Provider Groups, MedPACs Proposed Payment Rate AHA AMA
Provider groups medpacs proposed payment rate AHA AMA – Provider Groups, MedPAC’s proposed payment rate: AHA AMA – this is a hot topic shaking up the healthcare world! MedPAC, the Medicare Payment Advisory Commission, recently released their proposed payment rates for various healthcare providers. This has sent ripples through the industry, with the American Hospital Association (AHA) and the American Medical Association (AMA) weighing in with their own perspectives.
The potential impact on access to care, quality of services, and the overall financial health of provider groups is significant, making this a debate we need to understand.
This post will delve into the specifics of MedPAC’s proposals, examining the different provider groups affected, analyzing the AHA and AMA’s responses, and exploring the potential consequences for patients and the healthcare system as a whole. We’ll also look at alternative payment models and the evidence behind MedPAC’s recommendations.
Provider Groups and MedPAC’s Role
The proposed Medicare payment rates, as recommended by the Medicare Payment Advisory Commission (MedPAC), significantly impact various healthcare provider groups. Understanding MedPAC’s role and the diverse responses from different provider types is crucial for navigating the complexities of the healthcare financing landscape. This discussion will delve into the specific effects on various provider groups and analyze MedPAC’s historical influence on Medicare payment policy.MedPAC’s influence on Medicare payment policies is substantial.
Established by Congress in 1997, MedPAC provides independent advice to Congress on Medicare payment policy. Their recommendations, while not binding, often carry significant weight in shaping legislation. Their analyses consider various factors including the costs of care, quality of care, and the financial viability of different provider types. Over the years, MedPAC’s reports have led to significant changes in how Medicare reimburses providers, influencing everything from physician payments to hospital reimbursements.
MedPAC’s Historical Involvement in Shaping Medicare Payment Policies
MedPAC’s history is marked by a consistent effort to balance the needs of beneficiaries with the financial sustainability of the Medicare program. Their recommendations have often involved adjustments to payment rates, aiming to control costs while maintaining the quality of care. For example, MedPAC has advocated for value-based payment models, shifting reimbursement from a fee-for-service model to one that rewards quality and efficiency.
They have also played a key role in analyzing and recommending adjustments to the sustainable growth rate (SGR) formula, a complex calculation that historically determined physician payments under Medicare. While the SGR was ultimately repealed, MedPAC’s analysis of its flaws contributed significantly to that outcome. The commission continues to actively monitor the impact of payment reforms and provide recommendations for improvements.
The debate around provider groups and MedPAC’s proposed payment rates, involving the AHA and AMA, is intense. A key factor influencing these discussions is the escalating cost of Medicare, particularly concerning GLP-1 medications, as highlighted in this insightful KFF report: medicare glp1 spending weight loss kff. Understanding these rising drug costs is crucial for shaping fair and sustainable payment models for providers, ultimately impacting the final MedPAC recommendations.
Comparison of MedPAC’s Proposed Payment Rates to Previous Years
Comparing MedPAC’s proposed payment rates to those of previous years reveals trends and informs potential impacts. While specific numbers vary annually based on economic factors and analyses of healthcare costs, a consistent theme is the effort to balance cost containment with provider viability. For instance, a year with significant increases in healthcare inflation might see a recommendation for higher payment rates to avoid significant financial strain on providers.
Conversely, a year with relatively stable costs might see a recommendation for lower increases or even decreases in payment rates. Detailed analysis of the historical data, including the justifications provided by MedPAC in their annual reports, is necessary to understand the rationale behind each year’s recommendations.
Characteristics of Different Provider Groups and Potential Responses to Proposed Rate Changes, Provider groups medpacs proposed payment rate AHA AMA
The impact of MedPAC’s proposed payment rates varies significantly depending on the type and size of the provider group.
| Provider Group Type | Size | Geographic Location | Potential Impact of Rate Changes |
|---|---|---|---|
| Large Hospital Systems | Multiple hospitals, extensive network | Urban, Suburban | May absorb rate decreases through cost-cutting measures; may lobby for adjustments. Larger systems generally have more financial flexibility. |
| Small Rural Hospitals | Single hospital, limited resources | Rural, Underserved areas | Rate decreases could severely impact financial stability; potential for closures or service reductions. |
| Large Physician Groups | Numerous physicians, extensive administrative support | Urban, Suburban | May adjust staffing or services; may negotiate contracts differently. Larger groups have greater negotiating power. |
| Solo/Small Physician Practices | Single physician or small number of physicians, limited resources | Rural, Suburban, Urban | Rate decreases could significantly impact profitability; potential for practice closures or mergers. |
AHA and AMA Perspectives on Proposed Rates

Source: slideplayer.com
The proposed Medicare payment rates for providers are a contentious issue, sparking significant debate between key stakeholders. Understanding the perspectives of the American Hospital Association (AHA) and the American Medical Association (AMA) is crucial to grasping the complexities surrounding these adjustments. Both organizations represent significant portions of the healthcare industry, and their positions reflect the potential impact on hospitals and physician practices nationwide.
AHA’s Stance on Proposed Payment Rates
The AHA consistently argues that proposed Medicare payment rate cuts are unsustainable for hospitals, particularly those serving vulnerable populations. They contend that these cuts fail to adequately account for the rising costs of providing care, including labor, supplies, and technology. The AHA emphasizes that hospitals operate on thin margins and that further reductions could jeopardize access to care, forcing closures or service reductions, especially in rural and underserved communities.
They often cite data showing the increasing financial strain on hospitals due to factors like inflation and understaffing, illustrating the detrimental effects of proposed cuts. For example, they might highlight a specific study showing the correlation between Medicare reimbursement rates and hospital closure rates in certain regions.
AMA’s Perspective on Proposed Payment Rates
The AMA shares concerns regarding the proposed payment rates, focusing on their potential impact on physician practices. They argue that inadequate reimbursement jeopardizes the financial viability of physician practices, potentially leading to physician burnout, shortages, and reduced access to care, particularly in specialty areas. The AMA highlights the administrative burden placed on physicians by complex billing and coding systems, further impacting their profitability.
They often advocate for adjustments to reflect the true cost of providing care, considering factors like inflation and the increasing complexity of medical procedures. They might use examples of specific specialties facing particularly severe reimbursement challenges, demonstrating the potential for reduced access to care in those areas.
Comparison of AHA and AMA Arguments
Both the AHA and AMA fundamentally agree that the proposed rates are inadequate and threaten access to care. However, their arguments emphasize different aspects of the healthcare system. The AHA focuses on the macro-level impact on hospitals, including potential closures and service reductions. The AMA, on the other hand, emphasizes the micro-level impact on individual physician practices and the potential for physician burnout and shortages.
While both organizations advocate for increased reimbursement, their approaches to advocating for change might differ based on their specific priorities and membership.
Hypothetical Scenario Illustrating Impact of Proposed Rates
Consider a rural hospital serving a large elderly population. The proposed Medicare payment rate cuts could result in a significant reduction in their annual revenue, potentially exceeding $1 million. This loss could force the hospital to reduce services, such as cutting back on elective procedures or reducing staffing levels. Simultaneously, the local physician practices, already struggling with low reimbursement rates, might experience further financial strain.
This could lead to physician burnout, potentially forcing some to retire early or relocate to areas with better reimbursement rates. The net effect would be reduced access to care for the vulnerable population served by this hospital and its associated physician practices, highlighting the potential consequences of insufficient Medicare reimbursement.
Impact of Proposed Rates on Healthcare Access and Quality
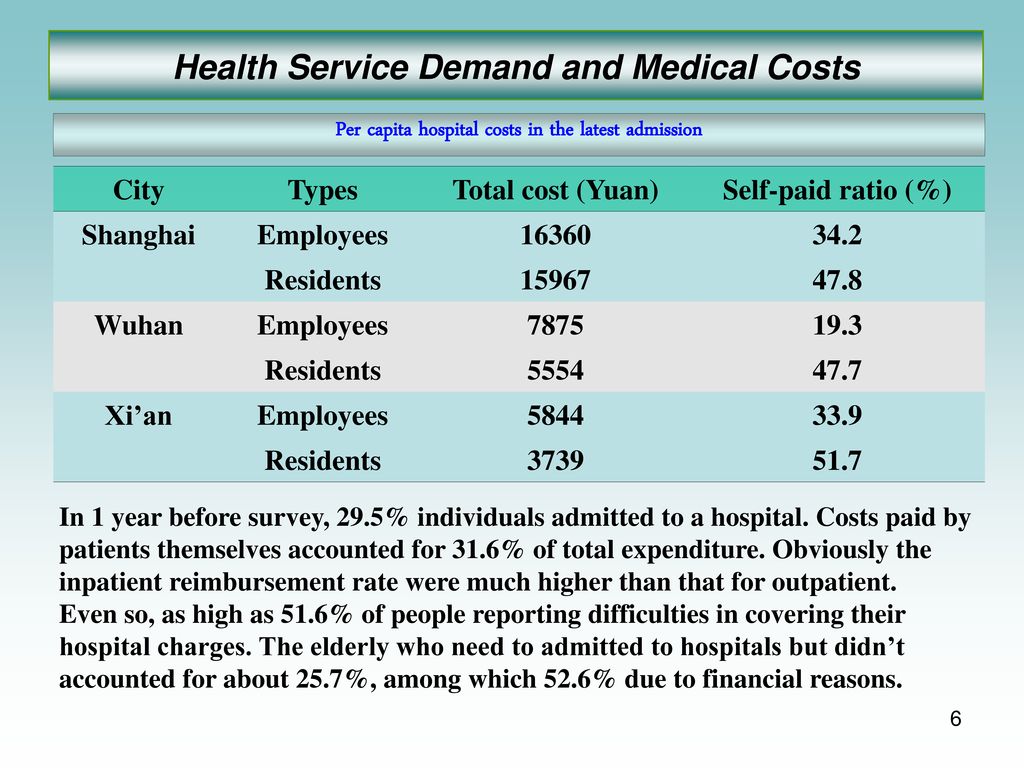
Source: slideplayer.com
The proposed Medicare payment rates, as suggested by MedPAC and considered by the AHA and AMA, have significant implications for the accessibility and quality of healthcare services for Medicare beneficiaries. These changes, whether they involve increases or decreases in reimbursement, ripple through the healthcare system, impacting providers, patients, and the overall efficiency of care delivery. Understanding these potential effects is crucial for policymakers and stakeholders alike.
Potential Effects on Access to Care
Proposed rate adjustments directly influence the financial viability of healthcare providers, particularly those heavily reliant on Medicare reimbursement. Reductions in payment rates could force providers, especially those in rural or underserved areas with already thin margins, to reduce services, limit patient acceptance, or even close their doors. This would undeniably restrict access to care for vulnerable populations who rely on Medicare.
Conversely, increases in rates might incentivize expansion of services, but could also lead to increased costs for the Medicare program. For example, a significant decrease in reimbursement for rural hospitals could lead to the closure of emergency rooms or the elimination of specific specialized services, forcing patients to travel long distances for essential care, potentially impacting timely access to treatment and worsening health outcomes.
Influence on Quality of Care
The quality of care isn’t solely determined by access; it also depends on the resources available to providers. Decreased reimbursement could lead to staff reductions, limiting the time physicians can spend with patients, reducing the availability of advanced diagnostic equipment, and potentially hindering the implementation of innovative treatment approaches. This could translate into a decline in the overall quality of care.
Conversely, appropriate increases in reimbursement could enable investments in technology, staff training, and improved infrastructure, potentially enhancing the quality of care provided. For instance, reduced funding for preventative care programs due to lower reimbursement rates could lead to a rise in more expensive hospitalizations later on.
Potential Unintended Consequences
Implementing proposed payment rates carries the risk of unforeseen repercussions. For example, a drastic reduction in reimbursement for specific procedures might incentivize providers to focus on higher-paying services, potentially leading to an imbalance in the types of care available. This could disproportionately affect patients requiring less profitable, yet essential, services. Similarly, an increase in reimbursement for certain services might lead to an increase in demand and potentially unnecessary utilization of those services, driving up overall healthcare costs.
A real-life example of this is the potential overutilization of certain diagnostic tests due to higher reimbursement rates, leading to increased costs without necessarily improving patient outcomes.
Categorization of Potential Impacts
The impacts of proposed payment rates can be broadly categorized as follows:
- Financial Impacts: These include changes in provider revenue, profitability, and the overall financial stability of healthcare organizations. Reduced reimbursement can lead to financial strain, impacting providers’ ability to invest in infrastructure and staff. Increased reimbursement might alleviate financial pressure but could also lead to increased costs for the Medicare program.
- Operational Impacts: These include changes in service offerings, staffing levels, and the efficiency of healthcare operations. Lower reimbursement could lead to service reductions, staff layoffs, and longer wait times. Increased reimbursement might allow for service expansion but could also lead to increased administrative burdens.
- Patient-Related Impacts: These include changes in access to care, quality of care received, and patient satisfaction. Reduced reimbursement could limit access to care, impacting patient outcomes and satisfaction. Increased reimbursement could improve access and quality but might also lead to increased costs for patients through higher premiums or cost-sharing.
Alternative Payment Models and Their Relevance: Provider Groups Medpacs Proposed Payment Rate AHA AMA

Source: slideplayer.com
The proposed Medicare payment rates are not operating in a vacuum; they interact significantly with the evolving landscape of alternative payment models (APMs). Understanding these models and their potential interplay with the proposed rates is crucial for predicting their impact on healthcare providers and the overall system. This section will explore several key APMs and analyze their relationship with the proposed reimbursement changes.
Several alternative payment models are currently employed or under consideration by CMS, each aiming to shift reimbursement from fee-for-service to value-based care. This shift rewards providers for the quality of care delivered rather than the quantity of services provided. Comparing these models to the proposed rates allows for a more comprehensive understanding of their potential collective effects.
Accountable Care Organizations (ACOs)
ACOs are groups of doctors, hospitals, and other healthcare providers who come together to give coordinated high-quality care to their Medicare patients. The proposed payment rates could either support or hinder ACO success depending on their specific structure and negotiation power. For example, if the proposed rates are significantly lower than current fee-for-service rates, ACOs might find it more challenging to meet their financial targets, potentially discouraging participation.
The proposed payment rates from MedPac for provider groups, a topic hotly debated by the AHA and AMA, have me thinking about the bigger picture of healthcare access. News of HSHS Prevea closing Wisconsin hospitals and health centers, as reported in this article hshs prevea close wisconsin hospitals health centers , highlights the financial pressures facing healthcare systems.
This directly impacts the viability of those provider groups and ultimately influences the feasibility of the MedPac proposed rates.
Conversely, if the rates are set at a level that allows ACOs to maintain profitability while focusing on quality, it could encourage greater adoption. A hypothetical example: An ACO aiming for shared savings under a bundled payment model might struggle to achieve profitability if the bundled rate is significantly reduced by the proposed payment cuts, potentially leading to decreased patient access and quality compromises.
Bundled Payments
Bundled payments involve a single payment for an episode of care, encompassing multiple services. This model incentivizes efficiency and coordination, as providers share in the financial risk and reward. The proposed payment rates could impact bundled payments by influencing the overall amount paid for each episode. If the proposed rates decrease significantly, the bundled payment amount might also need adjustment to reflect the reduced reimbursement for individual services within the bundle.
A scenario: A hospital receiving a bundled payment for hip replacement surgery might see a reduction in its overall revenue if the individual payments for pre-operative consultations, surgery itself, and post-operative care are all lowered due to the proposed rate changes. This could potentially lead to hospitals negotiating higher bundled rates to compensate, or to reduce the services offered within the bundle.
Value-Based Purchasing (VBP)
VBP programs link payment to the quality of care provided. The proposed rates, if significantly reduced, could potentially conflict with VBP incentives. Providers might be less inclined to invest in quality improvement initiatives if their base reimbursement is already significantly lower. Conversely, a well-designed VBP program could mitigate the negative effects of reduced rates by rewarding providers who achieve superior outcomes, thus offsetting the reduced base payments.
For example, a hospital achieving high scores on patient satisfaction and readmission rates under a VBP program could receive performance-based bonuses that compensate for the lower payment rates for individual services. However, if the VBP bonuses are insufficient to cover the losses from reduced rates, it could still negatively impact hospital finances and potentially limit investments in quality improvement.
Patient-Centered Medical Homes (PCMHs)
PCMHs focus on providing comprehensive, coordinated care to patients. The proposed rates could influence the financial viability of PCMHs. Reduced payments for individual services could decrease the revenue generated by PCMHs, especially those relying heavily on fee-for-service. This might lead to decreased staffing levels or reduced access to services. Conversely, a well-managed PCMH that effectively coordinates care and reduces unnecessary services could mitigate the impact of lower rates through increased efficiency and cost savings.
For instance, a PCMH effectively managing chronic conditions could reduce hospital readmissions, leading to cost savings that offset lower reimbursement for individual visits.
Data and Evidence Supporting Proposed Rates
MedPAC’s proposed payment rates for providers are based on a complex analysis of various data sources and methodologies. Understanding the underpinnings of these proposals is crucial for stakeholders to assess their potential impact on the healthcare system. This section delves into the data and evidence used, highlighting both strengths and limitations.MedPAC’s justification for proposed payment rates relies heavily on analyzing Medicare spending data, specifically focusing on trends in physician services and hospital care.
They utilize extensive datasets encompassing claims information, provider demographics, and geographic variations in costs. This data allows them to identify areas where spending deviates significantly from national averages or established benchmarks. Furthermore, they incorporate data from other sources, including private payer claims data, to gain a broader perspective on national healthcare spending trends.
MedPAC’s Data Sources and Methodology
MedPAC’s analysis incorporates multiple data sources, including Medicare Part A and Part B claims data, which provides a comprehensive view of physician and hospital payments. They also leverage data from the Centers for Medicare & Medicaid Services (CMS) on provider costs and utilization rates. The methodology involves statistical modeling to account for factors such as geographic location, provider specialty, and patient characteristics, aiming to isolate the impact of payment rates on overall spending.
These models adjust for case mix differences, meaning they attempt to account for variations in patient illness severity, which could affect the cost of care. However, perfect adjustment is difficult to achieve, leading to some uncertainty in the results.
The proposed payment rate changes from provider groups like MedPAC are impacting healthcare, and understanding the financial implications is crucial for everyone. This reminds me of the challenges faced by families managing conditions like Tourette Syndrome, where consistent, quality care is paramount. For helpful resources on strategies to manage Tourette Syndrome in children, check out this informative article: strategies to manage Tourette syndrome in children.
Ultimately, navigating these complex healthcare issues, whether financial or clinical, requires a collaborative approach between payers, providers (like the AHA and AMA), and families.
Methodological Limitations and Uncertainties
While MedPAC employs sophisticated statistical techniques, inherent limitations exist. The accuracy of the models depends on the quality and completeness of the underlying data. Data inaccuracies or missing information can bias the results. Furthermore, predicting future costs and utilization patterns is inherently uncertain. Changes in medical technology, healthcare utilization patterns, and the adoption of alternative payment models can all affect the accuracy of MedPAC’s projections.
For example, the increasing use of telehealth may not be fully captured in their models, potentially leading to an underestimation or overestimation of future costs. Another challenge lies in accurately accounting for the complexities of physician practice variations and the influence of non-payment factors on costs.
MedPAC’s Rate Determination Process
MedPAC’s process begins with analyzing historical trends in Medicare spending. They then use their statistical models to project future spending under different payment scenarios. This involves considering the impact of various factors, including changes in physician supply, patient demographics, and technological advancements. They aim to balance the need to control costs with the need to maintain access to quality care.
Their recommendations are based on a complex interplay of cost containment goals, quality metrics, and the potential impact on provider incomes and healthcare access. The final proposed rates reflect a balance of these competing considerations, often involving adjustments and compromises.
Visual Representation of Key Data Points
A bar chart could effectively visualize key data points. The horizontal axis would represent different provider specialties (e.g., Cardiology, Oncology, Primary Care). The vertical axis would show the percentage change in proposed payment rates compared to the current rates. Each bar would represent a specific specialty, with its height corresponding to the percentage change. For example, a bar for Cardiology might show a 2% decrease, while a bar for Primary Care might show a 1% increase.
A key would indicate whether the change represents an increase or decrease. The chart would clearly illustrate the differential impact of the proposed rates across various specialties. Additional data points, such as the average Medicare spending per beneficiary for each specialty, could be added to the chart as supplementary information. This would provide a comprehensive view of the relationship between proposed rate changes and current Medicare spending.
Closing Summary
The proposed payment rates from MedPAC are a game-changer for healthcare providers. The differing opinions of the AHA and AMA highlight the complexities involved, with significant implications for access to care and the quality of services. Understanding the data behind these proposals, as well as exploring alternative payment models, is crucial for navigating this evolving landscape. Ultimately, the debate surrounding these rates underscores the need for a thoughtful and comprehensive approach to Medicare payment reform that balances the needs of providers with the well-being of patients.
FAQ Guide
What are the potential unintended consequences of these proposed rates?
Potential unintended consequences include provider consolidation, reduced access to care in underserved areas, and a shift towards less comprehensive services to maintain profitability.
How will these changes affect smaller physician practices?
Smaller practices may be disproportionately affected, potentially facing financial hardship and even closure if the proposed rates don’t adequately cover their costs.
What is MedPAC’s overall goal with these proposed payment adjustments?
MedPAC aims to ensure the long-term solvency of Medicare while striving to maintain quality care. Their proposed rates are intended to control costs and potentially incentivize the adoption of more efficient and effective care models.
What is the timeline for implementing these proposed rates?
The timeline depends on Congressional action. The proposals need to be reviewed and approved by lawmakers before implementation can begin.