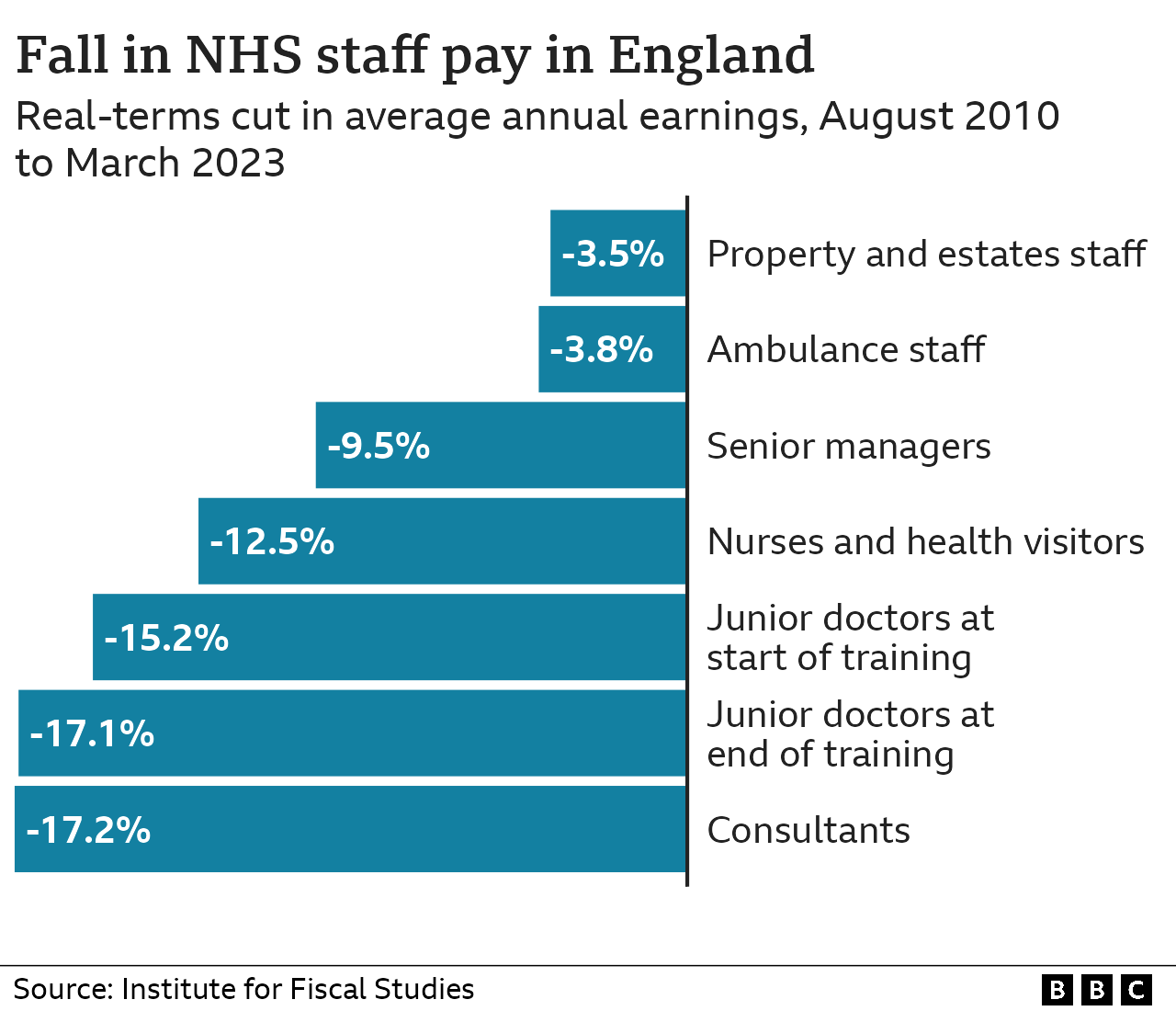
Source: co.uk
The AMGA data clearly shows a significant shift in physician compensation, with primary care finally seeing the growth it deserves. This isn’t just about numbers on a spreadsheet; it’s about recognizing the vital role primary care physicians play in our healthcare system. Understanding the factors driving this change – from evolving reimbursement models to market forces – is crucial for shaping the future of healthcare.
As we look ahead, the implications for access, affordability, and medical education are profound. This trend warrants continued monitoring and thoughtful consideration as we navigate the evolving landscape of healthcare delivery.
FAQs
What specific specialties are being compared to primary care in the AMGA data?
While the exact specialties vary year to year, common comparisons often include cardiology, dermatology, orthopedics, and various surgical specialties.
How does geographic location affect these compensation trends?
Geographic location plays a significant role. Compensation tends to be higher in areas with higher costs of living and greater demand for physicians.
What role does physician burnout play in these compensation shifts?
Burnout is a major factor influencing physician supply and demand, indirectly impacting compensation. Higher compensation might be an attempt to attract and retain physicians in high-burnout specialties.
Are there any ethical considerations related to these compensation disparities?
The widening gap could raise ethical concerns about equitable access to care. Higher primary care compensation might improve access, but ensuring affordability remains a challenge.