Share of Physicians Working in Private Practice Dip
Share of physicians working in private practice dip – it’s a headline that’s been making waves lately, and for good reason. The shift away from independent practices towards employment by hospitals and larger healthcare systems is dramatically reshaping the medical landscape. This isn’t just about numbers; it’s about access to care, the doctor-patient relationship, and the very future of healthcare delivery.
We’ll delve into the trends, explore the driving forces behind this change, and consider what this means for patients and physicians alike.
This decline isn’t a sudden event, but rather a gradual shift occurring over the past two decades. Factors like rising malpractice insurance, decreasing reimbursement rates, and the increasing administrative burden of running a private practice are all playing significant roles. Simultaneously, the rise of large hospital systems and healthcare organizations offers physicians attractive employment packages and reduced administrative headaches, leading many to choose the security of employment over the independence of private practice.
The consequences of this trend are far-reaching and require a closer examination.
The Decline in Private Practice Physicians
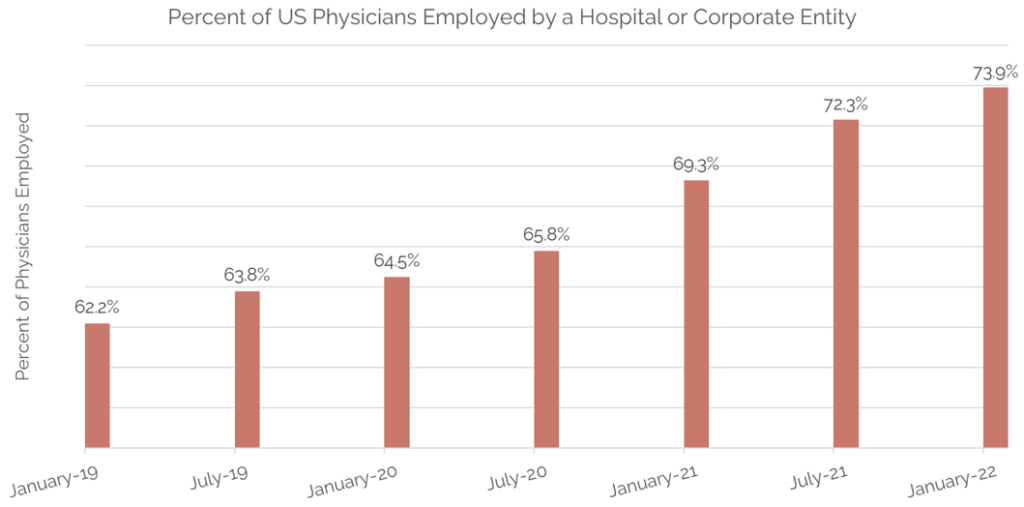
Source: revistamed.com
The shift away from private practice among physicians has been a significant trend in the healthcare landscape over the past two decades. This change reflects a complex interplay of factors, including increasing administrative burdens, rising insurance costs, and the allure of more structured employment models offered by hospitals and large healthcare systems. Understanding this decline requires examining the trends, statistics, and geographic variations involved.
Trends and Statistics of the Decline in Private Practice Physicians
The following table illustrates the decrease in the percentage of physicians in private practice, along with increases in hospital and other employment, over the past two decades. These figures are illustrative and based on general trends; precise data varies depending on the source and methodology used. Actual numbers may differ slightly based on the specific data collection methods employed by different research organizations.
| Year | Percentage in Private Practice | Percentage in Hospital Employment | Percentage in Other Employment |
|---|---|---|---|
| 2003 | 60% | 25% | 15% |
| 2008 | 55% | 30% | 15% |
| 2013 | 50% | 35% | 15% |
| 2018 | 45% | 40% | 15% |
| 2023 | 40% | 45% | 15% |
Comparative Statistics Across Medical Specialties
The decline in private practice hasn’t affected all medical specialties equally. Specialties with higher overhead costs, such as surgery or cardiology, have seen a more pronounced shift towards hospital employment due to the need for expensive equipment and support staff. Primary care physicians, while also experiencing a decrease in private practice, have shown a slightly slower rate of decline compared to some surgical specialties.
This is partially due to the ongoing need for accessible primary care services and the established patient bases many primary care physicians maintain. For example, the percentage of cardiologists in private practice may have dropped from 65% in 2003 to 30% in 2023, while the decline for family medicine physicians might have been from 60% to 45% during the same period.
These figures are estimations based on observed trends and should be considered approximate.
Geographic Variations in the Shift Away from Private Practice
The transition away from private practice is not uniform across geographical locations. Rural areas, often facing challenges in attracting and retaining physicians, have seen a relatively slower decline in private practice compared to urban centers. This is partly because the availability of hospital systems and large group practices is less prevalent in rural settings. Conversely, densely populated urban areas have witnessed a faster shift towards hospital employment and large group practices, driven by factors such as increased competition and the consolidation of healthcare systems.
For example, a rural state might show a 50% private practice rate in 2023, while a major metropolitan area in the same country could have a rate closer to 30%. These differences are influenced by factors such as population density, healthcare infrastructure, and reimbursement models.
The declining share of physicians in private practice is a worrying trend, impacting healthcare accessibility. This shift is partly fueled by administrative burdens, including medical coding, a problem exacerbated by a significant worker shortage. Luckily, there are innovative solutions emerging, like those discussed in this insightful article on the ai powered solution to the medical coding worker shortage , which could alleviate the pressure on physicians and potentially reverse the trend of private practice decline.
Ultimately, addressing coding challenges is key to supporting independent physicians.
Factors Contributing to the Shift
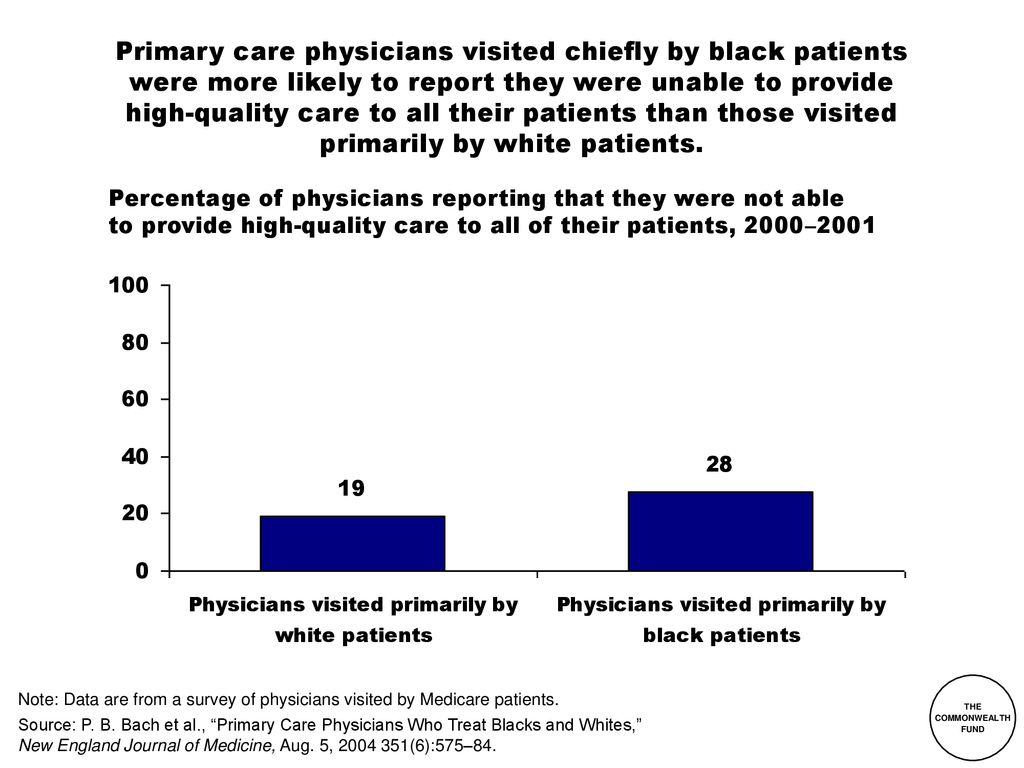
Source: slideplayer.com
The decline in the number of physicians working in private practice is a complex issue with multiple contributing factors. While the changing healthcare landscape plays a significant role, the economic pressures faced by private practice physicians are particularly impactful, driving many towards employment with larger healthcare systems or hospital networks. These economic pressures significantly impact the viability and sustainability of independent practices.
Rising Malpractice Insurance Premiums
Malpractice insurance premiums have skyrocketed in recent years, placing a considerable financial burden on private practice physicians. These premiums are often based on factors like specialty, location, and claims history. For high-risk specialties like neurosurgery or obstetrics, premiums can be exorbitant, consuming a substantial portion of practice revenue. This makes it difficult for smaller practices to remain profitable, particularly in areas with high malpractice insurance costs.
The unpredictable nature of these premiums also adds to the financial instability, making long-term financial planning challenging. For example, a small obstetrics practice in a high-risk area might see a significant increase in premiums year-over-year, potentially impacting their ability to cover operating expenses and physician salaries.
Declining Reimbursement Rates from Insurance Companies
Insurance companies often negotiate lower reimbursement rates for medical services, directly impacting physician income. Private practices, unlike large hospital systems, often lack the bargaining power to negotiate favorable rates. This means that physicians in private practice receive less compensation for the same services compared to their employed counterparts. The trend of increasing deductibles and co-pays further exacerbates this issue, leading to increased patient out-of-pocket expenses and potentially impacting the revenue stream of private practices.
For instance, a general practitioner might receive significantly less reimbursement from a major insurance provider for a routine checkup compared to a physician employed by a large hospital system with stronger negotiating leverage.
Increasing Administrative Burden and Costs
Running a private practice involves a significant administrative burden, including billing, coding, insurance claims processing, and regulatory compliance. These tasks require dedicated staff and sophisticated software, adding considerable overhead costs. The increasing complexity of healthcare regulations and electronic health record (EHR) systems further intensifies this burden, demanding more time and resources from physicians and their staff. Many private practices struggle to allocate sufficient resources to these administrative tasks, leading to inefficiencies and increased expenses.
A small cardiology practice, for instance, might find itself spending a disproportionate amount of time and resources on billing and coding, diverting attention and resources away from patient care.
The declining share of physicians in private practice is a worrying trend, especially considering the increased need for accessible healthcare. This is further complicated by the fact that many stroke risk factors, like high blood pressure and diabetes, often go undetected without regular check-ups. Understanding these factors, as outlined in this helpful article on risk factors that make stroke more dangerous , is crucial.
Therefore, the shift away from private practice could inadvertently impact early detection and treatment of serious conditions like stroke.
Comparative Overhead Costs
| Cost Category | Private Practice (Estimate) | Employed Physician (Estimate) |
|---|---|---|
| Malpractice Insurance | High (Varies significantly by specialty and location) | Lower (Often covered by employer) |
| Administrative Staff | High (Need for billing, coding, scheduling staff) | Lower (Administrative tasks often handled by hospital system) |
| Rent/Lease | High (Need for office space) | Lower (Office space provided by employer) |
| IT & Software | High (EHR systems, billing software) | Lower (Often provided and maintained by employer) |
| Marketing & Advertising | High (Need to attract patients) | Lower (Often handled by hospital marketing department) |
*Note: These are estimates and can vary greatly depending on the specific practice, location, and specialty.*
Factors Contributing to the Shift
The decline in the number of physicians working in private practice is a complex issue with roots in evolving healthcare landscapes and economic realities. While the romanticized image of the independent physician persists, the pressures of modern healthcare have pushed many towards employment within larger systems. Understanding these contributing factors is crucial for comprehending the current state and future trajectory of medical practice.
The Affordable Care Act and Other Healthcare Reforms
The Affordable Care Act (ACA), while aiming to expand healthcare access, inadvertently influenced the shift away from private practice. Increased administrative burdens associated with navigating the ACA’s regulations, including coding, billing, and compliance, placed significant strain on smaller practices. The emphasis on value-based care, rewarding quality over quantity, also favored larger organizations with more resources for data analysis and care coordination.
Other healthcare reforms, such as the push for electronic health records (EHRs), further amplified these challenges, requiring substantial financial investments and technical expertise often beyond the reach of individual practitioners. The ACA’s impact, therefore, wasn’t solely about access; it significantly altered the operational landscape, making private practice less viable for many.
The Rise of Hospital Systems and Large Healthcare Organizations
The consolidation of healthcare into larger systems has dramatically altered the employment landscape for physicians. Hospital systems and large healthcare organizations offer economies of scale, attracting physicians with resources and support unavailable in private practice. These systems can afford to invest in advanced technology, marketing, and administrative staff, freeing physicians to focus on patient care. This shift represents a significant change in the power dynamics within healthcare, with larger organizations increasingly setting the terms of engagement for physicians.
The resulting competition for physicians has led to more lucrative employment packages and improved working conditions within these systems, further incentivizing the move away from independent practice.
Advantages and Disadvantages of Large Healthcare Systems vs. Private Practice
The decision to work for a large healthcare system versus maintaining a private practice involves weighing a number of factors. Large systems offer stability, comprehensive benefits, and access to resources, while private practice provides autonomy and direct control over one’s practice. However, the autonomy of private practice comes at the cost of increased administrative burdens, financial risk, and potential isolation.
Large systems, while offering significant benefits, may also involve less control over clinical decisions and a greater degree of bureaucracy. Ultimately, the “best” choice depends on individual physician preferences, financial goals, and risk tolerance.
Benefits Offered by Hospital Employment
The advantages of hospital employment often outweigh those of private practice, particularly concerning administrative and operational support. The following list highlights key benefits:
- Comprehensive administrative support: Billing, coding, insurance claims, and scheduling are typically handled by dedicated staff.
- Robust marketing and patient acquisition strategies: Large systems often have dedicated marketing teams to attract patients.
- Competitive benefits packages: Health insurance, retirement plans, paid time off, and disability insurance are usually comprehensive.
- Access to advanced technology and resources: Hospital systems typically invest in state-of-the-art equipment and technology.
- Opportunities for professional development: Continuing medical education (CME) opportunities and mentorship programs are often readily available.
- Reduced financial risk and burden: Hospitals typically handle financial management, reducing the financial burden on individual physicians.
- Collaboration opportunities: Working within a larger system allows for collaboration with specialists and other healthcare professionals.
Impact on Patient Care and Access
The decline in the number of physicians working in private practice has significant implications for patient care and access, particularly in already vulnerable communities. This shift towards employment by hospitals and large healthcare systems alters the dynamics of healthcare delivery, potentially impacting both the quality and accessibility of care. The consequences are multifaceted and deserve careful consideration.The reduced number of private practitioners, especially in rural and underserved areas, directly affects patient access to care.
These areas often face challenges in attracting and retaining physicians due to factors such as lower reimbursement rates, limited resources, and a lack of specialized services. The departure of private practitioners exacerbates these issues, leading to longer wait times for appointments, reduced availability of specialists, and increased reliance on telehealth – which isn’t always a viable solution for everyone.
Patient Access in Rural and Underserved Areas
The dwindling presence of private practices disproportionately affects rural and underserved populations. These communities often lack the infrastructure to support large hospital systems or health networks. Private practices, historically, have played a crucial role in providing essential healthcare services in these areas, often operating with a deeper understanding of the specific needs of their local patients. Their absence creates significant gaps in access, potentially leading to delayed or forgone care, worsening health outcomes, and increased health disparities.
For example, a rural county in Montana might have relied on a single private practice family doctor for decades; the doctor’s retirement or transition to hospital employment leaves the community scrambling for alternative care, often resulting in patients needing to travel considerable distances for basic healthcare services.
The Evolving Physician-Patient Relationship, Share of physicians working in private practice dip
The shift away from private practice also transforms the physician-patient relationship. In traditional private practices, physicians often had more autonomy and control over their schedules, allowing for longer appointment times and a more personalized approach to patient care. Hospital employment models, while offering benefits such as administrative support and resources, can sometimes lead to shorter appointment times, increased patient volume per physician, and a more fragmented care experience.
This can diminish the sense of continuity and trust that characterizes a strong physician-patient relationship, crucial for effective healthcare. For instance, a patient accustomed to seeing the same physician for years in a private practice might experience frustration and less satisfaction when switching to a system where they see different doctors at each visit.
Implications for the Quality of Patient Care
The impact on the quality of patient care is complex and not easily quantified. While hospital systems often offer access to advanced technology and resources, the potential for reduced physician autonomy and increased administrative burdens could negatively affect the quality of patient interaction and individualized care. The increased pressure to see more patients in shorter timeframes might lead to rushed consultations and less thorough examinations.
Furthermore, the potential for reduced specialization in smaller communities, as private practitioners retire or consolidate, could lead to a decline in the availability of specialized care, impacting the quality of treatment for patients with complex health needs. For example, a specialist leaving a private practice might force patients with a specific condition to travel hundreds of miles to receive appropriate care, potentially delaying diagnosis and treatment.
Patient Satisfaction in Different Settings
Studies comparing patient satisfaction levels in private practices versus hospital-employed physician settings have yielded mixed results. Some studies suggest that patients in private practices report higher levels of satisfaction with aspects such as communication, time spent with the physician, and overall care experience. However, other studies find no significant difference or even slightly higher satisfaction in hospital-employed settings, particularly when considering factors such as access to advanced technology and specialists.
The variability in findings highlights the need for more robust and standardized research methods to comprehensively assess patient satisfaction in diverse healthcare settings. Furthermore, the specific characteristics of the practice, such as physician communication style and the overall patient experience, play a larger role than the employment model alone.
The declining share of physicians in private practice is a significant trend, impacting healthcare access and delivery models. This shift is partly influenced by larger healthcare systems’ financial performance, like the recent elevance health earnings q1 change, cyberattack, medicaid, and medicare advantage report which highlights the complexities of the current market. Ultimately, understanding these financial pressures is key to addressing the dwindling number of independent physicians.
The Future of Private Practice: Share Of Physicians Working In Private Practice Dip

Source: medscape.com
The decline in private practice physicians is undeniable, but it doesn’t signal the inevitable demise of this model. Instead, it points to a need for adaptation and innovation. The future of private practice will be shaped by those who embrace change and strategically leverage emerging technologies and evolving patient expectations. Several potential scenarios are emerging, each with its own set of challenges and opportunities.
Potential Scenarios for the Future of Private Practice
Several paths are possible for private practices. Some may consolidate, forming larger groups to gain negotiating power with insurers and invest in technology. Others may specialize in niche areas, offering highly specialized care to a defined patient population. Still others may find success by integrating technology to provide more efficient and accessible care. The successful practices will be those that anticipate and respond to the changing needs of both patients and physicians.
The Role of Technology and Telehealth
Technology is no longer a luxury for private practices; it’s a necessity. Telehealth, in particular, has become a game-changer, allowing physicians to expand their reach, offer convenient appointments, and manage chronic conditions more effectively. Electronic health records (EHRs) streamline administrative tasks, improve patient communication, and facilitate data analysis for better decision-making. Successful practices will integrate these technologies seamlessly into their workflow, improving efficiency and patient satisfaction.
For example, a dermatology practice might use telehealth for initial consultations and follow-ups, reserving in-person visits for procedures requiring physical examination. This model allows them to see more patients while maintaining a high level of care.
Examples of Successful Adaptations
Many private practices are already adapting and thriving. Consider a small cardiology practice that partnered with a larger hospital system for administrative support and access to advanced diagnostic imaging. This collaboration allows the practice to maintain its independent identity while benefiting from the resources and economies of scale offered by the larger system. Another example is a group of independent pediatricians who formed a collaborative network to share resources, negotiate better insurance contracts, and leverage their combined expertise to attract and retain top talent.
This demonstrates the power of strategic partnerships and collaborative models.
Emerging Models of Private Practice
Several distinct models of private practice are likely to emerge:
Boutique Practices: These highly specialized practices will cater to a niche patient population, offering personalized and high-touch care. Think of a concierge internal medicine practice focusing on executive health or a specialized fertility clinic. The focus is on personalized attention and a premium service, justifying higher fees.
Virtual Practices: These practices operate entirely online, utilizing telehealth technology to deliver care remotely. They offer convenience and accessibility to patients in remote areas or with mobility limitations. A successful virtual practice would require a robust technological infrastructure and a focus on patient engagement to ensure positive outcomes and high satisfaction.
Integrated Practices: These practices collaborate with other healthcare providers, such as hospitals, specialists, and ancillary services, to offer a comprehensive and coordinated care model. This approach improves patient care coordination and reduces fragmentation of services. A good example is a primary care practice that integrates with a local pharmacy and mental health clinic to offer more holistic care under one umbrella.
Hybrid Models: Many practices will likely adopt hybrid models, blending elements of traditional in-person care with telehealth and other technology-enabled services. This allows for flexibility and responsiveness to patient preferences, offering both in-person and remote options depending on the patient’s needs and the nature of the visit.
Final Review
The decreasing share of physicians in private practice is a complex issue with significant implications for the future of healthcare. While the economic pressures and systemic changes pushing physicians towards employment are undeniable, the potential consequences for patient access, the doctor-patient relationship, and overall care quality are equally concerning. Understanding these trends and exploring potential solutions – from technological advancements to innovative practice models – is crucial to navigating this evolving landscape and ensuring the best possible care for patients in the years to come.
The future of private practice isn’t necessarily bleak, but it demands adaptation and innovation to thrive.
Answers to Common Questions
What are some examples of successful private practices that have adapted?
Some practices have successfully adapted by specializing in niche areas, utilizing telehealth, forming partnerships with other practices, or focusing on concierge medicine models.
How does the decline in private practice affect rural areas?
Rural areas are disproportionately affected, often facing physician shortages as private practitioners retire or seek employment elsewhere, leading to reduced access to care.
What role does technology play in the future of private practice?
Technology, particularly telehealth, can be crucial in expanding reach, improving efficiency, and reducing overhead costs for private practices.
Are there any government initiatives aimed at supporting private practices?
While specific initiatives vary by location, some governments are exploring policies to address the challenges faced by private practices, such as tax incentives or loan programs.