Hundreds Rural Hospitals Risk Closing Healthcare Reforms Impact
Hundreds rural hospitals risk closing center healthcare quality payment reform. It’s a chilling headline, isn’t it? The reality is even more stark: rural healthcare is facing a crisis, a perfect storm brewed from dwindling patient populations, outdated reimbursement models, and the increasingly complex demands of nationwide healthcare quality payment reforms. This isn’t just about numbers on a spreadsheet; it’s about the lives and well-being of countless individuals in already vulnerable communities.
We’re going to dive deep into the heart of this issue, exploring the challenges, the potential solutions, and the urgent need for change.
The financial struggles of rural hospitals are multifaceted. Declining populations mean fewer patients, directly impacting revenue. Reimbursement models often fail to adequately compensate for the unique challenges of providing care in rural settings, such as higher transportation costs and specialized staffing needs. Add to this the complexities of meeting the stringent requirements of healthcare quality payment reform, and you have a recipe for disaster.
Many rural hospitals are simply unable to keep up, leading to closures and leaving communities without access to essential healthcare services.
The Current State of Rural Hospitals
The plight of rural hospitals across the nation is a growing concern, marked by increasing financial instability and the looming threat of closure. These facilities, often the sole providers of healthcare in their communities, face unique challenges that significantly impact their ability to deliver essential services. Understanding these challenges is crucial to developing effective solutions and ensuring continued access to healthcare in rural areas.
Financial Challenges Faced by Rural Hospitals
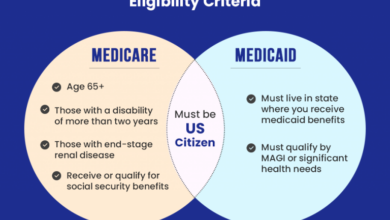
Rural hospitals operate within a complex financial ecosystem characterized by several key stressors. Lower patient volumes compared to urban counterparts directly translate to reduced revenue. These hospitals often serve a population with higher rates of chronic illnesses and lower socioeconomic status, leading to a higher proportion of patients relying on government insurance programs like Medicare and Medicaid, which typically reimburse at lower rates than private insurance.
The added burden of providing uncompensated care further exacerbates their financial difficulties. Additionally, rural hospitals often struggle to attract and retain qualified medical professionals due to limited compensation and opportunities for professional development, adding to their operational costs. The high cost of maintaining facilities and specialized equipment in sparsely populated areas also contributes significantly to their financial fragility.
Impact of Declining Patient Populations on Rural Hospital Viability
Declining populations in rural areas are a significant driver of financial distress for rural hospitals. As the population ages and young people migrate to urban centers seeking employment opportunities, the patient base shrinks, resulting in decreased admissions and revenue. This trend is particularly pronounced in areas experiencing economic hardship and limited job growth. The reduction in patient volume forces hospitals to cut services or even close entirely, leaving residents with limited access to critical healthcare services and increasing the burden on neighboring facilities.
The resulting “healthcare deserts” disproportionately affect vulnerable populations.
Role of Reimbursement Models in the Financial Stability of Rural Hospitals
The current healthcare reimbursement models play a critical role in the financial stability (or instability) of rural hospitals. Traditional fee-for-service models, where hospitals are reimbursed for each service provided, often fail to adequately compensate for the complexities of rural healthcare delivery. The shift towards value-based care models, which emphasize quality and efficiency, presents both opportunities and challenges. While value-based models can incentivize cost-effective care, rural hospitals may lack the resources and infrastructure to effectively participate in these programs.
Furthermore, the complexity of these models and the administrative burden they impose can place a strain on already limited staff and resources.
Examples of Rural Hospitals Facing Closure and Reasons Behind Their Struggles
Many rural hospitals are struggling to remain financially viable, and numerous closures have already occurred. The reasons are multifaceted and often interconnected. Here are a few examples:
| Hospital Name | Location | Reason for Financial Distress | Current Status |
|---|---|---|---|
| [Hospital Name 1 – Replace with actual hospital name] | [State, County – Replace with actual location] | [e.g., Low patient volume, high uncompensated care, low reimbursement rates] | [e.g., Closed, bankrupt, acquired by larger system] |
| [Hospital Name 2 – Replace with actual hospital name] | [State, County – Replace with actual location] | [e.g., Declining population, difficulty recruiting physicians, outdated facilities] | [e.g., Closed, bankrupt, acquired by larger system] |
| [Hospital Name 3 – Replace with actual hospital name] | [State, County – Replace with actual location] | [e.g., High operating costs, low reimbursement from Medicare/Medicaid, competition from larger urban hospitals] | [e.g., Closed, bankrupt, acquired by larger system] |
The Impact of Healthcare Quality Payment Reform: Hundreds Rural Hospitals Risk Closing Center Healthcare Quality Payment Reform
The shift towards value-based care through healthcare quality payment reform presents significant challenges for rural hospitals, often exacerbating existing vulnerabilities. These reforms, while aiming to improve overall healthcare quality and efficiency, frequently overlook the unique circumstances and resource limitations faced by rural providers. The result is a disproportionate impact, threatening the financial stability and even the survival of many rural healthcare facilities.
Disproportionate Effects of Quality Payment Reform on Rural Hospitals
Rural hospitals face several unique obstacles in adapting to the requirements of quality payment reform programs like the Merit-Based Incentive Payment System (MIPS) and value-based purchasing models. These programs often prioritize metrics heavily reliant on access to advanced technology, specialized staff, and robust data infrastructure – resources often scarce in rural settings. The focus on population health management, another key component of these reforms, is also challenging in rural areas with dispersed populations and limited transportation options.
Furthermore, the smaller patient volumes common in rural hospitals make it difficult to achieve the statistical power needed to demonstrate significant improvements in quality metrics, hindering their ability to earn positive payment adjustments.
Challenges in Meeting Reform Requirements
Meeting the requirements of quality payment reform presents a multifaceted challenge for rural hospitals. Firstly, the technological infrastructure needed for data collection, analysis, and reporting is often lacking. Many rural hospitals struggle with outdated electronic health record (EHR) systems and lack the dedicated IT staff needed to manage the complex data requirements of these programs. Secondly, recruiting and retaining qualified staff, particularly specialists needed for certain quality metrics, is a major hurdle.
Rural areas often face shortages of physicians, nurses, and other healthcare professionals, making it difficult to build the teams necessary for effective quality improvement initiatives. Thirdly, the financial resources available to rural hospitals are often limited, making it difficult to invest in the necessary technology, training, and personnel to meet these requirements.
Resource Disparities Between Urban and Rural Hospitals
A significant disparity exists between urban and rural hospitals in terms of resources available to meet quality payment reform requirements. Urban hospitals generally have greater access to capital, technology, and specialized personnel. They often have larger IT departments, dedicated quality improvement teams, and established relationships with technology vendors. These resources allow them to more easily invest in the necessary infrastructure and expertise to meet the demands of these reforms.
In contrast, rural hospitals often operate with tighter budgets, limited staff, and less access to cutting-edge technology. This resource imbalance creates an uneven playing field, placing rural hospitals at a significant disadvantage.
Administrative Burden on Rural Hospitals
The administrative burden imposed by quality payment reform is particularly heavy for rural hospitals. The complex reporting requirements, coupled with the need to track numerous quality metrics, place a significant strain on already limited administrative staff. This administrative burden diverts resources away from direct patient care and can lead to increased operational costs. The smaller size of rural hospitals means that even a small increase in administrative workload can have a disproportionate impact on their overall operations.
The complexity of navigating various reporting systems and understanding the nuances of different payment models adds to the burden.
Hypothetical Case Study: Impact on a Rural Hospital’s Budget
Consider a small rural hospital with 25 beds serving a population of 10,000. Let’s assume that implementing the necessary technology and training to meet MIPS requirements costs $50,000 annually. This represents a significant portion of their already limited budget, potentially requiring cuts to other essential services or increased reliance on debt. Furthermore, if the hospital fails to meet the performance targets set by MIPS, it could face payment reductions, further impacting its financial stability.
This scenario illustrates how quality payment reform, while well-intentioned, can have a devastating financial impact on rural hospitals, potentially leading to service reductions or closure.
Potential Solutions and Mitigation Strategies
The looming crisis of rural hospital closures demands immediate and comprehensive action. Simply throwing money at the problem won’t suffice; we need innovative, sustainable solutions that address the root causes of rural healthcare’s financial instability. This requires a multi-pronged approach involving policy changes, innovative care models, and a renewed focus on leveraging technology.Policy changes are crucial for alleviating the financial burden on rural hospitals.
Current reimbursement models often disadvantage rural providers, who frequently serve sicker, poorer populations with limited resources. These disparities must be addressed through fairer reimbursement rates that reflect the higher costs and unique challenges of rural healthcare delivery. Furthermore, streamlining administrative burdens and reducing regulatory complexity can free up valuable resources for direct patient care.
Policy Changes to Support Rural Hospitals
Increased federal and state funding specifically allocated for rural hospitals is essential. This funding should be targeted towards infrastructure improvements, recruitment and retention of healthcare professionals, and the implementation of innovative care delivery models. Examples of successful interventions include the establishment of rural health clinics and critical access hospitals, which offer increased flexibility in reimbursement and regulatory requirements.
Furthermore, exploring alternative payment models, such as value-based care, can incentivize efficiency and quality improvement while reducing the reliance on fee-for-service reimbursements. These models could reward hospitals for positive patient outcomes rather than simply the volume of services provided. This shift in focus could incentivize preventative care and reduce overall healthcare costs.
Successful Interventions in Other Regions
The state of Vermont’s innovative approach to rural healthcare serves as a strong example. Their focus on creating regional healthcare networks, integrating telehealth services, and strengthening primary care has helped improve access to care and reduce costs. Similarly, initiatives in states like North Carolina and Montana have seen success through partnerships between rural hospitals and larger healthcare systems, sharing resources and expertise to improve efficiency and sustainability.
These collaborative models offer a promising pathway for other regions to emulate.
Innovative Models of Care Delivery
Telehealth offers a powerful tool to improve access to specialized care and reduce costs in rural areas. Remote monitoring of chronic conditions, virtual consultations with specialists, and telehealth-enabled mental health services can significantly reduce the need for costly travel and hospital admissions. For example, a rural hospital in Montana implemented a telehealth program for stroke patients, enabling rapid access to neurologists and reducing the need for costly transfers to urban centers.
The integration of telehealth with other innovative models, such as mobile health clinics and community health worker programs, can further enhance access to care and improve health outcomes in rural communities. Additionally, exploring the expansion of community paramedicine programs could reduce emergency room visits and hospital admissions, thereby saving costs and improving patient care.
Actionable Steps for Policymakers
Policymakers can take several concrete steps to prevent rural hospital closures:
- Increase federal and state funding for rural hospitals.
- Reform reimbursement models to better reflect the costs of rural healthcare.
- Streamline administrative burdens and reduce regulatory complexity.
- Invest in telehealth infrastructure and training.
- Support the development of regional healthcare networks and collaborative partnerships.
- Incentivize the recruitment and retention of healthcare professionals in rural areas through loan forgiveness programs and other incentives.
- Promote the adoption of innovative care delivery models, such as value-based care and community paramedicine.
The Role of Telehealth in Rural Healthcare
Telehealth’s potential to transform rural healthcare is immense. By connecting patients with specialists and providing remote monitoring capabilities, telehealth can bridge geographical barriers and improve access to timely, high-quality care. This not only improves health outcomes but also reduces the need for expensive travel and hospital admissions, leading to significant cost savings for both patients and healthcare systems.
For example, a telehealth program connecting rural patients with cardiologists has shown a significant reduction in hospital readmissions for heart failure. This illustrates the potential of telehealth to enhance the efficiency and sustainability of rural healthcare systems.
The Impact on Patient Care and Access

Source: henrykotula.com
The looming closure of hundreds of rural hospitals across the nation presents a grave threat to the health and well-being of millions. The impact extends far beyond the immediate loss of jobs and services; it fundamentally alters the landscape of healthcare access and profoundly affects the lives of rural residents. This section will explore the devastating consequences of these closures on patient care and access to essential medical services.The potential consequences of widespread rural hospital closures are far-reaching and deeply concerning.
It’s scary to think about hundreds of rural hospitals facing closure due to the healthcare quality payment reform. This isn’t just a rural problem; we’re seeing similar struggles with larger systems, like the recent news about Steward Health Care’s Ohio hospital closures and a Pennsylvania facility at risk, as reported in this article: steward ohio hospitals closures pennsylvania facility at risk.
The financial pressures impacting these larger systems highlight the systemic issues contributing to the rural hospital crisis, making access to care even more precarious.
Reduced access to timely and appropriate care is the most immediate and significant impact. This lack of access disproportionately affects vulnerable populations, exacerbating existing health disparities.
Reduced Access to Care
The closure of rural hospitals forces patients to travel significantly longer distances to reach the nearest alternative healthcare facility. This increased travel time translates to delayed or forgone care, particularly for time-sensitive conditions like heart attacks or strokes. The burden falls heavily on the elderly, individuals with disabilities, and those lacking reliable transportation. For example, a patient living 50 miles from the nearest hospital might face a two-hour round trip, potentially delaying critical treatment and worsening their prognosis.
This scenario is replicated across numerous rural communities facing hospital closures.
The news about hundreds of rural hospitals risking closure due to the Center for Medicare & Medicaid Services’ (CMS) quality payment reforms is truly alarming. It highlights the precarious financial state of many healthcare providers, a situation mirrored by larger systems like Steward Health Care, which recently secured financing to emerge from bankruptcy as reported in this article: steward health care secures financing bankruptcy.
This bankruptcy, while seemingly separate, underscores the systemic challenges facing healthcare in the US, further jeopardizing those already struggling rural hospitals.
Impact on Health Outcomes
Reduced access to preventative care and specialized services directly impacts health outcomes in rural communities. Delayed diagnoses, lack of ongoing monitoring, and limited access to specialists lead to poorer health outcomes and higher mortality rates. This is especially true for chronic conditions like diabetes, heart disease, and cancer, which require regular check-ups and specialized treatments. For instance, a rural resident with diabetes might miss crucial appointments for blood glucose monitoring, leading to uncontrolled blood sugar levels and potentially serious complications.
Increased Travel Distances and Costs
The increased travel distances associated with rural hospital closures impose significant financial burdens on patients. The costs of transportation, including fuel, tolls, and potentially overnight accommodations, can be prohibitive for many rural residents, particularly those with limited incomes. These additional expenses can force individuals to forgo necessary care, leading to a vicious cycle of worsening health and increased financial strain.
Imagine a family already struggling financially having to travel hundreds of miles for specialized care, incurring substantial travel and lodging expenses, further jeopardizing their economic stability.
Social and Economic Consequences
The loss of local healthcare services has profound social and economic consequences for rural communities. Hospitals are often major employers, and their closure leads to job losses and economic decline. Furthermore, the closure of hospitals can negatively impact the value of homes and properties in the area, hindering economic development and potentially triggering a downward spiral. The social fabric of the community can also be damaged, as local healthcare professionals leave, resulting in the loss of social support networks and a sense of community cohesion.
For example, the closure of a small rural hospital might lead to the departure of several doctors and nurses, impacting not only healthcare provision but also the overall vitality of the town.
| Consequence | Description | Affected Population | Mitigation Strategy |
|---|---|---|---|
| Reduced Access to Care | Longer travel times to reach alternative healthcare facilities, leading to delayed or forgone care. | Elderly, individuals with disabilities, those lacking reliable transportation, and those with time-sensitive conditions. | Increased telehealth services, mobile health clinics, and transportation assistance programs. |
| Negative Impact on Health Outcomes | Delayed diagnoses, lack of ongoing monitoring, and limited access to specialists leading to poorer health outcomes and higher mortality rates. | Individuals with chronic conditions requiring regular check-ups and specialized treatments. | Improved access to preventative care, telehealth consultations with specialists, and community-based health programs. |
| Increased Travel Distances and Costs | Higher transportation costs, including fuel, tolls, and potentially overnight accommodations, placing a financial burden on patients. | Low-income individuals and families in rural areas. | Financial assistance programs for transportation, subsidies for medical travel, and expanded telehealth options to reduce the need for travel. |
| Social and Economic Consequences | Job losses, economic decline, decreased property values, and disruption of social support networks. | Rural communities and their residents, healthcare workers, and local businesses. | Investment in rural healthcare infrastructure, job creation initiatives, and community-based economic development strategies. |
Long-Term Sustainability of Rural Healthcare

Source: umn.edu
The current crisis facing rural hospitals isn’t just about immediate closures; it’s about the long-term viability of healthcare access in vast swathes of the country. The trends we’re seeing – declining populations, aging infrastructure, and unsustainable reimbursement models – paint a concerning picture for the future of rural healthcare, impacting not only the hospitals themselves but also the well-being of entire communities.
Understanding these long-term implications is crucial for developing effective solutions.The future viability of rural hospitals hinges on a complex interplay of factors. Simply throwing money at the problem won’t suffice; a multifaceted approach is required, addressing economic realities, technological advancements, and the evolving needs of rural populations. Ignoring these interconnected factors will only accelerate the decline.
It’s scary to think about hundreds of rural hospitals potentially closing due to the complexities of the Center for Medicare & Medicaid Services’ Quality Payment Program. The news that HSHS Prevea is closing some Wisconsin hospitals and health centers, as reported here: hshs prevea close wisconsin hospitals health centers , highlights the financial pressures facing healthcare providers nationwide.
This only underscores the urgency of addressing the issues driving rural hospital closures before more communities lose access to vital care.
Key Factors Determining Rural Hospital Viability
Several key elements will determine whether rural hospitals can survive and thrive in the coming years. These include sustainable funding models that account for the unique challenges of serving geographically dispersed populations, the adoption of innovative telehealth technologies to bridge geographical barriers and improve access to specialist care, the recruitment and retention of healthcare professionals willing to work in rural settings, and the development of strong partnerships with other healthcare providers and community organizations.
Failure to address any one of these will significantly weaken the overall system.
Interconnected Factors Contributing to Rural Hospital Closures: A Visual Representation, Hundreds rural hospitals risk closing center healthcare quality payment reform
Imagine a central circle labeled “Rural Hospital Closure.” Radiating outwards from this central circle are several interconnected circles, each representing a contributing factor. These include: “Declining Rural Population” connected to “Reduced Patient Volume”; “Aging Infrastructure” connected to “High Capital Costs”; “Inadequate Reimbursement Rates” connected to “Financial Unsustainability”; “Physician Shortage” connected to “Limited Access to Care”; and “Lack of Telehealth Infrastructure” connected to “Inefficient Care Delivery.” Lines connect these circles to show their interdependence.
For instance, a declining rural population directly leads to reduced patient volume, exacerbating financial unsustainability. Similarly, inadequate reimbursement rates and a physician shortage are mutually reinforcing factors contributing to hospital closure. The visual representation emphasizes the cascading effect of these interconnected challenges.
Successful Adaptation Strategies in Rural Healthcare
Several rural hospitals have successfully adapted to the changing healthcare landscape. For example, some have embraced telehealth technologies, offering remote consultations and monitoring, thus expanding their reach and reducing the need for patients to travel long distances. Others have formed collaborative partnerships with larger healthcare systems, sharing resources and expertise to improve efficiency and financial stability. Some have focused on niche services, specializing in areas where they can attract patients from a wider region, such as specialized geriatric care or trauma services.
These examples demonstrate that proactive adaptation, rather than simply reacting to challenges, is key to long-term sustainability. The success of these strategies highlights the importance of innovation, collaboration, and a focus on meeting the specific needs of rural communities.
Closing Summary
The looming closure of hundreds of rural hospitals is a critical issue demanding immediate attention. While the challenges are significant, the situation isn’t hopeless. Through innovative care delivery models, targeted policy changes, and a renewed focus on supporting rural healthcare systems, we can avert this crisis. The future of rural healthcare depends on our collective commitment to finding sustainable solutions that ensure access to quality care for everyone, regardless of their location.
It’s time to move beyond simply acknowledging the problem and actively work towards a future where rural communities thrive, with healthcare access at the forefront.
Query Resolution
What specific aspects of healthcare quality payment reform are most challenging for rural hospitals?
Rural hospitals often struggle with the data reporting and technology requirements, lacking the resources of their urban counterparts. They may also find it difficult to meet certain quality metrics due to limited specialist access and smaller patient populations.
Are there any successful examples of rural hospitals adapting to these challenges?
Yes, some rural hospitals have successfully implemented telehealth programs to expand access to care and reduce costs. Others are forging partnerships with larger healthcare systems to share resources and expertise.
What role does the government play in addressing this issue?
The government can play a crucial role through policy changes, increased funding for rural healthcare, and initiatives to support the adoption of innovative care models. Targeted financial incentives can also encourage investment in rural healthcare infrastructure and technology.